The Australian allied health workforce, as with other health professions, is maldistributed and in short supply in rural and remote areas1,2. Continuing allied health workforce insufficiency affects many rural services and communities2,3. Staff retention is a core element of sustainable health service delivery4 but rural services encounter persistent recruitment and retention problems to the extent that some positions are filled only sporadically. Workforce shortages result in rural allied health professionals working long hours and having little peer or service support4. Service delivery to rural and remote communities is further complicated because relatively small numbers of people in need are dispersed over large geographic areas4, while allied health professionals tend to be located in large regional centres. Thus, considerable time and distance costs are incurred by health professionals who travel to people in need, and by those people who travel to access services. These issues are amplified in the case of people with disabilities, their carers and those who provide specialist support services5,6.
The allied health workforce falls into two broad sectors: health and disability. Allied health professionals in the health sector are generally located in hospitals, primary health care services, acute rehabilitation services, and private practice. In the disability sector, allied health professionals work within government and funded or charitable non-government agencies, schools, communities, and private practice7. In New South Wales (NSW), disability services are planned, funded and supported by the state Department of Family and Community Services - Ageing, Disability and Home Care, which is ministerially, administratively and financially separate from the state health department (NSW Health)8. Allied health professionals such as physiotherapists, occupational therapists and speech pathologists assist people with disabilities (clients) and their families to maximise their participation in the community. Disability services provide therapy, case management, behaviour support, accommodation, employment, day services, respite care, information and advocacy across the life span to people with a disability and their families7,8. Allied health professionals in the disability sector are commonly called 'therapists' and that term will be used in this article.
A person with a disability is covered by the NSW Disability Services Act 1993 if the disability is (p4)7:
...attributable to an intellectual, psychiatric, sensory, physical or like impairment/s; and is permanent; and results in significantly reduced capacity in one or more major life activities such as communication, learning, mobility, decision-making or self-care; and has a need for support.
Thus, the disability sector encompasses a broad range of conditions and needs, including children and adults with intellectual and developmental disabilities (from birth) such as cerebral palsy, autism spectrum disorders, and Down syndrome; people with acquired disabilities such as brain injury and spinal cord injury; and irreversible physical injuries such as burns and amputations9.
The project's aim was to investigate service delivery and workforce retention issues of importance to policy-makers , service managers, and senior therapists providing services to people with disabilities in rural and remote western NSW. This project is a discrete phase of a larger multi-phase program of research reported elsewhere10.
Setting
The region under study accounts for more than 70% of the land area of NSW, stretching from the state's borders with Victoria in the south, South Australia in the west, Queensland in the north, and to the Great Dividing Range in the east. In 2009, the estimated resident population was approximately 604 00010,11. The region's population is dispersed among large regional towns of 20-40 000 residents, smaller towns of 1-3000 residents, and isolated rural communities of less than 1000 people. Some people live on remote properties (farms) many kilometres from their nearest neighbours and hundreds of kilometres from towns. At the 2006 Census, the region's population accounted for 9% of the state's population (Pers. comm; NSW Department of Family and Community Services - Ageing, Disability and Home Care, 2011)10. People aged over 65 years accounted for 14.9% of the region's population, compared with 13.8% for the state as a whole. Indigenous people accounted for 5.6% of the region's population compared with 2.1% for the state as a whole. People with a disability accounted for 7.2% of the region's population. Two of every three people with a disability required some type of assistance with activities (Pers. comm; NSW Department of Family and Community Services - Ageing, Disability and Home Care, 2011)10.
Recruitment and data collection
Policy documents: Purposeful12 and snowballing13 sampling techniques were used to collect 40 relevant policy documents and operational guidelines providing current direction to staff working in government disability services in NSW. The documents spanned the years 1993-2016 (from the introduction of the NSW Disability Services Act 19937 to the end of the Stronger Together14 initiative). With the assistance of key government department staff, 20 documents were initially identified as relevant to the study. A further 3 policies were identified by searching the initial 20 documents for related documents. Government websites were searched directly to access a further 8 documents. One member of the research team (KB) was seconded to work on the project from the policy section of the government department and using her 'insider' knowledge an additional 9 policy documents were collected. All documents were collected and reviewed between October 2010 and December 2010.
Each document was read and a summary made of the key policy content. Based on this initial summary, the documents were divided into 3 tiers:
- Tier 1 included 12 overarching NSW Government policy documents including major disability-specific (n=6) and general population (n=6) related documents.
- Tier 2 included 18 government agency specific policies which were divided according to whether they were client-focussed (n=12) or workforce-focussed (n=6).
- Tier 3 related to the implementation of Tier 2 policies and included 10 government agency operational guidelines which were also divided into client-focussed (n=9) and workforce-focussed (n=1).
The collation and qualitative content analysis13 of these documents generated themes that informed development of the semi-structured interview proforma.
Senior staff discussions: Purposeful sampling12 resulted in discussions with 50 senior staff employed either by government or by non-government agencies (NGOs) supporting service delivery to people with a disability in western NSW (Table 1). Government agency regional staff identified 27 key senior staff based in either western region, or in the central office. In western region, senior staff (n=12) included executive team members, planning team members, senior therapists who provide clinical supervision to therapists, and senior managers overseeing community support staff including therapists. Central office staff (n=15) included senior therapy practice leaders, and the senior managers overseeing relevant directorates. Regional staff also identified contacts within non-government disability and health agencies (n=23). Twelve senior staff managed services delivered in western NSW via outreach from head offices in Sydney. Eleven staff managed agencies based in western NSW. Within the disability sector, the majority of agencies received some level of funding from the state government agency.
Table 1: Characteristics of government and non-government participants by location
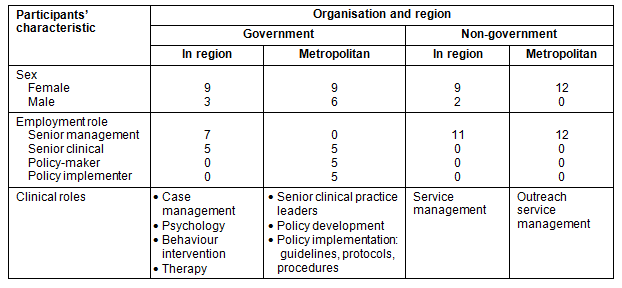
Semi-structured interviews were chosen as a data collection method because they provide an opportunity for participants to address broad topics relevant to the project aims, and to expand on issues arising from these topics12,13. Interviews were sometimes held with individuals and sometimes with small groups, depending on participants' availability and location. With small groups, the interaction between participants created a group dynamic as they both explained their own position to the group and questioned others' points of view15. Two research team members (AD and KB) conducted all interviews.
Data collection with senior staff occurred from October 2010 to April 2011. Government agency senior staff were asked to describe the issues that influenced policy development, discuss the unintended outcomes of policy, comment on how policy was interpreted 'on the ground' and describe how they measured the impact of policy. Non-government organisation senior staff were asked to describe how the services they provided were influenced by state government agency policy directions and guidelines and to describe challenges they encountered in implementing policy. Background data were also collected about the structure and mode of western region-based service delivery for each organisation (eg centre-based, outreach, technology-based). With participants' permission, interviews were audio-recorded. Sessions ranged from 90 min to 2 hours duration.
Data analysis
Comprehensive summary notes derived from the audio-recordings of interviews were sent to participants for review and comment. Participants verified the content of the summaries with minor clarifications. Summaries were analysed using thematic analysis to identify the main issues related to policy development and implementation16. Constant comparison was then used within and across data sets to identify commonalities and differences17,18.
Ethics approval
Ethics approval was granted by the University of Sydney Human Research Ethics Committee (#10-2009/12194). Written consent was obtained from all study participants. All interviews were anonymised. All data were kept confidential.
There was significant overlap between the issues raised by government agency and NGO senior managers demonstrating a joint understanding of the issues facing government and non-government agencies delivering services to people with a disability in regional, rural and remote areas of NSW. The issues identified by government agency senior staff and those raised by NGO managers were synthesised (Fig1) to develop 5 themes:
- Challenges to implementing policy in rural and remote NSW
- Impact of geographic distribution of workforce and clients
- Workforce issues - recruitment, support, workloads, retention
- Equity and access issues for rural clients
- Important role of NGOs in rural service delivery and support.
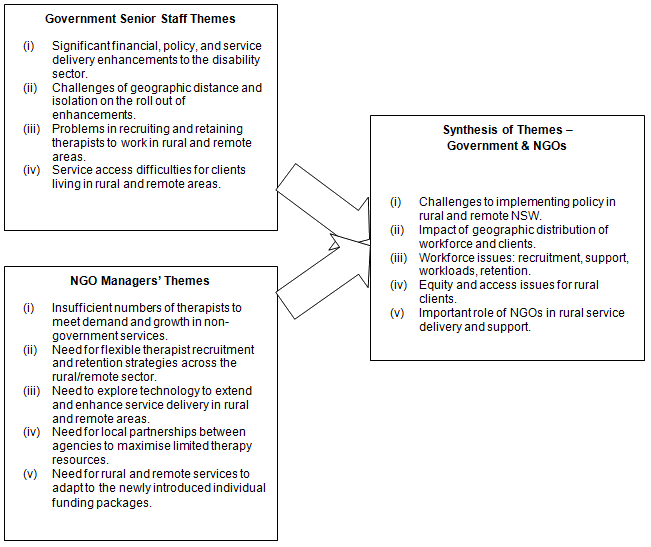
Figure 1: Stage 1 - Synthesis of themes. NGO, Non-government organisation; NSW, New South Wales.
Challenges to implementing policy in rural and remote NSW
Policy-makers and senior managers described a centralised process of policy development which incorporated feedback from regional staff. The intention of policy-makers is to develop policy which provides direction to therapists, regardless of location, ostensibly to ensure that services are provided to clients in a coordinated and equitable manner related to best practice. Not surprisingly, different organisations had different priorities and policies.
Sometimes the policies are written with metro populations in mind and they are not necessarily applicable to how we can deliver services in this region but in other ways I think we work really well to accommodate the policies and still provide services in a way that is doable. (Senior therapist, government agency, region)
An example of the mismatch between policy intent and implementation can be demonstrated by considering the impact of workforce shortages on service provision. Therapists described circumstances where certain clients might not receive services, not because they were ineligible per se, but because policy-imposed service practices and priorities, combined with limited workforce, resulted in those clients simply never receiving services.
They [policies] don't take into account where the person lives. It's about their needs. We try to cluster those [high, medium and low referrals] when allocating to make it travel efficient for the therapist. (Senior therapist, government agency, region)
We prioritise according to [the policy], but for our immediate response people, we do not meet the time frames associated with that. The time frames for response are a regional issue - not always possible to respond in time. There's no context allowed to be applied to that. (Senior therapist, government agency, region)
The literature and lay media are replete with accounts of the negative impacts of funding reductions and service contraction on service users in rural areas. However, increased funding and service expansion can also have unanticipated impacts. For example, the new policy initiative (Stronger Together14) resulted in increased funding aligned with changed policy expectations and requirements. Although not raised as a negative per se, senior managers noted that rapid increases in availability and accessibility of services could not be achieved for various reasons: (i) it was rarely possible to increase the rural workforce rapidly, regardless of the funds available; (ii) changes in role responsibilities and inter-linkages take time to enact and achieve their full potential; (iii) later policy changes may overtake or supersede earlier changes, such that 'change fatigue' becomes a risk to service and workforce sustainability.
We really don't have enough staff to cover what we need to cover. We used to talk about recruitment being a real problem but that's improving for us. We are always down someone somewhere ... and that does have an impact on service delivery, and because our numbers are not large that is a significant issue. (Senior manager, government agency, region)
It is a challenge to keep up enthusiasm levels of staff. We do want to become an employer of choice. (Senior manager, government agency, region)
Recent initiatives such as Stronger Together14 had enabled the number of therapy assistants in the region to increase, although participants believed the opportunity to be currently under-utilised.
I think it needs to be recognised that there are 3 [government agency] therapy assistant positions across the region which makes it very difficult to manage how we are going to maximise the effectiveness of those positions. (Senior manager, government agency, metropolitan)
Therapy assistants reportedly support clients and assist therapists in ways that enhance service delivery and client wellbeing, as well as alleviating certain workload demands on therapists. Participants acknowledged that the implementation of these therapy assistant positions and their inclusion in the rural workforce, while welcome, required careful management. Most particularly, therapists believed that existing staff needed to be fully informed of, and understand, the nexus between their own roles and those of the new service providers such as therapy assistants.
At the moment in terms of how those positions are going to be best utilised will probably depend on where they are based ... I think the expectation is that referrals will be put in for them ... but as a senior group how we are going to manage that, we're at a bit of a loss to know. (Senior therapist, government agency, region)
Impact of geographic distribution of workforce and clients
The vast distances encountered in rural and remote NSW complicate service delivery to people with a disability and their family members. The 'hub and spoke' model of service delivery enables larger 'hub' towns to provide services along 'spokes' to smaller towns, and rural and remote communities19,20. However, managers and therapists noted that operating a 'hub and spoke' model of service delivery resulted in extensive travel for staff and clients leading to a number of related issues:
- constraints in balancing the implementation of policy with geography:
There are pros and cons - it does create more travel and we have discussed whether there is equity in service provision - higher level of frequency of service to people living in that town. (Senior therapist, government agency, region) - difficulty operating an interdisciplinary model given distribution of staff positions
- limited opportunities for personal and professional development:
There are challenges ... in regional areas. If you lived in Melbourne or Sydney, the local hospital or local agencies or universities will offer free workshops or seminars so people can nip out in their lunch hour and tick off some PD [professional development] hours, learn something new. We get flyers about it but I'm not going to fly to Sydney for a 2 hour talk so we can't do that. (Senior therapist, government agency, region) - Variation in availability of services provided by others (ie NGOs, other government departments and private therapists)
- Occupational health and safety issues related to travel time and method (eg flying or driving):
[Travel] is part of the job and it is expected. The manager's role is to ensure that they [therapists] don't do too much [travel]. It's almost just down to normal practice. You can't often fly so there's lots of driving involved for people in those locations. We try to plan it so you don't drive constantly, keep the 'to and fro' to a limit. That doesn't fit particularly well with the policy...you don't make someone drive 2-3 hours to see one person you try to get the most benefit from that trip [and] pick up other people who are a lower priority. (Senior manager, government agency, region)
There's a lot of down time for therapists in cars. (Senior manager, government agency, region)
All participants reported widespread use of email and telephone as modes of communication between therapists, and between therapists and clients.
A mobile phone that works and has good area coverage has been, I think, the single best invention ... Even in the remote areas they have towers ... and along with that is internet access ... it's just changed our lives. (Senior therapist, government agency, region)
Managers in rural and remote locations discussed the potential of the National Broadband Network (NBN) to improve internet connection and speed, thus making use of web-based technology a more reliable and sustainable option for the future.
NBN certainly will make a difference to [internet access in] some of our remote communities because in places like [very remote community] there are only certain places where you can take a mobile phone call and access the internet. So [the NBN] will have implications for our therapy service delivery in very remote communities. (Senior manager, government agency, region)
We will look at our practices, we will look at our marketing and then we are also looking to innovate...so what can and cannot be done using web technology? We'd like to 'push the envelope' with that as much as we can. It enhances access to the service in terms of therapy, rather than doing it in a block we might be able to space it out and we might be able to increase the impact of the therapy that we give. In terms of our client flow it gives us more flexibility in our service delivery, and it adds to the evidence base of what works and do they still work if you do it in this way? (NGO, clinical director, metropolitan)
Workforce issues - recruitment, support, workloads, retention
Therapist recruitment and retention in rural and remote areas is a common theme in the literature, and was often raised in the interviews. A particular issue was the retention of therapists who had developed skills pertinent to rural and remote practice.
Recruiting therapists and then retaining them is an issue ... we have had a number of therapists come straight out of university and then probably only stay for 2 years [although] they get good support and training from us. (NGO, senior manager, region)
Some participants noted that a clear career path would likely assist in that respect.
There needs to be a career path in therapy. (Senior manager, government agency, metropolitan)
Government agency managers reported one strategy aimed at enhancing retention through career development and support: the creation of senior therapy positions designed, in part, to provide a career structure for the agency's therapists in the region. The role of these experienced senior therapists was to provide supervision, mentoring and support for less-experienced therapists. However, an unintended effect has been that the senior therapist roles involve greater administrative responsibilities and so they now have much less direct clinical involvement. Promotion of existing staff to senior positions thus left gaps in the numbers of therapists providing direct service interventions.
An innovative recruitment strategy employed by the government agency's regional office enabled therapists to choose where they live, rather than moving to a town in which the position was nominally located, provided they agreed to deliver outreach services to surrounding areas. The strategy, anecdotally, has resulted in increased recruitment and greater retention of therapists in the region.
This is a recruitment strategy in [the region], our therapy positions are [geographically] flexible and we usually advertise them as flexible. (Senior manager, government agency, region)
There is a note on the advertisement that there is an expectation that you will travel because the service needs to be provided to an area. (Senior manager, government agency, metropolitan)
At least you have a skilled person whereas you might not have anyone ...it is one of our most successful recruitment strategies. (Senior therapist, government agency, region)
Managers and therapists working in NGOs reported a range of recruitment and retention strategies used to attract and retain therapists to work in western region. These strategies included financial incentives, flexible work arrangements and new graduate scholarships.
The salary packaging is good, but people see it as a benefit only over and above the award rate. It is difficult to advertise the benefit of packaging, because it is so individualized. (NGO senior manager, region)
Equity and access issues for rural clients
Policy-makers and managers reported an increasing, policy-driven, movement towards a person-centred approach to delivering services to people with a disability and their families. These participants reported that the person-centred approach fitted with the outputs-based funding model being implemented with non-government service providers and individualised funding packages increasingly provided to clients. Receiving individualised funding and advocating a person-centred approach were acknowledged by participants as good policy initiatives. However participants were concerned that the individualised funding initiative potentially exacerbated inequity issues for clients living outside the main regional towns. Outreach therapy services to people living in smaller towns, and rural and remote areas were dependent on the availability, location, and expertise of therapists. Thus, for many clients living in isolated rural communities the services are not available for clients to purchase. Reported barriers to equitable access to therapy services for rural clients included:
- restrictive and differing service eligibility policies
- geographic distance and isolation resulting in some areas receiving little or no services while others have a choice of local service providers:
[When we do outreach to remote communities] the families and the other therapists, like Health therapists, expect the same level of support as they would if they lived in a large town. (Senior therapist, government agency, region) - lack of transport to services
- lack of choice with limited numbers of suitably experienced private therapists
- uncoordinated and disjointed service delivery:
Our rural therapists do need to be very skilled because they will be going into potentially an area where there is not a lot of other support and they'll be asked all sorts of questions by all sorts of people and the more experience they have they will be able to deliver a very good service. (Senior therapist, government agency, region) - lack of therapists who are 'hands-on' clinicians
- lack of follow up after assessment and intervention
- lack of follow up after 'fly-in fly-out' specialist service providers have conducted outreach
- lack of access to trial and modification of equipment and long waiting times for assessment of the need for equipment.
There was consensus amongst participants that equity of access issues are more marked for clients from Aboriginal backgrounds. The region has the highest proportion of rural and remote Aboriginal people in NSW11. However, Aboriginal people are under-represented in accessing government and non-government disability services. Participants thought some of the reasons for this under-representation included:
- disability services not targeting the needs of Aboriginal people
- Aboriginal communities having a different view of disability
- Aboriginal communities having an historical distrust of 'welfare' services
- The time and effort required to make links with different Aboriginal communities:
Local knowledge is very important [working with Aboriginal people] and if you are going into an area where you don't have that local knowledge, then you find someone who has by word of mouth. (Senior therapist, government agency, region)
We try to take the service to the [Aboriginal] person in the context where they feel comfortable so we wouldn't be expecting them to come into a centre-based program because it's been shown time and time again that they won't come. (Senior therapist, government agency, region)
There is a sense in the Aboriginal communities that they don't want fly-in fly-out services, they want people on the ground or they want someone they can trust. You need to have the respectful communication in place. (Senior manager, government agency, region)
Important role of non-government organisations in rural service delivery and support
There are many NGOs that receive government funding to provide specialised services and support to clients with a disability in the region. Participants acknowledged the desirability of government and non-government services collaborating in order to enhance service provision generally, as well as at the individual client level. Nonetheless, managers reported current levels of collaboration were variable and often dependent on relationships formed between individuals rather than sustained by systemic arrangements.
We see ourselves in isolation at a locality rather than seeing ourselves as part of a fluid, complex allied health service system. How do we integrate [our] very sparse resources into that so we get a seamless allied health system? (Policy-maker, government agency, metropolitan)
We work on a case-by-case basis ... potentially it can very murky for the family ... needs a lot of communication and close collaboration between those therapists. (Senior therapist, government agency, region)
Participants suggested strategies such as:
- developing a local area plan for utilising the expertise of therapists across organisations
- pooling resources to recruit and retain therapists working in western region
- encouraging formal (eg professional development) and informal networking opportunities for therapists across agencies working in an area:
It can get very messy ... in some areas the government agency therapist and the NGO therapist are involved with the one client and in other areas there is clear demarcation ... it's quite variable across the region dependent on skills of therapists in either organisation, very dependent on if the position is filled. (Senior therapist, government agency, region)
There do not seem to be clear communication channels between NGO therapy service provision and [government agency] therapy service provision ... there aren't formal or clear guidelines around that so it comes back to the individual therapist ... that's definitely a gap that we have in the region. (Senior manager, government agency region)
Just by sharing information [between organisations], there is a win-win situation. (NGO senior manager, region)
Discussion
Participants came from three broad levels within disability services: policy development, management, and clinical management. It appeared that information transfer between the levels was inconsistent, although commitment to providing best-practice services was universal. However, the existing situation appeared to be a source of disappointment and frustration at various times and in varying ways to participants. There would appear to be benefit in developing strategies for effectively passing relevant information between people within each broad level and between organisations.
Participants raised some issues that are commonly reported in the rural health literature with respect to workforce and service delivery but rarely in the context of allied health and disability services. Some innovative strategies were reported, such as the approach to recruiting therapists. However, the full ramifications in terms of balancing workload and travel, and a clinical workload management system that was designed for metropolitan practice, are yet to be appreciated. Likewise, the potential influence of relatively recent innovations in service delivery, such as therapy assistants, information technology, and trans-disciplinary approaches, are important considerations within the region and across rural and remote areas in general. These and other innovations will likely extend the coverage provided by therapists within the region.
Non-government organisations play a significant role in service delivery and support in the region. Participants recognised the potential benefits of collaboration, between therapists from different organisations, both in terms of peer support, and service delivery to clients. Inter-sectoral collaboration between therapists, in the context of a relatively small but widely distributed workforce, could have considerable benefits in terms of peer support, professional development, and efficiency of service delivery. Greater collaboration could result in more clients receiving timely clinical care and support.
Strengths and limitations
Although the coverage of disability services and service managers providing care to people with a disability in rural and remote western NSW was comprehensive (numerically and geographically), the findings might not be representative of the broader rural and remote allied health workforce in mainstream health-service settings. Some findings may be specific to the disability sector and/or rural and remote western NSW. That said, the findings are broadly in line with rural health workforce literature1,2,21.
Issues relating to disability services delivery and workforce in rural and remote areas have been little researched. Participants in this qualitative study raised some workforce and service delivery issues similar to those reported in the rural health literature, but rarely in the context of allied health and disability services. Other issues appeared to be especially related to the disability sector; most notably the significant service delivery and support role played by NGOs. Participants recognised the need for practitioners working for different organisations, in rural areas, to collaborate both in terms of peer support, and in terms of service delivery to clients. Later phases of this project will monitor developments with respect to such issues, and develop evidence that can be used by policy-makers, managers and therapists to address the issues.
Further research is required to investigate clients', carers' and parents' perceptions of service delivery for people with a disability in rural and remote areas in order to ensure that service changes are based on comprehensive input from all stakeholders. The perceptions of policy-makers , managers and senior therapists need to be established empirically in terms of client service provision and workforce statistics. The results of this study provide guidance about the types of data that may best inform future policy development.
Acknowledgements
The authors thank the participants who generously gave their time to this phase of the study. This project is supported by a NHMRC Partnership Grant (ID571446) and NSW Department of Family and Community Services: Ageing, Disability and Home Care.
References
1. Keane S, Smith T, Lincoln M. A survey of the rural allied health workforce in New South Wales to inform recruitment and retention. Australian Journal of Rural Health 2011; 18: 38-44.
2. Department of Health and Ageing. Report on the audit of health workforce in rural and regional Australia. Canberra, ACT: Commonwealth of Australia, 2008.
3. Battye K. Workforce shortages or dysfunctional service models? In: Proceedings, 9th National Rural Health Conference; 7-10 March 2007; Albury, NSW, Australia; 2007.
4. Veitch C, Battye KM. Rural health workforce: planning and development for recruitment and retention. In: S-T Liaw, SI Kilpatrick (Eds). A textbook of Australian rural health. Canberra, ACT: Australian Rural Health Education Network, 2008; 113-127.
5. Dew A, Veitch C, Lincoln M, Brentnall J, Bulkeley K, Gallego G et al. The need for new models for delivery of therapy intervention to people with a disability in rural and remote areas of Australia. Journal of Intellectual & Developmental Disability 2012; 37(1): 50-53.
6. Dew A, Bulkeley K, Veitch C, Bundy A, Gallego G, Lincoln M et al. Addressing the barriers to accessing therapy services in rural and remote areas. Disability & Rehabilitation 2012 (in press).
7. New South Wales Government. Disability Services Act 1993 No.3. Sydney, NSW: New South Wales Government, 1993.
8. Bundy A, Hemsley B, Brentnall J, Marshall E. Therapy services in the disability sector: Literature review. Sydney, NSW: NSW Department of Ageing, Disability and Home Care, 2008.
9. Australian Institute of Health and Welfare. Disability in Australia: intellectual disability. Canberra, ACT: AIHW, 2008.
10. Veitch C, Lincoln M, Bundy A, Gallego G, Dew A, Bulkeley K et al. Integrating evidence into policy and sustainable disability services delivery in western New South Wales, Australia: the 'wobbly hub and double spokes' project. BMC Health Services Research 2012; 12: 70.
11. Australian Bureau of Statistics. 2009 Estimated Resident Population by Statistical District. (Online) 2009. Available: http://www.abs.gov.au/AUSSTATS/abs@.nsf/DetailsPage/3235.02009 (Accessed 15 January 2011).
12. Creswell J. Qualitative Inquiry & Research Design: Choosing among five approaches, 2nd edn. Thousand Oaks, CA: Sage, 2007.
13. Bryman A. Social Research Methods, 3rd edn. Oxford: Oxford University Press, 2008; 529-533.
14. NSW Department of Ageing, Disability and Home Care. Stronger together: a new direction for disability services in NSW 2006-2016. Sydney, NSW: NSW Government, 2006.
15. Braun V, Clarke V. Using thematic analysis in psychology. Qualitative Research in Psychology 2006, 3: 77-101.
16. Freeman T. 'Best practice' in focus group research: making sense of different views. Journal of Advanced Nursing 2006; 56: 491-497.
17. Glaser BG, Strauss AL. The discovery of grounded theory: strategies for qualitative research. London: Weidenfeld and Nicolson, 1968.
18. Charmaz K. Constructing grounded theory. Thousand Oaks, CA: Sage, 2006.
19. Battye KM, McTaggart K. Development of a model for sustainable delivery of outreach allied health services to remote north-west Queensland, Australia. Rural & Remote Health 3(3): 194. (Online) 2003. Available: www.rrh.org.au (Accessed 26 April 2012).
20. Jones P, May J, Creighton A. Health service models. In: S-T Liaw, SI Kilpatrick (Eds). A textbook of Australian rural health. Canberra, ACT: Australian Rural Health Education Network, 2008; 105-112.
21. Davies S. An innovative model to attract and retain allied health professionals in rural areas. In: Proceedings, SARRAH 2006 Conference; 13-16 September 2006. (Online) 2006. Available: http://www.ruralhealth.org.au/conferences/sarrah2006/Docs/Program/index.htm (Accessed 26 April 2012).


