Introduction
At first glance, the list of challenges facing remote and rural communities appears much the same as 20 years ago. Access continues to be the major rural health issue with most resources concentrated in urban areas, along with widespread transport and communication difficulties and shortages of healthcare providers. On closer inspection, however, although the themes may be the same, much of the content is remarkably different. The purpose of this article is to reflect on the development and achievements of the Wonca Working Party on Rural Practice (WWPRP) following its inception in 1992 until 2012 as it has focused internationally on rural health and practice and led debate around issues in rural health care globally over the past 20 years.
There have been significant achievements in rural health care in a number of countries, but many areas remain untouched despite growing recognition of the importance of this issue. The authors believe that looking back will encourage others to look forward and to take up the challenge, so that the vision of health for all rural people may be attained.
The early years: policies, conferences and declarations
The WWPRP arose during the world family doctors conference held in Vancouver in 1992, when a conversation between a couple of rural doctors around their posters led to a meeting of practising rural doctors from developed and developing countries. A small core group started interacting internationally through teleconferences, and the working party on rural practice was born, with a vision of addressing the need for health care of all rural people.
The group was recognised formally as a working party by Wonca, the World Organization of Family Doctors, in 1995, at the Wonca Council meeting in Hong Kong, and Dr Roger Strasser from Australia was confirmed as the first chairperson. However, the working party had already been living up to its name - it had been hard at work and presented to the Wonca Council its first policy document, which was adopted as the Wonca policy on training for rural general practice1. The policy stated that 'there is an urgent need to implement strategies to improve rural health services around the world. This will require sufficient numbers of skilled rural family doctors to provide the necessary services.' In support of this, Wonca adopted a set of recommendations proposed by the group, which specifically listed the following:
- increasing the number of medical students recruited from rural areas
- substantial exposure to rural practice in the medical undergraduate curriculum
- specific flexible, integrated and coordinated rural practice vocational training programs
- specific tailored continuing education and professional development programs which meet the identified needs of rural family physicians
- appropriate academic positions, professional development and financial support for rural doctor-teachers to encourage rural research and education.
All of these recommendations were adopted in international documents and articles in the years that followed. However, the focus at this stage was specifically on rural medical practitioners, and family physicians in particular.
The First Wonca International Conference on Rural Medicine was held in 1996 in China. This landmark conference, the first in an ongoing series of gatherings (Table 1), combined a 3-day conference in Shanghai city with 3 days of visiting health centres, hospitals and traditional medical schools in rural Fengxian. Three hundred rural physicians and academics attended from 28 countries. The deliberations of the many workshops and group discussions were condensed into a resolution that was adopted at the final plenary session. One of the enduring memories was the remarkable sense of camaraderie amongst conference participants as they realised that, despite the great differences between developed and developing countries, many of the issues of concern in rural practice and rural health services are the same worldwide.
The Shanghai conference was significant in that it started a movement of rural doctors2, which has continued to grow, with developing relationships across countries based on shared experiences that, despite the differing contexts and resources, were and are remarkably similar. Those shared challenges include problems of access and equity, shortages of health professionals, the need to work in integrated teams, and the development of generalist practitioners while maintaining advanced procedural skills in isolated environments. Despite the close bonds and support that physicians build with their own communities, they often have distant and difficult relationships with established medical organisations and professional bodies. Discussions took place at the conference about the possible formation of a world organisation of rural doctors (WORD) but this never gained strong traction, perhaps because the WWPRP drew members from across the globe (Table 2).
At this time, the WWPRP began to appreciate the potential benefits that information technology could bring to rural practice and a subcommittee was established, known as the Wonca Rural Information Technology Exchange (WRITE). WRITE's policy statement Using information technology to improve rural health care3 was adopted by the WWPRP and endorsed later by Wonca Council. The document was based on the premise that low-level and relatively low cost technologies have the potential to offer access to useful telehealth services for many rural communities, yet they mostly had little say in the design and development of these, and it sought to provide participants, funders and planners of rural health services with guidelines for the introduction of telehealth services to rural communities. While setting out critical steps for the implementation of telehealth services, it also argued that telehealth should never be intended to replace local health services delivered by rural health workers to their community at the local level.
The next conference was held in Durban, South Africa, in September 1997. The conference was billed as the second World Rural Health Congress, dropping medicine from the title and shifting the emphasis to health and the wellbeing of rural people and communities. The Durban congress is significant in that it adopted the Durban Declaration, Health for all rural people, which was in essence a statement of intent that has guided the working party since then. It proposed a global initiative for the advancement of the health of the world's rural people. It outlined a series of principles and a Call for Action, renewing the Health for All initiatives and calling on WHO, UNICEF, the World Bank and national governments to work with local communities and health professionals. The Declaration called for a combined effort to redress the historical inequities facing rural and disadvantaged communities.
The third World Conference on Rural Health followed in July 1999 in Kuching, Malaysia. This sought to take forward the need for action and produced An action framework for the conference participants and the Wonca working party on rural practice, under the title of 'Emerging issues and initiatives'. This covered sustainable models for rural health services, investment in rural health, women's issues, telehealth, a rural health research agenda, education and training, compulsory rural service and the health of indigenous peoples. The latter was given particular prominence with the adoption by the conference of the Kuching statement on the health of indigenous peoples4, which noted with concern that in many countries the health status of indigenous peoples, who commonly reside in rural areas, is significantly worse than that of the population as a whole, and that they largely represent the most marginalised and poorest populations of the world. It affirmed the rights of indigenous people, and called for indigenous people to be involved in efforts to improve their health status and to be trained as health professionals at the same time as calling for health professionals to play an advocacy role in this regard.
In August 2000, Calgary, Canada, provided the venue for the fourth World Rural Health Conference. In addition to continued work on developing a policy for rural practice, the conference highlighted the role of female physicians in rural practice, and adopted the Calgary commitment to women in rural family medical practice5. This recognised the essential contribution that women in rural practice have made to the health of their communities. It called for the development of a policy document, and subsequently, in 2003, the Policy on female family physicians in rural practice6 was adopted by the working party and endorsed by Wonca. This had three key objectives, which were to support women working in rural and remote family medical practice, to increase the number of female doctors working in such practices, and to ensure that female doctors from these contexts have equitable input into the development of policy and programs affecting the rural medical workforce.
Through these years there was a sustained effort by the WWPRP to develop a broader policy document to underpin its efforts. The Policy on rural practice and rural health7 was initially produced in 1998, essentially derived from the recommendations of the first two conferences, and was endorsed by the Wonca executive in Kuching in 1999. It underwent another reiteration in Calgary and a revised document was adopted by the WWPRP, and subsequently endorsed by Wonca Council in 2001.
The Policy on rural practice and rural health contains strategies to assist governments and professional bodies to ensure that real progress is made toward the goal of improving the health of rural people. Key recommendations included that:
- rural practice should be incorporated by medical schools and medical schools should take responsibility to educate appropriately skilled doctors to meet the needs of their geographic region, including underserved areas
- specific continuing medical education should be developed for rural practitioners
- strategies should be implemented to support recruitment and retention of doctors in rural practice
- the unique needs of rural communities should be met through primary care, flexible health service delivery, multidisciplinary teamwork and the use of information technology
- the state must recognise its pressing responsibility for ensuring equitable access to health care in rural areas by developing a framework for rural health care and supporting research in the field.
The policy endeavoured to take into account the interests and contributions of all health workers, recognising that health workers must work together in multidisciplinary and multiskilled teams. While many of these issues are now very familiar to everyone involved in rural healthcare service, education or research, they were not widely accepted at the time.
Table 1: The Wonca World Rural Health Conferences, 1996-2012
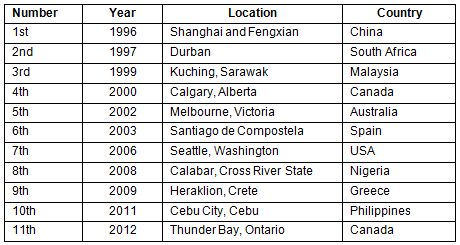
Table 2: Country of origin of members of the Wonca Working Party
on Rural Practice, 1992-2012 (in alphabetical order)
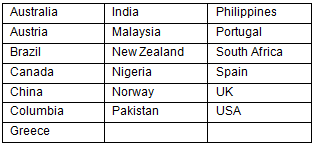

Figure 1: At the third conference in Sarawak in 1999, (from L to R) Dr John Wynn-Jones (Wales),
the late Dr MK Rajakumar (host organiser, Malaysia), Dr Roger Strasser (Chair, WWPRP, Australia), Dr Jim Rourke (Canada), the late
Dr John McLeod (Scotland).
The middle years: engaging with WHO
The WWPRP had recognised that if it was going to make any impact on rural heath globally it needed to work with WHO. A series of meetings and ongoing discussions with WHO led in May 2002 to a WHO-Wonca co-sponsored invitational conference, entitled Health for All Rural People, which was held in Traralgon, Victoria, Australia. The conference brought together the working party, WHO officials, key representatives from targeted countries faced with major rural health issues and health policy experts. Guiding principles for the meeting included the need for equitable distribution of health resources and investment, the use of a systems approach for more efficient and effective solutions, policy planning and service delivery, a community- and people-centred approach and the building of capacity through integrated team work.
The conference produced the Health for All Rural People (HARP) action plan8, built on three key pillars:
- action for equity
- action for a rural paradigm
- a local action process.
The latter was seen to include community empowerment, building unity and social capital, providing rural health care, action-oriented research, and the education of health professionals. It was intended that the HARP action plan would be adopted by Wonca and WHO, but sadly only the former adopted it, due to changes and restructuring at WHO. While elements of the document were used, the WWPRP eventually accepted that the WHO was not going to publish the plan, and instead engaged WHO in other ways.
Immediately following the invitational meeting, the fifth World Rural Health Conference was held in Melbourne. This adopted the Melbourne manifesto: a code of practice for international recruitment of health care professionals9, which sought to address the international migration of rural doctors from developing countries to higher income countries. This was one of the first international guidelines on ethical recruitment and became a standard. It was premised on the idea that, while individuals should have the absolute right to move freely according to their personal needs, richer countries should not be recruiting actively from poorer countries10. It also proposed the payment of compensation in instances where this did occur. At the same time the conference promoted international exchanges for learning and development. The conference also adopted both the Policy on female family physicians in rural practice11, mentioned above, and the Policy on quality and effectiveness of rural health care12, which sought to provide a framework to encourage the development of direct and indirect targets for and measures of the quality and effectiveness of rural health care.
The sixth World Rural Health Conference was held in Santiago de Compostela, Spain, in September 2003, the first such conference in Europe. This conference has become a talking point in the working party because the convenor was adamant that there would not be any conference resolutions and instead multiple Santiago statements were adopted at the end of the conference. They provided updates on many previous statements and policies, and also covered the new issues of child labour, HIV-AIDS, and rural health research.
Dr Jim Rourke from Canada was elected to succeed Roger Strasser as the chair of the working party at the 2004 Wonca Global Conference in Orlando, Florida. The pattern for the world rural health conferences had now been set: in each of the two intervening years between the triennial global family doctor conferences, the working party would plan to hold conferences, hosted by local organisations in different countries and continents, on a rotational basis based on proposals submitted to the working party. However, in 2005 there was no conference. Attempts had been made for some time to work more closely with the International Association of Agricultural Medicine and Rural Health (IAAMRH) and the working party accepted an invitation to join their international conference in Japan that year. Unfortunately, the efforts to collaborate with IAAMRH within the conference and subsequently were not as productive as hoped, leading to greater caution amongst WWPRP members going forward.
The seventh World Rural Health Conference, with a focus on education, was held in 2006 in Seattle, USA, the home base for the University of Washington's Washington, Wyoming, Alaska, Montana, Idaho (WWAMI) program. This conference did not produce any formal statement but was significant because it established a pattern for future conferences with a very successful post-conference meeting in Alaska, where delegates had time to relax and share ideas while visiting local health services and doctors. During the Alaska meeting a new strategic plan was adopted for the working party going forward, with its mission being 'Rural doctors REACHing towards rural health in partnership with like-minded groups', the REACH referring to the key objectives of 'repositioning and relationship', 'education', 'activism', 'conferencing and communication', and the Health for All Rural People vision.

Figure 2: A full house - attendees at the Wonca Working Party
on Rural Practice meeting in Traralgon, Victoria, Australia, in 2002.
Recent years: global focus on health human resources
In 2007, at the global family doctor conference in Singapore, Dr Ian Couper from South Africa was elected as the new chair of the working party, and received the symbolic stag horn gavel, which was donated by the late founding member of the WWPRP, Scotland's Dr John Macleod. Arising from the Seattle meeting, it was agreed to work towards developing an international guidebook on rural medical education, with Dr Bruce Chater from Australia as editor.
This was followed by the eighth World Rural Health Conference in Calabar, Cross River State, Nigeria, in February 2008. Although the international delegation at this conference was smaller than normal, there was a large and enthusiastic West African contingent. The conference highlighted the importance of the working party looking at how the conferences can impact on local initiatives and it helped to further the development of a family medicine department at the University of Calabar. One day of the conference was held at a rural health centre - providing some logistical challenges - and the leadership of the working party were inducted as honorary chiefs by the local Okoyong community in recognition of the efforts of the working party in furthering rural health care generally and in bringing the conference to the region in particular. This meeting also endorsed efforts by Dr John Wynn-Jones from Wales to involve rural doctors in the WHO-initiated process to develop guidelines on increasing access to health workers in remote and rural areas, in which a number of members of the working party subsequently became engaged. This drew on the growing evidence base to which members of the working party had contributed13.
The ninth World Rural Health Conference in Heraklion, Crete, held in June 2009, was preceded by a 1-day workshop to map out contributions to and contents for the guidebook on rural medical education. During the conference, very positive meetings and a combined workshop took place with members of the WHO Department of Human Resources for Health. The subsequent launch of the WHO global recommendations, which the working party supported enthusiastically, was hosted by the University of the Witwatersrand Centre for Rural Health in Johannesburg, of which the working party chair was director. This document, Increasing access to health workers in remote and rural areas through improved retention: global policy recommendations14,15, was a significant milestone in global efforts to put rural health issues on the table, representing the first time that WHO has taken such issues seriously at an international level and including many of the ideas and strategies that were contained in the working party policy documents and statements over the years.
At the Crete conference, discussions were held and agreement was reached with the International Commission on Occupational Health (ICOH) Scientific Committee on Rural Health on collaboration going forward. Specifically, the parties agreed to support each other in the mutual aspirations of improving the health and wellbeing of rural people and their communities, and in highlighting issues associated with occupational health and disease in agriculture, forestry, fishing and associated rural occupations at all levels including government, planners, educational institutions, professional bodies and individual practitioners. This was ratified in a memorandum of understanding signed between the two committees in 2010.
At the global family doctors conference in Cancun, Mexico, in 2010, the working party endorsed the journal Rural and Remote Health (http://www.rrh.org.au) as the international journal of rural health policy, practice, research and education. It also agreed to establish the John Macleod Oration in memory of this iconic champion of rural practice (who died soon after the Crete conference), to be delivered at future world rural health conferences.
In 2011, the 10th World Rural Health Conference was held in Cebu, Philippines, as a joint conference with the 18th Wonca Asia Pacific regional conference and the Philippine Academy of Family Physicians golden anniversary celebration. There were many lessons learnt from holding a joint conference, in particular the need for a clear identity and dedicated programming that would appeal to rural doctors globally, as well as influencing the ethos of the conference. There was a review of progress on the Melbourne Manifesto, leading to the adoption of the five Cebu Strategies16, which were to develop measurable indicators for the Melbourne Manifesto (score card), promote social accountability of medical education, provide support for healthcare professionals and education programs, engage with recruiting organisations and market the manifesto.
The 11th World Rural Health Conference, held in Thunder Bay, Ontario, Canada, was another joint conference, known as Rendez-Vous 2012; this brought together the Wonca Working Party, the Network: Towards Unity for Health (TUFH), the Training for Health Equity Network (THEnet), the Consortium for Longitudinal Integrated Clerkships (CLIC) and the series of meetings on community-engaged medical education arranged by Finders University and the Northern Ontario School of Medicine. The focus was on community participation in health professional education, research and service. Despite different conference and organisational cultures, the common commitment of the different groups to address the needs of underserved people, particularly through health professions education, made for an exciting meeting. The Thunder Bay Communique: new ways of thinking17 adopted by the conference is a visionary document regarding the way forward for community participation in education, research and service.

Figure 3: Pictured after their investiture as honorary chiefs by the Okoyong community, near Calabar, Nigeria,
during the eighth conference (from L to R), Dr Roger Strasser (Canada), Dr Ndifreke Udonwa (host organiser, Nigeria),
Dr Ian Couper (chair, Wonca Working Party on Rural Practice, South Africa), Dr Victor Inem (Nigeria) and Dr Bruce Chater (Australia).
This has become an iconic image for the WWPRP - hardly a conference goes by without this being shown at least once!

Figure 4: At the Rendez-vous 2012 conference, Dr Ian Couper presented the inaugural John McLeod Oration,
in memory of the late founding member and doyen of the Wonca Working Party on Rural Practice;
he was presented with a certificate to commemorate this by Mrs Lorna McLeod (John's widow, centre)
and Mr Alistair McLeod (John's son, behind). Tributes to John were offered by Dr John Wynn-Jones (far left),
who chaired the session, and Dr Sarah Chalmers (far right).
The current context
The working party has focused on themes and policies that address the right of rural and remote communities to high quality health care, the need for specifically trained and skilled rural doctors (male and female) from diverse ethnic backgrounds to deliver this health care, the importance of strategies to recruit and retain rural health professionals at a national level while addressing international migration, and the development of information technology to facilitate optimal healthcare solutions.
Recent international trends have the potential to facilitate progress in relation to these issues. The growing movement in global medical education to bring about both a scaling up and transformation of health professional training, so that there are sufficient, relevant, appropriately trained health workers available in and for every nation18,19, is an important development that needs to be embraced, because of the potential it has to enhance efforts to address rural healthcare needs. Alongside this, there is increasing focus on social accountability in medical education20, in terms of which medical schools are challenged to take greater responsibility for the health needs of a geographical area, exemplified in the Global consensus on social accountability in medical education21. This highlights the importance of rural medical schools with innovative curricula, that are designed specifically to meet the needs of rural areas, such as Memorial University of Newfoundland and the Northern Ontario School of Medicine in Canada, James Cook University School of Medicine in Australia, Ateneo de Zamboanga School of Medicine and the University of Philippines School of Health Sciences, Leyte, in the Philippines, and Walter Sisulu University Medical School in South Africa22,23.
Outside of the educational arena, greater attention has been given to equity as a fundamental principle in the provision of health care24,25, one example of which was the World Conference on Social Determinants of Health in Rio de Janeiro, 201126. Equity is a lens that has been used increasingly by rural health activists, including the WWPRP, as the fundamental ethical principle on which their calls for action are based. The World Health Report of 2008, Primary health care: now more than ever, was a clarion call to nations to address health equity through primary care27, but little has changed over the past 5 years.
These trends provide unique opportunities for the WWPRP. However, the working party and like-minded individuals need to speak up consistently in global arenas to ensure that the needs and issues of rural communities do not somehow become marginalised, but remain central in any initiatives. Funding models of healthcare service delivery and education must take into account the special circumstances of rural people.
Conclusions
Much has been achieved, but there is still much more to do. There is a need to review and consolidate, but also to move forward in terms of new challenges. The importance of rural medical education has been accepted, with the WWPRP's Guidebook on rural medical education having now being published28, but equally there is a need to intensify support for rural practitioners on the ground and to ensure the 'rural proofing' of policies adopted by governments29 as key to the goal of Health for All Rural People.
New areas that need to be tackled in relation to rural communities include the global pandemic of chronic non-communicable diseases, the continuing problems of HIV-AIDS and tuberculosis, particularly in developing countries, the impact of climate change on the rural environment and the health of rural people, and the ongoing effects of the global financial crisis.
The WWPRP has functioned effectively because of the passion of its members, who are committed to the health and wellbeing of rural communities, and the relationships that have been forged because of shared experiences and goals. The working party is striving towards recruiting members who are younger, from a greater diversity of backgrounds and from all parts of the world, as well as being balanced from a gender perspective. Just as new technology (the conference call and the fax machine) helped connect WWPRP members and rural doctors around the world in the early years, the WWPRP now uses available social media communication technologies to link rural doctors who cannot attend traditional meetings. There is no doubt that new ways will be found in the future that will support a new group of passionate individuals to join together to impact on the delivery of rural health care over the next 20 years. There is also no doubt that much work still needs to be done.
References
1. Wonca Working Party on Rural Practice. Policy on training for rural general practice. (Online) 1995. Available: http://www.globalfamilydoctor.com/groups/WorkingParties/RuralPractice.aspx (Accessed 1 May 2014).
2. Strasser R. From Shanghai to Durban: international rural health conferences. Australian Journal of Rural Health 1997; 5(3): 165-168.
3. Wonca Rural Information Technology Exchange (WRITE). Policy on using information technology to improve rural health care. (Online) 2002. Available: http://www.globalfamilydoctor.com/groups/WorkingParties/RuralPractice.aspx (Accessed 1 May 2014).
4. Wonca Working Party on Rural Practice. Kuching statement on the health of indigenous peoples. (Online) 2003. Available: http://www.globalfamilydoctor.com/groups/WorkingParties/RuralPractice.aspx (Accessed 1 May 2014).
5. Wonca Working Party on Rural Practice. Calgary commitment to women in rural family medical practice. (Online) 2000. Available: http://www.globalfamilydoctor.com/groups/WorkingParties/RuralPractice.aspx (Accessed 1 May 2014).
6. Wonca Working Party on Rural Practice. Policy on female family physicians in rural practice. (Online) 2003. Available: http://www.globalfamilydoctor.com/groups/WorkingParties/RuralPractice.aspx (Accessed 1 May 2014).
7. Wonca Working Party on Rural Practice. Policy on rural practice and rural health. (Online) 2001. Available: http://www.globalfamilydoctor.com/groups/WorkingParties/RuralPractice.aspx (Accessed 1 May 2014).
8. Wonca Working Party on Rural Practice. Creating unity for action: an action plan for rural health. (Online) 2003. Available: http://archive.globalfamilydoctor.com/aboutWonca/working_groups/rural_training/rural_actionplan.asp (Accessed 1 May 2014).
9. Wonca Working Party on Rural Practice. Melbourne manifesto: a code of practice for international recruitment of health care professionals. (Online) 2003. Available: http://www.globalfamilydoctor.com/groups/WorkingParties/RuralPractice.aspx (Accessed 1 May 2014).
10. Couper I, Worley PS. The ethics of international recruitment. Rural and Remote Health 2: 196. (Online) 2002. Available: www.rrh.org.au (Accessed 1 May 2014).
11. Wonca Working Party on Rural Practice. Policy on female family physicians in rural practice. (Online) 2003. Available: http://www.globalfamilydoctor.com/groups/WorkingParties/RuralPractice.aspx (Accessed 1 May 2014).
12. Wonca Working Party on Rural Practice. Policy on quality and effectiveness of rural health care. (Online) 2002. Available: http://www.globalfamilydoctor.com/groups/WorkingParties/RuralPractice.aspx (Accessed 1 May 2014).
13. Wilson NW, Couper ID, De Vries E, Reid S, Fish T, Marais BJ. A critical review of interventions to redress the inequitable distribution of healthcare professionals to rural and remote areas. Rural and Remote Health 9: 1060. (Online) 2009. Available: www.rrh.org.au (Accessed 1 May 2014).
14. World Health Organization. Increasing access to health workers in remote and rural areas through improved retention. Geneva: WHO, 2010.
15. Rourke J. WHO recommendations to improve retention of rural and remote health workers - important for all countries. Rural and Remote Health 10: 1654. (Online) 2010. Available: www.rrh.org.au (Accessed 1 May 2014).
16. Wonca Working Party on Rural Practice. Cebu strategies. (Online) 2011. Available: http://www.globalfamilydoctor.com/groups/WorkingParties/RuralPractice.aspx (Accessed 1 May 2014).
17. Wonca Working Party on Rural Practice. The Thunder Bay Communique: new ways of thinking. (Online) 2012. Available: http://www.globalfamilydoctor.com/groups/WorkingParties/RuralPractice.aspx (Accessed 1 May 2014).
18. Frenk J, Chen L, Bhutta ZA, Cohen J, Crisp N, Evans T, et al. Health professionals for a new century: transforming education to strengthen health systems in an interdependent world. Lancet 2010; 376(9756): 1923-1958.
19. Celletti F, Reynolds T, Wright A, Stoertz A, Dayrit M. Educating a new generation of doctors to improve the health of populations in low- and middle-income countries. PLoS Medicine 2011; 8(10): e1001108.
20. Boelen C, Woollard B. Social accountability and accreditation: a new frontier for educational institutions. Medical Education 2009; 43(9): 887-894.
21. Global Consensus for Social Accountability of Medical Schools. Global Consensus for Social Accountability of Medical Schools. Position statement. (Online) 2011. Available: http://www.healthsocialaccountability.org (Accessed 1 May 2014).
22. Palsdottir B, Neusy AJ. Global health: networking innovative academic institutions. Infectious Disease Clinics of North America 2011; 25(2): 337-346.
23. Tesson G, Curran V, Pong RW, Strasser R. Advances in rural medical education in three countries: Canada, the United States and Australia. Rural and Remote Health 5: 397. (Online) 2005. Available: www.rrh.org.au (Accessed 1 May 2014).
24. Starfield B, Birn AE. Income redistribution is not enough: income inequality, social welfare programs, and achieving equity in health. Journal of Epidemiology and Community Health. 2007; 61(12): 1038-1041.
25. Welch VA, Petticrew M, O'Neill J, Waters E, Armstrong R, Bhutta ZA, et al. Health equity: evidence synthesis and knowledge translation methods. Systematic Reviews 2013; 2: 43.
26. World Health Organization. Summary report: World Conference on Social Determinants of Health. (Online) 2012. Available: http://www.who.int/sdhconference/resources/Conference_Summary_Report.pdf (Accessed 1 May 2014).
27. World Health Organization. The World Health Report 2008: Primary health care - now more than ever. Geneva: World Health Organization, 2008.
28. Chater AB, Rourke J, Couper ID, Strasser RP, Reid S (eds.) WONCA rural medical education guidebook. (Online) 2014. Available: http://globalfamilydoctor.com/groups/WorkingParties/RuralPractice/ruralguidebook.aspx (Accessed 1 May 2014).
29. Swindlehurst HF, Deaville JA, Wynn-Jones J, Mitchinson K M. Rural proofing for health: a commentary. Rural and Remote Health 5: 411. (Online) 2005. Available: www.rrh.org.au (Accessed 1 May 2014).




