full article:
This article describes the adaptation and evaluation of a postgraduate agricultural medicine program, originally developed at the University of Iowa, School of Medicine, in the USA, to rural professionals across Australia through a partnership with a regional health service and an Australian university in the southern state of Victoria. Agricultural medicine is the multidisciplinary specialty area of occupational and environmental health focusing on the anticipation, evaluation, diagnosis, treatment and prevention of occupational illnesses and injuries in agricultural populations1.
Agriculture, fishing and forestry remain the most hazardous industries in the USA, with a rate of 24.4 fatalities per 100 000, which is seven times greater than the national average rate of 3.5 fatalities per 100 0002. Similarly, in Australia, a report from Safe Work Australia, an independent statutory agency, shows agriculture, fishing and industry workers accounted for the highest number of workplace fatalities in 2011 and 2013 and the second highest for all years from 2003 to 20143.
The health, wellbeing and safety concerns of farming populations have not been well integrated into the general fabric of medical and healthcare services4-8 and the disparity between the healthcare services in urban and rural areas has been previously noted9,10. In Australia, health outcomes generally worsen as distance from a major city increases. This is evidenced by above-average rates of earlier death through diabetes, heart disease, cancer and suicide in rural and remote populations11,12. Different but in some ways similar patterns are also seen in the USA, with higher rates of obesity and disadvantage observed in both outer rural and inner urban areas, but reduced overall cancer mortality in farming populations, highlighting the importance of place in health disparity10,13. The reasons for this are multifactorial, with such aspects as access to health services, socioeconomic factors, attitudes towards health-seeking behaviours and cultural differences or influences being important. Long-term and consistent underresourcing in health has also occurred in rural areas of Australia and farming populations as a subset of rural populations have also been affected14,15.
Globally, agricultural communities share some common but distinct needs that may differentiate them from other populations. For example, home is often the workplace, with the employees - usually husband, wife, children and extended family - having both an emotional relationship and an economic one. Models of care and interventions that have been designed for urban populations may not account for these differences, leaving the health of farmers unaddressed and at increased risk16-19.
However, the training of rural professionals (health, medical, safety and agricultural) and the availability of appropriate preventive services to both agricultural and rural populations remains small in comparison to the amount spent per capita in urban areas6,14. This is of both national and international concern, with some nations, such as Australia, providing generous individual financial rewards and substantial resourcing to entice healthcare providers, mainly medical practitioners and medical specialists, to locate and stay for a minimum period in rural areas19-21.
Not surprisingly, many rural health practitioners who relocate to work in farming communities then learn through experience, and sadly by trial and error. Because very few formal or even informal programs globally focus exclusively on training medical and health professionals in agricultural health and medicine, this is not unexpected. Interviews with rural healthcare providers in the US highlighted that whilst local healthcare practitioners can positively affect workers' health, most rural providers have very limited knowledge about agricultural work22.
The landmark US national report Agriculture at risk23 documented back in 1989 that 'the rural health and safety work force could justify the services of 500-1000 agricultural hygienists, 1000 physicians and 8000 nurses trained in agricultural health to meet the needs of the serious health and safety concerns in agriculture'. This report was a driving force behind the development of the postgraduate Agricultural Medicine: Occupational and Environmental Health for Rural Health Professionals course at the University of Iowa. This program evolved over the years to include elective training for medical students and nurses as well as many other health professional students, family medicine residents and academic graduate programs in the field24. In 2006, the Building Capacity Program in Agricultural Medicine was established as a component of the National Institute of Occupational Safety and Health-funded Great Plains Center for Agricultural Health with the goal of establishing a universal core curriculum for agricultural medicine in industrialised countries. This was accomplished by convening a working group of 16 nationally recognised agricultural health professionals who established core topics and competencies utilising a group-consensus process as described by Fisher and Donham25.
In 2008, recommendations to develop a similar agricultural medicine postgraduate unit in Australia were made to the Victorian Government, in partnership with Western District Health Service (based in the agricultural centre of Hamilton) and Deakin University26. The resulting course, Agricultural Health and Medicine, was developed at the National Centre for Farmer Health, within the School of Medicine at Deakin University, adapting the curriculum framework from the University of Iowa to Australian environs. The curriculum was designed to enable healthcare providers to deal more efficaciously with illnesses and conditions particular to Australian farmers, as distinct from other rural people. Additionally the curriculum aims to support agricultural professionals (agronomists, agricultural extension officers and veterinary surgeons) to play a role in preventing occupational illness and injury through increased health literacy27.
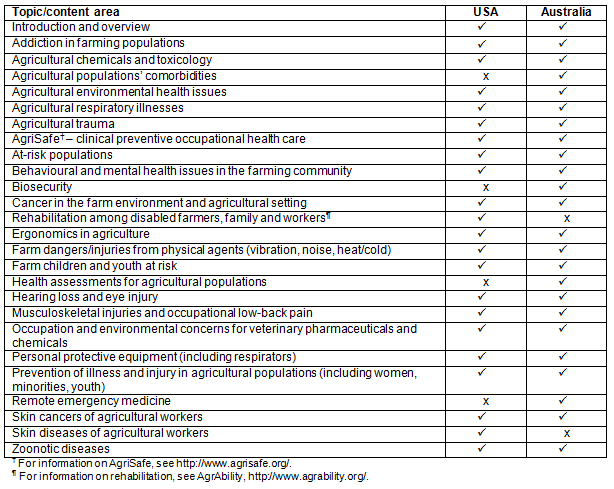
The Australian program consulted with the USA and, when local epidemiological differences were found to exist, the curriculum was adjusted and/or appropriate topics added. Table 1 shows the curricula for the US and Australian courses. Since commencing in 2010, the Australian course has been marketed to encourage and develop relationships across medicine, public health, agriculture, nursing, health sciences, veterinary science, safety and health promotion, reflecting the diversity of agriculture and rural communities in Australia.
Between 2010 and 2013, 151 students from 29 US states and three countries (the UK, Turkey and Indonesia) attended the agricultural medicine course in Iowa, USA. In Australia, between 2010 and 2013, 91 students attended the agricultural medicine course, representing all Australian states and mainland territories. Students in both the US and Australia came from the nursing, medical doctor, veterinary, mental health, safety and agricultural professions.
Both the US and Australian courses were guided by the textbook Agricultural medicine: occupational and environmental health for the health professions28. The US course is modified to include regional and national differences in agricultural processes and exposures, cultural and climatic variations, and variations in the availability and type of health services. It is noted that Donham and Thelin's 2006 book focused on North American agricultural populations, so the Australian course utilised relevant published Australian articles.
In aiming to successfully deliver agricultural medicine education to predominantly postgraduate or returning mature age students, both courses have utilised Kolb's adult learning model29 and Kirkpatrick's four levels of learning evaluation30. Kolb's model helped with the structure of course components, such that the core curricula include a 5-day, 40-hour, face-to-face intensive course with opportunities for knowledge assessment, group discussion and feedback, and hands-on farm and saleyard assessments. The iterative nature of Kolb's model29 encourages students to reflect on the current approach to prevention and delivery and practice of health services in agricultural populations, providing insight into the gaps and the attitudinal challenges of serving these populations. As noted by Mahoney et al31. there are the growing societal expectations that health professionals make prevention a larger priority and be more knowledgeable about specific population-based issues. This article evaluates and compares the outcomes - in terms of attitudes, knowledge retention and service delivery - for rural health care and safety providers that have undertaken one of these two agriculture medicine courses in the USA or Australia between 2010 and 2013.
Table 1: Agricultural medicine course curriculum comparison: USA and Australia
Teleconferences were held between course facilitators and study investigators in Iowa, USA, and Hamilton, Australia, to identify the study objectives, define the study population and discuss the survey methodology and design. Five objectives were identified, which were to:
- determine the changes in students' attitudes towards agricultural health and safety since taking the course
- identify self-reported professional behavioural changes towards agricultural health and safety since taking the course
- evaluate if participants found the course to be professionally valuable and useful
- determine the level of knowledge retention since taking the course in terms of major course concepts/objectives
- identify future topics of interest within agricultural health and safety.
The target study population was determined to be students who had taken the agricultural medicine course in Iowa City or Hamilton between 2010 and 2013.
In the USA, 151 students completed the course during the study time period, but the sample only included 122 students due to inadequate email addresses. In Australia, 91 students completed the agricultural medicine course during the relevant years, but the study population consisted of 80 students following email bouncebacks.
As the target population spanned two continents, an online survey was identified as the most efficient method of reaching the population. Since the late 1980s, the internet has been a valuable tool in conducting surveys and is now the most commonly used survey model32. Web-based surveys have the potential to reach large populations and are highly cost-effective and time efficient when compared with other methods33. The absence of human interaction with the web-based survey mode eliminates any interviewer bias and increases respondents' willingness to disclose information32 but is offset by a generally poorer response rate when compared with alternative modes33. This evaluation limitation was addressed by using Dillman's recommended five-contact approach, making each contact appear unique and different to the one before34.
This study's survey design addressed Kirkpatrick's four levels of evaluation: reaction, learning, behaviour and result30. The survey instrument was composed of three distinct sections: the students' background including demographic information and reaction to course content (reflecting Kirkpatrick's reaction level), a knowledge and content retention section (reflecting Kirkpatrick's learning level), and a section on current practice and attitudes and behaviours towards agricultural populations (reflecting Kirkpatrick's behaviours and result levels).
Throughout the survey a variety of questions were used, including multiple choice, true and false and opened-ended questions. Five-point Likert scale-style questions, one of the most common question methods used to measure attitudes, were used to evaluate attitudes and behaviours33. The survey was drafted, revised and piloted to identify issues of comprehension, retrieval and reporting. To ascertain differences between the USA and Australia student populations (eg gender, occupation, populations served, age, behavioural and attitude changes, retained knowledge), data were analysed using descriptive statistics, frequencies, the χ2 test with statistical significance p<0.5. Possible future continuing education topics (19) were listed and participants requested to scale as either not interested, interested or very interested. They were also given the opportunity to add any topics not listed and any additional comments regarding the course and their experience.
Ethics approval
The Institutional Review Board, College of Medicine, University of Iowa, reviewed the project and it has been exempted from ethics as an educational evaluation project.
The response rates were 48% for the USA and 55% for Australia, with an overall response rate of 54.5%. Table 2 shows the characteristics of the respondents and highlights that students from all 4 years (2010-2013, inclusive) participated, with 50% of the US responses coming from 2013, and Australian responses more evenly spread across the 4 years.
The majority of students (59.6%) completing the survey had spent 11 or more years in practice, reflecting the return-to-study and continuing-education characteristics of course participants. In both courses, most students were female, with a higher percentage of females undertaking the course in Australia than in the USA (86.3% and 66.7%, respectively (p=0.016)). The age distribution of students was evenly spread between the USA and Australia. Differences were noted in the type of population they currently worked in (p=0.027), with more Australian than US respondents working in rural populations (66.7% and 38.3%, respectively).
As shown in Table 3, self-reported professional behaviours towards agricultural health and safety since taking the course were very similar, with no differences noted and high numbers of students indicating that their abilities in anticipating, diagnosing, treating and preventing occupational injuries had improved (USA, 86.5%; Australia, 98.8%). Most students (USA, 83.1%; Australia, 90.0%) agreed or strongly agreed that the course had helped them address occupational and environmental hazards in agricultural communities and that the course had been appropriate to their profession.
Eighty-eight percent of US students and 98% of Australian students felt confident discussing agricultural health and safety in their respective communities and with their peers. This result reflects the major goal of both the US and Australian courses to nurture and grow interdisciplinary and cross-sectoral relationships and develop health professionals who are able to advocate for their agricultural communities in addition to preventing, diagnosing and treating agricultural health conditions and injuries. This recognition of agricultural health and medicine and the importance of advocacy is reflected in the following comment made by one US respondent:
This was one of the most educational classes I have taken. Although I have lived in a farming community, I did not have the appreciation I currently have. I hope when I graduate, I will be able to become an ambassador to farmers.
Students from both the USA (86.4%) and Australia (88.2%) indicated that since taking the course their approaches to the health and safety of farmers and their families had increased. This was also seen in their reported ongoing efforts to seek out information on the health of farmers and their families (USA, 79.7%; Australia, 86.3%). There were no significant differences between the responses of US and Australian respondents, but the higher percentages for Australian respondents may reflect the higher number of graduates servicing Australian rural communities, as shown in Table 2.
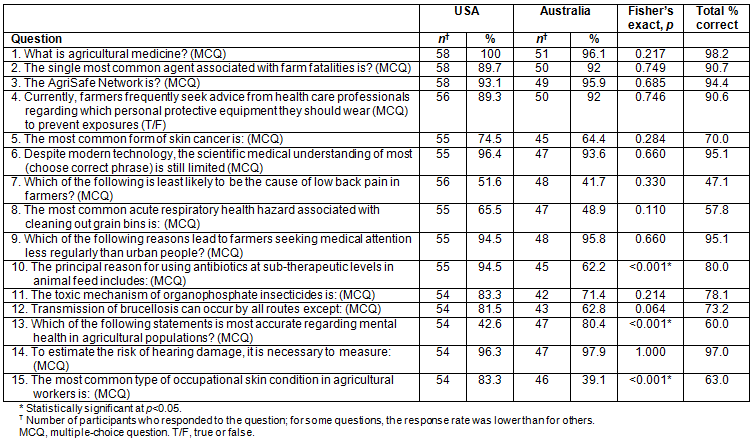
To investigate whether students from the USA and Australia differed in terms of their retention of knowledge, a Fisher's exact test was used. The results of the 15 knowledge questions (a mixture of multiple-choice questions and true and false statements) are shown in Table 4. No significant differences were seen for 12 of the 15 questions.
Respondents also indicated their ongoing interest in agricultural health and safety areas not currently covered by either the Australia or US courses and these included water contamination, agrichemical exposure and Parkinsonism, food chain and food security. Results also showed that 92.7% (102) of respondents wanted further education on agricultural environmental health issues, agricultural trauma and prevention of illness and injury in agricultural populations and 88.2% (97) specified interest in agricultural health and common comorbidities such as diabetes and cardiovascular disease. Injuries from physical agents, behavioural and mental health issues in the farming community, and zoonotic diseases also rated highly, with 91.8% (101), 90% (99) and 87.8% of respondents, respectively, expressing an interest in these topics. Respondents were also asked to highlight any barriers to implementing or being able to use their new skills/knowledge in their workplace or community. Despite poor health outcomes and high injury and fatality rates on farms, some respondents reported frustration and apathy from their workplace as illustrated by this comment from an Australian respondent:
I am a diabetes educator. While very enthusiastic when I returned from completing the course, my work place was not. My demanding role in diabetes education has not allowed me to further develop my skills and interest. However, I do focus more broadly with my farming clients.
The survey also gave respondents a list of learning approaches and asked them to choose preferred methods. Online learning was chosen, but only if there would be opportunity for interaction between the students and presenters, reflecting a preference for Kolb's model of experiential adult learning29. Only four respondents (3.6%) indicated they were not interested in participating in any further continuing-education activities. Other evaluation and testing by the Australian host university occurs through an annual Student Evaluation of Teaching and Units (SETU) to assess the students' experience of the course. Students are invited to agree or disagree to questions using a five-point Likert score on 10 questions, which cover areas such as the use of appropriate online technologies, resourcing, teaching quality, workloads and whether students would recommend the unit to others. The Australian Agricultural Health and Medicine course has repeatedly received an overall average SETU score of above 4.0, out of a possible 5.0 and well above university faculty average27. In 2014, the Australian course was awarded the Vice Chancellors Award for Excellence in Teaching and Learning.
Table 2: Demographic characteristics of Australian and US respondents
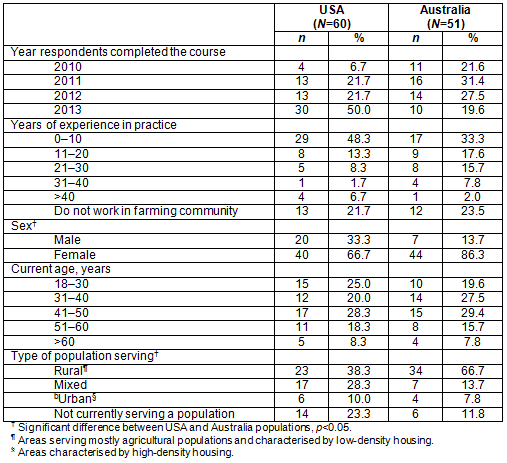
Table 3: Self-reported professional behavioural and attitude changes in US and Australian students since taking the course
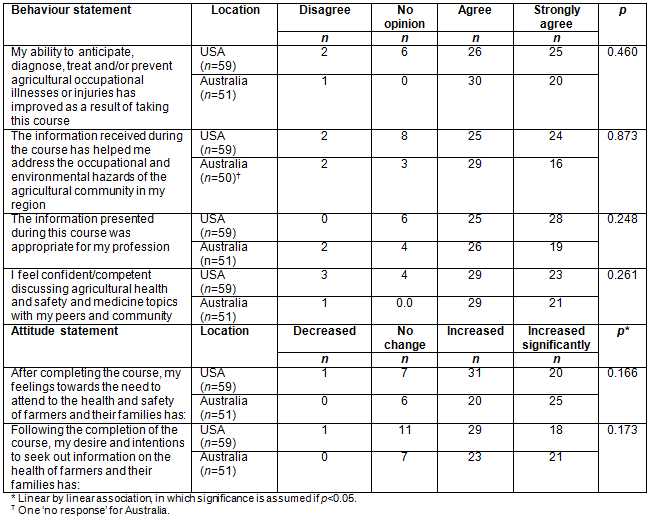
Table 4: Comparison of knowledge retention between Australian and US respondents
Discussion
Both the US and Australian courses were very positively viewed, with respondents agreeing or strongly agreeing they had increased knowledge, skills and confidence for working with agricultural populations. This is an important and reassuring finding, particularly for Australia where over 80% of respondents are continuing to serve a rural or mixed population.
The US course attracted significantly more males than the Australian course: 33.3% and 13.7% respectively. There may be a couple of reasons for this. The University of Iowa's Agricultural Health and Safety course now sits within the College of Public Health, Department of Occupational and Environmental Health, and boasts the only agricultural safety and health program in the country. They offer a Master of Science and a PhD in Agricultural Safety and Health of which the Agricultural Health and Safety course is a required core course component. It is also offered as an elective within various occupational hygiene and public health streams. The Australian course sits within the Faculty of Health and through the School of Medicine (a new medical school) at Deakin University. Deakin does not have an occupational health and safety, occupational hygiene or ergonomics course, which may attract more males and subsequently through the course as a core or elective unit. To date, most Australian students take the course as a standalone unit, and are already working in rural areas (predominantly nurses, mostly female), travelling great distances to attend, as opposed to the US model, where many are already enrolled students. These differences highlight the importance of incorporating the Agricultural Health and Medicine courses as both stand-alone units (for those already working in rural areas) and as part of larger university offerings to provide broader skills and competence.
Overall, high levels of knowledge had been retained by both Australia and US respondents which is pleasing. The three knowledge retention questions that showed significant differences (questions 10, 13 and 15 in Table 4) can be attributed to work practice differences between the USA and Australia. For example, differences noted in question 10 concern the principal use of antibiotics in livestock operations. While 94.5% of the US respondents gave the correct answer, only 62.2% of the Australian respondents did so. This is not surprising given intensive feedlotting is a more common production system in the USA than in Australia, where pasture-based livestock production methods are used more often35.
Question 13 focused on mental health outcomes in rural populations, in which recent work in rural Australia has highlighted substance abuse, particularly of alcohol. Responses to this question indicate that further focus on mental health outcomes and patterns of addiction may require further review in the US curricula. In question 15, the majority (61%) of Australian respondents selected skin cancer as the most common occupational skin condition in agricultural workers rather than contact dermatitis. This reflects the high percentage of skin cancer cases seen in agricultural workers and the major marketing campaign undertaken by the Cancer Council in Australia in 2009 and beyond36 to prevent skin cancers in farming populations. It also highlights that the topic of occupational skin conditions (as opposed to skin cancers) has not been included in the Australian curriculum and this provides some future direction for coverage of this matter.
This is a new area of academic study, with few formal courses globally1, with most health professionals learning about health, wellbeing and safety issues of agricultural populations through experience (trial and error) or informal education. These reviewed courses do address competence in rural workforces by providing appropriate preparation and education for both health and rural professionals working in agricultural communities. In addition, attending the course provides a 'realistic job preview' and a ready-made network to engage with whilst making possible a career path in agricultural health and medicine. This may also assist in rural workforce retention.
Limitations
Whilst 50% of all students participated in the survey, it is possible that those dissatisfied with the educational experience chose not to respond. Whilst the percentage response was satsifactory and more than 50% for both the USA and Australia, the sample size was relatively small. This can result in the directions of responses changing if more past students had participated. It is anticipated that this survey will be repeated when a further two or three courses have been run.
The course Agricultural Medicine: Occupational and Environmental Health for Rural Health Professionals has run many times in the USA and has been adapted successfully to Australia as Agricultural Health and Medicine, demonstrating the feasibility of an international curriculum focused on agricultural health and medicine. The results of this evaluation indicate the benefits of both the US and Australian course to rural practitioners. No difference was seen between Australian and US respondents in knowledge gain, attitude change and professional behaviours. Importantly, both groups of respondents rated the training highly, reporting improved work practices in their agricultural and rural communities. Whilst Australian respondents were more likely to be servicing rural communities, barriers to implementing their new knowledge were highlighted, despite the well-documented health, injury and safety outcomes of farming populations. Embedding the Australia course more cohesively as an elective or core components would be beneficial. The ability to study the course as a standalone unit provides current rural practitioners an opportunity to undertake a relevant course being confident of bringing benefits back to their rural communities.
This innovative and transferable approach bodes well for supporting the new scholarship of agricultural medicine, multidisciplinary and cross-sector approaches, and addressing rural health inequities and poorer health outcomes in agricultural populations. The second edition of the Donham textbook (Agricultural medicine: rural occupational and environmental health, safety, and prevention) includes more extensive and welcome international considerations, including a chapter on Australian and New Zealand agricultural populations37.
Both the Agricultural Medicine: Occupational and Environmental Health for Rural Health Professionals course in the USA and the Agricultural Health and Medicine course in Australia recognise the specialised nature of agricultural health and medicine as a discipline. Continuing opportunities for further development and establishment of the discipline are required. This requires a multipronged focus through the university and academic context with formal courses, the continuing education environment as a stand alone for those already practising and recognition by health service organisations (providers and professional bodies) of agricultural health and medicine education as a vital competence for rural health professionals. Agricultural production remains important to Australia, the USA and the world as major exporters and food producers. Appropriate initiatives for supporting rural health workforces are necessary globally, and especially in countries where the economy is closely related to agriculture and contradictory health outcomes remain. Increased effort towards global translation remains a high priority, with further international translation coming from Australia, the USA or collaboration between these two countries.
Acknowledgements
The authors would like to thank the Australian and US students who completed the surveys, and Kai Wang for his assistance with the statistical analysis. Thanks also to the Helen and Geoff Handbury Trust, the Victorian Government (Australia) Future Farming Strategy and the Great Plains Center for Agricultural Health Building Capacity Project for funding.
References
1. Donham KJ, Thelin A (Eds). Agricultural medicine: rural occupational and environmental health, safety, and prevention. 2nd edn. Iowa: Wiley-Blackwell, 2016. https://doi.org/10.1002/9781118647356
2. Bureau of Labor Statistics. Census of fatal occupational injuries in 2011. Washington, DC: U.S Department of Labor, 2012.
3. Safe Work Australia. Work-related traumatic injury fatalities, Australia 2014. Canberra: Safe Work Australia, 2015.
4. DeRoo LA, Rautiainen RH. A systematic review of farm safety interventions. American Journal Preventive Medicine 2000; 18(4 Suppl): 51-62. https://doi.org/10.1016/S0749-3797(00)00141-0
5. Brumby S, Willder S, Martin J. The Sustainable Farm Families Project: changing attitudes to health. Rural and Remote Health (Internet) 2009; 9(1): (1012) Available: www.rrh.org.au (Accessed 23 November 2014).
6. Simmons PD. Rural medicine: its own specialty? Journal of Rural Health 2009; 25(3): 231-232. https://doi.org/10.1111/j.1748-0361.2009.00223_1.x
7. Hegney D. Agricultural occupational health and safety: farming families presenting a challenge to wellness. Australian Journal of Rural Health. 1993; 1(3): 27-33. https://doi.org/10.1111/j.1440-1584.1993.tb00077.x
8. Demos K, Sazakli E, Jelastopulu E, Charokopos N, Ellul J, Leotsinidis M. Does farming have an effect on health status? A comparison study in West Greece. International Journal of Environmental Research and Public Health 2013; 10(3): 776-792. https://doi.org/10.3390/ijerph10030776
9. Mutel CF, Donham KJ. Medical practice in rural communities. New York: Springer-Verlag, 1983. https://doi.org/10.1007/978-1-4757-1804-1
10. Eberhardt MS, Pamuk ER. The importance of place of residence: examining health in rural and nonrural areas. American Journal of Public Health 2004; 94(10): 1682-1686. https://doi.org/10.2105/AJPH.94.10.1682
11. Chondur R, Li SQ, Guthridge S, Lawton P. Does relative remoteness affect chronic disease outcomes? Geographic variation in chronic disease mortality in Australia, 2002-2006. Australian and New Zealand Journal of Public Health. 2013; 117-121.
12. Australian Institute of Health and Welfare. Australia's health 2010. Canberra: AIHW, 2010.
13. Befort CA, Nazir N, Perri MG. Prevalence of obesity among adults from rural and urban areas of the United States: findings from NHANES (2005-2008). The Journal of Rural Health 2012; 28(4): 392-397. https://doi.org/10.1111/j.1748-0361.2012.00411.x
14. Australian Insititute of Health and Welfare. Australian health expenditure by remoteness: a comparison of remote, regional and city health expenditure. Health and welfare expenditure series no. 41. Cat. no. HWE 50. Canberra: AIHW, 2011.
15. Gregory G, Phillips R, Brumby S. Three decades of rural health. In: A Hogan, M Young (Eds). Rural and regional futures. Abingdon, Oxon: Routledge, 2014; 206-225.
16. Fragar L, Depczynski J, Lower T. Mortality patterns of Australian male farmers and farm managers. Australian Journal of Rural Health 2011; 19(4): 179-184. https://doi.org/10.1111/j.1440-1584.2011.01209.x
17. Brumby S, Chandrasekara A, McCoombe S, Kremer P, Lewandowski P. Cardiovascular risk factors and psychological distress in Australian farming communities. Australian Journal of Rural Health 2012; 20(3): 131-137. https://doi.org/10.1111/j.1440-1584.2012.01273.x
18. Miller K, Burns C. Suicides on farms in South Australia, 1997-2001. Australian Journal of Rural Health 2008; 16(6): 327-331. https://doi.org/10.1111/j.1440-1584.2008.01011.x
19. Jones M, Humphreys JS, Prideaux D. Predicting medical students' intentions to take up rural practice after graduation. Medical Education 2009; 43(10): 1001-1009. https://doi.org/10.1111/j.1365-2923.2009.03506.x
20. Scott A, Witt J, Humphreys JS, Joyce C, Kalb G, Jeon SH, et al. Getting doctors into the bush: general practitioners' preferences for rural location. Social Science and Medicine 2013; 96: 33-44. https://doi.org/10.1016/j.socscimed.2013.07.002
21. Wheat JR, Leeper JD, Brandon JE, Guin SM, Jackson JR. The rural medical scholars program study: data to inform rural health policy. Journal of the American Board of Family Medicine 2011; 24(1): 93-101. https://doi.org/10.3122/jabfm.2011.01.100013
22. Kelley MA, Flocks JD, Economos J, McCauley LA. Female farmworkers' health during pregnancy: health care providers' perspectives. Workplace Health and Safety 2013; 61(7): 308-313. https://doi.org/10.1177/216507991306100706
23. Merchant JK, Kross BC, Donham KJ, Pratt DS. Agriculture at risk - a report to the nation. Iowa City: National Coalition for Agricultural Safety and Health, 1989.
24. Donham KJ, Venzke JK. Agricultural Occupational Health Nurse Training and Certification. Journal of Agromedicine 1997; 4(1-2): 105-116. https://doi.org/10.1300/J096v04n01_13
25. Fisher EL, Donham KJ. Agricultural medicine core course: building capacity for health and safety professionals. Journal of Agromedicine 2011; 16(2): 106-116. https://doi.org/10.1080/1059924X.2011.560065
26. McCoombe S, Brumby S. Agricultural health and medicine - a multidisciplinary approach to educating tomorrow's rural and remote health leaders. In: Proceeding , 11th National Rural Health Conference, 13-16 March, 2011. Perth: National Rural Health Alliance, 2011.
27. Brumby S, Cotton J, Todd B. Agriculture, health and medicine: promoting people, places and possibilities across disciplines. In: Proceedings, 13th National Rural Health Conference, 12-14 March, 2015. Darwin: National Rural Health Alliance, 2015.
28. Donham KJ, Thelin A (Eds). Agricultural medicine - occupational and environmental health for the health professions. Iowa: Blackwell Publishing, 2006.
29. Kolb DA. Experiential learning: experience as the source of learning and development. Englewood Cliffs: Prentice Hall, 1984.
30. Kirkpatrick DL. Evaluating training programs: the four levels. New York: Berrett-Koehler, 1998.
31. Mahoney JF, Fox MD, Chheda SG. Overcoming challenges to integrating public and population health into medical curricula. American Journal of Preventive Medicine 2011; 41(4): S170-S175. https://doi.org/10.1016/j.amepre.2011.06.025
32. Tourangeau R, Rips LJ , Rasinski KA. The psychology of survey response. Cambridge, UK: Cambridge University Press, 2000. https://doi.org/10.1017/CBO9780511819322
33. Ary D, Jacobs L, Sorensen C. Introduction to research in education. 8th edn. Belmont, USA: Wadsworth, 2010.
34. Dillman DA. Mail and internet surveys: the tailored design method - update with new internet, visual, and mixed-mode guide. 2nd edn. New York: Wiley, 2007.
35. Wolfe E. Country pasture/forage resource profiles - Australia. Rome: Food and Agriculture Organisation, 2009.
36. Cancer Council of Victoria. Protect your farm's most important asset - you. Melbourne: Cancer Council of Victoria, 2009.
37. Brumby S. Australia and New Zealand. In: KJ Donham, A Thelin (Eds). Agricultural medicine: rural occupational and environmental health, safety, and prevention. 2nd edn. Iowa: Wiley Blackwell, 2016; 487-493.



