Introduction
A greater proportion of Indigenous Australians than non-Indigenous Australians live in rural and remote areas and they are more likely to suffer disadvantage1. Additionally, in rural and remote areas, the availability of health professionals, and the distance to the nearest health facilities compromise access to appropriate health services1.
A recent study has shown that Indigenous Australians living in rural communities endure multiple musculoskeletal conditions that impact significantly on their activities of daily living2. Those affected reported enduring high levels of pain with a majority of participants suffering from their principal condition for at least 7 weeks. This suggests a high level of chronic, disabling musculoskeletal conditions that require attention2.
The responsibilities, knowledge, status and duties of Aboriginal health workers (AHWs) make them ideally suited to promoting the health of their community through screening, assessing and managing patients3.
The results of a musculoskeletal prevalence study2 prompted the community to investigate approaches that would enable AHWs to screen, quantify and then assist in the management of commonly identified musculoskeletal conditions.
The objectives of this study were to develop a musculoskeletal screening survey for use by AHWs in Kempsey, New South Wales (NSW), Australia, on a rural Indigenous community; pilot test the survey for cultural acceptability, clarity, face and content validity; and its logistical delivery. An additional objective was to compare the screening survey to an independent clinical assessment for correlation.
Method
Ethics approval
Ethics approval to undertake the studies was obtained from three sources: community representatives via the Durri Aboriginal Medical Service Board of Management; the Human Research Ethics Committee of The University of Newcastle (HREC Approval No: H-455-11102); and on an individual basis from participating members.
The development of the musculoskeletal screening survey
Design: Four stages were used to develop and test a screening survey in a community of Indigenous people from rural NSW. The first included a search of the literature to examine existing surveys for screening these conditions. The second stage involved consulting key-informants to ensure cultural acceptability and utility of the measurement instrument in the community. Third, a standardised clinical examination utilising clinically accepted protocols, conducted by registered chiropractors, was used to measure correlation with the AHW-administered survey. Fourth, the screening survey was pilot tested to determine its efficacy and effectiveness.
Stage I: Literature search A literature search was conducted to specifically identify potential measurement instruments that could be used as screening surveys and assessments. The primary search strategy included MEDLINE, Pubmed, ABI, Sociofile, Core Biomed, and Nursing Collection for the period January 1980 to July 2000. Only journals written in English were accessed. Key words used in the search included: surveys; prevalence; pain; musculoskeletal conditions; Australian; Indigenous. Bibliographies of papers were examined for other key papers, and direct contact was made with selected researchers in musculoskeletal health.
Stage II: Key-informant discussions for cultural acceptability and applicability of the screening survey The first screening survey, known as the Community Survey of Muscle Joint and Bone Conditions (CSMJBC) was modelled on the survey used by the Community Oriented Programme for the Control of the Rheumatic Diseases (COPCORD). The COPCORD instrument has been used in rural communities throughout the world4. The CSMJBC was then reviewed through key-informant groups. Formulating these key-informant groups involved a process of obtaining informed opinion from members of the community with a close understanding of the community as a whole, or particular aspects of interest5. Group discussions were conducted among AHWs and health professionals involved with the participating Aboriginal Medical Service (AMS). The groups consisted of 10 AHWs, one medical practitioner and one physiotherapist. Each key-informant discussion group was divided into subsets of three to four people.
The aim of the key-informant discussion groups was explained verbally and members of the groups were given copies of the developed survey for review and asked to provide general (verbal) and independent (written) comments in relation to: the clarity of questions; cultural sensitivities; the content and presentation of the survey; and the logistics of completing a survey of this kind. The ultimate instrument was titled the Revised Kempsey Survey (RKS).
Stage III: Piloting of the Revised Kempsey Survey (RKS) To further evaluate the clarity, cultural appropriateness and the delivery logistics of the proposed survey instrument, a pilot project was conducted at the AMS with a convenience sample of 17 community members.
The cross-section of participants included AHWs, employees of the AMS and patients in attendance at the AMS at the time of conducting the pilot study. Community members were asked to participate in the pilot study by the appointed AHW who contacted them in person or via the telephone. An attempt was made to select male and female participants in each of the following age groups: 15-24; 25-34; 35-44; 45-54; 55-64; and >65.
Fifteen minutes were allocated for the AHW to conduct the screening survey and 30 min for the researcher, an experienced chiropractor, to complete the clinical assessment (which included a history and regional examination of painful anatomical sites). The screening survey was immediately followed up by the clinical assessment; the researcher performed the clinical assessment blinded to the outcome of the survey.
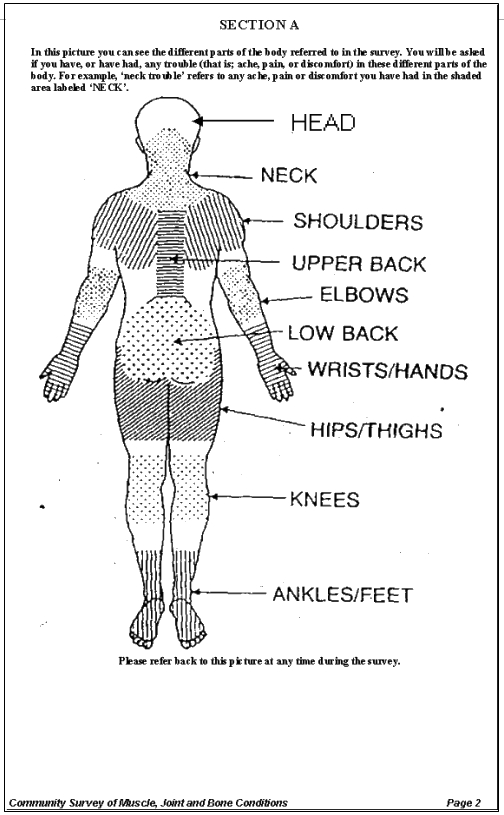
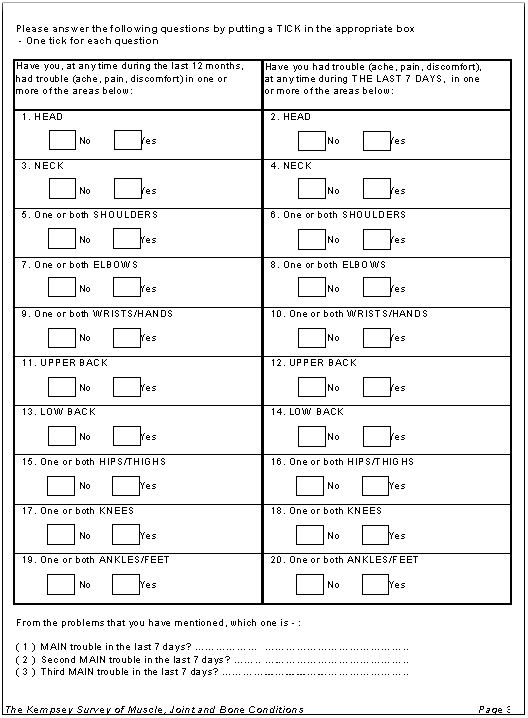
The Survey Section A of the ultimate RKS survey (Appendix 1) consisted of a diagram which delineated the body sites and allowed respondents to comment on any present or past symptoms such as 'aches, pains or discomfort' experienced in the last 7 days and/or the last 12 months. Section B attempted to measure pain and disability 'on average'. A positive pain finding in the survey was noted by AHWs ticking a box that indicated one of the 10 anatomical sites of pain as expressed by participants.
Clinical assessment The clinical assessment consisted of both a musculoskeletal history and a clinical examination (based on the standard clinical assessment procedures used in an undergraduate chiropractic programme at Royal Melbourne Institute of Technology (RMIT) University, Victoria, Australia6).
A positive pain finding in the clinical assessment was derived by practitioner-based examination, including the patient's history of involved site(s), followed by standard orthopaedic and range-of-motion tests to localise sites of pain and restricted movement. A negative pain finding was indicated by the absence of reported pain and/or restricted orthopaedic and range-of-motion findings, as examined by the practitioner. The history component sought further information related to any condition(s) experienced in the last 7 days. In particular, probable causes of symptoms, past history, initial episode(s) of symptoms, duration of symptom(s), 'average' severity of symptoms, and any associated limitation of daily activities, social routine and work activities, the type of treatment received, and any barriers to receiving treatment were sought. Because of time limitations, only the top three most painful conditions could be clinically assessed.
Stage IV: independent comparison of the RKS findings with the clinical assessment Participants in the survey and clinical examination were selected from an estimated Indigenous population of 600 in Kempsey, NSW. The minimum age was set at 15 years. For those aged between 15 and 16 years, permission to perform an assessment was first obtained from the parent or guardian. Fifteen years was chosen as the cut-off age to allow for comparisons with the COPCORD studies that assessed people from this age group onwards as part of their protocol4. Indigenous participants were selected at random using a sampling procedure drawn from a previously conducted Indigenous census which stratified for age and sex7.
In this census, AHWs were employed to perform a door-to-door survey to accurately determine the occupancy of Aboriginal residents within the community. Approximately 550 community members (aged 15 years and over) were identified as Aboriginal according to the definition of the Department of Aboriginal Affairs that 'an Aboriginal person is one who is of Aboriginal descent and both personally identifies himself/herself as Aboriginal and is accepted as an Aboriginal person by his/her community'8. A proportional allocation of the various age groups was ultimately necessary to accommodate the smaller number of Elders in the population7.
The study sample was grouped according to 10-year age brackets. The proportions (%) of those in each age group were used to obtain the sample sizes required in each age category. Random numbers, generated by computer, were then assigned to the remaining census names to determine the final sampling list. This procedure was designed to provide a representative sample that allowed for the smaller proportion of older people in the community9. The sample was compared with the community census conducted by the Kempsey Shire10. The results of the Indigenous census compared favourably with the Kempsey Community Profile10.
Participants screened by the AHW-administered survey subsequently underwent a clinical examination conducted by four chiropractors previously trained and assessed in standardised, clinical assessment procedures according to a procedural manual which outlined the cultural considerations and logistical processes required by researchers. The content of the procedural manual was revised in a two-hour workshop for participating researchers to clarify study requirements6. The examination was based on accepted clinical parameters for conducting musculoskeletal conditions and included the domains of assessment used by the teaching institutions. Thus, attempts were made to fulfil content and face validity requirements.
Four senior chiropractic educators (two from each of the two principal chiropractic teaching institutions, RMIT University and Macquarie University, NSW, Australia) were also consulted to determine what current clinical assessment procedures were available and suitable for use in conducting musculoskeletal clinical assessments. The primary variables measured in this study included participants' levels of pain and any limitations imposed by musculoskeletal pain.
Although some authors argue that a 'gold standard' does not exist in many areas of musculoskeletal practice11, standard clinical assessments (including a patient history and examination) performed by musculoskeletal health professionals, have been reported as the best available tools for measuring painful and limited ranges of motion and giving a provisional diagnosis12.
The four chiropractors, blinded to the findings in the screening survey, performed a history (including the subjects' experience of pain during the last 7 days) and musculoskeletal assessment (including palpation, range of motion, orthopaedic and neurological tests) to independently report levels of pain, disability and associated risk factors. These independent findings allowed the survey and clinical assessment findings to be compared. Because of logistical limitations, inter-rater reliability measures for consistent clinical assessment outcomes were not performed in this study but are likely to improve the rigour of future investigations.
Analyses
The most painful musculoskeletal condition identified by AHWs in the RKS was compared with the most painful musculoskeletal condition as identified by the chiropractors. In the RKS, overall pain was measured using a 10 point Likert scale, and the results were categorised thus: 0 = no pain, 1-3 = slight pain, 4-6 = moderate pain, 7-10 = severe pain.
In the clinical assessment overall pain was measured using a categorical scale and the results grouped: 0 = no pain, 1-3 = slight pain, 4-6 = moderate pain, 7-10 = severe pain.
The objective was to see if the clinical assessment diagnosis correlated with the RKS performed by the AHWs.
The 7 day prevalence findings in the screening survey (RKS), performed by AHWs, were compared with the notional gold standard (history and clinical findings performed by chiropractors) to determine the sensitivity and specificity of the screening survey13. Kappa scores were calculated to measure the levels of agreement between the Chiropractors' assessment and the survey administered by AHWs.
Results
Subjects
The clinical assessment was conducted on 189 participants comprising 87 males (46%) and 102 females (53%). Participants' mean age was 44 years (±14.8). The findings of this study have been previously reported in detail2.
Stage I: The literature search
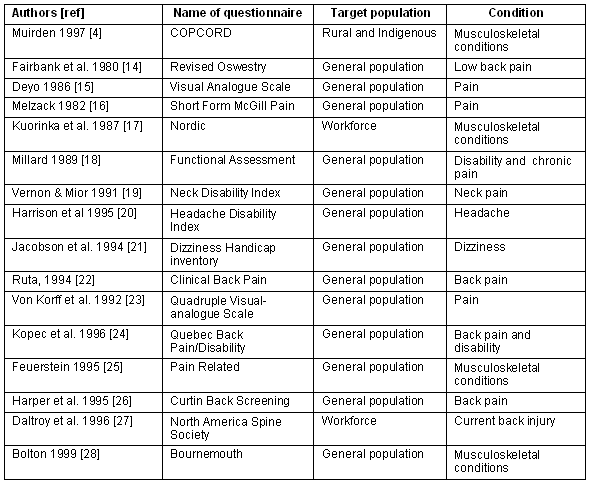
The literature search for validated surveys are summarised (Table 1). Sixteen validated surveys were identified for assessing musculoskeletal conditions. Three of these assessed musculoskeletal conditions in general, and one had been specifically designed to assess musculoskeletal conditions among rural and Indigenous communities4.
Table 1: Previous musculoskeletal screening surveys (1980-2003)
Stage II: The development of the survey instrument using key informant discussions
Key participants generally agreed that the proposed survey needed to be significantly reduced in length and the language simplified. The key informants decided that the original Community Oriented Programme for the Prevention of the Rheumatic Diseases (COPCORD) survey was not suitable and, therefore, it was not used in the study, although some of its components were retained.
Instead, a modified survey, the RKS, was subsequently designed based on CSMJBC and other musculoskeletal screening surveys17,28. Included were questions that were concise yet simple in accordance with the suggestions of the key-informant groups. These groups felt that the new survey achieved clarity in its questions, cultural appropriateness, covered all relevant content, was clearly presented and was logistically feasible. The RKS is shown in Appendix I.
Stage III: The pilot study
The pilot study was conducted between January 2001 and July 2002 in the Kempsey district of NSW. The primary suggestions of key informants who undertook the pilot study were to substantially reduce the length of the survey and to prioritise the top three conditions of pain. Beyond these suggestions, verbal and written feedback by participants described the final version of the RKS as clear, culturally acceptable, sufficiently comprehensive in content and logistically feasible to implement in the community.
Stage IV: Independent comparison of the RKS findings with the clinical assessment
Results from the screening survey showed that the areas of the body with the highest prevalence of musculoskeletal problems reported in the previous 7 days were the lower back, neck, head and shoulders. The results appear in Table 2. A significant correlation was obtained between the most prevalent musculoskeletal condition as assessed by the AHWs and the chiropractors (0.896). A significant correlation was also obtained between the overall pain as assessed by the AHWs and chiropractors (0.350).
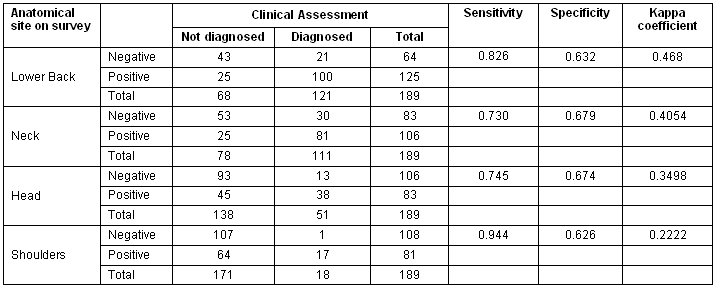
Table 2: Sensitivity and specificity of the Revised Kempsey Survey (n = 189)
Sensitivity and specificity of the RKS survey
The mean sensitivity of the RKS was 81% for lower back, head, neck and shoulder pain.
The mean specificity was 65% for lower back, head, neck and shoulder pain. Table 2 outlines the sensitivity and specificity for each anatomical site. According to these findings, it appears that the RKS is a very useful tool for detecting those who have musculoskeletal conditions, with a sensitivity above 70%. It also has reasonably high specificity (above 60%) for ruling out those who do not have the musculoskeletal condition.
For the screening survey, 83% of all the participants reporting lower back pain were positive for lower back pain and 73% were positive for neck pain. For the survey, 74% of all the participants with head pain were positive for head pain and 94% of all the participants with shoulder pain in the RKS were positive for this condition in the clinical assessment. Instruments that have a high specificity are clinically useful in ruling out disease. This means that a negative result is very likely to exclude the possibility of a participant having the musculoskeletal condition of interest.
Assessing the RKS against the gold standard (chiropractor assessment)
Kappa scores are seen in Table 2. As all Kappa scores were higher than 20%, it can be concluded that the RKS achieved a moderate level of agreement when compared with the notional gold standard29.
Discussion
The Kempsey survey was designed for screening musculoskeletal conditions in rural Indigenous communities. The survey appeared to satisfy criteria of face and content validity, clarity, cultural appropriateness and logistical feasibility. A significant correlation was obtained between the most prevalent musculoskeletal condition (lower back pain) and between overall pain as assessed by AHWs and chiropractors. It also achieved high sensitivity in detecting musculoskeletal conditions when compared with other validated screening procedures for musculoskeletal conditions28 and a moderate level of agreement with the gold standard clinical assessment28-30.
Table 2 shows a comparison of the musculoskeletal prevalence findings of the survey and identifies the conditions independently diagnosed via the clinical assessment components of the study. Sensitivity and specificity of the RKS were assessed at each body site.
When compared with the clinical assessment, the screening survey correctly identified 94% of shoulder conditions, 83% of lower back pain, 74% head pain and 73% of neck conditions.
The discrepancies may, in part, be due to the difficulty AHWs experienced in identifying conditions which are more readily identified via palpation and measuring limited and/or painful ranges of joint motion. Comparing a culturally relevant screening instrument with a more traditional clinical model may be flawed.
Another weakness was the use of 7 day prevalence instead of point prevalence as the comparison variable with the clinical assessment. It is possible that a subject may have had pain in the preceding 7-days but not at the time of clinical assessment.
The problem with under-diagnosing via the screening process is that those with conditions that are amenable to treatment or management may not receive the care that they require.
Incorporating basic clinical skills as part of the musculoskeletal assessment administered by AHWs may help to localise painful anatomical sites to improve the sensitivity and specificity of this measure within a culturally sensitive framework.
The screening survey allows AHWs to provide prevalence estimates of musculoskeletal conditions, their associated risk factors and barriers to managing these conditions in their communities as a step towards developing effective community-based interventions. A simple to administer, sensitive measure is crucial in this context, given the importance of identifying those in the community with a potentially painful and disabling musculoskeletal condition. The development of this measure demonstrated the successful implementation of a measure with community ownership and participation. It has the potential to be adapted and delivered in other rural Indigenous communities.
Though a clinical assessment as conducted by a musculoskeletal health professional in this setting provides a comprehensive examination tool, it is also more likely to be more time consuming and costly and may not be the most culturally sensitive procedure if conducted by non-Indigenous personnel.
Long-term validation of the screening survey is a topic worthy of further research but impractical given the often transient nature of Aboriginal people living in rural communities31.
Other worthwhile research questions include whether the process of involving AHWs and other members of the community in the development and implementation of the screening survey promote community satisfaction and, importantly, if screening those with musculoskeletal conditions improves the health outcomes of the community.
Screening surveys of this kind may be of benefit in providing efficient, cost-effective and culturally sensitive tools in the measurement of other causes of morbidity and mortality in Aboriginal communities (including asthma, nutrition and physical activity) as precursors to implementing health promotion initiatives - another topic worthy of further investigation.
References
1. Pacza T, Steele L, Tennant M. Development of oral health training for rural and remote Aboriginal health workers. Australian Journal of Rural Health 2001; 9: 105-110.
2. Vindigni D, Parkinson L. Blunden s, Da Costa C. Perkins J. Prevalence of musculoskeletal conditions, associated pain and disability and the barriers to managing these conditions in a rural, Australian Aboriginal community. Rural and Remote Health 4: 230. (Online) 2004. Available: http://rrh@deakin.edu.au (Accessed 27 February 2006).
3. Steele L, Pacza T, Tennant M. Rural and remote oral healthy, problems and models for improvement: A Western Australian perspective. Australian Journal of Rural Health 2000; 8: 22-28.
4. Muirden KD. The origins, evolution and future of COPCORD. APLAR Journal of Rheumatology 1997; 1: 44-48.
5. Key Informant Groups. Program Planning and Assessment, University of Illinois extension. Key informant interviews. (Online) no date. Available: http://www.aces.uiuc.edu/~PPA/KeyInform.htm (Accessed: 11 January 2006).
6. Royal Melbourne Institute of Technology. History and clinical assessment proforma for 4th and 5th year student preceptorship. Melbourne, VIC: School of Chiropractic, RMIT, 1999.
7. Perkins J, Rochow K, Welsh K. A door-to-door survey to ascertain the occupancy of Aboriginal residents within the Kempsey study boundaries. A collaborative venture between the Durri Aboriginal Corporation Medical Service and the School of Medical Practice and Population Health. Newcastle, NSW: School of Medical Practice and Population Health, Faculty of Health, The University of Newcastle, 2000.
8. Department of Aboriginal Affairs Constitutional Section. Report on a review of the administration of the working definition of Aboriginal and Torres Strait Islander. Canberra, ACT: Department of Aboriginal Affairs, 1981.
9. Sekaran U. Research methods for business, 3rd edn. New York: John Wiley & Sons, 2000.
10. Kempsey Shire Council. Community profile 2000. Kempsey Local Government Area. West Kempsey, NSW: Kempsey Shire Council, 2000; 7.
11. Beruskens AJ, de Vet HC, Koke AJ, van der Heijden GJ, Knipschild PG. Measuring the functional status of patients with low back pain. Assessment of their quality of disease-specific questionnaires. Spine 1995; 20: 1017-1028.
12. Haldeman S, Chapman-Smith D, Petersen DM (Eds). Guidelines for chiropractic quality assurance and practice parameters (Mercy Guidelines). Burlingame, CA: Congress of Chiropractic State Associations, 1992.
13. Bioanath. Sensitivity and specificity. (Online) 2004. Available: http://www.bioanth.org/ANTH147/screening.htm (Accessed: 11 January 2006).
14. Fairbank JC, Couper J, Davies JB, O'Brien JP. The Oswestry low back pain disability questionnaire. Physiotherapy 1980; 66: 271-273.
15. Deyo RA. Comparative validity of the sickness impact profile and shorter scales for functional assessment in low-back pain. Spine 1986; 11: 951-954.
16. Melzack P. Pain measurement and assessment. New York, NY; Raven, 1982.
17. Kuorinka I, Jonsson B, Kilbom A et al. Standardised Nordic questionnaires for the analysis of musculoskeletal symptoms. Applied Ergonomics 1987; 18: 233-237.
18. Millard RW. The Functional Assessment Screening Questionnaire: application for evaluating pain-related disability. Archives of Physical Medical Rehabilitation 1989; 70: 303-307.
19. Vernon H, Mior S. The Neck Disability Index: a study of reliability and validity. Journal of Manipulative Physiology and Therapy 1991; 14: 409-415.
20. Harrison E, Quinney H, Magee D, Sheppard MS, McQuarrie A. Analysis of outcome measures used in the study of patellofemoral pain syndrome. Physiotherapy Canada 1995; 47: 264-272.
21. Jacobson GP, Ramadan NM, Aggarwal SK, Newman CW. The Henry Ford Hospital Headache Disability Inventory (HDI). Neurology 1994; 44: 837-842.
22. Ruta DA, Garratt AM, Wardlaw D, Russell IT. Developing a valid and reliable measure of health outcome for patients with low back pain. Spine 1994; 19: 1887-1896.
23. Von Korff M, Ormel J, Keefe FJ, Dworkin SF. Grading the severity of chronic pain. Pain 1992; 50: 133-149.
24. Kopec JA, Esdaile JM, Abrahamowicz M et al. The Quebec Back Pain Disability Scale: conceptualization and development. Journal of Clinical Epidemiology 1996; 49: 151-161.
25. Feuerstein M. Multidisciplinary rehabilitation of occupational musculoskeletal disorders: rationale, assessment strategies and clinical interventions. LACC Post-graduate program notes, session 1 of the 2nd 100 hours course, class notes. Chicago: LACC Postgraduate Division, 1995.
26. Harper AC, Harper DA, Lambert LJ. Development and validation of the Curtin Back Screening Questionnaire (CBSQ): a discriminative disability measure. Pain 1995; 60: 73-81.
27. Daltroy LH, Cats-Baril WL, Katz JN, Fossel AH, Liang MH. The North American spine society lumbar spine outcome assessment Instrument: reliability and validity tests. Spine 1996; 21: 741-749.
28. Bolton JE. Accuracy of recall of usual pain intensity in back pain patients. Pain 1999; 83: 533-539.
29. Jekel JF, Elmore JG, Katz DL. Epidemiology, biostatistics and preventive medicine. Philadelphia, PA: WB Saunders, 1996.
30. Bolton JE, Breen AC. The Bournemouth Questionnaire: a short-form comprehensive outcome measure. I. Psychometric properties in back pain patients. Journal of Manipulative Physiology and Therapy 1999; 22: 503-510.
31. Burden J. Health: An holistic approach. In: C Bourke, E Bourke, E Edwards (Eds). Aboriginal Australia. An introductory reader in Aboriginal studies, 2nd edn. Brisbane, QLD: University of Quensland Press, 2003; Chapter 10.