Context
There has been an over-representation of Indigenous Australian workers in low-skilled manual jobs and community service jobs1-3. This is due to historical restrictions of educational opportunities combined with a higher concentration of Indigenous workers in areas with fewer employment opportunities1,3. Thus, Indigenous Australians have been exposed to manual handling stress, which, combined with inadequate knowledge of risks and psychological stressors, has led to significant levels of musculoskeletal and stress-related illnesses, few of which have been formally reported or compensated4,5.
Musculoskeletal conditions in rural and remote Indigenous Australian populations are also complicated by the poor health suffered by this group6. Obesity, for example, may predispose to low back pain (LBP) and increase stress and pain in other weight bearing joints7. It is also a risk factor for cardiovascular disease and diabetes.
The purpose of the present report is to describe the process of developing and implementing a pilot, accredited musculoskeletal training program (MTP; subsequently renamed the sports massage course), including the use of culturally appropriate methods for evaluating the changes in skills, knowledge and attitudes of participants in the course.
Issue
The Durri Community of Kempsey, NSW, Australia, comprises one of Australia's largest rural Aboriginal communities8. A quasi-random cross-sectional musculoskeletal prevalence study was conducted in the Kempsey district, New South Wales (NSW) between January 2001 and July 2002, among 189 Indigenous members of this community9.This study showed that Indigenous Australians living in this rural community suffered from multiple musculoskeletal problems that significantly impaired their activities of daily living9. The results showed that LBP, followed by neck, head and shoulder pain were the most common conditions. Approximately 40% of participants suffered from between two and four musculoskeletal conditions. A majority of participants had suffered from their principal condition for 7 weeks or more, indicating high levels of chronicity in the community. Researchers concluded that the majority of people living in this large rural, Indigenous community had learnt to live with chronic levels of pain affecting multiple anatomical sites largely due to financial and socio-cultural barriers9. For instance, approximately 25% of community members who reported experiencing pain had not accessed any treatment for their musculoskeletal condition. When questioned about why this was the case, the most common reasons given were that they had 'learnt to live' with the problem, that they were 'unaware of what might help them', or a belief that 'private therapies were too expensive'.
This research9 was the genesis of the Kempsey sports massage course for Aboriginal Health Workers (AHWs). Apart from the high prevalence of musculoskeletal pain and disability at Durri9, the researchers identified various risk factors which, if addressed, presented an opportunity to prevent or minimize the occurrence of the most commonly identified musculoskeletal conditions. These findings informed the development, implementation and evaluation of a MTP for AHWs.
The program was also informed by ongoing discussions with a Community Advisory Group (CAG). The CAG consisted of community Elders, AHWs, a community nurse and researchers from the University of Newcastle. The CAG highlighted the need for an accredited, practical and culturally sensitive massage program that raised an awareness of bush medicines in the management of pain and disability to preserve and affirm traditional healing practices. Community participation, ownership and sustainability in the design and implementation of the program were seen by the CAG as fundamental to its success.
A gathering of Cultural Elders of the community stated:
We strongly endorse this collaborative, community-based project that affirms our traditional methods of healing and integrates these within an accredited course of study for our health workers and Elders. It is a valuable first step towards providing our community with sustainable health care to reduce the great pain and suffering that our people have learnt to live with [Durri Community gathering, July, 2002].
Cultural considerations
Why sports massage? Ongoing discussions with AHWs and Elders of the Community underlined the importance of first gaining the trust of the community before addressing deeper problems of pain and disability. Sport has historically provided a bridge between Aboriginal and non-Aboriginal people8. Sports massage was chosen as a framework for developing the MTP on the advice of the CAG because sports featured in the life of the community, and therefore sports massage was likely to be culturally acceptable. In addition, the principles of managing musculoskeletal conditions could be incorporated into a course of this kind.
An opportunity for health promotion: Through sport, Aboriginal people of all ages and backgrounds meet regularly on common ground to enjoy activities that promote their health in a broader sense (J Griffin, pers. comm., 2000). The widespread appeal that sports massage engendered in this community presented a valuable opportunity for addressing not only the pain and disability associated with musculoskeletal conditions but also some of the major risk factors associated with mortality and morbidity from cardiovascular disease and diabetes in this and other Aboriginal communities. These risk factors included smoking, obesity, the lack of regular exercise and significant levels of physical trauma and injury. As part of their training, AHWs were instructed in the value of incorporating health promotion messages as part of their management of sports-related and lifestyle illnesses. Smoking cessation handouts and weight loss guidelines could be made available to patients as part of a wholistic approach to promoting their patients' musculoskeletal and general health.
Why train Aboriginal Health Workers? AHWs have been found to provide effective health interventions for their communities10-12. Durri AHWs were well placed to understand the cultural factors involved and social barriers to implementing interventions within their community13. The Aboriginal Medical Service (AMS) was the primary venue for delivering the program as this is the preferred access route for the healthcare delivery undertaken by AHWs13.
Autonomy and self-regulation: 'Health' to Aboriginal people is not merely the provision of doctors and hospitals14. It is a matter of determining all aspects of life, including control over the physical environment, and retaining dignity, community self-esteem and justice14. The message conveyed by many Aboriginal Elders in this and other communities15 was the need for collaboration between Aboriginal and non-Aboriginal people while retaining a measure of independence. Acknowledging traditional healing strategies was recognised as important by the CAG and has previously been accorded priority by national Indigenous health forums16,17.
Development of the sports massage course
The course was developed after first conducting a literature search to determine existing musculoskeletal health programs for AHWs (none were found). The expertise of an experienced course-accreditation consultant was obtained. Ongoing recommendations of the CAG were sought.
Priorities for conducting the sports massage course identified by the CAG are summarised (Fig 1). They included that it be an accredited course, delivered flexibly, on-site with cultural relevance and sensitivity. The course should have potential to be adapted by other rural and remote Aboriginal Communities via the distance learning approaches conducted by Booroongen Djugun College, NSW18.

Figure 1: Suggestions by the community advisory group for developing and delivering the sports massage course for Aboriginal health workers.
The CAG believed that the Murray School of Health Education, NSW, was a training organisation particularly suitable for implementing the sports massage course. This was due to the Murray School of Health Education's practical focus and its flexibly delivered, on-site approach to teaching. Because existing massage courses did not include Indigenous approaches to treating musculoskeletal conditions, this component was subsequently incorporated into the newly designed course and submitted for accreditation (Fig 2).

Figure 2: Summary of the sports massage course content.
Delivery of the sports massage course
AHWs were advised about the course via the normal means of disseminating information in the AMS. This included inclusion of course details in the agenda of regular AMS staff meetings, and via the distribution of a flyer outlining the content and scope of the sports massage course. All administrative components of the course such as registering prospective students and liaising with teaching personnel throughout the program were carried out by the distance learning course co-ordinator at Booroongen Djugun College18.
A lecturer in massage with extensive experience in administering a private massage school, and experience in teaching Aboriginal people, conducted the on-site sports massage course. Apart from the support and encouragement offered by CAG and the principal lecturer, four tutors with relevant massage experience and massage qualifications, one of whom resided in the community, participated in the program, as well as acting as mentors to students throughout the course.
Participants: Twenty participants enrolled in, and completed, the sports massage course (17 females and 3 males). Included were 18 AHWs and two community Elders. Participants' mean age was 38 years. There were two avenues for participation. The first was either a nationally accredited qualification as an AHW, an Assistant in Nursing (AIN) or other allied health qualification. The second enabled community Elders with an interest in the sports massage course to participate and share their own skills and knowledge.
Logistics: The sessions included theoretical and practical components (Fig 3). Participants paired off to practise practical components. The sessions were conducted 3 days per week (Monday, Wednesday and Friday) over a 2 week period. The weekend in between provided students with an opportunity to practise their newly acquired skills as part of a sporting event. In accordance with the recommendations of the CAG the course was delivered with as much flexibility as possible. This included presenting the same session in the morning and the afternoon so that it accommodated the demanding work requirements of AHWs and other participants.
Evaluation of the sports massage course
Practical homework tasks were reviewed by the lecturer and tutors at the commencement of the following session as a way of consolidating prior learning and recording the satisfactory acquisition of learning goals. Each student was subsequently followed up until the tutor was satisfied that the learning tasks had been adequately achieved. Students were deemed to have adequately completed their learning activities if their allocated tutors observed an acceptable level of competence.
Baseline and post-training levels of knowledge and skills were assessed via the individual and group questioning techniques utilised by Booroongen Djugun College18. Baseline skills and knowledge were measured via 'round table' informal questioning prior to each session. Attempts were made to discretely question each participant. AHWs were accustomed to this approach to learning and assessment because it formed the basis of their existing training methods18. Individualized clinical teaching strategies such as these have been successfully employed in training AHWS in other settings19. These informal and interactive methods of teaching and assessment have reportedly optimised strengths and improved weaknesses of AHWs involved in the study of specialised clinical skills20,21. This process for evaluating skills, knowledge and attitudes in the sports massage course is outlined (Fig 3). In addition, an anonymous post-course questionnaire was completed by all participants (Appendix I).
Despite the informal nature of the assessment process, it was clear that, on average, for each topic in the course, only 20-30% of participants appeared to have any significant pre-existing knowledge or skills. By the end of the two weeks of instruction, all participants were observed to have developed adequate competence in all topics.
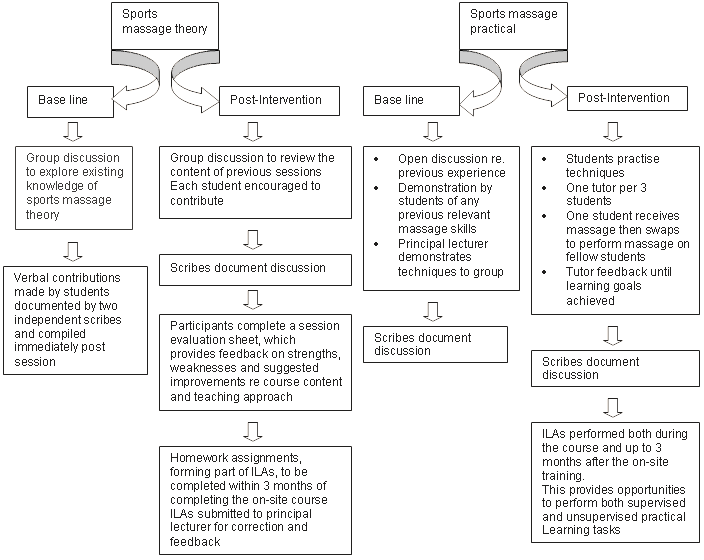
Figure 3: Outline of the process for developing skills, knowledge and attitudes in the sports massage course. ILA, Integrated learning activity.
The training program appeared to be culturally acceptable to the participants of the course. Participants found individual sessions enjoyable, well organised, useful and personally relevant. The acceptability of the course to participants is summarised (Fig 4).
The most common concern reported by students was the level of course difficulty, which was rated as 'relatively difficult' by the majority of respondents, yet practice sessions were not considered 'too difficult' by the majority of participants. The tutors were considered 'very knowledgeable, 'very helpful', and 'very clear' in directing activities.
Encouraging comments brought added meaning to these results.
Personally, I have gained the importance of touch and feel. Professionally, I've learned to make sure that your client doesn't feel intimidated or embarrassed. This was explained and demonstrated professionally. As a nurse working in diabetic health, I can already see the potential to improve patients suffering from stress as well as the pain and discomfort of poor circulation. [Female AHW, aged 38 years].
My father and grandfather were traditional healers of this country. They didn`t go to any white School. They had a gift for it. As a child, I remember that people would come from everywhere to be helped by my father, and he would go to them. My father had a lot of love and healing to give. He would sometimes warm his hands around the camp-fire and touch different points on the face and neck to cure our headaches and other wounds. We need to go back to the bush and to our Elders to learn about the great ways of caring for each other. [Male Elder, aged 50 years].
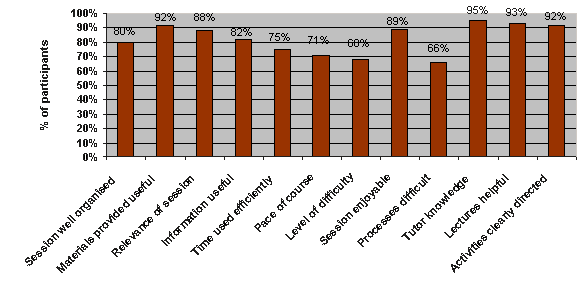
Figure 4: Participants' positive evaluation of the sports massage course (according to rating each item 1 or 2 on the evaluation form, Appendix I).
Lessons
Ongoing practice sessions were developed by AHWs and CAG, and these sessions served to review and refine skills and knowledge.
An important extension of the training program was the use of massage in areas other than sports injuries. For instance, the primary cardiovascular health worker in the community has used massage palliatively in stroke patients with painful soft tissue contractures. Those working in mental health have used relaxation massage for stress reduction of both their colleagues and patients. Some maternal health workers have adapted their skills to infant massage.
The incorporation of introductory lectures on the traditional use of local bush-medicines and massage oils, affirmed aspects of the traditional system of healing, historically adopted by the Dunghutti and Gumbangirr people of the Kempsey district.
The collaborative development of the program according to the needs expressed by the community and articulated via the CAG formed a valuable foundation for the program. The active participation of AHWs throughout all aspects of the program appeared crucial to its success.
Our experience with this program suggests that if Indigenous musculoskeletal health is to be improved in the long term, programs should consider education, the environment and cultural factors, as well as traditional health paradigms. Although this pilot sports massage course relied on volunteer assistance, for sustainability, appropriate funding is essential for training AHWs, who play major roles in health promotion as well as healthcare.
The sports massage course was subsequently accredited nationally by the Industry Training Accreditation Body as the first Indigenously developed and administered massage course.
Acknowledgements
The authors would like to acknowledge the assistance of the Durri ACMS, NSW, as well as the Booroongen Djugun College, NSW, The Murray School of Health Education, NSW, and volunteers from the RMIT University, Victoria, Australia. The authors also thank Hands on Health Australia for funding the program.
References
1. Boreham PG, Whitehouse and Harley B. The labour force status of Aboriginal people: a regional comparison. Labour and Industry 1993; 5: 16-32.
2. Burden J. Health: an holistic approach. In: C Bourke, E Bourke, E Edwards (Eds). Aboriginal Australia. An introductory reader in Aboriginal studies. University of Queensland Press, 2003; 189-218.
3. Australia's Health 2002. The eighth biennial health report of the Australian Institute of Health and Welfare. Australian Institute of Health and Welfare Cat. No. AUS 25. Canberra: AIHW, 2002; 229-230.
4. Mayhew C. Aboriginal and Torres Straight Islander occupational health and safety: a pilot study in Queensland. Australian Aboriginal Studies 1996; 2: 61-68.
5. Vindigni D, Perkins J. The Prevalence of Musculoskeletal Conditions Among Indigenous People Living in Rural Australia: an Opportunity for Health Promotion? Australian Indigenous Health Worker Journal 2003; 27: 4-8.
6. Australian Institute of Health and Welfare. Australia's Health 2002. The eighth biennial health report of the Australian Institute of Health and Welfare. Cat. no. AUS 25. Canberra: Australian Institute of Health and Welfare, 2002.
7. Lecerf JM, Reitz C, de Chasteigner A.l. Evaluation of discomfort and complications in a population of 18102 overweight or obese patients. Presse Medicale 2003; 32: 689-695.
8. Kempsey Shire Council. Community Profile 2000. In: B Huntington. Kempsey Local Government Area, March 2000. Kempsey: Kempsey Shire Council, 2000; 7.
9. Vindigni D, Griffen D, Perkins J, Da Costa C, Parkinson L. Prevalence of musculoskeletal conditions, associated pain and disability and the barriers to managing these conditions in a rural, Australian Aboriginal community. Rural and Remote Health 4: 230. (Online) 2004. Available http://rrh.org.au (Accessed 21 September 2004).
10. Pacza T, Steele L. Dental train-the-trainer program for Aboriginal health workers in the Kimberley Region. A report prepared by the School of Oral Health Sciences, The University of Western Australia. Perth: University of Western Australia, 2000.
11. Doyle MJ, Keeffe JE, Harper CA et al. Training Koori health workers for effective community-based eye care services. Ninth National Health Promotion Conference People, Places and Programs. Darwin; 18-20 May 1997.
12. Ezzy J. Competency based nutrition education and training for trainee Aboriginal health workers at Batchelor College. In: Nutrition Networks `95 Conference, Proceedings of the 4th National Conference, 'Waranyjarrigun Yagarrama Yagarrayirr' Gathering and Sharing'; Broome, Western Australia; 1995.
13. Saggers S, Gray D. Aboriginal health and society: the traditional and contemporary Aboriginal struggle for better health. Sydney, NSW, Australia: Allen and Unwin, 1991.
14. Durie MH . The health of indigenous peoples. BMJ 2003; 326: 510-511.
15. Li'Dthia Warrawee'a K. There once was a tree called Deru. Sydney, NSW: Harper Collins (Australia), 2002
16. National Aboriginal Health Strategy Evaluation Committee. The National Aboriginal Health Strategy: an Evaluation. Canberra, ACT, Australia: Aboriginal and Torres Strait Islander Commission, 1994.
17. Department of Health and Ageing. Aboriginal and Torres Strait Islander Health Workforce National Strategic Framework, AHMAC. Canberra, ACT, Australia: Office for Aboriginal and Torres Strait Islander Health, Department of Health and Ageing, 2002.
18. Booroongen Djugun College and Macleay Valley Workplace Learning Centre Inc. Description of school/organisation. Booroongen Djugun College. Online (no date). Available: http://www.ecef.com.au/WaduResource/objects/157.htm (Accessed 30 July 2003).
19. Pincombe J. Integrating Aboriginal students into the general nursing course. Australian Nursing Journal 1986; 15: 47-49.
20. Keefe J, McCarthy C, Doyle M, Taylor H. The Rumbalara Eye Care Project: initial results of vision screening by Aboriginal health workers. Proceedings, 28th Annual Conference of the Public Health Association of Australia. Threats to Public Health: Challenges and Strategies. 29 September-2 October 1996, Perth, Western Australia; 1996.
21. King M, Sin A. An account from five Aboriginal health workers who undertook the Diabetes educators course at Flinders University. Aboriginal And Torres Straight Islander Health Worker Journal 1999; 23: 19-23.
_____________________





