The health needs of rural populations are a significant issue in Canada as almost 9 million Canadians, or 30% of Canada's population, live in rural, remote and northern areas1. Compared with the organization and delivery of urban health care, rural systems have been described as being less complex, having limited funding, being challenged on the availability of qualified service providers and having insufficient workers and overworked healthcare providers2. Kaasalainen and colleagues reported that distances traveled by community nurses to patients' homes were perceived as a major challenge to providing care in a rural area3. Similarly, Wilkes and Beale indicated that, compared with their urban counterparts, rural nurses providing palliative care within the home setting had the additional stress of providing care over vast distances and with a lack of financial resources4. Overall, individuals in rural areas show different patterns in their use of health services compared with their urban counterparts: while some services are used less frequently (eg fewer hospital admissions, fewer visits to physicians), rural residents use other services to a greater extent than do urban residents (eg more emergency room visits)5.
Hospitalization is also an issue for rural populations in Canada. Burge and colleagues found that patients with cancer from rural areas were less likely to die out-of-hospital than were those living in urban areas6. Hwang and colleagues suggested that the higher rates of hospitalization observed among patients with cancer in rural areas were likely linked to the difficulties experienced in recruiting and retaining family physicians, who are essential in providing adequate outpatient care for patients with terminal cancer7. Against this backdrop of issues related to the provision of health care in rural areas, there is growing concern regarding the adequacy of care that is provided, particularly for patients who are terminally ill living with these regions.
While considerable progress has been made in the care of the terminally ill in urban regions, the quality of care at the end of life for individuals residing in rural settings is gathering greater attention8-10. The research literature has identified a number of barriers common to the provision of care to the terminally ill in rural areas, including the difficulty in recruiting and retaining healthcare workers and lack of funding for service development8.
The unique challenges associated with the provision of health care to terminally ill patients in rural settings suggests informal carers assume a greater role than their urban counterparts. Unfortunately, little is known about the experience of informal caregivers in rural settings, as little research has been conducted examining the role of informal caregiving in rural regions at the end of life8,11,12. Further, few studies have included both urban and rural caregivers in order to allow for comparison of their experiences13. The absence of consistent measurement and comparison across urban and rural settings has made it difficult to develop an understanding of the caregiving experience in rural Canada11.
The purpose of this article is to address this gap in the research literature by reporting on the experiences of active caregivers from urban and rural settings. Using a consistent measurement approach across both urban and rural locations, this study documented caregivers' perceived health status, the experience of burden in caregiving and caregivers' assessment of social supports. The study also examined the pattern of formal care used by the terminally ill and their families in both settings.
Study design and setting
This was a cross-sectional, community-based interview study conducted in northeastern Ontario, Canada. In the province of Ontario, Canada, health care is administered by 14 Local Health Administration Networks (LHINs); the study region was bounded by the administrative coverage of the North East LHIN. Geographically, the study region covers an area of approximately 400 000 km2, with a population of only 551 000 individuals. The definition of rural as determined by an expert panel established by the Ontario Ministry of Health and Long-Term Care to examine healthcare issues in northern and rural Ontario was used for this study14. According to this definition, communities with 30 000 or more residents typically have a broad range of specialty and sub-specialty inpatient hospital services, have expanded community-based services and serve as hubs for regional programs14. Over 60% of the population living in this region are located within the boundaries of four centres meeting this criterion for urban: Sudbury (population 157 857), Sault Saint Marie (74 948), North Bay (53 966) and Timmins (42 997). Rural areas comprise rural and isolated communities through the vast area that comprises northeastern Ontario outside the four designated urban centres and represent 40% of the total population living in this region14.
Study population
The study sample comprised participants obtaining formal services from the North Eastern Community Care Access Centre (CCAC). Community Care Access Centres are publicly funded agencies designed to provide a unified service access point to community care services in Ontario. They are responsible for client service planning, case management and the brokering of community-based services. Participants included both urban and rural family caregivers. The urban sample (n=56) comprised family caregivers living within one of the four urban centres within the catchment area of the North Eastern CCAC (Sudbury, Sault Saint Marie, North Bay and Timmins). Individuals living outside of the four designated urban centres formed the rural sample (n=44).
Informal caregivers living within the North Eastern CCAC catchment area were eligible to participate if they were providing care on a regular basis to a palliative care patient (ie care recipient); were not receiving remuneration from the patient or other sources for care provided; and were able to communicate in English. In addition, the care recipient had to be over 19 years of age and receiving formal services from the North Eastern CCAC.
Participant recruitment
Informal caregivers were recruited from 2009 to 2011. Potential participants were identified through a review of North Eastern CCAC client records conducted by CCAC staff. Informal caregivers meeting the study eligibility criteria were telephoned by a CCAC representative and invited to participate in the study. The name and contact information of interested informal caregivers who provided verbal consent was shared with the study investigators. Study information packages were mailed to consenting caregivers. A research assistant then contacted potential participants by telephone to explain the study and, for those interested, obtain informed verbal consent and schedule a convenient time to conduct the telephone-based interview. Written consent from family caregiver respondents was also obtained through the mailing of a signed consent form to the study team.
Data collection
Data were collected using a telephone-based survey conducted by a research assistant. The survey collected care recipient and caregiver characteristics; caregiver perceived burden; social support; and service use. Caregiver demographic information collected included sex, age, education, income and self-reported health status15. Care recipient characteristics collected included sex, age and living arrangements.
Caregiver perceived burden: To assess caregiver perceived burden, caregivers completed a modified version of the Caregiver's Burden Scale in End-of-Life Care (CBS-EOLC). The CBS-EOLC is a self-report instrument consisting of 16 items; higher scores indicate greater caregiver strain16.
Perceived social support: Perceived social support among caregivers was assessed using a modified version of the Multidimensional Scale of Perceived Social Support (MSPSS). The MSPSS is a 12-item instrument using a 7-point Likert scale that provides a total score and three subscale scores: significant others, family and friends17. Higher scores indicate greater support. Unlike the original instrument, the present study used a 5-point Likert scale (versus the original 7-point Likert scale).
Health service use: To catalogue services used by caregivers in the previous 2 weeks, the investigators developed a detailed list of 15 services that the care recipient could receive at home. Respondents were also given the option to identify other services being used that were not included in the list provided.
Care recipient functional status: The functional status of the care recipient was assessed using the Eastern Collaborative Oncology Group (ECOG) performance scale, which measures functional independences as reported by the caregiver18.
Data analysis
Data were analyzed in Statistical Package for Social Sciences v20 (SPSS Inc; www.spss.com) using appropriate descriptive and inferential statistics. For care recipient and caregiver characteristics, caregiver perceived burden, social support and service use, data are presented as means and standard deviations (SD) for continuous variables, and as percentages for categorical variables. Chi-squared tests, or the likelihood ratio test or Fisher's exact test as appropriate, were performed to examine group differences (ie urban versus rural) among categorical variables, while independent Student's t-tests were used to examine group differences for continuous variables. The significance level used for hypothesis testing was p=0.05.
Ethics approval
Ethics approval was obtained from McMaster University Faculty of Health Sciences Research Ethics Board (approval number: 08-328).
Caregiver and care recipient characteristics
A sample of 479 potential participants was identified as eligible and approached by the CCAC to participate in the study (Fig1). A total of 140 individuals completed the telephone survey (29% response rate). In this paper, findings are presented for the caregivers who were actively caregiving (n=100: rural = 44, urban = 56). Focusing on only those individuals who were actively caregiving ensures a consistency for both caregiver status (ie active caregiver) and measurement tools between the two groups.
The characteristics of the caregiver respondents and care recipients are presented (Tables 1,2). Rural and urban caregivers did not differ significantly for any assessed characteristic. Informal caregivers were more likely to be female, caring for their spouse and caring for an older care recipient. The majority of both rural and urban caregivers reported that they were not employed while caregiving. In addition, there were no differences observed between urban and rural caregivers for level of caregiver strain (CBS-EOLC). Caregiver's Burden Scale in End-of-Life Care scores for the modified instrument can range from 14 to 56; thus, caregivers in both groups reported lower levels of caregiver strain. The majority of caregivers in rural and urban groups reported their general health as good or very good (72.8% and 73.2%, respectively) and very few unhealthy days in the 30 days prior to the interview (Table 1). Most caregivers in both groups described their care recipient as either capable of all self-care or experiencing some limitation in self-care (Table 2). It was observed that rural caregivers were significantly more likely to report that they had relocated to assume caregiving responsibilities (rural 82.1%, urban 18.8%, χ² p=0.001).
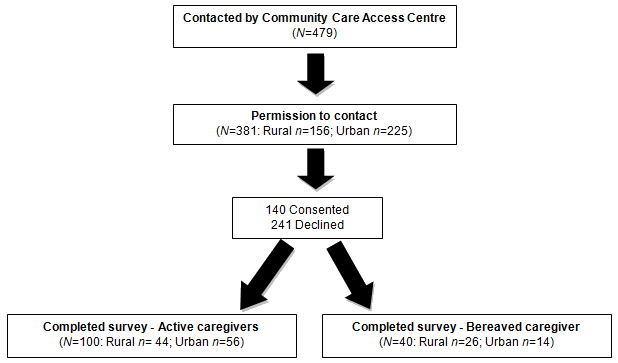
Figure 1: Flow of caregiver participants through the telephone survey study.
Table 1: Caregiver demographics
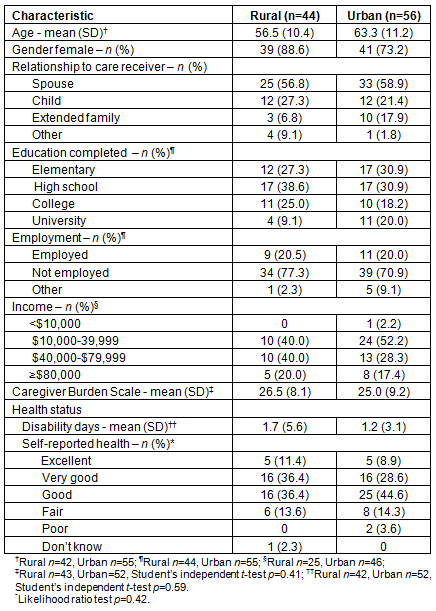
Table 2: Care recipients' characteristics
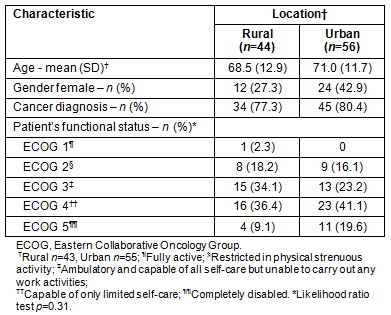
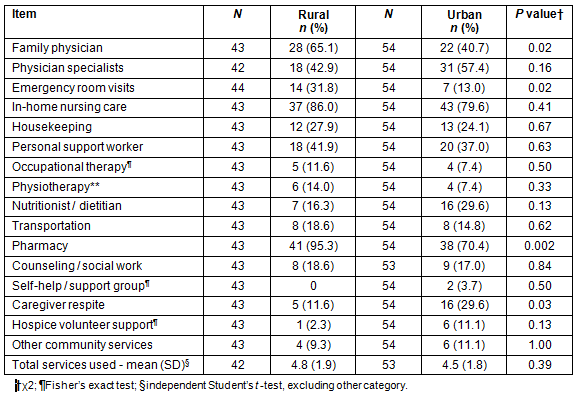
It was revealed that there were no significant differences between the two groups on perceptions of social support (Table 3). Both groups perceived high levels of social support from family, friends and significant others. Although there were no differences between rural and urban caregivers in the number of services used in the previous 2 weeks, significant variations in the types of services used by the two groups were observed (Table 4). Rural caregivers reported greater use of family physicians, emergency room visits and pharmacy services, while urban caregivers reported greater use of caregiver respite services.
Table 3: Caregiver perceptions of social support
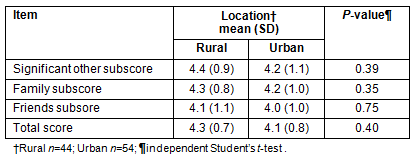
Table 4: Services used by caregivers in the previous 2 weeks
Discussion
The present study examined the subjective experience of family caregivers regarding their perceived access to care and strain burden related to caregiving. The results demonstrate there are a number of commonalities in the caregiving experience for informal care providers across rural and urban settings. Rural and urban caregivers reported similar levels of low perceived strain related to caregiving and both showed high levels of social support. Further, both groups were providing care to recipients with similar limitations in self-care activities and used a comparable number of services. Despite these similarities, some differences between rural and urban caregivers were observed: caregivers in rural settings used different services than did urban caregivers and were also more likely to have relocated in order to provide care.
Previous work comparing service use between rural and urban settings has reported greater numbers of hospital and home visits among rural populations5,8. Similar variations in the services accessed by rural and urban caregivers were also observed in the present study, as rural caregivers reported greater use of hospital services (through increased number of emergency room visits), while urban caregivers reported greater use of caregiver respite services. Given the recognized barriers to health service access in rural areas, it is likely that respite care was not available to the caregivers residing in rural areas2,4. Additionally, the greater use of physician visits, pharmaceutical services and emergency room visits reported by rural caregivers suggest there is more need for pain and symptom management in the rural setting as opposed to the urban setting.
Research has identified consistent barriers to the access of care in rural settings, including the scarcity of available healthcare providers5,8,14,19 and issues of transportation imposed by geography8,14,20,21. Surprisingly, despite these known barriers to care that are common among rural populations, no significant differences were observed for level of caregiver burden between urban and rural caregivers; caregivers in both groups reported relatively low levels of burden. In keeping with this observation, the number of services caregivers reported using in the previous 2 weeks did not differ between groups. Additionally, both groups also reported high levels of social support from family, friends and significant others. The high levels of social support perceived by caregivers in both groups likely provided a buffering effect, thus protecting both rural and urban caregivers from undue burden or strain. These findings are consistent with previous work suggesting that some aspects of the caregiver experience are common among family members regardless of the setting12.
Recruitment of participants from this population can be quite challenging, as evidenced by the low response rate of the present study: close to 500 potential participants were contacted yet only 100 caregivers actively providing care participated in the study. Family members actively providing care were likely so busy completing daily caregiving tasks that participation in a study may have been viewed as too time-consuming in comparison to the numerous demands already placed on their time. Thus, study findings should be interpreted within the context of the response rate. For example, it is likely that these results underestimate the true level of burden among family caregivers as it is likely that caregivers with the most amount of burden were those who could not take the time to participate in the study. As well, the similar levels of perceived burden and social support reported by caregivers in both groups cannot be confirmed given the small sample size. Despite these limitations, significant differences were observed between rural and urban caregivers, which confirm that although there are common aspects to the caregiving experience, there are differences as well. These findings are consistent with previous literature8. The unique contribution of the present study to this body of literature is the comparative nature of the work, where the experiences of rural informal family caregivers providing palliative care were explored and contrasted against the experiences of their urban counterparts.
The present study expands the existing research literature examining end-of-life care in rural settings by comparing the caregiving experiences of rural and urban caregivers in order to identify and describe aspects unique to the rural experience. Although the caregiving experience has common features across both settings, given the differences we observed, location should still be considered when crafting interventions as the types of services required and used can differ by location, such as pain and symptom services for rural/isolated patients and their caregivers. The standardized tools employed in the present study allow for the identification of rural caregiver needs to be undertaken; this is a step that is key to the development of successful interventions. Future research may require utilizing a mixed methods approach to insert meaning into the results and allow for in-depth exploration of the caregiver experience.
Acknowledgements
This study was funded by the Canadian Institutes of Health Research.
References
1. Ministerial Advisory Council on Rural Health. Rural health in rural hands: strategic directions for rural, remote, northern and Aboriginal communities. Ottawa, ON: Office of Rural Health, 2002.
2. Goodridge D, Duggleby W. Using a quality framework to assess rural palliative care. Journal of Palliative Care 2010; 26(3): 141-150.
3. Kaasalainen S, Brazil K, Wilson DM, Willison K, Marshall D, Taniguchi A et al. Palliative care nursing in rural and urban community settings: a comparative analysis. International Journal of Palliative Nursing 2011; 17(7): 344-352.
4. Wilkes LM, Beale B. Palliative care at home: stress for nurses in urban and rural New South Wales, Australia. International Journal of Nursing Practice 2001; 7(5): 306-313.
5. Pong RW, DesMeules M, Heng D, Lagace C, Guernsey JR, Kazanjian A et al. Patterns of health services utilization in rural Canada. Chronic Diseases and Injuries in Canada 2011; 31(1Suppl): S1-S36.
6. Burge F, Lawson B, Johnston G. Where a cancer patient dies: the effect of rural residency. Journal of Rural Health 2005; 21(3): 233-238.
7. Hwang S, Chang V, Alejandro Y, Osenenko P, Davis C, Cogswell J et al. Caregiver unmet needs, burden, and satisfaction in symptomatic advanced cancer patients at a Veterans Affairs (VA) medical center. Palliative and Supportive Care 2003; 1(4): 319-329.
8. Wilson DM, Justice C, Sheps S, Thomas R, Reid P, Leibovici K. Planning and providing end of-life care in rural areas. Journal of Rural Health 2006; 22(2): 174-181.
9. Crooks D, Schuurman N. Reminder: palliative care is a rural medicine issue. Canadian Journal of Rural Medicine 2008; 13(3): 139-140.
10. Kelly ML, Sletmoen W, Williams AM, Nadin S, Puiras T. Integrating policy, research, and community development: a case study of developing rural palliative care. In: JC Kulig, AM Williams (Eds). Health in rural Canada. Vancouver: UBC Press, 2012: 219-238.
11. Hughes P, Ingeton C, Clark D. Providing cancer and palliative care in rural areas: a review of patient and carer needs. Journal of Palliative Care 2004; 20(1): 44-49.
12. Robinson CA, Pesut B, Bottorff JL, Mowry A, Broughton S, Fyles G. Rural palliative care: a comprehensive review. Journal of Palliative Medicine 2009; 12(3): 253-258.
13. Donovan R, Williams A. Shifting the burden: the effects of home-based palliative care on family caregivers in rural areas. In: JC Kulig, AM Williams (Eds). Health in rural Canada. Vancouver: UBC Press, 2012: 316-333.
14. Ontario Ministry of Health and Long-Term Care. Rural and Northern Health Care Framework / Plan: Stage 1 report. Toronto, Ontario: Ontario Ministry of Health and Long-Term Care, 2011.
15. Centers for Disease Control and Prevention. Measuring health days. Atlanta, GA: CDC, 2000.
16. Dumont S, Fillion L, Gagnon P, Bernier N. A new tool to assess family caregivers' burden during end-of-life care. Journal of Palliative Care 2008; 24(3): 151-161.
17. Zimet GD, Dahlem NW, Zimet SG, Farley GK. The Multidimensional Scale of Perceived Social Support. Journal of Personality Assessment 1988; 52(1): 30-41.
18. Oken MM, Creech RH, Tormey DC, Horton J, Davis TE, McFadden ET et al. Toxicity and response criteria of the Eastern Cooperative Oncology Group. American Journal of Clinical Oncology 1982; 5(6): 649-655.
19. Pitblado JR. Geographical distribution of rural health human resources. In: JC Kulig, AM Williams (Eds). Health in rural Canada. Vancouver: UBC Press, 2012, 219-238.
20. Waldorp D, Kirkendall AM. Rural-urban differences in end-of-life care: implications for practice. Social Work in Health Care 2010; 49(3): 263-289.
21. Moss A, Racher F, Jeffery B, Hamilton C, Burles M, Annis RC. Transcending boundaries: collaborating to improve access to health services in Northern Manitoba and Saskatchewan. In: JC Kulig, AM Williams (Eds). Health in rural Canada. Vancouver: UBC Press, 2012.

