In 2006, the suicide rate for Australia as a whole was 8.9/100 000 people1. The Northern Territory (NT) of Australia had a suicide rate of 13/100 000 people, well above the national average1. 'Based on the revised Accessibility/Remoteness Index of Australia (ARIA+), a nationally consistent measure of geographic remoteness, most of the NT falls within the classifications of 'remote' and 'very remote', with even the capital Darwin being classified as 'moderately accessible' in contrast with all other Australian metropolitan centres. The NT has a larger proportion of the population living in rural areas, and it has a much higher proportion of Indigenous people (25%) compared to the national average (<4.0%). Demographically, the NT has a younger population, with a median age of 31.3 years compared with the national median age of 36.8 years.
The life expectancy of Australian Indigenous people is 17 years shorter than the national average2. The 2006 Australian Bureau of Statistics figures reveal that nationally, suicide accounted for 4.9% of Indigenous deaths and 1.8% of non-Indigenous deaths1. A study of the NT data for the years 2001-2006 found a non-Indigenous suicide rate of 14.7 and an Indigenous suicide rate of 36.7 (which is 2.5 times the local non-Indigenous rate and four times the national average)3. Similar results have been found in Queensland for the years 1999-2007, with the Indigenous rate being 2.2 times higher than it was for non-Indigenous people4.
Indigenous peoples of many - but not all5 - other countries, including Canada6, Greenland7, New Zealand8, Norway9, the USA10 and Taiwan11, have high suicide rates. These situations have been described as the result of anomie, when the social integration and regulation of society begins to fail12. Another explanation is 'acculturation', which occurs when a culture encounters a dominant alternative culture and there is extreme pressure for physical, biological, political, economic, cultural, social and psychological change13.
The suicide rate among Indigenous Australians began to rise dramatically in the 1970s14. A number of explanatory factors have been proposed that note some distinctive features of Indigenous suicide15 and recognise the impact of political and cultural factors, the legacies of colonialism, chronic unemployment and alcohol and drug use, along with a range of other disadvantages16. This 'specialness' of Australian Indigenous suicide has been challenged17, but the myriad cultural, social and economic difficulties remain18.
In more general circumstances, risk factors for suicide include mental / psychiatric disorders19; however, the importance of these factors has recently been challenged, namely in studies from China, which note mental disorder in less than half the young people who complete suicide20, and India, which identify mental illness in only 37% of completed suicides21. It would appear that adverse events increase suicide risk, independent of any mental disorder19,22,23, and that relationship conflict and separation are particularly powerful24. Further, poverty25, unemployment26, exposure to violence and hunger27, and even factors such as being born to a younger mother28 or a mother in an unstable marital relationship29 also increase risk. While links between rurality and suicide risk are unclear30-33, it is recognised that this important issue would benefit from enhanced levels of conceptualisation34.
Some key conceptualisations have recently arisen from rural suicide research. In rural China a 'strain theory of suicide' has been suggested35 and in rural Scotland a model of self-injury and suicide noting the 'cry of pain/entrapment' has been proposed34. In Australia, a 'predicament model' has been proposed in which suicide is seen as an escape mechanism from painful circumstances, which may include untreated or unresponsive mental disorder, social circumstances or a combination of both36.
The current study is based on the understanding that suicide usually occurs in the context of several compounding social, contextual and psychological factors, and that these require further research and elaboration37,38. It follows the premise that the most appropriate methods for investigating such complex factors are mixed qualitative and quantitative methods. One such method, the 'sociological autopsy', has been described in which the information in coroners' files is used to develop an integrated understanding of suicide24. A sociological autopsy using coroners' reports found mental disorder in almost two-thirds of 100 UK completers, while in more than half of all cases relationship problems were identified and in one-third of cases these problems were believed to be the main trigger for suicide39.
The aim of the current project was to conduct a quantitative and qualitative thematic exploration of coronial information to identify factors associated with completed Indigenous and non-Indigenous suicides in the rural NT over approximately one decade. It is noted that in the NT all unexpected deaths are investigated by the coroner. Generally, the coroner reviews the post-mortem reports from a forensic pathologist, the toxicology analysis and police reports including circumstances surrounding the death. Police typically will have interviewed anyone who might be able to assist with information around the circumstances of the death, including family members, friends and work colleagues. Reports include police interactions with the deceased prior to the event, evidence of the deceased making statements of intention to others and information from others regarding the deceased's mood, state of mind, level of intoxication and other relevant matters. Formal public inquests are occasionally held in specific circumstances such as deaths in police custody or death of 'a person in care' while in hospital.
The sample of coronial reports used for this research was from the national Internet-based data storage and retrieval system for Australian coronial cases, the National Coroners Information System (NCIS). The full complement of reports from the Northern Territory was included in which the coroner had determined that the cause of death was as a result of intentional self-harm and where an electronic record of the coroners' findings was available. To avoid ambiguity and exclude potential non-suicide cases recorded as 'undetermined cause', only cases where 'intentional self-harm' was determined by the coroner were retrieved and analysed. The timeframe of deaths reported was between July 2000 and December 2010.
In total 411 reports met these criteria and were included, consisting of 198 Aboriginal and/or Torres Strait Islander cases and 213 non-Indigenous cases. Electronic copies of the coronial reports were downloaded as Portable Document Format (PDF) files (Adobe; www.adobe.com) into separate Indigenous and Non-Indigenous folders. These folders were then imported into QSR NVivo Qualitative Data Analysis Software v8 for structured thematic analysis (www.qsrinternational.com). To avoid bias in coding over time, files were analysed year by year but not in chronological order. Also, the order of coding was alternated between Indigenous and non-Indigenous cases.
A qualitative thematic analysis was undertaken of each case report to identify factors noted by coroners that led to each suicide and the possible cause of the person taking their own life. This was an inductive process and due to the nature of the data (standardised coronial reports and not personal communication), identified issues were coded once for each report to quantify the presence of the underlying issues present in all cases24. The categorised themes were also summarised numerically.
To ensure consistency of coding and maximise efficiency, one researcher extracted and coded all data. To ensure quality of coding and as a verification of the accuracy of coding, all three researchers met to discuss (i) the coding process (tracing data from reports to themes) and (ii) the content of themes (to validate the accuracy of coding). Consensus was established in the form of agreement across researchers to verify the coding process. All reports were analysed by one researcher (JA).
Ethics approval
Ethics approval was obtained, consistent with National Coronial Information Service requirements: Victorian Department of Justice - Human Research Ethics Committee (CF/10/3519), with additional Indigenous ethical review.
Findings in the current study are presented in numerical form, in figures and a table, and in text form, as quotes at relevant points, to represent the nature of statements in coroners' reports. De-identified excerpts of the reports are coded as follows after each quote (Indigenous status / gender / year and case number).
Demographic overview
The experimental estimated resident Indigenous population of the NT at 30 June 2006 was 64 000 people, or 30% of the total NT population. As noted, the total number of suicides among Indigenous people and among non-Indigenous people in the current sample is almost equal. With 30% of the population accounting for over 48% of the suicides, the current study confirms earlier findings that the Indigenous population is highly over represented in the suicide statistics in the NT3.
This sample was predominately male: males comprised 88% of Indigenous and 86% of non-Indigenous suicides (Table 1). These data confirm that suicide is clearly a gendered issue34,40. In keeping with data from rural and remote areas elsewhere, male suicides far outweighed female in the current sample, but to an even greater extent40. However, it is noteworthy that the gendered nature of suicide in the NT was reflected similarly across Indigenous and non-Indigenous cases.
Table 1: Demographics of sample
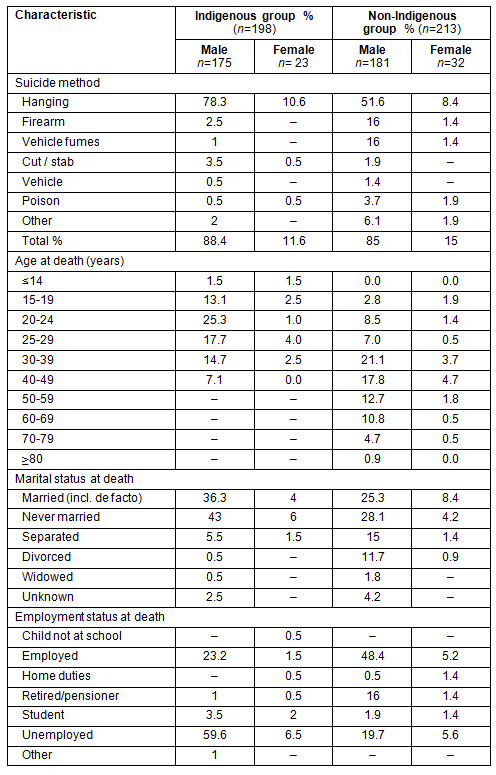
Hanging was the primary means of suicide, with the Indigenous group much more likely to use this method than the non-Indigenous group (89% Indigenous, 60% non-Indigenous). In contrast with relatively high rates of firearm-related suicides reported in rural areas, in this sample 17% of non-Indigenous coroners' cases died using a firearm but only 3% of Indigenous cases32. The age at death was substantially younger for the Indigenous sample. There were similar percentages across those who were married or in de-facto relationships as those never married in both Indigenous and non-Indigenous groups.
The age at death of the different groups is also provided, reflecting that the peak incidence of suicide was much younger in the Indigenous population (age 20-24 years) than in the non-Indigenous population (age 30-39 years; Table 1).
Relative proportions of factors associated with suicide
With regard to the thematic analysis of factors associated with suicide, while the current study identified many factors across 411 coroners' reports, the key factors that were linked with the suicides in the thematic analysis were the presence of alcohol and other drugs, conflict and relationship breakdown, and indication of mental health issues. The relative proportions of these are depicted (Fig1). Other factors that were less frequently reported, and less clearly associated with the suicide event, are also described further in this article.
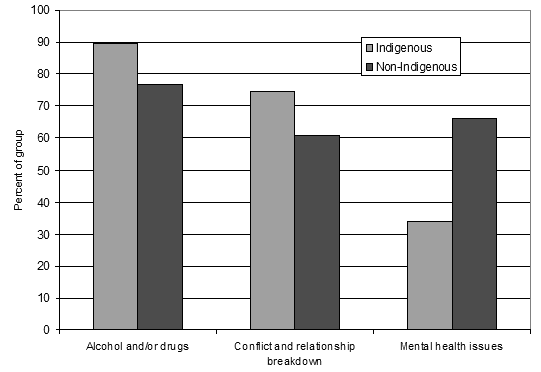
Figure 1: Relative proportions of key factors associated with suicide
Presence of alcohol and drugs
Coronial reports in this sample routinely included results of toxicological analysis including levels of alcohol and cannabinoids from blood and/or urine samples. Indicators of prescription or illegal drugs, over the counter medications or carbon monoxide metabolites were also reported. Where no toxicology information was provided, but other parts of the report indicated clear evidence of alcohol, cannabis, inhalant or other drug use associated with the suicide, these were also coded. For example:
The Deceased, his wife and a small group of friends were at [place], where they had been drinking very heavily and most of them were very intoxicated. The group started drinking inside the premises and then went out to the front yard to continue drinking. (I/M/2001.51)
Alcohol was either present in the blood or alcohol abuse was mentioned in 261 (64%) of all suicide reports (72% of Indigenous and 55% of non-Indigenous cases) (Fig2). Of these, 61% of Indigenous cases and 33% of non-Indigenous cases had a blood alcohol level greater than 0.05% at the time of death.
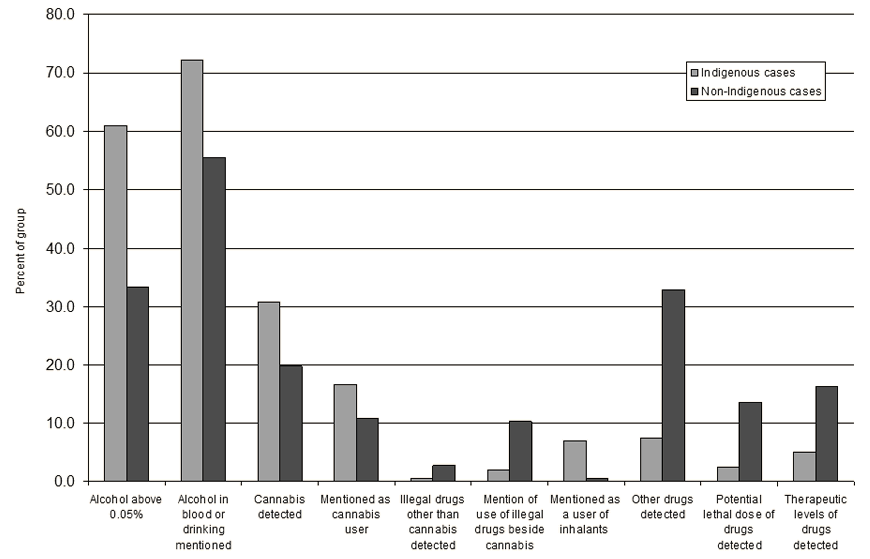
Figure 2: Presence of alcohol and drugs at time of death, or substance use mentioned
These results align with other published research41 and given that such substance abuse heightens suicide risk, influencing inhibition and impulsive behaviour42, it would appear that chronic abuse of alcohol has substantial influence on suicide rates, particularly for Indigenous people. This further indication of the association between alcohol abuse and suicide should inform policy and public health debates in rural remote and Indigenous contexts such as the NT.
Cannabis was formally detected in 31% of Indigenous and 20% of non-Indigenous cases (and generally noted as a factor in 17% and 11% of case reports, respectively). These results are consistent with earlier studies noting the role of cannabis in 30% of young Indigenous suicide cases and 20% of older adult suicides43. As with alcohol, high cannabis use is associated with increased suicidal ideation, particularly in Indigenous communities44.
In keeping with recent research in Queensland, the reverse pattern was present for illegal drugs (other than cannabis), which were identified in 0.5% Indigenous and 2.8% of non-Indigenous cases4. Prescription and over-the-counter medicines were detected in 8% and 33% of cases, respectively, and potentially lethal levels of drugs/substances were detected in 2.5% and 14% of cases.
Such differences between Indigenous and non-Indigenous cases may be related to differences in a number of factors including historical patterns, availability, social acceptability, remoteness, and physical and financial access to medical services, prescription medicines and illegal drugs. However, the number of cases linked with alcohol as a contributing factor would indicate that addressing alcohol abuse should be a key factor in suicide prevention, particularly in Indigenous communities43.
Conflict and relationship breakdown
Thematic coding identified numerous coinciding instances of relationship concerns, relationship breakdown, arguments with spouse/partner or others (Fig3). More long-term instances are also noted, such as history of domestic violence, separation from partner or ongoing relationship concerns with relatives and others.
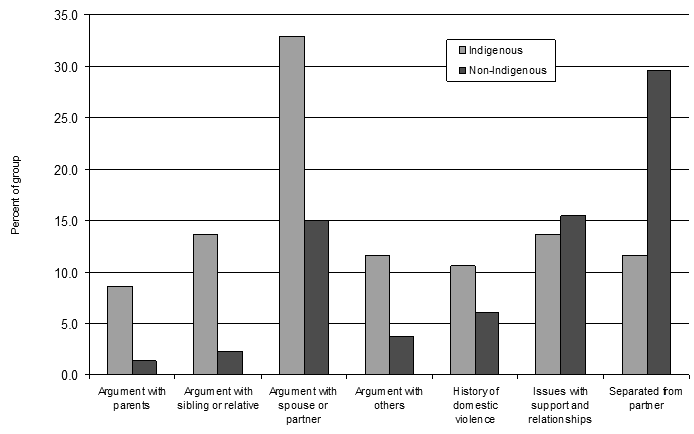
Figure 3: Indication of conflict and relationship breakdown
These data on recent instances of conflict indicate that 33% of Indigenous people represented in the coroners' reports had had a fight or argument with their spouse or partner prior to their suicide. Fourteen percent argued with a sibling or relative, 9% had an argument with their parents and 12% had an argument or fight with someone outside the family. Examples of how these instances are reported include:
On arriving at their residence in [place], the couple again started arguing. This argument extended into a fight between them with both parties exchanging blows and insults. (I/M/2001.280)
The Deceased went to ask his mother for some money to purchase the cigarettes, but she refused. At this time the Deceased has left his friends and returned to his residence yelling loudly along the way. (I/M/2002.89).
Such examples are mirrored, but to a lesser extent, for non-Indigenous cases with 15% having argued or fought with their spouse or partner, 2% with a relative, 1.4% with their parents and 4% with others, prior to suicide. For example:
After an argument [partner] and the children left the house, and went to stay at her parents' home in [place]. During the Friday the deceased phoned [partner] and abused her for taking the car and leaving him with no money, so her father returned the car to him. (N/M/2004.64)
... the deceased and Mr [name] had an argument. The reason for the argument was that Mr [name] accused the deceased of having an extra-marital affair. (N/M/2001.52)
Differences in intimate partner conflict between the two population groups may in part be a function of the younger age of the Indigenous cases at suicide (they may have been less likely to have been married or partnered) and differences in marital patterns between the populations. The data depicted suggest that in a number of cases, particularly Indigenous cases, the suicide may have been an impulsive act following an argument or conflict (Fig3). Likewise from the qualitative analysis, it appeared that many of the reported arguments were fuelled by excessive alcohol consumption and resulted in seemingly impulsive suicide acts.
Descriptions of longer term history of conflict included domestic violence in 11% of Indigenous and 6% of non-Indigenous cases. Separation from partner showed the opposite trend, with mention in 12% of Indigenous cases and almost 30% of non-Indigenous cases. Other general concerns with support and relationships were reported in similar numbers (14% Indigenous cases and 16% Non-Indigenous cases).
There is evidence from other witnesses that the deceased and [partner] were in a romantic relationship and that [partner's] family were unhappy with the relationship and wanted it to end due to the clan group relationship of the families. There is evidence that it was taboo for them to be in a relationship due to it being considered 'wrong skin'. (I/M/2007.226)
In general, the relative importance of relationship factors to completed suicide reinforces the importance of psychosocial factors as contributors to suicide for this predominantly rural population.
Mental illness
In this sample, mental health issues were mentioned far less frequently in Indigenous than non-Indigenous reports. These were coded into four discrete categories (Fig4).
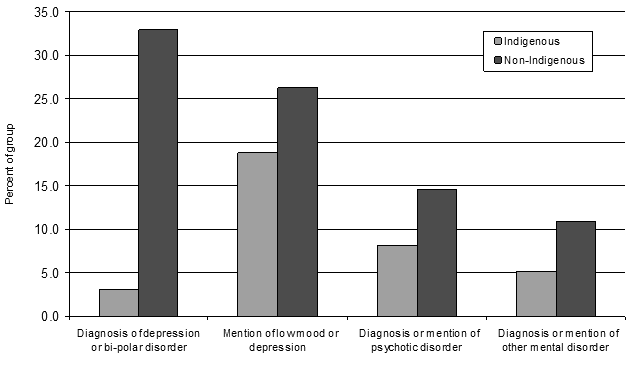
Figure 4: Indication of mental health issues
The greatest difference between Indigenous and non-Indigenous cases was for cases in which there was evidence of a diagnosis or treatment for major depressive disorder or bi-polar disorder. For example:
The deceased had a medical condition being Severe Chronic Bipolar Disorder, which she had for a considerable time and for which she received treatment. (N/F/2000.281)
Reports in which there was mention of low mood or depression were categorised accordingly. In such reports, terms such as depressed, sad, unhappy and despondent were often used with no indication of a formal diagnosis or treatment prior to the event. For example:
Whilst there is no evidence that the deceased told anyone that he wished to end his life, he was seen to be sad and crying for several days prior to his death. Many family members had recently passed away, and the deceased's father was ill in [place]. (I/M/2003.91)
Almost 4% of non-Indigenous cases were diagnosed with bi-polar disorder but no Indigenous cases. The same pattern was seen for psychotic disorders (8% for Indigenous compared with almost 15% for non-Indigenous reports) and other mental disorders such as anxiety (5% for Indigenous vs 11% for non-Indigenous cases). Thus, such conditions were half as likely to be mentioned in the coronial reports for Indigenous people as they were for non-Indigenous people.
As represented, diagnosed depression was reported in only 3% of Indigenous cases but in 33% of non-Indigenous cases (Fig4). This is a striking finding, which is also echoed (although to a less dramatic extent) in other diagnosed mental illnesses. It may at least in part be reflective of reduced access of Indigenous (and particularly remote Indigenous) people to the diagnostic system45. However, beyond formal diagnosis, while it was more likely for low mood or depression to be mentioned in reports of Indigenous suicide (19%), this still occurred less frequently than in non-Indigenous suicide reports (26%). These lower rates of depression specifically, and mental illness generally, in Indigenous suicide are reflective of other findings4. They are also consistent with the views of Tatz, who rejected the 'Western medical/mental health model' and drew attention to political and cultural factors, the legacies of colonialism, chronic unemployment, and alcohol and drug use, along with a range of other disadvantages15,16. It is likely that an array of such factors pertain to the current sample.
These findings have considerable relevance to the treatment and support of those at risk of suicide. Likewise, appropriate suicide prevention activities in rural, remote, Indigenous or urban settings should acknowledge the relative importance of these mental illness and treatment factors. As a result, treatment and prevention initiatives may seek to target mental health interventions differently across the different populations and complement professional mental health interventions with initiatives to build social and community capital.
Physical illness
To obtain consistent data on physical illness, information was largely gleaned from autopsy reports, with some information inferred from other parts of the coronial reports. While generally accurate, these data are less numerically based than previously described categories and should be taken as an indication for these cases.
One percent of Indigenous cases and 9% of non-Indigenous cases were reported with some type of terminal chronic disease, such as cancer, at the time of death (Fig5). The autopsies of a larger number, 15% and 23%, respectively, were reported with a chronic disease, such as heart disease or hepatitis, that was unlikely to cause death in the immediate future.
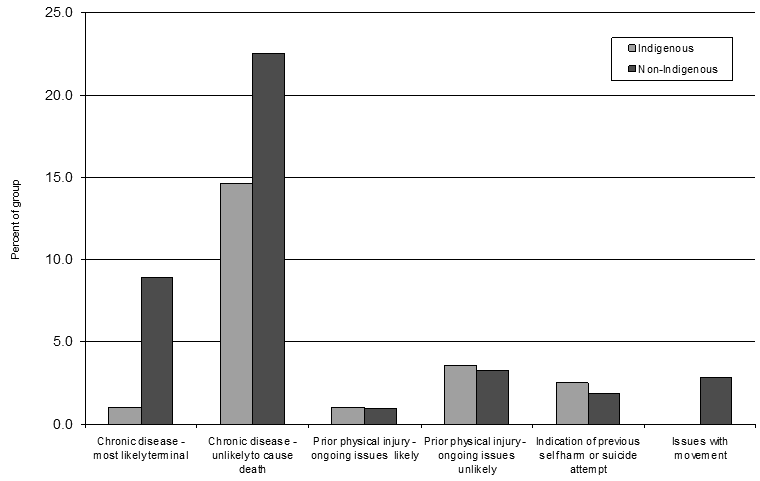
Figure 5: Indication of physical health issues at time of death
Approximately 3% of both Indigenous and non-Indigenous cases had prior physical injuries that were unlikely to have resulted in continuing health concerns. Approximately 1% of both groups had ongoing issues related to prior physical injuries and approximately 3% of non-Indigenous cases suffered conditions that resulted in decreased mobility. There were physical indications, such as scars, consistent with previous self-harm or suicide attempts in 2.5% of Indigenous cases and approximately 2% of non-Indigenous cases.
While the limited role of physical illness has been noted in Indigenous suicide4, in this case the lower incidence of chronic disease evidenced in Indigenous suicide cases is most likely due to the younger age of the Indigenous cohort (with no cases over the age of 50 years). It is unlikely to be reflective of poorer access to services and treatment since findings arose from autopsy reports rather than medical records. In general, it would appear that physical illness issues were not as strongly associated with suicide as other factors for the current sample.
Suicide precedents
With regard to concerns over suicide clusters, a number of social precedents and behavioural factors that were reported prior to the suicide and considered important enough to be included in the coronial reports were categorised and are provided (Fig6)41.
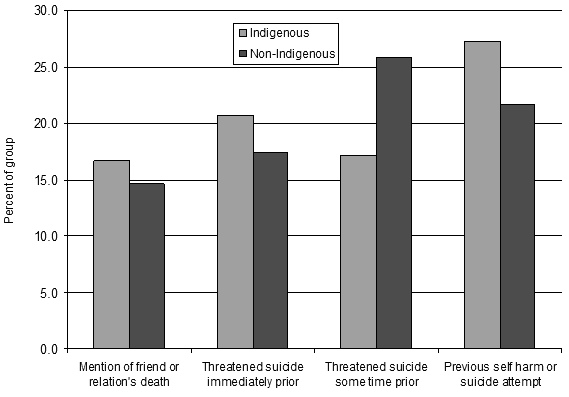
Figure 6: Suicide precedents reported prior to death
In 17% of Indigenous cases and almost 15% of non-Indigenous cases, coroners' reports mentioned the circumstances of a friend or relative's death, or bereavement, prior to the completed suicide. Between 17% and 26% of both cohorts had threatened suicide either immediately prior to, or at least some time prior to, actually carrying it out. For example:
He threatened to hang himself if he was not given money. His sister and her family did not take his threat to kill himself seriously because he had over time, and in particular during the preceding month often threatened to kill himself when he was not given money for grog. (I/M/2002.287)
As well as threatening to commit suicide, approximately a quarter of cases (27% of Indigenous and 22% of non-Indigenous) had attempted suicide previously. It would appear that personal and social precedents of suicide are important considerations. Likewise, as with relationship breakdown, the importance of social factors in suicide prevention (and postvention) should be noted, and this may have particular relevance to smaller rural and remote communities.
Other issues
Other factors that were less prominent numerically and qualitatively include mention of contextual issues such as worries about money, problems at work and legal issues. Just over 3% of Indigenous cases mentioned issues with money as a factor in suicide, but approximately 10% of non-Indigenous cases reflected this concern. It would appear that financial issues were not often identified as major factors in the coronial reports of suicides of Indigenous people, possibly as a function of expectations, the nature of their income or their financial obligations.
Similarly, problems at work were hardly mentioned as having an impact on the suicide of Indigenous people (and according to NCIS data, only 23% of the current sample of Indigenous suicide cases was employed at the time of their death). In keeping with social and contextual models of suicide, this may reflect that coroners consider that these issues are not noteworthy in this population and therefore they are less well documented as factors contributing to suicide. The majority of the cases in this category were non-Indigenous. Around 10% of non-Indigenous reports indicated that the deceased had financial issues and 11% reported that the deceased had had difficulties at work. For example:
[The deceased] did not find any other work. With his bank account savings slowly running out, the deceased on [date] borrowed money from Cash Converters. At this time his bank account was empty and he was three weeks behind in his rent. (N/M/2003.144)
An example of work issues reported by a coroner is provided here:
The deceased had an ongoing dispute with his employer over promotion. In [date] two employees were promoted without going through the normal process ... The deceased was angry at not being promoted. (N/M/2003.250)
Ten percent of both Indigenous and non-Indigenous groups were noted as having some dealings with the legal system or the police prior to their suicide. For example:
When the deceased died he was being investigated by police as a suspect in the killing of [name], who was found dead from head wounds on [date]. The deceased had been interviewed by police on [subsequent date] and a search warrant had been executed at his house. (I/M/2008.329)
Limitations
While these findings provide useful information on key dimensions of suicide, a number of limitations of the method should be noted. First, coroners' reports are not originally intended as clinical or epidemiological documents. Despite this, given that they use rigorous procedures and are informed by a range of expert witnesses, friends, relatives and others, the current study determined that they are valid data sources and hold considerable potential and relevance in this area of research.
Second, it is possible the current findings differ from what may have been gleaned through psychological autopsies, which are highly detailed procedures for investigating a death by reconstructing what the person thought, felt and did. Typically, these reconstructions are based on information gathered from personal documents, reports, records and face-to-face interviews with families, friends and others who had contact with the person before the death. The psychological autopsy method may have provided scope to explore the questions regarding differences in diagnosed mental disorder across populations. However, while such methods provide rich data46,47, they have been found to suffer bias, confounding influence of extraneous variables and lack of standardisation of assessment instruments42,48, which the current study sought to avoid.
Third, the categorisation of Indigenous and non-Indigenous may be overly simplistic in that it does not inform more nuanced questions of lifestyle, cultural practices, beliefs and remoteness. Such important questions, beyond the scope of the current data set, may be topics for future research.
Finally, thematic coding may be seen as subjective, lacking the criteria and rigour of formal tools. In this study, the authors sought to address this concern by coding consistently according to established criteria and by verifying the method across researchers.
A number of key factors of relevance to suicide research and prevention, particularly in remote and Indigenous communities, have been identified in this study. In keeping with previous research on Indigenous suicide, the current study has underlined and quantified the relative importance of key themes including alcohol abuse, interpersonal conflict, depression and mental disorder. Also evident across these themes was the apparent impulsiveness reflected in Indigenous suicide cases4,15,49.
The current study is unique in quantifying a number of social and contextual factors as they are associated with suicide of Indigenous and non-Indigenous people in the NT. The current detailed and methodical analysis of coroners' reports demonstrates that while diagnosed mental disorder is important as a factor in the suicide of both groups, it is not the most commonly associated factor and was much less relevant in Indigenous suicide cases. This finding may be reflective of underdiagnosis of Indigenous cases by professionals or, indeed, the overdiagnosis of mental disorders in the non-Indigenous population. These data suggest the importance of recognising the social construction of mental disorder and that Indigenous people perceive, report and accept mental disorder differently50. Interestingly, low mood was present in roughly equal numbers across both populations.
In contrast, the abuse of alcohol and other drugs, and instances of relationship breakdown were far more strongly associated with suicide in the current sample. In response, suicide prevention among rural, remote and Indigenous people should balance the treatment of mental disorder with more holistic and social approaches, which may include community development. Investment in addressing the social determinants of suicide would appear to be a key priority to lower suicide rates in rural, remote and Indigenous communities, and beyond.
Acknowledgements
The authors gratefully acknowledge that support for this project was provided by the University of Tasmania, School of Medicine, Research Fund.
References
1. Australian Bureau of Statistics (ABS). Causes of death, 2006. Canberra, ACT: ABS, 2008.
2. Australian Institute of Health and Welfare (AIHW). Indigenous life expectancy. Canberra, ACT: AIHW. (Online) 2011. Available: http://www.aihw.gov.au/indigenous-life-expectancy (Accessed 25 November 2012).
3. Pridmore S, Fujiyama H. Suicide in the Northern Territory, 2001-2006. Australian and New Zealand Journal of Psychiatry 2009; 43(12): 1126-30.
4. De Leo D, Sveticic J, Milner A, McKay K. Suicide in Indigenous populations of Queensland. Brisbane, QLD: Australian Academic Press, 2011.
5. Lester D. Suicide and culture. World Cultural Psychiatry Research Review 2008; 3: 51-68.
6. Kirmayer LJ, Malus M, Boothroyd LJ. Suicide attempts among Inuit youth: a community survey of prevalence and risk factors. Acta Psychiatrica Scandinavica 1996; 94(1): 8-17.
7. Bjerregaard P, Lynge I. Suicide - a challenge in modern Greenland. Archives of Suicide Research 2006; 10(2): 209-220.
8. Beautrais AL, Fergusson DM. Indigenous suicide in New Zealand. Archives of Suicide Research 2006; 10(2): 159-168.
9. Silviken A, Haldorsen T, Kvernmo S. Suicide among Indigenous Sami in Arctic Norway, 1970-1998. European Journal of Epidemiology 2006; 21(9): 707-713.
10. Olson LM, Wahab S. American Indians and suicide. Trauma, Violence, & Abuse. 2006; 7(1): 19-33.
11. Chen C-S, Yang M-S, Yang M-J, Chang S-J, Chueh K-H, Su Y-C et al. Suicidal thoughts among elderly Taiwanese aboriginal women. International Journal of Geriatric Psychiatry 2008; 23(10): 1001-1006.
12. Durkheim E. Suicide: a study in sociology. New York: Free Press, 1951.
13. Berry JW. Acculturation and adaptation in a new society. International Migration 1992; 30: 69-85.
14. Hunter E, Milroy H. Aboriginal and Torres Strait Islander suicide in context. Archives of Suicide Research 2006; 10(2): 141-157.
15. Tatz C. Aboriginal suicide is different. Canberra, ACT: Aboriginal Studies Press, 2001.
16. Tatz C. Aboriginal, Maori, and Inuit youth suicide: avenues to alleviation? Australian Aboriginal Studies 2004; 2004(2): 15-25.
17. Dudley M. Addressing indigenous suicide: a special case? A response to Colin Tatz. Australian Aboriginal Studies 2004; 2004(2): 26-33.
18. Hayman N. Reducing the inequalities in indigenous health: a new way forward. Internal Medicine Journal 2008; 38(7): 543-545.
19. Cavanagh JT, Carson AJ, Sharpe M, Lawrie SM. Psychological autopsy studies of suicide: a systematic review. Psychological Medicine 2003; 33(3): 395-405.
20. Phillips MR. Rethinking the role of mental illness in suicide. American Journal of Psychiatry 2010; 167(7): 731-733.
21. Manoranjitham SD, Rajkumar AP, Thangadurai P, Prasad J, Jayakaran R, Jacob KS. Risk factors for suicide in rural south India. The British Journal of Psychiatry 2010; 196(1): 26-30.
22. Rich CL, Warstadt GM, Nemiroff RA, Fowler RC, Young D, Warsradt GM. Suicide, stressors, and the life cycle. The American Journal of Psychiatry 1991; 148(4): 524-527.
23. Foster T. Adverse life events proximal to adult suicide: a synthesis of findings from psychological autopsy studies. Archives of Suicide Research 2011; 15(1): 1-15.
24. Scourfield J, Fincham B, Langer S, Shiner M. Sociological autopsy: an integrated approach to the study of suicide in men. Social Science & Medicine 2012; 74(4): 466-473.
25. Rehkopf DH, Buka SL. The association between suicide and the socio-economic characteristics of geographical areas: a systematic review. Psychological Medicine 2006; 36(2): 145-157.
26. Ying YH, Chang K. A study of suicide and socioeconomic factors. Suicide and Life Threatening Behavior 2009; 39(2): 214-226.
27. Maselko J, Patel V. Why women attempt suicide: the role of mental illness and social disadvantage in a community cohort study in India. Journal of Epidemiology and Community Health 2008; 62(9): 817-822.
28. Riordan DV, Selvaraj S, Stark C, Gilbert JSE. Perinatal circumstances and risk of offspring suicide. The British Journal of Psychiatry 2006; 189(6): 502-507.
29. Gravseth HM, Mehlum L, Bjerkedal T, Kristensen P. Suicide in young Norwegians in a life course perspective: population-based cohort study. Journal of Epidemiology and Community Health 2010; 64(5): 407-412.
30. Qin P. Suicide risk in relation to level of urbanicity - a population-based linkage study. International Journal of Epidemiology 2005; 34(4): 846-852.
31. Middleton N, Gunnell D, Frankel S, Whitley E, Dorling D. Urban-rural differences in suicide trends in young adults: England and Wales, 1981-1998. Social Science & Medicine 2003; 57(7): 1183-1194.
32. Stark C, Gibbs D, Hopkins P, Belbin A, Hay A, Selvaraj S. Suicide in farmers in Scotland. Rural and Remote Health 6(1): 509. (Online) 2006. Available: www.rrh.org.au (Accessed 25 November 2012).
33. Stark C, Hopkins P, Gibbs D, Belbin A, Hay A. Population density and suicide in Scotland. Rural and Remote Health 7(3): 672. (Online) 2007. Available: www.rrh.org.au (Accessed 25 November 2012).
34. Stark CR, Riordan V, O'Connor R. A conceptual model of suicide in rural areas. Rural and Remote Health 11(2): 1622. (Online) 2011. Available: www.rrh.org.au (Accessed 25 November 2012).
35. Zhang J, Wieczorek WF, Conwell Y, Tu XM. Psychological strains and youth suicide in rural China. Social Science & Medicine 2011; 72(12): 2003-2010.
36. Pridmore S. Suicide and predicament: life is a predicament. Oak Park, IL: Bentham Publishers, 2010. Available: http://www.benthamscience.com/ebooks/9781608051694/index.htm (Accessed 5 December 2012).
37. Goldsmith SK, Pellmar TC, Kleinman AM, Bunney WE (Eds). Reducing suicide: a national imperative. Washington, DC: National Academies Press, 2002.
38. Department of Health and Ageing (DoHA). Commonwealth response to The Hidden Toll: Suicide in Australia. Report of the Senate Community Affairs Reference Committee. Canberra, ACT: DoHA, 2010.
39. Shiner M, Scourfield J, Fincham B, Langer S. When things fall apart: gender and suicide across the life-course. Social Science & Medicine 2009; 69(5): 738-746.
40. Ostry AS. The mortality gap between urban and rural Canadians: a gendered analysis. Rural and Remote Health 9(4): 1286. (Online) 2009. Available: www.rrh.org.au (Accessed 25 November 2012).
41. Hanssens L. The search to identify contagion operating within suicide clusters in Indigenous communities, Northern Territory, Australia. Aboriginal and Islander Health Worker Journal 2007; 31(5): 27-33.
42. De Leo D, Evans R. International suicide rates and prevention strategies. Cambridge, MA: Hogrefe & Huber, 2004.
43. Hanssens L. Indigenous dreaming: how suicide in the context of substance abuse has impacted on and shattered the dreams and reality of Indigenous communities in Northern Territory, Australia. Aboriginal and Islander Health Worker Journal 2007; 31(6): 26-34.
44. Clough AR, Lee KSK, Cairney S, Maruff P, O'Reilly B, D'Abbs P et al. Changes in cannabis use and its consequences over 3 years in a remote indigenous population in northern Australia. Addiction 2006; 101(5): 696-705.
45. Hunter E. Disadvantage and discontent: a review of issues relevant to the mental health of rural and remote Indigenous Australians. Australian Journal of Rural Health 2007; 15(2): 88-93.
46. Bertolote JM, Fleischmann A, De Leo D, Wasserman D. Psychiatric diagnoses and suicide: revisiting the evidence. Crisis 2004; 25(4): 147-155.
47. Scocco P, Marietta P, Tonietto M, Dello Buono M, De Leo D. The role of psychopathology and suicidal intention in predicting suicide risk: a longitudinal study. Psychopathology 2000; 33(3): 143-150.
48. Pouliot L, De Leo D. Critical issues in psychological autopsy studies. Suicide and Life Threatening Behavior 2006; 36(5): 491-510.
49. Hunter E. 'Best intentions' lives on: untoward health outcomes of some contemporary initiatives in Indigenous affairs. Australian and New Zealand Journal of Psychiatry 2002; 36(5): 575-584.
50. Brown A, Scales U, Beever W, Rickards B, Rowley K, O'Dea K. Exploring the expression of depression and distress in Aboriginal men in central Australia: a qualitative study. BMC Psychiatry 2012; 12: 97.



