Introduction
Privatising healthcare costs
As a result of the impact of economic rationalism, health services in Australia have increasingly been made to conform to market principles. Wakerman and Lenthall remind us: 'Healthcare policy has also been influenced by broader economic policy and subsequent political events' (p. 134)1. The costs borne by individuals, groups and communities have been increasingly privatised. Casemix funding and early discharge procedures (among others) are significant ways in which hospitals and other health services attempt to offload some of their costs onto patients, carers, communities and other parts of the health and welfare system2,3. In this way, a greater proportion of healthcare costs are borne outside the traditional healthcare system.
Significant equity, access and other social justice issues arise from these changes. With regard to hospital treatment, it is increasingly recognised that patients now tend to enter hospital later and leave hospital earlier in a less recovered state. The burden of care and responsibility falls more and more on primary care-givers in the community4,5 (M Ward, S Hutchinson, unpubl. report, James Cook University, 1998). Thus, while health service organisations may struggle to 'do more with less', there are also significant implications for the quality and continuity of care of patients, for the welfare of carers and for the long-term wellbeing of the local communities, especially rural and remote communities, which may not benefit from economies of scale or from the availability of collateral infrastructure1,6.
It is known that early discharge from hospital has a considerable impact on patients, carers and communities in rural and remote areas5,6. In comparison with urban areas, rural and remote regions lack the critical mass on which to build appropriate infrastructure and collateral services. They are influenced by distance and dispersed demand7. It would appear, therefore, that the needs of people living in rural and remote communities could only be met effectively where new methods of organisation, service delivery and funding are developed8.
Thus, while early discharge may result in lower costs for hospitals, the burden of cost and responsibility is shifted to others, including patients and their carers. This occurs particularly in rural and remote areas. In a study of discharges from the Royal Darwin Hospital (RDH), Northern Territory, Australia, Mackenzie (G Mackenzie, unpubl. report, University of Melbourne, 1995) concluded that communication between RDH, district medical officers and community health clinics had been problematic, particularly with respect to discharge summaries. Information regarding patient identification, referral source, discharge medication and details of follow up were often deficient. Discharge medication was recorded poorly and community health centre staff were frequently dissatisfied with the duration of discharge medication supplied by RDH. The discharge planning role was not well understood 4,5 (G Mackenzie, unpubl. report, University of Melbourne, 1995).
Study focus
But first some contextual information. Townsville General Hospital (TGH) is the largest public hospital in Queensland outside the Brisbane metropolitan area, 1400 km to the south, and the only level 5 tertiary referral hospital outside southern Queensland. The TGH catchment area covers the Northern Zone of Queensland Health, extending from St Lawrence (550 km south of Townsville), north 1200 km to the tip of Cape York Peninsula and the Torres Strait, and 1100 km west to the Northern Territory border (Fig 1). Approximately two-thirds of patients admitted to TGH are from the Townsville District Health Service (TDHS) area, which itself includes significant population centres (for example Ingham and Palm Island) which are more than 50 km from the hospital (50 km being the point of eligibility for the Patient Travel Subsidy Scheme: PTSS). One-third of patients are admitted from regional, rural and remote areas of the Northern Zone outside the TDHS. The total catchment area serves one of the largest Aboriginal and Torres Strait Islander populations in Australia with Indigenous persons comprising 7.1% of the population of the Northern Zone compared with a figure of 2.9% for Queensland as a whole.
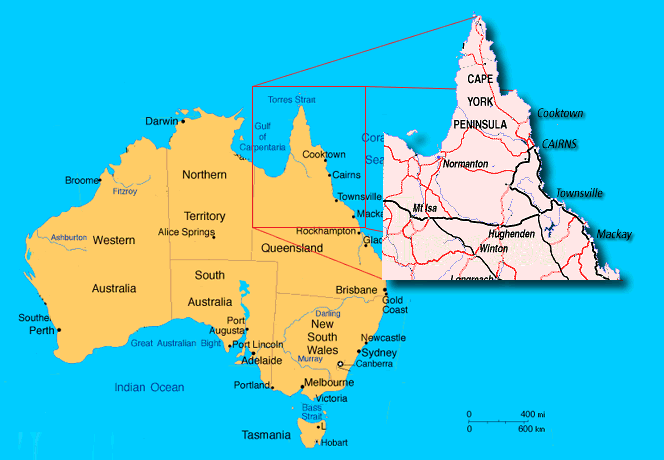
Figure 1: Northern Queensland, the study area, Australia.
For a number of years social workers at the TGH, Queensland, Australia, and academics of the School of Social Work at James Cook University, Queensland, were keen to undertake research into the impact of early discharge and other cost-saving measures on patients and carers in rural and remote communities.
In 2000, a research project was designed to focus on the experiences of patients and their carers attending TGH from locations beyond the 50 km PTSS boundary. The main focus of the study was on patients and carers from rural towns and remote areas. However, patients and carers from coastal cities such as Mackay and Cairns, Queensland, were also included, because it was anticipated that the experience of having to travel 350 km to hospital would be a significant dislocation even if community services were more readily available on discharge than in country areas and the (remote) 'outback'.
The aims of the study were to:
- Examine, from the patient and carer perspective, the social, economic, cultural and emotional cost of hospitalisation away from home communities.
- Identify the needs of rural and remote patients and their carers before, during and after hospitalisation a long way from home.
- Make recommendations for improved policies and practices concerning the continuum of care: from admission planning, through hospitalisation, discharge planning, and post-discharge support, in the context of rural and remote locations.
The present study has focused on the social, economic and cultural impacts of early discharge from TGH into rural and remote communities in north Queensland. We have envisaged these as dimensions of human experience. Economic impact refers to costs incurred by patients and carers either as direct expenses and/or income forgone. Economic impact also refers to the shifting of costs from the health system to the community that occurs when patients are discharged early. We were concerned about the social impact on families and communities and also experiences of cultural disconnectedness when people (particularly indigenous patients and carers) are separated from their social and community supports.
Methods
The present study follows the completion of a collaborative pilot study conducted by James Cook University and TGH, entitled 'The Social and Emotional Impact of Hospitalisation on Patients and Carers from Rural and Remote Communities'. The primary intention of the pilot study was to trial and critique the research methodology chosen for the present project. The following design reflects this critique.
Consistent with the aims of this research, the present project was designed to elicit information from patients and carers during and post-hospitalisation. Accordingly, patients were contacted during their hospital stay and 2-5 weeks post-discharge. Carers were also contacted during the period of hospitalisation of their relative and also 2-5 weeks post-discharge of their relative. It was not required that the patients and the carers participating in the research project be related. Patient and carer participants were required to meet criteria consistent with the attributes of all rural admissions to hospital (patients), the general rural population (carers) and also relevant to the aims of the present study. These criteria included age, gender, ethnicity, type of illness, admission status and place of residence.
Difficulty in accessing patients and carers during the hospitalisation period and post-discharge in rural and remote communities was identified as a study limitation by the pilot study. Therefore, acknowledging this limitation and the criteria for participant selection, the study entailed the administration of 20 structured survey interviews with each participant group during hospitalisation and also post-discharge. A total of 80 survey interviews were conducted with 20 patients and 20 carers. In addition, 24 qualitative semi-structured interviews were held with selected individuals from each participant group during hospitalisation and also post-discharge.
Qualitative, in-depth interviews with patients and carers were fundamental to the success of this project. Qualitative research 'refers to research about persons' lives, lived experiences, behaviours, emotions, and feelings ...'(p. 11)9. It is applicable to research problems that seek to understand the nature of people's experiences within complex systems. In the present study, qualitative interviews provided in-depth information about individual experiences of hospitalisation and post-discharge care in rural settings, allowing exploration beyond the narrow confines of a survey instrument. Patients and carers raised and explored original issues and, importantly, told their own stories, adding to the research the strength of personal experience. These interviews provided the consumers' perspective as well as in-depth information on the social, economic, cultural and emotional cost of early discharge in rural communities.
The four vignettes presented in this paper are taken from the in-depth, qualitative interviews with 12 patients and 12 carers. Results from the quantitative data will be presented in future publications. Ethics approval to conduct the study was applied for and received from James Cook University and TGH Ethics Committee.
Results
A depth of experience
In analysing the findings of the quantitative components of the study it could be concluded that both patients and carers coming to TGH from outlying areas were stoically accepting of the various circumstances involved in leaving their home communities, being admitted to and receiving treatment at the TGH and being discharged back into their own communities. In other words, much of the quantitative data appeared to reveal few issues or problems that might be generalisable to larger similar populations. Hudnell Stamm reminds us that popular myths about rural life can obscure the 'reality of rural life' and that these 'reported assumptions may lead to shortcomings in effective policies, programming and services' (p.6)10.
Analysis of the qualitative material, however, revealed a depth of experience that remained hidden in the quantitative studies. While it is true that these experiences were unique to the circumstances of the patients or carers in question, nevertheless there was sufficient commonality of experience for these findings to be of interest. However, in saying this we are reminded of Thorpe's urging for the respect of the voice:
In searching for multiple voices, there is an emphasis on valuing difference as well as similarities; a commitment to not homogenising research findings nor privileging shared themes and thereby obscuring the differences which are shaped by multiple realities. (p. 4)11
The four vignettes encapsulate what are considered to be some of the most significant issues and problems that are likely to arise for patients and carers coming to the TGH from outlying areas. The respondents have been given pseudonyms.
Joe and Joy - a nightmare from beginning to end
The case of Joe and Joy highlights a number of issues that are likely to affect patients and carers coming to Townsville from a long distance. The case exemplifies problems that may arise in relation to travel, communication with the hospital, accommodation for the primary carer in Townsville, discharge planning and post-discharge care.
Two years ago, Joe had a hip replacement operation at TGH. He was returning to have his second hip replaced. He and his wife (and carer), Joy, came to Townsville by road and bus from a small community in the Gulf of Carpentaria, some 1200 km away. The journey was a logistical nightmare.
... he did the 7 hour trip to Mt Isa in the car, he drove down and because he couldn't drive all the way to Townsville, we decided to go by bus. We couldn't afford a plane trip, and we went by bus and that was a 12 hour trip. And he sat on a cushion all the way over and hung on to the seats, and he got out at a couple of the stops with a lot of difficulty, because of the nature of the big bus.
However, the travelling was only one part of the nightmare. On arrival in Townsville, the couple were informed that the operation had been cancelled. Joe said:
But the disadvantage of that to me was that I was all ready for the Tuesday and then all this dramatic news that it was cancelled, and I had to face up to the thought now - how are we going to get home? We have got to go out to Mt Isa and pick up the car and then we have got to drive all the way home to the Gulf and that is going to cost a lot of money, and we really can't afford it.
After several days of uncertainty the hospital eventually agreed that the operation would be rescheduled to occur in approximately one week. In the meantime, the couple had to find accommodation outside the hospital. To find affordable accommodation was difficult. Although Joy was booked already for cheap accommodation, Joe had expected to be in a hospital bed:
We could have gone to Red Cross House but I was booked in and he wasn't booked in, and he was booked in for a week later, after the operation because we expected to be staying then, for physio to be done.
Eventually the operation took place successfully and Joe spent 2 weeks in hospital. However, there was only 24 hours notice of impending discharge and there does not appear to have been any discharge planning. Joy observed:
... he didn't know he was going to leave hospital until the day before when the doctor told him that he could go home. But the problem was how to get us home.
The couple debated whether Joe should stay in Townsville for a bit longer for physiotherapy, as they had expected to do after the first hip operation, but had not. The only affordable accommodation had beds that were too low for Joe to manage. They decided to go home without the physiotherapy.
... we wanted to stay over the road at Red Cross House but of course he couldn't stay there [the beds were too low] and there was nowhere for him to stay that could take him, unless we paid motel bills or hotel bills or that sort of thing. And we are both on the pension so there was no way we could go paying $75 and $80 a night for a week or so. [Joy]
On the return journey, Joe and Joy had hoped to fly back to the Gulf. Having been transported to Cairns by air ambulance, they then discovered it was not possible for Joe to be seated in a small plane. After several days wait in a motel in Cairns (at $65 a night) Joe and Joy caught a coach from Cairns back to Townsville and again from Townsville out to Mount Isa. At Mount Isa they picked up their car and drove back to the Gulf.
...I had to make sure Joe was taking Panadol all the time for his pain, and keeping his fluids up, and making sure he could get to the toilet all right wherever we stopped. [Joy]
Once home the difficulties were not over because Joe needed to get back to Mount Isa for further medical care and physiotherapy. Reflecting on their difficulties, Joy said:
...organising people, transport and accommodation and telephone calls and faxes to people who can't or don't want to help or are not interested or motels that only want $148 a night. Where else can you go to stay in a place that would be suitable for a man on crutches, who has just had a hip replacement? I don't know where the people go myself, when they come to Cairns or Townsville and they have got these ailments. Where do they go, how do they get on, you know?
Greg and Brenda - cost and confusion
Greg, an elderly man who lives in a caravan in a regional town several hundred kilometres from Townsville, developed a deeply infected foot. No one was able to ascertain what had caused this. His GP admitted Greg to the local base hospital on three occasions. On the last admission to the base hospital a new doctor arranged for Greg to be transferred to TGH. However, the arrangements were unclear and medical and nursing staff were confused about whether the transfer was going to take place. This was particularly distressing for Brenda (Greg's ex-partner) who could not get a clear picture of what was required and who found herself trying to pressure hospital staff to get the matter sorted out. She was given contradictory advice about whether or not she was permitted to take Greg's X-rays with her. Brenda was given no information about transport.
... they came back and said they would pay your fare, and I would have to pay my own. [Brenda]
On arrival in Townsville by air ambulance, Greg immediately received a diagnosis and began receiving appropriate treatment. The foot responded well, albeit slowly. He then spent 2 months in TGH. Eventually he was discharged but continued to receive treatment on an outpatient basis. During this time he lived in a nearby hotel and his expenses were paid by the referring hospital. Brenda's expenses, however, were not covered. She was very stressed and became ill. Eventually, she had to leave Greg in Townsville and return to her hometown. While Brenda carried a number of personal costs to her health, her financial costs were considerable. She reflected:
And I'm sorry now that I didn't, being a rather practical person, I didn't keep any records of what it cost, but it would run into quite a bit of money ... I said as far as money, all I did was pay, pay, pay. But it was worth it to save Greg's foot.
This case offers a good example of the difficulties faced by patients and their carers when appropriate services are not available in their own communities. The case also highlights the high cost, both emotional and financial, to carers. Also worth noting was that Brenda was Greg's ex-partner, which suggests a reliance on carers who may have only a tenuous and uncertain relationship with the patient.
Geoff and Tracey - a long way from home
This vignette concerns Geoff who had a serious accident at work in a small regional town approximately 2 hours out of Townsville. He was transported to TGH by ambulance. His wife Tracey had no idea what was happening to her husband and was unable to get an accurate picture from anyone in the hospital.
The breaks were that bad that they had no idea why he was still alive. The worst part was not knowing, they would not tell me anything. That was what I found was very hard, especially where I was. The fact that I was so far away and I was so tied up with our life, not having time to get away because it was impossible.
Geoff was in hospital for 3 months. Tracey had no idea what this would involve for her. In fact she spent a lot of time driving between her home town and Townsville (a distance of 200 km round trip), trying to be with Geoff, trying to keep her business afloat at home, trying to look after her children. Tracey's travelling also caused anxiety for Geoff.
Just the fact that it was so far away and she had to pack up and drive home at nighttime made it hard for her, but it used to leave me worried at the same time. I'd be waiting all the time until she rang me up from home to say she was home.
The process of driving backwards and forwards to the hospital exhausted Tracey.
I was so tired before that I was actually going insane. I was so tired it made me lose control of my mind.
When Geoff came home, things began to improve, even though it was still very hard work. After all, Geoff still needed some fairly intensive 'nursing' and Tracey was the untrained nurse.
Being a carer slows your life down. You know he's home and you know you don't have to drive [to Townsville] but you can't sleep in. If I don't get home till 10 at night, I'm tired, I start at 5 and I don't come home until 10 or 11 at night. I own the shop and I have to do those hours. I still have to bath [Geoff] and still have to do his pins. It takes half an hour to three-quarters of an hour to bath [Geoff]; it takes up to about half an hour to do his pins, to do it thoroughly.
Geoff and Tracey's story highlights the complexity of the impact of living at some distance from the hospital, and what this means for the competing demands of caring, household and business management.
Luis and Carmelita - no support what-so-ever
The final vignette concerns Luis and Carmelita, a non-English speaking background couple who live in a small country town approximately 3 hours by car from Townsville. Their story brings home some of the enormous difficulties borne by patients and carers a long way from a regional hospital.
Luis' involvement with TGH was stressful and traumatic from the beginning. Initially he was on the waiting list for bowel surgery for almost 7 months. Luis stayed in TGH not for the expected 2 weeks but for 3 months. When he was discharged home, further surgery was still needed. At the time of his interview he had been waiting another 3 months for the surgery to complete the repair to his bowel.
On arrival at his hometown, Luis had little idea about how to deal with his colostomy bag. His wife worked outside the home and also cared for their young child, and was not able to be his primary carer. Eventually, Luis learnt to deal with the bag by trial and error. Yet Luis and Carmelita received no assistance in the local community or from the hospital.
Well any help is always good. If anybody would have come around and said, 'How are you doing?' or said, 'Do you need something?' You know it would have been welcome. On my own it is very difficult, it is really hard ... no support what so ever! I am very much on my own and just see what happens... hoping for the best.
The cost of Luis' illness was not only physical. His business collapsed and Carmelita's work as a cleaner at a local school provided little money. Luis and Carmelita's relationship became strained.
I think it is getting worse every time, all the time it is getting worse. Because we are just becoming more distant from each other all the time ... She is suffering and I am suffering.
While waiting for the hospital to be ready to complete the repair of his bowel, Luis reflected ironically on the other impacts on his life.
That's [the bowel's] suppose to repair given time ... but the economic damage, the psychological damage and the marriage - are these ever going to be repaired or is it going to be too late?
This case highlights the impact of an extended stay in hospital, which again is financial and emotional. Luis's situation was further complicated by a breakdown in the domiciliary referral process. When initially discharged to family in Townsville he received domiciliary care. However when Luis returned to his home community no subsequent referral was received to ensure ongoing domiciliary care. It is not uncommon for patients from rural locations to stay temporarily in Townsville prior to being able to undertake the trip home. This temporary local residency may prevent them receiving the additional support normally supplied for patients returning directly to their rural community.
Discussion
Veitch et al. undertook a study that was in many ways similar to the present study 8. They focused on patient access to specialist care in rural and remote locations across Queensland and reported '...the negative effects of distance barriers in obtaining specialist medical services...' (p. 105). The findings of the Veitch et al. study, although not referring to the experiences of carers as the present study has, were consistent with and therefore strengthen the findings of the present research 8.
The four stories of the present study offer a range of perspectives on the experiences of hospital patients who come to Townsville from outlying areas. Clearly, when patients are admitted to a major tertiary referral hospital they are suffering from a condition that requires serious medical or surgical intervention, regardless of whether it is planned or an emergency admission. In such circumstances distress, anxiety and fear are common among patients and their carers. Hospital admission will cause disruption to their everyday lives, and will entail encounters with a large, and perhaps unfamiliar, institution from a position of vulnerability and relative powerlessness.
To some extent, therefore, many of the experiences identified in the present research are not unique to people who are hospitalised a long way from home. The stories do suggest, however, that the effects of dislocation from home communities and social networks may exacerbate negative experiences.
There seems to be little question that patients' family and friends (including previous partners) do most of the caring work in rural and remote communities. The present study shows that little use is made of other human services. As suggested earlier, there may be a number of possible reasons for this, for example the lack of appropriate referrals, the legendary self-sufficiency of rural people, or the fear of invasion of privacy. Whatever the reason, it appears that carers are there to fill the gaps. The responsibility for recovery and rehabilitation is now substantially in the hands of unskilled family and friends.
Emerging recommendations
The present study also suggests considerable inadequacy in the communication and dissemination of information to carers living in rural and remote communities about a range of issues. We therefore make the following recommendations:
- Information should be provided to rural and remote patients and carers about Townsville and TGH, the nature of hospital admission and what to expect post-discharge.
- Information should be provided about travel options and entitlements. Difficulties accessing PTSS assistance need to be acknowledged, often based on a poor understanding of the eligibility requirements for PTSS, particularly in relation to escorts. While the referring doctor or hospital should provide information, often this is not the case. Crisis admissions are very likely not to have been provided with appropriate information.
- Dissemination of information on accommodation options and entitlements. Some carers appear to be expected to bear a much greater proportion of the costs of accommodation and travel than others.
- Recognition of the level of care required from the carer post-discharge. Improving the nature and extent of information provided to the carer about the post-discharge care requirements and recognition of the carer role and its responsibilities.
- Improve the quality of information provided about support services in the local community. Lack of information may seriously limit choices and preparedness for the post-hospital experience. Services taken for granted in urban areas may be limited, inappropriate or non-existent in rural and remote areas.
Conclusion
Overall, the cases in this study suggest that the position of both patients and carers has been negatively affected by the current earlier discharge from hospital, and that carers themselves have not been able to enjoy the benefits of discharge planning.
These trends are indicative of the significant ways in which hospitals and other health services are offloading some of their costs and 'inefficiencies' onto patients, carers, communities and other parts of the health and welfare system, and shifting the burden of care and responsibility more and more onto primary care givers in the community.
Acknowledgements
The authors would particularly like to thank Monica Ward and Suzanne Hutchinson who assisted with data collection and identification of relevant literature. The study was assisted by the support of a JCU Merit Research Grant, value AU$18,000 (Hospitalisation and Rural Patients; R. Thorpe, C. Williams and N. Harris, 2000).
References
1. Wakerman J, Lenthall S. Remote health. In: Wilkinson D, Blue I (Eds). The new rural health. Melbourne: Oxford University Press, 2002; 126-148.
2. Palmer G, Short S. Healthcare and public policy, 3rd edn. Melbourne: Macmillan, 2000.
3. Clemens E. Multiple perceptions of discharge planning in one urban hospital. Health and Social Work 1995; 20: 254-261.
4. Health Issues Centre. A woman's work is never done: the impact of shifting care out of hospitals. Melbourne: Health Issues Centre, 1997.
5. Kelcher E, Ellis J. Rural people utilising urban hospitals: issues for service provision. Australian Journal of Rural Health 1996; 4: 144-150.
6. McDermott R. Redressing urban bias: a needs based approach to healthcare. In: Proceedings, Issues Affecting Rural Communities, Townsville, 10-15 July 1994. Townsville: Rural Education and Research Development Centre, 1994.
7. Williams C, Dunn P. The elderly in rural and remote Australia: some perspectives on social justice and efficiency in human service delivery. Proceedings of the 26th Annual National Conference of the Australian Association of Gerontology, Sydney: AAG, 1991.
8. Veitch P, Sheehan M, Holmes J, Doolan T, Wallace A. Barriers to the use of urban medical services by rural and remote area households. Australian Journal of Rural Health 1996; 4: 104-110.
9. Strauss A, Corbin J. Basics of qualitative research: techniques and procedures for developing grounded theory. Thousand Oaks: Sage, 1998.
10. Hudnall Stamm B. Rural behavioral care: an interdisciplinary guide. Washington: American Psychological Association, 2003.
11. Thorpe R. Foster care research in Australia: can we count on making a difference to policy and practice? (Keynote Address) In: Proceedings, Protecting Children What Counts? An Overview of Research Conference, 8 August 2003. Airlie Beach: Centre for Research on Community and Children's Services (Mackay), 2003.

