Between 2000 and 2010, the Hispanic population almost doubled in Georgia, USA, and now accounts for 8.8% of the population1. Unlike Hispanic populations in southwestern USA who have lived there for multiple generations, in Georgia, the Hispanic population consists of a higher percentage of more recent immigrants, primarily from Mexico.
The current estimated rate for completion of at least one dose of the 3 dose HPV vaccine series in Georgia is 38.6%, compared with 44.3% for the entire USA2. The US federally funded Vaccines for Children (VFC) program provides free vaccines to low-income children. The VFC provider status is associated with consistent humanpapilloma virus (HPV) vaccine recommendation for early adolescents3. However, nationally, there are disparities in vaccine awareness among Whites and ethnic and racial minority groups, with Whites reporting greater awareness compared with other groups4,5.
Moreover, there are health disparities with cervical cancer incidence and mortality rates for rural populations and Hispanics in the USA6. Latinas have twice the rate of developing cervical cancer than Whites7. In addition, Hispanics have lower rates of receiving regular Pap tests and lower health insurance coverage rates than Whites8. Given that either insurance coverage to cover the cost of vaccination or eligibility for the VFC program is one of the strongest predictors for HPV vaccination, it follows that immigrant Hispanics, who have low insurance coverage rates, may be less likely to take advantage of vaccination opportunities and will continue to experience cancer health disparities9.
The objective of this pilot study was to understand issues regarding vaccine access and compliance for rural, low-income, Hispanic adolescents of immigrant parents from the perspective of VFC providers and the parents themselves. This pilot study used qualitative methods to explore HPV vaccine access barriers for Hispanic adolescents by interviewing VFC providers and Hispanic immigrant parents in rural southern Georgia, USA.
Study sample
Individual structured interviews were conducted with VFC providers. The providers were practicing in a rural Georgia state health district (Fig1) and identified through a VFC provider list. Also conducted were two focus groups with Hispanic immigrant parents - mothers and fathers separately - of girls aged 9-18 years, aided by a local Hispanic-serving non-profit organization.
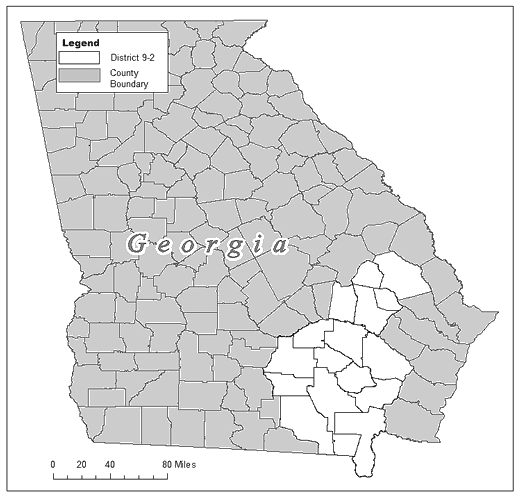
Figure 1: Rural Georgia state health district.
Study instruments and recruitment
For both the interview questions and the focus group guide, the researchers used instruments developed in a previous study which demonstrated credibility and face validity10. The 8 question structured interview instrument contained open-ended questions about common health topics discussed with patients, challenges with vaccine administration, Hispanic beliefs and attitudes toward the HPV vaccine, and the role of outreach and health education to improve vaccination rates. The 14 question focus group guide contained questions about knowledge of cervical cancer and the HPV vaccine, health-seeking behavior regarding vaccinations, barriers and benefits, and access and sources of health information. The focus group guide was translated into Spanish, and the groups were facilitated by a native Spanish speaker.
Beginning with a comprehensive list of 29 VFC providers, introduction letters were sent, followed by phone calls to recruit and schedule individual interviews with the providers either in person or via telephone. Recruitment efforts were ceased after three failed recruitment attempts. To recruit parents to the focus groups, only recruitment with the assistance of the Hispanic-serving non-profit was successful, which directly contacted participants and invited them to attend the focus group.
In response to an issue raised in the ethical review process, the importance of maintaining confidentiality after leaving the session was explained to focus group participants. All participants completed informed consent documents and received a US$10 stipend.
Data analysis
All interviews were digitally recorded and transcribed. Content analysis was used to code transcripts using a codebook based on social marketing conceptual categories to understand behaviors related to the HPV vaccine (barriers, benefits, product, price, place, and promotion), and containing 28 sub-codes. Pairs of coders coded transcripts independently using MAXQDA qualitative data analysis software (www.maxqda.com) and then compared with coded transcripts to improve reliability and consistency. The coders met to resolve inconsistencies, and then recoded transcripts either with the same refined code or a new code to improve reliability. For example, under the parent code of barriers, one of the coders identified language barriers for Hispanic patients as a potential new code. However, after reaching consensus, it was agreed that the quotes could be covered under the code for 'low English proficiency'.
Ethics approval
The study was approved by the Georgia Southern University institutional review board (approval no. H11035) prior to data collection.
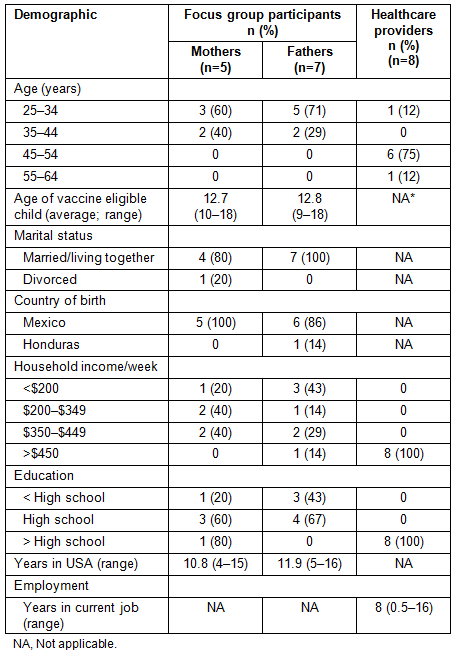
Participant characteristics of the two focus groups (mothers and fathers separately) and VFC providers are listed (Table 1). The sample of eight VFC providers included nurse practitioners, nurse managers, registered nurses, physician assistants, and one physician. The sample represented seven ZIP codes in the state health district. Interviews with VFC providers identified numerous barriers to delivering the HPV vaccine to Hispanic adolescents including: (i) low English proficiency of the parents; (ii) Medicaid reimbursement shortfalls; (iii) difficulty in completing the 3-dose HPV vaccine series with a mobile population; (iv) lack of transportation access; and (v) lack of knowledge and misperceptions about the HPV vaccine. One provider stated:
There's a communication gap with those patients. Like, if I get 10 Hispanic patients, almost 6 won't understand English; 4 will understand a little bit at least, I can tell them something about diet, or vaccines.
Overall, the VFC providers expressed that Hispanic patients were very positive toward vaccines, but there were cost issues for the provider, related to stocking the vaccine and reaching the population, since providers in many cases may have limited contact with adolescent patients, who do not routinely seek healthcare services.
Table 1: Demographics of focus group participants and healthcare providers
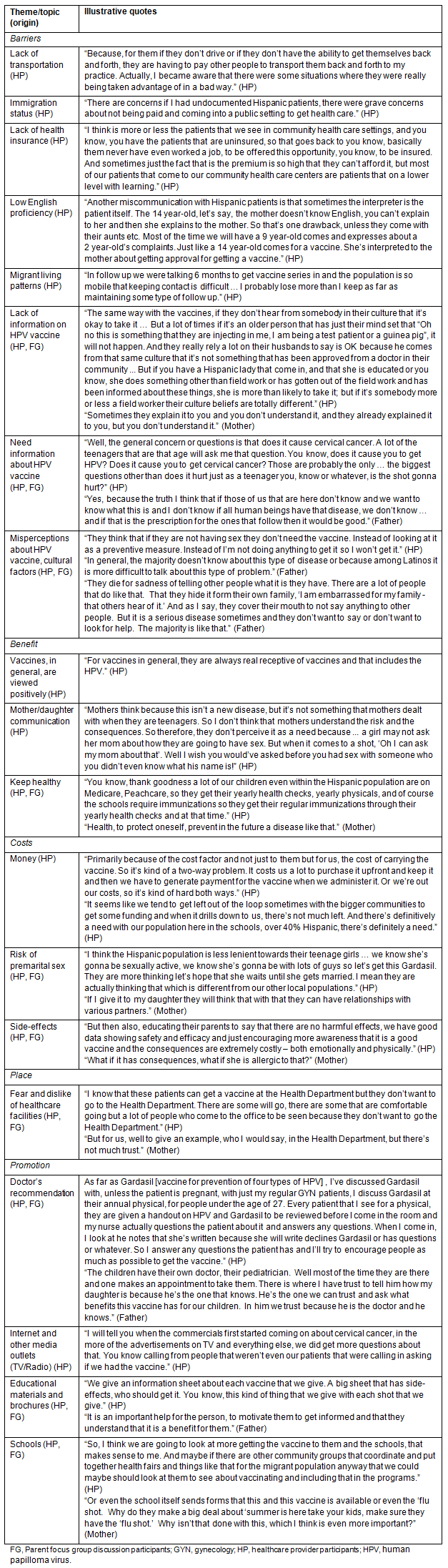
The two focus group discussions with mothers and fathers revealed that most Hispanic parents were not aware of the HPV vaccine, nor the VFC program. One mother said that the schools should promote the vaccine to increase access and awareness. Another mother believed that a patient needed to see a gynecologist before receiving the vaccine. Fathers were mostly unaware of the HPV vaccine, compared with mothers. However, both mothers and fathers expressed positive views toward childhood vaccinations. There were exceptions, however. For example, one mother believed that if her daughter received the vaccine, she might pursue sexual relations with multiple partners as a consequence. The parents identified numerous barriers to HPV vaccination for their daughters including: (i) undocumented status preventing access; (ii) fear of not knowing about cancer; (iii) cultural issues, especially related to diseases caused by sexual behaviors; (iv) low English proficiency; (v) lack of information; and (vi) distrust of particular healthcare facilities. Illustrative quotes from the VFC provider interviews and parent focus groups are organized and presented by thematic code (Table 2).
Table 2: Thematic codes and quotes from healthcare provider interviews and parent focus groups
Discussion
Hispanic subgroups vary according to their HPV awareness and knowledge as a function of acculturation and socioeconomic status11,12. Recent studies have found that certain Hispanic subgroups have more favorable beliefs and attitudes toward the HPV vaccine and higher completion rates13,14. Increasing HPV vaccination rates for Hispanic adolescents is an important public health priority because Hispanic women have been found to have high incidence and mortality rates from cervical cancer compared with other groups for multiple reasons, including lack of a regular healthcare provider and convenient access to timely screening and follow up15.
Further research is needed to design interventions which increase Hispanic parental awareness and knowledge of HPV vaccine availability, and to decrease the barriers to adolescent vaccinations. A large proportion of the Hispanic population living in this area of rural Georgia works in low wage occupations, such as farm labor. Such occupations do not include health insurance benefits, so healthcare providers might wrongly assume that many of their Hispanic patients do not work because they do not have insurance. Language barriers and lack of insurance coverage were listed by both VFC providers and parents as preventing access to health information and health services. Therefore, the provision of professional medical translation services is one priority area to address to ensure that parents receive information in Spanish from a healthcare provider about programs such as the VFC to provide the HPV vaccine at no cost for their vaccine-eligible children. Moreover, health behavior change programs geared toward Hispanic immigrant populations must address the issue of trust in healthcare institutions, as well as cultural barriers to engaging in preventive healthcare practices, including sexually transmitted infections. In addition, policy changes at the state level, such as HPV vaccine mandates for school entry, are both acceptable to Hispanic parents and the most likely upstream approach to increase overall HPV vaccination rates16.
Limitations
As a small pilot study, there were several limitations. The sample size was small because of recruitment challenges for both the parent focus groups and the VFC provider interviews, possibly related to the new Georgia anti-immigration law, as well as media-driven controversy surrounding the HPV vaccine. While alternative recruitment strategies were attempted to recruit two additional parent focus groups (eg flyers at community meetings and Mexican grocery stores), these efforts were ultimately unsuccessful. For the VFC provider interviews, resistance to participation was encountered from some health department affiliated providers who stated their employment situation prevented them from participation in research activities. It was not possible to determine the reason for this excuse since some other health department affiliated providers agreed to participate in the interviews. Nevertheless, participants provided data indicating that numerous barriers exist and ultimately impact HPV vaccine uptake among Hispanic adolescents.
This study highlights the similarities in and differences between HPV vaccination barriers as perceived by VFC providers and Hispanic parents related to vaccinating Hispanic adolescents. The qualitative findings further explain quantitative results from a survey study of Georgia VFC providers which found that insufficent insurance coverage was the major barrier for not vaccinating adolescents, and that major predictors for not recommending the vaccine to 11-12 year old girls included parental barriers, such as reluctance to discuss sexuality and lack of education17. Barriers to HPV vaccination remain a major challenge for Hispanic immigrant parents who have limited contact with the healthcare system. The results of this study will be used to inform future quantitative research with Hispanic parents to develop a social marketing plan to increase HPV vaccination rates for adolescent Hispanics in rural southern Georgia.
Acknowledgments
Dr Luque received a Georgia Southern University internal grant to support this project. The authors thank Voces Unidas for assisting with the focus group recruitment and hosting the groups. Also thanked are Angela Rodriguez and Daniela Hazelwood for their assistance with data collection, transcribing, translating and coding.
References
1. US Census Bureau. United States Census 2010. (Online) 2010. Available: http://www.census.gov (Accessed 2 October 2011).
2. Centers for Disease Control and Prevention. FDA licensure of quadrivalent human papillomavirus vaccine (HPV4, Gardasil) for use in males and guidance from the Advisory Committee on Immunization Practices (ACIP). Morbidity and Mortality Weekly Report (MMWR) 2010; 59: 630-632.
3. Vadaparampil ST, Kahn JA, Salmon D, Lee JH, Quinn GP, Roetzheim R et al. Missed clinical opportunities: provider recommendations for HPV vaccination for 11-12 year old girls are limited. Vaccine 2011; 29(47): 8634-8641.
4. Hughes J, Cates JR, Liddon N, Smith JS, Gottlieb SL, Brewer NT. Disparities in how parents are learning about the Human Papillomavirus Vaccine. Cancer Epidemiology, Biomarkers, and Prevention 2009; 18(12): 363-372.
5. Cui Y, Baldwin SB, Wiley DJ, Fielding JE. Human Papillomavirus Vaccine among adult women: disparities in awareness and acceptance. American Journal of Preventive Medicine 2010; 39(6): 559-563.
6. Yabroff KR, Lawrence WF, King JC, Mangan P, Washington KS, Yi B et al. Geographic disparities in cervical cancer mortality: what are the roles of risk factor prevalence, screening, and use of recommended treatment? Journal of Rural Health 2005; 21(2): 149-157.
7. US Cancer Statistics Working Group. United States Cancer Statistics: 1999-2007 Incidence and Mortality Web-Based Report. Atlanta, GA: Department of Health and Human Services, Centers for Disease Control and Prevention, and National Cancer Institute, 2010.
8. Flores K, Bencomo C. Preventing cervical cancer in the Latina population. Journal of Women's Health (Larchment) 2009; 18(12): 1935-1943.
9. Drewry J, Garces-Palacio IC, Scarinci I. Awareness and knowledge about Human Papillomavirus among Latina immigrants. Ethnicity and Disease 2010; 20: 327-333.
10. Luque JS, Castañeda H, Martinez Tyson D, Vargas N, Meade CD. Formative research on HPV vaccine acceptability among Latina farmworkers. Health Promotion Practice 2011; http://www.ncbi.nlm.nih.gov/pubmed/21881079 (in press).
11. Kobetz E, Kornfeld J, Vanderpool RC, Finney Rutten LJ, Parekh N, O'Bryan G et al. Knowledge of HPV among United States Hispanic women: opportunities and challenges for cancer prevention. Journal of Health Communication 2010; 15(Suppl3): 22-29.
12. Luque JS, Castañeda H, Tyson DM, Vargas N, Proctor S, Meade CD. HPV awareness among Latina immigrants and Anglo American women in the southern U.S.: cultural models of cervical cancer risk factors and beliefs. NAPA Bulletin 2010; 34(1): 84-104.
13. Lechuga J, Swain GR, Weinhardt LS. The cross-cultural variation of predictors of human papillomavirus vaccination intentions. Journal of Women's Health 2011; 20: 225-230.
14. Yeganeh N, Curtis D, Kuo A. Factors influencing HPV vaccination status in a Latino population; and parental attitudes towards vaccine mandates. Vaccine 2010; 28(25): 4186-4191.
15. Scarinci IC, Garcia FA, Kobetz E, Partridge EE, Brandt HM, Bell L et al. Cervical cancer prevention: new tools and old barriers. Cancer 2010; 116(11): 2531-2542.
16. Robitz R, Gottlieb SL, De Rosa CJ, Guerry SL, Liddon N, Zaidi A et al. Parent attitudes about school requirements for human papillomavirus vaccine in high-risk communities of Los Angeles, California. Cancer Epidemiology, Biomarkers, and Prevention 2011; 20(7): 1421-1429.
17. Dixon ET. An assessment of HPV vaccination among Georgia physicians: knowledge, barriers, supports, practices, and adherence to ACIP guidelines and recommendations (Thesis). Statesboro, GA: Georgia Southern University, 2011.
