One of the leading causes of disability in the USA and Canada is mental health disorders, which accounts for 25% of all years of life lost to disability and premature mortality1. The National Institutes of Mental Health (NIMH) estimates approximately 1 in 17 American adults have a seriously debilitating mental illness2. Mental illnesses are health conditions that are distinguished by changes in thinking, mood or behavior, or any combination thereof, associated with distress and/or impaired functioning3. The majority of people who experience a mental illness do not die by suicide; however, of those who do commit suicide, more than 90% have a diagnosable disorder4. People who die from suicide are frequently experiencing undiagnosed, undertreated, or untreated depression5. As of 2008, suicide was the tenth leading cause of death in the USA6.
As concern regarding mental health (MH) issues arise throughout the USA, the situation may be worse for those who live in rural communities. Major depression rates in some rural areas significantly exceed those in urban areas7, and teens and older adults in rural areas have significantly higher suicide rates than their counterparts in urban areas8. Though there is a demand for more MH services to be made available for those in rural areas, there are many obstacles that prevent rural Americans from receiving necessary mental healthcare treatment. These obstacles revolve around issues of availability and accessibility. In many rural areas, MH services are simply not available9. In fact, more than 85% of the 1669 federally designated MH professional shortage areas are rural10. The National Advisory Committee on Rural Health11 found that there were entire counties in rural America with no practicing psychiatrists, psychologists, or social workers10.
Because of the scarcity of health services in rural areas, it is no surprise that distance to MH providers and a lack of public transportation to reach care can prevent rural people from accessing MH services9. However, ever when care may be available there are other barriers that prevent individuals from accessing mental healthcare. One barrier that exists is the social stigma that is attached to MH issues. This stigma combined with a general lack of anonymity in small rural communities leads some people to not seek treatment9. Furthermore, one of the greatest barriers to accessing mental healthcare services in rural America is the lack of affordable and meaningful health insurance coverage9. Mental healthcare is largely unaffordable because most rural Americans are less likely to have health insurance that covers mental or behavioral health services compared with their urban counterparts11.
Studies from the Department of Health and Human Services, American Psychological Association, National Association for Rural Mental Health, and other sources have indicated that rural communities generally have fewer MH services and professionals than their urban counterparts12-15. A national study of workforce issues regarding rural health professionals indicates major gaps and shortages exist in the rural healthcare workforce16. Among the rural hospital CEOs responding to this prior study, almost 46% indicated the need for psychiatrists and 28% indicated the need for psychologists in their communities. The current study examined the perceived shortages of MH professionals in rural communities as well as the impact of inadequate MH service access on rural hospitals, especially their emergency departments (EDs).
The overall objective was to examine the extent and impact of shortages of MH professionals on the community and rural hospitals. Specifically, the characteristics regarding access to MH services including distance to services, wait time, and perceived need for a variety of mental healthcare providers were assessed. The differences in insured or private pay versus Medicaid and uninsured access by community residents were also examined to help inform policy related to reimbursement. Finally, unique difficulties faced by rural areas were evaluated to begin to explore ideas for solving or ameliorating these problems.
Design
This descriptive study employed a cross-sectional mailed survey design. A two-page survey was mailed to each hospital CEO with follow up performed using the Dillman Total Design Method, seeking to maximize the response rate17. This method includes sending an initial questionnaire with a postage-paid return envelope, a follow-up reminder postcard one week later, and finally sending an additional copy of the survey 4 weeks after the initial mailing.
Sample
A sample frame of 1162 rural hospitals in the USA was compiled with rurality determined based on United States Department of Agriculture (USDA) Rural-Urban Commuting Area (RUCA) codes18. The RUCA codes are designed to define the level of rurality based on census information. Attributes taken into account include population density, proximity to a metropolitan area, and commuting patterns. All rural hospitals in this study were located in a ZIP code with a RUCA code of 4 or greater. Of those in the target population, 56.8% were in a designation of Very Rural (≥ RUCA code 6). The current CEO for each rural hospital was then identified and mailed the two-page survey. All respondents were contacted at least three times seeking response to the survey questions.
Measures
The survey included several types of questions, including distance to referral center and wait time at hospitals, and the number of various MH professionals that were needed. Using Likert-scale questions, community sentiment towards MH professionals and how well needs were being met by the current number of professionals were assessed. Open-ended questions about what makes the hospital's area unique, as well as questions regarding the major barriers to mental healthcare and how these barriers might be overcome, were also included. Finally, demographic questions regarding the hospital, town, state and ZIP code were included.
Data analysis
As the surveys were returned, they were assigned a reference number, and entered into SPSS v17 (www. SPSS.com). After 6 months of collecting surveys, data collection was complete and data analyzed using SPSS v17. Frequency distributions, comparison of means and cross-tabulations were used in the analysis.
Ethics approval
This research was approved by the University of Illinois College of Medicine at Rockford IRB, Rockford, Illinois (approval no. 20070048).
A total of 228 surveys were collected of the 1162 sent out (response rate 19.6%). Responses were received from 30 of the 50 US states. Primary care shortage status and rurality was similar among the sample frame and respondents with 56.5% of the sample frame being located in a Very Rural area (≥ RUCA code 6) in comparison with 59.3% of responding hospitals being in a Very Rural area. Likewise, the percentage of hospitals located in a primary care shortage area comparing sample frame hospital to respondent hospitals was similar, 42.6% and 42.0%, respectively. Hospital CEOs were surveyed due to the lack of MH providers in rural areas. In this way, the viewpoint of those surveyed was standardized.
Over 90% of CEOs reported that patients travel more than 32.2 km (20 miles) for a mental healthcare referral, and over 50% reported that patients have to travel approximately 96.5 km (60 miles) or more for a MH service referral. The CEOs also reported that a larger proportion of patients living in very Rural Areas (≥ RUCA code 6) must travel more than 96.5 km (60 miles) than patients living in a less rural areas, as is shown (Fig1). The reported distance patients traveled for a MH referral differed significantly between Rural and Very Rural areas (χ2 = 14.417, df = 4, p = .006).
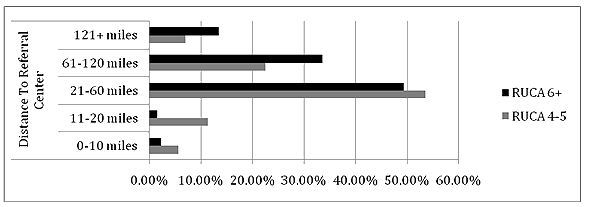
Figure 1: Distance to referral center. RUAC, Rural-Urban Commuting Area Code.
The reported distance patients traveled for a MH referral differed significantly
between Rural and Very Rural areas (χ2 = 14.417, df = 4, p = .006).
When asked if there was a shortage of mental healthcare professionals in their area, CEOs overwhelmingly reported (approximately 90%) that there is a shortage of mental healthcare providers. Indicators of shortage used for the purposes of this study were the time taken for a patient/client to receive an appointment and the distance travelled to access care. 'Shortage' was defined as patients/clients having to wait for an appointment more than 30 days or travel more than one hour for care. The CEOs from both Rural and Very Rural areas showed consistent results, with approximately 90% reporting a shortage (Fig2). No statistically significant difference was observed between Rural and Very Rural areas (χ2 = 0.386, df = 2, p = .824).
The CEOs were asked about the average wait time for mental healthcare to be provided in EDs. More than 50% of the CEOs reported that patients have to wait over one hour to be seen for MH-related complaints in EDs (Fig3). There were no statistically significant differences in wait time between Rural and Very Rural areas (χ2 = 4.135, df = 5, p = .530).
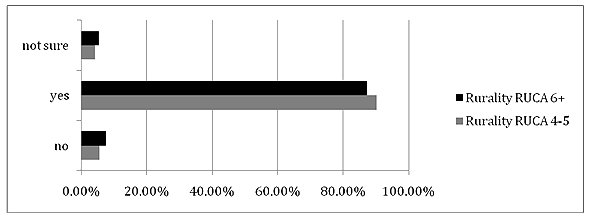
Figure 2: Results of question: 'Is there a shortage of mental health professionals in your area?'
RUAC, Rural-Urban Commuting Area Code. No statistically significant difference
was observed between Rural and Very Rural areas (χ2 = 0.386, df = 2, p = .824).

Figure 3: Average wait time in emergency departments. RUAC, Rural-Urban Commuting Area Code.
No statistically significant difference was observed between Rural and Very Rural areas (χ2 = 4.135, df = 5, p = .530).
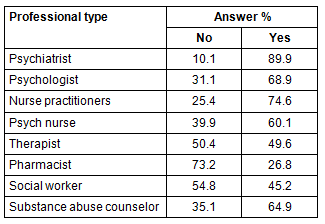
The CEOs were then asked about the number of additional MH professionals needed in the community. Based on mean number needed, the highest reported needs were for psychiatric nurses, substance abuse counselors, nurse practitioners, and psychiatrists. Pharmacists had both the lowest average and highest maximum reported number needed. The mean number of MH professionals reported as needed by a community was 18 (range 1-34) (Table 1). Surveys also asked if people currently have difficulty getting a visit with these types of MH professionals. Almost 90% of respondents stated that people have difficulty making an appointment with psychiatrists. The majority of respondents also stated there is difficulty making an appointment with psychologists, nurse practitioners, and substance abuse counselors. Respondents were about equally divided (between 'yes' and 'no') as to whether there was difficulty in making appointments with psychiatric nurses, social workers, and therapists. In any given community, there was a 50% or more reported difficulty in getting an appointment with six of the eight different types of MH professionals (Table 2). For five of the eight professions the number needed was significantly higher (p <.05) in Rural areas than in Very Rural areas.
Respondents were asked if there was a shortage of these same professions within a 48.3 km (30 mile) radius. Just over two-thirds of the CEOs clearly indicated that there is a shortage of psychiatrists, nurse practitioners, psychologists, and substance abuse counselors. Shortage was again defined as patients/clients having to wait for an appointment more than 30 days or travel more than one hour for care. As is shown (Table 3), respondents were less likely to agree that there was a shortage of pharmacists (26%) or social workers (45%).
Table 1: Number of mental health professionals needed
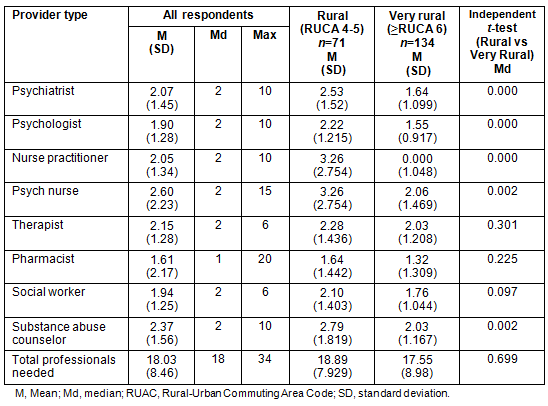
Table 2: Results of question, 'Do people have difficulty getting
an appointment with this type of mental health professional?'
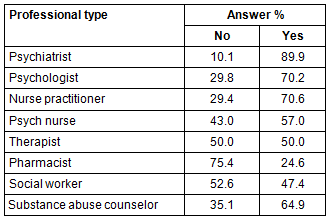
Table 3: Results of question, 'Is there a shortage
of this profession within a 48.3 km (30 mile) radius?'
The survey asked a series of Likert-scaled questions regarding MH professionals in the area. Based on average ratings, respondents agreed that psychiatrists are well respected, and that there is a large need for MH professionals in their areas. They disagreed that it is easy to recruit psychiatrists, or other MH professionals, in their area. There is a statistically significant (p < .05) difference between Rural and Very Rural areas regarding their rating of difficultly in recruiting other MH professionals, with Very Rural respondents reporting more difficulty.
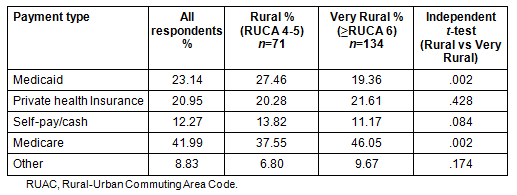
The CEOs were asked about their patients' sources of payment, which was then divided into 'rural' and 'very rural' groups. Among all respondents, 23.1% used Medicaid, 21.0% private health insurance, 12.3% self-pay or cash, and 42.0% Medicare. All other forms of payment made up 8.8%. A significant difference (p= .002) was found between Rural and Very Rural respondents in use of both Medicaid and Medicare (Table 4). Rural respondents were more likely to use Medicaid than Very Rural respondents (27.5% vs 19.4%), and Very Rural respondents were more likely to use Medicare than Rural respondents (46.1% vs 37.6%).
Table 4: CEOs' responses as to patients' sources of payment
The survey also included open-ended questions. The first asked about major issues that CEOs thought impacted the mental health of area residents. The most common answers were lack of funding, resources, and infrastructure (39% of respondents answered ≥ one of these). The CEOs also noted inability to pay, because of unemployment, poverty, low income, local economy, or lack of insurance coverage (35% answered ≥ one of these). Drug/alcohol abuse (28%) and lack of MH professionals in the area (22%) were also common. Other problems included lack of communication/help from the state, high suicide rates, high pregnancy rates, homelessness, stigma against MH, low education generally, low education in regard to MH, and ongoing care and treatment. It should be noted that most CEOs indicated multiple concomitant problems, not just a single problem.
The next open-ended question asked what other characteristics were common in the CEOs' area. Many CEOs reported absolutely no MH services (15%), and absolutely no MH professionals (26%). The reasons given for this included lack of reimbursement, lack of incentives to draw providers, and turnover. Extremely long waits for care in EDs were also reported (8%). Other problems included lack of MH training for staff, lack of beds for MH patients, lack of state/federal funding, and non-English speaking populations. Many respondents said telehealth services would be viable in their area. Again, most CEOs indicated multiple responses, not just a single response.
Finally, respondents were asked what they would like to improve or change. Nearly one-third (32%) would like an increase in support/funding in order to increase recruitment and retention; 42% would like to see better pay or incentives such as debt forgiveness for rural MH professionals (ie the repayment of educational loans based on time served in a shortage area after professional training). Other ideas included increased treatment services available for low income or low insurance patients, using telehealth to increase coverage, and increased or improved facilities.
Discussion
Over one-half of CEO respondents indicated there is at least a 60 min wait when patients seek care. Only 10% have a referral center within 32.2 km (20 miles), and almost 50% of the Very Rural CEO respondents were further than 96.5 km (60 miles) away from the nearest referral center. The longest most people are willing to travel is about 60 min from home19; therefore, it is likely that many patients do not obtain mental healthcare as often as they should, or perhaps not at all.
At least 60% of the CEOs indicated there was a shortage of one or more types of MH professionals in their area. The most needed included psychiatrists, psychologists, psychiatric nurses, and substance abuse workers. While most CEOs reported slight agreement that psychiatrists are well respected in their area, they also strongly agreed that it is difficult to recruit them. They agreed that recruiting other MH professionals is difficult, though not to the extent as for psychiatrists. The highest rating on the Likert questions was that MH professionals are greatly needed in these areas. This rating indicates that the shortage of MH professionals in rural areas is not confined to one area, but is common throughout rural areas of the USA12.
Payment methods were somewhat similar in both Rural and Very Rural areas regarding the general distribution of payment type. In Very Rural areas (≥ RUCA 6), Medicare was significantly more common than in Rural areas (RUCA 4 or 5), and Medicaid was significantly less common as a payment mechanism. This is consistent with the high usage of Medicare for payment among residents in Rural areas, as has been shown previously20,21.
There are potential solutions for many of these problems. Telepsychiatry has been suggested as an option for increasing rural MH service access22. This would involve professionals in distant areas using video conferencing to communicate with patients. Patients and primary care physicians both agree that telehealth is an excellent option if local MH providers are not available23. Rural psychiatry residencies could be an option24. Having a residency specific for rural areas would guarantee an influx of mental healthcare workers. Another idea is to expand prescribing power for certain classes of psychoactive medications to other healthcare professionals such as primary care physicians, nurse practitioners, or physician assistants who have been trained to provide basic mental healthcare. Access by these other healthcare providers to consultation with a psychiatrist would be important to ensure quality of care. Previous research found the largest shortages (as here) were in psychiatry, so expanding prescribing power could alleviate the shortage25. Finally, the use of e-screening could allow for more mental healthcare availability26. Screening is the first step of secondary prevention, and because of its effectiveness in reducing overall expenditures, screening has been identified as a preventative healthcare intervention that should be promoted27. Because of the shortage of medical professionals and fewer health services available in rural communities, screening becomes especially important28-30. A pilot study investigating the use of electronic screening for MH in a rural primary care setting indicated that subjects found the e-screening useful26. The technology used was a computer with touch-screen and audio-assisted technology that 90% of subjects found to be an easy to use system26. This tool provided a printout of the e-screening results to both the patient and the healthcare provider which increased the power of intervention to inform clinical practice26. It was found that the e-screening tool was an acceptable and effective means of screening for depression in a rural population26.
Limitations
The limitations of this study must be noted. Of the 1162 CEOs who were sent surveys, 228 responded (19.6% response rate) and thus the results may not be representative of the target population. However, based on primary care shortage designation and rurality the respondents appear similar to the target population. The sample frame for the current study on MH service topics was used previously in conducting a more general study about rural workforce issues and this may have reduced the response rate. Given that mental healthcare services are not a major focus of service for many rural hospitals and the same hospitals had been surveyed the prior year, the response rate was likely reduced. As mentioned earlier, this study followed the Dillman Total Design Method as closely as possible within the constraints of the design to maximize the response rate. It is recommended that future mailed surveys of rural hospital CEOs seek to involve endorsement and cover letters from state hospital associations in an effort to increase response rates. An incentive or chance at a reward could also be offered for responding.
Second, this study was important because it focused on hospital CEOs who are knowledgeable about their hospital's and the surrounding community's needs. However, future studies should be conducted based on views of other health practitioners, providers or consumers, in order to create a more complete understanding of mental healthcare shortages.
Overall, many rural people are not receiving care because of what is viewed as excessive travel distances and wait time. Many rural areas reported a great need for more MH professional recruitment and retention as well as funding, resources, and infrastructure improvements. Many rural areas across the USA have major problems with unemployment, depression, and substance abuse. Most areas see solutions as larger recruitment and financial incentives, and several want to be able to offer alternative modes of treatment such as using telehealth.
References
1. World Health Organization. The world health report 2004: changing history. Annex Table 3: Burden of disease in DALYs by cause, sex, and mortality stratum in WHO regions, Estimates for 2002; A126-A127. Geneva: WHO, 2004.
2. Kessler RC, Chiu W, Demler O, Merikangas KR, Walters EE. Prevalence, severity, and comorbidity of twelve-month DSM-IV disorders in the National Comorbidity Survey Replication. Archives of General Psychiatry 2005; 62(6): 617-627.
3. US Census Bureau, Population Division. US Census Bureau population estimates by demographic characteristics: National population estimates - characteristics. Table 2 (NC-EST2004-02): Annual estimates of the population by selected age groups and sex for the United States: April 1, 2000, to July 1, 2004; A18. Washington: US Census Bureau, 2005.
4. US Department of Health and Human Services. Mental health: a report of the Surgeon General. Rockville, MD: US Department of Health and Human Services, 1999.
5. University of Washington. Mental health reporting. Online (2012). Available: http://depts.washington.edu/mhreport/facts_suicide.php (Accessed 20 June 2012).
6. Minino AM, Murphy SL, Xu J, Kochanek KD. Deaths: Final Data for 2008. National Vital Statistics Reports 2011; 59(10): 01-127. Available: http://www.cdc.gov/nchs/data/nvsr/nvsr59/nvsr59_10.pdf (Accessed 25 September 2012).
7. Probst JC, Laditka S, Moore CG, Harun N, Powell MP. Depression in rural populations: prevalence, effects on life quality and treatment-seeking behavior. Rockville, MD: Office of Rural Health Policy, US Department of Health and Human Services, 2005.
8. Goldsmith SK, Pellmer TC, Kleinman AM, Bunney WE (Eds). Reducing suicide: a national imperative. Washington, DC: National Academy Press, Institute of Medicine, 2002.
9. Gustafson DT, Preston K, Hudson J. Mental Health: overlooked and disregarded in rural America. (Online) 2009. Available: http://files.cfra.org/pdf/Mental-Health-Overlooked-and-Disregarded-in-Rural-America.pdf (Accessed 25 September 2012).
10. Anon. New Freedom Commission on Mental Health. Subcommittee on Rural Issues: background paper DHHS Pub no SMA-04-3890. Rockville, MD: Substance Abuse and Mental Health Services Administration (SAMHSA), 2004. Available: http://www.annapoliscoalition.org/resources/1/President%27s%20New%20Freedom%20Commission%20Background%20Paper.pdf (Accessed 25 September 2012).
11. Sawyer D, Gale J, Lambert D. Rural and frontier mental and behavioral health care: barriers, effective policy strategies, best practices. Waite Park, MN: National Association of Rural Mental Health, 2006. Available: http://www.narmh.org/publications/archives/rural_frontier.pdf (Accessed 25 September 2012).
12. American Psychological Association. The critical need for psychologists in rural America. (Online) no date. Available: http://www.apa.org/about/gr/education/rural-need.aspx (Accessed 27 June 2012).
13. Fox J, Merwin E, Blank M. De facto mental health services in the rural South. Journal of Healthcare for the Poor and Underserved 1995: 6(4): 434-468.
14. Lambert D, Donahue A, Mitchell M, Strauss R. Mental health outreach: promising practices in rural areas. Waite Park, MN: National Association for Rural Mental Health, 2001. Available: http://www.narmh.org/publications/archives/REVISED_OUTREACH_PAPER.pdf (Accessed 25 September 2012).
15. Mohatt D, Adams S, Bradley M, Morris C. Mental Health and Rural America: 1994-2005. Rockville, MD: US Department of Health and Human Services, Health Resources and Services Administration Office of Rural Health Policy, 2006. Available: ftp://ftp.hrsa.gov/ruralhealth/RuralMentalHealth.pdf (Accessed 25 September 2012).
16. MacDowell M, Glasser M, Fitts M, Nielsen K, Hunsaker M. a national view of rural health workforce issues in the US. Remote and Rural Health 10: 1531. (Online) 2010. Available: www.rrh.org.au (Accessed 26 June 2012).
17. Hoddinott S, Bass M. The Dillman total design survey method. Canadian Family Physician 1986; 32: 2366-2368.
18. United States Department of Agriculture, Economic Research Service. Rural-Urban Commuting Area Codes. (Online) no date. Available: http://www.ers.usda.gov/topics/rural-economy-population/rural-classifications.aspx (Accessed 26 June 2012).
19. Fortney JC, Owen R, Clothier J. Impact of travel distance on the disposition of patients presenting for emergency psychiatric care. Journal of Behavioral Health Services Research 1999; 26: 104-108.
20. Hartley D, Loux S, Gale J, Lambert D, Yousefian A. Characteristics of inpatient psychiatric units in small rural hospitals. Psychiatric Service 2010; 61(6): 620-623.
21. Wagenfeld M, Stamm O, Hudnall B (Eds). A snapshot of rural and frontier America. rural behavioral health care: an interdisciplinary guide. Washington, DC: American Psychological Association, 2003; 33-40.
22. Gabel S. Telepsychiatry, public mental health, and the workforce shortage in child and adolescent psychiatry. Journal of the American Academy of Child and Adolescent Psychiatry 2009; 48(11): 1127-1128.
23. Swinton JJ, Robinson WD, Bischoff RJ. Telehealth and rural depression: physician and patient perspectives. Families, Systems, and Health 2009; 27(2): 172-182.
24. Gillig PM, Comer EA. A residency training in rural psychiatry. Academic Psychiatry 2009; 33(5): 410-412.
25. Thomas KC, Ellis AR, Konrad TR, Holzer CE, Morrissey JP. County-level estimates of mental health professional shortage in the United States. Psychiatric Service 2009; 60(10): 1323-1328.
26. Farrell SP, Mahone IH, Zerull LM, Guerlain S, Akan D, Hauenstein E et al. Electronic screening for mental health in rural primary care: implementation. Issues in Mental Health Nursing 2009; 30(3): 165-173.
27. Farrel SP, Zerull LM, Mahone IH, Guerlain S, Akan D, Hauenstein E et al. Electronic screening for mental health in rural primary care: feasibility and user testing. Computers, Informatics, Nursing 2009; 27(2): 93-98.
28. Rosenblatt RA, Hart LG. Physicians and rural America. Western Journal of Medicine 2000; 173(5): 348-351.
29. Patrick JH, Johnson JC, Goins RT, Brown DK. The effects of depressed affect on functional disability among rural older adults. Quality of Life Research 2004; 13: 959-967.
30. Ricketts TC. Health care in rural communities. Western Journal of Medicine 2000; 173: 294-295. ___________________________
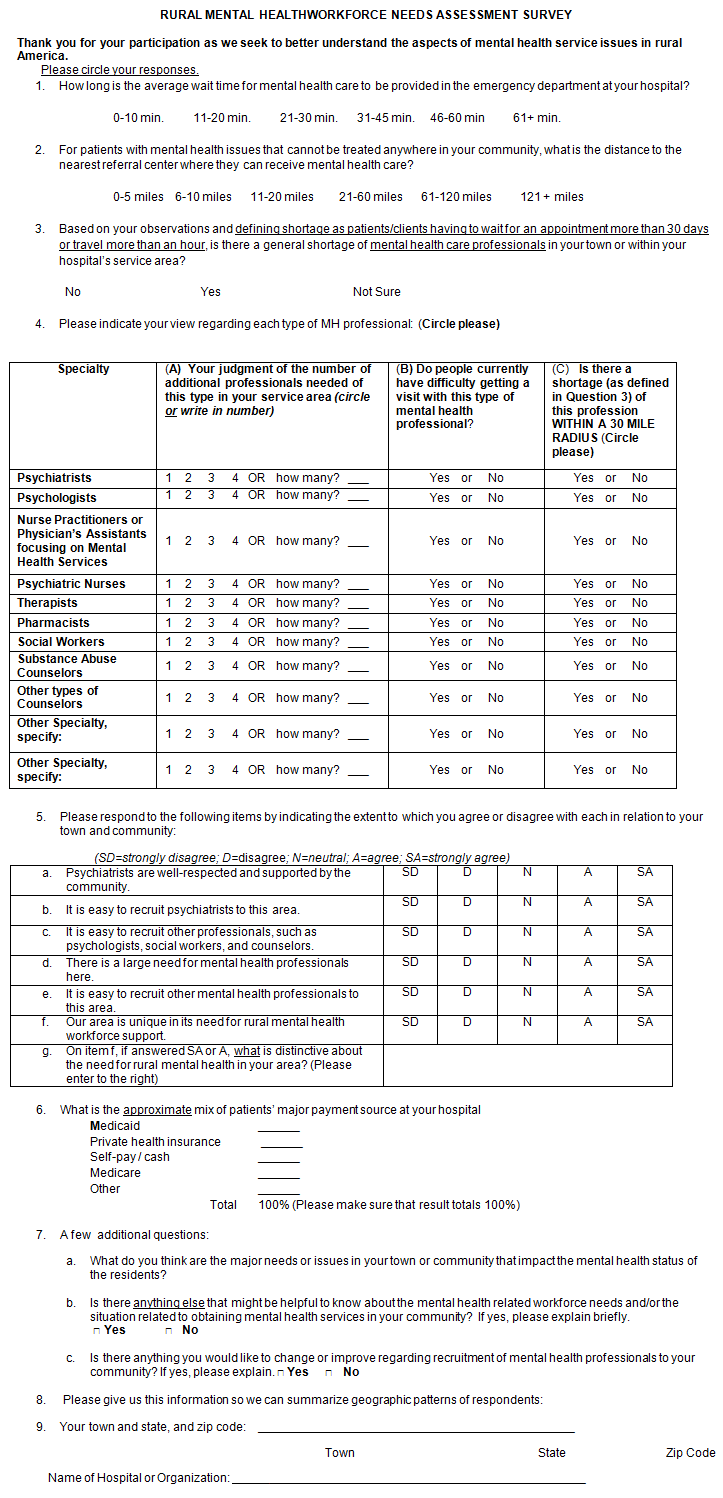
Appendix I: Rural Mental Healthworkforce Needs Assessment Survey