Recruitment and retention of qualified physicians and other clinical staff have long challenged rural communities. Due to demographic changes in the USA and the insurance expansions in the Patient Protection and Affordable Care Act, the healthcare legislation that will expand the number of Americans with health insurance, the Association of American Medical Colleges estimates that the national shortage of primary care physicians will increase from 9000 to 65 800 between 2010 and 20251. Thus, rural communities will face even greater difficulty competing for a tighter supply of physicians.
A few personal factors are known to positively influence physicians' decisions to practice in rural settings: returning to a community where the physician grew up, or one like it2-5, staying in the general area where a residency was completed4, lifestyle preferences3, spousal preference2,5, and earning potential2,5. There is evidence that workplace factors - including positive professional situation (eg access to continuing education, collegial support, degree of autonomy, career pathway), maintenance of adequate and stable staffing, sufficient infrastructure (including information technology), and sustainable workplace organization - may also affect recruitment and retention, although it is unlikely that these factors alone would lead a physician to choose rural practice if he or she were not already inclined to do so2,5,6.
A professional network likely encourages physician retention in rural practices, as physicians within a professional network can count on collegial support in a variety of situations4. The ongoing diffusion of telemedicine in rural areas has the potential to facilitate such a network for physicians who practice in isolated areas.
The possibility that telemedicine may enhance rural physician recruitment and recruitment has been frequently hypothesized, but rarely studied. In a recent systematic review, Gagnon et al. identified 13 studies related to the effects of information and communication technologies on recruitment and retention of healthcare professionals, of which nine showed a positive effect7. However, noting the diversity of telemedicine applications, healthcare professionals examined, geographic settings, and study methods included in these 13 articles, the authors suggested the need for more research. Dolea et al. identified telehealth technology as a possibly effective retention strategy in their global review of recruitment and retention of rural healthcare professionals8. In a third review, Moffatt and Eley identify 143 articles on reported benefits of telemedicine for rural Australians, of which three suggested that telemedicine could improve rural recruitment and retention of healthcare workers9. However, only one of these articles, an analysis of continuing medical education for psychiatrists delivered via videoconference, presents any evidence to support the hypothesis that telemedicine increases rural recruitment and retention10. In the case of rural physicians in the USA, Baker et al. included televideo technology in surveys that rank factors in rural US states11,12, concluding that the availability of televideo is one of the least important facility and community factors influencing physician recruitment and retention. However, these authors also found that other factors potentially influenced by telemedicine (eg working hours, call responsibilities, transfer arrangements, perception of quality) ranked among the more important influences on physician recruitment and retention.
While direct analyses of recruitment and retention are limited, the telemedicine literature indirectly suggests that tele-emergency services may improve the workplace for rural clinicians. For example, studies have noted that tele-emergency facilitates knowledge transfer between the hub staff and peripheral staff13-17, increases peripheral clinicians' comfort with decision-making18-23, and reduces professional isolation2,17.
The tele-emergency program studied here allows rural emergency departments (EDs) to communicate with an emergency medicine specialist in the tele-emergency hub, similar to services elsewhere that have been used to support general practice physicians, physician assistants (PAs), and nurse practitioners (NPs) who staff rural EDs. In the UK, some minor injury units (MIUs) are staffed by nurse practitioners, with consultation provided remotely by physicians13,15,17,24,25. Similarly, a physician shortage in rural Mississippi led the University of Mississippi at Jackson to provide physician backup via telemedicine for specially trained rural nurse practitioners in that state26,27. These telemedicine programs have generally reported satisfactory clinical results and staff acceptance13,15,17,24-27.
This article presents the results of a mixed-method study involving a broadly administered survey and a more focused interview approach of users of a widely implemented tele-emergency service in the Upper Midwest. The tele-emergency service in this study connected a large hub ED, including board-certified emergency medicine physicians and ED nurses, with multiple smaller hospital EDs. The client EDs were generally staffed by primary care physicians, nurse practitioners, or physician assistants. At any time, clinical staff at the peripheral hospitals could press a button for immediate, synchronous audio/video connection to the tele-emergency hub. The technology allowed staff, patients, and family members located at the client hospital to consult with the hub's staff, and also provided the hub clinicians access to patient medical records. Staff in the remote EDs typically consulted regarding patients who might be a candidate for transfer, may have complex traumatic injuries, or may have serious acute illnesses requiring rapid diagnosis (eg stroke, acute myocardial infarction).
This study makes an important contribution in several ways. First, none of the literature cited above has specifically examined the impact of a tele-emergency service on physician recruitment and retention. Thus, this article adds to the 'deeper reflection' on telemedicine and recruitment and retention recommended by Gagnon et al7. Second, field research was conducted in 2012 and 2013, by which time adoption of telemedicine in rural areas had become widespread. By this time, many survey respondents and interviewees had sufficient experience with telemedicine to comment directly on the question of whether and how telemedicine had influenced physician recruitment and retention. In light of the lack of evidence of direct effects in the few studies that address telemedicine's role in recruitment and retention, this is an important contribution. Finally, recent guidance from the Centers for Medicare and Medicaid Services (CMS), the government agency charged with administering US public insurance programs, allows rural hospitals more flexibility in using tele-emergency to alleviate local physician shortages. This research suggests ways in which hospitals and physicians might respond, given that this recent CMS guidance may increase hospitals' use of tele-emergency to staff rural EDs.
Following a review of the literature, a survey was designed to collect user perceptions on multiple facets of telemedicine care. The survey included separate components on tele-emergency and two other telemedicine services; respondents were provided links to only the component(s) pertaining to services provided at their own hospital. The tele-emergency survey component included questions about respondent's role, hospital characteristics, potential tele-emergency benefits, relationship between tele-emergency and recruitment and retention of healthcare providers, and physician work environment. For questions about tele-emergency benefits, recruitment and retention, and work environment, respondents indicated agreement or disagreement in one of six response categories. The full tele-emergency survey component is included as Appendix I.
The survey link was sent electronically to a single contact person at all 71 hospitals subscribing to the tele-emergency service. The health system providing the service selected these representatives because they had access to email as part of their regular work responsibilities, unlike many rural hospital staff. The selected representatives were asked to share the survey with all staff in their hospital, and to encourage those staff members to complete the survey. Due to the way in which the survey was distributed, the actual number of staff who received the survey is not known, and therefore a response rate cannot be calculated. However, at least one response was received from every hospital that received an electronic survey link for internal distribution. In all, 292 respondents completed surveys and indicated they were familiar with the tele-emergency service in use at their hospital. Hospital-level utilization data were obtained from the health system providing the tele-emergency service. Analysis of survey responses was conducted using SAS v9.3 software (SAS Institute; http://www.sas.com). Statistical differences between groups of respondents were tested using generalized estimating equations for ordinal responses, and χ2 or Fisher's exact test, as appropriate, for dichotomous response categories.
Phone interviews and site visits were also conducted with a sample of 52 clinicians and administrators at 16 rural hospitals that used this tele-emergency service. Protocols for the phone interviews and site visits are provided in Appendices II and II, respectively. The hub offering the tele-emergency service provided contact information for CEOs of 16 hospitals that might be willing to participate in an interview. Due to scheduling conflicts, two were not successfully reached for interviews. After semi-structured phone interviews with 13 CEOs (one of whom acted as CEO of two sites), eight hospitals were visited. These eight hospitals were selected from the original 16 to allow two co-authors to travel to conduct a maximum number of site visits in the allotted time period of 1 week.
Figure 1 displays the sampling approach. During each site visit, multiple clinical staff and administrators were interviewed. All interviews were recorded and subsequently transcribed. The co-authors analyzed the survey responses, read the interview transcripts, and agreed on the principal themes reported as findings in this article.
Table 1 provides background information on the 16 hospitals where interviews were conducted. 13 of 16 hospitals are critical access hospitals (CAHs), rural hospitals with 25 or fewer beds that are reimbursed by Medicare based on their costs. Medicare calculates payments for larger hospitals, including the other three where interviews were conducted, using a prospective payment system (PPS) that does not consider an individual hospital's costs.
Table 1: Characteristics of hospitals where interviews or on-site visits were conducted
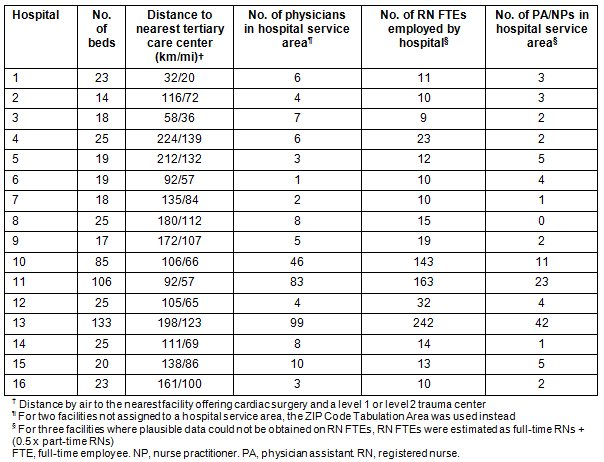
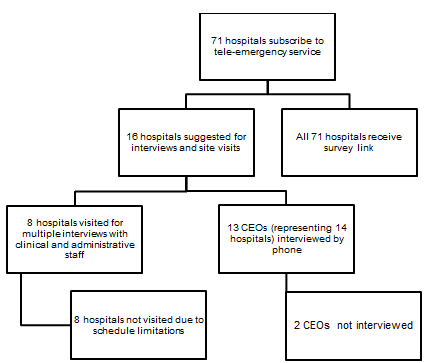
Figure 1: Interview and survey respondents.
Ethics approval
The protocols for the survey and interviews were approved by the University of Iowa Institutional Review Board (approvals #201111717, #201203722, and #201302760).
Survey responses
As shown in Table 2, the survey found that 65% of respondents agreed, and a majority of respondents (53%) agreed moderately or strongly, with the statement that tele-emergency helped with recruitment and retention of healthcare professionals. Sizeable majorities of respondents also responded positively to each of five other items related to the effect of tele-emergency on the work environment.
Table 3 summarizes how responses to the recruitment and retention question varied among subgroups. Among employees of CAHs, who constituted the vast majority of respondents, there was no significant difference between the responses of staff at smaller hospitals (1-15 beds) and the responses of staff at larger hospitals (16-25 beds). There was also no statistically significant difference in the responses provided by clinicians (staff with regular patient contact) and non-clinicians (administrators and managers), nor between physicians and PAs/NPs. However, providers (physicians, PAs, and NPs) responded significantly more positively than did nurses.
Table 4 presents analyses of the relationship between responses to the recruitment and retention item and the other work environment questions. Respondents who provided a positive response to the recruitment and retention item were significantly more likely to respond positively to three of five work environment questions. Also, responses to the work environment questions were examined to determine whether they varied by respondent role (provider vs non-provider, physician vs PA/NP), but responses did not vary significantly by clinical role.
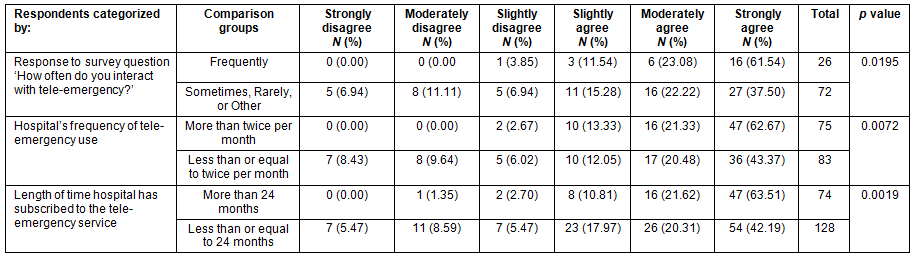
Table 5 contains the results of the relationship between responses to the recruitment and retention item and different measures of tele-emergency utilization. Respondents reporting a positive recruitment and retention effect were also more likely to work in hospitals where tele-emergency was more frequently utilized, and where the tele-emergency service had been available for a longer period of time. Respondents were also more likely to report positive recruitment and retention effects if they themselves reported frequent interaction with the tele-emergency service.
Table 2: Responses to selected survey items
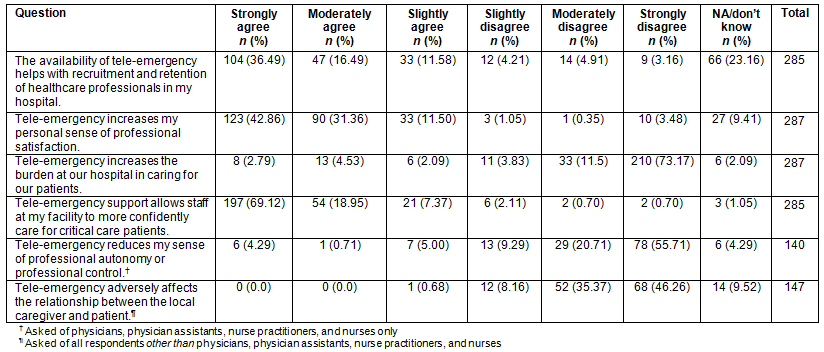
Table 3: Responses to 'The availability of tele-emergency helps with recruitment and retention of healthcare professionals in my hospital'
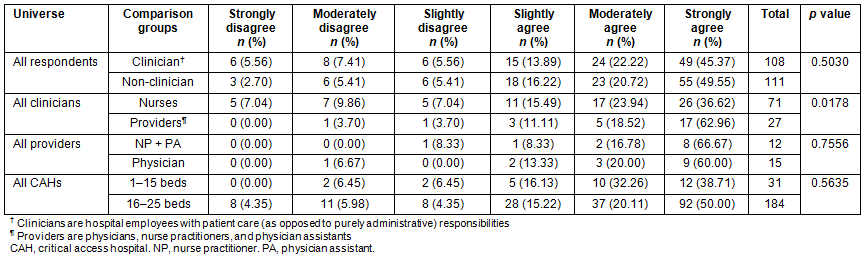
Table 4: Crosstab of recruitment and retention responses with other workplace-related questions

Table 5: Responses to recruitment and retention question by measures of tele-emergency utilization
Interviews
Detailed interviews provided a deeper understanding of how tele-emergency had an impact on recruitment and retention. Principally, interviewees reported that the tele-emergency service in this study directly improved both the local physician work environment and recruitment and retention. Interviewees stated that recruiting physicians to rural areas is extremely difficult. There was consensus among interviewed administrators, physicians, PAs/NPs, and nurses that tele-emergency helps attract physicians to rural hospitals, and helps them remain in rural practice, by reducing professional isolation and workload. Rural hospital administrators facing fiscal constraints often justified the expense of tele-emergency services by noting its effect on physician recruitment and retention. For some interviewees, this was the most important benefit of tele-emergency services.
I've got to admit, the two docs I've got on right now, ... both have made the statement to me directly that if it wasn't for tele-emergency, they would not have come out here because they were not comfortable with it. (Hospital CEO)
Physician confidence in patient care: Interviewees said that professional isolation is a drawback to rural practice, and that the availability of experienced board-certified emergency physicians through tele-emergency is reassuring for local primary care providers. Many interviewees discussed the challenge of recruiting physicians directly out of their residency programs. For these new physicians, accustomed to a semi-supervised work environment with immediate access to specialists and advanced diagnostic tools, the transition to a rural hospital can be particularly challenging and even intimidating. In the view of these interviewees, tele-emergency eases the transition from residency by creating a larger team of colleagues to provide clinical consultation and assist with processes of care.
Many experienced clinicians also shared anecdotes highlighting their increased comfort due to tele-emergency. Assuming sole responsibility for the full spectrum of care required by community members can be professionally and personally taxing. Rural physicians that were interviewed saw fewer traumas and other acute events than their urban counterparts; therefore, such events may be particularly stressful. Tele-emergency helped relieve this pressure for these rural physicians. Many used the phrase 'second pair of eyes' to describe their relationship with the emergency medicine specialists in the hub.
Tele-emergency is the reason why I'm happy and able to practice here. If that service were not here I would be very much more stressed out because my experience while in medicine is very strong, but it is not for emergency medicine and a lot of trauma and other things. (Physician)
If there was a car accident and a 16-year-old was in our ER and we were doing trauma care on this patient, then I would see the family in church on Sunday morning and we needed to be able to look people in the eye and say we've done everything we could do. And that's the peace of mind that tele-emergency gives for us. (Hospital CEO)
Physicians often commented on their increased comfort in cases where the hub's emergency medicine physician did not suggest additional clinical options. Apparently, much of these rural physicians' stress comes from uncertainty, not from their inability to make appropriate clinical decisions.
We had an adverse outcome here ... It was just nice for our provider to get the phone call from the [hub] folks, the docs and the nurses who said 'you know, you guys did everything possible that you could do'. (Hospital CEO)
For many interviewees, tele-emergency alleviated professional isolation that often impedes successful physician recruitment. Many respondents suggested that the availability of clinical backup directly improved recruitment and retention.
Like every other facility in the nation we're trying to find family practice docs and here we really only need one and then supplement that with some mid-levels. Well, our last physician here, she's kind of on an island. ... She can go in and push the button and say I'm thinking this but I'd like a second opinion. (Hospital CEO)
Educational opportunities: Professional networks that give providers an opportunity to trade ideas, discuss cases, and offer general advice, are generally less available to rural physicians28. Several interviewees noted that the relationship with tele-emergency hub physicians facilitates professional networking. Some interviewees used tele-emergency services as a more formal means of providing education, asking the hub to oversee simulation exercises or study for upcoming exams. Interviewees also noted that telemedicine allows their remote hospitals to keep and manage more clinically interesting patients than they would otherwise do, a phenomenon that has been noted in other studies of tele-emergency20,21. This permits rural providers to use and maintain the skills developed during training, and maintain a higher level of interest in their work.
Burden of being on-call: Interviewees observed that burdensome call schedules discourage physicians from practicing in rural areas. When describing their reasons for implementing tele-emergency services, many interviewees stressed that an intense call schedule can exacerbate physician burnout, and the intensity of call had played a role in job decisions for some.
[Physician's name] is from this area but she was the physician in [a nearby hospital] before she came here and if you were to ask her ... the main reason she came from there to here, it wouldn't be because of this location. It would be because the call schedule was so bad at [the other hospital]. She never felt like she was off. She was either on [service] or on call. (Hospital administrator)
When a PA/NP is able to stabilize a patient with the assistance of the tele-emergency hub, calls to the local on-call physician may be reduced. Interviewees suggested that the reduced number of calls can be significant; PAs/NPs often contact the tele-emergency hub as the first source of backup because the hub can obtain immediate visual access to the patient. Many respondents felt that the reduced call burden provided by tele-emergency services was sufficient to improve recruitment and retention.
However, nearly all respondents commented that federal regulations limited the ability of CAHs to further reduce rural physicians' call burden with tele-emergency. A few respondents reported confusion about differing requirements of the Emergency Medical Treatment and Labor Act (EMTALA) and the Medicare conditions of participation (CoPs). EMTALA is a US law that requires all hospitals to provide emergency services regardless of a patient's ability to pay. The CoPs are conditions that hospitals must meet to receive reimbursement from the federal Medicare program. Most respondents interpreted EMTALA to require that hospitals must always have a physician on call and able to be present within 30 minutes, even if emergency services were provided by a PA/NP with immediate access to emergency medicine specialists through tele-emergency. Because hospitals did not use tele-emergency to replace on-call physician backup for a PA/NP, interviewees noted that providing both services was expensive for the hospital and did not fully alleviate the on-call burden for the physician. Some respondents were concerned that the current EMTALA 30-minute response requirement was actually impossible, and several claimed to be aware of hospitals that could not ensure that a physician would be personally present within 30 minutes if requested. A number of hospital CEOs considered changing this regulation to be more important than getting reimbursement for the cost of tele-emergency services.
[Regulatory guidance will] allow PAs and NPs to be your main providers, primary providers, and then turn around and use your back-up physicians and give these guys true nights off. One, it'll help with recruitment, and two, it'll help with longevity with these docs out here. (Hospital CEO)
Of considerable importance to this issue, on 7 June 2013 CMS issued guidance clarifying that hospitals may employ a PA/NP, with access to a physician (MD or DO) via telemedicine, in order to meet EMTALA and Medicare CoP requirements related to immediate, on-call physician availability29.
Discussion
This research provides evidence that tele-emergency helps rural hospitals compete for a dwindling supply of physicians by alleviating professional isolation and a burdensome on-call schedule. Survey respondents indicated that tele-emergency service can directly enhance recruitment and retention, a result that was consistent across respondent groups. In particular, varying respondent roles in the hospitals (administrator vs clinician, physicians vs PAs/NPs) did not differ in their perceptions on this key issue, although providers gave more positive responses than did nurses. Not surprisingly, respondents reporting a positive recruitment and retention effect were more likely to report more frequent use of the system personally, and to work in hospitals where tele-emergency was more frequently utilized, and where it had been available for a longer period of time.
Responses to workplace-related items (professional satisfaction, burden of care, confidence in caring for critical patients, no negative effect on the caregiver-patient relationship) were also positive. Significant associations were found between responses to these items and respondents' views on recruitment and retention, indicating that respondents who believed tele-emergency mitigated some of the workplace challenges of rural physician practice also believed that the service could help physicians remain in rural practice.
Survey findings were further elucidated by interviews. Tele-emergency's effects on the workplace were captured in three themes that emerged from interviews. First, the availability of clinical backup increased physicians' confidence in patient care. Second, tele-emergency allowed rural physicians to become part of a virtual professional network, creating opportunities for on-the-job education in patient care and overcoming what might otherwise be a sense of professional isolation. Third, tele-emergency could reduce rural physicians' on-call burden when ED care could be completed by an onsite PA/NP in consultation with a remote tele-emergency physician. Interviewees explicitly articulated that by improving the work environment, tele-emergency improved professional recruitment and retention.
Rural practitioners in this study viewed telemedicine as one tool to enhance and sustain essential services into the future. Study participants also felt that regulatory guidance enabling tele-emergency to serve as physician backup for PAs/NPs in the ED could increase the recruitment and retention value of tele-emergency. Now that such guidance has been issued, rural hospitals are likely to accelerate their adoption and utilization of tele-emergency services.
Previous literature has not reached a clear consensus on the role of telemedicine in recruitment and retention of healthcare workers, and the effect may vary widely based on attributes of the service, the region, and the type of healthcare worker under consideration. The findings presented here suggest that, at least in the case of tele-emergency, a telemedicine service plays a direct role in recruiting and retaining physicians to rural practice.
This research has some limitations. First, an analysis of survey responses not presented here suggests that interviews were conducted in hospitals where staff more strongly agreed that tele-emergency could improve recruitment and retention. Therefore, while interview responses suggest that tele-emergency enhances recruitment and retention in the local hospital, the responses may not be consistent across a random sample of all small hospitals. Second, the survey question asked about recruitment and retention of 'healthcare professionals'. While the interview data strongly suggest that physician recruitment and retention is foremost on the mind of rural hospital staff, it is possible that some survey respondents had other types of healthcare workers in mind when responding to this question. Third, since this research surveyed and interviewed users of a single tele-emergency service, these findings suggest opportunities for replication elsewhere, but findings are not necessarily generalizable to other telemedicine services. Since tele-emergency is just one of many factors with a potential impact on rural physician recruitment and retention, further research is needed to confirm that the presence of a tele-emergency service is an independent predictor of positive physician recruitment and retention success.
If telemedicine increasingly provides physician backup for rural EDs, it will become even more important to synthesize and fill gaps in the tele-emergency literature, particularly the clinical differences between telemedicine backup and local on-call backup. Further research should also evaluate the impact of tele-emergency service on rural providers, a focus not always incorporated into evaluation studies. With changes underway promoting integration across the continuum, effective service configurations that enhance the roles of local providers will be valuable.
Optimal use of tele-emergency and other telemedicine applications in care models that integrate local and remote services may be achieved if payment and other policies align with applications of these technologies. The recent CMS guidance is one example of such alignment. Payment policies that reimburse sending and receiving telemedicine sites directly for their services could also spur greater use of these services. Health systems may be motivated to invest in tele-emergency technology not only to improve access to care, but also to improve recruitment and retention of the primary care physicians that sustain their systems.
Acknowledgements
This research was funded by a grant from the Leona M. and Harry B. Helmsley Charitable Trust (Grant #2010PG-RHC032). The authors thank Fred Ullrich and Smruti Vartak for assistance with data collection and analysis for this article.
References
1. AAMC Center for Workforce Studies. The impact of health care reform on the future supply and demand for physicians: updated projections through 2025. Washington, DC: Association of American Medical Colleges, 2010.
2. Gagnon MP, Duplantie J, Fortin JP, Landry R. Exploring the effects of telehealth on medical human resource supply: a qualitative case study in remote regions. BMC Health Services Research 2007; 7: 6.
3. Hancock C, Steinbach A, Nesbitt TS, Adler SR, Auerswald CL. Why doctors choose small towns: a developmental model of rural physician recruitment and retention. Social Science & Medicine 2009; 69(9): 1368-1376.
4. Viscomi M, Larkins S, Gupta TS. Recruitment and retention of general practitioners in rural Canada and Australia: a review of the literature. Canadian Journal of Rural Medicine 2013; 18(1): 13-23.
5. Duplantie J, Gagnon MP, Fortin JP, Landry R. Telehealth and the recruitment and retention of physicians in remote areas: a Delphi study. Canadian Journal of Rural Medicine 2007; 12(1): 30-36.
6. Buykx P, Humphreys J, Wakerman J, Pashen D. Systematic review of effective retention incentives for health workers in rural and remote areas: towards evidence-based policy. Australian Journal of Rural Health 2010; 18(3): 102-109.
7. Gagnon MP, Pollender H, Trepanier A, Duplaa E, Ly BA. Supporting health professionals through information and communication technologies: a systematic review of the effects of information and communication technologies on recruitment and retention. Telemedicine and E-Health 2011; 17(4): 269-274.
8. Dolea C, Stormont L, Braichet JM. Evaluated strategies to increase attraction and retention of health workers in remote and rural areas. Bulletin of the World Health Organization 2010; 88: 379-385.
9. Moffatt JJ, Eley DS. The reported benefits of telehealth for rural Australians. Australian Health Review 2010; 34: 276-281.
10. Greenwood J, Williams R. Continuing professional development for Australian rural psychiatrists by videoconference. Australasian Journal of Psychiatry 2008; 16(4): 273-276.
11. Schmitz DF, Baker E, Nukui A, Epperly T. Idaho Rural Family Physician Workforce Study: the Community Apgar Questionnaire. Rural and Remote Health 3(11): 1769. (Online) 2011. Available: www.rrh.org.au (Accessed 9 November 2013).
12. Baker E, Schmitz DF, Wasden S, Mackenzie L, Morris B. Assessing Critical Access Hospital (CAH) assets and capabilities for recruiting and retaining physicians: the North Dakota CAH community Apgar program. Prepared for the Center for Rural Health, University of North Dakota, School of Medicine and Health Sciences, 2011.
13. Darkins A, Dearden CH, Rocke LG, Martin JB, Sibson L, Wootten R. An evaluation of telemedical support for a minor treatment centre. Journal of Telemedicine and Telecare 1996; 2(2): 93-99.
14. Armstrong IJ, Haston WS. Medical decision support for remote general practitioners using telemedicine. Journal of Telemedicine and Telecare 1997; 3(1): 27-34.
15. Mair F, Ferguson J. More patients with minor injuries could be seen by telemedicine. Journal of Telemedicine and Telecare 2008; 14(3): 132-134.
16. Lamonte MP, Bahouth MN, Hu P, Pathan MY, Yarbrough KL, Gunawardane R, et al. Telemedicine for acute stroke: triumphs and pitfalls. Stroke 2003; 34(3): 725-728.
17. Wootton R, McKelvey A, McNicholl B, Loane M, Hore D, Howarth P, et al. Transfer of telemedical support to Cornwall from a national telemedicine network during a solar eclipse. Journal of Telemedicine and Telecare 2000; 6(Suppl 1): S182-186.
18. Bhandari G, Tiessen B, Snowden A. Meeting community needs through leadership and innovation: a case of virtual psychiatric emergency department (ED). Behaviour & Information Technology 2011; 30(4): 517-523.
19. Sakles JC, Mozier J, Hadeed G, Hudson M, Valenzuela T, Latifi R. Telemedicine and telepresence for prehospital and remote hospital tracheal intubation using a GlideScopeTM videolaryngoscope: a model for tele-intubation. Telemedicine and E-Health 2011; 17(3): 185-188.
20. Latifi R, Weinstein R, Porter J, Ziemba M, Judkins D, Ridings D, et al. Telemedicine and telepresence for trauma and emergency care management. Scandinavian Journal of Surgery 2007; 96(4): 281-289.
21. Rogers FB, Ricci M, Caputo M, Shackford S, Sartorelli K, Callas P, et al. The use of telemedicine for real-time video consultation between trauma center and community hospital in a rural setting improves early trauma care: preliminary results. Journal of Trauma 2001; 51(6): 1037-1041.
22. Rosengren D, Blackwell N, Kelly G, Lenton L, Glastonbury J. The use of telemedicine to treat ophthalmological emergencies in rural Australia. Journal of Telemedicine and Telecare 1998; 4(Suppl 1): 97-99.
23. Schwamm LH, Rosenthal ES, Hirshberg A, Schaefer PW, Little EA, Kvedar JC, et al. Virtual TeleStroke support for the emergency department evaluation of acute stroke. Academic Emergency Medicine 2004; 11(11): 1193-1197.
24. Miller DR, Alam K, Fraser S, Ferguson J. The delivery of a minor injuries telemedicine service by Emergency Nurse Practitioners. Journal of Telemedicineand Telecare 2008; 14(3): 143-144.
25. Ferguson J, Rowlands A, Palombo A, Pedley D, Fraser S, Simpson S. Minor injuries telemedicine. Journal of Telemedicine and Telecare 2003; 9(Suppl 1): 14-16.
26. Duchesne JC, Kyle A, Simmons J, Islam S, Schmieg RE Jr, Olivier J, et al. The impact of telemedicine upon rural trauma care. Journal of Trauma 2008; 64(1): 92-98.
27. Galli R, Keith JC, McKenzie K, Hall GS, Henderson K. TelEmergency: a novel system for delivering emergency care to rural hospitals. Annals of Emergency Medicine 2008; 51(3): 275-284.
28. Sargeant J, Allen M, Langille D. Physician perceptions of the effect of telemedicine on rural retention and recruitment. Journal of Telemedicine and Telecare 2004; 10: 89-93.
29. Center for Clinical Standards and Quality/Survey & Certification Group, Centers for Medicare & Medicaid Services. Critical Access Hospital (CAH) emergency services and telemedicine: implications for Emergency Services Condition of Participation (CoPs) and Emergency Medical Treatment and Labor Act (EMTALA) on-call compliance. (Ref: S&C: 13-38-CAH/EMTALA). Baltimore, Maryland: US Department of Health and Human Services, 2013.
____________________________
Appendix I: Tele-emergency survey instrument

Appendix II: Phone interview protocol

Appendix III: Site visit protocol

