Pregnancy is a period of a significant increase in iron requirement over and above the non-pregnant state1. Although iron requirements are reduced in the first trimester because of the absence of menstruation, they rise steadily thereafter from approximately 0.8 mg per day in the first month to approximately 10 mg per day during the last 6 weeks of pregnancy2. The increased iron requirement is due to expansion of maternal red blood cell mass for increased oxygen transport, including transfer of iron, to both the growing foetus and the placental structures, and as a needed reserve for blood loss and lochia at parturition3. Due to increased iron requirements, pregnancy is also a period of increased risk for anaemia. Thus, a high proportion of women become anaemic during pregnancy.
Worldwide, the prevalence of anaemia during pregnancy has been estimated at 41.8%, corresponding to 56.4 million women4. Sub-Saharan Africa is the most affected region, with anaemia prevalence estimated to be 17.2 million pregnant women, which corresponds to approximately 30% of total global cases5. In Uganda, 49% of the women of reproductive age are anaemic, and the prevalence is even higher (64.4%) among those who are pregnant6. Anaemia is further exacerbated by HIV/AIDS which has a prevalence among pregnant women in Uganda of approximately 5.9%7. Anaemia in HIV/AIDS can be a result of HIV infection, opportunistic infections and/or highly active antiretroviral therapy8.
Anaemia during pregnancy is of great concern because it contributes significantly to increased risk of maternal death during the prenatal period. Anaemia increases the risk of postpartum haemorrhage9, pregnancy-induced hypertension, placenta praevia, haemorrhage and cardiac failure10. Overall, 20-40% of the estimated 50 000 maternal deaths worldwide associated with child birth or the postpartum period are attributed to anaemia during pregnancy11. Anaemia is also an established risk factor for intrauterine growth retardation and subsequent low birth weight, preterm delivery, prenatal death12.
Uganda is among countries where there are very high levels of anaemia among women of reproductive age (15-49 years) and pregnant women. According to the 2006 Uganda Demographic and Health Survey (UDHS), 49.0% of Ugandan women aged 15-49 years were anaemic (Hb <12.0 g/dL), while 64.4% of those pregnant had sub-optimal haemoglobin (Hb) levels (Hb <11.0 g/dL)6. The Uganda Government has committed to a 30% reduction of maternal anaemia by the year 2010. To this effect, the government has been implementing a minimum public health package to combat pregnancy anaemia throughout public and private healthcare facilities. The public health package includes supplementation with iron and folic acid (IFA), promotion of antenatal care (ANC), prevention and control of malaria infection with intermittent preventive treatment (IPT), use of insecticide treated mosquito nets (ITNs), case management of fevers, treatment and control of helminths infestations and promotion of diet diversification to increase dietary iron intake.
Although Uganda is implementing a minimum public health package to combat pregnancy anaemia, the prevalence of anaemia in pregnancy remains high and increased from 41.2%13 in 2001 to 64.4% in 20066. Although risk factors for anaemia in pregnancy are well known, their interplay and relative strengths in Uganda, a culturally and geographically diverse country, need better understanding in order to improve intervention strategies. It is imperative to understand the factors responsible for the low uptake of public health interventions, as well as other immediate causes of anaemia in each locality in order to design appropriate behavioural change communications and other interventions. In particular, there is insufficient information about the influence of, and knowledge and attitudes towards anaemia and anaemia prevention interventional packages among the population. The objective of this study was therefore to assess the determinants of anaemia among pregnant women in Kiboga district.
Study area and population
The study was conducted in Kiboga, a rural district in the central region of Uganda. The district covers 4045 km2 and is administratively divided into three counties (Ntwetwe, Bukomero and Kiboga Central) with 13 sub-counties, and 540 villages. According to the 2001 Population and Housing census, Kiboga consisted of 51 305 households and a population of about 108 897 (53 668 female)14. The population in Kiboga is mainly rural and dependent on agriculture activities, which are dominated by the main food crop production of bananas, cassava, sweet potatoes, potatoes, maize and beans. Livestock keeping is especially prevalent in Bukomero and Lwamata sub-counties where the population largely comprises a pastoralist ethnic group. This study was conducted in Kiboga district, a purposely selected area due to its cosmopolitan populations with diverse cultural attributes that are representative of most ethnic groups in the country.
Study design
Design and sample size: This was a cross-sectional study focusing on anaemia levels among women of reproductive age (15-49 years). The population size from which the sample was drawn was estimated to be 5400, based on the estimated pregnancy rate (5.2%) and anaemia prevalence among pregnant women in Uganda (64.4%). The sample size was computed using the formula used by Leslie15; 64% was used for prevalence of anaemia, as adopted from the UDHS 20066. The sample size of 276 was calculated. However, a 10% non-response rate raised the sample size to 304. A sample size of 304 was achieved; however, the actual non-response rate was 2.6%.
Sample selection: Sample selection was done using two-stage cluster sampling technique with the village as the primary sampling unit. In the first stage, 6 sub-counties were randomly selected from the 13 sub-counties in Kiboga district using a random-number table. The village was used as the enumeration area. Two villages from each sub-county were then selected from all villages in a sub-county using the probability proportionate to size method. In the second stage, households in each village were randomly selected, based on a complete listing of eligible households. Households' eligibility for inclusion in the study was the presence of a pregnant woman. In households where more than one pregnant woman lived, one woman was selected randomly. Twenty-six households were selected from each village.
Data collection
The study consisted of a socioeconomic and a food intake component, each consisting of various sections.
Socio-demographics, knowledge and practices: Data on socio-demographic factors, iron and anaemia-related knowledge and attitudes of the pregnant women; consumption of iron rich foods, access and utilization of the minimum public health intervention package were collected using a structured questionnaire.
Anaemia status: Anaemia status of the pregnant women was determined by measuring their Hb levels. The Hb measurements of the pregnant women were performed using a portable heme analyser (Hemocue Hb 301, HemoCue AB, Sweden)16. The middle finger of the pregnant woman was cleaned using disinfectant and then pricked at the side of the fingertip. The first 2 or 3 drops were discarded and the next drop was drawn and placed onto a micro-cuvette, which was then inserted into the heme analyser and a reading was obtained within 45 sec. The value was recorded, and disclosed to and discussed with each participant.
Data analysis
Data entry was performed using EPI Data software (www.cdc.gov/epiinfo) and analysis used SPSS software (www.spss.com).
Haemoglobin-defined anaemia status: Anaemia was defined according to the WHO criterion that is, Hb below 11 g/dL17. The anaemia status of the pregnant woman was measured and categorized by degree of severity into one of four levels. Severe anaemia was defined as Hb below 7.0 g/dL; moderate anaemia was Hb 7.0-9.9 g/dL and mild anaemia as Hb 10.0-10.9 g/dL18. Pregnant women with Hb above 11 g/dL were considered non-anaemic. Descriptive statistics was used to assess the Hb levels of the pregnant women.
Socio-demographics, knowledge and practices: Descriptive statistics were used to determine the pregnant women's knowledge of anaemia and iron, establish their consumption levels of foods rich in iron as well as their access and utilization of the minimum public-health intervention package of anaemia prevention and control.
Household wealth quintiles: With regard to wealth quintiles of households, limited study resources did not permit the collection of detailed data on household income and household consumption. Therefore, the study used a simple household asset-based wealth index to measure household wealth relative to others in the study, and to examine a relationship with anaemia following the method suggested by Wagstaff and Watanabe19. A list of common household assets was included in the survey questionnaire. However, those used in generating the wealth quintiles were: bicycle, motorcycle, radio and telephone which were owned by at least 10% of the households. Each asset was assigned a score of '1' or '0' depending on whether the household possessed that asset or not, respectively. A composite household score was then created by summing up all the individual scores. Households were then ranked and divided into quintiles, with the lowest 20% as the lowest wealth quintile and the highest 20% as the highest quintile. Due to the limited number of household assets and housing characteristics used, the wealth quintiles in this study were used as a proxy indicator of household wealth.
Associations between risk factors and anaemia: Taking anaemia status to be the dependent variable, bivariate and multivariate analyses were carried out to elicit the impact of each factor on prevalence of anaemia among pregnant women in Kiboga district. Odds ratios and their 95% confidence intervals (CIs) were calculated. Only models with good fit were presented in the findings.
Ethics approval
Every interviewee was informed about the objectives of the survey and their consent was obtained. Individual anaemia status results were shown and explained to each participant. The study received ethical approval from the Uganda National Council for Science and Technology (#SS1941).
Socio-demographic Characteristics of the Study Population
The sociodemographic characteristics of the study population are shown (Table 1). The study population was mostly rural and farm-dependent with an average household size of five individuals and wood fuel was the dominant source of energy for cooking. Majority of the respondents (58.2%) were in their early reproductive age (15-25 years). Nearly all women (93.4%) were either married or in a quasi-marital relationship. Approximately one-quarter (26.3%) of the study population had no formal schooling while 18.4% had only 4 years of primary education. Over half the respondents had at least 5 years formal schooling, with 1 in 10 having attained some secondary education. Approximately 60% of the respondents reported that they were able to read and write.
Table 1: Sociodemographic characteristics of respondents in Kiboga district

Relative wealth levels: The modal wealth quintile was middle, with 42.4% of respondent households. The percent distribution of asset ownership by wealth rank is shown (Table 1). Households in the lowest rank were least likely to own any of the key assets (radio and bicycle (7.7%), motorcycle (None) and they are more likely to be staying in houses with grass thatch, straw walls, and bare earth. Conversely, households in the highest wealth rank were most likely to live in iron sheet roofed houses, with brick walls and cement floors as well as own at least two of the key assets.
Proximity to healthcare facility: For most respondents (60.3%), the nearest health facility was more than one hour away (> 5 km). Approximately 23.1 % of the women were located within 3-5 km of a healthcare facility.
Prevalence of anaemia
Approximately two-thirds (63.1%) of pregnant women had sub-optimal Hb levels (Hb<11g/dL). This was close to the national prevalence (64.4%) as reported by the 2006 UDHS6. Severe anaemia (Hb<7.0g/dL) and moderate anaemia (Hb 7.0-7.9g/dL) were found to occur in 2.6% and 35.0 % of the respondents, respectively. Approximately 25% of pregnant women had mild anaemia (Hb 10.0-10.9g/dL).
Anaemia by background characteristic: Anaemia was more prevalent among women in the second and third trimesters of pregnancy (63.3%). Generally respondents with primary education had a higher prevalence of any anaemia compared with those without formal education and those of higher levels of education. Respondents who were distant from the nearest health centre were more likely to be anaemic. Anaemia was more prevalent among women from households that did not have a radio.
Respondents' knowledge about iron and anaemia
Awareness of anaemia and its symptoms and signs: Only 80.9% of the respondents had ever heard about anaemia. In decreasing frequency, intermittent dizziness, general body weakness, and persistent fatigue were the top three most commonly known and recognized symptoms of anaemia by the respondents. Only 45.1% of the respondents knew at least 3 symptoms of anaemia but knowledge of anaemia symptoms was not found to be significantly associated with the presence of anaemia.
Awareness of negative consequences of anaemia during pregnancy: Only 45.7% of respondents were aware of some negative consequences of anaemia during pregnancy to both the mother and child. Excessive blood loss (haemorrhage) was the most widely cited consequence of anaemia .
Access and use of the public health intervention for anaemia prevention and control
Timing and frequency of ANC visits: Sixty percent of pregnant women had made at least one ANC visit (Table 2), the majority of which were in the third trimester of pregnancy (Fig1). Only 9.3% and 34.2% of respondent women in the first and second trimester, respectively, had made an ANC visit (Fig1). Among those who had an ANC visit, the median gestational age at the first ANC visit was 5 months. The total number of ANC visits made by respondents in the third trimester of pregnancy (n=47) were further examined. While 43.5% of the respondents attended ANC at least once, only 6.1 % made the recommended minimum of four ANC visits (Fig1).
Table 2: Frequency and percent distribution of pregnant women by number of antenatal care visits during current pregnancy
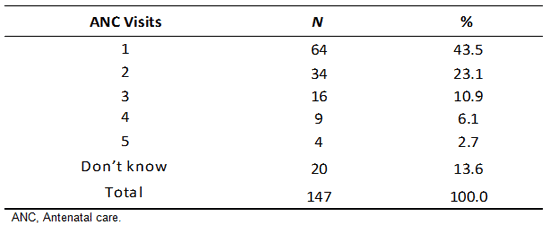
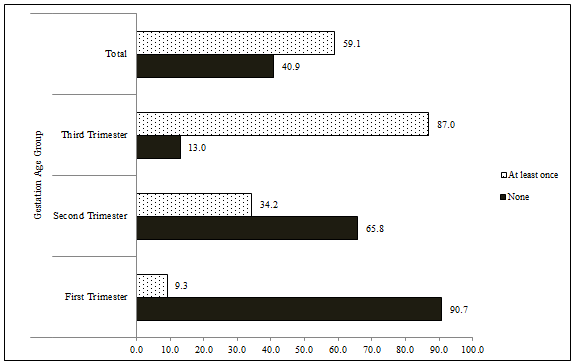
Figure 1: Percent distribution of pregnant women by frequency of antenatal care visit and gestation age group.
Iron/folic acid (IFA) supplementation: Forty-eight percent of the respondents had never taken IFA but 13.2% women had taken IFA during the current pregnancy (Fig2). Among those who had taken IFA during the current pregnancy, only 9 of 40 respondents knew how many pills they had taken.
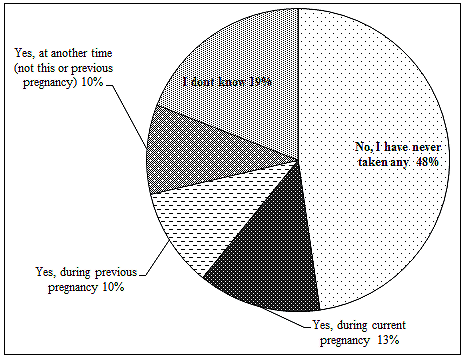
Figure 2: Percentage of respondents based on whether they had taken iron and folic acid.
Intermittent preventive treatment of malaria: Less than half of the respondents (45.4%) reported having taken anti-malarial prophylaxis (Table 3). Of those, only 4.3% had received the recommended two doses during both second and third trimesters of pregnancy, with the majority (54.9%) receiving only one dose of IPT and within the second trimester.
Table 3: Percent distribution of respondents by intermittent treatment of malaria

Use of insecticide treated nets and de-worming medicine: Only 1 in 5 pregnant women slept under mosquito nets (Fig3). Only 14.5% of respondents had received any de-worming medication although majority of respondents were already in the third trimester of pregnancy.
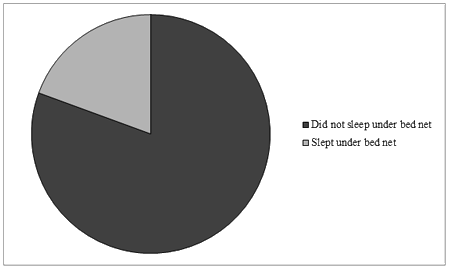
Figure 3: Proportion of respondents who slept under any bed net the previous night.
Association between anaemia and selected background characteristics
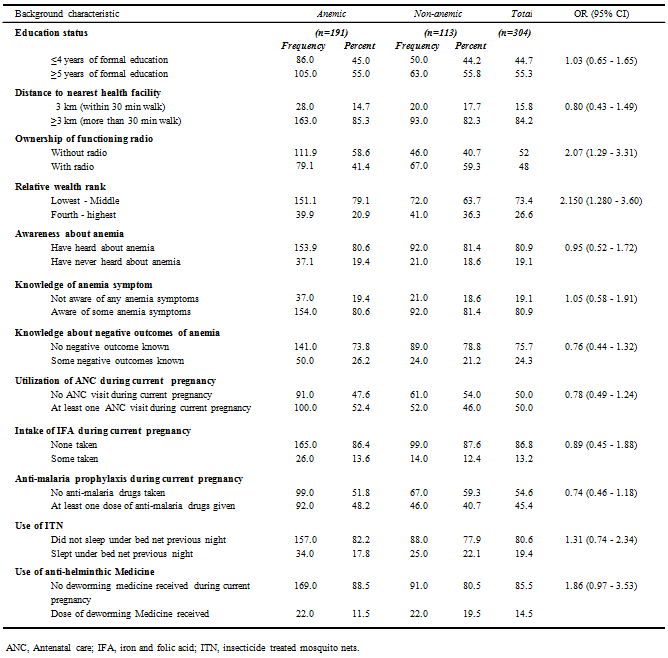
Bivariate analysis: Most factors did not have significant influence on the anaemia status of respondents (Table 4). However, ownership of radio and relative wealth ranking exhibited some influence on anaemia status (p<0.05). The results suggest that those without a functioning radio were 2.07 times more likely to have anaemia than those who had a functioning radio. Pregnant women from households in the lower three relative wealth quintiles were 2.15 times more likely to have anaemia than those from higher category rankings. Women who had not received de-worming medicine during their current pregnancy were 1.86 times more likely to be anaemic compared with those who had received a de-worming tablet, the association was, however, not found to be statistically significant.
Table 4: Bivariate analysis of factors associated with anaemia status among pregnant women in Kiboga district
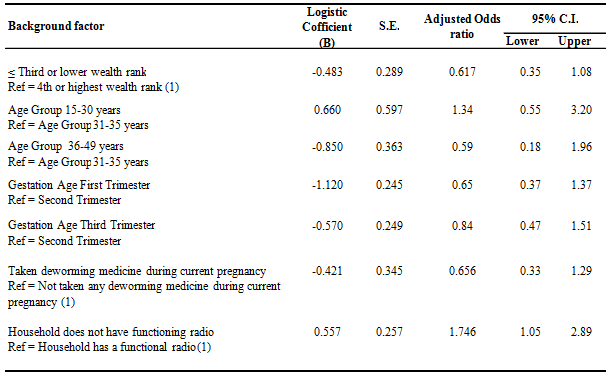
Multivariate analysis: Results of the multiple regression analysis are presented (Table 5). The regression model shows that radio ownership was the only factor that was associated with anaemia status (p=0.024).
Table 5: Multivariate analysis of factors associated with anaemia status among pregnant women in Kiboga district
Discussion
The occurrence and aetiology of anaemia during pregnancy are well established20. Nonetheless, effective control of anaemia requires empirical data about prevalence and interplay of causative factors in each country and locality, especially against a background of diminishing health intervention expenditure. The observed high anaemia prevalence among pregnant women in Kiboga was greater than the average (57.1%) reported for the Africa region21, but consistent with the 64.4% reported by the Uganda Demographic and Health Survey6. The results of this study provide more evidence of the confluence of well-established underlying factors among all population groups, and more so among those who are pregnant.
Since 2001 the Uganda government has been implementing a minimum public-healthcare package for prevention of anaemia among pregnant women. The results of this study indicate that the uptake of this package has been inadequate. The minimum public healthcare package is available at health centres and, therefore, requires pregnant women to make regular ANC visits. Due to low rates of ANC visits, most pregnant women miss anaemia interventions and health education sessions. The low ANC attendance registered in this study is consistent with those of the recent UDHS which reported that only 17% of women have their first ANC visit in the first trimester and only 47.2% have four or more antenatal visits as recommended by the Uganda Reproductive Health Policy Guidelines22. A number of studies have assessed factors leading to low and late ANC in Africa. According to Asiimwe, affordability in terms of physical inability to travel long distances, transport and other related costs explains the limitations to more ANC visits, even when free health services are available23. Additionally, late ANC attendance is associated with a perceived lack of services and relevant medicines at these health centres24. This study established that more than half of the pregnant women in Kiboga are more than a one hour's walk (5 km) away from the nearest healthcare facility. The results also showed that the ANC services received by the women were not at a satisfactory standard. Such factors were possible reasons for the low ANC attendance in Kiboga. According to a study by Mwadime, almost 80% of the women complained of long waiting times at the ANC clinics, but said that they did not mind this as long as they received the services and 'medicines' they expected25. It is important to ensure that the pregnant women receive all required ANC services at healthcare centres after travelling long distances.
Based on the results of this study, reducing road distances to healthcare centres is a worthy consideration for improving ANC utilization and, implicitly, reduction of anaemia during pregnancy. However, in the context of constrained national budgets in resource-poor countries like Uganda, alternative approaches must be considered that integrate health care and nutritional education in poverty eradication programs. For example, community mobilization such an approach in women's microfinance support activities could contribute to reduced anaemia prevalence through increased ANC attendance. According to Garg, Gupta et al, a similar approach implemented in Wardha India increased ANC and health-facility deliveries from 11.6% to 25.0% and 79.0% to 90.0%, respectively26.
Even in developed countries where diets are largely optimal with respect to total iron content and bioavailability, daily iron requirements for pregnant women cannot be met from dietary sources alone27. Consequently, daily supplements of iron and folic acid has been universally recommended28. Under Uganda's current regime of implementing anaemia-reduction interventions through healthcare facilities, the low ANC attendance found in this study implies that access to and use of IFA supplements is low among pregnant women, consistent with the 2006 UDHS that found only 0.7% of pregnant women in Uganda had taken the recommended minimum IFA. The present study found 13.2% IFA use rate, which was considerably lower than the overall ANC attendance (22.5% by third trimester). This implies other barriers to IFA intake, even within increased ANC attendance.
Prevention and control of malaria using the IPT approach is another essential component of the Uganda Government's intervention package to combat anaemia during pregnancy, given that malaria is one of the major causes of anaemia in endemic countries like Uganda29. As with IFA use, IPT coverage in Kiboga was unacceptably low and the results indicate that this was a result of low overall ANC attendance, and is in agreement with the 2006 UDHS which reported national IPT coverage of 36.6%6. Intermittent preventive treatment is a directly observed therapy which should be taken by pregnant women at the ANC in the presence of health workers. Hence, the low uptake of IPT suggests that either health workers did not provide IPT services or they did not give appropriate advice during ANC sessions, so many women do not return for follow-up doses.
Another strategy for malaria prevention and control among pregnant women advocated by Uganda is the promotion of ITNs. The study results show that use of ITNs, indeed any beds nets, was very low among pregnant women, in agreement with the 2006 UDHS which reported that only 23.2% of pregnant women had slept under any bed net the night before interview. The average price of US$5 per bed net means that few households can afford to provide these for pregnant women or other members of the household. This further underlines the need to integrate public health interventions against anaemia with anti-poverty strategies.
Helminths infestations are a major cause of anaemia among all population groups in resource-low communities30-32. This has merited the use of anti-helminths drugs during pregnancy as part of the broader strategy to prevent and control anaemia18. Providing anti-helminths drugs during the second trimester is, thus, part of Uganda's public health intervention package against anaemia in pregnancy. The results of this study showed that, as with IFA and IPT use being dependent on ANC visits, the majority of pregnant women in Kiboga had not received any anti-helminths drugs. According to Brooker et al, in many developing countries it is policy that pregnant women receive anti-helminths treatment but, in practice, coverage rates are often unacceptably low33. It can be argued, therefore, that without improvement in ANC attendance, de-worming may not result in a reduction of anaemia among pregnant women in Kiboga.
Knowledge is the springboard for action34. The results of the study establish that awareness of anaemia as a health problem during pregnancy is relatively widespread in Kiboga district. However, there was low awareness about the negative outcomes of anaemia, especially the long-term effects on the child's growth and development. Since it is believed that increasing awareness motivates behavioural change, it is possible that limited knowledge about the negative outcomes of anaemia interferes with ANC attendance, IFA use, dietary practices, and the use of anti-helminths medicine.
Concerning knowledge of iron rich foods, the study findings showed that only a small proportion of pregnant women could positively identify a food rich in iron. Organ meat and red meat were rarely known to be rich sources of iron. Pregnant women are supposed to be given nutrition education as early as possible during pregnancy with ANC visits as the main channel for this delivery35. The low levels of awareness about these aspects can, therefore, be attributed to low ANC attendance by pregnant women. It is also possible that even if women attend ANC, nutritional education sessions may not be available. Mwadime et al reported that the workload within health facilities deprives health workers of sufficient time to carry out meaningful health and nutritional education36.
Regarding attitudes, pregnant women may believe there are no advantages in attending ANC in the first 3 months of pregnancy37, because ANC is viewed primarily as curative, rather than preventive. Neema reported that pregnant women do not have confidence in the health system because of inadequate services and medicines, which in part contributes to the high usage (73%) of traditional indigenous medicine as an alternative to ANC in Uganda38. It is possible that such attitudes and misconceptions contribute to the high prevalence of anaemia among pregnant women in Kiboga. Thus, apart from availing all ANC services and medicines at health facilities, community based health education programs are needed to correct negative attitudes and misconceptions about ANC.
In a bivariate analysis, the study found that anaemia prevalence was significantly affected by only two (among several) factors: relative wealth ranking and radio ownership. Poverty with its implications underlies most of the anaemia cases39,40. Poverty reduces timely access to accurate information. Poverty translates into limited access to adequate and nutritious food at both household and individual levels39. Further, foods that are rich in available iron (red meats, organ meats, fish and poultry) are expensive and not affordable to those in the lower ranks of society41. Strategies for the prevention of anaemia among pregnant women and other population groups must, therefore, be integrated with poverty-reduction programs at household level.
In a multivariate analysis, only radio ownership was found to be significantly associated with anaemia prevalence. These findings underscore the importance of access to right and targeted information, education and communication in the reduction of anaemia. Radio transmission has been frequently used to educate the public about various aspects of health, including the prevention and control of anaemia, and is still by far the most dominant mass medium in use in Africa42. The use of radios for health education should be strengthened for better outcomes of anaemia programs.
The high prevalence of anaemia observed in Kiboga district can be attributed to poverty and limited access to nutrition and health education information, leading to low uptake and utilization of the public health intervention package to combat anaemia in pregnancy. The health-facility based anaemia prevention and control package alone may not be effective in combating anaemia among pregnant women. Approaches that integrate health and nutrition education into poverty eradication strategies need to be designed, confirmed and adopted.
Acknowledgement
The authors acknowledge that funding for this research was from the A2Z USAID Micronutrient and Child Blindness Project.
References
1. Zavaleta N, Caulfield L, Garcia T. Changes in iron status during pregnancy in Peruvian women receiving prenatal iron and folic acid supplements with or without zinc. Journal of American Nutrition 2000; 71: 956-961.
2. Bothwell T H. Iron requirements in pregnancy and strategies to meet them. American Journal of Clinical Nutrition 2000; 72(1): 257S-S264.
3. Beaton GH. Iron needs during pregnancy: do we need to rethink our targets? American Journal of Clinical Nutrition 2000; 72(1): 265S-271S.
4. McLean E, Egli I, Wojdyla D, Cogswell M, de Benoist B. Worldwide Prevalence of anaemia in preschool aged children, pregnant women & non-pregnant women of reproductive age. (Online) 2006. Available: www.a2zproject.org/pdf/ (Accessed 12 June 2012).
5. WHO. Worldwide Prevalence of Anaemia 1993-2005: WHO Global Database on Anaemia. (Online) 2008. Geneva: World Health Organization. Available: http: //whqlibdoc.who.int/publications/2008/9789241596657_eng.pdf (Accessed 12 June 2012).
6. Uganda Bureau of Statistics. Uganda Demographic and Health Survey, 2006. Kampala: Uganda Bureau of Statistics, & ORC Macro International, 2006.
7. Uganda UNGASS. Progress Report: Jan 2008-Dec 2009. (Online) 2010. Available: http: //data.unaids.org/pub/Report/2010/uganda_2010_country_progress_report_en.pdf (Accessed 6 January 2013).
8. Volberding PA, Levine AM, Dieterich D, Mildvan D, Mitsuyasu R, Saag M. Anaemia in HIV infection: clinical impact and evidence-based management strategies. Clinical Infectious Diseases 2004; 38: 1454-1463.
9. Poggi SBH. Postpartum hemorrhage and abnormal puerperium. In: AH DeCherney, L Nathan, TM Goodwin, N Laufer (Eds); Current Diagnosis and Treatment, Obstetrics and Gynecology, 10th edn. New York: NY: McGraw-Hill Medical, 2007; 477-484.
10. Allen LH, de Benoist B, Dary O, Hurrell R. Guidelines on food fortification with micronutrients. Geneva: World Health Organisation, 2006; 3-15. Available: http: //www.who.int/nutrition/publications/guide_food_fortification_micronutrients.pdf (Accessed 11 June 2012).
11. Nasreen H, Ahmed SM, Begum HA, Afsana K. Maternal, neonatal and child health programmes in Bangladesh: review of good practices and lessons learned. Series 32 research monograph. Dhaka: BRAC Center, 2010.
12. Khan KS, Wojdyla D, Lale S, Gulmezoglu M. Van Look P. The World Health Organisation Analysis of Causes of Maternal Deaths: A Systematic Review. Lancet 2006; 367: 1066-1074.
13. Uganda Bureau of Statistics. Uganda Demographic and Health Survey. Kampala: Uganda Bureau of Statistics, & ORC Macro International, 2001; 159-161.
14. Uganda Bureau of Statistics. Uganda Population and Housing Census Population Size and Distribution, 2002. Kampala: Uganda Bureau of Statistics, 2002.
15. Leslie K. Survey Sampling. New York: John Wiley, 1965; 216-219.
16. von Schenk H, Falkensson M, Lundberg B. Evaluation of "HemoCue", a new device for determining hemoglobin. Clinical Chemistry 1986; 32(3): 526-529.
17. Meda N, Mandelbrot L, Cartoux M, Dao B, Ouangre A, Dabis F. Anaemia during pregnancy in Burkina Faso, West Africa: Prevalence and associated factors. Bulletin of the World Health Organization 1999; 77: 11-12.
18. WHO. Opportunities for Africa's newborns. Geneva: World Health Organization, 1999. Available: http: //www.who.int/pmnch/media/publications/oanfullreport.pdf (Accessed 11 June 2012).
19. Wagstaff A, Watanabe N. What difference does the choice of SES make in health inequality measurement? Health Economics 2003; 12(10): 885-890.
20. Crawley J. Reducing the Burden of Anaemia in Infants and Young Children in Malaria Endemic Countries of Africa: from evidence to action. American Journal of Tropical Medicine and Hygiene 2004; 71(2): 25-34.
21. Klemm R, Sommerfelt AE, Boyo A, Barba C, Kotecha P, Steffen M et al. Are we making progress on reducing anaemia in Women? Cross-country comparison of anaemia prevalence, reach, and use of antenatal care and anaemia reduction Interventions. Washington, DC: Academy for Education Development, 2011; 31-35. Available: http://a2zproject.org/pdf/ReducingAnemia_low_res_06212011.pdf (Accessed 11 June 2012).
22. Ministry of Health. The National Policy Guidelines and Service Standards for Sexual and Reproductive Health and Rights, 2006. Kampala: Ministry of Health, 2006.
23. Asiimwe KJ. Utilization of Antenatal Services among adolescents in Western Uganda. MSc Dissertation. Kampala: Makerere University, 2004.
24. van Eijk AM, Ayisi JG, ter Kuile FO, Slutsker L, Otieno JA, Misore AO et al. Implementation of intermittent preventive treatment with sulphadoxine-pyrimethamine for control of malaria in pregnancy in Kisumu, western Kenya. Tropical Medicine and International Health 2004; 9(5): 630-637.
25. Mwadime RKN, Harvey WJ, Naikoba S, Sserunjogi L, Bachou H, Arinaitwe L et al. Overcoming barriers to effective maternal anaemia interventions during antenatal services in Uganda. Arlington, VA: MOST Project, 2002. Available: http: //www.a2zproject.org/~a2zorg/pdf/Overcoming%20Barriers.pdf (Accessed: 12 June 2012).
26. Garg BS, Gupta SS, Datta SS, Boratne A, Chauduri M, Gandhi A. Community-led Initiatives in child survival (CLICS). In: Annual Report 2006. Wardha, Maharashtra: Aga Khan Foundation, 2006; 11-29. Available: http: //nipccd.nic.in/mch/fr/vhc/erl9.pdf (Accessed 11 June 2012).
27. Bendich A, Zilberboim R. Iron and women's health. In: S Yehuda, DI Mostofsky (Eds); Iron deficiency and overload: from basic biology to clinical medicine. New York: Humana, 2009; 337-350..
28. Stoltzfus RJ, Dreyfuss ML. Guidelines for the use of iron supplements to prevent and treat iron deficiency anaemia. Washington, DC: ILSI Press, 1998. Available: http: //www.who.int/nutrition/publications/micronutrients/guidelines_for_Iron_supplementation.pdf (Accessed 12 June 2012).
29. Ekejindu IM, Okeke EK, Akah B, Okpala E, Ezeagwuna DA, Onwurah O. Malaria and hookworm co-infection among pregnant and non-pregnant women in a semi-urban area in Anambra State, Nigeria. Journal of Medical Sciences 2011; 6(1): 33-35.
30. Smith JL, Brooker S. Impact of hookworm infection and deworming on anaemia in non-pregnant populations: a systematic review. Tropical Medicine and International Health 2007; 712 (12): 1515-1523.
31. Ayub J. Association of anaemia with parasitic infection in pregnant Nepalese women: results from a hospital based study done in eastern Nepal. Journal of Ayub Medical College Abottabad 2005; 17(1): 5-9.
32. Brooker S, Hotez PJ, Bundy DAPS. Hookworm-related anaemia among pregnant women: a systematic review. PloS Neglected Tropical Diseases 2008; 2(9): e291.
33. Brooker S, Hotez PJ, Bundy DA. Hookworm-related anaemia among pregnant women: a systematic review. PLoS Neglected Tropical Diseases 2008; 2(9): e291.
34. Family Health International. Behavior change - a summary of four major theories. (Online) 2004. Available: http://www.fhi360.org/sites/default/files/media/documents/Behavior%20Change%20%E2%80%93%20A%20Summary%20of%20Four%20Major%20Theories%20%281996%29.pdf (Accessed 30 April 2013).
35. Ministry of Health. Health Sector Strategic Plan II- 2005/06-2009/2010. Kampala: Ministry of Health, Government of Uganda, 2005.
36. Mwadime RKN, Harvey P, WJ, Sserunjogi L. Improving the Performance of Maternal Anaemia Interventions in Africa. Arlington, VA: MOST Project, 2004. Available: http: //www.a2zproject.org/~a2zorg/pdf/AFRAnaemia Intrvntions.pdf (Accessed 12 June 2012).
37. Ndidi EP, Oseremen IG. Reasons given by pregnant women for late initiation of antenatal care in the Niger Delta, Nigeria. Ghana Medical Journal 2010; 44(2): 47-51.
38. Neema S. Mother and midwives: maternity care options in Ankole southwest Uganda. (PhD thesis). Copenhagen: University of Copenhagen, 1994.
39. Semba RD, Kumwenda N, Hoover DR, Taha TE, Mtimavalye L, Broadhead R. Assessment of iron status using plasma transferrin receptor in pregnant women with and without human immunodeficiency virus infection in Malawi. European Journal of Clinical Nutrition 2003; 54: 872-877.
40. Karaoglu L, Pehlivan E, Egri M, Deprem C, Gunes G, Genc MF et al. The prevalence of nutritional anaemia in pregnancy in an east Anatolian province, Turkey. BioMedical Public Health Journal 2010; 10: 329.
41. Demment MW, Neumann CG, Nimrod OB, Murphy SP, Allen LH, Sigman M et al. Animal source foods improve dietary quality, micronutrient status, growth and cognitive function in Kenyan school children. Journal of Nutrition 2003; 133: 3941S-3949S.
42. Madzingira N. Culture, Communication and Development in Africa. Institute of Development Studies, University of Zimbabwe. (Online) 2001. Available: http: //unpan1.un.org/intradoc/groups/public/documents/IDEP/UNPAN003348.pdf (Accessed 12 June 2012).

