Aboriginal peoples is a collective name for the original peoples of North America and their descendents. Over the last few decades, rapid cultural change has occurred in many Aboriginal populations affecting their dietary patterns; transitioning from locally harvested traditional foods to a diet of primarily market food purchased from stores1,2. In particular, Aboriginal youth have departed greatly from traditional food consumption patterns1. Traditional foods such as game meat, fish, berries and plant foods have been replaced by processed foods, high fat meals, and added sugars; especially in Aboriginal adolescents3-6. Numerous studies have reported low consumption of vegetables and fruit and dairy products by Aboriginal children3,7-9. Nutrient inadequacies in Aboriginal children and adolescents from certain communities have been documented for iron, folate, vitamin D, calcium and vitamin A6,7,10.
Recent studies have found associations between overall diet quality and academic performance11, and a systematic review found that school breakfast programs can have positive effects on academic performance12. Schools are an ideal setting for promoting healthy eating due to the number of weekday hours that students spend there and the opportunity to teach children and youth about healthy foods and eating behaviours. Eating habits start during childhood and can be influenced by a healthy school food environment. School breakfast and snack programs can provide nutritionally balanced, free meals to students each school day. This is especially important in remote northern communities where many households are food insecure2,13,14; fresh produce and other nutritious perishable foods are inconsistently available and can be extremely expensive15,16. School snack and breakfast programs have been suggested as viable actions to combat food insecurity in Aboriginal populations17-22.
Aboriginal peoples in Canada refers to three groups: Indian (commonly referred to as First Nations), Métis, and Inuit. Nearly two-thirds of the Aboriginal population in Canada identify themselves as First Nations people and there are more than 600 First Nation communities. An environmental scan of nutrition programs in First Nations schools in Canada found that more than 85% of the 303 schools surveyed reported having a school nutrition program and 75% of those schools offered their program daily17. Despite the large number of nutrition programs existing in Canadian First Nations schools, there are few publications in the academic literature that report on school meal programs (breakfast, lunch, and/or snack) in these communities23,24. These programs have contributed substantially to calcium, dietary fiber, vitamin A, vitamin C, and vitamin D in students18,19,23,24.
The current study examined the impact of an existing school snack program on the dietary intakes of grade six to ten First Nation students living in the remote sub-arctic community of Fort Albany, Ontario. The main objective was to examine the dietary intakes of students participating in the snack program compared with those who did not participate, using a validated web-based survey called the Waterloo Web-based Eating Behaviour Questionnaire (WEB-Q). Two data collections were conducted in separate years, 2004 and 2007. Given that fewer than half of students reported participating in the school snack program on the days of the 2004 data collection, the repeat evaluation in 2007 incorporated questions to assess the habitual participation in the program and obtain feedback on perceived program strengths and suggestions for improvement.
Participants
Participants in this study were students in grades six to ten at Peetabeck Academy in Fort Albany, Ontario. Fort Albany is situated on the west coast of James Bay along the Albany River and houses the community of Fort Albany First Nation which is home to approximately 850 Cree people. Fort Albany is remote and isolated as it is accessible only by plane year round. The community is connected with other James Bay coastal communities by boat and barge during the ice-free season and by a snow/ice road after freeze-up. Peetabeck Academy serves Fort Albany First Nation students from kindergarten to grade 12. The school snack program has been provided to students in Fort Albany for more than 15 years. At the time of this study, the snack program at Peetabeck Academy provided a morning snack to all students and an afternoon snack to all elementary (kindergarten to grade 8) students each school day. Morning snacks were usually breakfast type foods such as cereal with milk or whole wheat toast with a spread (cheese or jam) and fruit juice, while afternoon snacks usually consisted of cut up fruit and fruit juice or milk to drink. Boiled eggs, yogurt, or homemade muffins were usually offered once a week when there were more volunteers to assist with snack preparation and distribution. Vegetables were offered occasionally when time and availability allowed. Traditional foods, such as bannock and game meats, were sometimes offered during special events.
Data collections
For this study, two separate data collections in 2004 and 2007 were used to assess the impact of the school nutrition program. Because time and availability of computer terminals did not permit single-day data collections, the data were collected in each year over the course of 2 days. The WEB-Q was conducted in Fort Albany in November 2004 with 63 grade six to ten students (Data Collection #1). The two day data collection took place with grade six and seven students completing the WEB-Q on 11 November and grade eight, nine, and ten students completing the WEB-Q on 12 November. In December 2007 data were collected with grade six and seven students on 12 December and grade eight, nine, and ten students on 13 December with 50 students (Data Collection #2). All 24 hour recall dietary data were collected to reflect weekday consumption (ie the impact of the school snack program), as the data were collected from Tuesday to Friday.
Web-based survey
The WEB-Q is a validated web-based survey tool developed at the University of Waterloo to assess food and physical activity behaviors of children and adolescents25-39. The survey includes a 24 hour dietary recall which asks students about what types of food and how much of those foods they consumed on the previous day.
The WEB-Q simulates a dietitian interview and includes prompts for missed food items, pictures and comparisons to common objects to aid in portion size estimation, as well as immediate feedback for students to compare their individual food intake to recommendations.
The WEB-Q has been used to collect nutrition and physical activity information from over 15 000 non-Aboriginal students in Canada and over 500 First Nation students in Ontario and Quebec. The WEB-Q was adapted for First Nation students through previous quantitative and qualitative research which included input through a local community advisory committees from a number of First Nations communities in southern Ontario, northern Ontario, and northern Quebec. The survey underwent some adaptation for each community; such as, adding questions related to school breakfast and snack programs (as applicable to each community), questions regarding traditional food intake, factors influencing traditional food intake, and questions to assist local planning. Specific to this study, adaptations relevant to Fort Albany and suggested by the community advisory committee were made to the WEB-Q. The primary adaptation involved the addition of traditional Aboriginal foods to the list of approximately 900 possible food choices in the 24 hour dietary recall.
Following adaptations, validity testing of the WEB-Q was conducted with First Nations students. Dietitian-administered interviews were conducted with twenty-five Fort Albany students during a data collection in 2004 and compared with the web-survey that had first been completed for the same 24 hour recall period. Food models from the Ontario Food Survey assisted with portion estimation during dietitian interviews. The results for Fort Albany (n=25) showed that there was good agreement for energy and key nutrient intakes (intraclass correlation coefficients for calories, carbohydrates, protein, iron, vitamin C, and fibre >0.67, n=25, grades six to ten) from the web-based survey versus dietitian administered interviews27.
The WEB-Q asked 'At which times did you eat anything yesterday?' Students were to indicate all options that applied to them: breakfast, middle of the morning snack, lunch, middle of the afternoon snack, after school snack, dinner, early evening snack, later evening snack, school snack/breakfast program. This question was used to capture whether students had participated in the school nutrition program on the previous day. Based on input from the director of the program and questions used by FAVES - an evaluation survey of a school fruit and vegetable snack intervention conducted in London, Ontario40, five questions were added to the WEB-Q and asked during the second data collection with grade six to ten students in Fort Albany in December of 2007. The five additional questions on the WEB-Q related to the Fort Albany school nutrition program were as follows:
- How often do you participate in the school snack/breakfast program? (Response options: Every school day, More than half of the week [3 or more days each week], Less than half of the week [2 or fewer days each week], Rarely or never, Not answered)
- What do you like most about the school snack program? (Check all that apply: I get a snack at school every day; It helps me to focus in class; It keeps me from feeling hungry at school; Juice; Eggs; Cereal or toast; Cut up fruit)
- Is there a different vegetable or fruit you would like to get as a snack at school? (Open-ended)
- If you could change one thing about the snack program, what would it be? (Open-ended)
- Because of the school snack program... (Agree, disagree, not answered: I am motivated to eat healthier; I make better choices about what I eat; I eat more vegetables; I eat more fruit; I have asked my parents to buy or serve vegetables or fruits I try at school).
Participant recruitment, consent, and data collection
Parental passive consent/information letters were sent home with students one week before each scheduled data collection, as passive consent is culturally appropriate in this community. In addition, students had to provide active consent on the first page of the WEB-Q, by selecting the checkmark on the screen to participate or the 'X', to decline participation in the study. The lead author or her colleagues supervised students while they completed the WEB-Q and answered any questions the students had about the survey. Each student was assigned a unique login and password which ensured anonymity and confidentiality. The surveys were completed during class time using computers with internet access in the computer room at Peetabeck Academy. This study used a convenience sample of all consenting students who were in attendance on the days of each data collection; the participation rate was 100% because all students in attendance participated.
Data analysis
From the WEB-Q data, food group consumption and nutrient intake (from the 24 hour dietary recall) of students participating in the school snack program on the previous day were compared with students who did not participate for 2004 and 2007, respectively. Descriptive statistics (means, standard deviations, frequencies, percentages) were calculated. For both the food-group and nutrient datasets, multivariate analysis of variance (M)ANOVA was used to assess differences between groups (snack program participants and non-participants), and by gender and grade. Owing to the small sample size, grades were categorized into two groups with elementary students in grades six, seven, and eight versus high school students in grades nine and ten. Differences in grade were assessed because an afternoon snack was not offered to high school students (grades 9 and 10) and from past research indicating that older students tend to eat differently from younger students. Individual participant intakes were compared with current Canadian dietary recommendations for food groups and nutrients with an Estimated Average Requirement (EAR) value to determine the percentage of participants that were not meeting recommendations. The EAR has been used in dietary studies to describe the population prevalence of inadequate intakes. Data were analyzed using SPSS statistical software v18 (www.spss.com). Statistical tests were considered significant with p-values <0.05.
From the December 2007 data, analyses for the questions: 'How often do you participate in the school snack/breakfast program?', 'What do you like most about the school snack program?' and 'Because of the school snack program...' consists of frequencies and results are presented as descriptive characteristics. Frequencies from these questions were compared by gender. For the open-ended school nutrition program questions ('Is there a different vegetable or fruit you would like to get as a snack at school?' and 'If you could change one thing about the snack program, what would it be?'), responses were grouped according to common themes and ordered according to the most common theme (or response) versus the least common theme (or response).
Ethics approval
Permission to conduct this study was obtained from Fort Albany First Nation (the locally elected government), Mundo Peetabeck Education Authority (the local First Nation administered school board), and the Office of Research Ethics at the University of Waterloo (#14081).
Characteristics of the study population for the two data collections are shown (Table 1). The morning and afternoon snacks that were provided to students on the days prior to the data collection, which are the days reported in the 24 hour dietary recall of the WEB-Q, are listed by grade (Table 2). This is a typical example of the snacks that are offered in the school program each day.
Overall for Data Collection #1, the majority of students did not meet current dietary recommendations for almost half of the food groups and nutrients that were examined (Table 3). More than three-quarters of the students did not meet recommendations for 'Milk and Alternatives', calcium, and vitamin D. With the exception of 'Meat and Alternatives', there was a trend for a higher percentage of students to meet dietary recommendations if they participated in the snack program. The majority of snack program participants met recommendations for eight of the 12 food group/nutrient variables; whereas, the majority of non-participants only met five recommendations. For the 'Vegetables and Fruit' food group and folate, the percentage of non-participants failing to meet recommendations was more than double the percentage of snack participants (78% vs 35% and 60% vs 30%, respectively).
Similarly, Data Collection #2 showed that the majority of students were not meeting current dietary recommendations (Table 3) and more students tended to meet recommendations if they participated in the school nutrition program.
For Data Collection #1, students participating in the snack program (37%; n=23) had significantly higher (p<0.05) intakes for six of the 12 variables examined than those who did not participate (63%; n=40). For example, participants in the snack program had higher mean intakes of servings from the Vegetables and Fruit category (7.5 vs 3.4 servings) than non-participants. Mean values and differences in food group and nutrient intakes between participants and non-participants are shown (Table 4). Differences in intake also occurred by gender for Meat and Alternatives, calcium, and iron, by gender and grade for 'Other' Foods, vitamin A and dietary fiber, and by grade only for folate and vitamin C.
Table 1: Characteristics of study population according to data collection
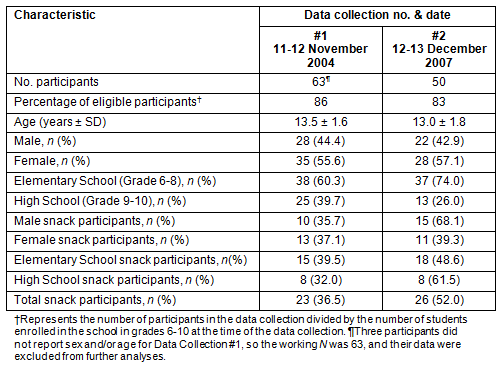 Table 2: Morning and afternoon snacks provided prior to data collection
Table 2: Morning and afternoon snacks provided prior to data collection
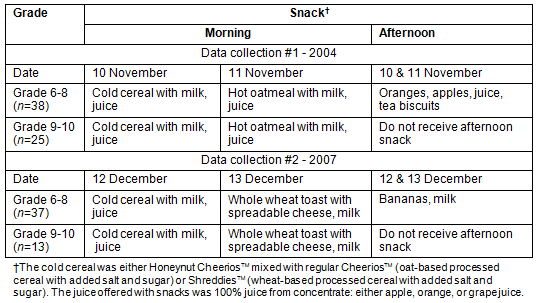 Table 3: Percentage of children not meeting dietary recommendations by snack participation and sex (N = 116)41,42
Table 3: Percentage of children not meeting dietary recommendations by snack participation and sex (N = 116)41,42
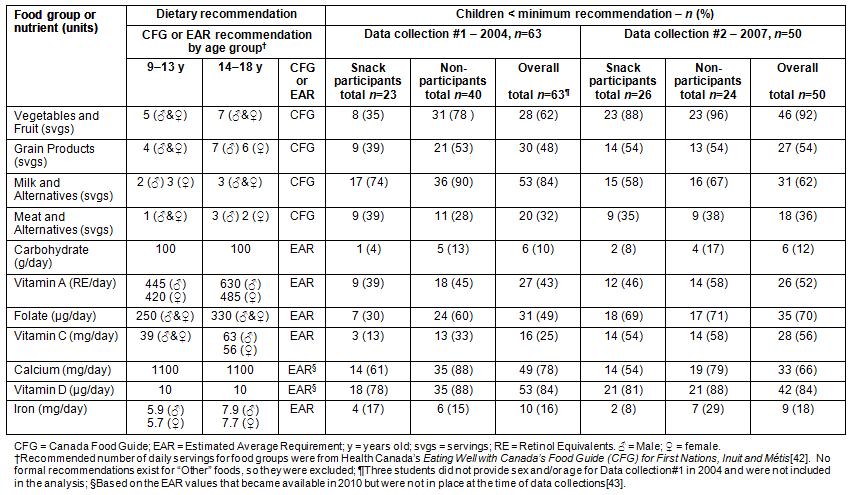 Table 4: Differences in food group and nutrient intakes between snack program participants and non-participants41
Table 4: Differences in food group and nutrient intakes between snack program participants and non-participants41
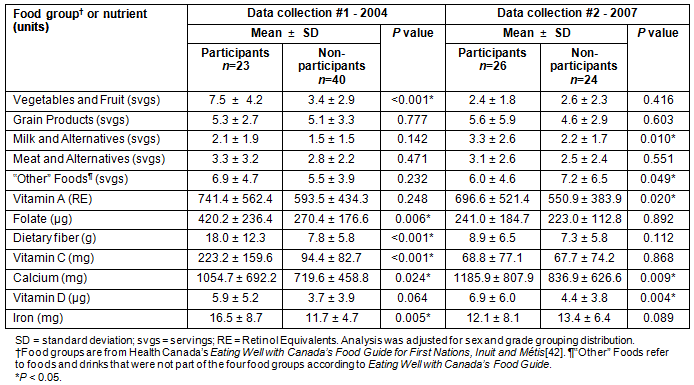
For Data Collection #2, students participating in the snack program (52%; n=26) had significantly higher intakes for five of the 12 variables examined than those who did not participate (48%; n=24) and with the exception of calcium, differed from the food groups and nutrients that were significant from the analysis for Data Collection #1. For example, participants in the snack program had higher mean intakes of servings from the Milk and Alternatives food group (3.3 vs 2.2 servings) as well as vitamin A (697 vs 551 RE [retinol equivalents]) and vitamin D (6.9 vs 4.4 µg) than non-participants. Vitamins A and D are nutrients that are added to most of the fluid milk sold in Canada. For Data Collection #2, differences in intake occurred by gender for nearly all the food groups and nutrients with the exception of Vegetables and Fruit, 'Grain Products', and vitamin C. Differences in food group intake are shown by sex for snack program participants and non-participants in 2007 (Fig1). There were differences by grade for Other foods, vitamin A, calcium, and vitamin D.
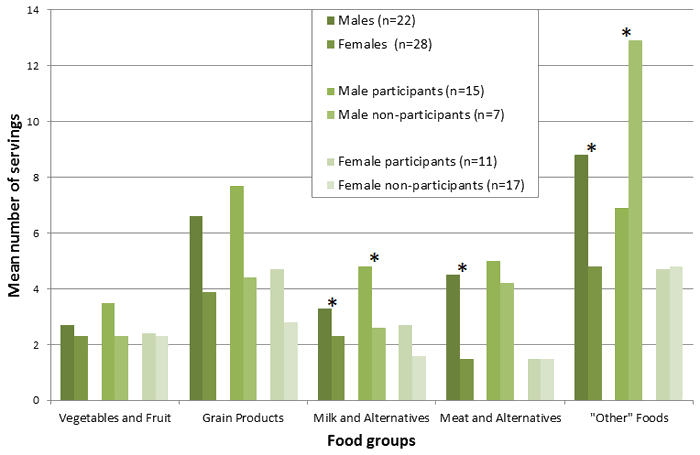 Figure 1: Differences in food group intake by sex between snack program participants and
Figure 1: Differences in food group intake by sex between snack program participants and
non-participants in 2007 (N=50). *Significant differences between paired columns, p<0.05.
For both data collections boys generally had higher intakes from all food groups and nutrients than girls. High school students generally had higher intakes from all food groups and nutrients than elementary students. There were no significant (p ≥ 0.05) interaction effects between snack participation and gender or snack participation and grade for either of the two data collections.
Despite only half of students participating in the snack program on the day of the second data collection, 78% students reported that they usually participate in the school snack and breakfast program more than half of the week or every day (Fig2).
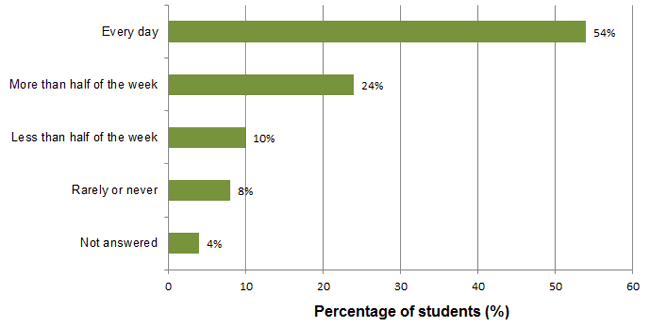 Figure 2: How often students reported participating in the snack program in 2007 (N = 50).
Figure 2: How often students reported participating in the snack program in 2007 (N = 50).
Students were asked to check 'all that apply' when asked, 'What do you like most about the school snack program?'. However, the majority of students (33 of 50, 66%) only chose one response option. Students indicated that the three things they liked most about the school snack program were the juice (50%), that the program kept them from feeling hungry at school (40%), and that they got a snack at school every day (32%).
Students were asked, 'Is there are different vegetable or fruit you would like to get as a snack at school?' This was an open-ended question, so students could choose whatever vegetables or fruit that they wanted. Many students suggested more than one vegetable and/or fruit. Of the 46 students who responded to this question, the six most common responses were grapes (n=8), bananas (n=6), apples (n=6), juice (n=6), kiwifruit (n=5), and strawberries (n=5). Apples and juice were already regularly served to students from the snack program as they were easier to transport into the community. Bananas were served occasionally, grapes and strawberries rarely and often only for very special events. At this time, kiwifruit had never been served at school.
When students were asked what they would change about the program, only 64% (n=32) of the students submitted a response. The most common response (n=16, 50%) was that they would change nothing about the program or that they didn't know what they would change. The next most common response was that students wanted more fruit (n=6, 19%). Other program changes suggested were that students could help out more in the kitchen and that they wanted to eat their snack in the cafeteria instead of in the classroom. A few students wanted to also have a lunch program offered at school.
Students indicated that the snack program helped them to eat healthier by motivating them (74%), eating more fruit (86%), and making better dietary choices (68%) (Fig3). However, the majority (50%) did not think that the snack program encouraged them to ask their parents to purchase vegetables or fruit that they had tried at school. For this question, students could choose all responses that applied to them.
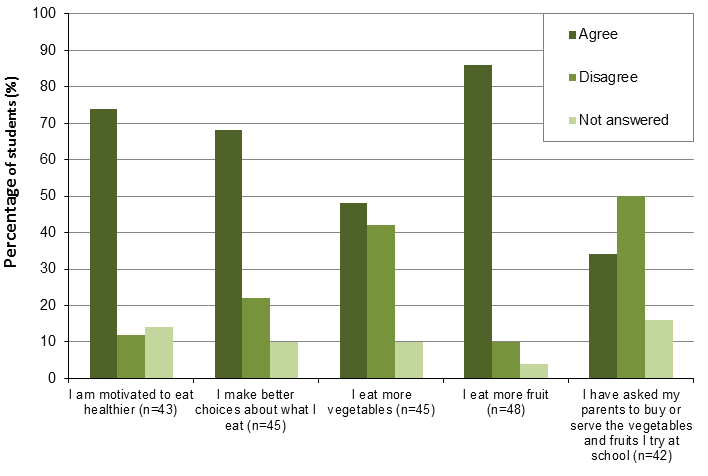 Figure 3: Student responses to 'Because of the school snack program...'
Figure 3: Student responses to 'Because of the school snack program...'
Discussion
The findings from this study suggest that the school snack program at Peetabeck Academy in Fort Albany is having a positive impact on the dietary intake of grade six to ten students. Although the long-term effects of the school snack program were not examined, the fact that the program has been providing healthy food for students for more than a decade and the findings from the WEB-Q showing improved nutritional benefits to students shows that the program is likely to be very important with respect to increasing food security for children and adolescents in Fort Albany.
Similar to other studies of school nutrition programs in Canadian Aboriginal children, the snack program in Fort Albany helped to improve the dietary intake of fiber18,23, and vitamin C18 in 2004, calcium19,24 in 2004 and 2007, and vitamin A24 and vitamin D19,24 in 2007. Gates et al found that the impact of their snack programs in First Nations were only maintained over the short-term and not sustained at one year follow-up18,19. It is important to note that their projects were pilot intervention programs that had not existed prior to their studies. The sustainability of their programs were hindered by a lack of funding and personnel resources over the long term. In contrast, the snack program in Fort Albany has become institutionalized in the community and the school and has been sustained and gradually improved over the course of many years. In the past few years, the program in Fort Albany has been expanded further to include an extensive and daily offering of breakfast with various breakfast food options for all high school students. The success of the school nutrition program in Fort Albany has been attributed to the dedication of a 'program champion' throughout the program's history20, adequate food preparation and storage facilities, continuous financial resources20, and widespread community support43,44.
As in other studies of Aboriginal children, Vegetables and Fruit consumption for the majority of students was below guidelines3,9,18,45. It is promising that participants in the 2004 snack program in Fort Albany had significantly higher intakes of Vegetables and Fruit and more than double the percentage of snack participants met Vegetable and Fruit recommendations compared with non-participants. In a population where the majority of children and youth do not meet dietary recommendations for many food groups and nutrients, the snack program appears to make an important contribution to meeting national nutritional guidelines. It is important to note that the EAR values are expected to satisfy the needs of only 50% of the people in that age group based on a review of the scientific literature, whereas the Recommended Dietary Allowance (RDA), a higher value, is the daily dietary intake level of a nutrient considered sufficient to meet the requirements of nearly all (97-98%) healthy individuals in each life-stage and gender group. The RDA is calculated by adding 2 standard deviations to the EAR values46. Therefore, despite improvements in dietary intakes for participants of the snack program, intakes of important nutrients were still very low. It also is important to point out that although oranges and apples were offered during the afternoon snack in 2004, the majority of the 7.7 servings of Vegetables and Fruit for snack program participants came from the consumption of fruit juice. The majority of students also reported that the juice was what they liked most about the snack program. The Canada Food Guide suggests that people have vegetables and fruit more often than juice, as they have more fiber and are more nutrient dense than fruit juice41. Also recommended by the Canada Food Guide is to eat one dark green and one orange vegetable each day; a recommendation not met by the Fort Albany snack program. The program does not regularly offer vegetables, as they are extremely expensive and can be more difficult to transport, store, and prepare. Wein et al conducted a study of food preferences for traditional and store-bought foods with Aboriginal and non-Aboriginal school children in northern Alberta and suggested that nutrition programs for Aboriginal communities should use a variety of preferred foods as a means for achieving a more nutritious diet. Most students in the study indicated that they did not think the program required any changes, although there were a few types of fruit that they would like to receive more often47. Because the students in Fort Albany were keen to have grapes, kiwifruit and strawberries - three fruits that were rarely or never provided - offered by their snack program, it may be important to attempt to present these fruits more frequently. Acknowledging that these specific fruits are more expensive than other fruit, difficult to transport, and to store, it would be beneficial for the school to conduct a future survey with students of the vegetables and fruit that they like. The results of this survey could contribute valuable information about how the snack program could be improved to combine student food preferences with more of the Canada Food Guide recommendations.
Interestingly, the study by Wein et al found higher mean preference scores by Native children for milk than soft drinks, with apples, chicken and milk receiving the highest preference scores for store-bought food47. Despite the preference for drinking milk, many of the mothers participating in their study mentioned being unable to afford milk in large enough quantities to supply their families for more than one or 2 days a week. Milk or a milk alternative (cheese spread) was offered by the program during both morning and afternoon snacks during the 2007 data collection. Findings from the second data collection in this study, with significantly higher Milk and Alternatives, calcium, vitamin A, and vitamin D intakes in snack program participants than non-participants, indicate that the actual content of the snacks provided were having an impact on student consumption. The cost of a 4 L bag of milk in January of 2007 at the grocery store in Fort Albany was $12.19 compared with $4.49 at the same time point in southern Ontario (unpubl. data; the southern Ontario price was an average price from 3 grocery stores in one city). Many studies of Canadian Aboriginal children have reported very low intakes from the Milk and Alternatives food group as well as low intakes of related nutrients such as calcium and vitamin D3,7,9,19,44,48. Milk insecurity, a phenomenon described by Williams et al49 as a lack of access to affordable milk for families, is probably a very common issue for northern First Nations households. The ability to offer milk and milk products to First Nations children and adolescents through a school nutrition program may be an important contributor to healthy dietary intakes in this population.
In this study, only single 24 hour dietary recalls were used and limitations of this method include recall error, inaccurate estimation of portion sizes, underreporting of foods, and the inability to capture a complete picture of usual dietary intake. However, the WEB-Q has incorporated several techniques to minimize the weaknesses of this form of assessment. For each selected food, the student could choose an estimate of the serving size, which was aided by pictures of portion sizes and comparisons to common objects. Prompts were used throughout the dietary recall to capture missed questions and forgotten foods, drinks, and toppings. Visual and hands-on tasks are culturally appropriate and appealing for First Nations students50-58. There was also improved reporting of sensitive information, (eg 'junk' food [food of little nutritional value] intake and body weights) during the WEB-Q validation study, compared with dietitian interviews27. Wein states that dietary recalls are much better suited to the survey needs of Aboriginal communities in comparison to dietary records because they are less labour intensive for the respondent59. Although multiple 24 hour recalls can better capture typical dietary intakes, the concern for respondent burden in participating children was taken into account and several studies of nutrition in Aboriginal children have successfully used a single 24 hour recall approach3,6,8,23,60-62.
It is surprising that only 37% of students reported participating in the snack program during the first data collection in 2004. It is possible that some students were absent from school on the previous day, and therefore would not have participated in the program. For the second data collection in 2007, more than half of grade six to ten students participated in the program. The difference in participation between 2004 and 2007 may be a result of better school attendance in 2007, as well as small improvements made to the snack program itself over time. There was an increase in financial resources applied to the program in 2007 which enabled the program to have a wider variety of foods offered, as well as more program equipment such as bowls and beverage cups. The director of the snack program has been constantly looking for ways to improve the program and to meet the needs and wants of the students. Responses from the additional questions in 2007 supported benefits from the program and offered few suggestions for improvement.
In a study by Gates et al conducted in a nearby First Nation18, the question 'Because of the school snack program...' was also asked. Results were similar, where 64% of students reported being motivated to eat healthier, 67% reported making better choices about what they ate, and 81% reported eating more fruit, compared with the findings of this study at 74%, 68%, and 86%, respectively18. A comprehensive school nutrition program, including nutrition education curriculum63, was implemented over a five week period in Fort Albany in the spring of 201064. This program was shown to improve knowledge, exposure to, and preferences for, vegetables and fruit, but did not impact intentions or self-efficacy towards these foods. Despite the positive impression of the program by teachers, parents, and students, it was acknowledged that the affordability, accessibility, and availability of vegetables and fruit remained a barrier to increasing consumption in Fort Albany64. While the snack program can help to alleviate some of the barriers to food security for children and adolescents in Fort Albany, improved food security policies and programs and support for local community initiatives remain necessary.
Given the positive impact of the program on the food and nutrient intake of school snack program participants, qualitative feedback will be used to enhance the program. The results of this study encourage the initiation, support, and continuation of similar healthy school breakfast and snack programs in other remote, northern communities. Clearly, school snack programs can be an important venue to address the nutritional vulnerability of First Nation youth living in remote communities.
Acknowledgements
The lead author was supported by a Doctoral Research Award from the Canadian Institutes of Health Research. This study was funded by the Canadian Institutes of Health Research, the Danone Institute of Canada, the Indigenous Health Research Development Program, and the Ontario Ministry of Research and Innovation. The authors are grateful to all the children that participated, and for the support of Peetabeck Academy, Mundo Peetabeck Education Authority, and Fort Albany First Nation.
References
1. Kuhnlein HV, Receveur O, Soueida R, Egeland GM. Arctic Indigenous Peoples experience the nutrition transition with changing dietary patterns and obesity. Journal of Nutrition 2004; 134: 1447-1453.
2. Egeland GM, Johnson-Down L, Cao ZR, Sheikh N, Weiler H. Food insecurity and nutrition transition combine to affect nutrient intakes in Canadian Arctic communities. Journal of Nutrition 2011; 141(9): 1746-1753.
3. Khalil CB, Johnson-Down L, Egeland GM. Emerging obesity and dietary habits among James Bay Cree youth. Public Health Nutrition 2010; 13: 1829-1837.
4. Assembly of First Nations. First Nations regional longitudinal Health Survey (RHS) 2002/2003, 2nd edn. Ottawa, ON: First Nations Information Governance Committee. (Online) 2007. Available: http://fnigc.ca/sites/default/files/ENpdf/RHS_2002/rhs2002-03-the_peoples_report_afn.pdf (Accessed 2 November 2011).
5. Szathmary EJ, Ritenbaugh C, Goodby CS. Dietary change and plasma glucose levels in an Amerindian population undergoing cultural transition. Social Science and Medicine 1987; 24: 791-804.
6. Wolever TMS, Hamad S, Gittelsohn J, Hanley JG, Logan A, Harris SB, et al. Nutrient intake and use in an Ojibwa-Cree community in Northern Ontario assessed by 24H dietary recall. Nutrition Research 1997; 17: 603-618.
7. Downs SM, Arnold A, Marshall D, McCargar LJ, Raine KD, Willows ND. Associations among the food environment, diet quality and weight status in Cree children in Quebec. Public Health Nutrition 2009; 12(9): 1504-1511.
8. Ng C, Young TK, Corey PN. Associations of television viewing, physical activity, and dietary behaviors with obesity in aboriginal and non-aboriginal Canadian youth. Public Health Nutrition 2010; 13(9): 1430-1437.
9. Taylor JP, Timmons V, Larsen R, Walton F, Bryanton, J, Critchley K et al. Nutritional concerns in Aboriginal children are similar to those in non-Aboriginal children in Prince Edward Island, Canada. Journal of the American Dietetic Association 2007; 107: 951-955.
10. Moffatt MEK. Current status of nutritional deficiencies in Canadian Aboriginal people. Canadian Journal of Physiology and Pharmacology 1995; 73: 754-758.
11. Florence MD, Asbridge M. Veugelers PJ. Diet quality and academic Performance. Journal of School Health 2008; 78(4): 209-215.
12. Hoyland A, Dye L, Lawton CL. A systematic review of the effect of breakfast on the cognitive performance of children and adolescents. Nutrition Research Reviews 2009; 22(2): 220-243.
13. Power E. Food security for First Nations and Inuit in Canada background paper. Ottawa, ON: First Nations and Inuit Health Branch, Health Canada, 2007.
14. Power E. Conceptualizing food security for Aboriginal people in Canada. Canadian Journal of Public Health 2008; 99(2): 95-97.
15. Willows ND. Determinants of healthy eating in Aboriginal people in Canada. Canadian Journal of Public Health 2005; 96(S3): S32-36.
16. Wein EE. The high cost of a nutritionally adequate diet in four Yukon communities. Canadian Journal of Public Health 1994; 85(5): 310-312.
17. Assembly of First Nations. An environmental scan of nutrition programs and policies in First Nations schools. Ottawa, ON: Assembly of First Nations, 2008.
18. Gates A, Hanning RM, Gates M, McCarthy D, Tsuji LJS. Inadequate nutrient intakes in youth of a remote First Nation community: challenges and the need for sustainable changes in program and policy. ISRN Public Health. (Online) 2012. Available: http://www.isrn.com/journals/ph/2012/504168/ (Accessed 10 May 2012).
19. Gates M, Hanning RM, Gates A, McCarthy D, Tsuji LJS. Assessing the impact of pilot school snack programs on milk and alternatives intake in two remote First Nation communities in northern Ontario, Canada. Journal of School Health (in press).
20. Hanning RM, Skinner K, Gates M, Gates A, Tsuji LJS. School nutrition programs in remote First Nation communities of the western James Bay region: impact, challenges and opportunities. Ottawa, ON: CIHR-IPPH and CIHI-CPHI Population Health Intervention Research Casebook (Online) 2011. Available: http://www.cihr-irsc.gc.ca/e/43472.html#toc (Accessed 10 November 2011).
21. Northern Territory Government: Department of Health and Community Services. The public health bush book, 2nd edn. Darwin, NT: Northern Territory Government. (Online) 2002. Available: http://www.nt.gov.au/health/healthdev/health_promotion/bushbook/volume2/chap3/index.html (Accessed 2 November 2011).
22. Rideout K. Canada's food system: does it exclude our most vulnerable people? SPARC BC 2005; 22(3): 8-10.
23. Saksvig BI, Gittelsohn J, Harris SB, Hanley AJG, Valente TW, Zinman B. A pilot school-based healthy eating and physical activity intervention improves diet, food knowledge, and self-efficacy for Native Canadian Children. Journal of Nutrition 2005; 135(10): 2392-2398.
24. Wein EE. Food consumption patterns of native school children and mothers in Northern Alberta. Journal of the Canadian Dietetic Association 1993; 53(4): 267-273.
25. Forbes LE, Storey KE, Fraser SN, Spence JC, Plotnikoff RC, Raine KD et al. Dietary patterns associated with glycemic index and glycemic load among Alberta adolescents. Applied Physiology Nutrition and Metabolism 2009; 34: 648-658.
26. Hanning RM, Woodruff SJ, Lambraki I, Jessup L, Driezen P, Murphy CC. Nutrient intakes and food consumption patterns in grades six, seven, and eight. Canadian Journal of Public Health 2007; 98: 12-16.
27. Hanning RM, Royall D, Toews JE, Blashill L, Wegener J, Driezen P. Web-based food behaviour questionnaire: validation with grades six to eight students. Canadian Journal of Dietetic Practice and Research 2009; 70: 172-178.
28. Hlimi T, Skinner K, Hanning RM, Martin ID, Tsuji LJS. Traditional food consumption behaviour and concern with environmental contaminants among Cree schoolchildren of the Mushkegowuk Territory. International Journal of Circumpolar Health 71. (Online) 2012. Available: http://www.circumpolarhealthjournal.net/index.php/ijch/article/view/17344 (Accessed 10 May 2012).
29. Minaker LM, McCargar L, Lambraki I, Jessup L, Driezen P, Calengor K et al. School socio-economic status and geographic locale is associated with food behaviour of Ontario and Alberta adolescents. Canadian Journal of Public Health 2006; 97: 357-361.
30. Storey KE, Forbes, LE, Fraser SN, Spence JC, Plotnikoff RC, Raine KD et al. Diet quality, nutrition and physical activity among adolescents: the Web-SPAN (Web-Survey of Physical Activity and Nutrition) project. Public Health Nutrition 2009; 12: 2009-2017.
31. Storey KE, Hanning RM, Lambraki I, Fraser SN, Driezen P, McCargar LJ. Determinants of diet quality among Canadian adolescents as assessed by a web-based survey. Canadian Journal of Dietetic Practice and Research 2009; 70: 58-65.
32. Sutherland C, Skinner K, Hanning RM, Montgomery M, Tsuji LJS. A Cree perspective on gathering community input for physical activity programming in the Mushkegowuk Territory. Pimatisiwin 2007; 5: 169-184.
33. Vance VA, Woodruff SJ, McCargar LJ, Husted J, Hanning RM. Self-reported dietary energy intake of normal weight, overweight, and obese adolescents. Public Health Nutrition 2009; 12: 222-227.
34. Woodruff SJ, Hanning RM. Associations between family dinner frequency and specific food behaviours among grade six, seven, and eight students from Ontario and Nova Scotia, Canada. Journal of Adolescent Health 2009; 44: 431-436.
35. Woodruff SJ, Hanning RM. Effect of meal environment on diet quality rating. Canadian Journal of Dietetic Practice and Research 2009; 70: 118-124.
36. Woodruff SJ, Hanning RM. Associations between diet quality and physical activity measures among a Southern Ontario Regional sample of grade 6 students. Applied Physiology Nutrition and Metabolism 2010; 35: 826-833.
37. Woodruff SJ, Hanning RM, Lambraki, I, Storey KE, McCargar L. Healthy eating index-C is compromised among adolescents with body weight concerns, weight loss dieting, and meal skipping. Body Image 2008; 5: 404-408.
38. Woodruff SJ, Hanning RM, McGoldrick K. Lunch-time food intake and portion size are influenced by the physical and social context of eating among students in grades six, seven, and eight from Southern Ontario. Journal of School Health 2010; 80: 421-428.
39. Woodruff SJ, Hanning RM, McGoldrick K, Brown KS. Healthy Eating Index-C is positively associated with family dinner frequency among students in grade six, seven, and eight from Southern Ontario, Canada. European Journal of Clinical Nutrition 2010; 64: 454-460.
40. Population Health Research Group. Evaluation of the Fruit and Veggies for Every Student (FAVES) snack program in the London District Catholic School Board. Waterloo, ON: University of Waterloo, 2009.
41. Health Canada. Eating well with Canada's food guide for First Nations, Métis and Inuit. Ottawa: Health Canada (Online) 2007. Available: http://www.hc-sc.gc.ca/fn-an/pubs/fnim-pnim/index-eng.php (Accessed 15 January 2012).
42. Institute of Medicine. Dietary reference intakes for calcium and vitamin D. Washington, DC: National Academies Press, 2011.
43. Skinner K, Hanning RM, Tsuji LJS. Barriers and supports for healthy eating and physical activity for First Nation youths in northern Canada. International Journal of Circumpolar Health 2006; 65(2): 148-161.
44. Skinner K, Hanning RM, Sutherland C, Edwards-Wheesk R, Tsuji LJS. Using a SWOT analysis to inform health promotion planning for a remote First Nation community. American Journal of Health Promotion 2012; 26(6): e159-e170.
45. Bernard L, Lavallee C, Gray-Donald K, Delisle H. Overweight in Cree schoolchildren and adolescents associated with diet, low physical activity, and high television viewing. Journal of the American Dietetic Association 1995; 95: 800-802.
46. Institute of Medicine. Dietary reference intakes: applications in dietary assessment. Washington, DC: National Academies Press, 2000.
47. Wein EE, Hawrysh ZJ, Gee MI. Food preferences and food health beliefs of native school children and mothers in northern Alberta. Ecology of Food and Nutrition 1993; 29(4): 259-273.
48. Sharma S, Cao X, Gittelsohn J, Ho LS, Ford E, Rosecrans A, et al. Dietary intake and development of a quantitative food-frequency questionnaire for a lifestyle intervention to reduce the risk of chronic diseases in Canadian First Nations in north-western Ontario. Public Health Nutrition 2007; 7(8): 831-840.
49. Williams PL, McIntyre L, Glanville TN. Milk insecurity: accounts of a food insecurity phenomenon in Canada and its relation to public policy. Journal of Hunger & Environmental Nutrition 2010; 5(2): 142-157.
50. Aboriginal Services Branch and Learning and Teaching Resources. Our words, our ways: teaching First Nations, Métis, and Inuit learners. Alberta Education. (Online) 2005. Available: http://education.alberta.ca/media/511990/words.pdf (Accessed 2 November 2011).
51. Battiste M, McLean S. State of First Nations learning and education. Prepared for the Canadian Council on Learning. Saskatoon, SK: Aboriginal Education Research Centre, University of Saskatchewan. (Online) 2005. Available: http://www.ccl-cca.ca/pdfs/AbLKC/StateOfFirstNationsLearning.pdf (Accessed 2 November 2011).
52. Byrnes J. Aboriginal learning styles and adult education: is a synthesis possible? Australian Journal of Adult and Community Education 1993; 33(3): 157-171.
53. Canadian Council on Learning. Redefining how success is measured in First Nations, Inuit and Métis learning, report on learning in Canada. Ottawa, ON: Canadian Council on Learning (Online) 2007. Available: http://www.ccl-cca.ca/NR/rdonlyres/212C03D9-7B43-4F94-BAFB-784A3199F06E/0/Redefining_How_Success_Is_Measured_EN.pdf (Accessed 2 November 2011).
54. McMullen B, Rohrbach A. Distance education in remote aboriginal communities: barriers, learning styles and best practices. Prince George, BC: College of New Caledonia Press, 2003.
55. Pewewardy C. Learning styles of American Indian/Alaska Native students: a review of the literature and implications for practice. Journal of American Indian Education 2002; 41(3): 1-81.
56. Ryan J. Aboriginal learning styles: A critical review. Language, Culture and Curriculum 1992; 5(3): 161-181.
57. Stairs A. Learning processes and teaching roles in native education: cultural base and cultural brokerage. In: M Battiste, J Barman (Eds). First Nations education in Canada: the circle unfolds. Vancouver, BC: UBC Press, 1995; 139-153.
58. Toulouse PR. What works? Research into practice: integrating Aboriginal teaching and values into the classroom. Toronto: Literacy and Numeracy Secretariat . (Online) 2008. Available: http://www.edu.gov.on.ca/eng/literacynumeracy/inspire/research/Toulouse.pdf (Accessed 2 November 2011).
59. Wein EE. Evaluating food use by Canadian Aboriginal Peoples. Canadian Journal of Physiology and Pharmacology 1995; 73: 759-764.
60. Hanley AJG, Harris SB, Gittelsohn J, Wolever TMS, Saksvig B, Zinman B. Overweight among children and adolescents in a Native Canadian community: prevalence and associated factors. American Journal of Clinical Nutrition 2000; 71: 693-700.
61. Receveur O, Morou K, Gray-Donald K, Macauley AC. Consumption of key food items is associated with excess weight among elementary school-aged children in a Canadian First Nations community. Journal of the American Dietetic Association 2008; 108: 362-366.
62. Trifonopoulos M, Kuhnlein HV, Receveur O. Analysis of 24-hour recalls of 164 fourth to sixth-grade Mohawk children in Kahnawake. Journal of the American Dietetic Association 1998; 98: 814-816.
63. Isogai AD, Gates A, Gates M, Hanning RM, Tsuji LJS. A qualitative evaluation of the efficacy of the delivery of the educational component of a nutrition program in a remote First Nation Community. Pimatisiwin: A Journal of Aboriginal and Indigenous Community Health 2011; 9: 349-362.
64. Gates A, Hanning RM, Gates M, Isogai A, Metatawabin J, Tsuji LJS. A school nutrition program improves vegetable and fruit knowledge, preferences, and exposure in First Nation youth. Open Nutrition Journal 2011; 5: 1-6.


