Introduction
Supportive relationships are the key to establishing supportive work settings, work places where people want to stay. Mentoring is gaining popularity among Australian rural nurses as a strategy to increase the recruitment of new staff and the retention of current staff. In the workplace, though, there are often different understandings about what mentoring is and how it might play out in practice. There are also other support strategies that need to be considered in the same context.
This article will define the three main supportive relationships identified in the nursing literature: mentoring, clinical supervision and preceptoring. Highlighting the similarities and differences among them will illuminate the range of possible supportive relationships that could be fostered by those who strategically plan for rural health care facilities.
Background
Australian rural nurses: emerging trends
Australian rural nurses work in diverse settings and across a range of practice roles1. The most recent labour force data accounts for 59 301 rural nurses who make up 26.4% of Australia's nursing work force1, p.15. These are nurses who work in a rural town or area with a population centre of fewer than 99 999 and greater than 50002, p.5.
Undoubtedly the most significant issue in rural nursing is a shortage of clinicians. This is being compounded by an ageing work force, poor rates of pay, and the difficulties and conditions of work3. The importance of improving or finding new work-force support strategies for rural nurses was highlighted in the recommendations of recent reviews of nursing carried out by the Australian government: Our Duty of Care4 and The Patient Profession: Time for Action5.
In October 2002, the National Rural Health Alliance (NRHA) convened a stakeholder forum, Action on Nursing in Rural and Remote Areas, in response to a recommendation from the 6th National Rural Health Conference, held in March 20016. The provision of mentoring to support rural nurses was considered to be a high priority due to a number of factors impacting on Australian rural nurses (Table 1).
Table 1: Factors impacting on Australian rural nurses7
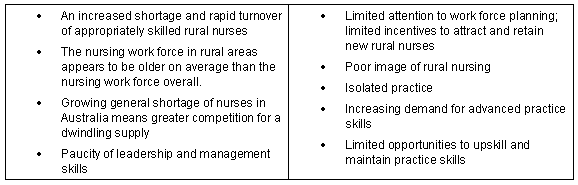
The forum concluded with the preparation of a set of recommendations that would set the rural nursing agenda for NRHA organisations for the next five years. The rural and remote nurses who participated in the forum made their first priority the establishment of mentoring programs.
Supportive relationships in nursing
Mentoring
There is a paucity of literature explicitly dealing with rural nurse mentors. Only one study involving rural nurses and mentoring has been located8. This study examined the outcomes of mentoring partnerships arranged between academic mentors and beginning rural nurse practitioners in the USA.
In Australia, there are formal mentoring programs for undergraduate rural and remote nurses, aged care nurses and re-entry to practice nurses who hold Australian government scholarships. The purported benefit of these scholarships is that they will encourage students from rural and remote Australia to gain nursing qualifications that they will then use on their return home.
The Association for Australian Rural Nurses (AARN) initiated its Mentor Development and Support Project in 2003 to provide training and support for rural nurse mentors involved in the Royal College of Nursing, Australia (RCNA), Undergraduate Mentor Program. This was a direct response by AARN to the recommendations of the Action on Nursing in Rural and Remote Areas forum. A comprehensive evaluation of this project has highlighted the influence of continuing education on rural nurse mentors and the relationships that they form with their mentees (J Mills, pers. data, 2005)9.
Elsewhere in the literature, the Institute of Nursing Executives in New South Wales has been identified as providing mentoring for new nurse managers working in isolated areas. This mentoring program involved both continuing professional development and access to a support network10.
The general literature on mentoring in nursing is vast and, as would be expected, there are many definitions of mentoring from which to draw11-13. However, two important concept analyses of mentoring in nursing, Yoder14 and Stewart and Krueger15, are useful in reaching a consensus on the definition. Concept analysis in nursing is a relatively recent research method that has emerged over the past 20 years. Rodgers' theory of evolutionary concept development16 is often used as a method for undertaking concept analysis. Each of the concept analyses of mentoring drew upon Rodgers' work, which uses a literature-based method14,15,17.
Stewart and Krueger's study15 is described in its title as 'evolutionary', in that it builds on the work of Yoder and follows Rodgers' belief that significant concepts develop and change over time. It is this definition that most adequately reflects the concept of mentoring in nursing today:
Mentoring in nursing is a teaching-learning process acquired through personal experience within a one-to-one, reciprocal, career development relationship between two individuals diverse in age, personality, life cycle, professional status, and/or credentials. The nurse dyad relies on the relationship in large measure for a period of several years for professional outcomes, such as research and scholarship; an expanded knowledge and practice base; affirmative action; and/or career progression. Mentoring nurses tend to repeat the process with other nurses for the socialization as scholars and scientists into the professional community and for the proliferation of a body of nursing knowledge15, p.315.
A comparison of the outcomes of Yoder's and Stewart and Krueger's concept analyses of mentoring in nursing shows that there has been a shift over time, from mentoring being solely a way to promote career advancement, to it being a broader-based concept that includes the development of the body of nursing knowledge14,15.
This conceptual shift is illustrated in Stewart and Krueger's six key attributes of mentoring: that there should be a teaching-learning process; a reciprocal role; a career development relationship; a knowledge or competence differential between participants; and a duration of several years; and that it should be a resonating phenomenon15.
Because of the evolving nature of mentoring, there is a greater emphasis on some attributes of the concept as opposed to others, depending on the context to which it is being adapted. This is important to remember, because scholars trace the ongoing development of mentoring as a strategy in more diverse clinical and academic practice areas such as research, minority student retention, creative thinking, writing and scholarly productivity18-28.
Clinical supervision
As with mentoring, there are many definitions of clinical supervision in nursing29-31. Using Rodgers' method of concept analysis, Lyth examined the literature about clinical supervision in order to clarify the concept and the term that represents it. This definition appears to include the commonly held attributes of clinical supervision and has been adopted for this paper:
Clinical supervision is a support mechanism for practising professionals within which they can share clinical, organisational, developmental and emotional experiences with another professional in a secure confidential environment in order to enhance knowledge and skills. This process will lead to an increased awareness of other concepts including accountability and reflective practice17, p.728.
Clinical supervision is a term not often used in Australian nursing outside of the practice area of mental health29,32. Traditionally, clinical supervision developed in many health disciplines, although primarily in psychotherapy and social work29,30,33. In the UK, clinical supervision for nurses was introduced in the late 1980s, and since then it has become an integral part of clinical governance and quality assurance in the public health system.
Australia has been slow to recognise the place of clinical supervision for nurses. The Australian Health Ministers' Advisory Council recommended that access to formal and informal clinical supervision be available for mental health nurses only29.
The literature about clinical supervision in nursing therefore originates predominantly in the UK, with the landmark work of Brigid Proctor commonly cited as underpinning the implementation of a variety of practice models. Proctor's model of clinical supervision incorporated three key elements: normative (managerial); formative (educative); and restorative (pastoral support)29,30,32,34-40.
There are three main forms of clinical supervision: one-on-one; triad; and group37. Research about the outcomes of clinical supervision has found that group clinical supervision is particularly effective, especially if conducted off-site. Group sessions are also more effective if held frequently (at least monthly) and if they are able to last longer than 60 min29.
Individual or one-on-one clinical supervision is also deemed to be effective, but there is considerable discussion in the literature about potential role conflicts should supervisors also be supervisee's line managers31,41. Conversely, however, there is also an argument that the clinical supervisory relationship can create greater understanding and mutual respect between managers and practitioners42.
Two accounts in the literature discussed the outcomes of clinical supervision for rural nurses in the UK42,43. One in particular explored the use of videoconferencing to facilitate such relationships over a wide geographical area (although their idea of long distances - a 35 mile round trip - and ours would be quite different!). The three rural nurses who wrote their accounts were involved in one-on-one and group clinical supervision. The rural nurses felt that their clinical supervision experiences were valuable in improving their understanding about their practice, as well as increasing their self-awareness and ability to critically reflect43.
Preceptoring
Unlike mentoring and clinical supervision, preceptoring in nursing has not been subjected to a concept analysis. Preceptorship is a method of preparation for practice, utilising clinical staff, as opposed to faculty staff, who provide supervision and clinical instruction to new practitioners: undergraduate or newly registered, or new to a specific clinical environment44,45.
Usually preceptoring relationships are one-on-one. However, another model of preceptorship discussed in the literature is that of the clinical teaching associate, in which healthcare facilities are funded by universities that are seeking clinical placements for undergraduates so that a clinician, the clinical teaching associate, is able to assume responsibility for supervising and teaching a small group of students46.
A preceptor, therefore, can be defined as 'an experienced practitioner who teaches, instructs, supervises and serves as a role model for a student or graduate nurse, for a set period of time, in a formalised programme'47, p.507. Experienced nurses usually assume this role over a short period, in addition to their existing clinical responsibilities. The authors would also argue that another key action of the preceptor is to provide formal feedback on the preceptee's performance to his or her supervisor or lecturer. As a part of their responsibilities, Australian rural nurses often fulfil the role of preceptor to undergraduate nursing students undertaking clinical placements, as well as preceptoring new staff48.
Discussion
In Australia, New Zealand, Canada, the USA and Sweden30,45,49-55 the concepts of mentoring and preceptoring, as defined in this paper, are used consistently in the vast majority of cases. In the Australian literature, there are two exceptions where they become confused. Lo and Brown discuss an undergraduate mentoring program that involves short-term clinical placements and student assessment by mentors56. Similarly, this model of clinical mentoring was reported by Wright57. Morton-Cooper and Palmer refer to this as 'pseudo-mentoring'30, p.46 although it could be argued that this type of supportive relationship really constitutes a model of preceptoring.
The remaining Australian publications about mentoring demonstrate an agreement about the role10,13,44,58-68 that is congruent with the adopted theoretical definition of Stewart and Krueger15. Mixed messages about the definitions of mentor and preceptor are prevalent, however, in the literature from the UK, and it is this writing that has caused authors from other countries to note a continuing thread of confusion in the literature about the terms mentor and preceptor14,59,60,62,65.
Clinical supervision as defined in this article has received little attention in the nursing literature outside of the UK. In Australia, its role in providing a supportive relationship with a clinical focus has not been widely adopted outside the practice area of mental health nursing. A different use of the term clinical supervision can be observed in the nursing literature from Australia, New Zealand and Canada, where it has been written about in relation to the supervision of nursing students on clinical placement69-71.
The literature contains several key areas that provide points of difference between mentoring, clinical supervision and preceptoring. These areas are level of commitment, time, context, relationship reporting and expected outcomes (Table 2).
Mentoring and clinical supervision require a very similar high level of commitment from each participant for the relationship to be established. Both are conducted over long periods; in some cases they can be sustained over years. The main point of difference between these relationships is the focus of discussions between participants. Mentoring allows for a more all-encompassing level of discussion that could range from day-to-day clinical issues to the 'bigger picture' of all parts of the mentee's life - should they choose to discuss such issues. Clinical supervision confines itself to the novice's life as a nurse, although this can often encompass their personal lives as they impact on their work lives. This is described as the pastoral aspect of clinical supervision.
It seems, from the literature, that the boundaries between mentoring and clinical supervision are not clear-cut, and that there are no distinctive characteristics that conclusively define a relationship as either one or the other. In both relationships, participants are accountable to each other with a minimal amount of reporting to the outside world about the discussions that take place within their mutually created space.
Preceptoring, however, is quite different from mentoring and clinical supervision in the levels of time and commitment that characterise relationships, as well as the requirement for formal reporting of the outcomes of the relationship. These outcomes are based on the acquisition of clinical skills that are observable and measurable by the preceptor. Mainly because of the short time frame of preceptoring, the relationship developed is unlikely to be as intense as those formed during mentoring or clinical supervision.
Table 2: Key points of difference between mentoring, clinical supervision and preceptoring

Implications
Mentoring, clinical supervision and preceptoring are extremely important concepts for the development and support of rural nurses. In Australia the concept of clinical supervision and its potential for supporting rural nurses remains largely unexplored, although indications in the literature from the UK are that rural nurses, especially in small groups, stand to benefit from the use of this concept in their practice lives.
Mentoring, with its broader focus, has the potential to develop a professionally stronger and more rounded work force, with the fostering of scholarship and research, as well as clinical expertise, through the development of relationships between wise and experienced rural nurses and those who are beginning their careers as rural nurses. Positive preceptoring experiences for a student or newly graduated nurse experiencing rural nursing for the first time, can shape future career decisions and are vitally important in succession planning.
Each of these support strategies can contribute to a more sustainable rural nursing work force, improving staff retention through the development of more supportive work settings. For nurses contemplating a shift to a rural environment, offering to establish a supportive relationship for them at the beginning of their employment may provide an enticement to try. For existing rural nurses, establishing supportive relationships within the workplace may demonstrate a pragmatic commitment to supporting staff that entices them to stay. Either way, the provision of access to mentoring, clinical supervision and preceptoring is a key measure that needs to be factored into rural health service planning as a matter of course.
Conclusion
Australian rural nursing is problematic for policy-makers and managers on a range of fronts. Going some way towards addressing the difficulty of recruiting and retaining rural nurses is valuing and planning for supportive relationships within the work setting. Mentoring, clinical supervision and preceptoring are all valuable strategies in meeting this particular challenge and are essential tools to be included in strategic work-force planning for the future.
References
1. Australian Institute of Health and Welfare. Nursing labour force 2001. Canberra: AIHW, 2003.
2. Australian Institute of Health and Welfare. Rural, regional and remote health: a guide to remoteness classifications. Canberra: AIHW, 2004.
3. National Rural Health Alliance. Current issues for Australia's rural and remote health workforce. Canberra: National Rural Health Alliance, 2004.
4. Australia Senate Community Affairs References Committee. The patient profession: time for action. Canberra: Senate Community Affairs References Committee Secretariat, 2002.
5. National Review of Nursing Education (Australia). The National Review of Nursing Education 2002: our duty of care. Canberra: Australia Department of Education, Science and Training, 2002.
6. Project Organising Committee. Action on nursing in rural and remote areas - draft: April 2002. Canberra: National Rural Health Alliance, 2002.
7. National Rural Health Alliance. Nursing in rural and remote areas. Canberra: National Rural Health Alliance, 2002.
8. Hanson CM, Hilde E. Faculty mentorship: support for nurse practitioner students and staff within the rural community health setting. Journal of Community Health Nursing 1989; 6: 73-81.
9. Lennon D. kMentor Development and Support Project: achievements and outcomes March 2003-2004. Canberra: Association for Australian Rural Nurses, 2004.
10. Waters D, Clarke M, Harris Ingall A, Dean-Jones M. Evaluation of a pilot mentoring programme for nurse managers. Journal of Advanced Nursing 2003; 42: 516-526.
11. Vance C, Olson R. The mentor connection in nursing. New York: Springer Publishing, 1998.
12. Rolfe-Flett A. Mentoring in Australia. Sydney: Prentice Hall, 2002.
13. Madison J, Watson K, Knight BA. Mentors and preceptors in the nursing profession. Contemporary Nurse 1994; 3(3): 121-126.
14. Yoder L. Mentoring: a concept analysis. Nursing Administration Quarterly 1990; 15: 9-19.
15. Stewart BM, Krueger LE. An evolutionary concept analysis of mentoring in nursing. Journal of Professional Nursing 1996; 12: 311-321.
16. Rodgers B. Concept analysis: an evolutionary view. In: B Rodgers, K Knafl (Eds). Concept development in nursing: foundations, techniques, and applications. 2nd edn. Philadelphia: WB Saunders, 2000, 77-102.
17. Lyth G. Clinical supervision: a concept analysis. Journal of Advanced Nursing 2000; 31: 722-729.
18. Peluchette J, Jeanquart S. Professionals' use of different mentor sources at various career stages: implications for career success. Journal of Social Psychology 2000; 140: 549-565.
19. Byrne MW, Keefe MR. Building research competence in nursing through mentoring. Journal of Nursing Scholarship 2002; 34: 391-396.
20. Byrne MW, Keefe MR. A mentored experience (KO1) in maternal-infant research. Journal of Professional Nursing 2003; 19: 66-75.
21. Thorpe K, Kalischuk R. A collegial mentoring model for nurse educators. Nursing Forum 2003; 38: 5-15.
22. Kalischuk R, Thorpe K. Thinking creatively: from nursing education to practice. Journal of Continuing Education in Nursing 2002; 33: 155-163.
23. Records K, Emerson RJ. Mentoring for research skill development. Journal of Nursing Education 2003; 42: 553-557.
24. Jacelon C, Zucker D, Staccarini J, Henneman EA. Peer mentoring for tenure-track faculty. Journal of Professional Nursing 2003; 19: 335-338.
25. Morrison-Beedy D, Aronowitz T, Dyne J, Mkandawire L. Mentoring students and junior faculty in faculty research: a win-win scenario. Journal of Professional Nursing 2001; 17: 291-296.
26. McGivern DO. The scholars' nursery. Nursing Outlook 2003; 51: 59-64.
27. Wills C, Kaiser L. Navigating the course of scholarly productivity: the protege's role in mentoring. Nursing Outlook 2002; 50: 61-66.
28. Sword W, Byrne C, Drummond-Young M, Harmer M, Rush J. Nursing alumni as student mentors: nurturing professional growth. Nurse Education Today 2002; 22: 427-432.
29. Winstanley J, White E. Clinical supervision: models, measures and best practice. Nurse Researcher 2003; 10: 7-38.
30. Morton-Cooper A, Palmer A. Mentoring, preceptorship and clinical supervision. 2nd edn. Oxford: Blackwell Science, 2000.
31. Howatson-Jones IL. Difficulties in clinical supervision and lifelong learning. Nursing Standard 2003; 17(37): 37-41.
32. Walsh K, Nicholson J, Keough C, Pridham R, Kramer M, Jeffrey J. Development of a group model of clinical supervision to meet the needs of a community mental health nursing team. International Journal of Nursing Practice 2003; 9: 33-39.
33. Houghton C. A mentoring program for new school nurses. Journal of School Nursing 2003; 19: 24-29.
34. Aston L, Molassiotis A. Supervising and supporting student nurses in clinical placements: the peer support initiative. Nurse Education Today 2003; 23: 202-210.
35. Stevenson C, Jackson B. Egalitarian consultation meetings: an alternative to received wisdom about clinical supervision in psychiatric nursing practice. Journal of Psychiatric and Mental Health Nursing 2000; 7: 491-504.
36. Winstanley J. Manchester Clinical Supervision Scale. Nursing Standard 2000; 14(19): 31-32.
37. Sloan G, Watson H. Clinical supervision models for nursing: structure, research and limitations. Nursing Standard 2002; 17(4): 41-46.
38. Teasdale K, Brocklehurst N, Thom N. Clinical supervision and support for nurses: an evaluation study. Journal of Advanced Nursing 2001; 33: 216-224.
39. Teasdale K. Practical approaches to clinical supervision. Professional Nurse 2000; 15: 579-582.
40. Sloan G, Watson H. John Heron's six-category intervention analysis: towards understanding interpersonal relations and progressing the delivery of clinical supervision for mental health nursing in the United Kingdom. Journal of Advanced Nursing 2001; 36: 206-214.
41. Jones A. The influence of professional roles on clinical supervision. Nursing Standard 2001; 15(33): 42-45.
42. Marrow CE, Macauley DM, Crumbie A. Promoting reflective practice through structured clinical supervision. Journal of Nursing Management 1997; 5: 77-82.
43. Marrow CE, Hollyoake K, Hamer D, Kenrick C. Clinical supervision using video-conferencing technology: a reflective account. Journal of Nursing Management 2002; 10(5): 275-282.
44. Barnett T. Preceptorship. In: G Gray, R Pratt (Eds). Issues in Australian nursing 3. Melbourne: Churchill Livingstone, 1992.
45. Ohrling K, Ingalill R. Student nurses' lived experience of preceptorship. Part 1 - in relation to learning. International Journal of Nursing Studies 2000; 37: 13-23.
46. Ryan-Nicholls K. Preceptor recruitment and retention. Canadian Nurse 2004; 100(6): 19-22.
47. Usher K, Nolan C, Reser P, Owens J, Tollefson J. An exploration of the preceptor role: preceptors' perceptions of benefits, rewards, supports and commitment to the preceptor role. Journal of Advanced Nursing 1999; 29: 506-514.
48. Duffy E, Siegloff L, Kent C. Education training and support for Australian rural nurses. Vol. 3. Undergraduate preparation of nurses for rural practice. Canberra: Association for Australian Rural Nurses, 1998.
49. Myrick F. Preceptor questioning and student critical thinking. Journal of Professional Nursing 2002; 18: 176-181.
50. Dilbert C, Goldenberg D. Preceptors' perceptions of benefits, rewards supports and committment to the preceptor role. Journal of Advanced Nursing 1995; 21: 1144-1151.
51. Hall L. Mentoring relationships of New Zealand nurses: an empirical study (part 1). Collegian 1997; 4(4): 28-31.
52. Myrick F, Yonge O. Enhancing critical thinking in the preceptorship experience in nursing education. Journal of Advanced Nursing 2004; 45: 371-380.
53. Ohrling K, Hallberg I. The meaning of preceptorship: nurses' lived experience of being a preceptor. Journal of Advanced Nursing 2001; 33: 530-540.
54. Ohrling K, Hallberg I. Student nurses' lived experience of preceptorship. Part 2 - the preceptor-preceptee relationship. International Journal of Nursing Studies 2000; 37: 25-36.
55. Paton B, Martin S, McClunie-Trust P, Weir N. Doing phenomenological research collaboratively. Journal of Continuing Education in Nursing 2004; 35: 176-181.
56. Lo R, Brown R. A clinical teaching project: evaluation of the mentor-arranged clinical practice by RN mentors. Collegian 2000; 7(4): 8-13,42.
57. Wright C. An innovation in a diploma program: the future potential of mentorship in nursing. Nurse Education Today 1990; 10: 355-359.
58. Pelletier D, Duffield C. Is there enough mentoring in nursing? Australian Journal of Advanced Nursing 1994; 11(4): 6-11.
59. Theobald K, Mitchell M. Mentoring: improving transition to practice. Australian Journal of Advanced Nursing 2002; 20(1): 27-33.
60. Glass N, Walter R. An experience of peer mentoring with student nurses: enhancement of personal and professional growth. Journal of Nursing Education 2000; 39: 155-160.
61. Glass N, Walter R. Exploring women's experiences: the critical relationship between nursing education, peer mentoring and female friendship. Contemporary Nurse 1998; 7: 5-11.
62. Yates P, Cunningham J, Moyle W, Wollin J. Peer mentorship in clinical education: outcomes of a pilot programme for first year students. Nurse Education Today 1997; 17: 508-514.
63. Roberts K. Nurse academics' scholarly productivity: framed by the system, facilitated by mentoring. Australian Journal of Advanced Nursing 1997; 14(3): 5-14.
64. Madison J, Huston C. Faculty-faculty mentoring relationships: an American and Australian perspective. NASPA Journal 1996; 33: 316-330.
65. Madison J. The value of mentoring in nursing leadership: a descriptive study. Nursing Forum 1994; 29(4): 16-23.
66. Madison J, Knight BA, Watson K. Mentoring amongst academics in Australia: a case study. Australian Educational Researcher 1993; 20: 77-91.
67. Wright C. Critical issues in nursing: the need for a change in the work environment. Collegian 1995; 2(3): 5-13.
68. James J, Proctor M. On mentoring. In: G Gray, R Pratt (Eds). Issues in Australian Nursing 3. Melbourne: Churchill Livingstone, 1992.
69. Wellard SJ, Williams A, Bethune E. Staffing of undergraduate clinical learning programs in Australia. Nurse Education Today 2000; 20: 548-554.
70. Kirkpatrick H, Byrne C, Martin ML, Roth ML. A collaborative model for the clinical education of baccalaureate nursing students. Journal of Advanced Nursing 1991; 16: 101-107.
71. McLeland A, Williams A. An emancipatory praxis study of nursing students on clinical practicum in New Zealand: pushed to the peripheries. Contemporary Nurse 2002; 12: 185-193.


