Risk-taking behaviors
Behavioral risk-taking and unhealthy behaviors have been recognized as the 'actual' leading causes of death across nearly all populations in the USA1,2. These behaviors are diverse, ranging from not wearing a seatbelt to eating a high-fat diet, and affect a variety of acute and chronic outcomes (such as motor vehicle accidents and heart disease). While the reasons individuals engage in such risky or unhealthy behaviors are complex and beyond the scope of this article, the fact remains that educational programs and behavioral interventions focusing on modifying these behaviors present unique opportunities for decreasing the impact of many of the leading causes of death across the lifespan3,4. Unfortunately, behavioral interventions (frequently developed in urban research centers) sometimes fail to reach the populations most at need - particularly populations that are rural and uninsured. Both of these populations have repeatedly been demonstrated to have poorer health status and less access to regular physician services regardless of income level5-7, and the need for interventions specifically tailored to the unique cultural and contextual realities of these groups has been repeatedly articulated8-10.
When considering health risk-taking behaviors in particular, rural groups have been shown to have higher levels of risk-taking behaviors than their urban counterparts. In a sequence of comprehensive examinations of behavioral risk-taking differences between rural and urban groups in 1998 National Health Interview Survey (NHIS) data, Patterson and colleagues found that tobacco use and heavy drinking were comparable or higher in rural settings (varying by racial/ethnic group), that seat belt use was lower in rural settings across all racial/ethnic groups, and that rural residents were less likely to engage in recommended levels of daily physical activity (regardless of racial or ethnic group)8,9. Because of the unique cultural realities of rural living such as increased religiosity, higher rates of poverty, lower access to care and more permissive attitudes toward substance use, differences in risk behaviors indicate the strong need for rural-focused interventions designed to reach populations most at-risk11. The literature surrounding risk-taking behaviors among the uninsured is less robust, but in addition to having lower self-rated health (even when controlling for socioeconomic status and health behaviors)12, the uninsured also have lower attention to health messages across media and are therefore less likely to be affected by traditional health promotion intervention messages10. Because of the lower rates of health literacy and decreased access to care seen in uninsured populations, they represent an especially underserved group in all areas, but particularly in rural settings10.
Caring for the needs of the rural uninsured
While there is no comprehensive safety net of medical providers for uninsured and underinsured Americans, the nationwide system of Federally Qualified Health Centers (FQHCs) provides reduced cost care to more than 16 million patients through 63 million patient visits each year, serving 20% of the low-income uninsured, 33% of individuals who live in poverty and nearly 15% of all rural Americans13. Despite the fact that rural residents only comprise approximately 20% of the US population14, more than 40% of FQHCs are located in rural settings, providing nearly 3,500 locations nationwide that provide natural health behavior intervention access points for underserved rural groups15,16. FQHC patients represent some of the most at-risk groups in the United States: over 70% of FQHC patients live below 100% of the Federal Poverty Line and only 15% have private insurance13. In addition, FQHC patients are more than twice as likely to have a chronic illness (for instance, 11.4% of all FQHC patients are hypertensive, whereas only 4.0% of office-based physician patients are hypertensive)13. Each of these factors make FQHC locations a unique intervention point for reaching groups traditionally underserved by health promotion efforts, particularly rural and uninsured patients. The current literature has largely failed to examine the unique needs that this particular patient group has with regards to behavioral intervention needs, and any variation that may exist between its insured and uninsured patients.
Need for sub-rural investigations
As mentioned, rural-urban differences in risk-taking behaviors have been consistently found. While there are many nationally-representative surveillance programs (such as the national Behavioral Risk Factor Surveillance System [BRFSS] and the National Health Interview Survey [NHIS]) that elucidate population-level differences between geographical groups (eg rural vs urban), these national efforts are not fully able to describe risk-taking within rural areas17. There is remarkable diversity within rural settings where unique cultural factors and socioeconomic circumstances greatly influence behaviors and unexamined subpopulations (such as the rural uninsured) may have individual needs masked by population-level investigations18. This gap in knowledge is even more pronounced when examining the risk-taking behaviors of rural clinical populations, particularly those receiving care in reduced-cost settings such as FQHCs. Knowledge of the most common risk-taking behaviors in rural FQHC populations, and any variations that may exist between insured and uninsured patients, can have a broad impact on what types of programs are most needed within rural FQHC settings. This can guide the development of culturally-tailored, behaviorally-focused interventions designed to directly improve health outcomes in rural areas.
The current study was undertaken to examine the most common risk-taking behaviors of rural FQHC populations and to examine if risk-taking behaviors vary between insured and uninsured rural patients with the goal of informing future behavioral intervention development specific to rural populations.
These methods were originally published in the journal Health and Technology19.
Sampling
A sample of 199 patients was collected at an FQHC in the rural South US using convenience sampling techniques. The FQHC clinic is located in a federally-recognized rural county that is both a Health Professional Shortage Area (HPSA) and a Medically Underserved Area (MUA). The recruitment FQHC is dedicated to serving the uninsured and underserved residents of the local rural area. Potential participants were approached by clinic staff at an already-scheduled clinic appointment. If interested, participants were screened for eligibility (18 years of age or older and able to understand written or spoken English) and informed consent was conducted. Participants were then asked to complete an Audio Computer-Assisted Self-Interview (ACASI), which allowed participants at all literacy levels to complete the questionnaire. Upon completion of the questionnaire, participants were compensated US$5 for their time and effort.
Measures
Participants completed a battery of assessments including demographics (including health insurance coverage), a brief medical history and a survey of the frequency of selected health risk behaviors (the Health Risk Questionnaire). Health insurance was defined to participants as 'any type of health plan that helps pay for your medical services, including health insurance, Medicaid, Medicare, etc'. The Health Risk Questionnaire (HRQ) is a 28-item instrument assessing self-reported frequency of engagement in a variety of health risk behaviors, including diet, exercise, substance use, motor vehicle risks, sexual behaviors, violence and medical risk-taking (eg not taking prescribed medication). Items are scored on a five-point frequency scale (never, rarely, sometimes, most of the time, always or almost always).
Analysis
Descriptive statistics were calculated to describe both the demographic characteristics and the health risk-taking behaviors of the sample. To examine potential differences in health risk-taking behaviors between insured and uninsured participants, differences in frequencies of behaviors were examined using nonparametric Mann-Whitney U-tests. Because of the number of behaviors being examined, an omnibus test was not conducted. All analyses were conducted using Statistical Package for Social Sciences v17 (IBM; Armonk, NY, USA; http://www-01.ibm.com/software/analytics/spss/).
Ethics approval
All study activities were conducted with the approval of the Institutional Review Board of Georgia Southern University (protocol H11230).
Demographics
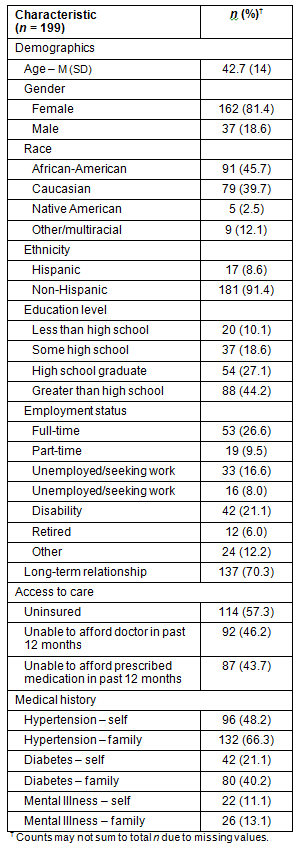
Average age of participants was 42.7 years (SD=14). The sample was predominantly female (81.4%), with wide racial/ethnic diversity: 45.7% of the sample identified as African-American, 39.7% as Caucasian and 8.6% as Hispanic. This racial/ethnic distribution is generally consistent with the overall FQHC population of Georgia (49% African-American, 37% Caucasian and 15% Hispanic20). The majority of the sample (55.8%) had a high school education or less, and only 26.6% of the sample was employed full-time. More than half of the participants (57.3%) had no medical insurance (consistent with the overall Georgia FQHC clinic population with 49.7% uninsured20), and the most commonly reported diagnoses among the patients were hypertension (48.2%) and diabetes (21.1%). Other demographic and medical history descriptive information is provided (Table 1).
Table 1: Participant characteristics
Health risk behaviors
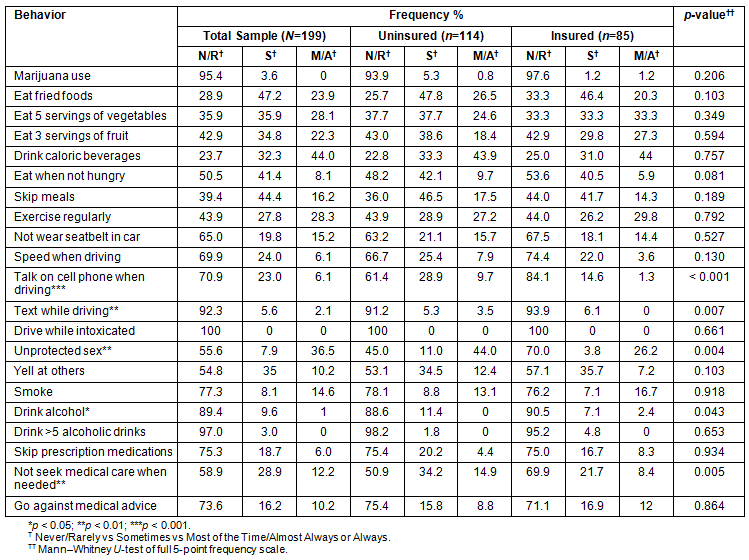
When examining health risk behaviors, the most commonly engaged in behaviors were eating fried foods (23.9% most of the time/always), not eating five servings of vegetables per day (35.9% never or rarely), not eating three servings of fruit per day (42.9% never or rarely), drinking caloric beverages (44% most of the time/always), not exercising regularly (43.9% never or rarely), not wearing a seatbelt (15.2% most of the time or always not wearing), having sex without a condom (36.5% most of the time/always) and smoking (14.6% most of the time/always). Additional health risk behaviors are provided (Table 2).
Differences between insured and uninsured patients in their health risk behaviors are also provided (Table 2). Uninsured patients were more likely to talk on their cell phones while driving (p<0.001), more likely to text while driving (p=0.007), more likely to have unprotected sex (p=0.004), more likely to drink alcohol (p=0.043) and more likely to not seek medical care when needed (p=0.005).
Table 2: Selected health risk behaviors of insured and uninsured patients
Discussion
This article suggests that the behavioral risk-taking of FQHC patients in the South USA is largely dietary- and exercise-related, with other specific risk behaviors (such as smoking and not wearing seatbelts) also high. More importantly, our findings suggest there may be important differences in risk-taking behaviors between insured and uninsured patients, even in a setting designed to address the needs of uninsured patients. This becomes particularly important when deciding what types of programs to offer in certain settings - in a clinic where many/most patients are uninsured (such as an FQHC), additional focus may need to be placed on behaviors such as proper cell phone use while driving or the importance of having protected sex. While the underlying cause of the differences between the insured and uninsured groups is likely due to a combination of socioeconomic factors such as income and education, examining these differences can help guide the types of interventions that may be most needed when reaching out to groups with a high representation of uninsured individuals.
Interestingly, two of the behaviors with demonstrated differences between rural insured and uninsured patients are related to cell phone use while driving (involving a relatively new technology). Historically, rural areas have been seen as technologically delayed21 and even today questions are still frequently raised about access to technologies among rural populations (particularly the underserved)19. It could be that assumptions about technology use among underserved rural residents have minimized prevention education surrounding safe cell phone use in rural settings. Future studies should examine the reasons behind these differences and explore ways to increase safe cell phone use among underserved rural groups.
When examining the difference in seeking medical care when needed, it is interesting that strong differences emerged despite the fact that all participants were active patients at a low-cost clinic. One would expect to see strong differences between general insured and uninsured populations with respect to seeking medical care when needed, but the fact that this difference emerged so strongly even within an active patient population indicates that the impact of not having insurance goes beyond perceptions of access to care. Nearly half of the uninsured participants (49.1%) reported that they sometimes or more often avoid going to the doctor even when they know they need to, whereas only 30% of insured patients reported this behavior. Given that all of these patients had access to care at greatly reduced cost through the FQHC, the continued barrier to seeking out care demonstrated by this difference between insured and uninsured patients needs further investigation to identify the additional barriers at play. Cultural factors such as traditions of self-reliance and avoidance of 'charity' care within rural settings may be influencing this process11. Until the barriers to seeking care faced by individuals with access to reduced cost services can be identified, efforts to improve access alone may not sufficiently address the needs of underserved rural patients.
The difference found in frequency of unprotected sex was strong: more than half of uninsured patients reported sometimes, most of the time, or always having unprotected sex, whereas 70% of insured patients reported never or rarely having unprotected sex. This strong difference has significant implications for sexual health, including STIs and HIV. While HIV rates in rural areas tend to be low compared to urban settings, rates of condom use are consistently low and indicate that the HIV epidemic could rapidly spread further into rural settings without new intervention22. It is therefore critically important to develop HIV-prevention interventions targeted to rural settings (particularly for the most underserved). The lasting perception that HIV is 'not a problem' in rural areas may be influencing both rural residents' perceptions of their own risk and the perceived importance of HIV prevention to care providers.
Limitations
The results of the study should be interpreted within the context of its design. All patients came from a single rural FQHC, therefore affecting the ability to generalize outside of the rural South US where traditions involved with risk (eg alcohol use, smoking, unhealthy diet) and protection (eg increased social connectedness and high religiosity) are somewhat unique in the nation. Additionally, while most demographic characteristics were generally representative of the larger Georgia FQHC patient population, participants in this study were disproportionately female (80% vs the Georgia average of 60%) and the study's results may be different if looking at male patients in particular. However, there was not a significant gender difference between the insured and uninsured groups (data not shown), minimizing the potential for artificiality of the differences found between the insured and uninsured groups. While frequency of health risk behaviors was assessed, no qualitative data were collected to examine why differences in behaviors may have emerged. Such data would be very illustrative for the development of behavioral interventions.
Rural FQHC patients demonstrate high levels of behavioral and health risk taking, including dietary-, exercise- and traffic-related risks. Differences exist between insured and uninsured patients, indicating that the reasons behind behavioral risk-taking may be context-specific and need to be explored further to help identify intervention targets that are culturally and situationally appropriate for diverse rural groups.
Acknowledgments
This study was supported by a Georgia Southern University CLASS/ORSSP Seed Grant. The authors acknowledge the leadership and staff of East Georgia Healthcare Center for their assistance with data collection.
References
1. Mokdad AH, Marks JS, Stroup DF, Gerberding JL. Actual causes of death in the United States, 2000. Journal of the American Medical Association 2004; 291(10): 1238-1245.
2. Schoenborn CA, Adams PE. Health behaviors of adults: United States, 2005-2007. Vital Health Statistics 2010; 245(1): 1-132.
3. Schwarzer R. Modeling health behavior change: How to predict and modify the adoption and maintenance of health behaviors. Applied Psychology 2008; 57(1): 1-29.
4. Glanz K, Rimer BK, Viswanath K. Health behavior and health education. San Francisco, CA: Jossey-Bass, 2008.
5. Ross JS, Bradley EH, Busch SH. Use of health care services by lower-income and higher-income uninsured adults. Journal of the American Medical Association 2006; 295(17): 2027-2036.
6. Ettner SL. The relationship between continuity of care and the health behaviors of patients: Does having a usual physician make a difference? Medical Care 1999; 37(6): 547-555.
7. Ayanian JZ, Weissman JS, Schneider EC, Ginsburg JA, Zaslavsky AM. Unmet health needs of uninsured adults in the United States. Journal of the American Medical Association 2000; 284(16): 2061-2069.
8. Patterson PD, Moore CG, Probst JC, Samuels ME. Prevalence of health related behavioral risk factors among non-metro minority adults. South Carolina Rural Health Research Center Report. Columbia, SC: SCRHRC, 2003.
9. Patterson PD, Moore CG, Probst JC, Samuels ME. Hypertension, diabetes, cholesterol, weight, and weight control behaviors among non-metro minority adults. South Carolina Rural Health Research Center Report. Columbia, SC: SCRHRC, 2002.
10. Cheong PH, Feeley TH, Servoss TJ. Understanding health inequalities for uninsured Americans: A population-wide survey. Journal of Health Communication 2007; 12(3): 285-300.
11. Smalley KB, Warren JC. Rurality as a diversity issue. In: KB Smalley, JC Warren, JP Rainer (Eds). Rural mental health: issues, policies, and best practices. New York: Springer Publishing Company, 2012; 37-47.
12. Hahn BA. Health status of the uninsured: an investigation of health behaviors and medical care usage (PhD thesis). Urbana-Champaign, IL: University of Illinois at Urbana-Champaign, 1992.
13. National Association of Community Health Centers. A sketch of community health centers: chart book 2009. Bethesda, MD: NACHC, 2010.
14. United States Census Bureau. 2010 Census urban and rural classification and urban area criteria. Washington, DC: USCB, 2012.
15. Office of Rural Health Policy. Effective collaboration between critical access hospitals and federally qualified health centers. Washington, DC: Health Resources and Services Administration, 2010.
16. The Henry J. Kaiser Family Foundation. Service delivery sites operated by federally-funded federally qualified health centers, 2010. Menlo Park, CA: KFF, 2011.
17. Nelson DE, Holtzman D, Bolen J, Stanwyck CA, Mack KA. Reliability and validity of measures from the behavioral risk factor surveillance system (BRFSS). Sozial- und Praventivmedizin 2001; 46(s1): S3-S42.
18. Smalley KB, Yancey CT, Warren JC, Naufel N, Ryan R, Pugh JL. Rural mental health and psychological treatment: A review for practitioners. Journal of Clinical Psychology 2010; 66(5): 479-489.
19. Warren JC, Smalley KB, Klibert J, Denmark JW. Access to emerging technologies and telehealth intervention modality preferences in rural patients. Health and Technology 2011; 1(2): 99-105.
20. HRSA Office of Primary Care. Uniform data system report: 2010 Georgia report. Washington, DC: HRSA, 2011.
21. Kline RR. Consumers in the country: technology and social change in rural America. Baltimore, MD: The Johns Hopkins University Press; 2000.
22. Oser CB, McDonald HMS, Havens JR, Leukefeld CG, Webster JM, Cosentino-Boehm AL. Lack of HIV seropositivity among a group of rural probationers: explanatory factors. Journal of Rural Health 2006; 22(3): 273-275.


