Medical schools attempt to recruit well-rounded individuals to reflect the diversity of the populations they will serve. Medical school applicants need to demonstrate a record of community service, leadership and clinical exposure, in addition to academic excellence1. Preference for admission to medical schools may be granted to students who have lived in, or are living in, particular geographical regions2.
The shortage of physicians in rural areas is well documented3, with only 9% of physicians practicing in rural areas, while 20% of the population lives in these areas3. Osteopathic medical schools have responded to the need for physicians in rural areas by producing physicians who are 1.5 times more likely to practice in a rural area than allopathic physicians4. Likewise, osteopathic medical schools yield physicians who are more likely to practice primary care compared with allopathic physicians5. Challenging these contributions from osteopathic medical schools are the increasing levels of student debt and lower income levels for primary care confronting medical students6,7. These financial issues contribute heavily to medical student intent to practice in rural areas.
The literature on the characteristics of medical students who intend to practice in rural settings spans several decades. One of the earliest works, by Steinwald and Steinwald, indicated that two of the most notable determinants of physician practice location were specialty type and the size of the community where the physicians were raised8. A decade later a study confirmed that the size of the community in which a physician is raised is a significant predictor of practice location9. Specifically, physicians raised in small or rural communities were more likely to have and follow through rural practice intentions9. Additional research has shown both personal and family characteristics to be predictive of intent to practice rural medicine. Personal characteristics predictive of intent for rural practice include graduating from high school in a small community, graduating from a small college and being in a relationship10-13. Family characteristics predictive of intent for rural practice include having parents without a university education and having parents, in-laws or grandparents living in a rural community10-13. Other factors, such as osteopathic training, being male and Caucasian have also been linked with the intent to practice in a rural setting4,5,14.
Evidence also suggests that personality type, based on the Myers Briggs Type Indicator (MBTI), is related to medical specialty choice15-17. The MBTI is a common personality assessment instrument used throughout the world. The MBTI uses four dichotomies to characterize personality type18. The first dichotomy is Extraversion-Introversion. This pair of preferences is intended to distinguish how an individual derives energy, more from the external world or the inner world of thoughts and feelings19. The second dichotomy is Intuitive-Sensing. This dimension focuses on how a person takes in information. Intuition indicates a preference for a more abstract focus of attention on patterns and possibilities. Sensing indicates a preference for a more practical focus of attention on facts and details19. The third dichotomy is Thinking-Feeling. The focus of this preference is how people make decisions. Individuals with a preference for Thinking tend to focus on logic and analysis, and individuals with a preference for Feeling tend to focus on personal values and priorities19. The last dichotomy is Judging-Perceiving. The focus of this dimension is on how people deal with their external world. Individuals with a preference for Judging tend to be decisive and prefer structure and control. Individuals with a preference for Perceiving tend to leave things open to gather more information and prefer spontaneity and flexibility19. The majority of physicians practicing in rural areas are family practitioners, and the SF (Sensing-Feeling) functional pair has been shown to be more common among family medicine physicians than specialty physicians15.
The literature indicates characteristics of medical students predictive of rural practice and these relate to the age of the medical student15, growing up in a rural location9,10, going to a smaller pre-medical college11, and having parents who did not attend college11. Few studies have focused specifically on osteopathic medical student characteristics predictive of rural intent. In addition, there are no studies correlating personality type based on MBTI to a medical student's intent for rural practice.
This study explored osteopathic student predictors of rural practice. This study also sought to assess the relationship between personality type and intent to practice in a rural setting. Identification of these relationships will assist osteopathic medical schools to effectively recruit future rural physicians based on documented relationships between demographic and family characteristics and their intent to practice in a rural area. Moreover, medical schools can provide career counseling sessions based on personality preferences and how personality preferences correspond to rural practice. It is imperative that medical schools understand characteristics and identifiers of medical students that predict intent to practice in a rural area to solicit applicants with these characteristics. Medical schools can influence medical student career choice in rural medicine by providing career planning sessions based on these results.
Research design
This was a correlational study using both cross-sectional and retrospective data. Cross-sectional data were collected via an electronic survey. Retrospective data were collected from MBTI assessments administered to students on a yearly basis as part of orientation to clinical clerkships. For the purposes of this study, 'rural' was defined as a community of less than 50 000 people in order to include all areas not defined as urbanized areas by the US Census Bureau20.
Participants
Eligible participants included 225 medical students at Pacific Northwest University of Health Sciences College of Osteopathic Medicine. There were approximately 75 students in each program year (second, third, and fourth). The student population was predominately White, ranging in age from 21 to 42 years, and equally divided between females and males. Approximately 70% of the student population was from the five-state Pacific Northwest Region (Alaska, Idaho, Montana, Oregon, and Washington). Participants were consented at a Friday afternoon didactic session and during the orientation to clinical clerkships by the primary investigator.
Data collection
The simple, one-section survey instrument (an approved, modified version for use in this study of a survey developed by Brian Whitacre of Oklahoma State University College of Osteopathic Medicine14) required 10-15 min to complete. Information on background characteristics and intent for rural practice was examined. Questions regarding medical school student opinions about factors important for considering rural practice and their opinions of physicians practicing in rural areas were also included. Additional demographic questions were based on previous research regarding factors related to physician practice-location choice13,21,22. The survey instrument was reviewed by three content experts.
The MBTI, developed by Isabel Myers and Katharine Briggs in 1942, is used to establish individual preferences and based on Carl Jung's theory of psychological types19. Personality types are made by a choice in each dichotomy resulting in 16 different personality types. Over time the instrument has been improved in the areas of: language, number of items, item format scoring method, sex differences and weighting18. The MBTI has been validated with exploratory factor analysis and confirmatory factor analyses18. The MBTI has been administered to over 2 million people, has been translated into 30 languages, and has been used in over 70 countries worldwide18.
Analysis
Three steps were involved in the analysis of the data; organizing, description, and testing the hypotheses23. Data were exported from the electronic survey instrument into a Microsoft Excel spreadsheet, where they were checked for accuracy and completeness. Data were then imported into in IBM SPSS Statistics v 19 (www.spss.com) for analysis. Data were described using frequencies, percentages, means, and standard deviations. Pearson's χ² test was used to determine which characteristics were significantly different between those with and without intent for rural practice. Factors significant in bivariate analysis were entered into a multiple logistic regression model predicting intent for rural practice. All α levels were set at 0.05, two-tailed.
Ethics approval
The research study was approved by the AT Still University Institutional Review Board (ATSU-#2011-32) and the Pacific Northwest University of Health Sciences Institutional Review Board (#2011-003).
A total of 141 students completed the survey giving a 63% response rate. Characteristics of respondents and comparisons by practice intent are summarized (Table 1). Response rates were higher for second and third year medical students (36.8% and 35.4%, respectively). This was expected, because the fourth-year medical students were on clinical rotations including electives that were outside the regional campus system. There was no significant difference in intent to practice rural medicine by age, sex or ethnicity. Intent for rural practice was significantly higher among students raised in rural communities, students whose parents lived in a rural area, and students whose father or mother had an educational level of a bachelor's degree or lower. Intent for rural practice was significantly greater among students whose spouse or significant other was raised in a rural area as well as among those whose spouse or significant other had parents who lived in a rural area.
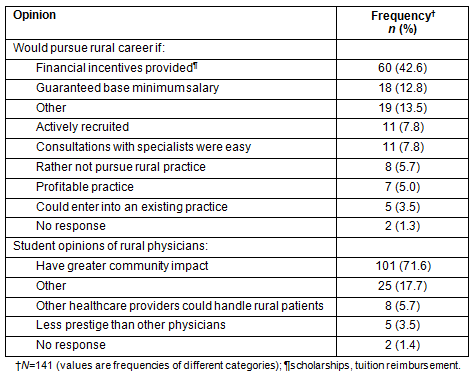
The MBTI results are summarized according to rural and non-rural intent (Table 2). There were significant differences between students with and without intent for rural practice in the Extraversion-Introversion dichotomy. Specifically, students with intent for rural practice had higher rates of Extraversion as opposed to Introversion compared with students without intent for rural practice. There was also a significant difference between students with and without intent for rural practice in the Judging-Perceiving dichotomy. Students with intent for rural practice had a higher rate for the Judging preference. Medical school students' opinions are summarized in relation to influences affecting their choice of rural practice and their opinion of physicians practicing in a rural area (Table 3). The majority of respondents indicated a desire for financial incentives or a base salary guarantee to pursue rural practice. Those who responded 'other' on the questions relating to influences affecting rural practice commented on the limited options for spouse's employment, lack of cultural activities in rural areas, issues of race and ethnicity, and limited educational opportunities in rural areas. On the subject of physicians practicing in rural areas, students indicated that physicians practicing in rural settings have a greater impact on the community than their urban counterparts.
Table 1: Characteristics of the sample
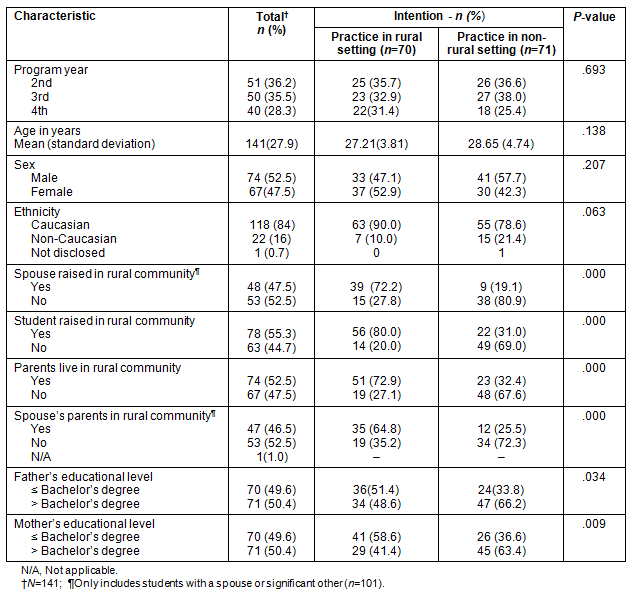
Table 2: Myers Briggs Type Indicator - personality type according to intent for rural practice
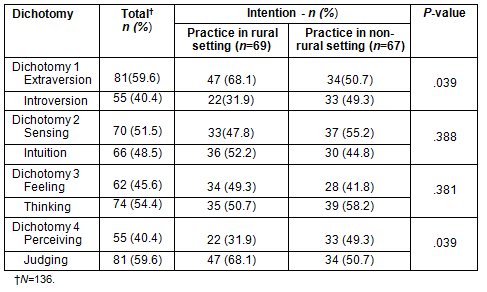
Table 3: Osteopathic medical students' opinions of rural practice
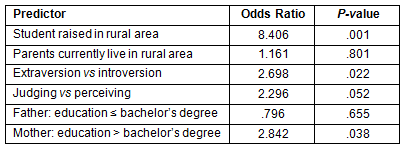
Factors significant in univariate analysis (Tables 1 & 2) were entered into a multiple logistic regression model to predict intent for rural practice. The results (Table 4) illustrate that the overall fit of the model was sound, with a pseudo R2 (Nagelkerke R2) of .289. There was a 75% correct prediction for both rural and non-rural practice intent. Students who were raised in rural areas as well as those whose mothers had a bachelor's degree or lower were more likely to have intent for rural practice. The results were also significant for students who preferred Extraversion (based on MBTI). Students who preferred Judging did not reach statistical significance at an α level of 0.05. However, the p-value was calculated at 0.052 indicating a strong relationship between rural practice and students who prefer Judging. A separate multiple logistic regression analysis was conducted for students in a relationship (N=101) to determine the effect of having a spouse or significant other who was raised in a rural area. This factor was significant (p<0.05) and positively related to intent for rural practice with an odds ratio of 8.87, while controlling for other factors.
Table 4: Multiple logistic regression analysis predicting intent for rural practice
Discussion
The purpose of this study was to determine if there are characteristics that predict medical students' intent to practice in rural communities and if there is a correlation between personality type and intent to practice in a rural setting.
The factor most often found to influence medical students' intent to practice in a rural area is having been raised in a rural area8-10,13. The current study supports past research, finding that rural upbringing is positively associated with intent for rural practice among osteopathic medical students. The odds ratio associated with rural upbringing was higher than has been reported in studies examining factors related to rural practice choice8. This is possibly due to the fact that the outcome measured in this study was intent rather than actual practice selection; rural upbringing may have a greater effect on intent than on final practice choice. Recruitment of students with a rural background is of utmost importance for medical schools desiring to produce physicians who will practice in rural locations. This recruitment strategy has been successful for many allopathic medical schools such as the University of Alabama, Jefferson Medical School in Pennsylvania, and Michigan State University Upper Peninsula Program2. These medical schools actively recruited undergraduate students who lived in a rural area. The recruitment of students with rural backgrounds may be difficult. There are a limited number of students from rural areas who are interested in becoming physicians, who achieve access to higher education, and who have strong enough academic performance to be admitted to medical school. Therefore, medical schools may want to create partnerships with high schools in rural communities offering pre-medical clubs. Current medical students from rural areas could serve as mentors. The use of web-based video conferencing could be used as the medium for these forms. Early mentoring of rural high school students could increase the pipeline of medical students from these areas, as mentoring programs of high school students has been proven to increase the likelihood of pursuing higher education24.
Studies have found that having a spouse with a rural background is a predictor of intent to practice in a rural setting9 and the findings of the current study were consistent with such research. Spouses' preference to live in communities of similar size to where they were raised has an influence on students' practice choice. Spouses from rural areas understand the social and cultural environment. This lends itself to adaptation and resilience in rural settings, which affects the family support system provided to the physician. The support system enhances physician wellbeing, an important factor in job performance25.
Although past studies have found that having parents who live in a rural area, age, ethnicity, being in a committed relationship, and the size of undergraduate college were predictive of rural practice, this study did not find these factors to be significant predictors of rural intent. Sample size, intent to practice rather than actual practice, new school, and differences in the variables collected and used may be reasons for this difference, Students in this study indicated that financial incentives are motivators for rural practice. Rising student debt has also been shown to affect decisions to avoid primary care and rural medicine6-8. Financial incentives may help students who have a large amount of debt choose rural practice. However, financial incentives may not be enough to retain physicians in rural areas. Further study should focus on the short- and long-term retention of physicians who received incentives to choose rural practice.
Students felt that physicians in rural communities have more impact on their community than their urban counterparts. Over 70% of students had this positive opinion of rural physicians. No student felt that rural physicians were less qualified than urban physicians. However, 3.5% of students felt that other healthcare professionals could provide care in rural areas. Students strongly suggested that physicians in rural areas become community leaders.
Students with intent to practice in a rural area were more likely to have mothers with a college education, a bachelor's degree or lower. This predictor was slightly different from past studies. Prior studies noted the relationship between rural intent and parent without a university education11. This difference may be due to small sample size. It could also be related to the type of students who were attracted to a new medical school.
Previous studies have explored MBTI personality type as it relates to medical students' choice of primary care and non-primary care specialties15-17. Studies using MBTI types found a correlation between personality type and medical specialty15. Feeling types were significantly more likely than Thinking types to choose primary care, family medicine, internal medicine and pediatrics. Introverts were significantly more likely than Extroverts to choose primary care15. The findings of this study revealed that respondents who preferred Extraversion as opposed to Introversion had higher odds of intent for rural practice. Extroverts are action oriented, open to new experiences, and have an ease of communication and sociability18. The Extrovert preference for the willingness to try new experiences supports the higher odds of Extroverts with intent for rural practice where the environment provides physicians to practice medicine utilizing the full scope of training due to lack of specialty trained physicians. This is demonstrated by rural family medicine physicians. While a preference for Judging as opposed to Perceiving was also associated with intent for rural practice, this association did not reach statistical significance (p=0.052) when other factors were controlled. These findings suggest that personality type may be important in demonstrating a correlation for rural practice. Future research is warranted to examine the effect of the Extraverted-Judging types, specifically on intent for rural practice. Extraverted-Judging types are suited to rural areas based on student opinions of the rural physicians being community leaders. They bring order and closure to what they do. Extraverted-Judging types are leaders; they tend to be fast moving, decisive, and are able to change directions with compelling new data19. Medical schools may be able to influence career location choices by providing career planning sessions utilizing MBTI. Career counseling sessions discuss opportunities and challenges for medical students in the context of practice locations, such as rural practice, based on their type26.
Limitations
This study was limited to one osteopathic college with a mission of providing physicians to rural areas. Therefore, the students may have been more likely to choose rural practice than students from other schools. The school was new, which may have attracted students with similar personal and family characteristics. In addition, a new school may have a limited applicant pool compared with a more established medical school. The curriculum of the medical school was focused on student rotations in rural and underserved areas which also may have biased the sample. The response rate, although adequate, was based on a small population. Additionally, this study measured students' intent to practice in a rural area, not their actual practice choice. Intent was measured prior to residency, so students were at least 4 years from a practice decision. Therefore, longitudinal data collection would assist to further as certain factors that affect medical practice choice.
This study examined and supported the hypothesis that certain characteristics affect medical school students' intent to practice in a rural area. Medical schools that recruit and select students who spent their childhood in a rural community may increase the provision of physicians to rural areas. Spouses and significant others of medical students impact career decisions related to practice location. Spouses and significant others who were raised in a rural area may influence a medical student's decision to practice in a rural setting. Furthermore, the educational level of a student's parents may impact the decision to practice in rural setting. In order to provide physicians to rural areas, medical school recruitment efforts should focus on students who display the characteristics that indicate intent for rural practice. Financial incentives and wage guarantee programs may motivate students to consider practicing in a rural area.
Finally, this study suggests that MBTI may be a useful tool in understanding aspects of personality and how personality relates to intent to practice in a rural setting. Career counseling that includes MBTI may be a useful method of promoting rural practice as students consider practice decisions.
References
1. American Association of Colleges of Osteopathic Medicine. General admission requirements. (Online) 2012. Available: http://www.aacom.org/InfoFor/applicants/becoming/Pages/AdmissionReq.aspx (Accessed 5 February 2012).
2. Rabinowitz H, Diamond J, Markham F. Medical school programs increase the rural physician supply: a systematic review and projected impact of widespread replication. Academic Medicine 2008; 83(3): 235-243.
3. Institute of Medicine. Quality through collaboration. Washington, DC: National Academic Press, 2005.
4. Bowman R. They really do go. Rural and Remote Health 8:1035. (Online) 2008. Available: www.rrh.org.au (Accessed 20 December 2010).
5. Miller T, Hooker R, Mains D. Characteristics of osteopathic physicians choosing to practice rural primary care. Journal American Osteopathic Association 2006; 106(5): 274-279.
6. Xu G. Debt and primary care physicians' career satisfaction. Academic Medicine 1998; 73: 11.
7. Hadley J, Cantor J, Willke R, Feder J, Cohen A. Young physicians most and least likely to have second thoughts about a career in medicine. Academic Medicine 1992; 67: 180-190.
8. Steinwald B, Steinwald C. The effects of preceptorship and rural training programs on physicians' practice location decisions. Medical Care 1975; 13(3): 219-229.
9. Leonardson G, LaPierre R, Hollingsworth D. Factors predictive of physician location. Journal Medical Education 1985; 60: 37-43.
10. Feldman K, Woloschuk W, Gowans M, Delva D, Brenneis F, Wright B et al. The difference between medical students interested in rural family medicine versus urban family or specialty medicine. Canadian Journal Rural Medicine 2008; 13(2): 73-79.
11. Wheat J, Brandon J, Carter L, Leeper J, Jackson J. Premedical education: the contribution of local colleges. Journal of Rural Health 2003; 19(2): 181-189.
12. Daniels Z, VanLeit B, Skipper B, Sanders M, Rhyne R. Factors in recruiting and retaining health professionals for rural practice. National Rural Health Association 2007; 23(1): 62-71.
13. Easterbrook M, Godwin M, Wilson R, Hodgetts G, Brown G, Pong R et al. Rural background and clinical rural rotations during medical training: effect on practice location. Canadian Medical Association 1999; 160(8): 1159-1163.
14. Colegrove D, Whitacre B. Interest in rural medicine among osteopathic residents and medical students. Rural and Remote Health 9:1192. (Online) 2008. Available: www.rrh.org.au (Accessed 20 December 2010).
15. Stilwell N, WallickM, Thal S, Burleson J. Myers Briggs type and medical specialty choice: a new look at an old question. Teaching and Learning in Medicine 2000; 12(1): 14-20.
16. Neral S, Collings J, Gandy M, Hampton H, Morrison J. Non-cognitive variables and residency choice. Journal Mississippi State Medical Association 2008; 49: 327-329.
17. Wallick M, Cambre K, Randall H. (1999). Personality type and medical specialty choice. Journal Louisiana Medical Society. Journal of the Louisiana State Medical Society 1999; 151: 463-469.
18. Myers I, McCaulley M, Quenk N, Hammer A. MBTI manual: a guide to the development and use of Myers-Briggs Type Indicator, 3rd edn. Mountain View, CA: CPP, 2009.
19. Keirsey D, Bates M. Please understand me: character and temperament types. Del Mar, CA: Prometheus Nemesis, 1984.
20. US. Census Bureau. Urban and rural classification. (Online) 2010. Available: http://www.census.gov/geo/www/ua/urbanruralclass.html (Accessed 10 June 2011).
21. Chan B, Degnai N, Critchton T, Pong R, Rourke J, James G et al. Factors influencing family physicians to enter rural practice: does rural or urban background made a difference? Canadian Family Physicians 2005; 51(9): 1247-1251.
22. Stagg P, Greenhill JW. A new model to understand the career choice and practice location decisions of medical graduates. Rural and Remote Health 9: 1245. (Online) 2009. Available: www.rrh.org.au (Accessed 20 December 2010).
23. Portney L, Watkins M. Foundations of clinical research. Upper Saddle River, NJ: Prentice Hall, 2000.
24. McCargo D. Improving the mentoring experience for pre-college program participants through organizational change and leadership. ERIC, Ipswich, MA: ProQuest LLC; 2011.
25. Ratanawongsa N, Wright S, Carrese J. Well-being in residency: effects on relationships with patients, interactions with colleagues, performance, and motivation. Patient Education &Counseling 2008; 72(2): 194-200.
26. Lawrence G, Martin C. Building people, building programs. Gainesville, FL: CAPT, 2001.

