Australia is a vast country with a comparatively small population density of just three persons per square kilometre (compared with 35 in the USA, 265 in the UK and 421 in India)1. One-third of Australia's 23 million people live in rural or remote locations. These people live in towns, communities and isolated locations that have limited access to services and small population counts (<10 000)2. People living in rural and remote locations of Australia experience disadvantages because of their location and generally experience poorer health outcomes compared with their urban counterparts3. National census data for people living in rural areas estimates mortality for people aged less than 65 years is double and life expectancy 4 years shorter compared to urban areas4. This may be attributed to poorer access to health care and sporadic use of health services. Equity of access to health care in rural locations is compromised by geography, time and distance. Consequently, health needs are less likely to be met; the coordination and continuity of care is more difficult to achieve and the monitoring of health outcomes unlikely due to the intermittent nature of health service delivery in these locations5.
With the escalating costs of health care, issues with recruitment and retention of health practitioners in rural areas, and poor economies of scale, the question of delivering people to services or services to people is a dilemma for health authorities around the world. The problem of how to provide health care and deliver services in rural locations is an ongoing challenge5,6. One solution to help address these problems is the use of telehealth to provide health care at a distance. Telehealth is defined as 'the delivery of health care services, where distance is a critical factor, by health care professionals using information and communication technologies (ICT) for the exchange of valid information for diagnosis, treatment and prevention of disease and injuries, research and evaluation, and for the continuing education of health care providers, all in the interests of advancing the health of individuals and their communities'7. Telehealth services may be delivered using real-time (live) or store-and-forward techniques, such as videoconferencing and email respectively.
There is growing evidence, including many systematic reviews, to support the use of telehealth for patients and healthcare providers with outcomes: showing reduced length of stay; reduced demand on emergency services; improved access to health care; improved quality of services; improved clinical outcomes; decreased costs; reduced inconvenience; improved management of chronic and complex conditions; and provision of peer support, networking and education3,8,9. Despite the obvious benefits of telehealth, the actual uptake and integration of telehealth into mainstream practice has been slow and fragmented10-12. The scale and pace of adoption of telehealth has not developed as quickly as anticipated and many pilot programs have not migrated into sustained services13. The barriers and challenges associated with telehealth in Australia have been well described and include clinician preference for face-to-face consultations, ethico-legal concerns, change management practices, resources (including time), funding models, service coordination and administration personnel13-15. These observations are not limited to Australia. Internationally, the uptake of telehealth has not been consistent with the rapid advances in health and communication technologies and the subsequent opportunities to apply these in the context of service delivery at a distance16-18.
Recognising the potential of telehealth to support Australians living in rural and remote areas, the Australian Government in 2011 introduced an important policy on telehealth funding. This policy led to the introduction of specific funding opportunities through Medicare, Australia's publicly funded healthcare scheme. The Medicare Benefits Schedule (MBS) lists the scheduled fee for consultations, procedure and diagnostic tests that the government considers appropriate and that it reimburses to healthcare users or providers when that item is claimed19. The intention of the new Medicare funding items was to encourage the use of telehealth, to improve access to specialist health services for patients in remote areas and enhance engagement between clinicians working in rural areas and specialists in major cities. For example, with the introduction of new telehealth Medicare item numbers, a specialist medical practitioner who provides a consultation by videoconference could claim additional payment from Medicare of up to 50% of the standard scheduled fee for providing the consultation face-to-face. Similarly a general practitioner or nurse supporting the patient end of a video consultation can also claim payment through Medicare for the same consultation.
The Medicare telehealth items have created a much -needed incentive for clinicians to deliver telehealth, and from a national perspective telehealth activity is steadily increasing10. In response to these funding opportunities, many professional societies and colleges including the Australian College of Rural and Remote Medicine, the Royal Australasian College of Physicians, the Royal Australian College of General Practitioners and the Royal College of Nursing Australia have developed specific guidelines and standards to support the use of telehealth20-23. Currently, MBS items for telehealth are only available for real-time (video) consultations involving a medical specialist. Under certain conditions, reimbursement for medical officers, nurses and Aboriginal health workers is available if they accompany the patient during a telehealth consultation with a medical specialist19. However, funding opportunities for general medical and allied health practitioners for the provision of telehealth services are very limited or non-existent, as are funding opportunities for store-and-forward telehealth applications.
For telehealth to reach its full potential, it is important to not only understand the barriers and challenges, but also to identify the factors associated with successful services. Success of a service may be defined as the sustained integration of telehealth into routine clinical practice, which is unlikely to occur by good chance24. There are few opportunities to learn from other services with little systemic knowledge about the range of existing services in Australia. Identification of what services are available, in which locations, and what elements have contributed to their success may help develop appropriate policy directives and support other health services to better integrate telehealth into practice. Thus, the aim of this study was to synthesise the literature regarding telehealth services operating in rural and remote locations of Australia, and to identify the reported factors associated with success and sustainability.
We conducted a systematic review of the literature according to established methodology. The study protocol was registered with PROSPERO number CRD42015015090 and adheres to the PRISMA checklist for preferred reporting items in systematic reviews25. We undertook the review in five phases: planning, searching, screening, appraisal and synthesis.
Planning and searching
In the planning phase, the research team agreed upon the tasks and responsibilities of each researcher. The research questions were developed, revised and agreed upon as a team:
- What are the characteristics of the telehealth services available in rural and remote Australia?
- What methodologies have been used to evaluate these services?
- What are the facilitators or enablers of successful services?
- What other factors are associated with successful or sustainable services?
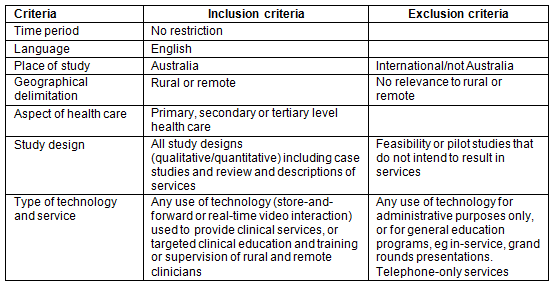
The search terms were developed with the research team and a university librarian scientist. A three-step search strategy was utilised. First, an initial limited search was undertaken of MEDLINE using the terms telemedicine AND 'rural Australia'. Analysis of text words contained in the resulting titles and abstracts, and of the index terms used to categorise the article, helped to inform the final search terms. The second step involved searching electronic databases with the search terms related to telemedicine or telehealth, rural and remote and Australia. The search was undertaken in November 2014 and updated in July 2015. We searched peer-reviewed electronic databases MEDLINE, Embase, CINAHL and sources of grey literature (Trove, Mednar, government and university websites) using the terms telehealth, telemedicine, video consultation, rural, remote, Australia as well as each state and territory in Australia. Terms were searched for as medical subject headings (MeSH), in titles or abstracts and with Boolean operators 'AND' and 'OR'. A snowballing strategy was used to identify other relevant articles in the retrieved articles reference lists. Articles were included if they met the criteria defined in Table 1.
The primary outcomes of interest for this review were the number, types and characteristics of telehealth services in rural Australia reported in the literature. Characteristics of services included the people, clinical aspects, location and purpose of the service.
Secondary outcomes of interests were: findings or important insights related to the success and sustainability of services,methods used to evaluate services, and outcomes that were measured, ie health-related outcomes (eg. quality of life, hospitalisation, clinical outcomes etc.); costs and resource utilisation; and process measures (eg. quality of care, adherence to standards, training and education and satisfaction). As satisfaction with processes is commonly measured, it was categorised separately.
Table 1: Study inclusion and exclusion criteria
Screening and appraisal phase
Two study authors (NB, LC) independently screened the titles and abstracts of all articles identified by the searches. Where there was any doubt, the article remained in the list for review by a third reviewer. At full text screening stage, one reviewer (NB) with content knowledge in the area reviewed the full text of each article and recorded a decision to include or exclude the article for full review and data extraction based on the inclusion/exclusion criteria and relevance to the research question. A second author (LC) reviewed the list of articles to be included and excluded and consensus was obtained. All articles that met the inclusion criteria were included in the review. Data extraction was undertaken systematically by one study author (NB) using a pre-specified list of variables and questions and was documented in a database developed for this study. The data extraction form was piloted on 10 articles and refined following discussion with all study authors. Extracted data included:
- author; year of publication; purpose of article (study, guideline, descriptive)
- geographical setting: rural; remote; state in Australia
- clinical specialty
- service details: purpose; clinicians; target clients; type of telehealth used
- methodological approach: data source; study design
- reported outcomes: categorised into health-related outcomes; costs; resource utilisation; process measures and satisfaction
- other outcomes: examples of evidence; study-author-identified facilitators of success; study-author-identified factors influencing sustainability.
A second reviewer (LC) completed independent data extraction for a random selection of 12 (10%) of articles. The results of data extraction by both reviewers were checked for accuracy, completeness and consensus. Discrepancies were resolved by discussion with all study authors. One reviewer (NB) appraised each article for the level of evidence according to the Joanna Briggs Institute (JBI) criteria26. The quality of each article was also appraised by the same reviewer using a modified tool developed for a systematic review of primary healthcare services in rural Australia5. The quality criteria assessed in this tool was deemed appropriate as it covered a range of important aspects pertaining to services rather than appraised the methodology used to evaluate services, and thus was relevant to the objectives of our review. Ten items were included; each item achieved scored 1 and items not achieved scored 0. Items included article informed by a literature review, explicit need for the service, transferability, clear aim, population representative of rural/remote, characteristics of service explained, methods accord with objectives, conclusions consistent with findings, limitations acknowledged. No articles were excluded on the basis of the level of evidence or quality assessment.
Synthesis phase
Data were categorised according to clinical speciality, discipline, geographical location and service details. Using an inductive approach, extracted data relating to the success or sustainability of services were grouped thematically to identify recurring elements in relation to the research questions. The research team met frequently to discuss consensus of findings. Data were synthesised into a narrative account summarising the overall evidence by comparing and contrasting the data.
Selection of articles
Searches identified 970 potentially eligible articles. A total of 116 articles published between 1988 and 2015 were included in the review. The results of the screening and selection processes are shown in Figure 1. The majority of excluded articles did not meet the inclusion criteria of reporting an Australian service. Other articles reported feasibility or pilot studies that were not intended as services and were also excluded.
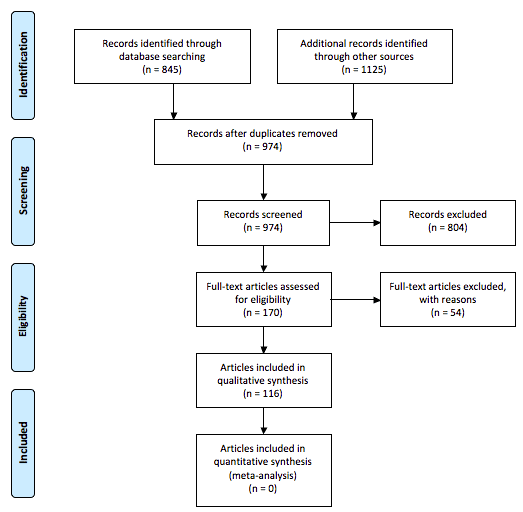 Figure 1: Flow chart of search strategy.
Figure 1: Flow chart of search strategy.
Characteristics of services
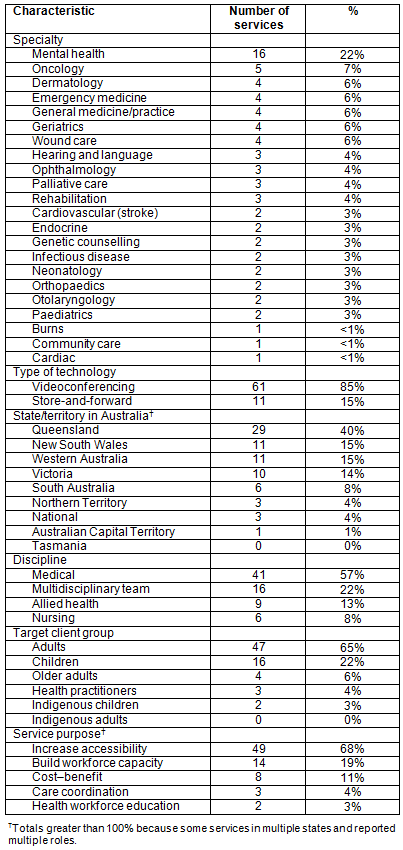
The 116 articles included in the review described 72 discrete telehealth services. Fifty-one services were reported individually and 21 in two or more papers each. Forty nine (68%) services operated from tertiary public hospitals into regional hospital facilities. The remainder of services were made up of either urban-based specialists (n=19, 26%), general practitioners (n=3, 4%) and community nurses (n=1, 4%) who provided telehealth to other locations including the patient's home. There has been a marked increase in the number of services reported over time (Fig2). The characteristics of the services were summarised and grouped into 22 different clinical specialities across Australia. The service purpose and discipline are described (Table 2). Full details of included articles can be found in the supplementary table, available in the online version of this article.
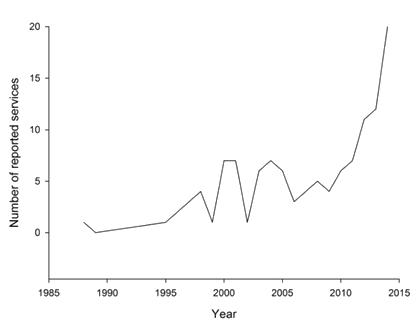 Figure 2: Number of reported Australian telehealth services over time
Table 2: Characteristics of Australian telehealth services (n=72)
Figure 2: Number of reported Australian telehealth services over time
Table 2: Characteristics of Australian telehealth services (n=72)
Methodologies used to report and evaluate services
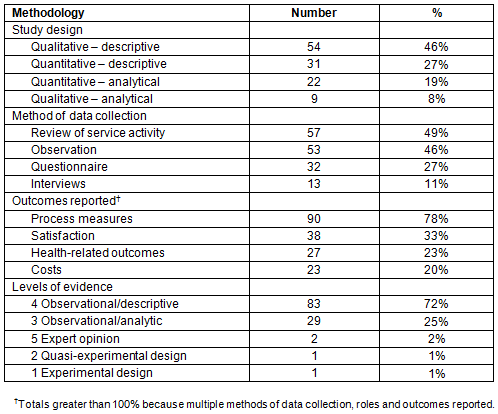
The methodologies used to report or evaluate services are summarised in Table 3. Further details of included articles are provided in Appendix I. Of the 116 articles included in this review, the majority were qualitative or quantitative descriptive accounts of services (n=85, 73%). These articles presented data or information regarding the service with little or no analysis. Half of the included articles presented a review of service activity (n=57, 49%), and used observational methods to document the processes used in the service. Use of interviews or questionnaires to collect data occurred in 13 (11%) and 32 (27%) articles. As such, most studies (n=83, 72%) were rated on the JBI level of evidence scale as a 4 (observational or descriptive studies)26. Two studies used an experimental or quasi-experimental design with a control group achieving a JBI level of evidence rating of rating of 1 or 2. The remainder undertook an analytical approach when describing or evaluating their service. A total of 22 (19%) studies used quantitative statistical methods in their analysis and 10 (8%) studies used qualitative analytical methods. Most articles (n=90, 78%) reported process measures related to the service, for example numbers of consultations, efficiency, technical skill or requirements. A large proportion of studies (n=38, 33%) measured either staff or patient satisfaction, with smaller numbers of studies reporting health-related outcomes (n=27, 23%), or costs (n=23, 20%).
Table 3: Methodologies used to report or evaluate Australian telehealth services
Factors influencing success and sustainability
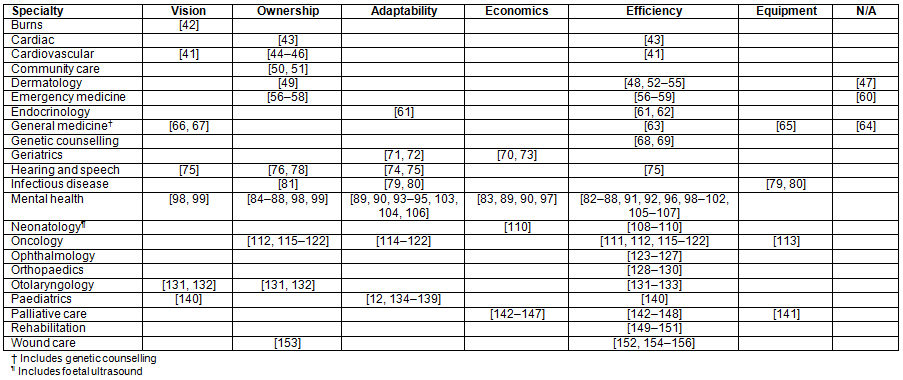
Factors influencing success and sustainability of services were identified from our analysis and grouped into six categories: vision, ownership, adaptability, economics, efficiency and equipment (Table 4). Services reported one or more of these factors being associated with the success and sustainability of the service (Table 5).
- Vision related to having a clear, realistic goal defining the purpose of the service.
- Ownership related to the clinical need, motivation and purposeful development of the service; success required both clinicians and management to be 'on board' and supportive of the initiative.
- Adaptability related to the recognition of the requirement to adapt the service model in response to the needs of patients, clinicians and health services, often going through several iterations before establishing a suitable model.
- Economics referred to the need for the service to offer value that was transparent, in terms of cost or time savings, with comparable clinical benefits to face-to-face services.
- Efficiency related to the development of procedures and processes. Successful and sustainable services did not always have high activity levels, but needed to be efficient with processes.
- Equipment related to consideration of infrastructure. Services did not require expensive equipment; many relied on low-cost alternatives. Services did however need to have processes in place to manage technical issues.
Table 4: Factors influencing success and sustainability of Australian telehealth services
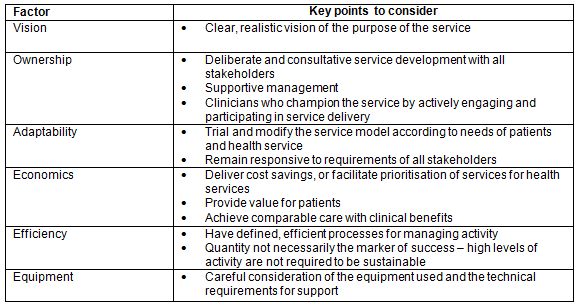 Table 5: Clinical specialties of Australian telehealth services and factors influencing success and sustainability27-142
Table 5: Clinical specialties of Australian telehealth services and factors influencing success and sustainability27-142
 Discussion
Discussion
In our systematic review, we identified a total of 72 telehealth services reported in 116 articles in the literature. The majority of the reported services involved the public health system. This is likely to reflect only a small proportion of the actual number of telehealth services in Australia, since many are not likely to have been published. Indeed, reports on government health websites indicate telehealth is a priority for all states in Australia, and work is being undertaken to integrate telehealth into mainstream practice143-149. Therefore, we can be confident that a broad variety of telehealth services exist and that successful implementation of telehealth services is possible. There are many examples of sustained services; however, as costs savings to the health system are as yet unproven, the sustainability of services is not assured.
The literature has highlighted numerous barriers and challenges to the uptake of telehealth services both in Australia and internationally13,24,150. Since there appears to be a positive growth in the amount of telehealth work being reported, it may be that some barriers are being overcome and more services are being developed and subsequently reported. In this review we found evidence of factors associated with successful and sustained telehealth services in Australia. These factors were distilled from the services reported and present a concise overview of areas to consider when developing services. Many factors are congruent with similar studies internationally151-153. However, our findings highlight the importance of adaptability and efficiency, which have not been reported previously. The need to adapt and modify the service model in response to need was a frequently reported factor for the success of services. Similarly, making a service more efficient by streamlining processes such as coordination of clinician time, room bookings, maintenance of equipment, sharing of test results and documentation, and troubleshooting technical problems, were also frequently reported as important factors for successful services.
Funding models to support clinicians who provide telehealth services are an important consideration for the government and health services. As the cost of travelling to access health care is often borne by the patient, the impetus of services to use telehealth as an alternative is reduced. Also, there is no clear understanding of the cost shifting involved in undertaking telehealth in the public hospital system. For telehealth to become integrated into the health system there needs to be a clear understanding of how services are funded, from what budget source, where the savings are generated, and how they are distributed back into the health system. We found a considerable number of services provided by allied health and multidisciplinary teams that are not eligible for MBS reimbursement. These services are likely to be operating within public hospitals or obtaining a fee for service in private practices. For providers charging a fee for service, review of MBS item numbers to support their services may be warranted. Incorporating the findings from this review will be an important 'evidence into policy' initiative for health services and governments to consider.
Concerns within government, health services and industry that telehealth is not being used to its full potential still remain11,154. In 2014, the Queensland Parliament reported on an inquiry into telehealth services - to appraise a $31 million investment into telehealth services in Queensland155. One of the findings in the report was the need for a more deliberate approach to planning the implementation of telehealth. According to the report, a more common understanding of plans to increase the use of telehealth was needed within the health service to promote telehealth adoption as well as greater collaborations between health services so that best practice approaches and lessons learnt were more accessible155.
The intention of this review was to identify telehealth services in Australia. Our focus was not on the critique of methodological quality of articles. In this review, the majority (86, 73%) of studies found were descriptive reports. The majority of outcomes reported were process measures such as patient or clinician satisfaction rather than specific clinical outcomes or economic measures. Whilst process measures are important for demonstrating feasibility and factors associated with service development, specific clinical outcomes and cost measures are likely to have an important influence on the justification and uptake of telehealth24,156.
Telehealth services are primarily intended to improve access to services by reducing the need to travel, both for the patient and the clinician. Other common reasons for telehealth services include cost efficiencies related to the service, improved processes, improved clinical outcomes and education for healthcare clinicians4. Thus, these are the appropriate outcomes to measure and report for the evaluation of services. In our review we also identified additional roles of services including capacity building and care coordination. These could be considered other aspects to measure in service reports or evaluations. It is important that effort is extended to ensure the evidence regarding telehealth is strengthened by including well-defined outcome measures that are able to inform clinicians, health services and policy makers of both the direct and indirect benefits that telehealth can achieve.
Limitations
There may be other factors reported in the literature regarding success and sustainability of services that were not identified in this review. Additionally, there may be other reported services that we did not identify, despite our search strategy being comprehensive and covering a broad range of services across Australia. Data extraction was complicated by the variety of methodologies and reporting styles used. In this study, the data extracted relating to the success or sustainability of services was not generally presented in the results section but was integrated into discussion.
Telehealth has the potential to address many of the key challenges to providing health in Australia, with its substantial land area and widely dispersed population. We identified a wide variety of telehealth services being provided in rural and remote areas of Australia. There is great potential to increase this number by scaling up and replicating successful services. Consideration of the factors associated with the success and sustainability should be an integral part of developing services. This review identified factors associated with successful and sustainable telehealth services in rural and remote areas of Australia. Many of these have been previously reported. However, the success factors of adaptability and efficiency were newly identified by this review.
References
1. World Bank. Population density. (Internet) 2015. Available: http://data.worldbank.org/indicator/EN.POP.DNST (Accessed 25 February 2015).
2. Australian Bureau of Statistics. Regional population growth, Australia 2012-13. (Internet) 2014. Available: http://www.abs.gov.au/ausstats/abs@.nsf/Products/3218.0~2012-13~Main+Features~Main+Features?OpenDocument - PARALINK0 (Accessed 25 February 2015).
3. Wakerman J, Humphreys JS. Sustainable primary health care services in rural and remote areas: innovation and evidence. The Australian Journal of Rural Health 2011; 19(3): 118-124. http://dx.doi.org/10.1111/j.1440-1584.2010.01180.x
4. Department of Health and Ageing. Rural and Regional Health Australia: National strategic framework for rural and remote health. (Internet) 2015. Available: http://www.ruralhealthaustralia.gov.au/internet/rha/publishing.nsf/Content/NSFRRH-homepage (Accessed 25 February 2015).
5. Wakerman J, Humphreys J, Wells R, Kuipers P, Entwistle P, Jones J. A systematic review of primary health care delivery models in rural and remote Australia 1993-2006. Melbourne: Monash University, 2006.
6. Wakerman J, Humphreys JS. Sustainable primary health care services in rural and remote areas: innovation and evidence. The Australian Journal of Rural Health 2011; 19: 118-124. http://dx.doi.org/10.1111/j.1440-1584.2010.01180.x
7. World Health Organization. Telemedicine: opportunities and developments in Member States. Geneva: WHO, 2009.
8. Moffatt JJ, Eley DS. The reported benefits of telehealth for rural Australians. Australian Health Review 2010; 34(3): 276-281. http://dx.doi.org/10.1071/AH09794
9. Wootton R. Twenty years of telemedicine in chronic disease management - an evidence synthesis. Journal of Telemedicine and Telecare 2012; 18(4): 211-220. http://dx.doi.org/10.1258/jtt.2012.120219
10. Wade V, Soar J, Gray L. Uptake of telehealth services funded by Medicare in Australia. Australian Health Review: a publication of the Australian Hospital Association 2014; 38(5): 528-532. http://dx.doi.org/10.1071/AH14090
11. Department of Health. Connecting health services with the future: moderinising medicare by providing rebates for online consultations. (Internet) 2011. Available: http://www.mbsonline.gov.au/internet/mbsonline/publishing.nsf/Content/connectinghealthservices-techandclinical (Accessed 28 September 2016).
12. Smith AC, Gray LC. Telemedicine across the ages. The Medical Journal of Australia 2009; 190(1): 15-19.
13. Wade V, Eliott J. The role of the champion in telehealth service development: a qualitative analysis. Journal of Telemedicine and Telecare 2012; 18(8): 490-492. http://dx.doi.org/10.1258/jtt.2012.GTH115
14. Wade VA, Eliott JA, Hiller JE. A qualitative study of ethical, medico-legal and clinical governance matters in Australian telehealth services. Journal of Telemedicine and Telecare 2012; 18(2): 109-114. http://dx.doi.org/10.1258/jtt.2011.110808
15. Moffatt JJ, Eley DS. Barriers to the up-take of telemedicine in Australia - a view from providers. Rural and Remote Health (Internet) 2011; 11(2): 1581. Available: www.rrh.org.au (Accessed 28 September).
16. Adler-Milstein J, Kvedar J, Bates DW. Telehealth among US hospitals: several factors, including state reimbursement and licensure policies, influence adoption. Health Affairs 2014; 33(2): 207-215. http://dx.doi.org/10.1377/hlthaff.2013.1054
17. Greenhalgh T, Procter R, Wherton J, Sugarhood P, Shaw S. The organising vision for telehealth and telecare: discourse analysis. British Medical Journal Open 2012; 2(4): e001574. http://dx.doi.org/10.1136/bmjopen-2012-001574
18. Taylor J, Coates E, Brewster L, Mountain G, Wessels B, Hawley MS. Examining the use of telehealth in community nursing: identifying the factors affecting frontline staff acceptance and telehealth adoption. Journal of Advanced Nursing 2015; 71(2): 326-337. http://dx.doi.org/10.1111/jan.12480
19. Australian Government. Telehealth: specialist video consultations under Medicare. (Internet) 2014. Available: http://www.mbsonline.gov.au/telehealth (Accessed 30 August 2015).
20. Australian College of Rural and Remote Medicine. National eHealth program - telehealth. (Internet) 2015. Available: http://www.ehealth.acrrm.org.au/ (Accessed 30 August 2015).
21. Australian Nursing and Midwifery Federation. Telehealth professional practice standards and guidelines for nursing and midwifery. (Internet) 2014. Available: http://anmf.org.au/pages/telehealth (Accessed 30 August 2015).
22. Royal Australasian College of Physicians. Guidelines and practical tips. (Internet) 2013. Available: https://www.racp.edu.au/docs/default-source/advocacy-library/telehealth-guidelines-and-practical-tips.pdf (Accessed 28 September 2016).
23. Royal Australian College of General Practitioners. Your practice. (Internet) 2015. Available: http://www.racgp.org.au/your-practice/ehealth/telehealth/ (Accessed 30 August 2015).
24. Armfield NR, Edirippulige SK, Bradford N, Smith AC. Telemedicine - is the cart being put before the horse. The Medical Journal of Australia 2014; 200(9): 530-533. http://dx.doi.org/10.5694/mja13.11101
25. Moher D, Liberati A, Tetzlaff J, Altman DG. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Annals of Internal Medicine 2009; 151(4): 264-269. http://dx.doi.org/10.7326/0003-4819-151-4-200908180-00135
26. Joanna Briggs Institute and University of Adelaide. New JBI levels of evidence. (Internet) 2014. Available: http://joannabriggs.org/assets/docs/approach/JBI-Levels-of-evidence_2014.pdf (Accessed 30 August 2015).
27. Jordan LA, Sewell C, Rudd J, Evans M, Kerr E, Nieass J, et al. Rural tele-thrombolysis protocol implementation: nurses leading change. International Journal of Stroke 2014; 9: 5-6.
28. Smith AC, Youngberry K, Mill J, Kimble R, Wootton R. A review of three years experience using email and videoconferencing for the delivery of post-acute burns care to children in Queensland. Burns 2004; 30(3): 248-252. http://dx.doi.org/10.1016/j.burns.2003.11.003
29. Justo R, Smith AC, Williams M, Van der Westhuyzen J, Murray J, Sciuto G, et al. Paediatric telecardiology services in Queensland: a review of three years' experience. Journal of Telemedicine and Telecare 2004; 10(Suppl 1): 57-60. http://dx.doi.org/10.1258/1357633042614258
30. Nagao KJ, Koschel A, Haines HM, Bolitho LE, Yan B. Rural Victorian Telestroke project. Internal Medicine Journal 2012; 42(10): 1088-1095. http://dx.doi.org/10.1111/j.1445-5994.2011.02603.x
31. Cadilhac DA, Vu M, Bladin C. Experience with scaling up the Victorian Stroke Telemedicine programme. Journal of Telemedicine and Telecare 2014; 20(7): 413-418. http://dx.doi.org/10.1177/1357633X14552389
32. Cadilhac D, Moloczij N, Bladin C, Kung F, Kilkenny M, Ermel S. Update on the Victorian Stroke Telemedicine (VST) project. International Journal of Stroke 2014; 9: 4.
33. See A, Lim AC, Le K, See J-A, Shumack SP. Operational teledermatology in Broken Hill, rural Australia. The Australasian Journal of Dermatology 2005; 46(3): 144-149. http://dx.doi.org/10.1111/j.1440-0960.2005.00166.x
34. Biscak TM, Eley R, Manoharan S, Sinnott M, Soyer HP. Audit of a state-wide store and forward teledermatology service in Australia. Journal of Telemedicine and Telecare 2013; 19(7): 362-366. http://dx.doi.org/10.1177/1357633X13506509
35. Hockey AD, Wootton R, Casey T. Trial of low-cost teledermatology in primary care. Journal of Telemedicine and Telecare 2004; 10(Suppl 1): 44-47. http://dx.doi.org/10.1258/1357633042614221
36. Van Ast P. Supporting community carers via videoconferencing. Journal of Telemedicine and Telecare 2005; 11(Suppl 2): S96-97. http://dx.doi.org/10.1258/135763305775124713
37. Van Ast P, Larson A. Supporting rural carers through telehealth. Rural and Remote Health (Internet) 2007; 7(1): 634. Available: www.rrh.org.au (Accessed 28 September 2016).
38. Australian College of Rural and Remote Medicine: Tele-Derm goes national. Australian Journal of Rural Health 2005; 13(3): 200. http://dx.doi.org/10.1111/j.1440-1854.2005.00696.x
39. Ou MH, West GA, Lazarescu M, Clay CD. Evaluation of Telederm for dermatological services in rural and remote areas. Artificial Intelligence in Medicine 2008; 44(1): 27-40. http://dx.doi.org/10.1016/j.artmed.2008.04.006
40. Muir J, Lucas L. Tele-dermatology in Australia. Studies in Health Technology and Informatics 2008; 131: 245-253.
41. Muir J. Telehealth: the specialist perspective. Australian Family Physician 2014; 43(12): 828-830.
42. Sweetman G, Brazil V. Education links between the Australian rural and tertiary emergency departments: videoconference can support a virtual learning community. Emergency Medicine Australasia 2007; 19(2): 176-177. http://dx.doi.org/10.1111/j.1742-6723.2007.00951.x
43. Sharpe K, Elcock M, Aitken P, Furyk J. The use of telehealth to assist remote hospital resuscitation and aeromedical retrieval tasking: a 12-month case review. Journal of Telemedicine and Telecare 2012; 18(5): 260-266. http://dx.doi.org/10.1258/jtt.2011.110906
44. Mathews KA, Elcock MS, Furyk JS. The use of telemedicine to aid in assessing patients prior to aeromedical retrieval to a tertiary referral centre. Journal of Telemedicine and Telecare 2008; 14(6): 309-314. http://dx.doi.org/10.1258/jtt.2008.080417
45. Desai S, Williams ML, Smith AC. Teleconsultation from a secondary hospital for paediatric emergencies occurring at rural hospitals in Queensland. Journal of Telemedicine and Telecare 2013; 19(7): 405-410. http://dx.doi.org/10.1177/1357633X13506528
46. Herrington G, Zardins Y, Hamilton A. A pilot trial of emergency telemedicine in regional Western Australia. Journal of Telemedicine and Telecare 2013; 19(7): 430-433. http://dx.doi.org/10.1177/1357633X13506531
47. Smith AC, Batch J, Lang E, Wootton R. The use of online health techniques to assist with the delivery of specialist paediatric diabetes services in Queensland. Journal of Telemedicine and Telecare 2003; 9(Suppl 2): S54-57. http://dx.doi.org/10.1258/135763303322596273
48. Fatehi F, Gray LC, Russell AW. Telemedicine for clinical management of diabetes - a process analysis of video consultations. Journal of Telemedicine and Telecare 2013; 19(7): 379-382. http://dx.doi.org/10.1177/1357633X13506524
49. Mitchell JG, Disney AP. Clinical applications of renal telemedicine. Journal of Telemedicine and Telecare 1997; 3(3): 158-162. http://dx.doi.org/10.1258/1357633971931075
50. Mitchell L, Schultz K, Clark D, Wilson JW. Telemedicine videoconferencing - breaking down the barriers for cystic fibrosis (CF) patients living in rural and remote areas. Journal of Cystic Fibrosis 2014; 13: S105. http://dx.doi.org/10.1016/S1569-1993(14)60363-5
51. Bowater M. The experience of a rural general practitioner using videoconferencing for telemedicine. Journal of Telemedicine and Telecare 2001; 7(Suppl 2): 24-25. http://dx.doi.org/10.1258/1357633011937038
52. Dillon E, Loermans J. Telehealth in Western Australia: the challenge of evaluation. Journal of Telemedicine and Telecare 2003; 9(Suppl 2): S15-19. http://dx.doi.org/10.1258/135763303322596147
53. Dillon E, Loermans J, Davis D, Xu C. Evaluation of the Western Australian Department of Health telehealth project. Journal of Telemedicine and Telecare 2005; 11(Suppl 2): S19-21. http://dx.doi.org/10.1258/135763305775124803
54. Zilliacus E, Meiser B, Lobb E, Dudding TE, Barlow-Stewart K, Tucker K. The virtual consultation: practitioners' experiences of genetic counseling by videoconferencing in Australia. Telemedicine Journal and e-Health 2010; 16(3): 350-357. http://dx.doi.org/10.1089/tmj.2009.0108
55. Hopper B, Buckman M, Edwards M. Evaluation of satisfaction of parents with the use of videoconferencing for a pediatric genetic consultation. Twin Research and Human Genetics 2011; 14(4): 343-346. http://dx.doi.org/10.1375/twin.14.4.343
56. Comans TA, Martin-Khan M, Gray LC, Scuffham PA. A break-even analysis of delivering a memory clinic by videoconferencing. Journal of Telemedicine and Telecare 2013; 19(7): 393-396. http://dx.doi.org/10.1177/1357633X13506532
57. Gray LC, Wright OR, Cutler AJ, Scuffham PA, Wootton R. Geriatric ward rounds by video conference: a solution for rural hospitals. The Medical Journal of Australia 2009; 191(11-12): 605-608.
58. Royal District Nursing Service. Telehealth tackles elderly health care. Australian Nursing Journal 2013; 21(1): 41.
59. Saligari J, Flicker L, Loh PK, Maher S, Ramesh P, Goldswain P. The clinical achievements of a geriatric telehealth project in its first year. Journal of Telemedicine and Telecare 2002; 8(Suppl 3): S53-55. http://dx.doi.org/10.1258/13576330260440862
60. McCarthy M, Duncan J, Leigh G. Telepractice: the Australian experience in an international context. Volta Review 2012; 112(3): 297-312.
61. Burns CL, Ward EC, Hill AJ, Malcolm K, Bassett L, Kenny LM, et al. A pilot trial of a speech pathology telehealth service for head and neck cancer patients. Journal of Telemedicine and Telecare 2012; 18(8): 443-446. http://dx.doi.org/10.1258/jtt.2012.GTH104
62. Unknown. New telehealth services for children in regional and remote areas. Australian Occupational Therapy Journal 2013: 16.
63. Constantinescu G. Satisfaction with telemedicine for teaching listening and spoken language to children with hearing loss. Journal of Telemedicine and Telecare 2012; 18(5): 267-272. http://dx.doi.org/10.1258/jtt.2012.111208
64. Davis A, Hopkins T, Abrahams Y. Maximizing the impact of telepractice through a multifaceted service delivery model at the Shepherd Centre, Australia. Volta Review 2012; 112(3): 383-391.
65. Schulz TR, Richards M, Gasko H, Lohrey J, Hibbert ME, Biggs BA. Telehealth: experience of the first 120 consultations delivered from a new refugee telehealth clinic. Internal Medicine Journal 2014; 44(10): 981-985. http://dx.doi.org/10.1111/imj.12537
66. Schulz TR, Leder K, Akinci I, Biggs BA. Improvements in patient care: videoconferencing to improve access to interpreters during clinical consultations for refugee and immigrant patients. Australian Health Review 2015; 39(4): 395-399. http://dx.doi.org/10.1071/ah14124
67. Nazareth S, Kontorinis N, Muwanwella N, Hamilton A, Leembruggen N, Cheng WS. Successful treatment of patients with hepatitis C in rural and remote Western Australia via telehealth. Journal of Telemedicine and Telecare 2013; 19(2): 101-106. http://dx.doi.org/10.1258/jtt.2012.120612
68. Greenwood J, Chamberlain C, Parker G. Evaluation of a rural telepsychiatry service. Australasian Psychiatry 2004; 12(3): 268-272. http://dx.doi.org/10.1111/j.1039-8562.2004.02097.x
69. Buckley D, Weisser S. Videoconferencing could reduce the number of mental health patients transferred from outlying facilities to a regional mental health unit. Australian and New Zealand Journal of Public Health 2012; 36(5): 478-482. http://dx.doi.org/10.1111/j.1753-6405.2012.00915.x
70. Saurman E, Johnston J, Hindman J, Kirby S, Lyle D. A transferable telepsychiatry model for improving access to emergency mental health care. Journal of Telemedicine and Telecare 2014; 20(7): 391-399. http://dx.doi.org/10.1177/1357633X14552372
71. Saurman E, Lyle D, Kirby S, Roberts R. Use of a mental health emergency care - rural access programme in emergency departments. Journal of Telemedicine and Telecare 2014; 20(6): 324-329. http://dx.doi.org/10.1177/1357633X14544422
72. Saurman E, Lyle D, Kirby S, Roberts R. Assessing program efficiency: a time and motion study of the mental health emergency care - rural access program in NSW, Australia. International Journal of Environmental Research and Public Health 2014; 11(8): 7678-7689. http://dx.doi.org/10.3390/ijerph110807678
73. Saurman E, Lyle D, Perkins D, Roberts R. Successful provision of emergency mental health care to rural and remote New South Wales: an evaluation of the Mental Health Emergency Care - Rural Access Program. Australian Health Review 2014; 38(1): 58-64. http://dx.doi.org/10.1071/AH13050
74. Saurman E, Perkins D, Roberts R, Roberts A, Patfield M, Lyle D. Responding to mental health emergencies: implementation of an innovative telehealth service in rural and remote New South Wales, Australia. Journal of Emergency Nursing 2011; 37(5): 453-459. http://dx.doi.org/10.1016/j.jen.2010.11.005
75. Dossetor DR, Nunn, KP, Fairley M, Eggleton D. A child and adolescent psychiatric outreach service for rural New South Wales: a telemedicine pilot study. Journal of Paediatrics and Child Health 1999; 35(6): 525-529. http://dx.doi.org/10.1046/j.1440-1754.1999.00410.x
76. Kopel H, Nunn K, Dossetor, D. Evaluating satisfaction with a child and adolescent psychological telemedicine outreach service. Journal of Telemedicine and Telecare 2001; 7(Suppl 2): 35-40. http://dx.doi.org/10.1258/1357633011937074
77. Clarke PH. A referrer and patient evaluation of a telepsychiatry consultation-liaison service in South Australia. Journal of Telemedicine and Telecare 1997; 3(Suppl 1): 12-14. http://dx.doi.org/10.1258/1357633971930788
78. D'Souza R. Telemedicine for intensive support of psychiatric inpatients admitted to local hospitals. Journal of Telemedicine and Telecare 2000; 6(Suppl 1): S26-28. http://dx.doi.org/10.1258/1357633001934834
79. Kavanagh S, Hawker F. The fall and rise of the South Australian telepsychiatry network. Journal of Telemedicine and Telecare 2001; 7(Suppl 2): 41-43. http://dx.doi.org/10.1258/1357633011937083
80. Kavanagh SJ, Yellowlees PM. Telemedicine - clinical applications in mental health. Australian Family Physician 1995; 24(7): 1242-1247.
81. Hawker F, Kavanagh S, Yellowlees P, Kalucy RS. Telepsychiatry in South Australia. Journal of Telemedicine and Telecare 1998; 4(4): 187-194. http://dx.doi.org/10.1258/1357633981932181
82. Griffiths L, Blignault I, Yellowlees P. Telemedicine as a means of delivering cognitive-behavioural therapy to rural and remote mental health clients. Journal of Telemedicine and Telecare 2006; 12(3): 136-140. http://dx.doi.org/10.1258/135763306776738567
83. Trott P, Blignault I. Cost evaluation of a telepsychiatry service in northern Queensland. Journal of Telemedicine and Telecare 1998; 4(Suppl 1): 66-68. http://dx.doi.org/10.1258/1357633981931515
84. Wood J, Stathis S, Smith A, Krause J. E-CYMHS: an expansion of a child and youth telepsychiatry model in Queensland. Australasian Psychiatry 2012; 20(4): 333-337. http://dx.doi.org/10.1177/1039856212450756
85. Ryan V-n, Stathis S, Smith AC, Best D, Wootton R. Telemedicine for rural and remote child and youth mental health services. Journal of Telemedicine and Telecare 2005; 11(Suppl 2): S76-78. http://dx.doi.org/10.1258/135763305775124902
86. Gelber H. The experience of the Royal Children's Hospital Mental Health Service videoconferencing project. Journal of Telemedicine and Telecare 1998; 4(Suppl 1): 71-73. http://dx.doi.org/10.1258/1357633981931542
87. Gelber H. The experience in Victoria with telepsychiatry for the child and adolescent mental health service. Journal of Telemedicine and Telecare 2001; 7(Suppl 2): 32-34. http://dx.doi.org/10.1258/1357633011937065
88. Buist A, Coman G, Silvas A, Burrows G. An evaluation of the telepsychiatry programme in Victoria, Australia. Journal of Telemedicine and Telecare 2000; 6(4): 216-221. http://dx.doi.org/10.1258/1357633001935383
89. Kennedy C, Yellowlees P. A community-based approach to evaluation of health outcomes and costs for telepsychiatry in a rural population: preliminary results. Journal of Telemedicine and Telecare 2000; 6(Suppl 1): S155-157. http://dx.doi.org/10.1258/1357633001934492
90. Kennedy C, Yellowlees P. The effectiveness of telepsychiatry measured using the Health of the Nation Outcome Scale and the Mental Health Inventory. Journal of Telemedicine and Telecare 2003; 9(1): 12-16. http://dx.doi.org/10.1258/135763303321159639
91. Hockey AD, Yellowlees PM, Murphy S. Evaluation of a pilot second-opinion child telepsychiatry service. Journal of Telemedicine and Telecare 2004; 10(Suppl 1): 48-50. http://dx.doi.org/10.1258/1357633042614186
92. Rees CS, Krabbe M, Monaghan BJ. Education in research findings from haematology patients in regional, rural and remote Queensland. The patient - cognitive-behavioural therapy for mental health professionals. Journal of Telemedicine and Telecare 2009; 15(2): 59-63. http://dx.doi.org/10.1258/jtt.2008.008005
93. Lessing K, Blignault I. Mental health telemedicine programmes in Australia. Journal of Telemedicine and Telecare 2001; 7(6): 317-323. http://dx.doi.org/10.1258/1357633011936949
94. Chan FY, Soong B, Lessing K, Watson D, Cincotta R, Baker S, et al. Clinical value of real-time tertiary fetal ultrasound consultation by telemedicine: preliminary evaluation. Telemedicine Journal 2000; 6(2): 237-242. http://dx.doi.org/10.1089/107830200415171
95. Chan FY, Soong B, Watson D, Whitehall J. Realtime fetal ultrasound by telemedicine in Queensland. A successful venture? Journal of Telemedicine and Telecare 2001; 7(Suppl 2): 7-11. http://dx.doi.org/10.1258/1357633011937290
96. Whitehall J, Blignault I, French C, Carson V, Patole S. Telemedicine in neonatology: lessons from North Queensland. The Australian Journal of Rural Health 1998; 6(3): 140-143. http://dx.doi.org/10.1111/j.1440-1584.1998.tb00300.x
97. Rutherford J, O'Sullivan R. Is there a role for telehealth in gynaeoncology? The experiences at John Hunter hospital Newcastle. International Journal of Gynecological Cancer 2014; 24(9): 1145.
98. George M, Ngo P, Prawira A. Rural oncology: overcoming the tyranny of distance for improved cancer care. Journal of Oncology Practice 2014; 10(3): e146-149. http://dx.doi.org/10.1200/JOP.2013.001228
99. Olver IN, Selva-Nayagam S. Evaluation of a telemedicine link between Darwin and Adelaide to facilitate cancer management. Telemedicine Journal 2000; 6(2): 213-218. http://dx.doi.org/10.1089/107830200415144
100. McGrath P. Technology-based patient consultations: research findings from haematology patients in regional, rural and remote Queensland. Patient-Centered Outcomes Research 2015; 8(2): 199-206.
101. Mooi JK, Whop LJ, Valery PC, Sabesan SS. Teleoncology for Indigenous patients: the responses of patients and health workers. Australian Journal of Rural Health. 2012; 20(5): 265-269. http://dx.doi.org/10.1111/j.1440-1584.2012.01302.x
102. Sabesan S, Kelly J. Are teleoncology models merely about avoiding long distance travel for patients? European Journal of Cancer Care 2014; 23(6): 745-749. http://dx.doi.org/10.1111/ecc.12251
103. Sabesan S, Kelly J, Evans R, Larkins S. A tele-oncology model replacing face-to-face specialist cancer care: perspectives of patients in North Queensland. Journal of Telemedicine and Telecare 2014; 20(4): 207-211. http://dx.doi.org/10.1177/1357633X14529237
104. Sabesan S, Larkins S, Evans R, Varma S, Andrews A, Beuttner P, et al. Telemedicine for rural cancer care in North Queensland: bringing cancer care home. Australian Journal of Rural Health 2012; 20(5): 259-264. http://dx.doi.org/10.1111/j.1440-1584.2012.01299.x
105. Sabesan S, Simcox K, Marr I. Medical oncology clinics through videoconferencing: an acceptable telehealth model for rural patients and health workers. Internal Medicine Journal 2012; 42(7): 780-785. http://dx.doi.org/10.1111/j.1445-5994.2011.02537.x
106. Thaker DA, Monypenny R, Olver I, Sabesan S. Cost savings from a telemedicine model of care in northern Queensland, Australia. The Medical Journal of Australia 2013; 199(6): 414-417. http://dx.doi.org/10.5694/mja12.11781
107. Sabesan S, Roberts LJ, Aiken P, Joshi A, Larkins S. Timely access to specialist medical oncology services closer to home for rural patients: experience from the Townsville Teleoncology Model. Australian Journal of Rural Health 2014; 22(4): 156-159. http://dx.doi.org/10.1111/ajr.12101
108. Sabesan S. Specialist cancer care through telehealth models. The Australian Journal of Rural Health 2015; 23(1): 19-23. http://dx.doi.org/10.1111/ajr.12170
109. Rosengren D, Blackwell N, Kelly G, Lenton L, Glastonbury J. The use of telemedicine to treat ophthalmological emergencies in rural Australia. Journal of Telemedicine and Telecare 1998; 4(Suppl 1): 97-99. http://dx.doi.org/10.1258/1357633981931650
110. Blackwell NA, Kelly GJ, Lenton LM. Telemedicine ophthalmology consultation in remote Queensland. The Medical Journal of Australia 1997; 167(11-12): 583-586.
111. Kumar S, Yogesan K, Hudson B, Tay-Kearney ML, Constable IJ. Emergency eye care in rural Australia: role of internet. Eye 2006; 20(12): 1342-1344. http://dx.doi.org/10.1038/sj.eye.6702104
112. Kumar S, Tay-Kearney ML, Chaves F, Constable IJ, Yogesan K. Remote ophthalmology services: cost comparison of telemedicine and alternative service delivery options. Journal of Telemedicine and Telecare 2006; 12(1): 19-22. http://dx.doi.org/10.1258/135763306775321399
113. Johnson KA, Meyer J, Yazar S, Turner AW. Real-time teleophthalmology in rural Western Australia. The Australian Journal of Rural Health 2015; 23(3): 142-149. http://dx.doi.org/10.1111/ajr.12150
114. Rowell PD, Pincus P, White M, Smith AC. Telehealth in paediatric orthopaedic surgery in Queensland: a 10-year review. Australian and New Zealand Journal of Surgery 2014; 84(12): 955-959. http://dx.doi.org/10.1111/ans.12753
115. McGill A, North J. An analysis of an ongoing trial of rural videoconference fracture clinics. Journal of Telemedicine and Telecare 2012; 18(8): 470-472. http://dx.doi.org/10.1258/jtt.2012.GTH110
116. McGill AF, North JB. Teleconference fracture clinics: a trial for rural hospitals. Australian and New Zealand Journal of Surgery 2012; 82(1-2): 2-3. http://dx.doi.org/10.1111/j.1445-2197.2011.05952.x
117. Smith AC, Williams J, Agnew J, Sinclair S, Youngberry K, Wootton R. Realtime telemedicine for paediatric otolaryngology pre-admission screening. Journal of Telemedicine and Telecare 2005; 11(Suppl 2): S86-89. http://dx.doi.org/10.1258/135763305775124821
118. Smith AC, Armfield NR, Wu W-I, Brown CA, Mickan B, Perry C. Changes in paediatric hospital ENT service utilisation following the implementation of a mobile, indigenous health screening service. Journal of Telemedicine and Telecare 2013; 19(7): 397-400. http://dx.doi.org/10.1177/1357633X13506526
119. Reeve C, Thomas A, Mossenson A, Reeve D, Davis S. Evaluation of an ear health pathway in remote communities: improvements in ear health access. Australian Journal of Rural Health 2014; 22(3): 127-132. http://dx.doi.org/10.1111/ajr.12098
120. Smith AC. Telepaediatrics. Journal of Telemedicine and Telecare 2007; 13(4): 163-166. http://dx.doi.org/10.1258/135763307780908021
121. Smith AC, Bensink M, Armfield N, Stillman J, Caffery L. Telemedicine and rural health care applications. Journal of Postgraduate Medicine 2005; 51(4): 286-293.
122. Smith AC, Scuffham P, Wootton R. The costs and potential savings of a novel telepaediatric service in Queensland. BMC Health Services Research 2007; 7: 35. http://dx.doi.org/10.1186/1472-6963-7-35
123. Smith AC, Youngberry K, Christie F, Isles A, McCrossin R, Williams M, et al. The family costs of attending hospital outpatient appointments via videoconference and in person. Journal of Telemedicine and Telecare. 2003; 9(Suppl 2): S58-61. http://dx.doi.org/10.1258/135763303322596282
124. Smith AC, Armfield NR, White MM, Williams ML, Koh TH, Hurley T, et al. Clinical services and professional support: a review of mobile telepaediatric services in Queensland. Studies in Health Technology and Informatics 2010; 161: 149-158.
125. Smith AC, Coulthard M, Clark R, Armfield N, Taylor S, Goff R, et al. Wireless telemedicine for the delivery of specialist paediatric services to the bedside. Journal of Telemedicine and Telecare 2005; 11(Suppl 2): S81-85. http://dx.doi.org/10.1258/135763305775124669
126. Jury SC, Walker AM, Kornberg AJ. The introduction of web-based video-consultation in a paediatric acute care setting. Journal of Telemedicine and Telecare 2013; 19(7): 383-387. http://dx.doi.org/10.1177/1357633X13506530
127. Olver I, Brooksbank M, Champion N, Keeley J. The use of videophones to enhance palliative care outreach nursing in remote areas. Progress in Palliative Care 2005; 13(5): 263-267. http://dx.doi.org/10.1179/096992605X57679
128. Bensink ME, Armfield NR, Pinkerton R, Irving H, Hallahan AR, Theodoros DG, et al. Using videotelephony to support paediatric oncology-related palliative care in the home: from abandoned RCT to acceptability study. Palliative Medicine 2009; 23(3): 228-237. http://dx.doi.org/10.1177/0269216308100251
129. Herbert A, Bradford N, Donovan L, Pedersen L-A, Irving H. Development of a state-wide pediatric palliative care service in Australia: referral and outcomes over two years. Journal of Palliative Medicine 2014; 17(3): 288-295. http://dx.doi.org/10.1089/jpm.2013.0400
130. Bradford N, Young J, Armfield NR, Bensink ME, Pedersen LA, Herbert A, et al. A pilot study of the effectiveness of home teleconsultations in paediatric palliative care. Journal of Telemedicine and Telecare 2012; 18(8): 438-442. http://dx.doi.org/10.1258/jtt.2012.GTH103
131. Bradford NK, Armfield NR, Young J, Smith AC. Paediatric palliative care by video consultation at home: a cost minimisation analysis. BMC Health Services Research 2014; 14: 328. http://dx.doi.org/10.1186/1472-6963-14-328
132. Bradford NK, Young J, Armfield NR, Herbert A, Smith AC. Home telehealth and paediatric palliative care: clinician perceptions of what is stopping us? BMC Palliative Care 2014; 13. http://dx.doi.org/10.1186/1472-684x-13-29
133. Bradford N, Herbert A, Walker R, Pedersen L-A, Hallahan A, Irving H, et al. Home telemedicine for paediatric palliative care. Studies in Health Technology and Informatics 2010; 161: 10-19.
134. Ray RA, Fried O, Lindsay D. Palliative care professional education via video conference builds confidence to deliver palliative care in rural and remote locations. BMC Health Services Research 2014; 14: 272. http://dx.doi.org/10.1186/1472-6963-14-272
135. Quilty S, Bachmayer L, Congdon A. Telehealth in remote NT: bridging the gap. The Medical Journal of Australia 2015; 203(1): 18. http://dx.doi.org/10.5694/mja15.00082
136. Finch J, Anastassiadis P, Rolan J, Killington M. Rural and remote tele-rehabilitation. Journal of the Australasian Rehabilitation Nurses' Association (JARNA) 2000; 3(4): 21-24.
137. O'Hara R, Jackson S. Integrating telehealth services into a remote allied health service: a pilot study. The Australian Journal of Rural Health 2015; 1 April. http://dx.doi.org/10.1111/ajr.12189
138. McGill M, Constantino M, Yue DK. Integrating telemedicine into a national diabetes footcare network. Practical Diabetes International 2000; 17(7): 235-238. http://dx.doi.org/10.1002/1528-252X(200010)17:7<235::AID-PDI101>3.0.CO;2-H
139. Khalil H, Cullen M, Chambers H, Steers N, Walker J. Implementation of a successful electronic wound documentation system in rural Victoria, Australia: a subject of collaboration and community engagement. International Wound Journal 2014; 11(3): 314-318. http://dx.doi.org/10.1111/iwj.12041
140. Manuel P. A prospective, interventional study of the effectiveness of digital wound imaging, remote consultation and podiatry offloading devices on the healing rates of chronic lower extremity wounds in remote regions of Western Australia. Wound Practice and Research 2012; 20(2): 103-109.
141. Santamaria N, Carville K, Ellis I, Prentice J. The effectiveness of digital imaging and remote expert wound consultation on healing rates in chronic lower leg ulcers in the Kimberley region of Western Australia. Primary Intention: The Australian Journal of Wound Management 2004; 12(2): 62.
142. Santamaria N, Clayton L. Cleaning up. The development of the Alfred/Medseed Wound Imaging System. Collegian (Royal College of Nursing, Australia). 2000; 7(4): 14-15, 17-18. http://dx.doi.org/10.1016/S1322-7696(08)60385-6
143. Western Australia Country Health Service. Telehealth. (Internet) 2015. Available: http://www.wacountry.health.wa.gov.au/index.php?id=telehealth&0= (Accessed 30 August 2015).
144. Country Health South Australia Local Health Network. Digital telehealth networks. (Internet) 2014. Available: http://www.sahealth.sa.gov.au/wps/wcm/connect/c121db004c759e5daac8baa496684d9f/DigitalTelehealthUpgradeGPs-CHSALHN-CS-1209.pdf?MOD=AJPERES&CACHEID=c121db004c759e5daac8baa496684d9f (Accessed 30 August 2015).
145. NSW Agency for Clinical Innovation. Telehealth resources package: considerations for success. (Internet) 2014. Available: http://www.aci.health.nsw.gov.au/__data/assets/pdf_file/0003/189201/ACI-Telehealth-Resource-Package.pdf (Accessed 30 August 2015).
146. Queensland Government Queensland Health. Telehealth support unit. (Internet) 2015. Available: https://http://www.health.qld.gov.au/telehealth/ (Accessed 30 August 2015).
147. Northern Territory Government. eHealthNT. (Internet) 2015. Available: http://www.ehealthnt.nt.gov.au/FOR_PROVIDERS/-_Contacts/index.aspx (Accessed 30 August 2015).
148. Primary Health Tasmania. TeleHealth. (Internet) 2015. Available: http://www.primaryhealthtas.com.au/telehealth (Accessed 30 August 2015).
149. State Government Victoria: Health. Telehealth. (Internet) 2015. Available: http://health.vic.gov.au/telehealth/ (Accessed 30 August 2015).
150. Zanaboni P, Wootton R. Adoption of telemedicine: from pilot stage to routine delivery. BMC Medical Informatics and Decision Making 2012; 12(1): 1. http://dx.doi.org/10.1186/1472-6947-12-1
151. Kvistgaard L, di Giuseppe G, Lopriore C. European momentum for mainstreaming telemedicine deployment in daily practice. (Grant agreement no 297320) Deliverable 3.2: Towards a personalised blueprint - for doers, by doers: consolidated version. (Internet) 2014. Available: http://www.telemedicine-momentum.eu/wp-content/uploads/2014/12/D3.2_v13_Momentum_ConsolidatedBlueprint.pdf (Accessed 28 September 2016).
152. Desai N. The 10 secrets of telehealth Success. USA: hands on telehealth. (Internet). Available: http://www.handsontelehealth.com/media/editors/codemirror/js/book/The_10_Secrets_Of_Telehealth_Success.pdf (Accessed 30 August 2015).
153. Joseph V, West RM, Shickle D, Keen J, Clamp S. Key challenges in the development and implementation of telehealth projects. Journal of Telemedicine and Telecare 2011; 17(2): 71-77. http://dx.doi.org/10.1258/jtt.2010.100315
154. Altman L, Fernando S, Holt S, Maeder A, Margelis G, Morgan G, et al. One in four lives: the future of telehealth in Australia. Sydney: Australian Information Industry Association, 2014.
155. Queensland Parliament. Inquiry into telehealth services in Queensland. Report no. 55. Brisbane: Parliamentary Health and Community Services Committee, 2014.
156. Mant J. Process versus outcome indicators in the assessment of quality of health care. International Journal for Quality in Health Care 2001; 13(6): 475-480. http://dx.doi.org/10.1093/intqhc/13.6.475
_____________________________________ Supplementary table: Characteristics of 72 services from 116 articles
Appendix I: Systematic review methods

