full article:
Advances in the scientific understanding of the long-term health and social costs of children failing to reach their developmental potential have led to calls for increased investment in policy and services to improve child development outcomes as a global priority1. The central role of primary healthcare services in the promotion and protection of child development - especially in more disadvantaged populations - has also been highlighted by recent influential international reports2-4. Routine developmental monitoring is an important function of primary health care5.
Developmental monitoring is a longitudinal process to enable early detection of children who may be at risk of developmental delays and more generally to promote healthy child development. During this process, health practitioners may utilise developmental screening instruments in addition to discussing parent concerns, obtaining a history of risks and making clinical observations. Notably this is not simply a one-off screen; rather, it is a process of following a child's development over time, providing advice and making referrals where necessary6,7.
Early detection of developmental difficulties is of global public health importance, particularly in 'at-risk' populations4. Evidence has consistently shown that the greater the exposure to cumulative risks, the more children's development may be compromised and hence the greater the potential inequality in future outcomes8. Many Australian Aboriginal children grow up in disadvantaged communities, with exposure to multiple risks that adversely impact on a range of social, economic and learning outcomes over the life course9.
Information about the prevalence of developmental delay and type of disability in Australian Aboriginal children is limited due to the lack of robust data10. In urban non-Aboriginal populations, approximately 17% of children have problems in one or more area of development11. It is generally presumed that the rates among remote-dwelling Aboriginal children are even higher given the levels of developmental adversity they face12. While reliable estimates of their rates of developmental delay are not yet available, there is ample evidence that Aboriginal children are faring worse than their non-Aboriginal counterparts in terms of their longer term psychosocial, health and educational outcomes13.
In recent years the Northern Territory (NT) Government has put considerable effort into the development of its Healthy Under 5 Kids (HU5Ks) program14. This program, implemented in 2009 in remote health centres, is a schedule of 10 'well-child' health checks provided to all Aboriginal children aged less than 5 years living in remote Aboriginal communities. The HU5Ks expanded the pre-existing child health program to include developmental monitoring at 7 of the 10 HU5Ks health checks: 2, 6, 12, 18, 24, 36 and 48 months15.
The aims of the comprehensive, structured child health checks include early identification of developmental delay and disability through key alerts and developmental pointers in the HU5Ks care plans15. In both paper and electronic health records, the care plan includes general questions about development, including 'any concerns about hearing ... vision ... general development?' and specific age-related developmental pointers, such as 'one year olds should be mobile - crawling, bottom shuffling, starting to walk with support'. Practitioners are advised that a medical referral is necessary if specific listed milestones are absent or the family is concerned. The care plan also includes anticipatory guidance on key topics - such as play and communication - recommending activities caregivers can use with children to promote development16.
Although the HU5Ks program was an essential practice improvement measure, few data have indicated developmental monitoring practices in remote health services. While there has been strong uptake in many services of the One21Seventy child health audit tool17 as part of clinical quality improvement efforts18, the main focus of that audit tool is the physical health of children. Although it collects data on developmental services provided, it does not collect information about how developmental assessments are made (such as whether milestones are reported or observed or whether structured tools are used) and collects minimal detail about any action taken17. Consequently there is a gap in knowledge of the quality of the developmental monitoring services provided in remote health services.
The present study has sought to address this gap by undertaking a service audit using a specifically designed audit tool to describe the developmental monitoring practice in two remote Australian Aboriginal health services. The audit study aimed to collect data on who completed the assessments and the quality of the monitoring practice.
Context
This study was conducted as part of a larger case-study evaluation exploring the implementation of an early childhood development program. After initial screening consultations with people knowledgeable about the potential communities, two very remote Aboriginal NT communities19 were selected as 'exemplary' cases. These cases had the conditions perceived necessary for the implementation to be successful20. The audit study was conducted in Community A in the northernmost part of the NT and in Community B in central Australia. The communities are similar in size, with a population just under 1000, of whom approximately 85% are of Aboriginal and Torres Strait Islander descent. These communities are broadly representative of other remote Aboriginal communities that experience significant socioeconomic disadvantage21.
Each of the study communities has a primary healthcare centre staffed with four to six Aboriginal health workers (AHWs), three to five remote area nurses, and visiting medical staff, who together are responsible for the provision of all primary healthcare services. Visiting child health nurses support the implementation of the HU5Ks program in both communities. These communities also have access to paediatric services: a visiting paediatrician in Community A, and, in Community B, a paediatric outpatient service in Alice Springs, which is 130 km away. Limited allied health services are available through a key community contact from the Disability Services Remote Team, consisting of multidisciplinary staff. At the time of the study, Community A was using a paper health record system, while Community B had an electronic health record.
Data sources
Audits were undertaken of the medical record of every resident Aboriginal child aged from birth to 5 years over a 12-month period. Health centre staff reviewed participant lists generated from health centre records to identify resident children. All attendances in the 12-month period were reviewed.
The audit tool was based on the One21Seventy child health audit tool17, which was modified and expanded to capture additional data identifying who provided the developmental service and the quality of the service provided. The data elements, which were collected and de-identified on paper forms, were:
- recorder's role or position
- number of total health centre attendances and primary reason for attendance
- number of attendances where a developmental service was provided
- record of developmental monitoring service provided including:
- enquiry about development on history
- observation of development
- advice provided (including anticipatory guidance)
- developmental screening tool used
- referral for assessment due to concerns
- follow-up of known disorder or delay. - identification of developmental delay or disorder.
- other child health outcomes as per HU5Ks guidelines (ie immunisations, growth parameters, respiratory checks and haemoglobin)
- evidence of diagnosis of chronic illnesses or congenital problems.
The first author (a paediatrician), a research assistant (a trained nurse and teacher) and a continuous quality improvement facilitator conducted data collection between November and December 2011. Training and written audit protocols were provided. For the purpose of the audit, a developmental check included any assessment or comment regarding gross motor, fine motor, communication/language, personal social or problem-solving skills, and hearing or vision. A developmental check was considered to have been completed if performed at least once in the 12-month audit period. Data recorded were included on the specific HU5Ks forms or written in progress notes. A sample of audits (10%), carried out by different auditors, was repeated to ensure consistency across all data collectors.
Data analysis
Two research assistants entered data into a database. The use of compulsory fields, ranges and validation rules minimised data entry errors. Data cleaning was conducted at data entry and again before analysis commenced.
Analysis was undertaken using the Statistical package for the Social Sciences v20.0 (IBM; http://www.spss.com.au). Descriptive statistics were used to summarise data. Frequencies and percentages were used to describe categorical data, and means and standard deviations or medians and interquartile ranges were used to summarise continuous variables.
Ethics approval
Ethics approval was obtained from the Human Research Ethics Committees of the Top End of the NT (HREC-2010-1403) and central Australia (2010.06.01).
The study was conducted in accordance with the National Health and Medical Research Council Guidelines for Ethical Conduct in Aboriginal and Torres Strait Islander Health Research. The study proposal was presented to and approved by the Menzies School of Health Research Indigenous Reference Group.
A total of 151 audits were completed, 80 in Community A and 71 in Community B. This is the total number of children who had any attendances during the 12-month period. The median number of clinic attendances per child in Community A was 10 (interquartile range (IQR) 5-15). The minimum number of attendances was one and there were three outliers, with 46, 50 and 57 attendances respectively. Community B had a similar distribution, with a median of 9 (IQR 5-13). Acute care was the most common reason for attendance in both communities (53% in Community A, 62% in Community B), followed by child health checks (24% and 17%, respectively).
Weight was checked in almost every child in both communities at least once in the 12-month period. In Community A, developmental checks were completed for 79% of children, which was comparable to the proportion who had their haemoglobin checked (80%) and who were immunised (76%), but was less than the proportion who had their height measured (95%) or respiratory system examined (88%). In Community B, the proportion of children who had immunisations and developmental checks was lower than for all other checks; 63% were recorded as having immunisations up to date and 59% as receiving at least one developmental check. As shown in Table 1, nurses were responsible for conducting around half the child health checks in both communities.
In Community A, AHWs saw 38% of all child attendances and were responsible for conducting and recording more of the acute child presentations and fewer of the 'well-child' checks (Table 1). In Community B, 18% of all child attendances were seen by AHWs and the proportion of attendances seen by AHWs for child health checks was 31%. However, developmental checks were conducted by AHWs in only one-fifth of clinical encounters (22%) in Community B. Notably, the majority of developmental checks in both communities were completed by nurses (Table 1).
Documentation of developmental checks varied across the two communities (Table 2). Community A used paper records and 93% of all the checks were recorded on the HU5Ks care plan. Additionally, some developmental notes were documented in the progress notes, with a proportion using both. Electronic records were used in Community B and very few had information regarding the developmental checks undertaken recorded on the HU5Ks care plan (9%). These were mostly documented on a checklist in the 'visit' section (90%).
In both the electronic and paper HU5Ks care plans, 'yes/no' tick boxes indicate simply whether developmental concerns were elicited and whether anticipatory guidance was provided. Where there was evidence of a developmental check, the 'yes/no' tick boxes were checked in the majority of records: 93% in Community A and 81% in Community B. Staff completing the developmental checks in Community A documented their overall clinical impression more so than in Community B (81% compared to 31%). Anticipatory guidance was recorded as having been given in 81% of developmental checks in Community A compared to only 9% of checks in Community B. While the tick boxes were checked, indicating that some form of assessment had been made, there was little information about how the assessment was undertaken (Table 2). Notably, the use of a developmental screening tool was only documented in one check.
Table 3 shows the action taken when a developmental problem was identified. While there was little evidence of any specific developmental advice provided or planned review in Community A, 60% had general advice provided and a referral made to the paediatric or allied health services. In Community B there were only four records that documented a developmental problem and they contained very little documentation about any subsequent intervention. The number of developmental difficulties referred to in Table 3 includes all health record entries where a developmental problem was identified. Therefore the same child could be included multiple times, as some children have more than one developmental check scheduled in a 12-month period. The prevalence of developmental difficulties was calculated by including the number of children in each community who had developmental difficulties identified: 17 in Community A (21%; n=80) and 4 in Community B (6%; n=71).
Table 1: Staff types and child services provided in communities A and B, December 2010 - November 2011
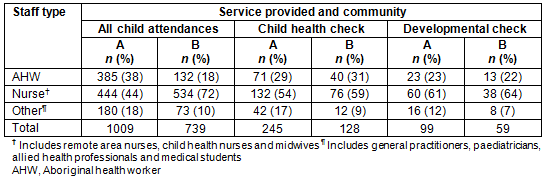
Table 2: Documentation of developmental checks in communities A and B, December 2010 - November 2011
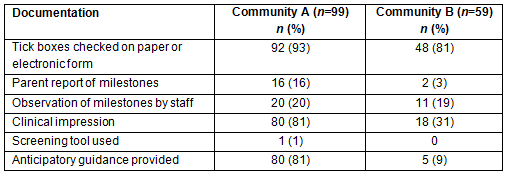
Table 3: Action taken if a developmental problem was identified in communities A and B, December 2010 - November 2011
Discussion
This audit study provides insights into the documented delivery of developmental monitoring services in two remote health services. Developmental checks are only one component of well-child checks, which in turn are a small part of a wide range of primary healthcare services that are the responsibility of remote health practitioners. In a work environment that was challenging for staff, the authors found that around two-thirds of children across the two study communities received at least one of their scheduled developmental checks during the 12-month audit period. While some gaps were identified in the quality of the developmental monitoring practice documented, these provide important insights for informing the improvement of developmental services.
Studies of developmental services provided in Australian remote health services are scarce. A clinical audit of remote Australian Aboriginal primary healthcare services revealed that 37% of children aged less than 5 years had a record of a developmental service in the previous 12 months22. The authors' findings are considerably higher than this previous report; the difference may be due to the modified audit tool capturing more instances of service. The HU5Ks program, introduced after Bailie's 2008 study, may have led to a higher proportion of children having a developmental check22. This apparent improvement in the number of children receiving developmental checks is encouraging, especially in view of the broad scope of responsibilities remote health practitioners face.
Paper HU5Ks forms were completed more thoroughly than were electronic forms; a difference that could be explained by the challenges of the electronic health record to the accurate documentation of consultation events23. Documentation as a record of care provided remains an important part of practice24. Forms need to be straightforward to use, with prompts to guide appropriate developmental checks. Moreover, an information technology system that has adequate infrastructure and staff support is necessary to facilitate accurate data recording data25.
This study found that the proportion of children with developmental difficulties was 21% in Community A and 6% in Community B. Both percentages are likely to be under-representations. These populations are exposed to significant, cumulative risks, known to impact on developmental outcomes. In low- and middle-income countries, with levels of disadvantage similar to many remote Aboriginal communities, the proportion of children with developmental difficulties has been found to be 23%1. Furthermore, numerous studies have shown that use of structured tools dramatically increases early detection of developmental difficulties and that the majority of children with delays will not be identified where clinical judgement alone is relied upon26-28. The authors of the present study found only one instance where the use of a developmental screening tool was documented. Although the use of developmental screening instruments is recommended as part of developmental monitoring services, this has not been recommended in remote health services in the NT because a culturally appropriate tool has not been available16.
More than half of children who had a developmental problem identified were provided with general advice and had an appropriate referral made. While this is a relative strength, review was arranged in only a third of children, and action taken once a problem is identified is an area for improvement across both communities. The apparent lack of follow-up has been highlighted previously as a challenge for remote primary healthcare services22. The need for effective systems for follow-up, however, applies equally to any setting where developmental screening is implemented, including urban paediatric clinics29. Without a system for ensuring appropriate follow-up has occurred, the benefits to children are diminished.
Although NT remote health practitioners have the responsibility for delivery of the HU5Ks checks15, they are not necessarily equipped with the skills to provide these services. Training in early childhood development is not included in AHW training and in 2011 less than 5% had completed the online HU5Ks training30 (L. Nuttall, personal communication, 11 March 2011). There is also a lack of child health expertise among remote area nurses, with fewer than 50% having completed the HU5Ks training and a lesser proportion having child health qualifications31 (L. Nuttall 2011, pers. comm.).
While the authors identified that the majority of checks were conducted by nurses, AHWs did undertake about a third of child health checks and one fifth of developmental checks. AHWs play an essential role in providing remote health services in the NT32 and it is a widely held view that better health outcomes are possible when health services include Aboriginal staff33,34. To support their role, AHWs require education and training to develop the necessary skills and capabilities to respond to the needs of their communities32,35,36.
The strengths of this study include the use of a specifically adapted audit tool, the comprehensive data collection, inclusion of every child in the relevant age group, and the contribution to the literature on approaches to assessing the quality of developmental care in primary care settings. This is the first study of which the authors are aware that focuses on the quality of developmental screening in primary health care in this context.
The study has several limitations. Caution must be taken in generalising the results of this study as only two health services were included. Audits of records may have limitations in the accuracy of data captured, resulting in an under-estimate of the true service delivered. However, failure to document the developmental monitoring service delivered is itself inadequate care, as it presents a considerable barrier to continuity of care, especially in areas of high staff turnover24. Finally, audits cannot easily distinguish between compliance with documentation of service and the quality of service provided: the level of engagement of the client and the detail of questioning or advice often remain largely undocumented.
The study has identified some gaps in the delivery of developmental monitoring services in remote health services, including the lack of a structured developmental screening tool for use in remote Aboriginal settings, difficulties with documenting electronic records and little evidence of specific advice or follow-up action. Addressing a number of system-wide factors may facilitate improved delivery of these services. The findings suggest that a more systematic approach to the delivery of developmental monitoring services and more uniform recording methods are needed. It has also reinforced the importance of investing in targeted training to support remote health staff. Finally, developmental practice in the remote Australian Aboriginal context cannot be expected to improve without the availability of a culturally appropriate, structured developmental screening measure.
Acknowledgements
Special thanks to the staff and management of participating health centres. We wish to acknowledge the Lowitja Institute for providing project funds to undertake this study. AD is supported by an Australian Research Council, Science of Learning Research Centre post-doctoral fellowship.
References
1. Engle PL, Fernald LCH, Alderman H, Behrman J, O'Gara C, Yousafzai, A et al. Strategies for reducing inequalities and improving developmental outcomes for young children in low-income and middle-income countries. The Lancet 2011; 378(9799): 1339-1353. http://dx.doi.org/10.1016/s0140-6736(11)60889-1
2. Engle PL, Young ME, Tamburlini G. The role of the health sector in early childhood development. In: PR Britto, PL Engle, CM Super (Eds). Handbook of early childhood development research and its impact on global policy. New York: Oxford University Press, 2013; chapter 9.
3. Richter LM. The importance of caregiver-child interactions for the survival and healthy development of young children: a review. Geneva: WHO, 2004.
4. World Health Organization Department of Child and Adolescent Health and Development. A critical link: interventions for physical growth and psychological development. Geneva: WHO, 1999.
5. American Academy of Pediatrics; Council on Children With Disabilities; Section on Developmental Behavioral Pediatrics; Bright Futures Steering Committee; Medical Home Initiatives for Children With Special Needs Project Advisory Committee. Identifying infants and young children with developmental disorders in the medical home: an algorithm for developmental surveillance and screening. Pediatrics 2006; 118: 405-420. http://dx.doi.org/10.1542/peds.2006-1231
6. American Academy of Pediatrics. Bright futures: guidelines for health supervision of infants, children, and adolescents. (Internet) 2008. Available: http://brightfutures.aap.org/3rd_Edition_Guidelines_and_Pocket_Guide.html (Accessed 1 August 2013).
7. Glascoe FP, Dworkin PH. The role of parents in the detection of developmental and behavioral problems. Pediatrics 1995; 95(6): 829-836.
8. Wachs TD, Rahman A. The nature and impact of risk and protective influences on children's development in low-income countries. In: PR Britto, PL Engle, CM Super (Eds). Handbook of early childhood development research and its impact on global policy. New York: Oxford University Press, 2013; chapter 5.
9. Australian Institute of Health and Welfare and Commonwealth Department of Health and Ageing. Progress of the NT emergency response child health check initiative: update on results from the child health check and follow-up data collections. Cat. no. IHW 28. Canberra: AIHW, 2009.
10. Australian Institute of Health and Welfare. A picture of Australia's children 2012. Cat. no. PHE 1672012. Canberra: AIHW, 2012.
11. Boyle CA, Boulet S, Schieve LA, Cohen RA, Blumberg SJ, Yeargin-Allsopp M, et al. Trends in the prevalence of developmental disabilities in US children, 1997-2008. Pediatrics 2011; 127(6): 1034-1042. http://dx.doi.org/10.1542/peds.2010-2989
12. Silburn SR, Robinson G, Arney F, Johnstone K, McGuinness K. Early childhood development in the NT: issues to be addressed. Topical paper commissioned for the public consultations on the Northern Territory Early Childhood Plan. Darwin: Menzies School of Health Research, 2011.
13. Silburn SR, McKenzie JW, Moss B. Northern Territory results for the Australian Early Development Index 2009. Darwin: Menzies School of Health Research and Northern Territory Department of Education and Training, 2010.
14. McKinnon T, Chatterji M. Beyond GAA to healthy under 5 kids in the bush: adapted from rationale for routine child health contacts draft. Northern Territory Disease Control Bulletin 2008; 15(4): 24-26.
15. Northern Territory Department of Health. Remote health atlas. (Internet) 2013. Available: http://www.health.nt.gov.au/Remote_Health_Atlas/Search_the_Atlas/ (Accessed 12 August 2013).
16. Department of Health and Families, Graduate School for Health Practice. Healthy Under 5 Kids Program, Education Package 2010. Darwin: Charles Darwin University and Northern Territory Government, 2009.
17. One21Seventy. Improving Indigenous health care using CQI. (Internet) 2013. Available: http://www.one21seventy.org.au/ (Accessed 1 August 2013).
18. Bailie R, Si D, Shannon C, Semmens J, Rowley K, Scrimgeour D, et al. Study protocol: national research partnership to improve primary health care performance and outcomes for Indigenous peoples. BMC Health Services Research 2010; 10(1): 129. http://dx.doi.org/10.1186/1472-6963-10-129
19. Australian Bureau of Statistics. Australian standard geographical classification. Cat. No. 1216.0. (Internet) 2011. Available: http://www.abs.gov.au/AUSSTATS/abs@.nsf/allprimarymainfeatures/8B8ABC8EC62D8F46CA2570AE000DD3B5?opendocument (Accessed 1 August 2013).
20. Yin RK. Case study research: design and method. 4th Edn. Thousand Oaks, CA: Sage, 2009.
21. Australian Bureau of Statistics. Community profiles. (Internet) 2011. Available: http://www.abs.gov.au/websitedbs/censushome.nsf/home/communityprofiles?opendocument&navpos=230 (Accessed 13 November 2014).
22. Bailie RS, Si D, Dowden MC, Connors CM, O'Donoghue L, Liddle HE, et al. Delivery of child health services in Indigenous communities: implications of the federal government's emergency intervention in the Northern Territory. Medical Journal of Australia 2008; 188: 615-618. http://dx.doi.org/10.1071/PY08022
23. Peiris D, Brown A, Howard M, Rickards B, Tonkin A, Ring I, et al. Building better systems of care for Aboriginal and Torres Strait Islander people: findings from the Kanyini health systems assessment. BMC Health Services Research 2012; 2(1): 369. http://dx.doi.org/10.1186/1472-6963-12-369
24. Bailie R, Si D, Connors C, Kwedza R, O'Donoghue L, Kennedy C et al. Variation in quality of preventive care for well adults in Indigenous community health centres in Australia. BMC Health Services Research 2011;11(1): 139. http://dx.doi.org/10.1186/1472-6963-11-139.
25. Clifford A, Shakeshaft A, Deans C. How and when health-care practitioners in Aboriginal Community Controlled Health Services deliver alcohol screening and brief intervention, and why they don't: a qualitative study. Drug & Alcohol Review 2012; 31(1): 13-19. http://dx.doi.org/10.1111/j.1465-3362.2011.00305.x
26. Hix-Small H, Marks K, Squires J, Nickel R. Impact of implementing developmental screening at 12 and 24 months in a pediatric practice. Pediatrics 2007; 120(2): 381-389. http://dx.doi.org/120/2/381 [pii]10.1542/peds.2006-3583
27. Guevara JP, Gerdes M, Localio R, Huang YV, Pinto-Martin J, Minkovitz CS, et al. Effectiveness of developmental screening in an urban setting. Pediatrics 2013; 131(1): 30-37. http://dx.doi.org/10.1542/peds.2012-0765
28. Marks KP, Glascoe FP, Macias MM. Enhancing the algorithm for developmental-behavioral surveillance and screening in children 0 to 5 years. Clinical Pediatrics 2011; 50(9): 853-868. http://dx.doi.org/10.1177/0009922811406263
29. Kingsley J, Phillips R, Townsend M, Henderson-Wilson C. Using a qualitative approach to research to build trust between a non-Aboriginal researcher and Aboriginal participants Qualitative Research Journal 2010; 10(1): 2-12. http://dx.doi.org/10.3316/QRJ1001002
30. Department of Education Employment and Workplace Relations. Training.gov.au (TGA), HLT40213 - Certificate IV in Aboriginal and/or Torres Strait Islander Primary Health Care Practice. (Internet) 2013. Available: http://training.gov.au/Training/Details/HLT40213 (Accessed 9 August 2013).
31. Lenthall S, Wakerman J, Opie T, Dunn S, MacLeod M, Dollard M, et al. Nursing workforce in very remote Australia, characteristics and key issues. Australian Journal of Rural Health 2011; 19(1): 32-37. http://dx.doi.org/10.1111/j.1440-1584.2010.01174.x
32. Health Workforce Australia. Aboriginal and Torres Strait Islander Health Worker project: environmental scan. Adelaide: Health Workforce Australia, 2011.
33. Nagel T, Thompson C. Aboriginal mental health workers and the improving Indigenous mental health service delivery model in the 'Top End'. Australasian Psychiatry 2006; 14(3): 291-294. http://dx.doi.org/10.1111/j.1440-1665.2006.02294.x
34. McGrath PD, Patton MAS, Ogilvie KF, Rayner RD, McGrath ZM, Holewa HA. The case for Aboriginal health workers in palliative care. Australian Health Review 2007; 31(3): 430-439.
35. Genat B, Bushby S, McGuire M, Taylor E, Walley Y, Weston T. Aboriginal healthworkers: primary health care at the margins. Perth: University of Western Australia Press, 2006.
36. Wise M, Angus S, Harris E, Parker S. Scoping study of health promotion tools for Aboriginal and Torres Strait Islander people. Melbourne: Lowitja Institute, 2012.
