full article:
Rural Appalachian food deserts have some of the highest cardiovascular disease (CVD) morbidity and mortality rates in the USA1. A rural food desert is defined as a low-income census tract (having either a poverty rate of 20% or higher, or a median family income at or below 80% of the area's median family income) where a substantial number of residents have limited access to a supermarket or large grocery store. Limited access is defined as at least 500 people and/or at least 33% of the census tract's population residing more than 16 km (10 miles) from a supermarket or large grocery store2. Diet plays a significant role in the development of CVD and the Mediterranean diet (MD) is one of the most cost-effective means of decreasing CVD risk. The antioxidants, fiber and fatty acids in the MD work in synergy to decrease low-density lipoprotein (LDL) cholesterol, triglycerides and inflammation while increasing protective high-density lipoprotein (HDL) cholesterol3,4. The MD pattern meets the guidelines of My Plate (the current nutrition guide published by the US Department of Agriculture) recommendations and is also high in unsaturated fatty acids, particularly olive and nut oils, which provide additional health benefits5,6. The MD also consists of fish as a frequent protein source and high omega-3 polyunsaturated fatty acid fish are available in rural Appalachian grocery stores.
Access to fresh fruits and vegetables, which are plentiful in an MD, can be difficult for many residents in rural Appalachia. Although some individuals living in this region plant seasonal gardens, the Cumberland Plateau, the region in which Kentucky's Appalachian counties are located, has a very rugged terrain and since the introduction of surface coal mining in the 1950s, the majority of farms in the region have disappeared. Many of the Cumberland Plateau counties are considered economically distressed and their economies rank in the worst 10% of the nation's counties7. Cost and access to healthy foods are characteristic barriers in all food deserts but other factors also contribute to poor dietary habits in rural Appalachia.
Identification of specific barriers to dietary change is necessary prior to the development of interventions aimed at increasing consumption of foods known to decrease CVD. The purpose of this study was to identify predisposing, reinforcing and enabling factors associated with eating an MD in a rural Appalachian food desert with disproportionately high rates of CVD. The secondary aim was to assess whether the factors varied based on age, gender and socioeconomic status.
Background and significance
Breathitt County, located in southeastern Kentucky, is a rural Appalachian food desert and 54% of residents have difficulty accessing healthy foods8. Breathitt ranks as one of the least healthy Kentucky counties with a cardiovascular mortality rate of 540 per 100 000 of population, compared to 409 for the entire state and a national rate of 3261. Poor dietary habits contribute significantly to the population's disproportionately high rate of heart disease.
Breathitt County is classified as 7 in the US Department of Agriculture's Urban-Rural continuum codes, ranging range from 1 (most urban) to 9 (most rural). Breathitt County has a population of 16 100 and is not adjacent to a metropolitan area9. It is one of the state's larger counties geographically at 796.8 km2 (495.1 miles2), with a population density of 21 households per km2 (32.5/mile2)10. Breathitt County has higher unemployment rates than the state and the nation11. At least 30% of employed individuals commute outside the county to more urban counties with greater job opportunities12.
Both grocery stores are located in the county seat, a small town located in the center of the county. Only 14.7% of the county's population lives in the county seat. Those living in the more rural parts of the county commute large distances to a grocery store. For some county residents, the commute to and from the grocery store is more than 97 km (60 miles)13. Although there have been recent improvements in primary roads into the Appalachian region, the majority of roads are still two-lane, secondary and tertiary roads that follow the mountainous terrain14.
The poverty rate in Breathitt County is 33.8%, compared to 16.9% for the state of Kentucky and the national rate of 15.1%15. In December 2011, more than 6000 of the county's 13 878 adult residents received US Supplemental Nutritional Assistance Program or Kentucky Transitional Assistance Program funds16. While cost can be a barrier to healthy eating, 26% of individuals in Breathitt County with limited access to healthy foods have middle to high incomes, indicating that other factors may inhibit food accessibility2. This county has small pockets of residential areas and most have local churches that tend to be social centers for the communities. Several of these churches also serve as free grocery distribution sites and offer free meals on a daily basis.
Healthy food accessibility is further compounded by the limited buying power of rural grocery stores and the inability to stock items that do not sell on a frequent basis. This economic reality creates a reciprocal cycle that results in only foods that are purchased frequently being available to the community. Although one of the two grocery stores in the county offers a 'stock upon request' option, very few community residents request that healthier items be made available for purchase. Dietary patterns are dependent on both individual and environmental factors, particularly in rural areas where socioeconomic factors contribute to poor eating habits. There is extensive evidence that an MD contributes significantly to decreased CVD and chronic disease risk. The MD has anti-inflammatory properties that protect against not only CVD but the majority of chronic diseases17. The plant-based MD is antioxidant-rich, consisting of a high intake of polyunsaturated and monounsaturated fatty acids and a minimal amount of saturated fats18. The MD does not consist of food found only in the Mediterranean, but is a dietary pattern. It includes the following daily intake: ≥5 servings of vegetables (where one serving is equal to œ cup raw or cooked, one cup raw leafy or œ cup vegetable juice); ≥5 servings of fruit (where one serving is equal to œ cup fresh, frozen or canned, Œ cup dried, œ cup juice or one medium-sized piece); ≥6 servings of whole grains (where one serving is equal to one cup dry cereal, œ cup cooked cereal, rice or pasta, or one slice of bread); one serving of yogurt or cheese; and one serving of beans or nuts (œ cup cooked beans, 42.5 g [1.5 oz] of nuts). It also includes at least two 113 g (4 oz) portions of fish weekly. Consumption of alcohol should be limited to one drink (142 g [5 oz] of wine, 340 [12 oz] of beer or 45.5 g [1.5 oz] of liquor) per day for women and two for men19.
The diet of Appalachia, the region in which Breathitt County, Kentucky is located, consists primarily of calorie-dense meats and starches that are often fried or have added animal fats. The top 10 foods identified as important to Appalachians are bacon, biscuits and gravy, chicken and dumplings, cornbread, coffee, fried potatoes, green beans, soup beans, stack cakes and vegetable soup20. These foods also have cultural implications in that they have endured over generations. Although there are very few similarities between an MD and the traditional diet of eastern Kentucky (ie high intake of legumes and some vegetables), a notable difference is the typical fats used in food preparation (ie animal fat added to legumes). The MD can be adapted to regional dietary patterns using locally available foods and altering methods of food preparation. Baking and broiling instead of frying fish, adding legumes and vegetables to recipes that are family favorites, and using frozen fruits and vegetables, which maintain most of their nutritional value, are methods of adapting current dietary habits into an MD. Fast food restaurants have also increased access to unhealthy foods in many Appalachian food deserts. It is important to assess both intrinsic and extrinsic factors that can impede adherence to this type of diet prior to the development of interventions to increase consumption of an MD.
Theoretical model
The PRECEDE-PROCEED model is based on the assumption that assessment and diagnosis should precede the development of community interventions. In rural communities, the PRECEDE-PROCEED model provides a systematic framework for assessment of all factors that affect health behaviors. The first two phases of the PRECEDE-PROCEED model consist of social and epidemiological assessments, including lifestyle impact on health outcomes. An earlier assessment of dietary patterns and the subsequent impact on cardiovascular biomarkers showed that many individuals in this rural Appalachian food desert do not consume a diet conducive to lower CVD risk. These findings necessitated the third phase of the model, PRECEDE, which includes the educational and ecological assessment.
PRECEDE refers to predisposing, reinforcing and enabling factors that contribute to or impede lifestyle behavior changes. The model also requires community participation in the development and evaluation of interventions. PROCEED refers to the policy, regulatory and organizational factors that affect behavior change21. By helping to identify key intrinsic and extrinsic barriers to behavioral change, participants are able to provide a framework on which interventions may be developed. Local factors such as culture, history and political climate, which play significant roles in food availability and choice, may be difficult to evaluate without the use of a comprehensive assessment model and interventions that do not consider these factors may be less likely to be effective health promotion strategies21.
Barriers to behavior change can be at the individual, family and environmental levels and recognition of the level of barriers dictates the intervention to be targeted22-25. In the PRECEDE component of the model, predisposing factors include knowledge, attitudes, beliefs, values, self-efficacy, intentions and skills21. Factors such as genetics and demographics are recognized as contributing to behavior change, but are treated as a special subcategory because they are not amenable to change. Reinforcing factors include feedback, both positive and negative, from significant others and rewards for behavior change21. Enabling factors include the availability, accessibility and affordability of resources that support or impede sustained behavior changes21.
Community engagement is critical during the assessment of factors that promote or impede health practices. Discussion suppers have successfully engaged rural communities in the development and implementation of lifestyle behavior programs that improve nutrition26. Meals served during focus groups also provide a relaxed atmosphere and promote communication27. In this study, a locally-prepared, catered meal served as a means to introduce a regionally-adapted MD.
Procedure
This cross-sectional mixed-methods convergent parallel study was undertaken from November 2011 to January 2012. This design was chosen so that participants could provide themes related to healthy eating barriers identified through personal experience and be able to quantify those themes by ranking them based on priority. Nominal group technique was used to familiarize participants with the MD and assess factors associated with adopting an MD. This technique generates more ideas than traditional discussion groups and allows groups to appropriately prioritize factors that affect diet28.
Pastors from four Breathitt County churches whose members had previously participated in studies with this investigator were contacted to establish interest. Churches were chosen from low and middle socioeconomic status areas of the county in order to recruit individuals within a range of household incomes. Volunteers were excluded if they were less than 21 years of age. The MD includes moderate alcohol consumption and it was anticipated that should alcohol consumption emerge as a discussion topic, only individuals of legal drinking age in Kentucky should participate. Using purposive sampling, four groups of 8-12 participants (n=43) each were recruited from the four churches. A recruitment announcement was made following Sunday morning services by the study investigator, a native of this Appalachian county. Volunteers provided contact information on a card and age eligibility was determined during a phone call by the investigator.
One nominal group session of 8-12 participants was conducted in the community kitchen areas at each of the four churches. The MD was explained to participants using an illustrated pamphlet. Participants were not given an in-depth explanation of the MD because predisposing factors can be remedied through educational interventions and part of the purpose of the study was to determine if individuals had preconceived notions of what constitutes an MD. A meal was prepared by a local caterer and included plant-based dishes of locally available food prepared with unsaturated fatty acids. Toward the end of the meal, participants were asked to answer the question written on a flip chart, 'What would have to change in order for you to, almost daily, eat a Mediterranean-style diet?'. Participants were instructed that if they were currently eating an MD, they should write down what would have to change in order for it to be easier for them to continue eating an MD. Each group member wrote down as many answers as appropriate and then presented one answer at a time in a round robin format. Answers were recorded by a registered nurse and read back to the group for clarification. The entire list of answers was discussed and questions clarified after all members had responded. Duplicate answers were collapsed into a single category. Group members were then asked to rate each item from not important to top priority. Each participant ranked the seven factors by priority, with a score of 7 as the most important factor and a score of 1 as the least important. Data on age, gender, household income and educational status were collected at the beginning of the session.
Analyses
Statistical Package for Social Sciences v18 (SPSS Inc; www.spss.com) was used to perform descriptive statistics and to determine mean priority scores for each factor. Multivariate ANOVA and independent t-tests were performed to determine if there were significance differences in factors affecting future adherence to an MD by age, gender, household income and educational level. All p values of ≤0.05 were considered significant.
Ethics approval
The study was approved by the University of Kentucky Medical Institutional Review Board (approval number 11-0709-P3H), which required letters of support from church officials and documented assurance of research ethics integrity by all members of the research team.
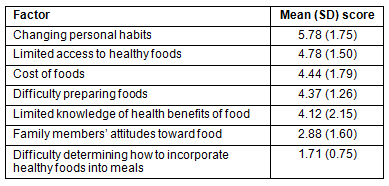
A total of 62% of participants were female with a mean age of 48.3 ± 18.0 years; 67% had at least an associate college degree and 39.6% reported a household income of <$35,000 (Table 1). The median age of Breathitt County residents is 40.7 ± 0.7 years and 48.4% are women. Predisposing, enabling and reinforcing factors that affect dietary choices were evaluated during the group sessions (Table 2) and were ranked by priority. These included (i) difficulty changing personal habits; (ii) limited access to healthy foods; (iii) cost; (iv) difficulty of preparation; (v) limited knowledge of health benefits of foods; (vi) family attitudes toward food; and (vii) difficulty determining how to incorporate healthy foods into meals (Table 3).
Table 1: Participant characteristics (n=43) and characteristics of county residents
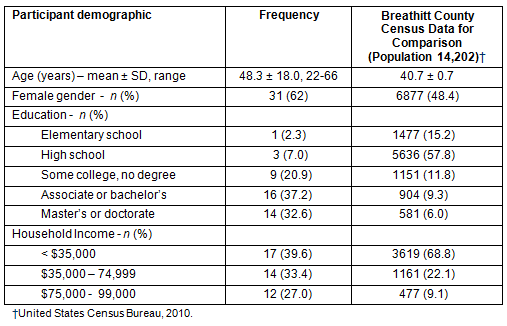
Table 2: Factors reported to affect the ability to adopt and adhere to a Mediterranean diet in a rural Appalachian food desert

Table 3: Priority score of factors reported to affect the ability to
adopt and adhere to a Mediterranean diet in an Appalachian food desert
ANOVA and t-test results are reported in Table 4. Younger participants and those with lower (<$35,000) incomes were more likely to identify food cost as a barrier to adherence compared to those who were older or with higher incomes. Participants with lower educational levels (no college degree) were more likely to report that family members' attitudes would be a factor in ability to adopt an MD (Table 4). Women were more likely than men to report knowledge of the health implications of foods (t = -7.18, p<0.000). Personal habits, limited access to healthy foods, difficulty of food preparation and difficulty in determining how to incorporate healthy foods into the diet did not vary based on age, gender or socioeconomic status.
Table 4: Participants' characteristics that affect factors that influence dietary choice

Discussion
Personal habits, limited access to healthy foods, food cost, difficulty of preparation, limited knowledge of health benefits of foods, family members' attitudes toward food and difficulty determining how to incorporate healthy foods into meals were reported as barriers to adopting and adhering to an MD. Younger age and lower income levels were significant in food cost being a barrier to healthy eating. Concern that family members' attitudes would hinder eating an MD was influenced by lower educational levels and men were less likely than women to understand the health implications of diet. Factors that affect the ability to adopt an MD were both individual and environmental. In this study, while cost and access were perceived as problems in the environment, other factors, such as personal habits and family acceptance, are more amenable to change through education and motivational strategies.
Successful strategies targeting nutrition would need to consider the influence of age and socioeconomic status on the perception that healthy eating is costly as well as the influence of educational status on how individuals expect family members to react to healthier menus. Programs that specifically target men's knowledge of the health benefits of foods may also be beneficial in changing dietary habits.
Several of the predisposing, reinforcing and enabling factors reported by participants in this study as barriers to eating an MD can be addressed using social cognitive strategies. Community-based programs that have multifaceted targets tend to be much more successful in altering dietary patterns than those programs that target only one contributing factor29-31. Therefore, all contributing factors that affect diet must be identified and assessed prior to development and implementation of community-based health promotion interventions. Social cognitive theory posits that human behavior is explained in a triadic and reciprocal model in which behavior, personal factors and the environment all interact to influence behavior.
Predisposing factors
Predisposing factors included a limited knowledge of health benefits of food and difficulty in determining how to incorporate healthy foods into meals. Changing personal habits, the most highly rated factor, is also a predisposing factor that affects dietary choice. Self-efficacy is key to sustaining healthy lifestyle behaviors and unless people believe they have the ability to achieve the desired results, they may have little to no incentive to act32,33. Both individual and group educational programs that focus on the benefits of healthy eating and instructions on how to incorporate healthy foods into the diet may be successful in changing dietary habits and, subsequently, lowering chronic disease risk34,35.
Establishing formalized nutrition classes presented by cooperative extension agents (as part of the US Cooperative Extension System) or local health department staff may be an effective strategy in changing dietary habits in rural communities. These classes can also be presented at local churches for individuals in more remote areas. Media campaigns, social marketing at the local level and group education are all effective in changing behavior related to healthy living36-38. Healthy-eating commentaries in local newspapers and a free 'shopper' newsletter could also disseminate information pertaining to healthy foods and methods of food preparation that afford the greatest protection against chronic disease. Male participants in this study were less likely than women to understand the health implications of eating an MD and providing information specifically related to men's health could potentially improve the likelihood of men adopting an MD. Cooperative extension agents often write regular columns in local newspapers or host radio shows in rural communities. In particular, a 'men's health' column might be beneficial in providing information related to the health benefits of certain foods.
Reinforcing factors
The reinforcing factor in this study was family attitudes toward healthy foods. Successful strategies to improve acceptance of dietary change are those that involve the entire family with the parent as a role model of behavior39. By providing learning opportunities for all family members, there may be less resistance to change as each member becomes a stakeholder in the sustained behavioral change40. Individuals often tend to revert back to previous nutritional patterns even if successful in changing eating habits initially41. Therefore, family education and participation in nutritional programs over a sustained period of time may be more successful in producing sustained dietary change. Family member involvement in local faith-based and/or cooperative extension programs may serve as an avenue to improve acceptance of new foods and/or methods of food preparation.
Educational level influenced how participants thought family members would react to changes in their current diet. Interventions tailored to those with lower levels of education and that include subtle, incremental changes to diet may be more successful than programs that promote a drastic dietary change over a very short period of time. Incorporating healthy foods into favorite family meals may be met with less resistance from family members.
Enabling factors
Enabling factors were cost, accessibility and difficulty in preparing foods. Grocers in these regions have limited buying power and may not be able to absorb the cost of stocking a greater variety of healthy foods without an increase in sales of those foods. The population density and poverty level in rural communities may contribute to poor dietary practices due to limited access to fresh produce. Many of the produce items that offer the greatest protection against CVD have a very short lifespan and spoil quickly42. Individuals with limited incomes and those who live in remote areas may not be able to afford the frequent grocery store commutes required to have fresh fruits and vegetables on a regular basis. For this reason, many people purchase canned fruits and vegetables, which provide fewer health benefits due to loss of nutrients during processing43. In the USA, nearly 20% of all produce is lost to spoilage each year44. Farmer to consumer loss for some produce, such as apples, is up to 45%, with 29% being at the consumer level45. Individuals who have limited incomes may not risk the loss to their food budget. Frozen fruits and vegetables, which retain much of their nutrient quality if stored at -18°C, may be an option for individuals with fewer opportunities to access fresh fruits and vegetables45.
Eating several servings of fruits and vegetables daily is a hallmark of the MD and an effective strategy in decreasing CVD risk. Participants reported that difficulty in preparing food was a factor that impeded eating a healthier diet. Increased availability of fruits and vegetables does not always result in increased consumption46. However, fruits and vegetables are consumed more frequently when they are either easy to prepare or are purchased ready-to-eat47,48. Facilitation strategies provide the necessary skills and tools to achieve behavior change. Basic fruit and vegetable preparation tools provided during cooking classes may facilitate consumption of more home-prepared produce during meals Enhanced awareness of the nutritional value of foods is an effective strategy in dietary change49,50. Social marketing strategies that help consumers identify less costly, healthy foods can be used to increase consumption of locally available risk-reducing foods. In more urban areas, home grocery delivery is an effective strategy in altering the home food environment to promote weight loss51. Development and testing of a grocery delivery service in rural food deserts is warranted to improve dietary habits and, subsequently, decrease CVD risk. While cost of delivery would be problematic for many rural residents, a policy (eg the Supplemental Nutritional Assistance Program) could be adopted to cover the costs of home delivery if it is found to be a successful strategy for improving nutrition.
In rural communities where a significant percentage of employed residents must commute, fast food is often a convenient, time-saving option. However, time constraints may not be a predictor of preparing meals at home. In a sample of 120 employed mothers, confidence in the ability to prepare a healthy meal was the only significant predictor of a healthy evening meal52. Strategies to assist rural residents to prepare more meals at home, such as cooking meals ahead on the weekends to be served on weeknights and cooking classes that focus on simple, minimal ingredient dishes, may be effective in promoting home cooking and fewer fast food meals.
Fast food marketing has been very successful in promoting high-fat, high-sodium foods and the marketing of healthy foods needs to be as aggressive as campaigns to promote unhealthy foods53. An additional problem in Appalachian food deserts is the marketing of high-fat, high-sodium fast foods as 'healthy menu options' at fast food restaurants based solely on calorie content. It can be difficult for consumers, particularly those living in rural food deserts, to understand exactly which foods contribute to risk reduction when the information presented is misleading.
Future research is needed to determine if healthy, affordable foods are available in rural Appalachian food desert communities and if there are effective strategies to decrease consumption of less-healthy fast food. The PRECEDE-PROCEED model provides the framework for developing effective educational strategies and assessing policy regulations that affect food availability. An important research consideration is to avoid an adversarial relationship with fast food business owners who are also community members and providers of employment. Developing a collaborative relationship with these individuals could result in greater cooperation to increase healthy food options that are acceptable and affordable to members of the community.
Limitations
Study participants were recruited from local churches, which limited the pool of available volunteers to those who may have been more likely to participate in social events, including community discussion suppers. These individuals may also have been more likely to have been participating in healthy lifestyle behaviors at the time of the study. However, this characteristic may have made participants more aware of barriers to healthy eating than others living in the county.
The nominal group process, which included group disclosure of perceived barriers to healthy eating, may have caused some participants to report fewer barriers than actually existed. Participants recorded all perceived barriers and these reports were collected and reviewed following the group discussions to ensure that all factors were noted. All recorded entries were categorized within the factors reported during the group discussions.
Participants in this study were more educated and had higher incomes than the general population. However, sampling resulted in a more even distribution of income status and certain participant-reported factors that affect dietary choice were significantly associated with lower educational level and lower income status. Although the results of this study are limited to people residing in a rural Appalachian area, there are commonalities that affect dietary habits in other rural areas.
In the USA, 13% of all counties are considered food deserts and 98% of these are non-metropolitan areas54. Although there are similar barriers to healthy eating in all regions, there may be unique local factors in rural food deserts. Several factors affected dietary habits in this group of adults living in a rural Appalachian food desert. While cost and accessibility play roles in poor dietary habits, individual factors such as changing personal habits and learning how to recognize and prepare healthy foods were also important. Interventions that target specific factors amenable to social cognitive strategies are more likely to be successful if a systematic assessment is performed prior to the development of community-based programs.
Programs that motivate individuals to change personal habits and improve their knowledge of the health benefits of CVD-risk reducing foods, while accounting for the specific environmental barriers of food cost and accessibility, may be successful in regions where poverty, culture and limited education are factors that affect food choices. Providing the means and methods of incorporating less expensive, locally available healthy foods into family meals and reducing preparation time could be achieved through community cooking classes integrated into faith-based and/or cooperative extension activities. Lowering cost and increasing access to a greater variety of healthy foods in rural food deserts may not be feasible options due to economic issues. However, these factors must be addressed prior to implementing community-based programs aimed at intrinsic factors that impede healthy eating. The results of successful strategies could be used to influence policymakers to find ways to increase access to, and lower the cost of, healthier foods and subsequently reduce CVD burden.
Acknowledgments
The author expresses gratitude to Ellen Hahn, PhD, RN, FAAN of the University of Kentucky College of Nursing for assistance in the preparation of this article.
References
1. Kentucky Institute of Medicine. The health of Kentucky: a county assessment. Lexington, KY. (Online) 2007. Available: http://www.kyiom.org/healthky2007a.pdf (Accessed 24 November 2012).
2. Ver Ploeg M, Breneman V, Farrigan T, Hamrick K, Hopkins D, Kaufman P et al. Access to affordable and nutritious food-measuring and understanding food deserts and their consequences: report to Congress. AP-306. Washington, DC: United States Department of Agriculture Economic Research Service, 2009.
3. De Lorgeril M, Salen P. The Mediterranean diet: rationale and evidence for its benefit. Current Atherosclerosis Reports 2008; 10(6): 518-522.
4. Katcher HI, Hill AM, Lanford JL, Yoo JS, Kris-Etherton PM. Lifestyle approaches and dietary strategies to lower LDL-cholesterol and triglycerides and raise HDL-cholesterol. Endocrinology Metabolism Clinics of North America 2009; 38(1): 45-78.
5. United States Department of Agriculture. Let's eat for the health of it. Home & Garden Bulletin No. 232-CP. (Online) 2011. Available: http://www.choosemyplate.gov/food-groups/downloads/MyPlate/DG2010Brochure.pdf (Accessed 10 October 2012).
6. Urpi-Sarda M, Casas R, Chiva-Blanch G, Romero-Mamani ES, Valderas-Martinez P, Arranz S et al. Virgin olive oil and nuts as key foods of the Mediterranean diet effects on inflammatory biomarkers related to atherosclerosis. Pharmacological Research 2012; 65(6): 577-583.
7. Appalachian Regional Commission. Distressed designation and county economic status classification system, FY2007 - FY 2013. (Online) 2012. Available: http://www.arc.gov/research/SourceandMethodologyCountyEconomicStatusFY2007FY2013.asp (Accessed 10 October 2012).
8. United States Department of Agriculture. Food desert locator. (Online) 2012. Available: http://www.ers.usda.gov/data-products/food-desert-locator.aspx (Accessed 1 October 2012).
9. United States Department of Agriculture. Measuring rurality: rural-urban continuum codes. (Online) 2012. Available: http://www.ers.usda.gov/topics/rural-economy-population/rural-classifications.aspx (Accessed 1 October 2012).
10. United States Census Bureau. Kentucky household density map. (Online) 2010. Available: http://www2.census.gov/geo/maps/dc10_thematic/2010_Profile/2010_Profile_Map_Kentucky.pdf (Accessed 1 October 2012).
11. United States Department of Labor. Unemployment rate in Breathitt County, Kentucky. Washington, DC: Bureau of Labor Statistics, 2012.
12. United States Department of Agriculture. Measuring rurality: rural-urban commuting area codes. Economic Research Service. (Online) 2010. Available: http://www.ers.usda.gov/data-products/rural-urban-commuting-area-codes.aspx (Accessed 1 October 2012).
13. Google Maps. Breathitt County, Kentucky. (Online) no date. Available: http://maps.google.com/maps?hl=en&tab=ll (Accessed 1 October 2012).
14. Kentucky Department of Transportation. Appalachian development highway system. (Online) 2012. Available: http://www.aaroads.com/arc/ (Accessed 26 November 2012).
15. United States Census Bureau. Poverty rates in Kentucky counties. (Online) 2010. Available: http://www.census.gov/prod/2011pubs/acsbr10-01.pdf (Accessed 1 October 2012).
16. Kentucky Cabinet for Human Resources. Statewide summary, 2012. (Online) 2011. Available: http://chfs.ky.gov/NR/rdonlyres/1735C870-040D-41A7-BA2D-58DC7967007C/0/Combined.pdf (Accessed 2 October 2012).
17. Giugliano D, Esposito K. Mediterranean diet and metabolic diseases. Current Opinions in Lipidology 2008; 19(1): 63-68.
18. O'Keefe JH, Gheewala NM, O-Keefe JO. Dietary strategies for improving post-prandial glucose, lipids, inflammation, and cardiovascular health. Journal of the American College of Cardiology 2008; 51(3): 249-255.
19. Tuttle KR, Shuler LA, Packard DP, Milton JE, Daratha K, Bibus DM et al. Comparison of low-fat versus Mediterranean-style dietary intervention after first myocardial infarction (from the Heart Institute of Spokane Diet Intervention and Evaluation Trial). American Journal of Cardiology 2008; 101(11): 1523-1530.
20. Sohn MF. Food origins: regional and cultural roots. In: Appalachian home cooking: history, culture and recipes. Lexington, KY: University of Kentucky Press, 2005.
21. Mohammed, S. Community health analysis and development of health care interventions. Saarbrucken: Verlag Dr Muller Aktiengesellschaft & Co, 2005.
22. Lucan SC, Barg FK, Long JA. Promoters and barriers to fruit, vegetable and fast-food consumption among urban, low income African Americans - a qualitative approach. American Journal of Public Health 2010; 100: 631-635.
23. Withall J, Jago R, Cross J. Families' and health professionals' perceptions of influences on diet, activity and obesity in a low-income community. Health & Place 2009; 15: 1078-1085.
24. Petrovici DA, Ritson C. Factors influencing consumer dietary health preventative behaviours. BMC Public Health 2006; 6: 222-234.
25. Dibonaventura MD, Chapman GB. The effect of barrier underestimation on weight management and exercise change. Psychological Health Medicine 2008; 13(1): 111-122.
26. Faust LA, Blanchard LW, Breyfogle DA, Baroni JK, Reed RE, Young MJ. Discussion suppers as a means for community engagement. Journal of Rural Health 2005; 21(1): 92-95.
27. Krueger RA, Casey MA. Focus groups: a practical guide for applied research, 4th edn. Thousand Oaks, CA: SAGE Publications, 2009.
28. Department of Health and Human Services. Gaining consensus among stakeholders through the nominal group technique, Evaluation Brief #7. Atlanta, GA: Centers for Disease Control and Prevention, 2006.
29. Correa NP, Murray NG, Mei CA, Baun WB, Gor BV, Hare NB et al. CAN DO Houston: a community-based approach to preventing childhood obesity. Preventing Chronic Disease 2010; 7(4): A88.
30. Dharod JM, Drewette-Card R, Crawford D. Development of the Oxford Hills Healthy Moms project using a social marketing process: a community-based physical activity and nutrition intervention for low-socioeconomic-status mothers in a rural area in Maine. Health Promotion Practice 2010; 12(2): 312-321.
31. Wrieden WL, Anderson AS, Longbottom PJ, Valentine K, Stead M, Caraher M et al. The impact of a community-based food skills intervention on cooking confidence, food preparation methods and dietary choices - an exploratory trial. Public Health Nutrition 2006; 10(2): 203-211.
32. Sharp PB, Salyer J. Self-efficacy and barriers to healthy diet in cardiac rehabilitation participants and nonparticipants. Journal of Cardiovascular Nursing 2012; 27(3): 253-262.
33. Piana N, Battistini D, Urbani L, Romani G, Fatone C, Pazzagli C et al. Multidisciplinary lifestyle intervention in the obese: its impact on patients' perception of the disease, food and physical exercise. Nutrition Metabolism and Cardiovascular Disease 2012; http://dx.doi.org/10.1016/j.numecd.2011.12.008 (in press).
34. Sharifirad G, Najimi A, Hassanzadeh A, Azadbakht L. Does nutrition education improve the risk factors of cardiovascular diseases among elderly with type 2 diabetes? A randomized controlled trial based on an educational model. Journal of Diabetes 2012; doi:10.1111/j.1753-0407.2012.00203.x.
35. Endevelt R, Lemberger J, Bregman J, Kowen G, Berger-Fecht I, Lander H et al. Intensive dietary intervention by a dietitian as a case manager among community dwelling adults. Journal of Nutrition and Healthy Aging 2011; 15(8): 624-630.
36. Suarez-Almazor ME. Changing health behaviors with social marketing. Osteoporosis International 2011; 22(3Suppl): S461-S463.
37. Beaudoin CE, Fernandez C, Wall JL, Farley TA. Promoting healthy eating and physical activity short-term effects of a mass media campaign. American Journal of Preventive Medicine 2007; 32(3): 217-223.
38. Dalziel K, Segal L. Time to give nutrition interventions a higher profile: cost effectiveness of 10 nutrition interventions. Health Promotion International 2007; 22(4): 271-283.
39. Scaglioni S, Arrizza C, Vecchi F, Tedeschi S. Determinants of children's eating behavior. American Journal of Clinical Nutrition 2011; 94(6Suppl): S2006-S2011.
40. Schwandt P, Bertsch T, Haas GM. Sustained lifestyle advice and cardiovascular risk factors in 687 biological child-parent pairs: the PEP family heart study. Atherosclerosis 2011; 219(2): 937-945.
41. Hoffman JA, Thompson DR, Franko DL, Power TJ, Leff SS, Stallings VA. Decaying behavioral effects in a randomized, multi-year fruit and vegetable intake intervention. Preventive Medicine 2011; 52(5): 370-375.
42. Produce Marketing Association. The Foodservice guide to fresh produce. TX612.F7F66. Newark, DE: DNAL, 1985.
43. Nicoli MC, Anese M, Parpinel MT, Franceschi S, Lerici CR. Loss and/or formation of antioxidants during food processing and storage. Cancer Letters 1997; 114(102): 71-74.
44. Kantor LS, Lipton K, Manchester A, Oliveira V. Estimating and addressing America's food losses. Food Review 1997; 20(1): 2-12.
45. Buzby JC, Wells HF, Axtman B, Mickey J. Supermarket loss estimates for fresh fruit, vegetables, meat, poultry and seafood and their use in the ER loss-adjusted food availability data. United States Department of Agriculture, Economic Research Bulletin 2009; 44: 1-27.
46. Befort C, Kaur H, Nollen N, Sullivan DK, Nazir N, Choi WS et al. Fruit, vegetable and fat intake among non-Hispanic black and non-Hispanic white adolescents: associations with home availability and food consumption settings. Journal of the American Dietetic Association 2006; 106: 367-373.
47. Delgado-Noguera M, Tort S, Martinez-Zapata MJ, Bonfill X. Primary school interventions to promote fruit and vegetable consumption: a systematic review and meta-analysis. Preventive Medicine 2011; 53: 3-9.
48. Glanz K, Hoelscher D. Increasing fruit and vegetable intake by changing environments, policy and pricing: restaurant-based research, strategies and recommendations. Preventive Medicine 2004; 39(2Suppl): S88-S93.
49. Severi S, Bedogni G, Manzieri AM, Poli M, Battistini N. Effects of cooking and storage methods on micronutrient content of foods. European Journal of Cancer Prevention 1997; 6(1Suppl): S21-S24.
50. Kuo T, Jarosz CJ, Simon P, Fielding JE. Menu labeling as a potential strategy for combating the obesity epidemic: a health impact assessment. American Journal of Public Health 2009; 99(9): 1680-1686.
51. Gorin AA, Raymor HA, Niemeier HM, Wing RR. Home grocery delivery improves the household food environments of behavioral weight loss participants. International Journal of Behavioral Nutrition and Physical Activity 2007; 14 (4): 58.
52. Beshara M, Hutchinson A, Wilson C. Preparing meals under time stress: the experience of working mothers. Appetite 2010; 55(3): 695-700.
53. Harris JL, Schwartz MB, Brownell KD, Sarda V, Ustjanauskas A, Javadizadeh J et al. Fast food FACTS: evaluating fast food nutrition and marketing to youth. Newhaven, CT: Rudd Center for Food Policy and Obesity, 2010.
54. Morton LW, Blanchard TC. Starved for access: life in rural America's food deserts. Rural Sociological Society 2007; 1(4): 1-5.
