It is widely recognised that major hospitals provide a learning environment that is neither representative of community morbidity nor conducive to a holistic approach to patients and their illnesses. Most patient care is delivered outside the hospital by primary-care providers1: general practitioners, specialists in their private rooms and other community-based medical and allied health-care providers. In two Australian rural communities, vast distances and a scarcity of medical educators, combined with the desire to base the curriculum in the community, provided the impetus for designing a novel, patient-centred, longitudinal, web-supported medical curriculum.
The program described was developed in the Greater Murray Clinical School of the University of New South Wales (UNSW), Australia, which was the first of the Commonwealth funded Rural Clinical School initiatives. The program began simultaneously in the school's two campuses in Wagga Wagga and Albury, NSW, in the year 2000 with students on rotation for year 4 (of a six-year course) and progressed to a cohort of 12 full-time students in 2001. Most of the early educational development described in this article took place at the School of Rural Health based at Wagga Wagga, with a major campus at Albury. The School lies within the area of the Greater Murray Area Health Service which covers an area equal in size to that of England and Wales and has a population of approximately 250 000 (Fig 1). The characteristics of the population are provided (Table 1).
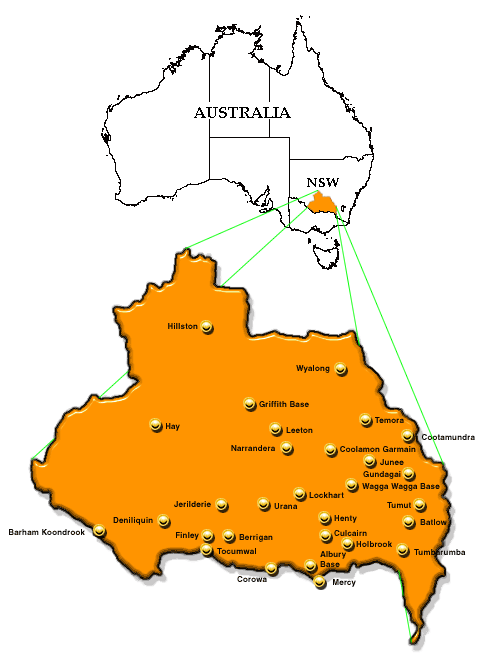
Figure 1: Map of the study area showing the two campuses at Wagga Wagga and Albury, New South Wales, Australia.
The basic approach of the program (termed the longitudinal, patient-centred method) was to introduce students to patients in community settings, ensuring that the students follow the progression of those patients' illnesses along the different pathways in the health-care system (Fig 2). From an educational viewpoint, this method of studying a few patients in depth has been shown to be more effective than seeing many patients superficially2. In addition to studying the patient's disease (the biomedical aspects of being unwell), sickness (the role of, and acceptance by society in relation to the unwell person), and illness (what the patient experiences) it was expected that students would explore the patient's semiotic (understanding the symbolism, meaning) needs of their illness(es). Thus, the somato-psycho-socio-semiotic model provided the educational philosophy underpinning the curriculum3.
Table 1: Population characteristics of those in the Greater Murray Area Health Service area
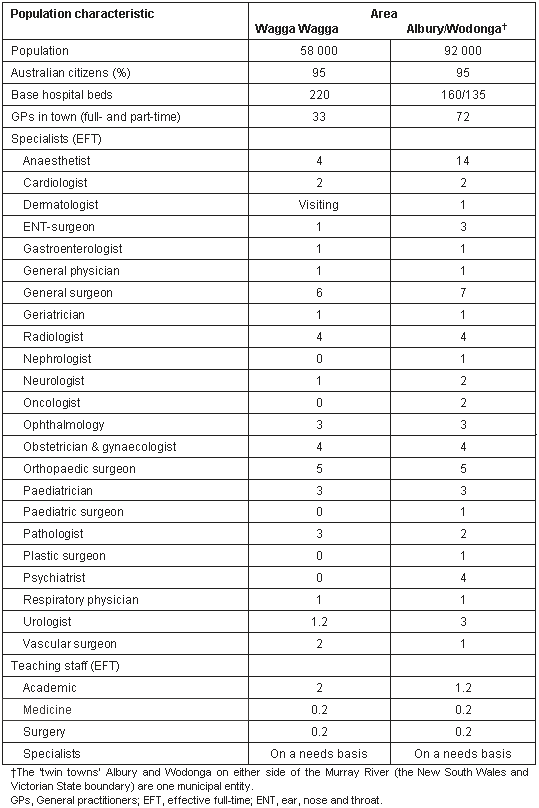
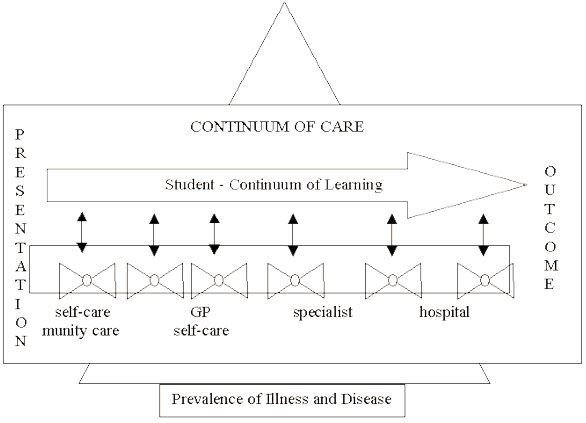
Figure 2: The longitudinal patient-centred curriculum in a community context.
To enable students to learn readily from patients, the academic staff devoted a large amount of time and energy to helping students learn proper 'history taking' prompted by clinical reasoning and hypothesis generation, rather than by the ritual collection of facts. This approach encouraged learning in the context of a patient, and attempted to integrate the students' developing clinical skills with their formal medical learning. One vivid example of this approach was when a student traced an elderly man who was breathless through pathology showing his anaemia, colonoscopy revealing his carcinoma, CT scan showing liver secondaries, breaking the bad news, attendance in theatre and presentation of the resected colon and photomicrographs of his carcinoma at the integration tutorial. This approach was resourced by clinical as well as academic teaching staff drawn from various disciplines, including general practitioners and, at one time or another, almost all the specialists in the town. Regular teaching of examination skills, both at the bedside and in the skills laboratory situated in the two teaching hospitals, complemented the teaching methodology. Pathology teaching was routinely conducted by local private pathologists. Symptom-based computer assisted instruction packages consolidated the students' real life experiences.
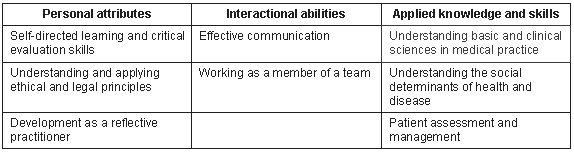
The overall design of the curriculum was appreciative of the limitations associated with focusing on competences (or, what individuals know to do in terms of knowledge, skills and professional behaviours) alone. Tomorrow's doctors need a much wider array of capabilities (the extent to which individuals actually perform, can adapt to change, generate new knowledge, and continue to improve, extend and adopt their performance) to be part of the evolving approach to health care based on the concept of health-care teams (Table 2). In addition, tomorrow's doctors need to be mindful of their economic responsibilities to their patients, the health-care team and the economy at large4.
Table 2: Summary of the desired capabilities of students at graduation as outlined in the program objectives of the to be developed curriculum of the University of New South Wales, Australia (source: Guidelines for scenario-based learning, University of New South Wales internal document (28 August 2001)
Reflecting the belief that student capabilities are enhanced through feedback and reflection on performance, students were required to maintain a personal reflective journal and a logbook of patient contacts. In addition, the weekly 'integration tutorial' served to provide a forum for discussion and assessment of their 'longitudinal patient contacts'. Here the staff assisted students to link the pathophysiological aspects of the patient's disease to the social and psychological circumstances in which it occurred. The tutorial and patient contact over time encouraged students to explore with patients what their disease meant to them (the semiotic component).
Teaching was process-focused. Rigid goals with prescriptive, inflexible content were largely avoided. Instead, learning was facilitated by the construction of learning goals; by reflecting on the experiences gained from following 'longitudinal' patients through the health-care system; by finding, absorbing and condensing information; by presenting to peers and tutors; and by receiving feedback from these individuals. Opportunities for consolidation of knowledge and skills occurred continuously throughout the student's day, with actively promoted critical appraisal and self-reflection. At an individual level, adequate coverage of the curriculum relied on self-directed and group learning, and the development of learning strategies that served as the foundation for lifelong learning.
In summary, the aim of the school was to produce graduates who are compassionate, communicative, clinically competent and economically-responsible. It was expected that graduates would be well equipped to enter any branch of medicine. A detailed curricular approach and its implementation have been described elsewhere5.
The first year's experience: evaluation and reflection
It was believed that this approach to curriculum delivery was based on the best available evidence in undergraduate medical education. It was also designed to be suitable for implementation in an environment with rich clinical resources, limited capacity to deliver formal lectures, and busy clinicians whose time is spent primarily with clinical work.
A paradigm shift for staff
The notion of a community-based medical course was foreign to many clinicians and teaching academics who were themselves taught by a system that relied heavily on the traditional hospital-based teaching model, in which students were required to be passive-receptive. Communication was according to a defined hierarchy, and hospitals functioned with long-stay in-patients and large outpatient departments. In recent times not only have there been changes from the traditional approach, but hospitals have also shifted to day cases and shorter stays for in-patients. In our situation, this shift was further exacerbated because, apart from the intention to be community-based, neither of the rural hospitals associated with our clinical school had outpatient departments. The issues for incoming clinicians and teaching academics were thus twofold: the educational philosophies and methodologies were new, and the familiar teaching environments had changed dramatically.
Ideally, staff induction sessions would have occurred prior to the arrival of the first cohort of students. Unfortunately such sessions did not occur and the lack of orientation to the philosophies underpinning the curriculum resulted in considerable uncertainty. Some staff were sceptical of the value of a facilitative approach to teaching, having been used to the traditional highly content-focused lecture format. In addition, other staff found the actual implementation of the facilitative approach difficult, particularly when teaching occurred during simultaneously consulting in private practice.
A paradigm shift for students
As well as the staff, the students had difficulties recognising the relevance of the community-based learning environment. Many were resistant to a context-based approach where they had to learn to think, to understand, to build upon previous knowledge and to apply this knowledge when and where appropriate.
Although examinations are recognised as one of the most powerful motivators to study, examinations largely assess factual knowledge (competences) but focus little on applied knowledge (capabilities). Many of the students had reached their fourth year of medicine by last-minute 'cramming', a phenomenon observed by Huxley in 18776. This method of learning ultimately results in a limited ability to reconstruct and apply information at a later date.
The students' lack of appreciation of the context in which a patient develops an illness, which itself enforces certainty, hindered the uptake of the many opportunities of the community-based learning environment. It was expected that the students would easily make the paradigm shift from one of separate, single foci (a disease-focused model), to one that required more lateral and expansive cognitive processing of the patient in context (a somato-psycho-socio-semiotic illness model). In practice this shift proved more difficult than was expected.
Initial student results
It was discovered that students have a strong tendency to compare their clinical experiences with one another, particularly with their urban peers. Considerable effort was required to allay their fears of missing out on 'that crucial case' without which they believed it would be impossible to pass their exams. Those anxieties may in part have been attributable to the fact that these students were the first cohort at the clinical school. It was anticipated that such fears would decrease as the school became established.
It was pleasing to discover that the first group of full-time fourth-year students of the School of Rural Health were placed in the top one-third of their year with an average aggregate mark above that of their Sydney-based (urban) peers. Of note were the comments of visiting examiners who were unanimous in their assessment of the students' impressive clinical capabilities. Due to circumstances beyond our control it was not possible to compare the students' performances in their pre-clinical years to their Year 4 marks, although the students themselves told us their performances were better than in previous years. Despite the success of the first year, many issues to be worked on were also identified.
Where to from here?
Staff and student induction
In hindsight, students and staff needed induction sessions to explain the principle of the longitudinal, patient-centred curriculum and the somato-psycho-socio-semiotic philosophy of patient care. Given the facilitatory nature of the curriculum, staff and students would benefit from joint sessions to explore fears and concerns with this curricular approach, and to establish teaching-learning responsibilities and accountabilities within this community-based course.
To overcome teachers' concerns with a facilitatory approach, and to allay feelings of inferior or inappropriate teaching resulting from juggling student support and running a busy private practice, professional development must address two important issues. The first involves exploring the suitability of a patient-centred, longitudinal approach in a community setting. In this regard the examination results provided reassurance that this teaching approach provided excellent exposures for clinical learning. The second point relates to exploring teaching strategies and goals within the patient-centred approach, including identifying when to use facilitation, didactic presentations or demonstrations. The latter two teaching approaches proved to be of value and must continue, as directed by the teaching context.
A substantial number of additional issues not covered adequately elsewhere in the curriculum could arise from contact with patients. The issues include topics as diverse as dietary assessment, effective counselling skills for preventive health, therapeutics, and ethical and medico-legal concerns which students need to understand in context. This is outside the expertise of most teaching clinicians and calls for the development of special teaching/learning activities within the patient-centred curriculum so that these issues become a natural part of the practice of medicine.
Log books and reflection
Both staff and students alike need to be sufficiently responsive, self-directed and flexible to maximize learning based on the availability of patients. To ensure that students receive a balanced clinical experience, they continue to be required to maintain a logbook of their patient contacts. This allows both students and staff to compare their exposures against those expected as outlined in the University of New South Wales Faculty of Medicine Curriculum Handbook.
Reflection on experiences makes them more valuable. To this end students will continue to be expected to keep a reflective journal that in conjunction with their patient logbook form the basis for tutorials. This was especially so for the 'integration tutorial' where students' longitudinal patient experiences and focus on the interplay of the somato-psycho-social with the semiotic aspects of the patient experience were evaluated.
Computer-assisted learning
It is hoped that the limitations in teacher resources will be reduced by the continuing development of computer-assisted instruction packages7. These resources must be integrated into student learning activities and referred to by all teachers. So far only the main symptom complexes have been covered; hence, faculty staff have had to devote a large proportion of their time to developing the missing areas. Equally these resources need ongoing review, as well as refinement from an educational point of view. Achieving this goal will require full time IM/IT (information management and technology) support.
Assessment reform
To achieve the full potential of this community-based program, examinations must be adapted to reflect the values and goals of the course. In broad terms, assessment tools should test knowledge-in-action, by allowing students to demonstrate their capabilities in the doctor-patient interaction. Written papers should also be structured to assess the contextual application of knowledge rather than the 'regurgitation' of facts alone.
Evaluation issues
As a final point, one of the responsibilities with the design and implementation of any new educational approach is the evaluation of that approach. The challenges lie in how to define, assess and accurately interpret the highly complex and multidimensional nature of the 'processes' and the 'products' involved. Are our students and ultimately our graduates fundamentally different from those from other clinical schools? Do those differences translate into clinical practice and how is their practice different and to what extent is it retained over time? Do the outcomes affect the doctor-patient interactions and how do those differences impact on health care? These questions must be addressed to understand the impact of our community-based, patient-centred, longitudinal approach. Further, at the micro-education level, which teaching methodologies are the most effective and the most efficient? Only with very careful in-depth qualitative and quantitative studies can this novel approach be evaluated. Such impact and outcome studies must occur within the decade following course commencement to be of benefit.
Conclusions
A community based, patient-centred, longitudinal model, as a means of delivering a clinical curriculum in a rural setting, has a sound theoretical basis. Reflecting on the first year's experience has highlighted the strength of this approach and identified areas for future improvements. To be clear about the true potential of this particular approach requires persistence with the ideals, and perseverance when resistance to or negative feedback on aspects of the program are identified.
The specific emphasis of this program on patient-based learning over, in some cases, a considerable period of time is new. In addition, the mix of community and base-hospital environments, combined with teaching by general practitioners, specialists, and other health professionals, in specialist rooms, pathology laboritories and radiology rooms represents a new approach. Our experiences have suggested that the use of this approach, combined with focused tutorials, is well able to overcome the limitations of restricted numbers of educators and available teaching time.
Furthermore, given that students reported considerable enjoyment and satisfaction with this style of and approach to learning, the long-term benefits of this patient-centred, community-based curriculum may be seen in its contribution to increased recruitment and retention of medical practitioners in rural and remote Australia.
Acknowledgement
The School of Rural Health, an Australian Commonwealth Government-funded project, is an initiative of the University of New South Wales and the Australian Department of Health and Ageing, supported by the communities of the Greater Murray and Mid-north Coast regions of New South Wales, Australia.
References
1. Gray D. Fit for the future - are medical schools going to produce the doctors the Health Service needs? Medical Education 1999; 33: 872-873.
2. Finlay I, Maughan T, Webster D. Portfolio learning: a proposal for undergraduate cancer teaching. Medical Education 1994; 28: 79-82.
3. Pauli H, White K, McWhinney I. Medical Education, research, and scientific thinking in the 21st Century (Part 1 of 3). Education for Health 2000; 13: 15-25.
4. O'Neil E. Education as part of the health care solution. Strategies from the Pew Health Professions Commission. JAMA 1992; 268: 1146-1148.
5. Sturmberg J, Reid A, Khadra M. Community based medical education in a rural area: a new direction in undergraduate training. Australian Journal of Rural Health 2001; 9(Suppl 1): S14-S18.
6. Buckley E. Basic medical education in transition. Medical Education 1993; 27: 113-115.
7. Sturmberg JP, Crowe P, Hughes C. Computer-assisted instruction - guiding learning through a key features approach in a community based medical course. Medical Teacher 2003; 25: 332-335.

