Introduction
Indigenous people comprise approximately 2% of the total population of Australia1. Almost 20% of the Indigenous population live in areas classified as 'very remote', compared with only 1% of the non-Indigenous population1. In 1998-1999, an estimated AU$12.45 billion was spent on health services for Aboriginal and Torres Strait Islander people, equating to 2.6% of national health expenditure2. Overall, it was estimated that for each $1 spent on health services for non-Indigenous people, $1.22 was spent on health services for Indigenous people2. Despite this, the health of Indigenous Australians is poor in comparison with the non-Indigenous population. Indigenous people experience lower levels of access to health services than the general population, in some part due to residing further away from health facilities and also as a result of socio-economic status, availability of transport, ability to speak English, and the availability of same-sex Aboriginal Health Workers2. The overall poverty rate among Indigenous families is almost three times that among non-Indigenous families, with half of all Indigenous children living in poverty in 19863.
According to the most recent national survey data, collected in 2001, asthma is the second most commonly reported health condition in the Aboriginal and Torres Strait Islander population. Indigenous Australians reported asthma as a long-term health condition more often than the non-Indigenous population (17% and 12%, respectively)4.
Asthma was identified as a national health priority area in Australia in 1999 following the 1996 introduction of the National Health Priority Areas Initiative. The government announced in the 1999-2000 budget $8 million over three years for new national initiatives in asthma5. The National Asthma Action Plan (NAAP) 1999-20026 was developed in order to provide guidance for how this allocated money should be spent in order to produce maximum impact5.
The NAAP identified priority population groups for asthma, with Aboriginal and Torres Strait Islander (ATSI) peoples highlighted. The plan recognised 'the need for an approach to asthma that takes into account the historical, social, environmental, economic and cultural issues that affect Aboriginal and Torres Strait Islander communities'6.
The asthma management strategies developed by the National Asthma Council in Australia in recent years, including the Six Step Asthma Management Plan and 3+Visit Plan, were designed for all Australians. There have been no Indigenous-specific asthma management programs or approaches officially developed to date.
In 2002 the Commonwealth Department of Health and Ageing commissioned 25 Asthma Innovative Management (AIM) projects that supported good asthma management for target populations and that identified and tested interventions to overcome barriers to effective management. Four of these short-term investigative projects focussed on Indigenous groups as the target population.
As an important component of one of these Indigenous AIM projects, conducted in rural South Australia, a systematic literature review was undertaken to ascertain what was understood about asthma in the Australian Indigenous population.
Methods
Aim
To systematically identify and review literature related to asthma in the Australian Indigenous population in order to determine the extent of previous research efforts, current knowledge about the prevalence and nature of asthma in this population, and the asthma management intervention models previously tested.
Search question
What is the current level of knowledge in the literature concerning asthma in the Aboriginal and Torres Strait Islander population?
Search strategy
This review used the approach described by the National Health and Medical Research Council7, whereby a transparent search strategy is outlined and systematically applied to available databases of published literature and to other available literature sources (using the Internet). The database searches were undertaken in January 2003, and the Internet searches were undertaken in March 2003.
Databases
Computerised bibliographical databases that were accessible through the University of South Australia's library were searched without any year restriction. The databases searched include Cochrane Library; Medline; CINAHL; AUSTROM - ATSIROM, APAIS-Health, Australasian Medical Index, RURAL, Health in Society, DRUG, AusportMED; PubMed; Science Direct; Academic Search Elite; Health Source (Consumer Education, Nursing/ Academic Education); Newspaper Source; PsycINFO; Sociological Abstracts; World Magazine Bank; International Pharmaceutical Abstracts; SPORTdiscus; ATSI-CDROM; ATSIC Library Catalogue; ATSI Health Bibliography; Factiva; Sportsdiscus; Current Contents; AMED; Uncover Plus; Ageline; Ideal (International Digital Electronic Access Library); ProQuest Digital Dissertations; Health and Society Database.
Websites
To reduce publication bias, searching was also undertaken on Internet websites to collect reports not published in academic journals or media. The websites searched included the National Asthma Council, Asthma Australia, Asthma South Australia, Asthma Northern Territory, Office for Aboriginal and Torres Strait Islander Health (an office of the Australian government's Department of Health and Ageing), and the Australian Bureau of Statistics.
Key words
The key words/ phrases used in the search of databases and Internet sites include the following:
- Asthma AND Aboriginal/Aborigin*
- Asthma AND Torres Strait Islander
- Asthma AND Indigenous
Study selection
Very broad criteria for consideration of studies were applied:
- Participants: a participant cohort that included Australian Aboriginal and Torres Strait Islander people of any age
- Interventions: all intervention models included
- Outcome measures: all outcome measures included
- Study design: all designs (both qualitative and quantitative research) were included as well as reviews, abstracts, letters, media releases and published reports
Exclusion criteria
- Studies of Indigenous peoples from other countries such as Canada, New Zealand and America
- Australian Bureau of Statistics publications produced greater than 10 years ago
- Those papers that were not accessible through the University of South Australia or University of Adelaide libraries
- Non-English language studies
Critical appraisal of studies
The READER instrument was used in this study to critically appraise the quality of studies and their relevance to practice in the Aboriginal Medical Service (AMS) setting. This tool was chosen because it is able to evaluate a range of study designs, and has been previously shown to be effective in applying an accurate and repeatable appraisal of studies8,9. It was also selected as it enabled each article to be evaluated in terms of scientific rigour as well as applicability to clinical practice. The tool has four criteria for assessment including Relevance, Education (usefulness in influencing behaviour), Applicability, and Discrimination (scientific quality). The maximum possible score is 25, with the first three categories having a maximum of five points allocated and the discrimination category a maximum of 10. Notably, the tool does have inherent bias in favour of experimental studies that feature high on hierarchy of evidence scales. The tool was designed for the general practice primary health care setting, and has been validated by general practitioners. It was utilised in the absence of a validated tool specific to the AMS setting. When using the tool, each evaluation question was posed within an AMS context, rather than the general practice paradigm. For example, when rating Applicability, one of the scores is described as 'impossible in my practice' - this, of course, was approached in terms of 'impossible in the AMS's practice'.
Assessment of the scientific quality of studies was undertaken with respect to a number of methodological issues such as sample size, participation rate, use of standardised survey instruments, validation of instruments, and utilisation of objective measures of respiratory function.
Hierarchy of evidence
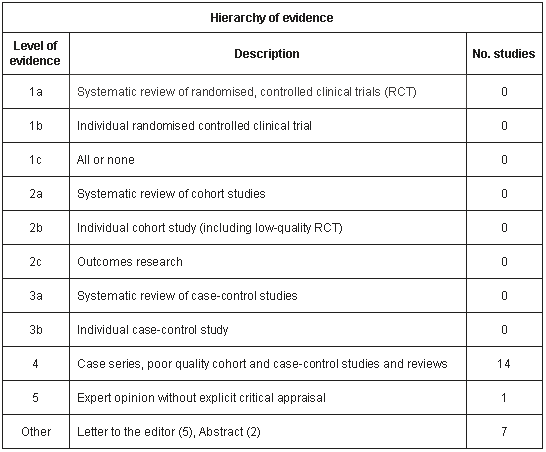
The literature was ranked according to the Sackett et al.'s 10 hierarchy of evidence (Table 1).
Table 1: Quality of evidence10: number and level of evidence of peer-reviewed papers and published national health survey reports
Meta-analysis
Meta-analysis of study findings could not be performed due to inconsistent epidemiological design, data definitions and collection methods.
Limitations of the review
- Only those papers available through the University of South Australia and University of Adelaide library were included
- Use of READER critical appraisal tool (designed for use in general practice) in the absence of a tool designed and validated for use in the AMS setting
- Grading of papers by a non-Indigenous junior researcher (24 months experience) due to the lack of available Indigenous personnel to undertake reviewing and scoring
Results
Extent of previous research
The number and level of evidence of peer-reviewed papers and published national health survey reports is outlined (Table 1). The search strategy identified 10 peer-reviewed descriptive studies, one review and three cross-sectional surveys undertaken by the Australian Bureau of Statistics in the past 10 years. It is clear that the available literature is largely low level evidence, in line with the nature of previous research efforts (cross-sectional and retrospective review studies). There have been no published studies of asthma prevalence in metropolitan Indigenous adults and children, and no randomised or controlled clinical trials have yet been undertaken. For the purposes of this review, studies of a minimum of Level 4 evidence will be outlined.
Critical appraisal
Methodological characteristics of studies are presented (Table 2) in order to compare and contrast study designs and scientific quality. The article by Veale and colleagues11 was the only study to utilise a definition of asthma prevalence that included both self-reported symptoms and objective signs, and hence was the most rigorous in this regard (because all other studies used only subjective reporting of asthma in their assessment of prevalence). While not formally validated, their specifically developed questionnaire was piloted in each community. The sample size of 1252 participants was a strength, although participation rates as low as 51% in one community is a weakness of the study affecting the validity of findings.
The study of remote communities by Valery et al. also had a large sample size, with an impressive 98% participation12. It used an internationally validated tool (International Study of Asthma and Allergy in Childhood) with modifications to local language, but did not validate it with local Indigenous individuals. Hamdorf and colleagues' Western Australian13 study was poor in relation to aspects of scientific quality. It consisted of 271 participants with a participation rate of 82%, and used a specially developed unvalidated questionnaire. Furthermore, the questionnaire was interviewer-administered and involved one member of the household answering health-related questions for all family inhabitants (hence responses were not self-reported in most cases). The definition of asthma prevalence was unusual, with interviewers asking about the occurrence of an asthma 'attack' in the past year, rather than, for example, previous diagnosis of asthma by a medical professional.
Bremner et al's study was also small in terms of sample size (n = 207), though participation rates were good (92%)14. It used a recognised questionnaire (British Medical Research Council questionnaire on respiratory symptoms) modified to local language and also assessed objective measures of respiratory function (spirometry, atopic testing and bronchial responsiveness tests). Downs and colleagues'15 study of rural children had a poor participation rate of 67% and used a survey tool that was not validated with Indigenous individuals or modified to local language. Because parents and guardians completed surveys regarding their children's symptoms in the absence of research staff, the accuracy of responses may potentially be questionable. The only objective respiratory function measures taken were skin prick tests to assess atopy. Verheijden and colleagues16 had a participant sample of 293, a participation rate of 90%, and used a validated questionnaire modified to local language, as done by Bremner and colleagues14, although this was not validated with Indigenous people. This was the only study in which research staff cross-checked subjective reports of asthma diagnosis with clinic files to ensure accuracy of reporting. The Australian Bureau of Statistics surveys4,17,18 vaguely defined asthma prevalence, simply asking respondents whether they experienced asthma as a current or long-term health condition. Consistent with national health surveys, there were no objective measures of asthma to accompany the subjective reports.
The only observational study of an intervention model, by Chang et al19, was an elementary description of the findings of a sub-specialist respiratory clinic in regards to accuracy of diagnosis, management of asthma and severity of disease in Indigenous children in a remote community. The intervention model was uncontrolled and did not involve complex scientific analysis. Finally, the retrospective reviews of hospitalisation data by Williams et al20, Ruben and Fisher21 and Whybourne et al22 in most cases outlined reproducible and sound methodologies. The inherent bias in Whybourne et al's22 paper regarding barriers to admission of rural and remote Indigenous children to the metropolitan tertiary hospital was identified.
None of the studies included in the review collected data on non-participants, thus failing to give any indication of recruitment bias. The recruitment procedures were also poorly described, if at all, and few papers made mention of study power.
Results of evaluation of studies using the READER instrument are also outlined (Table 2). Most studies rated quite poorly, in most instances due to a low score in relation to scientific quality (as descriptive studies like those included in the review can score a maximum of only 4 out of 10). In some cases low aggregate scores were due to poor scientific quality in combination with a lack of relevance and applicability to practice in the AMS setting.
 | Table 2: Analysis of study quality Click on thumbnail image |
Findings
The 1994 National Aboriginal and Torres Strait Islander Survey found that asthma was reported as a current health condition in 13.8% of males and 16.8% of females (15.3% overall). An estimated 56% of Indigenous males and 48% of Indigenous females aged 15 years and over were current smokers at the time, in sharp contrast to the estimated smoking prevalence in the Australian population as a whole (27% of males and 20% of females)17.
Results from the national health survey undertaken in 1995 showed that at a population level, asthma was reported by 19% of Indigenous people, compared with 11.2% of the total population of Australia. The increased prevalence of asthma in Indigenous people compared with non-Indigenous was reported in every age group. Within the Indigenous population, asthma was the most frequently experienced condition for individuals aged less than 24 years (17-23%), and while not the most common condition was experienced by 16-17% of older adults. Of note, asthma medication was the second most commonly used medication (10%) in Indigenous people. Among adults aged 18 years and over, just over half (51%) of Indigenous people reported they were current smokers, compared with 23% of non-Indigenous adults18.
In the 2001 national health survey, asthma was the second most commonly reported condition among Indigenous people (16%), after eye problems (29%). Once again, Indigenous people reported asthma as a long-term health condition more often than the non-Indigenous population (17% and 12% respectively)4.
Published scientific research undertaken on asthma in the Indigenous population is, as previously outlined, largely focused on studying prevalence of asthma in varying locations around Australia. There has also been a number of studies of hospitalisation rates, retrospectively reviewing hospital separation data.
The prevalence of current asthma in rural Indigenous communities in Queensland and Central Australia in 1990-1991 was found to be 0.5% among 8-12 year old children and 3.3% among adults. The prevalence of airway hyper-responsiveness (AHR) ranged from 2.2%-7.5%; and the overall prevalence of atopy ranged from 21% to 34%. The authors concluded that the prevalence of recent wheeze, AHR, current asthma and atopy in the rural Aboriginal communities they studied was low in comparison to the prevalence among non-Aboriginal Australians, and asthma in Aboriginal children was 'almost non-existent'. The authors suggested that the low prevalence of asthma was possibly due to environmental factors that influence the acquisition of atopy and AHR11.
A cross-sectional survey of Aboriginal health in the Peel region of Western Australia (WA) was undertaken in 1994-1995. In adults, 21% suffered from persistent cough or wheeze, and 14% had experienced asthma in the past year. Among children, 46% had had a respiratory tract infection and 15% had had an asthma attack13. Of note, data about families were gathered by interviewing the primary carer in the household; therefore reporting was subject to the perceptions of the single individual interviewed.
Levels of lung function in Aboriginal people in a remote tropical community in WA in 1993 were compared with a group of non-Indigenous Australians. The results of the study showed that lung function in the Aboriginal cohort was poorer than that in the non-Indigenous group. In Indigenous participants, a history of being diagnosed with asthma was more frequent in adults than children, and more common in females than males (children: M [5.4%], F [8.9%] and adults: M [8.5%] and F [15.2%]). Atopy was also more common in adults than in children, was slightly more common in women (36.4%) than in men (28.8%) and was predominantly due to positive responses to house dust mite. The authors recognised a limitation of the study was the use of a questionnaire validated with non-ATSI individuals14.
A study of asthma prevalence in children was undertaken in five remote Indigenous communities in the Torres Strait and northern peninsula area of Queensland. There were significant variations between communities, with an overall prevalence of self-reported ever wheezing of 20.6%. 12.4% of children had experienced wheezing in the previous year, and 15.8% reported ever having asthma. The authors stated that the prevalence of asthma in these communities was as high as that in Australian non-Indigenous children at the time12.
A study of Aboriginal and non-Aboriginal children living in two rural towns in New South Wales was performed to compare the prevalence and risk factors for wheeze, asthma diagnosis and hayfever in the two groups. The prevalence of wheeze in the last 12 months in Aboriginal children was 31%15, over 10 times higher than that measured in rural communities by Veale et al.11 The rate of diagnosed asthma was 39.4% in the Aboriginal children and 39.3% in non-Aboriginal children, and there was a similar level of asthma medication usage between the two groups. Aboriginal children were less likely to be atopic and to have hayfever than non-Aboriginal children. Having had bronchitis before age 2 years was a strong risk factor for wheeze and asthma in Aboriginal children. The authors suggested that while there are similar rates of wheezing illness in Indigenous and non-Indigenous children, their aetiology is possibly different (ie less allergic in the Aboriginal population)15.
A later study described the prevalence of respiratory symptoms, asthma and levels of lung function in two matched remote Aboriginal communities (one northern tropical [T] and one desert [D]) in WA. For both adults and children, shortness of breath and chest tightness were reported more frequently in the desert group than in the tropical group. There were no significant differences in cough, sputum, wheeze, or diagnosed asthma between the two groups. The prevalence of asthma in children was 12-17% (T) and 0-7% (D) and in adults was 7-20% (T) and 16-26% (D). Wheeze in children was 17-20% (T) and 7-20% (D) and in adults was 31-32% (T) and 38-44% (D). Overall, the desert group had greater respiratory symptoms and poorer lung function, and showed more positive responses to atopic testing. The presence of asthma was not related to and therefore could not explain these findings. The authors suggested that environmental factors such as infection may be responsible for the differences in lung function observed between the communities16.
It is evident that the cross-sectional studies undertaken to date have differed in their findings in relation to prevalence of asthma in the Indigenous population. The findings of the Australian Bureau of Statistics national health surveys and published prevalence studies are presented (Table 3), in descending order of scientific quality. While unstandardised data collection methods used by the various studies make direct comparisons of findings difficult, some preliminary analyses will be discussed in the following section.
Table 3: Prevalence of asthma - summary of findings
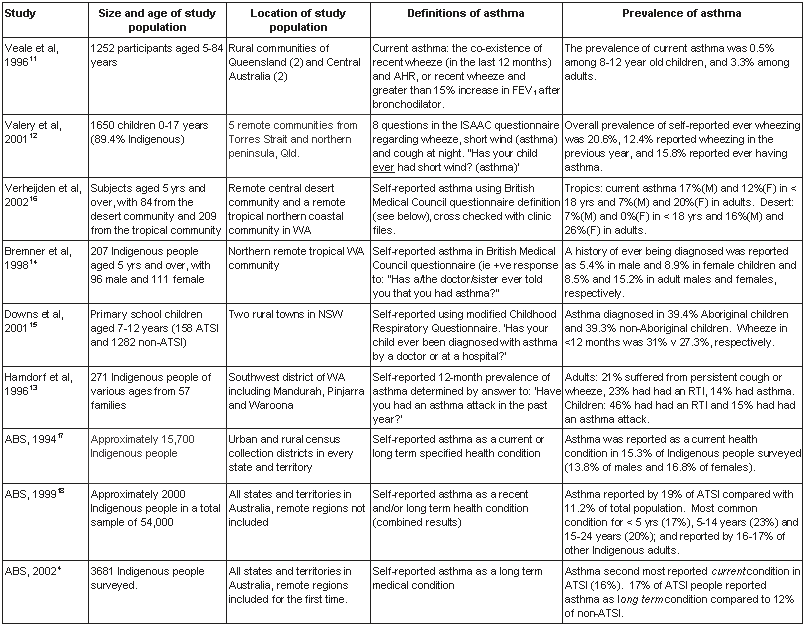
Only one study of asthma management models has been undertaken. This is a descriptive study of the management of Indigenous children with asthma in a remote community, delivering a sub-specialist service through a community controlled Indigenous health service19. Children referred by Aboriginal health workers to paediatric respiratory physicians were evaluated prospectively at a primary healthcare setting at Thursday Island, Queensland. Results showed that of 54 children who had a pre-evaluation diagnosis of asthma, 14 did not have clinical asthma and instead had other respiratory disorders. Those children who did have asthma were classified as persistent (30%), frequent episodic (13%) and infrequent episodic asthma (57%). This prevalence of persistent asthma (30%) was greater than the mainland Australia proportion of 5-13% at that time19.
There was considerable room for improvement in the management of asthma observed, since most asthma medications were wrongly prescribed with respect to delivery systems and dosage. The authors felt it demonstrated a need for educational interventions to be undertaken with treating local health professionals. They also felt that it showed that specialist medical services could be successfully provided through the community controlled health service with good attendance rates (98%)19.
Other studies looked at hospitalisation rates of Indigenous people with respiratory conditions. The first documented the epidemiological patterns of respiratory conditions as causes of hospitalisation in WA from 1988 through to 1993. Overall, age-standardised rates of hospitalisation were 5.6 times higher among Aboriginals compared with non-Aboriginals for diseases of the respiratory system. Admission rates for asthma were consistently higher in Aboriginals compared with non-Aboriginals, and in non-metropolitan compared with metropolitan areas. In fact, age-standardized rates of admissions for asthma were 3.1 times higher for Aboriginal people than non-Aboriginal people. Asthma was the main or second cause of hospitalisation for all Indigenous age groups other than infants (<12 months)20.
Another retrospective review of hospitalisation rates looked at 1991-1997 data for Indigenous and non-Indigenous children in the top end of the Northern Territory (NT). Results showed that the average annual hospitalisation rate per 1000 population with a principal diagnosis of asthma was 2.6 for rural Indigenous children, 4.7 for urban Indigenous children, and 5.5 for non-Indigenous children (rural and urban combined). The rates were significantly different only between rural Indigenous and non-Indigenous children. Asthma was diagnosed in 6.5% of Indigenous children's admissions (4% for rural and 13.8% for urban children) and 12.7% of non-Indigenous children's admissions. The authors felt that these results were evidence that asthma plays a far less significant role in the spectrum of disease affecting hospitalised Indigenous children compared with non-Indigenous children. The authors acknowledged that a possible bias in the results lay in the barriers to access experienced by Aboriginal children living in rural or remote areas (which equated to 53% of Indigenous children in the study) who require air evacuation in order to get admitted to the metropolitan hospital21.
The third study was another retrospective review of hospitalisation data from the tertiary hospital in Darwin in the NT. It looked at characteristics of children under 10 years discharged between 1991 and 1996 in relation to their hospital stay. Significantly more Indigenous children suffered multiple co-morbidities than non-Indigenous children. Also, a higher proportion of Indigenous than non-Indigenous children had prolonged hospital stays. Variables influencing length of stay included age <2 years, living in a remote area and presence of two or more co-morbidities. The most common reason for admission was gastroenteritis for rural Indigenous children and bronchitis and asthma for non-Indigenous and urban Indigenous cases22.
A review was undertaken to describe the burden of respiratory illness in the Australian Indigenous population and examine the evidence around aetiology of asthma23. In the last 25 years respiratory mortality in Aboriginal people was described as five times higher than in non-Indigenous people. Looking at asthma from an historical perspective, the authors described that there is no record of prevalent respiratory illness in anecdotal evidence documented during white settlement, nor during an American-Australian visit of Arnhem land in the 1950s23. In early epidemiological studies in the 1960s and 1970s, asthma prevalence was not specifically investigated or reported other than in adults from Bourke, NSW, where 5 cases were reported in a total of 320 Indigenous adults surveyed (1.6%) (whereby adults surveyed were individuals over 15 years of age and self-identifying as Aboriginal)24.
The authors cite Veale et al. as a study on remote communities, which is alternatively described in the original paper as having been undertaken in rural regions11. In the absence of data published by Valery et al.12 following the writing of the review, they conclude that rates of asthma are low in Indigenous children living in remote communities. They further the commentary around aetiology of disease, stating that the accumulating evidence suggests that many asthma symptoms may have an infectious rather than an allergic origin and are a result of inherently small airways that are further compromised by repeated or prolonged bacterial infections or cigarette smoking. They expressed the view that the misinterpretation of asthma-like symptoms in Indigenous communities as being of an allergic origin may be leading to high and possibly inappropriate rates of use of asthma therapies. The authors highlighted that there is an urgent need to identify the aetiology and the most effective treatments for asthma-like respiratory symptoms in Indigenous children23.
Discussion
Cross-sectional prevalence studies have been undertaken in many of the states and territories of Australia, and in some cases have yielded widely different results. Asthma prevalence in children has been described in rural communities to be as low as 0.5%11 and as high as 39.4%15. Prevalence of asthma in rural adults has been quantified in only one study, being a low 3.3%11. In remote communities, 15.8% of children were found to have ever had asthma, while 12.4% reported wheezing in the previous year12. Adult prevalence has been described in remote communities as 7-20%14, 16-26%16, and 8.5-15.2%14. ABS surveys have described that asthma is reported as a current health condition by 15.3%17, 19%18, and 16%4 of the Indigenous participants surveyed. Note that remote communities were included in data only in the 2001 national health survey18.
Hospitalisation data for Indigenous and non-Indigenous children admitted with asthma has shown differences between states. NT data showed rural Indigenous children were admitted significantly less than urban non-Indigenous children22, while Western Australian data showed that admissions were 3.1 times higher in Indigenous than non-Indigenous children, and higher in non-metropolitan compared with urban children20. Some trends were similar, though, in that asthma as the leading cause of admission was more common in urban Indigenous children compared to rural counterparts.
This divergence in findings highlights that prevalence of asthma, and/or the aetiology of asthma, may be different across and within demographics (ie metropolitan/ rural/ remote in different states and territories), or that the unstandardised epidemiological methods used lead to different results. Examples of this include different data collection methods (interview, self-report questionnaire) and different definitions of asthma (Table 3). The contrasting prevalence findings and uncertainty around aetiology of asthma in Aboriginal people have been the topic of debate and discussion in the academic literature25-28.
Looking at prevalence data in terms of scientific quality of studies, it is interesting to note that the two studies that utilised methods other than self-report (such as combined subjective and objective assessment by Veale et al11 and cross checking reports with medical records by Verheijden et al16) had among the lowest prevalence findings in children, with 0.5%11 and 0-7% in a desert community16. It is therefore worth considering the possibility that reliance on self-reporting of asthma diagnosis and symptoms in Indigenous participants, for whom English may be a second language, may lead to less accurate results than studies that use multiple data collection methods. For example, there may potentially be some confusion in participants regarding what asthma is, particularly if local terms such as 'short wind' are used to describe the condition, resulting in possible over reporting of prevalence. The accuracy of self-reporting methods to determine asthma prevalence in Indigenous participants could in itself be the focus of further research.
Conclusion
The research effort undertaken to date on asthma in the Australian Aboriginal and Torres Strait Islander population is not commensurate with the importance that should be placed on a disease frequently reported by the Indigenous community. That said, there have been increasing numbers of studies in the last decade, with all studies in this review being published since 1996. All studies undertaken reside at a low level on the hierarchy of evidence scale, possibly reflecting the type of studies Indigenous committees approve and Indigenous individuals wish to participate in. There remains no consensus of opinion around the prevalence and aetiology of asthma in Aboriginal and Torres Strait Islander individuals. There has been only one study to test an asthma management intervention, that utilised an Indigenous health service to administer a biomedical sub-specialist service, rather than utilising Aboriginal health workers to provide culturally specific asthma management programs. Extensive consultation with Indigenous communities is indicated in order to determine priorities for asthma research and preferences for study design. Following this, well-funded large-scale studies of a high methodological quality (whatever the design) investigating asthma in the Indigenous population should be commissioned. Any research with Indigenous communities should be undertaken using culturally respectful methods such as those outlined in the Iga Warta Agreement29. Results of research and development projects should be published and disseminated in order to further the understanding of asthma in the Australian Indigenous population.
Acknowledgements
The author would like to thank the Department of Health and Ageing who funded this review as part of an Asthma Innovative Management project grant, and to Gary Misan for providing comments on the original draft in the project report.
References
1. Australian Bureau of Statistics. Census of Population and Housing: Aboriginal and Torres Strait Islander Peoples, Australia, 1996. ABS cat. no. 2034.0. Canberra: ABS, 1998
2. Australian Bureau of Statistics. The Health and Welfare of Australia's Aboriginal and Torres Strait Islander Peoples, 2001. ABS cat. no. 4704.0. Canberra: ABS, 2001.
3. Australian Bureau of Statistics. Year Book Australia, 2002. Health: Centenary Article - Child health since Federation. ABS cat. no. 1301.0. Canberra: ABS, 2002.
4. Australian Bureau of Statistics. National Health Survey 2001: Aboriginal and Torres Strait Islander Results. ABS cat. no. 4715.0. Canberra: ABS, 2002.
5. Department of Health and Ageing. National Health Priorities. (Online) 2002. Available: http://www.health.gov.au/pq (accessed 4 April 2003).
6. Department of Health and Aged Care (DHAC). National Asthma Action Plan 1999-2002. Canberra: Commonwealth of Australia, 2001.
7. National Health and Medical Research Council. How to review the evidence: systematic identification and review of the scientific literature. Canberra: Biotext, 2000.
8. MacAuley D, McCrum E, Brown C. Randomised controlled trial of the READER method of critical appraisal in general practice. BMJ 1998; 316: 1134-1137.
9. MacAuley D, McCrum E. Critical appraisal using the READER method: a workshop-based controlled trial. Family Practitioner 1999; 16: 90-93.
10. Sackett DL, Straus SE, Richardson WS, Rosenberg W, Haynes RB. Evidence-based Medicine - How to practice and teach EBM (2nd edn). Oxford: Churchill Livingstone, 2000; 173-175.
11. Veale AJ, Peat JK, Tovey ER, Salome CM, Thompson JE, Woolcock AJ. Asthma and atopy in four rural Australian aboriginal communities. Medical Journal of Australia 1996; 165: 192-196.
12. Valery PC, Chang AB, Shibasaki S et al. High prevalence of asthma in five remote Indigenous communities in Australia. European Respiratory Journal 2001; 17: 1089-1096.
13. Hamdorf M, Wallace P, Gillam C, Stevenson M. Aboriginal health in the Peel region of Western Australia. Australian Family Physician 1996; 25(2): S81-S85.
14. Bremner PR, de Klerk NH, Ryan GH et al. Respiratory symptoms and lung function in aborigines from tropical Western Australia. American Journal of Respiratory and Critical Care Medicine 1998; 158: 1724-1729.
15. Downs SH, Marks BH, Belosouva EG, Peat JK. Asthma and hayfever in Aboriginal and non-Aboriginal children living in non-remote rural towns. Medical Journal of Australia 2001; 175: 10-13.
16. Verheijden MW, Ton A, James AL, Wood M, Musk AW. Respiratory morbidity and lung function in two Aboriginal communities in Western Australia. Respirology 2002; 7: 247-253.
17. Australian Bureau of Statistics. National Aboriginal and Torres Strait Islander Survey 1994. ABS cat. no. 4190.0. Canberra: ABS, 1994.
18. Australian Bureau of Statistics. National Health Survey 1995. ABS cat. no. 4806.0. Canberra: ABS, 1999.
19. Chang AB, Shannon C, O'Neil MC et al. Asthma management in Indigenous children of a remote community using an Indigenous health model. Journal of Paediatrics and Child Health 2000; 36: 249-251.
20. Williams P, Gracey M, Smith P. Hospitalisation of aboriginal and non-aboriginal patients for respiratory tract diseases in Western Australia, 1998-1993. International Journal of Epidemiology 1997; 26: 797-805.
21. Ruben AR, Fisher DA. The casemix system of hospital funding can further disadvantage Aboriginal children. Medical Journal of Australia 1998; 169(l): S6-S10.
22. Whybourne A, Lesnikowski C, Ruben A, Walker A. Low rates of hospitalisation for asthma among Aboriginal children compared to non-Aboriginal children of the top end of the northern territory. Journal of Paediatrics and Child Health 1999; 35: 438-441.
23. Peat JK, Veale A. Impact and aetiology of respiratory infections, asthma and airway disease in Australian Aborigines. Journal of Paediatrics and Child Health 2001; 37: 108-112 [Review].
24. Kamien M. The physical health of Aboriginal adults in Bourke, New South Wales. Medical Journal of Australia 1976; 1(l): 38-44.
25. Weiner JM, O'Hehir RE. Allergy and asthma in central Australia. Medical Journal of Australia 1996; 165: 526.
26. Prociv P. Could parasitic infections protect Aboriginal children against asthma and allergies? Medical Journal of Australia 1997; 166: 391-392 [Letter].
27. Torzillo PJ, Chang AB. Infection, wheezing and Aboriginal children. Medical Journal of Australia 2001; 175: 4-5.
28. Valery PC, Masters IB, Chang AB. Asthma is not prevalent in Aboriginal and Torres Strait Islander children - a myth. Journal of Paediatrics and Child Health 2002; 38: 105-106.
29. Department of Human Services. Human Services Research and Innovation Program. Appendix 1: Iga Warta Declaration. South Australia: DHS; 2000/2001. Available at http://www.health.sa.gov.au/hsrip/desktopdefault.aspx?panelid=70&tabindex=4&tabid=140 (accessed 21 May 2003).
