Enhanced teaching in community general practice has been suggested as an appealing strategy to meet the increasing demand for medical education1-3. Australia has recently undergone significant expansion of medical student, pre-vocational and vocational training programs in general practice, focusing interest on the financial cost of community-based medical education. A recent cost-benefit analysis of teaching in private general practice in South Australia reported a net financial cost for practices teaching medical students while costs of teaching pre-vocational and vocational trainees were offset by higher subsidies and income generated4. As the demand for such teaching practices was predicted to increase substantially over the next 5 years, the authors suggested a review of undergraduate teaching subsidies to improve recruitment and retention of general practices as an environment for medical student teaching.
Increased teaching subsidies may seem appropriate as medical student education is generally perceived as negatively impacting on clinical productivity and income. However, much of this perception has arisen from international studies conducted in primary care or ambulatory settings where cost has been measured in terms of time spent by faculty members (supervisors) teaching medical students, the decreased number or increased length of patient visits, or the amount of time students occupied rooms when seeing patients on their own5-11. The negative impact on physician productivity at one site was attributed to its location in a relatively rural area with a shortage of physicians, and to the higher quality program they offered senior students, with potential for future physician recruitment12.
In contrast, others have found no effect5 or even increased physician productivity13,14 when undergraduate medical students were present. However, it is difficult to quantify and accurately compare the costs, because studies have used inconsistent methodologies and involve students with differing levels of clinical experience5.
Most of the studies cited have only examined short-term student rotations to clinics in urban settings, limiting their generalisability to other contexts and models of clinical training. There is little reported evidence on the financial impact of longitudinal models of clinical education and delivery of community-based medical education in regional and rural areas, the context of the current study. In his call for better evidence on the impact of medical students on rural preceptors, Bowman highlighted positive financial outcomes from the Rural Physician Associate Program (RPAP) in rural Minnesota USA, where having a third-year medical student in a rural practice for 12 months could add an additional US$40,000 to $70,000 in patient billings15. Bowman emphasised not only this financial benefit but also that the ultimate savings may be in practices where the student returns after graduation, and the RPAP is a good example of this16.
In Australia, Worley and Kitto studied a subset of students who chose to spend the whole third year of their four-year course, based in rural general practice as part of the Parallel Rural Community Curriculum (PRCC), and challenged the traditional view that medical students may incur a financial burden on general practices17. Their retrospective study of 932 PRCC student consultations revealed that where students had already been actively involved in all aspects of the practice for at least 5 months, a positive effect on general practitioner productivity occurred without any loss in patient satisfaction17. They proposed a hypothetical model where initially practice income decreased while the student became familiar with the practice, and the supervisor checked that the student has the necessary skills; a 'turning point' occurred somewhere between 4 weeks and 5 months when the student becomes a financial benefit rather than burden; and the 'break even' point was the length of time needed in a practice in order for the financial benefit to counter the earlier loss. This model suggested that it is more economically sustainable if curricula allow extended attachments, of 5-6 months or longer, rather than traditional, shorter rotations.
Recent studies have further elucidated the impact of PRCC clerkships on GPs who supervise the students. A prospective cohort study revealed that consultation length did not increase when rural GPs supervised medical students using a parallel consulting model18. With this model, the senior student initially saw the patient by him/herself and then presented his/her findings, with an assessment plan, to the supervising clinician. A follow-up study revealed that the entire consultation took no longer when a student was 'parallel-consulting' as the supervising GP significantly re-organised clinical activity to meet the needs of both the student and the patient19.
Informed by this evidence, and in keeping with its mission to produce doctors for regional and rural Australia, the University of Wollongong, Graduate School of Medicine (GSM) recently implemented a 12 month integrated community-based clerkship for all, rather than a subset of, senior students in the third year of their 4 year graduate-entry medical course. The PRCC model20 was adopted as a pedagogical approach and modified as needed for each of 10 learning hubs in regional and rural New South Wales (NSW). The following research question was asked to explore regional and rural supervisors' perceptions of the financial impact of the initiative after the first year of implementation, and to test Worley and Kitto's hypothetical model17:
Are graduate-entry medical students on long-term placements in regional and rural general practice a financial help or a hindrance to their supervisors?
The first cohort of GSM students was based in regional or rural general practices in NSW from mid-July 2009 to early June 2010. Students undertook a minimum of two parallel consulting sessions per week in the practice, as well as another day engaged in consulting or working with other practice health professionals. The rest of the week consisted of academic and hospital-based learning.
Ethics approval was obtained from the University of Wollongong Human Research Ethics Committee for the two-part study. In Part 1, qualitative data were collected from supervisors immediately following the year-long placement of the first student cohort. For Part 2, financial data were collected from consenting practices for the two-year period from 1 July 2008 to 30 June 2010.
Part 1
Thirty-four medical practices which provide ambulatory primary care services in their community were invited to participate in semi-structured interviews, conducted by independent researchers. Each interview was recorded and transcribed and any identifying information removed. For the purposes of this article, responses to the following interview question about perceived financial impact after the student placement were analysed independently by two researchers (JNH & KMW) using inductive qualitative content analysis20:
Do you believe the medical student has had any impact on the activity or finances of the practice during the course of their placement?
After discussion, the researchers reached consensus on the categories identified in the transcribed data, and clustering of these into four central themes.
Part 2
Independent research assistants conducted visits to 7 practices that were able, and consented, to provide the following data electronically for Part 2 of the study: patient throughput/service utilisation and income/billings. Data were gathered retrospectively with one long visit to each of these practices, with follow-up emails and telephone calls to clarify issues as needed.
The multiple 'Patient Management Systems' used by practices made data collection challenging. While both financial and patient activity data were sought in all practices, not all these sources were accessible. Measures of patient throughput were mostly obtained by the number of patients seen each month but in one case, the number of Medicare Benefit Scheduled (MBS) items billed was used as a proxy. Despite differences in data access, comparable measures of practice activity (patient throughput and gross monthly income) were obtained.
To determine the effective number of days a practice was open each month, public holidays and Sundays were assigned a zero value, because no or limited patients were seen on these days. Saturdays were assigned a weight of 0.5 (half day) and the remaining days of the week a weight of 1. The weights were aggregated for each month. The average daily income and/or activity for each of the 24 months of the research period was then calculated using the effective days as determined above.
The fact that some practices charged patients a co-payment in addition to the MBS fee and others did not was not a significant influence on the outcome because individual practices were consistent in their pattern of charging over the 2 year sampling period. Likewise, any seasonal effects (eg the winter cold/influenza season) were addressed by calculating the differences in the averages when the students were based in the practice to those in the corresponding month of the previous year. This difference was then expressed as a percentage of the earlier year's activity.
Income included all those declared by the practice, including Practice-Incentive Payments (PIP) from the government. It was not possible to quantify the PIP-teaching component. All practices are eligible for the same PIP-teaching subsidy for GP supervision of student consultation with patients. However this subsidy was designed for more traditional short-term general practice teaching placements. The time-cost of practice staff and supervisors in orientating, assessing, providing feedback and mentoring a long-term student has not been captured in this study.
Part 1
Of the 28 GP supervisors from 26 practices who consented to take part (76% of invited practices), 4 (14%) had been in practice less than 10 years, 11 (39%) for 10-20 years, and 13 (47%) for greater than 20 years.
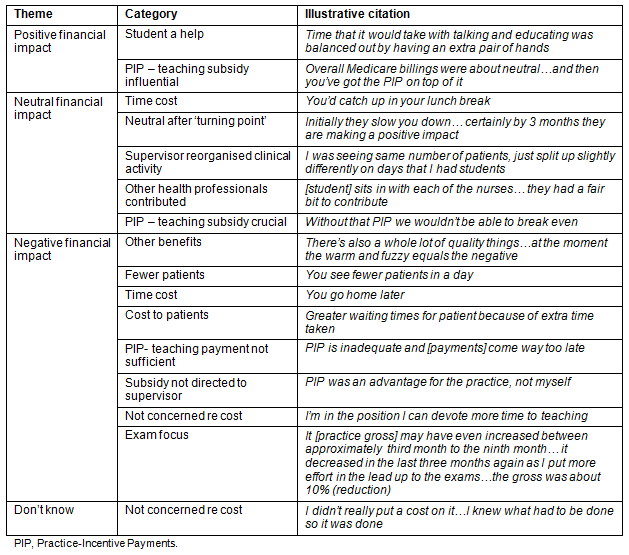
The categories identified from the transcribed data after the student placement were clustered into the following four themes: (i) 'zero impact' (cost neutral); (ii) 'negative impact'; (iii) 'positive impact'; and (iv) 'don't know' (Table 1). In each theme, supervisors commented on the PIP for teaching, expressing the importance of this teaching subsidy to achieve a neutral or positive teaching impact, or dissatisfaction with the amount, target or tardiness of the payment.
Table 1: Themes and categories, with illustrative citations, of preceptor perceptions post-placement
For each of the four themes, supervisors' perceptions of the financial impact following the placement ('reality') compared with their perceptions ('predictions') prior to the placement are illustrated in Figure 1. For the latter, data were collected using the same qualitative methodology in another study21 prior to the longitudinal student placement. Prior to the long-term placement, 22% of supervisors predicted a positive, 30% a negative, and 30% a neutral financial impact. Post-placement, these changed to 12%, 19% and 54%, respectively. The post-placement perceptions of cost were given without knowledge of the financial data reported (Fig2).
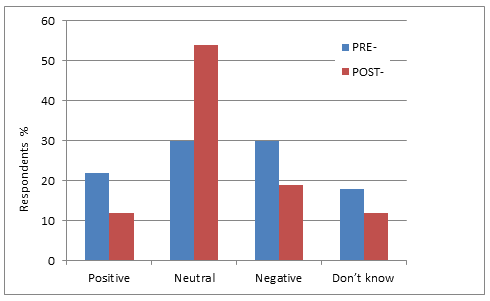
Figure 1: Supervisor perceptions of cost pre-placement (prediction) and post-placement (reality).
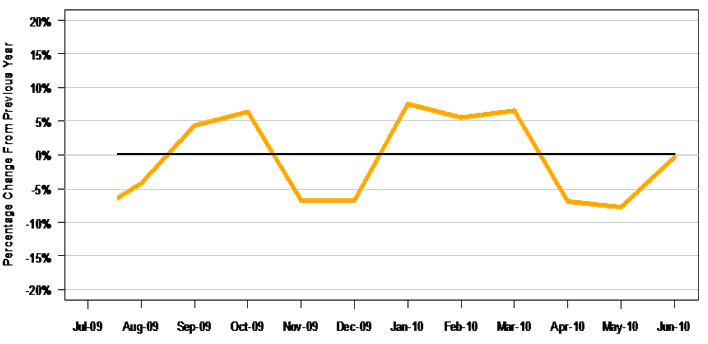
Figure 2: Pooled practice data: per cent change in practice income 2009-2010 compared with 2008-2009.
Part 2
The percentage change on previous year in average daily practice income for the 7 practices that provided financial data is shown (Fig2). These pooled practice data must be interpreted in the context of student short breaks in September and April; the summer break December to late January; the tendency for medical students to concentrate on academic studies as final exams approached (April/May); and, in 2009, the impact of the H1N1 influenza epidemic, with NSW hospital admissions peaking in mid-July just as the long-term placements began22. Considering these, the data reveal a general trend in keeping with Worley and Kitto's initial hypothesis. The present study students appeared to be cost-neutral after about 3 months (October 2009), with a 'turning point' at approximately 1-2 months after the student was based in the practice. Several supervisors supported the notion that the 'break-even' point was approximately 3 months.
While the quantitative and qualitative data (preceptor perceptions and the area under the curve [53%] and are above the curve [47%] in Fig2) from several practices suggested that the long-term student was cost-neutral or even beneficial, it must be remembered that acceptance of a long-term student requires considerably more investment in time and resources than merely consulting room supervision.
Discussion
This study suggests that students on long-term regional/rural clerkships are cost-neutral or even have a small positive financial impact on the practice, depending on the student, supervisor and/or host practice. As one study participant reported, this can be achieved by reorganisation of clinical activity by the supervising GP: 'I was seeing same number of patients, just split up slightly differently on days that I had students'.
This practice was also reported by Walters et al19. Several supervisors believed that after approximately 3 months the student became an 'extra pair of hands' contributing to a range of patient care activities, while learning with a range of practice health professionals. The following GP comment supports the finding presented in the financial graph: 'Initially they slow you down... certainly by 3 months they are making a positive impact'.
The present study's 'turning point' of 1-2 months was in keeping with the earlier prediction of a 'turning point' period of 4 weeks to 5 months17. The 12% of supervisors who reported a negative financial impact attributed this to the fewer number of patients seen, the inadequacy of the government teaching subsidy or the focus in the latter months on assessment preparation. One supervisor explained the financial loss noted in the closing months of the longitudinal placement by desire to assist the student to prepare for final exams: 'It [practice gross] decreased in the last 3 months again as I put more effort in the lead up to the exams'.
It also demonstrates the effort supervisors make beyond just supervising patient consultations. Several were unconcerned with financial loss feeling that other benefits compensated for this, or they were able or willing to contribute more time to teaching. Nevertheless preceptors making comments like the following citation tended to be clinicians in the latter part of their career: 'I'm in the position I can devote more time to teaching'.
For sustainability of the model and recruitment of a new cohort of potential teachers, evidence of possible positive or neutral benefits assumes greater importance. The qualitative data support the trend shown (Fig2), with 54% of supervisors believing that the longitudinal placement had neutral financial impact on the practice, despite predicting beforehand that the financial impact would be either positive or negative. This was in contrast to data obtained from a 2005 survey of Australian rural GP supervisors where approximately 50% believed that student attachments had a negative effect on their income, and 40% reported increased practice costs to their business23, although little of this evidence related to prolonged student attachments. Likewise, the recent study claiming that medical student teaching was less financially attractive to GP supervisors than pre-vocational and vocational supervision didn't examine the impact of longitudinal undergraduate education4.
Recent evidence suggests that positive and longitudinal rural undergraduate education experience offers potential for rural recruitment in Australia24. Many rural practices in NSW report spending thousands of dollars on advertisements and agencies to recruit rural doctors with little or no success (B Thompson, pers. comm; 2011). One study participant reported that the most cost-effective recruitment strategy has been via participation in the general practice post-graduate rural training pathway. The combination of minimal financial impact indicated in this paper and potential for future workforce recruitment may encourage more rural GPs to engage in longitudinal undergraduate education.
Conducting the study in the 'real world' of practice adds validity to the findings but introduces a range of difficult-to-control variables which must be taken into account when interpreting the data. The study is limited by only a small number of supervisors consenting to a review of their financial position over the 2 years of study. Funding for private general practice in Australia is complex and in some instances, while an individual supervisor agreed, not all their practice partners consented. Some supervisors examined their own inputs and outputs during the time of the study and reported on their own analysis of financial cost. A study of greater power is required to support these findings and to accurately determine the optimum length of placement that would encourage supervisors to engage in undergraduate teaching. As the present authors studied the longitudinal model at inception, it would also be valuable to re-examine financial impact after supervisors had more experience and systems in place to manage long-term students.
Long-term integrated community-based placements offer students holistic and authentic personal and professional development25. However, the required capacity for community-based undergraduate medical education cannot be realised until appropriate resources are provided to support the endeavour, especially when pre-vocational and vocational training is reported to be less of a financial burden for supervisors4. While the government PIP teaching subsidy attempts to compensate GPs in private practice, many supervisors stated it was too little, and reported delayed reimbursement. Teaching subsidies are critical in recruiting and sustaining the engagement of community-based practitioners for undergraduate teaching, a position supported by our GP supervisors. Appropriate remuneration for new models such as longitudinal community-based clinical education should also include the time that a supervisor spends managing the student experience and providing guidance and mentorship during a prolonged professional relationship, as well as the actual time spent in supervision of consultations.
Senior students learning in long-term clerkships are legitimate members of regional/rural communities of practice. These students can be cost-neutral or have a small positive financial impact on the practice within a few months. Further financial impact research should include consideration of various models of supervisor teaching subsidies. The ultimate financial benefit of a model may lie in the recruitment and retention of much-needed regional and rural practitioners.
Acknowledgements
The authors thank The Centre for Health Service Development at the University of Wollongong, for qualitative and quantitative data collection and compilation, advice on financial data collection and assistance with ethics approval. The Department of Health and Ageing, Commonwealth Government of Australia provided funding support for the project.
References
1. Pearce R, Laurence CO, Black LE, Stocks N. The challenges of teaching in a general practice setting. Medical Journal of Australia 2007; 187(2): 129-132.
2. Thistlethwaite JT, Kidd MR, Hudson JN. General practice: a leading provider of medical student education in the 21st century? Medical Journal of Australia 2007; 187(2): 124-128.
3. Van Der Weyden MB. Expanding primary care-based medical education: a renaissance of general practice? Medical Journal of Australia 2007; 187(2): 66-67.
4. Laurence CO, Black LE, Karnon J, Briggs NE. To teach or not to teach? A cost-benefit analysis of teaching in private general practice. Medical Journal of Australia 2010; 193(10): 608-613.
5. Kirz H, Larsen C. Costs and Benefits of Medical Student Training to a Health Maintenance Organization. Journal of American Medical Association 1986; 256(6): 734-739.
6. Vinson DC, Paden C. The Effect of Teaching Medical Students on Private Practitioners' Workloads. Academic Medicine 1994; 69(3): 237-238.
7. Grayson MS, Klein M, Lugo J, Visintainer P. Benefits and costs to community-based physicians teaching primary care to medical students. Journal of General Internal Medicine 1998; 13(7): 485-488.
8. Denton GD, Durning SJ, Hemmer PA, Pangaro LN. A time and motion study of the effect of ambulatory medical students on the duration of general internal medicine clinics. Teaching and Learning in Medicine 2005; 17(3): 285-289.
9. Adams M, Eisenberg JM. What is the cost of ambulatory education? Journal of General Internal Medicine 1997; 12(Suppl2): S104-110.
10. Usatine RP, Nguyen K, Randall J, Irby DM. Four exemplary preceptors' strategies for efficient teaching in managed care settings. Academic Medicine 1997; 72(9): 766-769.
11. Gress TW, Flynn JA, Rubin HR, Simonson L, Sisson S, Thompson T et al. Effect of student involvement on patient perceptions of ambulatory care visits: a randomized controlled trial. Journal of General Internal Medicine 2002; 17(6): 420-427.
12. Lawson RA. The cost of training third-year primary care medical students in an ambulatory setting. Research in Healthcare Financial Management 2002; 7: 21-32.
13. Abramovitch A, Newman W, Padaliya B, Gill D, Charles PD. The cost of medical education in an ambulatory neurology clinic. Journal of National Medical Association 2005; 97(5): 1288-1290.
14. Lindenmuth N, Stone A, Donaldson M. The Effect of Third-Year Clinical Clerks on Physician Productivity in a Primary Care Practice. Journal of Medical Education 1978; 53(4): 357-359.
15. Bowman R. Impact of medical students on rural preceptors - it's time for better evidence. Rural Remote Health 1(1): 191. (Online) 2001. Available: www.rrh.org.au (Accessed 25 April 2011).
16. Halaas GW, Zink T, Finstad D, Bolin K, Center B. Recruitment and retention of rural physicians: Outcomes from the Rural Physician Associate Program of Minnesota. Journal of Rural Health 2008; 24(4): 345-352.
17. Worley P, Kitto P. A hypothetical model of the financial impact of student attachments on rural general practices. Rural Remote Health 1(1): 83. (Online) 2001. Available: www.rrh.org.au (Accessed 25 April 2011).
18. Walters L, Worley P, Prideaux D, Lange K. Do consultations in rural general practice take more time when practitioners are precepting medical students? Medical Education 2008; 42(1): 69-73.
19. Walters L, Prideaux D, Worley P, Greenhill J, Rolfe H. What do general practitioners do differently when consulting with a medical student? Medical Education 2009; 43(3): 268-273.
20. Graneheim UH, Lundman B: Qualitative content analysis in nursing research: concepts, procedures and measures to achieve trustworthiness. Nurse Education Today 2004; 24(2): 105-112.
21. Hudson JN, Weston KM, Farmer EA. Why do rural supervisors engage in new longitudinal community clerkships during workforce shortage? BMC Family Practice 2011; 12(1): 103.
22. NSW Government, Health. Influenza Monthly Epidemiology Report, NSW. (Online) 2009. Available: http://www.health.nsw.gov.au/PublicHealth/Infectious/influenza/flu_reports_2009.asp (Accessed 16 July 2011).
23. Walters LS, Worley PS, Prideaux D, Rolfe H, Keaney C. The impact of medical students on rural general practitioner preceptors. Rural Remote Health 5(4): 403. (Online) 2005. Available: www.rrh.org.au (Accessed 25 April 2011).
24. Walker JH, DeWitt DE, Pallant JF, Cunningham CE. Rural origin plus a rural clinical school placement is a significant predictor of medical students' intentions to practice rurally: a multi-university study. Rural Remote Health 12: 1908. (Online) 2012. Available: www.rrh.org.au (Accessed 19 January 2012).
25. Couper I, Worley PS, Strasser R. Rural longitudinal integrated clerkships: lessons from two different programs on different continents. Rural Remote Health 11: 1665. (Online) 2011. Available: www.rrh.org.au (Accessed 15 July 2011).


