While group self-management programs have demonstrated effectiveness across multiple populations1-3, geography precludes participation in areas without a critical mass of participants or healthcare providers. Northwestern Ontario (NWO) is one such area. It is sparsely populated (0.45 people/ km2), with 48% of the population living in remote areas outside of the major city, Thunder Bay (Fig1)4. Healthcare human resources are limited, professionals often serve clients spanning the entire continuum of care, and peer support groups are limited. As noted in a report on healthcare in Canada, offering services via telehealth could improve access to care and services in remote areas5. Accordingly, the innovative videoconference delivery of the Moving On after STroke (MOST®) self-management program was developed to provide access to a supervised, community-based, self-management program with both group exercise and peer-support for those living in remote communities. This article reports on remote participants' satisfaction with the program, and offers suggestions for improvement.
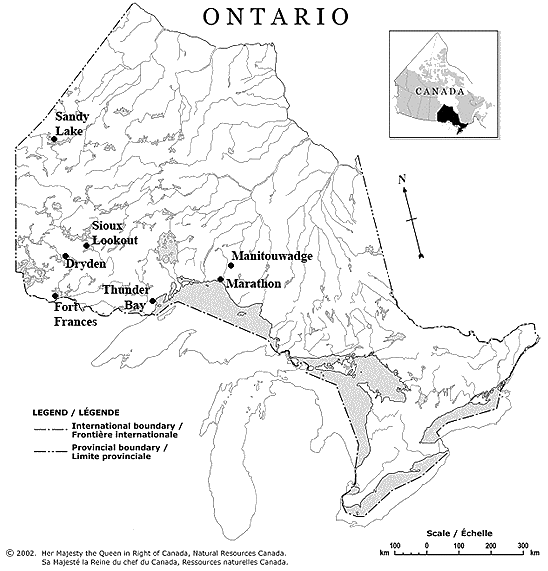
Figure 1: Map of participating Moving On after Stroke Telehealth Remote (MOST-TR) remote sites in Northwestern Ontario.
Telehealth
Telehealth is an all-inclusive term for the provision of health services using information and communication technology. Recently, videoconferencing, a type of telehealth, has been used to deliver caregiver support programs6-8 and self-management programs for people with chronic illnesses9,10 and stroke6,11. Some of these programs include an exercise component11,12.
Although videoconferencing has been found to better establish and maintain rapport compared with telephone conversations, it is not equivalent to in-person interactions13-15. Healthcare professionals have described benefits of videoconferencing, such as improved access to health services, improved health outcomes, cost-effectiveness, and enhanced social support14,16,17. Reported barriers include poor visual representation and 'audio lags'18,19, the lack of face-to-face presence which prevents usual aspects of communication such as shaking hands or being able to sense smell20, and the lack of local, onsite videoconference support13,14,21. Reported strategies to improve the videoconference experience include8,18,20:
- providing an initial face-to-face meeting
- using technological features such as switching between pre-set camera positions and zooming in for close-ups
- enhancing the social and technical role of a facilitator.
Less information is available about patient experiences and satisfaction with videoconferencing, and there are still many knowledge gaps16,22,23.
Moving on after Stroke (MOST®)
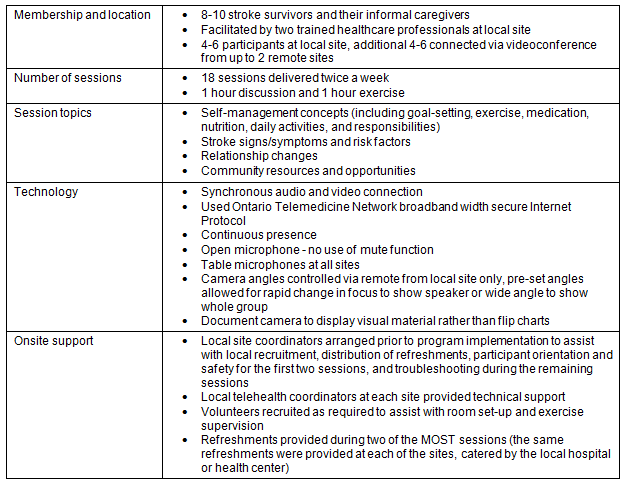
MOST® is a group-based, self-management program for stroke survivors and their caregivers living in the community24 (Table 1). The program provides information about stroke-related topics and facilitates discussion, problem solving, goal-setting, and self-management skills in a supportive environment25. Participation in MOST is associated with improved community reintegration and positive health behaviour changes in stroke survivors24. An initial pilot study investigated the feasibility of using videoconference technology between urban centres to co-facilitate MOST26. A subsequent study27, MOST Telehealth Remote (MOST-TR), used videoconference technology to connect facilitators and Thunder Bay participants with stroke survivors at remote videoconference sites in NWO.
Table 1: Description of Moving on After Stroke Telehealth Remote (MOST-TR) program
Videoconference impact on groups
MOST is delivered in a group format to promote and encourage information sharing, peer support, and connection among participants. The psychological benefits and therapeutic factors of groups include sharing experiences, being motivated by one another, and comparing oneself to others in the group28. These group benefits are impacted by the group's cohesion which is in turn influenced by the videoconference environment28.
The development of group cohesion, peer support, and participant involvement are critical to the success of MOST24. As such, an understanding of the unique experience of remote participants is necessary. The objectives of this research were to explore remote participants' experiences with the MOST-TR group intervention, to identify factors which enabled and/or created barriers to participation, and to learn about participants' perspectives on the technological, educational, and/or interpersonal strategies that may enhance the delivery of videoconference-based group programs.
Design
This qualitative study used an interpretive methodology29-34 to identify the experiences of the remote MOST-TR participants. Semi-structured, face-to-face interviews were used. Ethics approval was received from all participating sites.
Participants
Remote participants from MOST-TR were recruited post-program completion. Community-dwelling stroke survivors between 3 and 18 months post-stroke, and their caregivers were recruited to achieve a range of experiences30,32; and were chosen from different sites with varying numbers of local participants. Purposive sampling included women and men, younger and older participants, quieter and more active participants, stroke survivors and caregivers, those who completed the program and those who dropped out before completion.
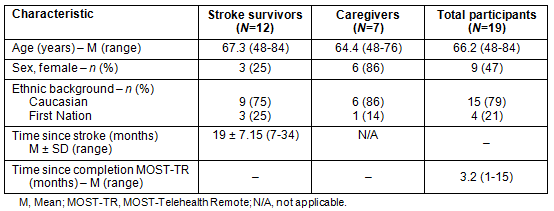
Three phases of recruitment occurred between March and October 2007 in an attempt to reach data saturation. Letters of invitation were sent to 27 potential participants. Those interested were telephoned to arrange an interview. Nineteen people from six communities within NWO participated in this study (Fig1, Table 2). Unfortunately, those who discontinued MOST-TR did not agree to participate in this study. Four of the participants were able to attend one MOST session in person, in Thunder Bay, on separate occasions.
Table 2: Description of participants
Data collection and analysisFollowing informed consent, interviews were conducted at the participants' home in all but four situations. For reasons of mutual convenience, one was held at the interviewer's workplace and three at the remote videoconference site. One stroke survivor-caregiver dyad was interviewed together at the couple's request.
An interview guide was used to elicit perspectives on the group videoconference experience; flexibility allowed for exploration and elaboration of participant experiences34. The guide, which was piloted prior to the study and subsequently revised, focused on four areas: (i) previous experiences with groups or videoconferencing; (ii) participation in the discussion portion of MOST-TR via videoconference; (iii) participation in the exercise portion of MOST-TR via videoconference; and (iv) factors enabling or limiting participation in the group (Fig2).

Figure 2: Interview guide.
Interviews were conducted by the first author who had a pre-existing relationship with participants as co-facilitator of the MOST-TR program. Each interview lasted between 30 and 60 min, and was audio-digitally recorded.
Interviews and analysis proceeded according to an iterative pattern, using methods of constant comparison. This involved continuously comparing new information with previously collected data and modifying the interview questions accordingly for ongoing data collection35. After each interview, the data were verified with the participant and clarifications made as required. Immediately post-interview the interviewer recorded reflections and attempted to identify possible new patterns.
Interviews were transcribed verbatim, reviewed, and re-read to absorb the data. New data were coded, analyzed, and compared with existing data, and the interview guide was modified to reflect any new patterns or emerging data.
An interpretive, thematic analysis was conducted29,31,33. Data were coded using preliminary categories from the interview guide33 using QSR NVivo v2.0 (www.qsrinternational.com). New categories were created as required. Segments of text were organized by codes across all interviews29. Data were retrieved by code and each code was read for patterns29. Patterns were then categorized and sorted based on common features emerging from the data32. An external committee reviewed the analysis.
Rigour
Integrity of the findings was optimized through written reflection and discussion with study advisors and peers on the investigator's identity and possible biases36. This research is fundamentally shaped by the fact that the investigator is a physiotherapist (physiotherapist and related words are official marks used with permission by registered physiotherapists) in stroke rehabilitation and co-facilitated the MOST-TR sessions, from which study participants were recruited.
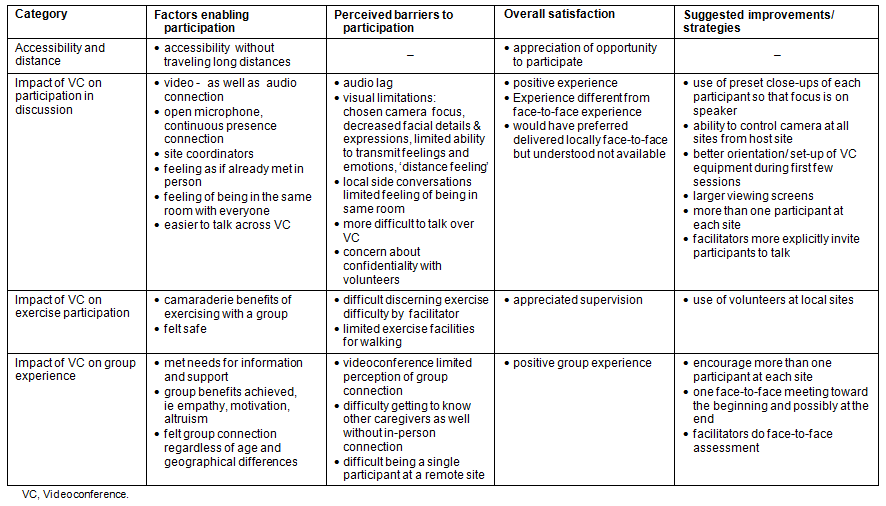
Most participants offered both positive and negative comments regarding their perceptions about the videoconferenced group experience. As summarized (Table 3) and discussed below, issues included:
- accessibility and distance
- experiences of participation in discussion and exercise across videoconference (including technology experiences)
- experiences of group involvement across videoconference
- suggestions for improvement.
Table 3: Summary of interview findings
Accessibility and distance
Participants indicated that due to their geographic isolation, they had come to expect that accessing healthcare services required travelling long distances. As one said:
I think you have to do it [travel] when you're in remote areas. The videoconferencing is much better than the traveling to Thunder Bay.
All participants appreciated the ability to participate in the MOST-TR program and recognized that their participation was only made possible by using videoconference technology.
Participation in discussion and exercise across videoconference
Influence of technology: Participants noted that having both visual and oral connection with others was a supportive factor to their participation. All participants appreciated the ability to see the room and the participants on the video screen, but the quality of the video output was not considered comparable to a face-to-face experience. With videoconferencing, facial details and subtle facial expressions were difficult to discern. These visual limitations were especially evident if there had not been a previous face-to-face interaction. In this case, most participants said it was difficult to recognize someone in person for the first time. As one said: '... like even you - when you came in, I would never have recognized you off the TV, in person'.
However, two participants did not experience the technology as making it difficult to recognize people when meeting them in person. At one point they had been able to participate in a session in Thunder Bay and said:
Well it was like I already knew you's very [pause]. That's the way I felt, when I walked in, I just felt, like, we were old friends.
Ten of the 19 remote site participants said they felt as though they were in the same room at least at some point during the program. One participant explained:
Oh, I felt like I was right there with yous [pause]. It was good. It was just like we were there. I was amazed.
Nevertheless, the technology did not allow all remote participants to feel as though they were in the same room as those at other sites. Some felt there was always a distance between the sites, although this did not necessarily impact their ability to communicate with those at other sites. For example:
I can't say that we were in the same room, because there'd be talking going on in Thunder Bay, that we didn't know anything about. ...I mean there is a distance feeling through telehealth.
The videoconference camera limited the visual connection with the whole group and participants' ability to read subtle facial expressions, body language, and gestures. Camera pre-sets zoomed in on the participant speaking; however, adjustments were only possible locally so the participants at the Thunder Bay site were unable to see a close-up of other remote participants. Within the videoconference environment, the camera chose the focus and one participant expressed frustration over not being able to see other group participants.
Participation in the discussion: Most people said that although they were able to participate in the discussion portion of the session, they would have participated slightly differently had they all been physically together. One participant noted:
I find it's funny if I'm here and if you're way out there and someplace, you know, TV and all that... Feels funny talking to, you know a TV? ... Talk to the TV and you wish you were there sitting, with all the, seeing everybody.
Another reported that he limited his participation because he felt he was disrupting another conversation: 'Yeah, like, like when I talked to them, that conversation stopped, and I didn't want to do that to them'. Upon further exploration, he felt that more invitation to talk by the facilitators would have made it easier for him to participate.
In contrast, one participant who was able to attend a session in person in Thunder Bay felt it was easier to participate across videoconference and found that she actually participated less in person. So, although most participants said that participating via videoconference limited their ability to participate in discussions, this was not a consistent finding.
Participation in group exercise: Participants reported they were comfortable with the exercise experience and were not concerned about safety. They talked about being motivated by the group and benefitting from the camaraderie despite it being across videoconference. However, one stroke survivor-caregiver dyad reported negative experiences with the exercises across videoconference. This couple was frustrated with the stroke survivor's difficulties following the instructions and keeping up with the group. It is possible similar difficulties could occur in a face-to-face environment; however, across the videoconference, his level of difficulty and associated frustration were not evident to the facilitators and therefore were not addressed. Despite the facilitators' ongoing attention to monitor exercise quality and participant safety, the ability to accurately perceive the level of difficulty and respond to the participants' need for support was limited.
Experiences of group involvement across videoconference: A drawback to using the technology was that side conversations and informal socializing at other sites represented a barrier preventing others from feeling part of a group, regardless of the visual and audio synchronicity. One participant felt he was unable to connect with the group well enough to participate as much as he would have liked. Most participants, however, reported feeling a connection with the larger group despite the geographical separation. As one said: 'I think we were part of that group, even though we weren't in the same room. So I think that worked well'.
Participants felt they could learn and share information with one another and receive support from the group. As one participant said:
Well the knowledge, as well as being able to talk to others, and that's what I found most fantastic, with the, with the MOST group. I thought, you know, there's other people out there that are going through the same thing as I'm going through and, I wasn't alone in this thing. 'Cause I had nobody here that I could talk to, that would understand.
Participants appeared to have made a true emotional connection and expressed ongoing concern for each other. During each interview, many asked about the wellbeing of other participants in the group.
Participants identified that across videoconference they were able to gain hope from one another and were motivated by the group. As one said:
The woman that was going to knit, you know, her aim was to start her knitting again. And you could see that she was quite pleased with herself. Like quite pleased. I, ah, consider that as a, a motivation for the group. Because they hey, you know, that's really positive [pause] I can, I can feed on that. Good things are happening in my group [pause]. It, it, it builds confidence I guess. I don't know.
Several participants compared themselves to other group members and in some cases, this provided a therapeutic value28,37.
And you know, when you talk to other people, you're, you uh, you see how, what they, how they handle their problems. Yeah, compared to yourself. So it helps to have somebody that's in the same, hm, category as you.
The videoconferenced connection allowed group members to develop a rapport and derive therapeutic benefits, but did not satisfy the desire to meet one another in person. Many study participants articulated a desire to have a chance to meet the group participants from other sites face-to-face at least once.
Suggestions for improvement
Face-to-face connection: After a participant suggested that it would be helpful to have a face-to-face meeting with other members of the group, others were asked for their opinion about meeting in person. Although several raised logistical concerns, all but three of the 16 consulted participants felt that meeting the entire group in person, early in the program, would be beneficial. One even suggested that it would be useful to have another face-to-face session at the end of the program:
That way uh, when you have uh, when you're done with the teleconference you get to know everyone. Yeah. And then we can have a big celebration that everyone had accomplished their goals and you knew that we got to meet. And it kind of is like a party at the end.
Others made similar comments about wanting an opportunity to talk with one another informally outside of the session. They wanted a chance to socialize and get to know one another better.
Videoconference-specific facilitation strategies: The participants felt that the open microphone strategy (Table 1) facilitated their participation. They commented that background noise from other sites did not disrupt the conversation. The open microphone additionally permitted the facilitators to be aware of and limit side conversations at individual sites. Strategies to limit side conversations included occasional reminders and sometimes humour to cue the participants that everyone was able to hear all the conversations in all the rooms.
Local site coordinators and volunteers: To optimize the videoconference experience of the remote participants, facilitators in Thunder Bay collaborated with local site coordinators and volunteers. All participants agreed that it had been important to have local site coordinators in place. Some felt that the presence of the site coordinators at only two sessions was enough; whereas others wished for more ongoing availability. Aware of the limited healthcare resources, they suggested that a volunteer might attend regularly to set up the room and be present for the first 10 min of the discussion. As one said:
You need a physical being there for the first ten minutes at least. After that, you know, you're part of the group ... I think, to have a warm body there for the first ten minutes... a warm welcoming, communicative, interpersonal kind of person would be helpful.
Those who had a volunteer at their site appreciated the assistance with exercise and walking safety. Participants with no volunteers at their site were concerned about confidentiality, not knowing who the volunteer would be. In small towns, participants felt the volunteer may limit their willingness to discuss personal issues.
Local participants: Many of the participants would have liked to have had a larger number of people in their local group for more social support, informal conversation outside of the session topic, and ongoing local connection. This was a particular concern for the three who completed the program as sole program participants at their site, and each independently raised the issue. As one said:
If there would have been another person or two with me, at my meetings [pause] then, it would have been more of a shared experience I think. It's you know, a little bit more personal from that side.
Similarly, one of the caregivers, who participated alongside stroke survivors but no other caregivers, talked about the videoconference format limiting her ability to make more of a connection with other caregivers.
Discussion
This study explored in detail the perspectives of participants regarding their experiences with a videoconferenced group stroke self-management program. Important components of the program were group exercise, discussion of stroke-related topics, and peer-support. A number of useful findings emerged to consider in future planning of videoconferenced programs. In general, patterns found regarding the satisfaction and limitations to participation across videoconference were consistent with previous reports. This study adds new information; specifically, details from a client perspective regarding: the subtleties lost in communication; the desire for connection to one another as part of a group experience; and the experience of participating in a group exercise program across videoconference.
Participants appreciated the ability to participate in MOST-TR via videoconference, a program that would otherwise only be offered in urban centres with sufficiently large numbers of participants and providers. The participants reported satisfaction with the videoconferenced delivery of MOST-TR and agreed that telehealth was beneficial in that it allowed them to stay in their home community to access health services, gave them access to health information, and meant decreased travel time and costs for them. These are benefits to telehealth that have also been described in existing literature38. However, given the opportunity, all the participants would have preferred face-to-face participation in their own community.
The findings of this study indicate that the videoconferenced connection was superior to a telephone connection because it allowed participants to see others at different sites, fostered the feeling of being in the same room, and thus improved their ability to connect with the group.
The findings from this study suggest the possibility of the safe delivery of an exercise class to a group across multiple sites connected by videoconference. This affords new opportunities for isolated areas. The videoconference permitted members to benefit from the group exercise and be motivated by one another. Some participants, however, did identify difficulties participating in the exercises, and it was not always possible for the facilitator to be aware of or satisfactorily address difficulties across videoconference. Although it is possible this would be the same in-person; in those situations, a facilitator may have been able to identify this more easily and could have more informal opportunities outside of the group to promote a positive experience.
The literature reports conflicting findings with respect to group communication and cohesion using videoconference. Meier examined the ability to develop and maintain a sense of 'groupness' during a business meeting39,40. He reported difficulties discerning subtle facial expressions and misinterpreted body language and gaze via videoconference. These difficulties with communication subtleties such as direct eye contact, gaze, gesture, and emotions were also reported by MOST-TR participants. Meier noted that laughter and having fun did not seem to carry over into other locales easily, but this was not the case in MOST-TR40. While it is possible that some humour was lost across videoconference, MOST-TR participants described incidents of laughter and humour shared across all sites. These conflicting findings suggest that the group's purpose influences the style of communication, and consequently alter the transmission of laughter and humour.
Most participants found they were able to share their experiences and to benefit from the information and peer support the program offered; however, their participation in the discussion portion of the program was altered by the videoconference connection when compared with an in-person experience. Some, for example, found it difficult to join in to conversations at other sites for fear of 'cutting off' the conversation. One participant required a greater sense of group cohesion to feel comfortable sharing with other group members. Another participant reported feeling more at ease sharing information and participating across videoconference. This is not surprising because the videoconference connection allows a more removed experience whereby one may feel less threatened by others' judgment in view of the physical distance. These types of experiences with videoconferencing have also been reported in other education sessions for patients or caregivers8.
The majority of the MOST-TR participants thought that the videoconference connection made no difference to their level of participation and that they were able to participate at the same level as if they were there face-to-face. It is possible that the participants' need and desire for support from others in a similar situation was met with the videoconference format and thus eliminated a need for a more intimate in-person experience. However, participants also said that they would have enjoyed more time for discussion, and some said that they desired more time to socialize informally, share stories and get to know each other.
Participants recommended continuing the use of the open microphone and close-up camera angle strategies to support the flow of the discussion. To use these strategies, the facilitator needs to become technically able to focus and readjust the camera to different pre-set positions while continuing to deliver and facilitate the content of the program. It is critical to co-facilitate in these situations in order to accommodate these additional roles. The present technology limits the ability to control the far-site camera when more than two sites are connected, making the camera angle strategy only available to a local participant. Using the camera remote control was overwhelming for some participants. One possible solution is to have the local telehealth coordinator set pre-set camera angles and orient the local participants to the pre-set positions. These suggestions are useful for future group programming across videoconference.
This study also confirmed the visual restrictions of videoconference as reported in the literature18,19. When meeting the group face-to-face, some participants felt as if they had met before; others felt the videoconference representation was limited and this was disconcerting. Participants suggested one of the early sessions are hosted face-to-face for all group members allowing for both an in-person visual connection as well as an informal opportunity for the group to get to know one another. A preliminary face-to-face meeting confirms similar suggestions in tele-psychiatry20. The group's suggestion of one in-person session is important because it has been identified that an in-person assessment is recommended for visual accuracy, rapport building, and prudent for safety in the group exercise. It is possible that this assessment could be performed by local staff, providing an opportunity for increased 'buy-in' and support from the local institution, but this would not satisfy the in-person connection and visual representation for program participants.
Limitations
This study included only participants who had completed the program and had generally positive experiences. Those who did not complete the MOST-TR program, although invited, chose not to participate in this study. The power differential between the participants and the healthcare professional interviewer may further have affected how participants responded to the invitation to participate and their responses to questions during the interview. They may have been reluctant to fully explore the role of the facilitator as a factor in their engagement and participation. The investigator's role as facilitator and enthusiasm for the technology additionally may have had an unintended impact on the participants' comfort sharing their fears, challenges, and barriers to participation. The findings therefore reflect a positive bias of satisfaction with the videoconference connection, group connection, and successful participation in the program.
Although the findings may nevertheless be suggestive of issues for people participating in group-based videoconference programs in general, it is not possible to generalize the findings beyond the study participants.
This study adds to the literature by presenting participant perspectives on the benefits and challenges of participating in a post-stroke self-management and exercise program via videoconference.
Overall, participants in this study were satisfied with the MOST-TR videoconference group experience. They felt the program increased their knowledge about their condition and assisted with participation in ongoing exercise. They reported being able to connect with the group and to benefit from this connection. The videoconference technology altered participation in the discussion, both negatively and positively. The videoconference environment limited opportunities for group members to connect with one another in informal discussions outside of the sessions. The videoconference environment permitted a safe, motivating exercise environment but limited the facilitator's ability to accurately assess whether participants were struggling to perform specific exercises or were finding the exercises too easy.
This research shows that videoconference technology has the potential to meet the need for community-based programming and exercise for individuals living in remote areas. Both facilitators and participants need to recognize that there are differences between videoconference and face-to-face participation. Future programs may wish to incorporate and strengthen where possible the supportive factors identified in this study, and explore solutions to overcome identified barriers to group videoconference implementation. This may increase meaningful access to group interventions, including social support programs and exercise programs, for residents in rural and remote areas where both patient numbers and healthcare resources are limited.
Acknowledgements
This study is partial fulfillment of a Master's in Public Health and honours the participants who were willing to share their experiences. The authors acknowledge Kirsti Reinikka and Esmé French for helpful comments on a draft of the manuscript. Financial support was provided by the Ontario Stroke System and St Joseph's Care Group, Thunder Bay. The Heart and Stroke Foundation of Ontario and Baycrest in Toronto were instrumental in financing the Moving on after Stroke Telehealth RCT.
References
1. Corbin J, Strauss A. Unending work and care: managing chronic illness at home. San Francisco, CA: Jossey-Bass, 1988.
2. Lorig K, Sobel D, Stewart A, Brown BJ, Bandura A, Ritter P et al. Evidence suggesting that a chronic disease self-management program can improve health status while reducing hospitalization: a randomized trial. Medical Care 1999; 37(1): 5-14.
3. Taal E, Rasker JJ, Wiegman O. Patient education and self management in the rheumatic diseases: a self-efficacy approach. Arthritis Care and Research 1996; 9(3): 229-230.
4. Northwest. Population Health Profile Northwest Local Health Integration Network (v 2). (Online) 2009. Available: http://www.northwestlhin.on.ca/uploadedFiles/Home_Page/Report_and_Publications/North%20West%20LHIN%20Population%20Health%20Profile%202009%20v.2.pdf (Accessed 7 March 2011).
5. Romanow HR. Report on the Future of Healthcare in Canada. Saskatoon, SK: Commission on the Future of Health Care in Canada, 2002.
6. Tran B, Buckley K, Prandoni C. Selection and use of telehealth technology in support of homebound caregivers of stroke patients. Caring 2002; 21: 16-21.
7. Van Ast P. Supporting community carers via videoconferencing. Journal of Telemedicine and Telecare 2005; 11(Suppl 2): S96-97.
8. Van Ast P, Larson A. Supporting rural carers through telehealth. Rural and Remote Health 7: 623. (Online) 2007. Available: www.rrh.org.au (24 January 2012).
9. Chan WM, Woo J, Hui E, Lau WWY, Lai JCK, Lee D. A community model for care of elderly people with diabetes via telemedicine. Applied Nursing Research 2005; 18: 77-81.
10. Po YM. Telemedicine to improve patients' self-efficacy in managing diabetes. Journal of Telemedicine and Telecare 2000; 6: 263-267.
11. Lai J, Woo J, Hui E, Chan W. Telerehabilitation - a new model for community-based stroke rehabilitation. Journal of Telemedicine and Telecare 2004; 10(4): 199-205.
12. Wong YK, Hui E, Woo J. A community-based exercise programme for older persons with knee pain using telemedicine. Journal of Telemedicine and Telecare 2005; 11: 310-315.
13. Birden H, Page S. Teaching by videoconference: a commentary on best practice for rural education in health professions. Rural and Remote Health 5: 356. (Online) 2005. Available: www.rrh.org.au (24 January 2012).
14. Gagnon M, Duplantie J, Fortin J, Landry R. Implementing telehealth to support medical practice in rural/remote regions: what are the conditions for success? Implementation Science 2006; 1: 18.
15. Moehr J, Schaafsma J, Anglin C, Pantazi S, Grimm N, Anglin S. Success factors for telehealth - a case study. International Journal of Medical Informatics 2006; 75: 755-763.
16. Currell R, Urquhart C, Wainwright P, Lewis R. Telemedicine versus face to face patient care: effects on professional practice and health care outcomes. Cochrane Database of Systematic Reviews 2000; (2): CG002098.
17. Jennett P, Gagnon M, Brandstadt H. Preparing for success: readiness models for rural telehealth. Journal of Postgraduate Medicine 2005; 51(4): 279-285.
18. Allen M, Sargeant J, Mann K, Fleming M, Premi J. Videoconferencing for practice-based small-group continuing medical education: feasiblity, acceptability, effectiveness, and cost. Journal of Continuing Education in the Health Professions 2003; 23: 38-47.
19. Hettrick C, Bullick T, Nelson T, Munro S, Jamieson J. The Northwestern Ontario Rehabilitation Network: Final Report. Thunder Bay, ON: St Joseph's Care Group; 2006.
20. Mielonen M, Ohinmaa A, Moring J, Isohanni M. The use of videoconferencing for telepsychiatry in Finland. Journal of Telemedicine and Telecare 1998; 4: 25-31.
21. Faulkner K, McClelland L. Using Videoconferencing to Deliver a health education program to women health consumers in rural and remote Queensland: an early attempt and future plans. Australian Journal of Rural Health 2002; 10(1): 65-72.
22. Jennett P, Affleck Hall L, Hailey D, Ohinmaa A, Anderson C, Thomas R et al. The socio-economic impact of telehealth: a systematic review. Journal of Telemedicine and Telecare 2003; 9: 311-320.
23. Mair F, Whitten P. Systematic review of studies of patient satisfaction with telemedicine. BMJ 2000; 320: 1517-1520.
24. Huijbregts M, Myers A, Streiner D, Teasell R. Implementation, process, and preliminary outcome evaluation of two community programs for persons with stroke and their care partners. Topics in Stroke Rehabilitation 2008; 15(5): 503-520.
25. Jones F. Strategies to enhance chronic disease self-management: how can we apply this to stroke? Disability and Rehabilitation 2006; 28(13-14): 841-847.
26. Huijbregts M, McEwen S, Taylor D. Telehealth delivery of a stroke self-management program: a controlled feasibility trial. Physiotherapy Canada 2009; 61(3): 210-221.
27. Taylor D, Cameron J, Walsh L, McEwen S, Kagan A, Streiner D et al. Use of videoconference to deliver a self-management program to rural participants with stroke: a pilot study. Telemedicine Journal and e-Health 2009; 15(7): 1-9.
28. Yalom ID. The theory and practice of group psychotherapy, 4th edn. New York: Harper-Collins, 1995.
29. Fereday J, Muir-Cochrane E. Demonstrating rigor using thematic analysis: a hybrid approach of inductive and deductive coding and theme development. International Journal of Qualitative Methods 2006; 5(1): 1-11.
30. Goering PN, Streiner DL. Reconcilable differences: the marriage of qualitative and quantitative methods. Canadian Journal of Psychiatry 1996; 41: 491-497.
31. Hsieh H, Shannon S. Three approaches to qualitative content analysis. Qualitative Health Research 2005; 15(9): 1277-1288.
32. Ohman A. Qualitative methodology for rehabilitation research. Journal of Rehabilitation Medicine 2005; 37: 273-280.
33. Rossman G, Rallis S. Learning in the field. an introduction to qualitative research, 2nd edn. Thousand Oaks, CA: Sage, 2003.
34. Wright JG, McKeever P. Qualitative research: its role in clinical research. Annals of Royal College of Physicians and Surgeons of Canada 2000; 33: 275-280.
35. Charmaz K. Constructing grounded theory: a practical guide through qualitative analysis. Thousand Oaks, CA: Sage, 2006.
36. Elliot J. The researcher as narrator: reflexivity in qualitative and quantitative research. Using narrative in social research: qualitative and quantitative approaches. Thousand Oaks, CA: Sage, 2005; 152-159.
37. Posthuma BW. Small groups in counselling and therapy. Boston: Allyn and Bacon, 2002.
38. Jennett P, Yeo M, Scott R, Hebert M, Teo W. Delivery of rural and remote health care via a broadband internet protocol network - views of potential users. Journal of Telemedicine and Telecare 2005; 11: 419-424.
39. Heath C, Luff P. Media space and communicative asymmetries: preliminary observations of video-mediated interaction. Human-computer Interaction 1992; 7: 315-346.
40. Meier C. Doing "groupness" in a spatially distributed work group: the case of videoconferences at Technics. In: L Frey (Ed.). Group communication in context: studies of bona fide group, 2nd edition. London: Lawrence Erlbaum, 2003, 367-397.

