full article:
A recent study exploring factors affecting rural physiotherapy service provision and service level decision making revealed considerable service variation between sites within the study1. Numerous influencing factors contributed to the variation including macro level policy and funding decisions, service priorities and fiscal constraints of regional health services and capacity and capabilities at the physiotherapy service level.
Understanding the issues that inform local service provision can provide insights into service availability of health services such as physiotherapy. The use of the term 'service availability', a reflection of service supply, is key to this discussion, as the presence of one or more health professionals in a community, for example physiotherapist(s), does not mean that a full range of service options are available.
Physiotherapists provide services across the service continuum and lifespan2. Available in Australia through both public and private health sectors3-5, physiotherapy has work settings in regional, rural and remote areas including in public hospitals, private practices, community based teams and non-government organisations3-5. Physiotherapy service provision and funding is service- and sector-dependent. Public sector physiotherapy services are funded through state and territory health departments and provided through regional health services and networks6. The Australian Government funds programs to enhance access in underserviced areas and specific service programs6-9. Private services are funded by the individual in a fee-for-service environment3, with a range of rebates or fee supports through private health insurance, third party insurance, compulsory employer workplace insurance and the chronic disease management items within the benefits schedule of Medicare, Australia's federal health insurance program8.
Neither the breadth of services nor service variation is revealed by simply quantifying the number of health professionals in rural areas. Descriptions of workforce maldistribution, such as physiotherapy, where only 20% of physiotherapists work beyond major cities10, imply, but do not describe, reduced service availability. Similarly, the dominant workforce focus prevailing in the rural physiotherapy literature3,4,11,12 tends not to progress the link between workforce shortages and impact on service provision. The diversity of services provided by physiotherapists4,5 further challenges generalisations about service availability.
This article draws upon participant comments describing local physiotherapy services and factors influencing service provision. Key influencing factors are then combined into a conceptual framework or possible measure of rural physiotherapy availability.
The research design was shaped by the aim of obtaining perspectives of multiple physiotherapy service stakeholders. A priority-sequence mixed methods model13 was used to guide the practical integration of qualitative and quantitative approaches to explore rural physiotherapy service provision and service level decision making. An interpretivist approach within a qualitative research paradigm supported understanding of stakeholder perspectives14. Stratified purposive sampling15 permitted exploration of subgroups of interest. The subgroups include physiotherapists, their colleagues (which may include other allied health professionals, nurses or doctors), managers and other key decision makers (eg hospital managers, team leaders and professional leaders).
Setting
The investigation area is a large part of one Australian state with a mix of regional, rural and remote communities. The scope of the study was bounded by the defined geographic area of two rural health service networks. This area offered the opportunity to explore rural physiotherapy services across many health service settings. Due to the relatively small proportion of physiotherapists working in regional, rural and remote areas, combined with the detail of perspectives offered, it is difficult to provide more detailed description of the investigation area and still maintain participant anonymity.
Participants
Public sector physiotherapists were prioritised in the research design, because a greater reliance on the public sector for the provision of allied health services, including physiotherapy, has been reported in rural and remote regions of Australia11. Private physiotherapists formed a second focus, because an increasing proportion of the physiotherapy workforce work in the private sector10. Key stakeholder groups included multidisciplinary team colleagues, consumers, managers and other decision makers. Stakeholder perspectives were obtained through surveys and in-depth interviews. Obtaining perspectives of multiple stakeholders avoided isolating the research to a physiotherapy-only perspective16.
Data collection
Use of an initial survey allowed the researcher to obtain the perspectives of a larger number of stakeholders than may have been feasible if only a qualitative approach had been adopted. Public sector physiotherapists were sent written invitations to participate in the research through local professional networks1. Senior physiotherapists in the investigation site provided key physiotherapy contacts in the public sector physiotherapy departments within the investigation site via email. The survey was purposefully designed and had previously been piloted in a rural location in another state17. Surveys were mailed to key physiotherapy contacts for distribution to colleagues in their facility. Physiotherapists were invited to complete the survey containing a mix of closed and open ended questions to describe service provision, setting and rurality, and factors influencing service provision. More specifically, the survey collected demographic data and information on rural experience, work setting and number of colleagues, services provided, perspectives on factors influencing service provision and decisions about service provision, including identities of the decision makers. Data collection occurred from January to September 2012.
Physiotherapists were also asked to distribute surveys to stakeholder groups relevant to the local service, including multidisciplinary team colleagues, managers and other decision makers18. The physiotherapists were thus able to guide or direct this data collection phase to stakeholders they identified as relevant to the decision making process locally. Private physiotherapists working in the same communities were identified through listings in a telephone directory for Australian businesses and invited by the researcher to complete the physiotherapy survey. The practice owners were prioritised as key to decision making about service provision within their private physiotherapy service.
Participants were asked if they would be willing to participate in a follow-up interview. Semi-structured in-depth interviews were conducted with survey participants who had agreed to participate in an interview. Interviews were also conducted with other key decision makers identified by local physiotherapists, to provide greater insight into issues raised in the surveys. The same approach had been adopted in the pilot study in another state17.
Data analysis
Survey data were recorded in Microsoft Excel spreadsheets and analysed using descriptive statistics. Thematic analysis of open ended survey questions informed the development of initial themes and areas for further exploration in interviews. Interviews were recorded and transcribed verbatim, with full interview transcripts and a summary developed by the researcher provided to interview participants for their review and comment. Transcribed interviews were then entered into NVivo v10 (QSR International; http://www.qsrinternational.com). An iterative approach was used to guide the thematic analysis of qualitative data. The levels of analyses included ongoing preliminary analysis to critique data as it came in; thematic analysis to develop tentative themes; and coding, including the generation of themes and concepts to develop codes, which were then used to frame account for the remaining data19. To maintain consistency, the principal researcher entered all transcripts into NVivo and completed the initial analysis. Then all four researchers discussed the coding before a random selection of interviews were coded by a second researcher to check for consistency20.
Ethics approval
Ethics approval was obtained from the Human Research Ethics Committee of both James Cook University (approval number H3799) and the health services of the study.
Participants and sites
Physiotherapy surveys were received from 11 of the 25 (44%) public sector facilities identified as providing physiotherapy services in the investigation area. The communities from which the public sector survey responses were received form the 11 sites of this study. The 16 completed public sector physiotherapy surveys received represented a 29.4% response rate (54 physiotherapy surveys were distributed across the investigation site). Five surveys were received from principals of private physiotherapy practices (Table 1). The average years of experience of physiotherapy participants in the public sector was less than that of the private sector, even when the three new graduates are discounted (Table 2). This is perhaps reflective of the sampling, which prioritised the principals of private practice and new graduate employment options in the public facilities within this study. However, both groups include clinical physiotherapists with many years of rural physiotherapy experience (Figure 1) and offer a breadth of perspectives from a range of service sites. Survey responses were received from 13 colleagues and managers. Descriptions of physiotherapy services provided within each community were obtained from stakeholders. Sixteen interviews were conducted by the principal researcher with physiotherapists and other key decision makers (Table 1).
Table 1: Survey and interview participant numbers
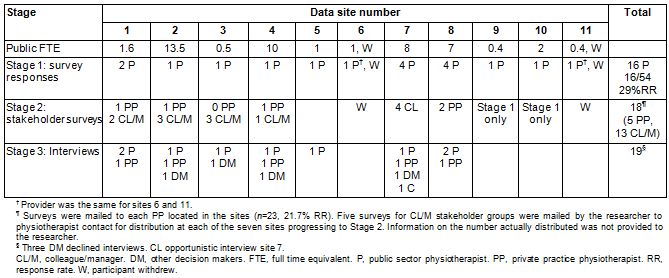
Table 2: Physiotherapist survey participant characteristics
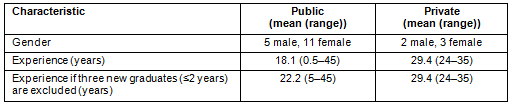
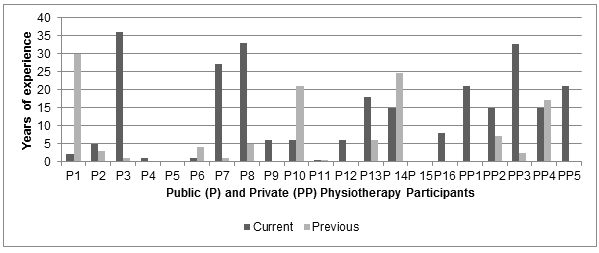
Figure 1: Years of physiotherapy experience: public and private physiotherapy participants.
Physiotherapy services across study sites
Four of the eleven sites (3, 6, 9 and 11) relied solely on physiotherapy services provided through the local public hospital or health service. Service provision at these sites, while primarily ambulatory, was generalist in nature and included musculoskeletal rehabilitation, hand therapy, some paediatrics and neurological physiotherapy. Cardiac and pulmonary rehabilitation, healthy lifestyle programs and other preventative groups were also provided at the largest of these four sites. Population at these sites ranged from 600 to 5000.
Three sites (5, 7 and 10) had only one private practice in addition to the public service. Population at these sites ranged from 3000 to 20 000. Population size appears not to be the only determinant for the establishment of private physiotherapy services. Public physiotherapy services in sites with a single private provider included a small rural hospital, a major rural referral hospital and a multipurpose centre. The variety in service availability begins to highlight issues of access to services. Private physiotherapy services, for example at site 7, were described as mainly for private patients with musculoskeletal conditions.
Four sites (1, 2, 4 and 8) had three or more private physiotherapy practices, with the larger regional centres having up to six practices. However, access to public sector outpatient physiotherapy services decreased with increasing population size. The demands on the larger public hospital services necessitate prioritisation of inpatient services with outpatient service availability variable. For example, site 2, with an approximate population of 40 000, has numerous private practices, but the public sector allocation to general outpatient physiotherapy (OPP) services was less than one full time equivalent (FTE) (≤1:40 000 public OPP).
In contrast, in smaller rural sites, outpatient services often form the majority of the caseload. For example the sole part-time public physiotherapist at site 3, where there is no other locally based physiotherapy provider, allocated approximately one half time equivalent to OPP services (approximately 0.5 FTE to 4700 public OPP). A similar OPP allocation occurs at site 5, which has a population of 3000, and a local private physiotherapy practice. The OPP services provided in the smaller sites included health promotion and prevention activities.
Service range and type
Services described by participants included those provided by physiotherapists in public hospitals or health services, private physiotherapy practices and specifically funded programs. Participants differentiated between physiotherapy service types. Public sector services included acute inpatients and general outpatient type services, for example musculoskeletal physiotherapy and hydrotherapy. Rehabilitation inpatient and outpatient services were distinguished from general medical and surgical inpatient services and also general outpatient physiotherapy services. Participants also differentiated paediatric physiotherapy into services for orthopaedic or neurological and developmental conditions. For example, physiotherapy for management of orthopaedic conditions such as congenital talipes equinovarus or developmental dysplasia of the hip were differentiated from physiotherapy for plagiocephaly, developmental delay and neurological paediatric conditions in terms of required skill sets and level of expertise.
In addition to public sector services, locally based private physiotherapy practitioners and, in some communities, specialised services such as rehabilitation and paediatric disability physiotherapy services, add to the service availability. Visiting or outreach services complement local services in some communities. However, four communities in this study had no local private physiotherapy practice (sites 3, 6, 9 and 11).
I'm point five, full time equivalent ... and there have been times this year that I've been the only one in thirty thousand square kilometres. (public physiotherapist 8)
Cerebral Palsy Alliance is based in [a nearby town]; they have a limited target group that they'll see. (public physiotherapist 1)
... we provide mainly musculo-skeletal from under five through to 100 and something. (private physiotherapist 2)
... having the sub-acute team has been probably the best innovation in the last 8 years ... they come out to the regional smaller sites. (public physiotherapist 5)
Only one community had a separate sub-acute rehabilitation facility (site 4), and two public sector services (sites 2 and 8) reported they had been recently required to reduce outpatient rehabilitation services due to decreased capacity and service priorities. Private practitioner respondents primarily provided musculoskeletal physiotherapy services to patients who elected to pay for treatment, use private health insurance or for whom services were otherwise compensated such as workers compensation, motor vehicle insurance or Medicare (chronic disease management items). Private practitioners did provide sessional visits to residential aged care facilities, but paediatrics and neurological rehabilitation were generally not provided.
So I do the aged care facilities and I still do my hydrotherapy, I'll see patients in a public pool, so any of the gyms or the aquatic centre, and that's usually a complement to treatment that we're doing in the rooms. (private physiotherapist 1)
The range of public inpatient and outpatient services in this study varied with facility size, role and function. In smaller rural communities it was more likely that a sole physiotherapist would be providing services across all age groups, balancing ambulatory and inpatient demands. Physiotherapists in larger communities hosting regional hospitals were required to prioritise inpatient activity and reported a decreasing capacity to meet ambulatory service demand in areas such as general outpatients, paediatrics and rehabilitation.
We do do out-patients - so if it was just one full time person [the role] would be half half - half in-patients half out-patients. (public physiotherapist 5)
2FTE for 120 beds ... which include the rehab beds. (public physiotherapist 1)
Priority one is the ICU [intensive care unit] sort of work, your very early stage orthopaedic patients, your day one gut surgeries, day one strokes ... then right down the bottom of the list is mobility aid assessments, mobility reviews and all of that sort of stuff. (public physiotherapist 2)
Participant descriptions of physiotherapy service range and type revealed considerable variation in service availability between the 11 communities of this study. This prompted the researchers to consider how such variation could be reflected or reported.
Considering both survey and interview participant descriptions of services provided, it seemed possible to view a number of influencing factors as key elements informing service availability. The elements that emerged from participant comments include rurality and population, size and funding model of public hospitals, the number of public sector physiotherapists and private practices and availability of specialised paediatric and rehabilitation services. Each of the elements are discussed below; however, it is the combination of elements that provides a more comprehensive picture of physiotherapy service availability. In order to develop that more comprehensive picture, key elements are then combined into a conceptual framework or possible measure of rural physiotherapy availability.
Rurality and population size
Participants described rurality as a significant influence on service provision. Rurality impacted the availability of physiotherapy services, the range and level of services provided, access to services, patient travel distance, recruitment and retention of physiotherapists, organisational structure and reporting lines, and the capacity to sustain private physiotherapy services. Examples of participant comments on the impact of a rural or remote location on physiotherapy services include:
And that was the big thing from city versus country physio or rural physio, a lot of my patients travel six hours to see me. (private physiotherapist 4)
There's no public transport ... unless you've got a car ... and with the cost of petrol at around $1.50 to $1.53 a litre, a 400km round trip's a barrier. (manager/decision maker 4)
I think you have to become more of a generalist specialist. (private physiotherapist 5)
Yeah and people look at where we are on the map and they go 'Oh my God it's all the way out there' you know? (private physiotherapist 5)
The capacity to access high level services is limited. ... So the capacity to access the higher level service I think is one of the things that defines this as remote. (manager/decision maker 4)
Participant comments suggested that physiotherapy service provision is influenced by population size, both in terms of service demands, the capacity to provide services and the viability of private sector services.
I don't think that the population could actually support a significant private practice. (manager/decision maker 4)
The more the community shrinks the harder it gets, because the less there is to offer. (manager/decision maker 1)
The Shire's about five and a half thousand; the town is about three thousand I think, and I'm point five for that size community. (public physiotherapist 8)
A lot of metro-centric approaches to how you deliver health and what health access equity and relevance is ... the population base doesn't align very nicely at all with rural remote populations. (colleague 1)
Public hospital and health service physiotherapy numbers and private practices
The increased reliance on public sector services reported for rural communities11 was reinforced by participant comments. While a number of communities had one or more private practices, adding valuable service capacity, four communities relied on public sector physiotherapy services. However, the range and type of private sector physiotherapy services reported by participants in this study was narrower than that of the public sector service, focusing primarily on musculoskeletal physiotherapy. Private capacity was influenced by financial viability and community size. Participant examples of the relative size and scope of some of the physiotherapy services are provided below. It should not be assumed that changes to service scope within the public sector physiotherapy would mean that private physiotherapists would be positioned to cover any emerging service gaps.
I'm in private practice, I do general physio ... so I don't do much neurological, I don't do many kids and I don't do anything really long term, chronic. I keep it to what I'm happy with. (private physiotherapist 1)
We've got specialties in in-patient care, rehab, out patients/fracture clinic, we've got a 0.42 of paediatrics specialty. One of our out-patient [physiotherapists] is a 0.42 and does a lot of lymphodoema and then there's also an emergency position. We've got a nice mix of specialties and senior staff and then there's the junior rotating staff, so that gives a broad mix of people and skills. It means the department can feed off each other quite well in terms of maintaining skills. In a hospital this size we're actually lucky to have that range of people. (manager/decision maker 1)
There are three private practices in town, so they are covering some of that outpatient caseload, but it's only for those who have the ability to pay or who qualify for that enhanced primary care Medicare rebate thing. That's it. They don't cover rehab. (public physiotherapist 1)
Public bed numbers and funding models
The number, type and level of inpatient beds were noted by many participants as a key factor influencing public sector physiotherapy service provision. The type of funding was also reported to influence activity, with participants often distinguishing between activity-based funding and non-activity-based or block funding21 when discussing factors influencing physiotherapy service provision.
Size of hospital, generalist skills required, being able to do a bit of everything, within the Department that needs to be able to cover everything off ... this hospital is about 150 beds, which includes quite a few renal chairs. (public physiotherapist 1)
Senior positions and expertise also goes with the size of the hospital, because it goes with the type of services that your hospital offers, not just the size of your department. It's about getting people out of hospital ... it's about the whole hospital, the business of the hospital. (manager/decision maker 1)
You try and maximise how much money you get for a particular patient type ... so they've worked out that on a certain day, say day three post hip or knee, that patient is going to get flowed out directly to a peripheral facility. So that we get the maximum amount of money, because they're not ABF [activity-based funding] funded they can then finish the job. (public physiotherapist 3)
Rehabilitation and paediatrics
The frequency of participant comments regarding rehabilitation and paediatric physiotherapy services suggested both were important issues when considering physiotherapy service availability. Recent reductions in outpatient rehabilitation services and the differentiation of the skill requirements for paediatric neurological and orthopaedic physiotherapy suggested potential constraints on the availability of these types of service.
The other group that misses out here is probably the rehab type ones, as in people who need ongoing physio for a long period of time. (private physiotherapist 3)
One of the gaps in our service in [our town] at the moment is rehab out-patients. (manager/decision maker 1)
... and the paediatrics demand is skyrocketing ..., there's quite a lot of referrals for kids who need serial casting, post botox, toe walking ... some of whom will qualify for Cerebral Palsy Alliance, some of whom don't, but will require quite a lot of intervention. There's a huge waiting list, we're now just focussing on the high priority and the very high priority referrals. We even triage the very highs, little babies that need a check-up or a follow up, a premmie [premature] baby: that just doesn't happen. (public physiotherapist 1)
Yes [in a sense I have prioritised paediatrics], especially when I have another physio. If I was just by myself - (and this is what I've done in the past) - I didn't, I just I said I can't or I ended up with an odd sneaky one that I shouldn't have done. The problem is that it [the child's condition] just lasts forever and they go through a crisis where you can really help them and other times, when I just have to refer them, but to me I just think it's dismal - it's a dismal state - it's so substandard that it is just crying out, and who else is there to look at the paediatric patients. (public physiotherapist 5)
A framework or possible measure for physiotherapy availability
Combining the elements described above forms a useful construct to consider physiotherapy availability. Each element can be divided into ordinal categories and assigned scores. For example, rurality uses the five categories of the Australian Standard Geographical Classification - Remoteness Area (ASGC-RA) system22, population is considered in nine categories ranging from 500 to 1000 to more than 1 million and the number of public sector physiotherapists are also considered in nine categories ranging from 'no local physiotherapist' to 'over fifty physiotherapists'. The number of categories for each element were selected to enable sufficient differentiation of physiotherapy service availability and will be the subject of future validation studies. Following the ASGC-RA categories, where major cities are referred to as ASGC-RA 1, the larger the population or number of physiotherapists, the lower the score assigned.
The elements described by participants provide a framework to consider the availability of physiotherapy services and were used to inform the development of a conceptual framework or index of availability. The framework was also developed into a visual tool, the Rural Physiotherapy Availability Index (RPAI), to enable easy calculation of the RPAI score for a given site (Figure 2).
Calculation of the RPAI score commences with identifying a score for population (the outer circle) and progressing to the inner circle, adding scores for each element. For example site 5, with a population less than 5000, and one public physiotherapist working in a rural block funded hospital with less than 50 beds, with local services including a private practice and a paediatric disability service but no specialised adult rehabilitation services, scores 33. In contrast, the inner regional site 2 scores 16. Site 2 has a population of nearly 40 000 and is the location of a large rural referral hospital with a range of physiotherapy services, both public and private (Table 3).
This enables insight into both specific aspects of physiotherapy service provision and a total as an indicator of rural physiotherapy availability (Table 4, Figure 3). The higher scores (40-59) are indicative of limited availability of physiotherapy services. Sites 9 and 11 (RPAI 42 and 43), for example, have only a visiting physiotherapy service providing general outpatient physiotherapy services. Mid-range scores (20-39) reflect the presence of local services yet still with considerable variability in availability of services. For example, site 3 (RPAI 39) has only a 0.5 FTE public sector physiotherapist with no local private practice, whereas sites 7 and 8 (RPAI 25 and 21, respectively) have between 6 and 10 physiotherapists, at least one private practice and a visiting paediatric service. Lower RPAI scores (0-19) are indicative of a range of locally based services; however, the higher scores within this range suggest limitations to the availability of some physiotherapy services. Site 2 for example, which has more than10 FTE physiotherapists and numerous private practices in the community, has limited rehabilitation and paediatric physiotherapy service availability.
The sites of this study were predominantly rural with RPAI scores clustering in the mid-range; however, the RPAI scoring would enable differentiation of major urban areas and more remote sites. The RPAI score provides a relatively speedy tool to gain insight into the availability of physiotherapy services. Such information could be considered by health service policy and decision makers prior to making decisions that may adversely affect the availability of physiotherapy services for local communities.
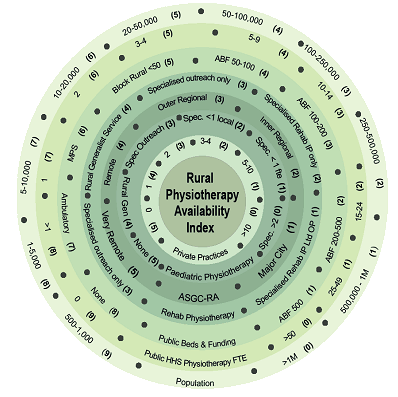
Figure 2: Rural Physiotherapy Availability Index.
Table 3: Rural Physiotherapy Availability Index scoring examples
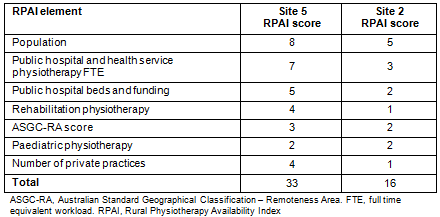
Table 4: Eleven sites of this study grouped by Rural Physiotherapy Availability Index scores
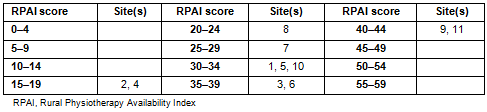
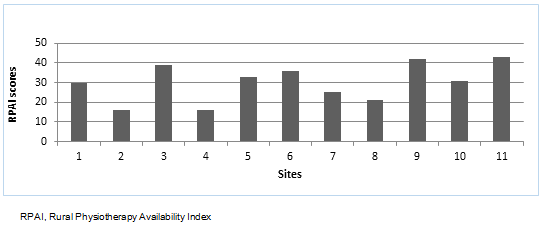
Figure 3: Differentiation of physiotherapy availability across sites.
Discussion
Simply quantifying the number of health professionals in rural areas does not reveal localised issues of service availability. It is important to make explicit the link between workforce maldistribution, the resultant rural workforce shortages and the implications for local service availability. This study sought to do so by investigating physiotherapy service provision within the rural communities of the investigation area. In doing so, varying levels of availability (or service supply) emerged within local communities.
Health workforce shortages are well documented in rural and remote areas. Physiotherapy workforce distribution patterns in Australia reveal only around 20% of physiotherapists work beyond major cities10. The strong workforce focus of the rural physiotherapy literature requires a complementary focus on service provision, including descriptions of local service availability. Service descriptions provided by the participants in this study offer insight into issues of local physiotherapy service provision and availability.
Important distinctions were made by participants about the size, sector and location of physiotherapy services. Factors influencing service availability in small rural services differed from larger regional services, as did services in public and private sectors. Consideration of distinguishing factors such as these adds layers of detail required to understand issues of service availability. There was limited availability of specialised services in both small and larger centres of this study. Private physiotherapy practices add valuable service capacity; however, many smaller communities cannot sustain a private practice. Affordability also challenges notions of availability because private physiotherapy services are generally not covered by Medicare: the exceptions are the chronic disease management items (previously Enhanced Primary Care or EPC items)8, where patients with a chronic condition can be referred by a general practitioner for a total of five allied health consultations per annum. This may change to some extent with the introduction of consumer based purchase models, for example the National Disability Insurance Scheme23 or other service purchasing models. However, the range of physiotherapy services available to the rural communities of this study was limited by the capacity of smaller rural communities to sustain a viable private practice and constraints in the public sector.
The conceptual framework or index of rural physiotherapy availability incorporates the differentiating factors or elements that emerged from participant comments. Scoring elements, such as the provision of rehabilitation services, make explicit the availability of specific services. The total score for the combination of elements then provides a more comprehensive picture and understanding of availability of rural physiotherapy services. Making local service availability more explicit, by using the RPAI for example, can assist decision making about local service provision by highlighting service variations and gaps. The advantage of the RPAI having both an aggregated score and a score for each element is that it enables insight into the specific service variations. For example, it can highlight gaps in service availability for specialised paediatrics or private physiotherapy services. This may enable better resource allocation decisions to address areas of unmet needs. Additionally, explicit descriptions of local service availability and capacity may be of assistance when developing models of care, for example outreach or hub and spoke models common in rural areas. The conceptual framework of rural physiotherapy availability may also be applicable to other rural allied health service providers.
Limitations
This study included a relatively small number of sites within one Australian state, which may not allow generalisation of findings. The recruitment strategy for colleagues, managers and other decision makers made it difficult to know how many surveys were actually distributed and should be more defined in any future research in this area. The conceptual measure of rural physiotherapy availability developed from this study may not be relevant to areas of Australia with a different mix of communities or health services. The varying scales for the scores for each element may unduly weight one element, and the validity of allocated scores will be the focus of future research. The conceptual RPAI measure should then be trialled across a larger number of sites to assess its broader applicability.
Descriptions of local services, such as physiotherapy, are important to make explicit the impact of key influences such as rurality and workforce shortages on service availability. Participant responses in this study provided insights into the detail of local service. The variation in availability and capacity of physiotherapy services between communities prompted the development of a possible measure to aid more localised description and reporting. The conceptual measure provides insight into specific aspects of physiotherapy service provision and an overall indicator of rural physiotherapy availability in a local community.
Acknowledgements
Barbara van Houts provided technical assistance in the development of the Rural Physiotherapy Availability Index diagram.
References
1. Adams R, Jones A, Lefmann S, Sheppard L. Decision making about rural physiotherapy services varies with sector, size and rurality. Internet Journal of Allied Health Sciences and Practice 2015; 13(2): 1-15.
2. Australian Physiotherapy Association. Position statement: rural and remote Australia. Melbourne: Australian Physiotherapy Assoication, 2014.
3. Struber J. Physiotherapy in Australia: where to now? Internet Journal of Allied Health Sciences and Practice. 2003; 1(2): 2-5.
4. Williams E, D'Amore W, McMeeken J. Physiotherapy in rural and regional Australia. Australian Journal of Rural Health 2007; 15(6): 380-386.
5. Sheppard L. Work practices of rural and remote physiotherapists. Australian Journal of Rural Health 2001; 9(2): 84-90.
6. Council of Australian Governments. (2011). National Health Reform Agreement. (Internet) 2011. Available: http://www.publichospitalfunding.gov.au/national-health-reform (Accessed 25 January 2014).
7. Department of Health and Ageing. Programs and initiatives: health workforce 2014. (Internet) 2014. Available: https://www.health.gov.au/internet/main/publishing.nsf/Content/work-pr-alli (Accessed 1 February 2014).
8. Department of Health and Ageing. Chronic Disease Management - Individual Allied Health Services under Medicare. (Internet) 2013. Available: http://www.health.gov.au/internet/main/publishing.nsf/Content/health-medicare-health_pro-gp-pdf-allied-cnt.htm (Accessed 25 January 2014).
9. Services for Australian Rural and Remote Allied Health. Nursing & Allied Health Scholarship and Support Scheme. (Internet) 2013. Available: http://www.sarrah.org.au (Accessed 25 January 2014).
10. Australian Institute of Health and Welfare. Allied health workforce 2012. National health workforce series no. 5. HWL 51. Canberra: Australian Institute of Health and Welfare, 2013.
11. National Rural Health Alliance. Under pressure and undervalued: allied health professionals in rural and remote Australia. Canberra: National Rural Health Alliance, 2004.
12. Lindsay R, Hanson L, Taylor M, McBurney H. Workplace stressors experienced by physiotherapists working in regional public hospitals. Australian Journal of Rural Health 2008; 16(4): 194-200.
13. Morgan DL. Practical strategies for combining qualitative and quantitative methods: applications to health research. Qualitative Health Research 1998; 8(3): 362-376.
14. Creswell JW. Research design: qualitative, quantitative and mixed method approaches. 3rd edn. Thousand Oaks: Sage Publications, 2009.
15. Patton MQ. Qualitative research and evaluation methods. 3rd ed. Thousand Oaks: Sage Publications, 2002.
16. Anaf S. Physiotherapy's role in emergency department settings: a qualitative investigation of emergency stakeholders' perceptions. PhD thesis. Townvsille: James Cook University, 2008.
17. Adams R, Sheppard LA, Jones A, Lefmann S. What factors influence physiotherapy service provision in rural communities? A pilot study. Australian Journal of Rural Health 2014; 22(3): 133-138
18. O'Meara P. Would a prehospital practitioner model improve patient care in rural Australia? Emergency Medicine Journal 2003; 20: 199-203.
19. Grbich C. Qualitative research in health: an introduction. Crows Nest, NSW: Allen & Unwin, 1999.
20. Thyer B. (Ed.). The Handbook of social work research methods 2nd edn. Thousand Oaks: Sage Publications, 2010.
21. Australian Government. The Independent Hospital Pricing Authority (IHPA). (Internet) 2016. Available: https://www.ihpa.gov.au/ (Accessed 5 March 2016).
22. Department of Health and Ageing. Australian Standard Geographical Classification - Remoteness Area (ASGC-RA) and Remoteness Area Categories. (Internet) 2011. Available: http://www.health.gov.au/internet/publications/publishing.nsf/Content/work-st-mrbs-2012-toc~work-st-mrbs-2012-asg (Accessed 29 October 2012).
23. Australian Government. National Disability Insurance Scheme Australia. (Internet) 2016. Available: http://www.ndis.gov.au/ (Accessed 5 March 2016).
