Complementary and alternative medicine (CAM) is defined by the National Center for Complementary and Alternative Medicine in the USA as therapies not considered to be part of conventional medicine as practiced by medical doctors, doctors of osteopathy, and allied health professionals1. CAM therapies include many diverse practices such as homeopathy, massage, chiropractic, relaxation techniques, and herbal medicine2. Alternative medicine is popular throughout the industrialized world1,3,4. CAM has become increasingly popular among Americans over the past several decades1,5, with a substantial proportion of the general population using CAM5. Up to 50-65% of adults in developed countries use some form of CAM for their health-related problems6,7. Many Americans use CAM therapies to complement rather than replace mainstream or conventional medicine5. The CAM products are used for various conditions and disease states including prostate cancer, diabetes, ulcerative colitis, pain management, inducing labor, and autism spectrum disorders8-11.
People seek out and use CAMs for multiple reasons, including (i) ethnic or cultural beliefs (many immigrant communities hold health beliefs and practices that favor CAM use)12, (ii) an interest in spiritual or personal growth, (iii) convenience12, (iv) availability of conventional medicine12, (v) dissatisfaction with the ability of conventional medicine to adequately treat chronic and terminal illnesses13-15, and (vi) the need to have greater control of their own health6. In addition, many people are worried about the cost of conventional care16 and many find CAM therapies to be cost-effective17. Overall, people use CAM therapies if they believe that these therapies will help to improve their health and wellbeing18,19.
A majority of CAM users tend to be female, affluent (eg higher incomes), middle-aged, better educated, white, and of poor health status5,7,18,20. Many people with chronic16 and terminal illnesses such as chronic pain, Alzheimer's disease, rheumatic diseases, cancer, headaches, anxiety and back pain use CAM therapies more than other patients13,18,21. Many Americans pay for CAM therapies out-of-pocket as many CAM therapies are not covered by third-party payers12 - Americans spent $33.9 billion out-of-pocket on CAM in 200712.
Notable safety and efficacy issues are associated with CAM use. Unlike conventional medicines, most of the alternative medicines sold over the counter are not heavily regulated by the US Food and Drugs Administration; therefore, their quality may not be consistent from one batch to another. The quality of products can vary significantly from one supplier to another. Few efficacy and safety studies have been conducted on CAM therapies prior to marketing22,23.
Some physicians do not endorse CAMs or certain CAMs3. CAM therapies, as with any medication, can interact with conventional medications9 prescribed by healthcare providers, causing them to be sub-therapeutic or supra-therapeutic. This underscores the need for physicians and other healthcare providers to be knowledgeable of the CAM therapies their patients are taking for optimal clinical care. However, many CAM users do not disclose their usage to their healthcare providers5.
The prevalence of use of CAMs varies markedly in the USA, most likely due to methodological and regional differences (eg rural vs urban)7,18. No known CAM study in the USA has included a predominantly rural population. A typical user of CAM in a rural area may have different characteristics to those reported in the literature. The purpose of this study is to evaluate CAM usage in the Central Appalachia region, a predominantly rural setting. Many Central Appalachia residents do not have access to health care. Reasons for this include lack of specialist services; long distances to access services; limited public transportation; lack of health insurance, cost; and shortage of healthcare professionals24 and specialist services such as dentistry, mental health services and obstetrics services.
The specific research objectives of the study are to determine:
- the prevalence in CAM usage among the adults in Central Appalachia
- the frequency of use of complementary and alternative medicine of Appalachians
- the main reasons people choose to use CAMs
- the main health problems for which the people used CAM therapies
- people's willingness to share their CAM usage information with their healthcare providers
- the relationship between CAM usage and demographic factors.
Design
The survey was administered in July and October 2012 at two different remote area medical events, in the Wise and Buchanan counties in Central Appalachia.
Instruments
Data were collected using a two-page survey consisting of 23 items developed for this study. The draft survey was circulated to four pharmacy faculty members to check the validity of the questions on the survey. Minor modifications were made after incorporating the changes suggested. The survey was completely voluntary and informed consent was obtained orally from prospective participants. Each survey began with the statement, 'Completing this survey serves as your informed consent. Your answers cannot be linked to you. It is completely voluntary.' The questions on the survey addressed various aspects concerning CAMs, such as whether patients had utilized CAMs before, frequency of use, the main reasons for using CAMs, and whether CAMs were their primary choice of treatment. Survey items included:
Q. Please check all forms of treatment you have used before: herbal/natural products/massage/chiropractic/osteopathic/vitamins/faith healing or minister/acupuncture/other (please specify).
Q. What are the main reasons why you choose complementary and alternative medications (choose all that apply): convenience/affordable/availability/works well/safety/less side effects than drugs/easy to use/other.
The survey also had questions about whether the participants were comfortable in telling their doctors or other medical personnel about their CAM usage, and the importance of these health care professionals knowing of their usage. Eight questions assessed patients' demographic characteristics such as gender, race/ethnicity, year born, insurance coverage, having a primary care provider, place of residence, annual gross income, and highest level of education attained.
Participants
The study targeted 250 participants who were 18 years or older, not pregnant, and residents of the Appalachian region who were attending free medical care clinics and agreed to participate.
Procedures
Prospective participants who were waiting for medical services at the remote area medical events in Wise and Buchanan counties were asked by Appalachian College of Pharmacy students if they would be willing to participate in the survey about CAM therapies. Those who agreed to participate in the study completed the survey. The survey took approximately 8 minutes to complete. Appalachian College of Pharmacy students were available to provide assistance in completing the survey. All the completed surveys were collected by the students and forwarded to the primary investigator (first author) upon completion.
Data analysis
All the data were entered into Microsoft Excel 2010 and then uploaded to PASW Statistics 18 (SPSS Inc.; http://www-01.ibm.com/software/analytics/spss) for analysis. The means, standard deviations, and frequency distributions of all variables were computed. Chi-square analysis was used to explore the association between CAM use and gender, having a primary care provider, having health insurance, annual gross income and highest level of education attained. An alpha level of 5% was used for statistical significance (p≤0.05).
Ethics approval
This cross-sectional descriptive study was approved by the Edward Via College of Osteopathic Medicine Institutional Review Board; approval number 2011/016.
Of the 250 surveys administered, 192 were useful and complete (a 76.8% response rate). Fifty-eight surveys were excluded from analysis because of missing data. Most of the respondents (n=108; 56%) were female, had a primary care provider (n=116; 61%), did not have medical insurance (n=105; 55%) and had annual incomes under $20,000 (n=105; 55%) (Table 1).
Prevalence and frequency of CAM usage
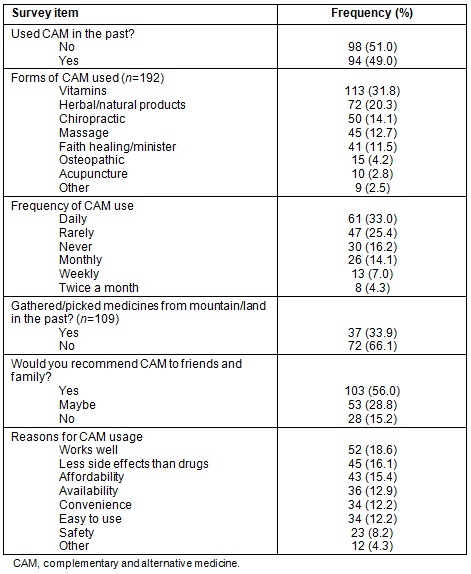
Ninety-four respondents (49%) reported having used CAM therapies in the past. Fifty-eight per cent (n=108) of respondents used CAM therapies at least once a month with 61 (33%) respondents reporting using CAM on a daily basis.
Most respondents utilized vitamins (n=113; 58.9%), and herbal/natural products which were utilized by 72 respondents (37.5%).
Thirty-seven respondents (34%) reported gathering or picking their CAMs from the land or mountain (Table 2).
Main reasons for using CAM
The top three reasons cited by respondents for CAM use were 'they work well' (n=52; 27%), 'they have less side effects' (n=45; 23%), and 'they are affordable' (n=43; 22%) (Table 2). Other reasons cited included availability, convenience, ease of use, and safety (Table 2). Most respondents (n=103; 56%) said they would recommend CAM therapies to their friends and family (Table 2).
Table 1: Respondent demographics
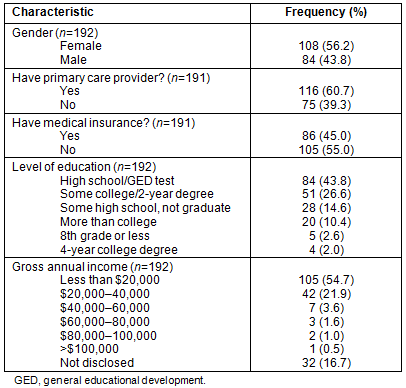
Table 2: CAM use: frequency, types and reasons
Health problems for which CAM was used
CAM therapies were mostly used for back pain (n=23; 15.6%), general health and wellbeing (n=22; 14.9%), depression and anxiety (n=11; 7.5%), and for general pain (n=11; 7.5%) (Table 3). In addition, CAM therapies were used for a host of other problems including arthritis, migraine or headaches, neck pain, energy, fatigue, diabetes, sleep, fibromyalgia, finger numbness, constipation, high blood pressure, cold/allergies, prophylaxis, anemia, nutrition, and weight problems (Table 3).
Relationship between CAM usage and demographic factors
There was no statistically significant association between having medical insurance (p=0.31) and gender (p=0.15) and CAM usage (p>0.05). Having a primary care provider, current level of education, and gross annual income were all significantly associated with CAM use (p<0.001).
Willingness to share information about CAM usage with healthcare professionals
Most (n=94; 85%) respondents reported that they felt comfortable telling their doctor or other medical personnel about their use of CAM therapies. Asked about the healthcare professionals with whom they were likely to share information about their use of CAM, respondents mentioned doctors (n=92; 44.0%), pharmacists (n=60; 28.7%) and nurses/nurse practitioners (n=53; 25.4%) (Table 4).
A total of 83 respondents (76.2%) considered it important or very important for them to share their CAM use information with their healthcare providers (Table 4).
Table 3: Health problems prompting CAM use
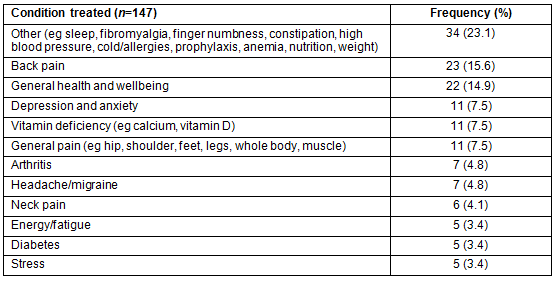
Table 4: Sharing information about CAM usage with health professionals

Discussion
Our research findings showed 49% of the respondents reported using CAM, a figure that is higher than CAM use prevalence reported in the literature. For example, results of a national survey found that 42.1% of the respondents used alternative therapies in 19975. In a separate survey in 1990, about 33.8% of the respondents used alternative therapies13. In a random sample of 1035 individuals in the USA, 40% of respondents had used some type of CAM during the previous year18. Relative to these, the findings of this study suggest that CAM use in Central Appalachia is high and that more Central Appalachia residents use CAM than the rest of the US population12.
The high CAM use in Central Appalachia could be explained by many factors. Central Appalachia residents have limited access to conventional medical care, especially specialist services24, and may use CAM therapies in place of conventional medical care. High usage could be explained by access to forests and herbal medicines within them. The Central Appalachia region has heavily wooded areas where CAM products can be grown and collected. The availability of these resources was cited by participants as one of the reasons for their usage of CAMs. The high usage could also be explained by poverty: in 2008, 24% of the Central Appalachian residents were poor25. Many residents of Central Appalachia are unemployed with unemployment rates higher than state (Virginia) and national averages25. Many of these people often cannot afford the cost of conventional medical care and medicines, and may be inclined to use CAM therapies.
CAM therapies were mostly used for back pain, general health and wellbeing, depression and anxiety and for general pain. Previous studies found that CAMs were mainly used for neck and back problems and arthritis5,16. A sizeable proportion of the respondents used CAM therapy for health promotion or disease prevention.
The high CAM usage among Central Appalachia residents has notable implications for delivery of conventional medical care in the region. It is important for physicians, pharmacists, and nurses to be aware of this wide usage of CAMs by their patients because CAM therapies may interact with other medications they prescribe or dispense. Healthcare professionals need to be made aware of these findings and be encouraged to be vigilant and ask their patients about their CAM usage to provide truly patient-centered care.
The results showed that many factors affect an individual's decision to use CAMs. The main reason respondents used CAM was that it worked well or was efficacious for their health concerns. Many other patients find CAM to be useful in improving their overall health as evidenced by the large and expanding global CAM market, estimated to be $113 billion10. This positive belief in the efficacy of CAMs persists despite lack of formal evidence for the effectiveness and cost-effectiveness of many CAM therapies.
Although some CAM therapies are expensive and are not covered by third-party payers, many patients (22%) chose CAM therapies, citing their affordability. Given that most of the people in Central Appalachia are poor and unemployed, affordability is of significant importance. Interestingly, there was no significant relationship between CAM usage and insurance coverage status (p>0.05). This may suggest that CAM therapies are more affordable than other treatment options available to the respondents.
Contrary to the results of previous studies13,25 most Appalachian patients (85.5%) were comfortable sharing their information about using CAM products with their healthcare providers, especially doctors and pharmacists. Eisenberg et al. found that 72% of the users did not inform their physicians about their use of CAMs13. Another national survey found that only 38.5% of the respondents disclosed their use of alternative therapies to their physicians5. It is unclear why respondents in this study were more willing and comfortable to share their CAM usage with their physicians and other healthcare professionals. The results could be explained by longer lasting and personal relationships that patients in small and rural communities in Central Appalachia have with their healthcare providers. Additionally, many healthcare professionals are not very opposed to the forms of CAM mostly used (eg vitamins, chiropractic, massage, and faith healing). These therapies are also frequently used by consumers in other parts of the USA13,18.
These study results show that level of education and annual gross incomes are significantly associated with CAM usage of respondents (p<0.05). This is similar to the results of Astin, who found that educational level predicted use of CAM18. Most CAM users in the Central Appalachia region tended to be of low income (<$20,000) and have high school education, contrary to previous studies which found that CAM users were mostly well-educated, affluent and middle-aged white people5,7,18,20. Another patient characteristic associated with CAM usage is having a primary care provider. The patients with a primary health care provider were more likely to use CAM therapies.
Future research
More studies should be conducted to investigate why the Central Appalachians are more comfortable telling their doctors and other medical professionals about their use of CAM therapies, especially from the healthcare professional's point of view. Also, more studies should replicate this study, using a random and bigger sample.
Limitations
This study did not provide a definition of CAM or alternative medicines, instead capturing the respondents' beliefs and opinions without biasing them. It is possible that different respondents had different ideas of what CAM is and is not. The study targeted participants who were seeking free conventional medical services at remote area medical events and therefore they may not be a good representation of the general population. Patients were not randomly selected - convenience sampling was used. This may limit the ability to generalize the findings. The study may not be generalizable to other areas given that Central Appalachia and its residents may be somewhat different to the rest of the US population in terms of access to forest and other natural products.
People in the Central Appalachia region reported a prevalence of CAM usage higher than the national average. Most people utilized CAM because they believed it worked well, had fewer side effects, and was affordable; and CAM was used mostly by poor, less educated patients who mostly had a primary care provider. Most people in Central Appalachia were comfortable sharing their CAM usage information with their healthcare providers. More research needs to be conducted to understand CAM usage in rural communities in the USA.
Acknowledgements
The authors thank the patients who voluntarily responded to the survey and the students who served as data collectors for this study.
References
1. National Center for Complementary and Alternative Medicine. Complementary, alternative, or integrative health: what's in a name? (Online) 2013. Available: http://nccam.nih.gov/health/whatiscam (Accessed February 2013).
2. Astin JA, Marie A, Pelletier KR, Hansen E, Haskell WL. A review of the incorporation of complementary and alternative medicine by mainstream physicians. Archives of Internal Medicine 1998; 158(21): 2303-2310.
3. Perry R, Dowrick C, Ernst E. Complementary medicine and general practice in an urban setting: a decade on. Primary Health Care Research and Development 10 April, 1-6. (Online) 2013. Available: http://dx.doi.org/10.1017/S1463423613000182 (Accessed 11 September 2013).
4. Posadzki P, Lee MS, Moon TW, Choi TY, Park TY, Ernst E. Prevalence of complementary and alternative medicine (CAM) use by menopausal women: a systematic review of surveys. Maturitas 2013; 75(1): 34-43.
5. Eisenberg DM, Davis RB, Ettner SL, et al. Trends in alternative medicine use in the United States, 1990-1997: results of a follow-up national survey. Journal of the American Medical Association 1998; 280(18): 1569-1575.
6. Astin JA. Why patients use alternative medicine: results of a national study. Journal of the American Medical Association 1998; 279(19): 1548-1553.
7. Ernst E. Prevalence of use of complementary/alternative medicine: a systematic review. Bulletin of the World Health Organization 2000; 78(2): 252-257.
8. Alaaeddine N, Okais J, Ballane L, Baddoura RM. Use of complementary and alternative therapy among patients with rheumatoid arthritis and osteoarthritis. Journal of Clinical Nursing 2012; 21(21-22): 3198-3204.
9. Barry DT, Savant JD, Beitel M, et al. Use of conventional, complementary, and alternative treatments for pain among individuals seeking primary care treatment with buprenorphine-naloxone. Journal of Addiction Medicine 2012; 6(4): 274-279.
10. DiNardo MM, Gibson JM, Siminerio L, Morell AR, Lee ES. Complementary and alternative medicine in diabetes care. Current Diabetes Reports 2012; 12(6): 749-761.
11. Klempner SJ, Bubley G. Complementary and alternative medicines in prostate cancer: from bench to bedside? Oncologist 2012; 17(6): 830-837.
12. Harris PE, Cooper KL, Relton C, Thomas KJ. Prevalence of complementary and alternative medicine (CAM) use by the general population: a systematic review and update. International Journal of Clinical Practice 2012; 66(10): 924-939.
13. Eisenberg DM, Kessler RC, Foster C, Norlock FE, Calkins DR, Delbanco TL. Unconventional medicine in the United States. Prevalence, costs, and patterns of use. New England Journal of Medicine 1993; 328(4): 246-252.
14. Mitchell S. Healing without doctors. American Demographics 1993; 15(7): 46-49.
15. Perelson GH. Alternative medicine: what role in managed care? FHP Journal of Clinical Research 1996; 5: 32-38.
16. Barnes P, Bloom B, Nahin R. Complementary and alternative medicine use among adults and children: United States, 2007. National Health Statistics Reports 2008; (12): 1-23.
17. Herman PM, Craig BM, Caspi O. Is complementary and alternative medicine (CAM) cost-effective? A systematic review. BMC Complementary and Alternative Medicine 2005; 5: 11.
18. Astin JA. Why people use alternative medicine: results of a national study. Journal of the American Medical Association. 1998; 279(19): 1548-1553.
19. Blair L. Opening Pandora's box. Family physicians and alternative medicine. Canadian Family Physician. 1995; 41: 1807-1810.
20. Paramore LC. Use of alternative therapies: estimates from the 1994 Robert Wood Johnson Foundation National Access to Care Survey. Journal of Pain and Symptom Management 1997; 13(2): 83-89.
21. Coleman LM, Fowler LL, Williams ME. Use of unproven therapies by people with Alzheimer's disease. Journal of the American Geriatrics Society 1995; 43(7): 747-750.
22. Levin S. Alternative medicine - a doctor's perspective. South African Medical Journal 1996; 86(2): 183-184.
23. Rees MK. Alternative medicine: down the slippery slope. Modern Medicine 1997; 6567-6568.
24. Behringer B, Friedell GH. Appalachia: where place matters in health. Preventing Chronic Disease 2006; 3(4): 1-4.
25. Appalachian Regional Commission. Economic assessment of Appalachia: an Appalachian Regional Development Initiative Report. Washington, DC: Appalachian Regional Commission, 2010.



