Rural medical education in Australia
The trend for medical education to be delivered through longitudinal placements in general practice and other community settings1,2 is now firmly in place in medical schools worldwide3,4. Curriculum components and methods that optimise effective teaching in rural placement have been developed5-8, and early meaningful exposure to patients has been shown to improve the transition from medical student to junior doctor9,10.
There is robust evidence that rural placements provide incentive for a decision to practise in a rural setting11-19, although this evidence is still contentious20. It has also been established that students who take training through rural placement do at least as well as students who study in traditional, metropolitan hospital-based training sites21-28. Clinical placements also facilitate the transfer from the learning orientation of medical school to the performance orientation of the clinical setting29. The informal curriculum is influential in determining the perceived worth of a primary care placement experience30.
Delivery of a rural educational program relies heavily on local practitioners. Placements are with a mix of rural General Practitioners (GPs), rural hospitals and local patient care services of other types, including mental health, community health and population health centres. Support systems for rural practitioners have been developed31,32.
It has been shown that students' individual resilience and ability to adapt to new and sometimes strange-seeming situations is a major determinant in whether a student thrives in a rural setting33. Student success in rural placements requires clinical educators who are well organised and develop close one-on-one relationships with students34.
The negative effects of social displacement must be balanced against the positive results of rural placements33, although even students raised exclusively in metropolitan environments consider rural training attractive for the benefits of enhanced patient access35.
This study
The medical program at the University of Western Sydney (UWS) is a 5 year program, established in 2007, that accepts school leavers and those with part or completed degrees. There is a strong focus on the health issues of western Sydney, but the program aims to produce doctors who can work comfortably in any community setting. The UWS curriculum incorporates an immersion experience in rural practice settings as an integral component of assimilation of clinical skills. These longitudinal community placements are modelled on the Flinders University Parallel Rural Community Curriculum (PRCC)21.
This study examines the experience of the first year cohort of the UWS Medical School long-term rural placement students. Results are placed in the context of other published results for rural training schemes, comparing and contrasting the present results to those of others.
Design
A mixed methods approach was taken for the evaluation. Each student completed a survey and participated in a focus group.
Population
All students who had completed a rural placement during the final year of their UWS medical program were invited to complete the evaluation. None declined. A total of 21 students completed the evaluation.
Data collection
Students filled out a 46 item quantitative survey consisting of 37 closed-ended and nine open-ended questions. The survey was modified from a validated instrument36. Closed-ended responses were captured in six item Likert37 scales.
Students also participated in one of two focus groups38. An audio recording was made of each focus group and the recording transcribed verbatim.
Class rankings of students, and changes over the time of their placement, were also examined. The evaluation was carried out at the end of the placement year.
Data analysis
Quantitative data were analysed in Microsoft Excel (descriptive statistics) and Statistical Package for Social Sciences (Pearson's χ2 test, paired t-test; SPSS Inc; www. spss.com). Data analysis for qualitative results was aided by NVivo v9 (QSR International; www.qsrinternational.com).
Ethics approval
The evaluation was carried out under approval of the University of Sydney Human Research Ethics Committee, protocol number 13006, issued 8 September 2010.
Overall, students were very pleased with their rural experience, both clinically and socially. Logistics and administrative support, both before the beginning of the placement and on arrival, were well regarded.
Survey results
Rating scores submitted by students regarding all aspects of the placement are summarised (Table 1). Clinical experiences in all areas received uniformly high scores across both groups. Clinical preceptors were highly regarded. The smaller realm of the medical world in a rural area was considered an advantage in providing more hands on experience and more interprofessional team approaches to health care provision. It was also considered a drawback by some in that more advanced cases of all kinds were sent out of the area to metropolitan hospitals. All students were critical of their required community medicine group research project, rating it collectively at less than 2.9 on a scale of 5.
Table 1: Survey results (n=21)
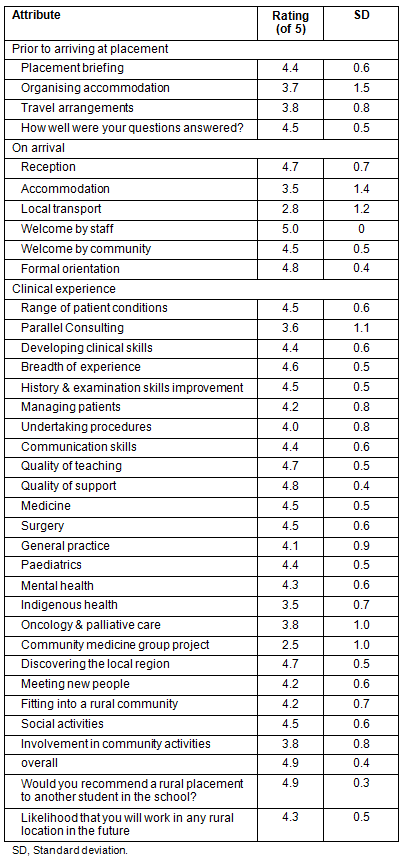
In the social realm, the placement experience was highly rated. Criticisms of the experience both socially and clinically were essentially anecdotal, with only one or two students voicing any particular criticism. Accommodation and local transport were universally mentioned as needing improvement.
Students considered it likely or highly likely that they would consider working in a rural location in future, although only three of 21 actually applied to do their internship in a rural setting. Students' future intentions regarding rural work are summarised (Table 2). Rural lifestyle, the nature of the rural clinical experience and work/life balance were the most frequently cited decision criteria in selecting a practice location. There was no statistically significant association of factors motivating for or against future rural practice nor for subsequent rural internship placement.
Table 2: Likelihood of future rural work (n=21)

Improvement in class standing
Between their ranking in the end of Year 3 examination and the examination in the middle of Year 5, during which period students undertook their year-long placement, 14 of 22 students increased their class rank while two experienced no change and six decreased their class rank. Overall, the rural cohort advanced on average 4.2 places compared to their urban-placed peers in the full cohort. The change in class rank was not statistically significant (p=0.138, paired t-test), but the improvement in test scores (mean=3.8, SD=2.28) between Year 3 and 5 exams (for rural placement students) was significant at p<0.0001 (paired t-test).
Focus group results
Verbatim quotes are included to exemplify major themes raised. Numbers are used to differentiate speakers within a dialogue and (I) is used to denote the interviewer. So as to maintain de-identification of speakers, no gender or ethnicity data are included.
Student participants in focus groups were quite enthusiastic about their experience away from the main campus. Students found the rural experience more comprehensive than they expected, or that they expect they would have received in a metropolitan area.
...when I heard [from fellow students] of the orthopaedics rotations in [city hospital] often they would focus on one or two joints, but in [rural clinical placement site] it really was everything and I think there was aspects of that in all the other rotations as well ... in [rural clinical placement site] they just sort of cover everything.
The staff support is immense. Especially in medicine and surgery they really went out of their way to give us teaching sessions and things.
... and physical examinations, we expected to learn them, but not as well as we were taught ... I think I got really good at them at the end, and I'm sure everybody else did as well.
They found their communities welcoming and supportive:
We were on the front page of the newspaper several times and people were stopping us on the street and saying, 'Oh, were you in that -?' They recognise you. They were very excited to have you.
I: How did that feel? Being sort of celebrities?
Awesome.
They also felt that they received more quality time from clinical educators:
1: I felt like I learned more in my year in [rural clinical placement site] than I probably did in the last two years before that in [city hospital] just because of the amount of time that you get to spend with your patients and the sort of breadth of experience that you get, and just the fact that so many of the clinicians are more willing to teach out there, as well.
2: I think I got a lot more direct contact with the specialists than I thought I would get ... and because of that there was a lot of not just clinical teaching, but about life as well.
3: I think I found several mentors ... that I hadn't found in any hospital, despite having a great time and a great learning experience in the city.
And they sensed that there was a camaraderie in rural placement that they would not have experienced elsewhere:
I ... liked the friendly sort of atmosphere between the consultants in the area and ... the students, so you sort of form a friendship with the consultants that are supervising you but they're also friends with each other, and they're also friends with the students from the other universities. And that whole atmosphere is just really nice ... You don't really get that in the city.
I think just being able to talk to them in the social environment, so when the time comes that we're in the clinical environment we're not scared to ask a question that we may have previously been, 'Oh, that's too stupid to ask out loud.' ... Also, they're more willing to engage with us.
And it's much easier to raise things that you're concerned about in a social environment rather than in the hospital, like you can just be like, 'Oh, man, I'm not doing that well at cannulating,' or something like that and the next day he'll take you around and be like, 'Oh, this is what you told me. Come on, let's do this.' And it's much easier to do that with a friend than with somebody that you see as your superior ...
Students came to their rural placement with some pre-conceived notions that they discovered were false:
When you think of going rural, you think makeshift contraptions they use to do so-and-so procedure because they don't have it because they're rural ... when you go to [rural clinical placement site], it's actually more advanced, in terms of some technologies, than [inner suburb teaching hospital].
Like, they have a cath lab and in [inner suburb teaching hospital] we don't have a cath lab. And they're probably closer to getting an MRI than we are.
... whereas we shopped all of our [city hospital] trauma to [suburban teaching hospital], [rural clinical placement site] keeps it.
... We became more city, ironically.
... when I initially left for [rural clinical placement site] I felt like I was losing a bit of the patient-centred aspect of medicine ... But then when I went to [rural clinical placement site], ... I felt like seeing a patient in hospital and then being able to see them somewhere out in the community, ... I felt like it sort of became more about the patients again rather than the disease process ...
Student GP experience differed by practice placement:
1: When I went to my GP ... with my learning objectives list, s/he crossed off four out of the eight because s/he said you'll never see those, and they were STIs, illegal drug use, and other things on that line. S/He said it was too middle class. I was in [town A]. S/He said, 'You just won't see that. There's no point in putting it as a learning objective'.
2: I saw all those.
1: Well, you were in [town B], and I was in [town A].
3: The practice I went to, it was pretty good in terms of asking me what I needed to get done and making sure they organised that. ... And seeing procedures in rural GP is really good, because they have a bigger role, I think ... in terms of procedural GPs I got to see circumcisions and things like that that I didn't even know a general practitioner could even do.
An intriguing dialogue was captured in one focus group regarding Aboriginal patients, who did not conform to the students' concept of Indigenous Australians:
1: ... one of the things I find that it was, maybe it was just the practice we went to, the Aboriginal Medical Service, a lot of the Aboriginals that turned up were mainstreams, so we didn't have very much in terms of -
I: What do you mean by mainstream?
[laughter]
1: Maybe not mainstream, but close to - to be honest, it was kind of like they could have gone to a general practitioner - I'm just digging a hole for myself.
2: They identified themselves as Aboriginal, but they may not have looked that way, I guess.
[laughter]
1: I guess the problem is, when you talk about Aboriginal health in lectures, they're always talking about the -
I: The big problems.
1: Yeah, the diseases ....
3: We have to keep in mind that we were seeing Aboriginal people in [regional centre], which isn't the outback.
1: Yeah, that's what I kind of mean by 'mainstream'.
3: We didn't get exposure to Aboriginal communities.
2: Quite clearly we're not very adept at community sensitivity.
I: So Aboriginal culture was missing?
Yeah.
Yeah.
I: Most people were mainstream and their issues weren't culture-specific?
Yeah.
3: I think where this is coming from is that we all noticed an incongruency between what we'd been taught about Aboriginal health, and what we actually saw in the practice.
4: ... the whole point of the Aboriginal rotation was to at the end of it feel like we could interact with Aboriginal people more and understand if we see an Aboriginal patient in the future what services are available and that sort of thing. And that wasn't aptly demonstrated...
This theme was not evident in all groups. In fact, one student offered this as a favourite memory of time spent in another rural placement site:
I think clinically one of my favourite experiences in the whole of the medical course to date was an indigenous attachment of a drug and alcohol rehab place out sort of the back of [rural town] that involved a lot of Aboriginal men who had come straight from prison, and I felt like that was a very useful experience for me to have as a [person with a different cultural background], to sort of learn to try and relate to people that I don't share very many cultural similarities with. It was both very, very challenging and very useful.
Students were concerned that if they continued in rural practice through their internship that they would have difficulty integrating into a metropolitan environment:
1:... a lot of training programs you have to go to a city hospital, ... and it's sort of scary, the idea of doing an internship at a rural hospital and then ... having the city interns ahead of you in terms of getting into those training programs because they're more well-known to the supervisors or they're already working at the hospital where the training program is based.
2: I think that's what deterred me from going rural straight away as an intern, because of the differing opinions of the people I talked to as to how easy it is to get into a registrar training program after going to a rural hospital. I think that was one of the factors.
The students felt that a rural setting was a good place to learn medicine because they saw more of the patient's journey:
I think I've had more of a chance to see and to follow patients through for quite a while because of the general term or general team you see everyone on the ward, and you can follow them through when you're doing oncology. At the same time you're doing oncology you might see them in their oncology context over at [outpatient clinic] and you might see them back in the hospital, and you might see them in the community and I got to see some of the communication between healthcare providers, whether it was good or bad, and how people reacted to it and reflected on it and I thought that was very interesting.
Discussion
The students in this study reported an overall high level of satisfaction along with some problems, which were mainly systems issues and early-days logistics issues. Findings were similar to other evaluations of rural medical training programs in that students:
- found the teaching and learning program satisfactory6-8,17,21,27,39-41
- relied on local coordinators to help them with the transition to, and functioning in, the new environment6,40,
- were apprehensive about whether their learning in the rural setting would adequately prepare them for assessment back on the main campus21,39,
- appreciated the collegiality and perceived beneficial life/work balance of rural living/practice6,21,40 ,
- considered themselves better prepared to advance to internship because of the perceived additional attention afforded in a rural location with higher student/educator interaction17,21,40,
- experienced a longitudinal, rather than cross-sectional, experience of a patient's journey7,21,42,
- were able to actively participate in providing actual patent care6,17,21,40
- appreciated the differences between rural and metropolitan general practice43
- developed trust and confidence in their clinical educators as role models44
- felt that they were part of a healthcare team, as opposed to learning observers45
- increased their receptiveness to a rural medical career12,13,27,46,47
- assimilated the concept that permissive boundary definitions and dual relationships, which are usually avoided or cautioned against in urban settings, are not only acceptable but can be beneficial when practising in a rural area48-51.
Some findings of evaluations of rural students published early in the history of rural placements in Australia were not evident here. These include:
- anxiety over the rural experience21,39
- frustration with the rural experience8
- lack of exposure to essential basic procedures such as suturing and airway management52.
Experience with Aboriginal health services
With regards to the comments of some of these students regarding their Aboriginal health experience, these students did recognise that part of this was context: they did not see Aboriginal people in their own environments. This is an example of the hidden curriculum at work53, and the inherent disconnection between the classroom and the clinic when it comes to the cultural and social realities of practice54. While these students are not racist, their use of language and their conceptual frameworks indicate that their training thus far had not completely prepared them for the reality of Aboriginal health work. They held a stereotypical view of Aboriginal people and Aboriginal health status, one founded on the 'plight'55 of Indigenous people. Knowing that the health status of Indigenous Australians is on aggregate worse than that of other ethnic groups, they had fallen into an ecological fallacy where they expected that the ill health (and a certain physical appearance) of all Aboriginal Australians was uniform. This expectation was so strong that it made them question whether the patients they saw - who did not conform to their mental models of what an Aboriginal Australian should look like or present with - should be seen at a dedicated Aboriginal health clinic.
Instruction in the life and health of Indigenous Australians is a vital part of the social mission of medical schools56. Curriculum designers should examine classroom teaching content to ensure that it accurately portrays the Aboriginal community as a whole57, emphasising the complexity of culture and range of living conditions that make up Aboriginal Australia43 and avoiding a 'deficit-based perspective'58 that emphasises extreme cases over routine presentations59, particularly as Indigenous Australians often come from diverse racial backgrounds60 and so do not conform to any classic notion of what an Indigenous person looks like.
A critical reflection tool60, developed by Medical Deans Australia and New Zealand to assist in framing Indigenous curriculum components and recently trialled and increasingly incorporated into the school's curriculum, may be an important element in achieving this. Other good guidance is also available61,62.
Future research is warranted examining:
- the extent to which the apprehension of students in rural placements (especially postgraduate years) regarding their ability to re-integrate into a metropolitan setting is warranted
- the 'cultural' effects of rural immersion programs - Are there important differences in the hidden and informal curricula between metropolitan and rural Australian medical education settings? What are the important dynamics of the interaction between metropolitan medical students and rural people?
- the reasons why rural students appear to perform better than their peers in traditional hospital-based clerkships.
The major criticisms revealed in this study are easily remedied; they are indications of start-up logistics problems, not fundamental deficits in program planning or delivery. The students in this study considered their experience worthwhile and indicated that it contributed to their interest in working in rural or regional Australia.
The results of this study are encouraging not only because they indicate that the UWS medical education program is off to a good start, but also because they confirm that rural placements have come into their own in Australia. Taken together, the results reported by Australian medical schools now offering long-term rural placements suggest that such placements are at least as effective as, and may even be more effective than, metropolitan hospital placements in providing clinical education to medical students in their senior years. The 'Australian rural health education revolution'63 is showing results.
Acknowledgements
The authors thank the students for their willingness to share their reflections on their experience; the Commonwealth Department of Health and Ageing for financial support; Heather Barger Talbot for transcribing focus group recordings; Jenny Akers, Rural Program Manager, UWS, for providing continuing support to students and faculty; and three anonymous reviewers.
References
1. Prideaux D. Medical education in Australia: much has changed but what remains? Medical Teacher 2009; 31(2): 96-100.
2. Birden H, Page S. 21st century medical education. Australian Health Review 2007; 31(3): 341-350.
3. Mattick K, Knight L. High quality learning: harder to achieve than we think? Medical Education 2007; 41(7): 638-644.
4. Eley DS. Postgraduates' perceptions of preparedness for work as a doctor and making future career decisions: support for rural, non-traditional medical schools. Education for Health 2010; 23(2): 374.
5. Page S, Birden H. Twelve tips on rural medical placements: what has worked to make them successful. Medical Teacher 2008; 30(6): 592-596.
6. Couper I, Worley P, Strasser R, Strasser I. Rural longitudinal integrated clerkships: lessons from two programs on different continents. Rural and Remote Health 11: 1665. (Online) 2011. Available: www.rrh.org.au (Accessed 12 February 2012).
7. Couper ID, Worley PS. Meeting the challenges of training more medical students: lessons from Flinders University's distributed medical education program. Medical Journal of Australia 2010; 193(1): 34-36.
8. Denz-Penhey H, Murdoch J. 'It's really, really good, but it could be a lot better': qualitative evaluation of a rural clinical school, four years on. Medical Teacher 2009; 31(10): 443-448.
9. Dornan T, Boshuizen H, King N, Scherpbier A. Experience-based learning: a model linking the processes and outcomes of medical students' workplace learning. Medical Education 2007; 41(1): 84-91.
10. Bleakley A, Brennan N. Does undergraduate curriculum design make a difference to readiness to practice as a junior doctor? Medical Teacher 2011; 33(6): 459-467.
11. Strasser R, Hogenbirk JC, Lewenberg M, Story M, Kevat A. Starting rural, staying rural: how can we strengthen the pathway from rural upbringing to rural practice? Australian Journal of Rural Health 2010; 18(6): 242-248.
12. Young L, Kent L, Walters L. The John Flynn Placement Program: evidence for repeated rural exposure for medical students. Australian Journal of Rural Health 2011; 19(3): 147-153.
13. Lee YH, Barnard A, Owen C. Initial evaluation of rural programs at the Australian National University: understanding the effects of rural programs on intentions for rural and remote medical practice. Rural and Remote Health 11: 1602. (Online) 2011. Available: www.rrh.org.au (Accessed 12 February 2012).
14. Stagg P, Greenhill JA, Worley PS. A new model to understand the career choice and practice location decisions of medical graduates. Rural and Remote Health 9: 1245. (Online) 2009. Available: www.rrh.org.au (Accessed 12 February 2012).
15. Henry JA, Edwards BJ, Crotty B. Why do medical graduates choose rural careers? Rural and Remote Health 9: 1083. (Online) 2009. Available: www.rrh.org.au (Accessed 12 February 2012).
16. Rice L, Stokes M-L, Brown MA, Campbell KA, Smith C. Will Australian rural clinical schools be an effective workforce strategy? Early indications of their positive effect on intern choice and rural career interest. Medical Journal of Australia 2008; 189(6): 346-347.
17. Eley D, Young L, Baker P, Wilkinson D. Developing a rural workforce through medical education: lessons from down under. Teaching and Learning in Medicine 2008; 20(1): 53-61.
18. Roberts C, Daly M, Kumar K, Perkins D, Richards D, Garne D. A longitudinal integrated placement and medical students' intentions to practise rurally. Medical Education 2012; 46(2): 179-191.
19. Strasser R, Neusy AJ. Context counts: training health workers in and for rural and remote areas. Bulletin of the World Health Organization 2010; 88(10): 777-782.
20. Ranmuthugala G, Humphreys J, Solarsh B, Walters L, Worley P, Wakerman J et al. Where is the evidence that rural exposure increases uptake of rural medical practice? Australian Journal of Rural Health 2007; 15(5): 285-288.
21. Worley P, Silagy C, Prideaux D, Newble D, Jones A. The parallel rural community curriculum: an integrated clinical curriculum based in rural general practice. Medical Education 2000; 34(7): 558-565.
22. Sen Gupta TK, Hays RB, Kelly G, Buettner P. Are medical student results affected by allocation to different sites in a dispersed rural medical school? Rural and Remote Health 11: 1511. (Online) 2011. Available: www.rrh.org.au (Accessed 12 February 2012).
23. Power DV, Harris IB, Swentko W, Halaas GW, Benson BJ. Comparing rural-trained medical students with their peers: performance in a primary care OSCE. Teaching & Learning in Medicine 2006; 18(3): 196-202.
24. Lenthall S, Wakerman J, Knight S. The frontline and the ivory tower: a case study of service and professional-driven curriculum. Australian Journal of Rural Health 2009; 17(3): 129-133.
25. Wilson M, Cleland J. Evidence for the acceptability and academic success of an innovative remote and rural extended placement. Rural Remote Health 8: 960. (Online) 2008. Available: www.rrh.org.au (Accessed 12 February 2012).
26. McLean RG, Pallant J, Cunningham C, DeWitt DE. A multi-university evaluation of the rural clinical school experience of Australian medical students. Rural and Remote Health 10: 1492. (Online) 2010. Available: www.rrh.org.au (Accessed 12 February 2012).
27. Lyon PM, McLean R, Hyde S, Hendry G. Students' perceptions of clinical attachments across rural and metropolitan settings. Assessment & Evaluation in Higher Education 2008; 33(1): 63-73.
28. Worley P, Esterman A, Prideaux D. Cohort study of examination performance of undergraduate medical students learning in community settings. BMJ 2004; 328(7433): 207-209.
29. Teunissen PW, Westerman M. Junior doctors caught in the clash: the transition from learning to working explored. Medical Education 2011; 45(10): 968-970.
30. Jerant A, Srinivasan M, Bertakis KD, Azari R, Pan RJ, Kravitz RL. Attributes affecting the medical school primary care experience. Academic Medicine 2010; 85(4): 605-613.
31. Moran J, Page S, Birden H, Fisher L. Doctors trading places: the Isolated Practitioner Peer Support Scheme. Medical Journal of Australia 2009; 191(2): 78-80.
32. Pond BR, Dalton LG, Disher GJ, Cousins MJ. Helping medical specialists working in rural and remote Australia deal with professional isolation: the Support Scheme for Rural Specialists. Medical Journal of Australia 2009; 190(1): 24-27.
33. Bayley SA, Magin PJ, Sweatman JM, Regan CM. Effects of compulsory rural vocational training for Australian general practitioners: a qualitative study. Australian Health Review 2011; 35(1): 81-85.
34. Goertzen J, Stewart M, Weston W. Effective teaching behaviours of rural family medicine preceptors. Canadian Medical Association Journal 1995; 153(2): 161-168.
35. Krahe LM, McColl A, Pallant J, Cunningham C, DeWitt D. A multi-university study of which factors medical students consider when deciding to attend a rural clinical school in Australia. Rural and Remote Health 10: 1477. (Online) 2010. Available: www.rrh.org.au (Accessed 12 February 2012).
36. Irby DM, Ramsey P, Gillmore G, Schaad D. Characteristics of effective clinical teachers of ambulatory care medicine. Academic Medicine 1991; 66(1): 54-55.
37. Likert R. A technique for the measurement of attitudes. Archives of Psychology 1932; 22(140): 44-53.
38. Nestel D, Ivkovic A, Hill RA, Warrens AN, Paraskevas PA, McDonnell JA et al. Benefits and challenges of focus groups in the evaluation of a new Graduate Entry Medical Programme. Assessment & Evaluation in Higher Education 2012; 37(1): 1-17.
39. Denz-Penhey H, Murdoch J, Lockyer-Stevens V. 'What makes it really good, makes it really bad.' An exploration of early student experience in the first cohort of the Rural Clinical School in the University of Western Australia. Rural and Remote Health 4: 300. (Online) 2004. Available: www.rrh.org.au (Accessed 12 February 2012).
40. Sen Gupta T, Muray R, McDonell A, Murphy B, Underhill A. Rural internships for final year students: clinical experience, education and workforce. Rural and Remote Health 8: 827. (Online) 2008. Available: www.rrh.org.au (Accessed 12 February 2012).
41. D'Amore A, Mitchell EKL, Robinson CA, Chesters JE. Compulsory medical rural placements: senior student opinions of early-year experiential learning. Australian Journal of Rural Health 2011; 19(5): 259-266.
42. Ogur B, Hirsh D. Learning through longitudinal patient care-Narratives from the Harvard Medical School - Cambridge integrated clerkship. Academic Medicine 2009; 84(7): 844.
43. Denz-Penhey H, Murdoch JC. A student view of the difference between general practice and rural and remote medicine. Rural and Remote Health 7: 641. (Online) 2007. Available: www.rrh.org.au (Accessed 12 February 2012).
44. Zink T, Halaas GW, Brooks KD. Learning professionalism during the third year of medical school in a 9-month-clinical rotation in rural Minnesota. Medical Teacher 2009; 31(11): 1001-1006.
45. Denz-Penhey H, Shannon S, Murdoch J, Newbury J. Do benefits accrue from longer rotations for students in Rural Clinical Schools? Rural and Remote Health 5: 414. (Online) 2005. Available: www.rrh.org.au (Accessed 12 February 2012).
46. Eley D, Baker P. The value of a rural medicine rotation on encouraging students toward a rural career: clear benefits from the RUSC program. Teaching & Learning in Medicine 2009; 21(3): 220-224.
47. Critchley J, DeWitt D, Khan M, Liaw S. A required rural health module increases students' interest in rural health careers. Rural and Remote Health 7: 688. (Online) 2007. Available: www.rrh.org.au (Accessed 12 February 2012).
48. Blue I, Fitzgerald M. Interprofessional relations: case studies of working relationships between registered nurses and general practitioners in rural Australia. Journal of Clinical Nursing 2002; 11(3): 314-321.
49. Zur O. Therapeutic boundaries and dual relationships in rural practice: ethical, clinical and standard of care considerations. Journal of Rural Community Psychology 2006; E9(1): 1-40.
50. Roberts LW, Battaglia J, Epstein RS. Frontier ethics: mental health care needs and ethical dilemmas in rural communities. Psychiatric Services 1999; 50(4): 497.
51. Campbell CD, Gordon MC. Acknowledging the inevitable: understanding multiple relationships in rural practice. Professional Psychology: Research and Practice 2003; 34(4): 430-434.
52. Worley P, Strasser R, Prideaux D. Can medical students learn specialist disciplines based in rural practice: lessons from students' self-reported experience and competence. Rural and Remote Health 4: 338. (Online) 2004. Available: www.rrh.org.au (Accessed 12 February 2012).
53. Ewen S, Mazel O, Knoche D. Exposing the hidden curriculum influencing medical education on the health of Indigenous people in Australia and New Zealand: the role of the critical reflection tool. Academic Medicine 2012; 87(2): 200-205.
54. Roberts JH, Sanders T, Mann K, Wass V. Institutional marginalisation and student resistance: barriers to learning about culture, race and ethnicity. Advances in Health Sciences Education 2010; 15(4): 559-571.
55. Augoustinos M, Tuffin K, Sale L. Race talk. Australian Journal of Psychology 1999; 51(2): 90-97
56. Biggs JSG, Wells RW. The social mission of Australian medical schools in a time of expansion. Australian Health Review 2011; 35(4): 424-429.
57. Seeleman C, Selleger V, Essink-Bot M-L, Bonke B. Teaching communication with ethnic minority patients: ten recommendations. Medical Teacher 2011; 33(10): 814-819.
58. Reid SJ. Pedagogy for rural health. Education for Health 2011; 24(1): 536.
59. Paradies YC. Beyond black and white essentialism, hybridity and indigeneity. Journal of Sociology 2006; 42(4): 355-367.
60. Onemda VicHealth Koori Health Unit, Medical Deans Australia and New Zealand. Critical Reflection Tool. (Online) 2007. Available: http://www.limenetwork.net.au/files/lime/Interactive_CRT_FINAL.pdf (Accessed 7 November 2012).
61. Pedersen A, Walker I, Paradies Y, Guerin B. How to cook rice: a review of ingredients for teaching anti-prejudice. Australian Psychologist 2011; 46(1): 55-63.
62. Downing R, Kowal E, Paradies Y. Indigenous cultural training for health workers in Australia. International Journal for Quality in Health Care 2011; 23(3): 247-257.
63. Wing L. The 'Australian rural health education revolution'. Australian Journal of Rural Health 2007; 15(6): 344-345.

