Employment has long been understood to be a key determinant of health. In the last decade, its importance to mental health and individual recovery has received increasing attention in the Canadian literature, in research, and policy1-5. For people with mental illness, employment is acknowledged to be important to their economic and social wellbeing, as well as fundamental to their mental and physical health6,7. In Canada, and Internationally, there has been a growing recognition of the influence of place on mental health and mental illness, especially policies related to public health, housing, income, education and employment8-11.
Employment has been linked to having better social networks, to enhanced quality of life and to overall wellbeing7. Yet, despite these health benefits, persons with disabilities in general, and those with serious mental illness (SMI), in particular, continue to experience unacceptably high levels of unemployment and limited participation in the workforce6,12,13. Serious mental illness is defined by diagnosis (schizophrenia, mood disorders, organic brain syndrome, paranoid and other psychoses, severe personality disorder, concurrent disorder and dual diagnosis), disability (significant difficulties that interfere with or limit an individual's capacity to function in one or more major life activities) and duration (episodic as opposed to continuous but anticipated to be longer than one year and recurrent)14. Unemployment rates for people with mental illness have typically been cited as between 75% and 89%12; however, the World Health Organization has suggested that global unemployment rates may be as high as 90% for persons with SMI15.
In general, people with SMI remain disproportionately underrepresented in the workforce, and simultaneously, over-represented in work characterized by low wage earnings, few hours (part-time and temporary or limited tenure), and limited security16. Their labour force participation rate, the percentage of those who are either working full-time or looking for work, has consistently hovered around 25% since the mid-1980s in the USA17. In the province of Ontario, Canada, employment rates for people with disabilities in general, and SMI in particular, remain low, suggesting that employment is not an integrated component of mental health and recovery programs1,18,19.
In Canada, there has been increasing support for the inclusion of employment in key national and provincial policies. In In Unison20, for example, meaningful employment for persons with physical or mental health disabilities is described as an important building block of full citizenship and participation16. In addition, a salient national report entitled, Out of the Shadows, recommends the establishment of a Canada-wide supported employment (SE) program to assist Canadians living with a mental illness in obtaining and retaining employment21. In Ontario, the Making it Work policy framework outlined the provision and implementation of a comprehensive employment supports strategy for people with SMI, inclusive of the specialized supports recommended by evidence-based practices3.
Despite these policy recommendations, provincial reports reveal that Ontario is not effectively assisting people who have SMI to find and maintain employment18. Further, survey data regarding service needs indicate that assistance with employment remains unmet. This is partly attributed to mental health service providers' lack of recognition of this client need22, especially in northern and rural places5. Research indicates that people with SMI who live in rural places are less likely than those living in urban centers to have access to satisfactory employment services or to become gainfully employed23. However, what the statistics and reports fail to inform us is why people with SMI experience limited employment success in northern places, and how this occurs despite the existence of a policy framework for employment, evidence based practices that can assist us to do better24,25 and a large investment in community mental health teams by the province of Ontario3,26. This was the focus of the larger study.
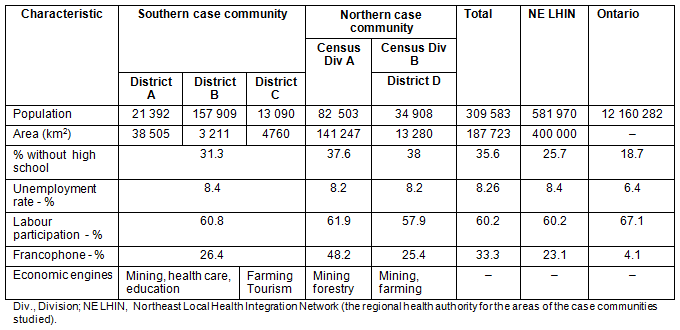
The purpose of this case study was to broadly examine access to competitive employment for persons who experience SMI and, in particular, to more fully explore the influence of place. A case study was designed to examine the experience of access to competitive employment for persons who experience SMI within and across two northeastern Ontario case communities. The cases chosen for study were two geographic areas in northeastern Ontario which provide best-practice mental health services to persons with SMI, specifically, assertive community treatment and intensive case management services. Each case community provided services in urban and rural places and could be purposively sampled for mental health users, providers and decision-makers involved in service planning and delivery. The northern case community spanned 117 400 km2 and was primarily rural. The southern case included 192 400 km2, of which approximately 35 000 km2 is rural (Table 1). The case studies were both descriptive, in that they provided a detailed account of the context of the communities within which persons within SMI lived their lives, received services and sought employment; and interpretive, because the goal was to develop conceptual categories and expand what is known about accessing employment in northern and rural places.
The case study design was guided by community-based participatory research (CBPR) methods27. Consumer and site partner advisory groups were established for the purposes of: (i) generating knowledge and understanding of access to employment at the local level and across an expansive geography; (ii) translating the knowledge gained with interventions, policy and social change to improve the health and quality of life of community members; and (iii) ensuring that the individuals, providers and decision-makers involved in employment services in northeastern Ontario were positioned to inform the process and products of this study.
Table 1: Demographic characteristics of case communities (data source28)
Data collection
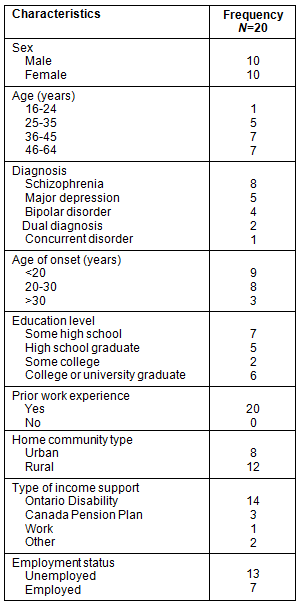
All participants completed a socio-demographic questionnaire which asked empirically-driven questions about variables known to foster employment success (Table 2). The primary data were augmented by customized statistical tables provided by the Ministry of Community and Social Services. These data tables related to the employment outcomes, tenure, earnings and economic self-sufficiency of 4112 persons with SMI who resided in the case communities and who were beneficiaries of the Ontario Disability Income Support Program (ODSP)29. The secondary data provided a portrait of employment rates for persons with SMI across the northeastern Ontario landscape during the data collection phase.
Qualitative data collection techniques included both individual and group interviews. In total, 46 individuals participated in interviews, including: 20 persons with SMI (12 rural- and 8 urban-residing), 18 providers and eight decision-makers. Most providers and all decision-makers were urban-residing. Providers included individuals providing employment services for either the mental health or vocational services sectors. Decision-makers were identified by the site partner agencies or consumer advisory as an individual who was positioned to inform financial or program decisions regarding employment services within the case communities. Decision-makers included Executive Directors, Chief Executive Officers, and/or program/regional directors. Interviews were conducted in both urban and rural case communities, audio-taped using a digital recorder and transcribed verbatim. Field notes were written following each interview to reflect the researcher's thoughts and observations, and were included in the data analysis. All participants were provided a letter of information about the risks and benefits of participation and signed a consent form prior to participating in an interview.
Ethics approval
The Laurentian University Research Ethics Board granted ethics approval for this study (#2008-07-10). All names and places are pseudonyms for the purposes of confidentiality.
Table 2: Aggregate socio-demographic characteristics
of Northeastern Ontario consumer participants
Data analysis
The interview transcripts were examined mainly through inductive analysis; that is, categories of meaning were derived from the data as opposed to imposing a pre-defined coding system. Transcripts were read several times looking for comments, patterns or interesting points that stood out in order to answer the research study questions. Categories which bore some relationship to the issues under investigation were amalgamated to form the central themes of the study. These themes were further scrutinized to see whether they were supported across all levels of data as well as across the two case communities30. Interviewing continued to the point of informational redundancy, whereby further interviews did not contribute new information or insights31.
Feedback was additionally requested from the community to engage them in dialogue regarding their interpretation of the findings, respecting their contextual understanding of the problem, and sharing their interpretation of what these findings mean for their community. The preliminary cross-case conceptualization was subjected to feedback from the consumer advisory, and from site partner agencies. All study participants provided feedback on the findings through a member checking process. The results presented draw upon the larger study, and highlight the influence of place on access to employment for persons with SMI.
The findings are drawn from the larger study and are informed by all 46 participants in the primary sample, and enhanced by the secondary data representing 4112 beneficiaries of income support residing in the case communities29.
Employment landscape of the case communities
In this study, consumer participants clearly indicated their interest in working, yet the primary and secondary data reveal that accessible and meaningful work opportunities were limited in the case communities. Despite the existence of best practice teams with dedicated vocational specialists, employment support specialists, and vocational service providers in the case communities, few individuals with SMI residing in the case communities were participating in employment during the study period. To provide some portrayal of the employment landscape of the case communities, data from the secondary tables is provided. In total, 358 individuals of the 4,112 beneficiaries (8.7%) reported employment earnings in the case communities. Similar rates of employment were reported for each case community (8.7%). Urban individuals, however, experienced greater employment success than rural beneficiaries. In the southern case community, 91.5% of the beneficiaries (n=43) who reported employment earnings resided in an urban area, compared with 8.5% of rural residents (n=4). In the northern case community, 76% of the beneficiaries (n=19) reporting earned income were urban-residing compared with 24% (n=6) who were rural-residing. Regarding employment tenure, of the 358 individuals reporting employment earnings, only 8.6% (n=31) retained their employment beyond 6 months, and none were employed beyond 12 months. Considering earnings, 37% of the beneficiaries reporting employment income earned less than $250, and 72% earned less than $750. Fewer than 3% reporting income between April 2008 and March 2009 earned enough income to exit the income support program during the study period29.
How does place influence access to employment?
In this study, place was found to influence access to employment in five ways: by limited access to employment support services in rural places, and to recommended ratios in urban places; by the use of different models and practices that were inconsistent with best practices for people with SMI; by the lack of a plan for the implementation of employment services in the case communities; by limited use of the available, dedicated vocational resources for employment purposes; and by inadequate supports provided to persons with SMI who wish to enter the workforce.
Limited access to employment services
Access to employment-support specialists in rural places was particularly problematic in the case communities, and the existence of vocational programs and services did not necessarily ensure access to employment for persons with SMI. Becker and Drake32 and Becker, Xie, McHugo, Halliday, and Martinez33 found that access was associated with the staffing and funding dedicated to SE, as well as by the percentage of SE specialists per client with SMI served by the mental health agency. According to Shawna, a local decision-maker, 'only one employment specialist existed for all of the northern case community' (an area in excess of 117 000 km2), 'and two specialists provided services for 10 000 clients' over an area of 192 000 km2 in the southern case community. Access to mental health agencies providing employment services in the case communities was similarly limited - no vocational specialist existed on any mental health team in the northern case community during the course of the study. Additionally, few vocational service providers were willing to travel to rural places within the case communities, often because the funding formula did not make it economically feasible. The existence of vocational services in urban places, however, did not necessarily provide access to employment in adjacent rural communities. Limited human resources and the need to travel large distances to provide these services often made the timeliness of access to services ineffective, and the ability to meet the SE principle of rapid placement (ie within 3 months of starting employment services) into employment unattainable in many rural communities.
Services not based in evidence-based practices
A second consideration of access is related to the effectiveness of the programs and services provided in the case communities. In general, employment services were provided by different programs, teams and agencies (eg Ministry of Health programs such as, Assertive Community Treatment Teams (ACTT) or Intensive Case Management (ICM); non-government organisations (NGOs) such as consumer initiatives or the March of Dimes; and, some private businesses which brokered employment services to persons with a disability), and were based in a variety of employment models and philosophies. Moreover, individuals with SMI were informed that while they had a choice of vocational service providers; however, few were given any parameters upon which to help guide their decision-making. Becker et al. found that rates of competitive employment were best predicted by fidelity to SE principles as well as to local employment rates33. However, despite the existence of a provincial policy framework for employment that is based upon key SE principles, there was little evidence of these principles in local practices within the case communities. In fact, where they did exist, there was little coordination of the various services and supports available in the community. Given that unemployment rates in northeastern Ontario typically exceed provincial rates, the development of local capacity to provide high-fidelity SE services would seem important to the issue of access. Providers described doing their best to provide a good service but few were able to articulate SE practices that might improve their success. Further questioning revealed that no regional or organizational plan existed for employment services among the mental health providers in the case communities, contributing to an inefficient use of their limited resources.
No plan for employment
A third consideration of access (also, related to the first and second considerations), is the lack of a local plan for employment supports for persons with SMI within the case communities. It was difficult to discern, either directly by questioning participants, or indirectly through observation, any local or regional plan for the employment of persons with SMI, especially on mental health teams. Limited provider knowledge of the Making it Work policy framework3 and best-practice SE models24,25,34 made it difficult for them to draw on this knowledge to guide local implementation of employment programs and practices. Where employment was considered by a mental health provider, services were provided largely in the absence of an organizational plan, lacking fidelity to best practice SE models, and without dedicated funding or staff time for providing employment services.
Limitations created by inefficiencies
A fourth consideration of access is related to the limited allocation of human resources to employment in the case communities, in general, and of the limited use of employment-dedicated human resources on mental health teams in particular. Where vocational specialists did exist on mental health teams within the case communities, primary data indicated that less than 25% of their time was dedicated to providing employment-related services. The limited participation of the mental health sector in employment resulted in these services being largely downloaded to the brokered vocational service agencies, despite a recognition by the Ministry of Health and Long Term Care that brokered services have been shown to be largely ineffective3. These brokered vocational services were largely unaware of SE practices for persons with SMI, and even less aware of the unique challenges that persons with SMI may face as they attempt employment. As Ken (participant, SMI) stated, 'as a brokerage agency that knows nothing about mental illness, that's a matter of mathematics for me'. Beyond mental health teams, access to employment remained limited by a lack of collaboration between those human and fiscal resources which are currently available and allocated for employment. There were a variety of vocational service providers in the case communities. There were fewer vocational providers, however, in the northern case community. Theoretically, people with SMI should experience improved access to effective and efficient employment services if vocational and mental health providers collaborate to bridge the effects of distance (place) and limited human resources for employment. In the case communities studied, collaboration was limited to the occasional phone call or letter reporting employment attempts made by the vocational agency. In neither case community was collaboration embedded in everyday practices.
In general, while resources dedicated to the employment of persons with SMI in the case communities would provide an impression of access, the limited employment rates in this region suggest otherwise. The availability of employment services did not ensure access to employment. Similarly, the lack of timely access to services due to geography and distance, the lack of collaboration of the limited human and fiscal resources dedicated to employment in the case communities, and the random manner with which employment services were provided all challenged access in the case communities. The limited employment success of individuals with SMI in the case communities raises the further question of why employment rates remain low despite an investment in community mental health teams26 and employment services?
Inadequate supports for employment success
A fifth and final consideration of access concerns the importance of supports, and of the existing association between employment services and benefits with an individual's funding source, instead of with their individual needs. There were several instances where participants lacked access to educational supports because they were not in receipt of benefits from Ontario Works, received less follow-along support because they were not an Ontario Disability Support Program beneficiary, or left a decent-paying job because they received Canada Pension Plan (CPP) income support (CPP imposes a low yearly-earnings ceiling). Instead of linking needed services and supports to particular income support programs, participants suggested linking supports to individuals in relation to their specific needs. A study by Rinaldi and Perkins found that people with more complex needs and those who have been in contact with services for longer periods may require a longer period of support if they are to secure and sustain competitive employment35. Differing levels of support are likely indicated in order to improve outcomes for all persons with SMI. However, implementing the individualized and comprehensive supports needed to ensure better outcomes will require a fundamental shift in how employment services and supports are currently envisioned, structured, and provided in Ontario.
Discussion
The present study suggests a need for place-related considerations in providing employment services in northern and rural places - especially given the large geography that service providers and mental health teams are expected to cover. Participants revealed how substantial physical distances between rural and small towns made it difficult for persons residing in these areas to have timely access to employment specialists, and ultimately to employment. In fact, during the course of the study, no service provider (other than a long-distance work-at-home provider) was willing to provide services to rural residents in the southern case community because the current funding model simply did not make it financially worthwhile. Services funded to include place-related costs will undoubtedly be more expensive and there may be limited political support for this recommendation in the current policy climate.
There was some indication from the literature that working in collaboration may be a feasible way to bridge the effects of place36 and to provide best practice SE services23. However, promoting collaborative practices will require several changes to how employment supports are currently structured and funded in Ontario. To this end, there are five suggested changes to the current funding structure of the ODSP, employment supports program that warrant consideration.
A first suggestion is to provide financial and other incentives to organizations and sectors for working collaboratively. Currently, providers are required to compete for clients, employer contacts and jobs. Instead, service providers could be incented for employer contacts and job development activities. Financial incentives for securing employer contacts regardless of which client fills the position, instead of the current competitive reimbursement schedule makes sense on many levels: it removes the need to retain developed jobs within one's agency and encourages matching the right person with the right job. The establishment of a minimum standard for the number of employer contacts and developed jobs to maintain a brokered provider status with ODSP might help to ensure that sufficient jobs are available for persons with a disability.
The second suggestion is the establishment of a centralized electronic database of jobs for persons with a disability. A central, accessible database will help providers to match the right job with the right client. In turn, this may help to reduce the competition that currently restricts access to jobs beyond the individual's current service provider.
A third suggestion is to make funding or becoming a brokered service provider contingent on collaboration with the mental health sector teams, and also, to place conditions on mental health teams that provide employment services to work collaboratively with vocational service providers. These collaboration agreements could be embedded into Multi-sectoral Service Accountability Agreements (M-SAAs) negotiated with regional health authorities on an annual basis. One of the strongest predictors of better employment outcomes involved collaboration between mental health and vocational service sectors25.
A fourth suggestion is to ensure that adequate supports are provided within the employment supports system to foster better outcomes; including, longer tenured employment for individuals with SMI and other disabilities. In this study, of the 8.7% ODSP beneficiaries in the communities who reported employment earnings, few worked beyond six months, and none beyond one year. Rewarding service providers for helping individuals to achieve longer employment tenure instead of rewarding them for the job placement or reaching arbitrary 13 week job retention targets may be a useful strategy. Likewise, expanding local authority to grant wage subsidies, including allowances for place-related effects, might improve the capacity of local communities to better meet the SE principle of rapid placement, and thereby, improve access to employment.
The fifth and final suggestion concerns the policy landscape of employment support programs and services in Ontario. Policy attention is required to build in incentives for collaboration or to provide an alternate mechanism for funding employment programs that accounts for physical distance and limited human health resources. Current structural divisions between the Ministry of Health, the Ministry of Community and Social Services, and the Ministry of Colleges, Universities and Training reinforce current silos and hinder addressing the social determinants of health (eg employment). Poland et al have suggested that the lack of collaboration and cooperation within Ontario's health system is not surprising given that funding silos in Ontario were seen to promote competition for 'turf' between agencies and largely discourage inter-sectoral collaboration and cooperation (p130)37. They found that in every 2 of the 4 sites studied, community collaboration was seen as 'a nice thing to do' if time and funds permitted, and that hospital motivation to engage in community collaborations had more to do with good PR than with effecting change or promoting a sense of community (p131)37.
Currently, employment programs and services appear organized for the providers of employment services and not necessarily for the recipients of the service. While prevailing ideas of government promote the notion that the existence of programs and services constitutes access to them, or that the availability of services provides equality of opportunity, the findings of the present study suggest otherwise. One of the objectives of this study was to better understand access to employment and how place might influence it. Based on the information provided by the research participants, the secondary data sources on employment rates of persons with SMI, and the limited knowledge of evidence-based SE practices for persons with SMI within the case communities, it would be fair to conclude that access is a problem. The mere presence of vocational programs - meeting the equality of opportunity condition - has not necessarily translated into programs or services that are effective and efficient and has not ensured access to employment for persons who experience SMI. The presence of service providers in the community and the availability of employment opportunities that neglect the influence of place on access fail to achieve equality-of-outcomes for individuals with SMI. To meet the equality-of-outcome in employment, this study's findings suggest that a variety of services and supports are required to meet people's diversity in age, education, skill/ability, and work experience across different contexts. Instead, the current system lines up everyone seeking employment and says, 'Here is what we have determined we will provide, and the rest is up to you'. Unfortunately, this is ineffective for people who are psychosocially and geographically vulnerable.
Provincial cross-sectoral policy attention is also required so that employment can be tucked into current mental health/health services. Local and regional health authorities can facilitate this integration process by assisting programs with the process of integration, by advocating for funding dollars that are freed up by the integration to be rolled back into the integrated service for team development, joint training initiatives and model fidelity evaluations, and by embedding a requirement for collaboration into funding agreements.
The social policy landscape is the final arena for comment, as expressed through the funding model and the organizational structure of employment support programs in Ontario (ie ODSP). In many ways, this funding model was found to be incompatible with the policy landscape of the health and community mental health sector. In fact, the inconsistencies were confusing to providers who were required to work within the funding framework, but who knew intuitively and experientially that these practices limited access to employment for people with SMI. According to Nelson, simply reallocating resources from institutions to community mental health services does not ensure that there is a fundamental transformation of mental health policy and services38. Some institutional programs may be repackaged in the community, yielding 'old wine in new bottles. For example, many community treatment and rehabilitation approaches have retained the character of the institutional paradigm' (p251)38. Clearly, a variety of challenges exist within social policy concerning the employment of persons with SMI. These challenges include income support programs and disincentives to employment, a focus on assessment and prevocational activities instead of employment, and a focus on risk and liability instead of fostering meaningful lives for persons with SMI.
This article drew on the findings of a larger study to highlight place as an important yet often neglected variable in accounting for the low employment success of persons with SMI in northeastern Ontario. In particular, connections are drawn between the ways in which place challenges the implementation of best practice SE and the low employment success experienced in this region of the province. While place does help to explain why people with SMI experience low employment success, it does not account for all of the blame. Instead, it was suggested that there are many aspects of the current structure and funding of employment supports in Ontario that are contrary to best practice evidence, and which do not reflect place-related considerations. Competitive models which do not foster collaborative practices, which reward providers rather than people with SMI, and which are more based in economic bottom lines than in best practice evidence are some of the policy issues requiring further attention.
Acknowledgements
The first author acknowledges the financial support of the Canadian Institutes for Health Research (CIHR) for a clinical fellowship and a research grant, and gratefully acknowledges the research participants, site partner agencies and advisory bodies for their insights, support and determination to raise the employment profile for people with SMI in northern Ontario.
References
1. Goering P. Making a difference: Ontario's community mental health evaluation initiative. Toronto, ON: Canadian Mental Health Association, 2006; 34.
2. Krupa T, Kirsh B, Gewurtz R, Cockburn L. Improving the employment prospects of people with serious mental illness: five challenges for a National mental health strategy. Canadian Public Policy 2005; XXXI(Suppl): S59-63.
3. Ministry of Health and Long Term Care. Making it Work: Policy framework for employment supports for people with serious mental illness. Cat.# 7610-4232419. Toronto, ON: Queen's Printer of Ontario, 2001.
4. Public Health Agency of Canada. Towards a healthy future: Second report on the health of Canadians. Cat. H39-468/1999E. Ottawa, ON: Xxxx, 1999.
5. Ministry of Health and Long Term Care, Northeastern Ontario Mental Health Implementation Task Force. The time for change is now: Building a sustainable system of care for people with mental illness and their families in the northeast region. Employment and education. Toronto, ON: Health Canada, 2002; 201-217.
6. Crawford C. Improving the odds: Employment, disability and public programs in Canada. North York, ON: L'Institut Roeher Institute, 2004.
7. Razzano LA, Cook JA, Burke-Miller JK, Mueser KT, Pickett-Schenk SA, Grey DD et al. Clinical factors associated with employment among people with severe mental illness: findings from the employment intervention demonstration program. Journal of Nervous and Mental Disease 2005; 193(11): 705-713.
8. DesMeules M, Pong R, Lagacé C, Heng D, Manuel D, Pitblado R et al. How healthy are rural Canadians? An assessment of their health status and health determinants, Summary Report. Ottawa, ON: Canadian Institute for Health Information, 2006.
9. Parr H, Philo C, Burns N. Social geographies of rural mental health: experiencing inclusions and exclusions. Transactions of the Institute of British Geographers 2004; 29(4): 401-419.
10. Twohig PL. Written on the landscape: health and region in Canada. Journal of Canadian Studies 2007; 41(3): 5-17.
11. Mental Health Commission of Canada. Towards recovery and well-being: a draft framework for a mental health strategy for Canada. Ottawa, ON: Canadian Institute for Health Information, 2009.
12. Mechanic D, Bilder S, McAlpine DD. Employment of persons with serious mental illness. Health Affairs 2002; 21(5): 242-253.
13. Sudbury Manitoulin Workforce Partnerships Board. 2009 TOP Report, vol 2(2). Sudbury, ON: SMWPB, 2009.
14. Ministry of Health and Long Term Care. Making it happen: Operational framework for the delivery of mental health services and supports. Cat.#2231489. Toronto, ON: Queen's Printer for Ontario, 1999. Available: http://www.health.gov.on.ca/english/public/pub/mental/pdf/MOH-op.pdf (Accessed 13 October 2006).
15. Harnois G, Gabriel P. Mental health and work: Impact, issues and good practices. Geneva: World Health Organisation, International Labour Organisation, 2000.
16. Wilton RD. Working at the margins: Disabled people and the growth of precarious employment. In: D Pothier, R Devlin (Eds). Dis-ability. Critical disability theory: Essays in Philosophy, Politics, Policy and Law, 1st edn. Vancouver, BC: UBC Press; 2006; 130-150.
17. Baron RC, Salzer MS. Accounting for unemployment among people with mental illness. Behavioural Science and Law 2002; 20(6): 585.
18. Koegl C, Durbin J, Goering P. Mental health services in Ontario: how well is the province meeting the needs of persons with serious mental illness? Analysis of data collected during the Provincial Psychiatric Hospital and Community Comprehensive Assessment Projects. 2923/03-04. Toronto, ON: Health Systems Research and Consulting Unit, Centre for Addictions and Mental Health, 2004.
19. Ontario Technical Advisory Panel. 2005/06 Ontario ACT data outcome monitoring report. Ottawa, ON: Ontario Technical Advisory Panel, 2007.
20. The Federal/Provincial/Territorial Ministers Responsible for Social Services. In unison: a Canadian approach to disability issues. Cat. MP43-390/1998E. Ottawa, ON: Human Resources Development Canada, 1998.
21. Standing Senate Committee on Social Affairs, Science and Technology. Out of the shadows at last: Transforming mental health, mental illness and addictions services in Canada. Ottawa, ON: Government of Canada, 2006.
22. Crane-Ross D, Roth D, Lauber BG. Consumers' and case managers' perceptions of mental health and community support service needs. Community Mental Health Journal 2000; 36(161): 178.
23. Gold PB, Meisler N, Santos AB, Carnemolla MA, Williams OH, Keleher J. Randomized trial of supported employment integrated with assertive community treatment for rural adults with severe mental illness. Schizophrenia Bulletin 2006; 32(2): 378-395.
24. Bond GR, Drake RE, Becker DR. An update on randomized controlled trials of evidence-based supported employment. Psychiatric Rehabilitation Journal 2008; 31(4): 280.
25. Drake RE, Bond GR. Supported employment: 1998 to 2008. Psychiatric Rehabilitation Journal 2008; 31(4): 274-276.
26. Systems Enhancement Evaluation Initiative (SEEI) Coordinating Centre. Moving in the Right Direction: SEEI Final Report. Toronto, ON: SEEI, 2009; 1-52.
27. Israel BA, Eng E, Schulz AJ, Parker EA. Introduction to methods in community-based participatory research for health. In: BA Israel, E Eng, AJ Schulz, EA Parker (eds). Methods in community-based participatory research for health. San Francisco, CA: Jossey-Bass, 2005; 3-26.
28. North East Local Health Integration Network (LHIN). North East LHIN Integrated Health Service Plan: Sociodemographic Profile. (Online) 2006. Available: http://www.nelhin.on.ca/uploadedFiles/Home_Page/Integrated_Health_Service_Plan/Sociodemographic.pdf (Accessed 13 October 2006).
29. Statistics and Analysis Unit, Policy Analysis and Research Branch. Characteristics of ODSP Adult Beneficiaries with mental disorders in northern Ontario. Toronto, ON: Social Policy Development Division, Ministry of Community and Social Services, 2009.
30. Stake R. The art of case study research. Thousand Oaks, CA: Sage, 1995.
31. Sandelowski M. Focus on research methods. Combining qualitative and quantitative sampling, data collection, and data analysis techniques in mixed-method studies. Research in Nursing & Health 2000; 23: 246.
32. Becker DR, Drake RE. Supported employment interventions are effective for people with severe mental illness. Evidence-Based Mental Health 2006; 9(1): 22.
33. Becker DR, Xie H, McHugo GJ, Halliday J, Martinez RA. What predicts supported employment program outcomes? Community Mental Health Journal 2006; 42(3): 303.
34. Becker DR, Drake RE. A working life: The Individual Placement and Support (IPS Program). New York: Oxford University Press, 1993.
35. Rinaldi M, Perkins R. Implementing evidence-based supported employment. Psychiatric Bulletin 2007; 31: 244-249.
36. Minore B, Boone M. Realizing potential: improving interdisciplinary professional/paraprofessional health care teams in Canada's northern aboriginal communities through education. Journal of Interprofessional Care 2002; 16(2): 139-147.
37. Poland B, Graham H, Walsh E, Williams P, Fell L, Lum JM et al. Working at the margins or leading from behind? A Canadian study of hospital-community collaboration. Health and Social Care in the Community 2005; 13(2): 125-135.
38. Nelson G. Mental health policy in Canada. In: A Westhues (Ed.). Canadian social policy: issues and perspectives, 4th edn. Waterloo, ON: Wilfrid Laurier University Press, 2006; 245-266.



