full article:
Two small rural towns on the south coast of the Australian state of New South Wales (NSW), where procedural general practitioners (GPs) provide primary care to the population, were early adopters of an innovative year-long integrated clerkship (clinical placement) designed to foster medical student skill attainment and a commitment to underserved rural communities. These towns, just 7 km apart, are 3 hours by road from Sydney, the capital city of the state. The GPs provide emergency, anaesthetic and obstetric services, supported by a range of health professionals and a 25-bed hospital. Medical specialist services are limited.
The essential and urgent need to provide equitable access to quality primary health services for Australian's rural communities has been highlighted by many authors, including Tham and colleagues1. Recruitment and retention of medical practitioners for the two towns in the present study was a challenge, with practices often making considerable financial investment in recruitment, with limited success. Clinical workload was especially high in the summer months given the coastal location of the towns and the attractiveness of local beaches to visitors. Engagement in postgraduate training of GPs was one strategy to encourage recruitment, and five of the GPs had been supervising vocational trainees for the past 10 years. Previously, they had only engaged intermittently and informally with undergraduate medical education. Clinicians in the region had no prior formal links with a university, no active involvement in undergraduate medical curriculum development or delivery, limited experience of medical student involvement in their community hospital service, little infrastructure for undergraduate teaching (eg extra consulting rooms for supervised student consulting), and student accommodation was limited.
In 2007, a new graduate-entry medical school with a shift in emphasis from teaching and learning in specialism to generalism2 was launched in the region, just 2 hours north of these towns. The school's mission, namely an aspiration to address the shortage and maldistribution of the Australian medical workforce and to develop competent patient-centred graduates, was of considerable interest to those aiming to build generalist medical practice in their rural communities.
The local practices first supervised short-term placements (a fortnightly afternoon session) for junior medical students which the school established to contextualise the students' early theoretical learning in the real world of clinical practice. The preceptors (supervising doctors) were encouraged to note that local patients were willing participants in junior student medical education, and actually would have accepted more student involvement than occurred3. After considerable university engagement with a range of healthcare clinicians and managers, including information sessions and workshops on the longitudinal integrated clerkship (LIC) model, teaching, learning and assessment, a local 'champion' emerged to foster the participation of two local general practices, each hosting one or two LIC students (N=3), commencing in 2009. LIC students commenced this year-long placement from mid-way through the third year of their 4-year medical program, leaving 6 months for an elective and hospital-based student internship in preparation for the first graduate year.
In a LIC placement, senior medical students spend one full academic year living and learning in a regional, rural or remote community in NSW4. The clerkship is an integrated placement, with students learning longitudinally and concurrently in both community and hospital healthcare settings, rather than in the traditional model of a series of short-term speciality-based hospital rotations in urban centres5. Each student is based in a general practice where they consult with patients, in parallel with and under the supervision of GP preceptors. In addition, students participate in all healthcare activities in the GP-staffed hospital. This small rural hospital received a modest infrastructure grant to improve education facilities for staff and students. Each general practice hosting a student received a one-off infrastructure grant to modify the practice, or add an extra consulting room for the student, funded by a Commonwealth government initiative for rural undergraduate medical education. In addition, the practice was eligible for a government practice incentive payment (PIP) for teaching. This comprised A$100.00 per session that the student was supervised in the practice. While the Australian government has recently doubled the PIP teaching payment, it was modest at the time when the LIC was established. Preceptors' commitment to their community, their profession, and recognition that the university valued generalism as an educational philosophy for medical education, were some of the expressed motivations for engagement with the LIC model4.
In 2011, when the practices in the town were hosting the second group of LIC students (N=5), it was apparent that something had happened after 'the LIC came to town'. Anecdotes from both the university and local community suggested that the initiative was having influence on more than student learning. This prompted a study seeking the perspectives of many stakeholders in local health care, with the following research question: What is the impact of the LIC medical education initiative on the healthcare community(s) of practice in two rural towns in NSW?
Semi-structured, face-to-face interviews were undertaken with 23 participants from a range of roles associated with the rural medical practices or local hospital: four in reception, three in business, five doctors (four GPs, one vocational trainee (GP registrar)), two immediate-past LIC medical students, eight in practice or hospital nursing or midwifery (including one emergency department specialist) and one in allied health. An independent interviewer travelled to the region and undertook all interviews, which were recorded and transcribed. Participants were recruited by convenience sampling due to their availability at the time that the interviewer was in the region. Because the healthcare community was small, a range of participants who were in the practice, or working in the hospital during the interviewer's visit, consented to interview. Questions probed the impact of the introduction of the LIC model of medical education on health service in the practice and community. Three researchers (JNH, KMW, PJK) independently analysed the data and organised emergent categories into themes using inductive content analysis6. Only one of these researchers was involved in the implementation of the LIC initiative.
Ethics approval
Informed consent was sought by the independent interviewer and ethics approval was obtained from the University of Wollongong Human Research Ethics Committee (HE09/244/10/080).
Four major themes emerged from the interview data, with a range of participants contributing to the generation of each theme. Participant comments that illustrate the multidisciplinary perspectives in relation to each theme are quoted (Tables 1-4).
Theme 1. Transforming a community of practice
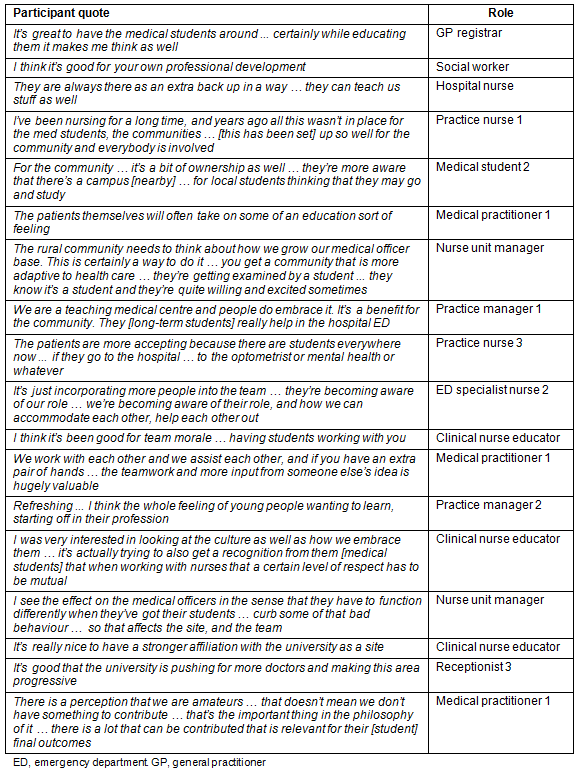
The community of practice delivering health care in the town was transformed by the introduction of a LIC. A teaching community was created, with impacts on individuals as well as healthcare teams. Morale and teamwork were improved by being valued as a community for medical education, with students contributing to the workload. There was enthusiasm for this teaching and learning role, and professionals and patients were enlivened by the opportunity to make a longitudinal contribution to the personal and professional development of medical students. These benefits were reported by those who supported as well as those who actively taught the learners.
Relationships in established community teams were improved, and a culture of helping each other was established. Some participants saw it as an opportunity to enhance the culture of mutual respect between members of the healthcare teams. The community was empowered by the partnership with the university in medical education.
Table 1: Participant quotes - theme 1
Theme 2. Realising the potential of the health service
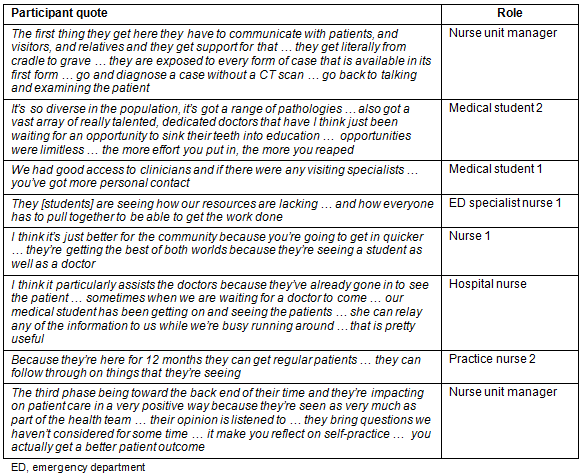
While the health service had been providing health care to the community and surrounds, the LIC initiative allowed the service to realise what they had to offer for quality medical education and appreciate what the long-term students added to the service provided. While it was acknowledged that, due to their supervision needs, medical students can decrease patient access to health care, many recognised that students actually improved access to care for patients by acting as assistant physicians in the team.
Patients of a supervising doctor first saw the student, and then the doctor together with the student, and this ensured that patients, in this area with workforce shortage, maintained access to their own doctor. Doctors improved their standard of care, and student participation enhanced coordination of patient care. Students had 'fresh eyes' on patient presentations, became part of the healthcare team over time and their perspectives promoted reflection on clinician practice.
Table 2: Participant quotes - theme 2
Theme 3. Investment in rural return
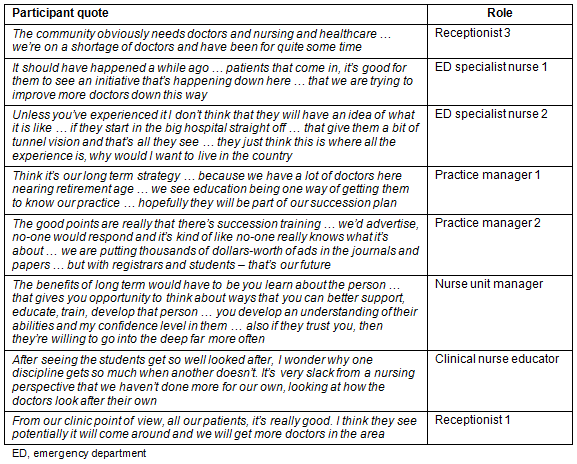
It was well recognised that rural communities need more doctors and the student was seen as potential for rural return. The practices had a commitment to the community and strategies for succession planning. The opportunity to engage with a long-term student was valued because both learner and educator could develop a greater appreciation of each other.
There were suggestions to extend the longitudinal model to nursing and allied health. Older doctors saw that the time costs were an investment in future rural workforce, and other participants reported that patients also saw the students as potential medical workforce in their area.
Table 3: Participant quotes - theme 3
Theme 4. Sustainability
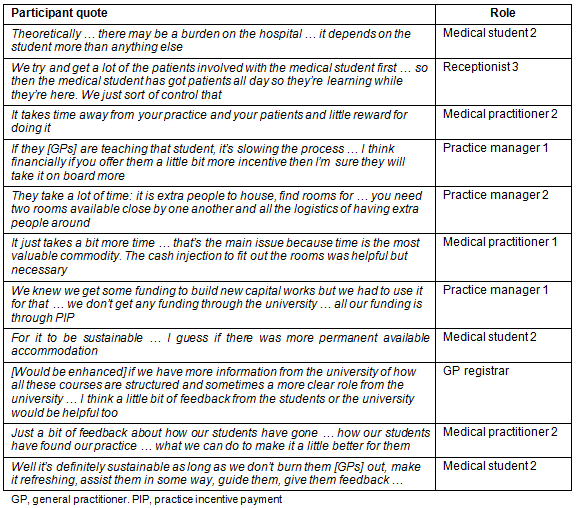
Participants advised that issues of time, resources and validation required ongoing attention to sustain the program. The teaching capacity of the community was finite and so needed monitoring. For the time cost, provider remuneration should be appropriate and value the teaching and mentoring contribution. The time cost of other practice professionals should also be acknowledged: they organised student parallel consulting, 'sold the student to the patient' and assisted the student with a range of tasks. Infrastructure was critical and the following were needed to sustain the program: extra practice rooms, financial incentives, improvement in hospital facilities, permanent student accommodation and reliable technology.
There was a recommendation to invest in good local leadership and leadership succession planning. A range of staff contributed to management and success of the initiative and they valued feedback from the institution on what they were doing well, and how to improve where needed.
Table 4: Participant quotes - theme 4
Discussion
Previous studies of longitudinal integrated clerkships have reported benefits for students, preceptors and patients7-9. The present study has provided novel evidence on the impact of a LIC initiative on the healthcare community of practice in two adjacent small rural towns in south-eastern Australia, from the perspective of a multi-professional group. The group comprised local medical practitioners, a general practice trainee, hospital specialists and managers, nursing, hospital and practice managers, practice reception staff, student alumni and an allied health professional. When a LIC came to town, study participants believed that integrating this innovative model of medical education within the health service transformed the culture and quality of care.
A teaching community was created by this expansion of primary care-based medical education in their region. There were positive impacts on individuals as well as local healthcare teams. Participants were enlivened and empowered by the opportunity to be integral to the personal and professional development of students. There was a sense of individual and collective ownership in the initiative. Team morale, mutual respect between members and relationships were enhanced. Van der Weyden10 suggested that doctors in teaching hospitals 'benefit from a profound professional advantage which flows from the academic ambience and collegiality of their workplace; their ability to shape the learning and interest of young minds' (p. 66). The perspectives of participants in the study suggested that the LIC initiative gave rural general practitioners, as well as their colleagues, opportunity to enjoy the same benefits in community practice.
The region offered students a broad clinical exposure and the longitudinal placement allowed time for the student to achieve the competence required for an active supervised role in patient care. Then the student was able to impact positively on patient access to care. This confirmed the university's view that the generalist learning environment was valuable for longitudinal placements for medical students. The diversity of patient presentations in general practice has already been acknowledged as a rich curriculum of acute and chronic medicine11, with rural preceptors reporting that they practise 'cradle-to-grave' medicine4.
Small rural towns with procedural GPs, practice nurses and a community hospital provide health care to their community. However, many rural communities in Australia struggle to maintain viable healthcare services due to infrastructure and workforce shortages1. Longitudinal engagement with senior students was seen as a new strategy to address the ongoing challenge of recruiting and retaining medical practitioners. Despite identified time and cost constraints, there was an overwhelming view that this strategy was an investment in rural health succession planning.
Time and costs are critical issues that must be addressed for sustainability. It takes time to guide and enthusiastically mentor medical students, and preceptors can face burnout and financial cost from engagement with a LIC initiative. Practice staff reported playing an active role in managing the impact of students on patient throughput, while also ensuring that students had access to patients. A LIC student participant identified that students themselves play a critical role in maintaining preceptor involvement, by assisting with the workload, guiding them on educational needs and giving feedback to the preceptor. The university continues to advise students that 'what they put in, they will get out' as a strategy to ensure they are active participants in the doctor-patient-student learning triad.
The practice infrastructure grants helped to recruit practices, but there were infrastructure challenges relating to student accommodation, improvement in hospital facilities and educational technology. The financial impact on preceptors can be neutral or even positive8 but most preceptors and some of their colleagues emphasised that reducing any negative financial impact was critical for sustainability. The doubling of the PIP for teaching and further rural general practice infrastructure funding in the 2014 Australian Commonwealth budget should make a positive contribution to the financial sustainability of the program12.
A range of participants requested more information about the course, more feedback from students and the university about how their students have performed in final assessments. They expressed commitment to providing a quality learning experience but that required validation of their performance for quality improvement and to maintain the perspective that they were valued by the institution. The university has endeavoured to address this issue, and with greater maturity of the program both students and preceptors appear more confident with the model. Finally, succession planning was identified. In this case, the solution (more clinicians in rural general medical practice) aimed to address the problem.
The patients' perspective was conveyed in the data collected, but given that patients are the key stakeholder in healthcare education initiatives a separate study was conducted to obtain a perspective from patients themselves7. This subsequently demonstrated that patients from remote, regional and rural settings (including the region of the present study) valued the LIC learning environment as both patient- and learner-centred. Patients reported that their health care improved and they also felt part of the community of practice7.
The qualitative data was analysed by three of the four authors of this article. Only one was involved in the development and implementation of the LIC initiative by the relevant university and this involvement facilitated understanding of the stated perspectives. The other two have subsequently been recruited by the university for academic roles that are separate to the LIC program but were not involved in the LIC when the data was collected. The second author was a preceptor in the region. He offered perspectives but was not involved in data collection or analysis. Use of an independent and separate interviewer enabled participants to provide anonymous comments. Some professions had limited representation in the sample, due to local workforce numbers and availability when the interviewer visited the town. While a convenience sample can limit the ability to generalise the findings, the population from which the sample was derived was small and the sample was representative of most of those interacting with the students. The health service work roster determined to some extent who was available for interview, reducing sample bias to some degree. The sample was diverse and the quotes illustrate that participants all raised similar issues such that data saturation was reached.
Medical workforce shortage is an important factor in the reduced access to health care experienced by many rural communities in Australia. The LIC initiative has enhanced the integration of education with health care in two small towns in rural NSW. The culture it has promoted will potentially have benefits for health care in the region, but also for the recruitment of LIC graduates to rural postgraduate education or service.
Acknowledgements
Thank you to the professional and clinical staff of the medical practices of the Milton Ulladulla region and Milton-Ulladulla Hospital and the Community Based Health Education Team at the University of Wollongong Graduate School of Medicine at the time of the study, for their support of the LIC students and/or study participation. Coast City Country GP Training provided funding support for independent data collection and transcription of the interviews.
References
1. Tham R, Humphreys JS, Kinsman L, Buykx P, Asaid A, Tuohey K. Study protocol: evaluating the impact of a rural Australian primary health care service on rural health. BMC Health Services Research 2011; 11: 52.
2. Van der Weyden MB. New medical school with a clear vision. Medical Journal of Australia 2007; 186: 217.
3. Hudson JN, Weston KM, Farmer EA, Ivers RG, Pearson RW. Are patients willing participants in the new wave of community-based medical education in regional and rural Australia? Medical Journal of Australia 2010; 192: 150-153.
4. Hudson JN, Weston KM, Farmer EA. Engaging rural preceptors in new longitudinal community clerkships during workforce shortage: a qualitative study. BMC Family Practice 2001; 12: 103.
5. Worley P, Silagy C, Prideaux D, Newble D, Jones A. The parallel rural community curriculum: an integrated clinical curriculum based in rural general practice. Medical Education 2000; 34: 558-565.
6. Graneheim UH, Lundman B. Qualitative content analysis in nursing research: concepts, procedures and measures to achieve trustworthiness. Nurse Education Today 2004; 24: 105-112.
7. Hudson JN, Knight PJ, Weston KM. Patient perceptions of innovative longitudinal integrated clerkships based in regional, rural and remote primary care: a qualitative study. BMC Family Practice 2012; 13: 72.
8. Hudson JN, Weston KM, Farmer EA. Medical students on long-term placements: what is the financial cost to supervisors? Rural and Remote Health 12: 1951 (Online). 2012. Available: www.rrh.org.au (Accessed 10 January 2014).
9. Walters L, Greenhill J, Richards J, Ward H, Campbell N, Ash J, Schuwirth LW. Outcomes of longitudinal integrated clinical placements for students, clinicians and society. Medical Education 2012; 46: 1028-1041.
10. Van der Weyden MB. Expanding primary care-based medical education: a renaissance of general practice? Medical Journal of Australia 2007; 187: 66-67.
11. Thistlethwaite JT, Kidd MR, Hudson JN. General practice: a leading provider of medical student education in the 21st century? Medical Journal of Australia 2007; 187: 124-128.
12. Australian Government, Department of Human Services. Budget 2014-15: health matters and health professionals. (Online) 2014. Available: http://www.humanservices.gov.au/corporate/publications-and-resources/budget/1415/measures/health-matters-and-health-professionals/ (Accessed 4 August 2014).



