Introduction
A quite comprehensive set of interventions designed to address inequalities in rural-urban health workforce distribution are now in place across Australia. At the undergraduate level these interventions were initially designed around research largely from other countries, that suggests that the chances of health graduates choosing rural practice are increased both by having a rural background, and by being exposed to rural practice during training1-4.
Overseas findings of a rural origin-rural practice correlation among health professionals have proven very robust and are now backed by a growing body of local research3,5-10. The evidence for the effectiveness of rural exposure in training is more variable and less robust3,5,7,11-14. This reflects the relatively short history of these programs, the lack of standardisation of programs among schools, and difficulties in controlling for the effects of pre-existing rural orientation3.
The ultimate test of the effectiveness of undergraduate interventions will be some eventual evening-out of the workforce mal-distribution. This is, however, a long-term prospect and of little help in understanding and managing undergraduate interventions in the short term. This will require more detailed research into the undergraduate experience and subsequent professional trajectories. The proposed Committee of Deans of Australian Medical Schools (CDAMS) tracking study will go some way towards this but it is doubtful whether it can provide the depth or richness of data needed for testing and refining the design and delivery of undergraduate programs, or to inform the ongoing restructuring of rural practice to reflect the changing social and professional aspirations and preferences of emerging cohorts of new practitioners. The effects of wider social changes can be seen already in the changing face of general practice3,15,16. Recent research on Australian youth17 suggests that future undergraduate interventions, and future models of rural practice, will need to take account of an increasing concern with work-life balance, mobility and career flexibility among emerging professionals.
The data reported below represent the initial component of a proposed long-term study to track several cohorts of health science students in the University of Tasmania, Australia, from course entry, through graduation and out into professional practice. It is designed to provide both long-term career trajectory, and short-term attitudinal and course evaluation data. This design does impose some limitations on the interpretation of data drawn from one early-stage component; however, within these limitations, the data do provide some insights into the Tasmanian undergraduate experience. They suggest that the undergraduates participating in the study are generally receptive to spending at least some of their career in rural practice but that present undergraduate interventions used in the Faculty need some refinement if they are to consolidate pre-existing commitments, let alone capture a significant percentage of those without such a commitment.
These preliminary results highlight the importance of ongoing detailed studies into the undergraduate experience in relation to rural practice. Such studies provide the data needed to firstly refine undergraduate interventions, and also to inform thinking about possible future models of rural practice.
Methods
These data were collected in the early weeks of the first semester 2004 through an on-line survey of first and final year students in the Faculty of Health Science at the University of Tasmania in the Schools of Medicine, Pharmacy and Nursing. All students within these years received an email directly from their schools informing them of the study and its purpose and inviting them to log on and complete the survey. All students were sent a further two email reminders before the survey cut-off date.
The survey response rate was 32.4% (148/457) for first years and 23.1% (87/376) for final year students. Despite this comparatively low response rate, available profile data on the target population suggest that the sample is sufficiently representative to support cautious generalisation to, but not beyond, that population. Comparisons across gender and discipline indicated only a slight bias in the sample towards medicine and pharmacy in the first years. Both samples also showed a slight bias towards overseas and interstate students over local. Rural students were slightly over-represented in the sample (64.2% of the sample vs 57.4% of the student population for first years, and 66.7% vs 62.2% for final years). These differences are unlikely to have major implications for the findings with the possible exception of a modest bias towards rurality.
The analysis of the data using SPSS (SPSS Inc, Chicago, IL, USA) was primarily descriptive given the nominal nature of most of the data and limited sample size.
The study was approved by the Human Research Ethics Committee (Tasmania) Statewide.
Results
The sampling frame of first and final year students was chosen with the aim of eventually accumulating comparative baseline (before exposure to rural health training of any sort) and end-of-training data concerning rural health experience and attitudes on a number of cohorts. All undergraduates received some exposure to rural health during their studies through content integrated into other units and/or rural options in clinical placements. Medical students had the option of undertaking a full sixth year rural educational unit placement. While first and final year data are juxtaposed in these results, it is recognised that these are different cohorts and that this places limitations on the interpretation of any comparison of results across the two samples. However, they do present a snapshot of students at the beginning and end of training that is at least suggestive of the processes and changes taking place between the two points.
Rurality
The survey contained a range of questions exploring students' links and attitudes to rural life and practice that were designed to test the relationship between rural origin, rural orientation on entry into training, and rural practice intentions. Approximately half of the total sample was of 'rural origin' with different measures covering the range of 43.9% - 53.4% for first years and 50.6% - 63.2% for final years. However, for the purposes of this paper, measures of rural orientation rather than rural origin are more apposite.
Rural orientation: Two measures of rural orientation are reported here: (i) self-identification as a person who would prefer to live and work in a rural area and: (ii) a more specific measure of a stated intention to enter rural practice on graduation. Over one-third (n = 57, 38.5%) of first years entered training with a preference for rural life and practice in that they agreed or strongly agreed that they 'were the sort of person who would prefer to live and work in a rural area'. This rural preference was considerably stronger among final years with 56.3% (n = 49) agreeing or strongly agreeing with this statement. The shift between first and final years appears to be the result of a move from the neutral position towards a rural preference (Table 1).
Table 1: 'I am the sort of person who prefers to live and work in a rural area'
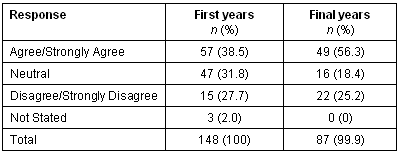
A more specific measure of rural practice orientation was drawn from responses to the statement 'I believe that, after University, I will work in a rural area' (Table 2).
Table 2: 'I believe that, after university, I will work in a rural area (in Australia)'
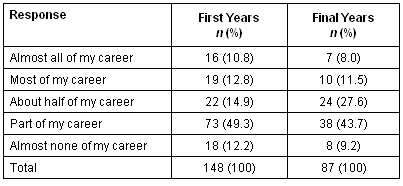
Only 12.2% (n = 18) of first year students ruled out rural practice almost entirely and almost a quarter (n = 35, 23.6%) indicated that they expected to spend the largest part of their career in a rural area. Among final years, this was somewhat lower at 19.5% (n = 7) although the shift was towards a middle position rather than away from rural practice entirely.
For cross-comparison purposes, these responses were collapsed to produce a new trichotomous variable 'rural practice orientation' with the values of orientated ('almost all' or 'most'), somewhat orientated ('about half'), and not orientated ('part' or 'almost none') (Table 3).
Table 3: Rural practice orientation
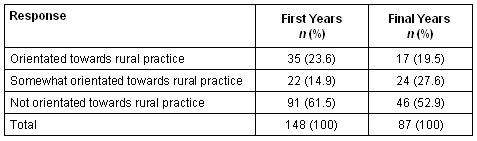
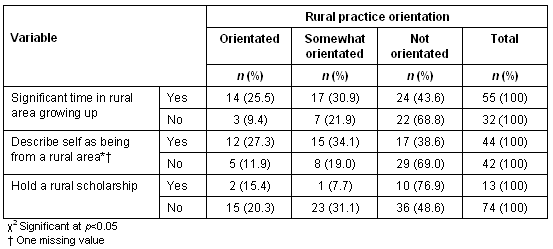
Rural origin by rural practice orientation: There was a strong and statistically significant relationship (tested using c2) among first years between rural practice orientation and both measures of rural origin. Similarly, first year students who held a rural scholarship were also significantly more likely to be rurally orientated (Table 4).
Table 4: First years: rural practice orientation by time in rural area growing up (n = 148)
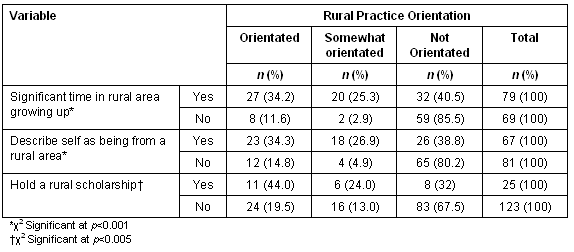
While these relationship appear to hold to some extent among final year students, the only one that remains statistically significant (p = <0.05) is the link between rural orientation and self-description as being 'from a rural area' (Table 5).
Table 5: Final years: rural practice orientation by time in rural area growing up (n = 87)
Future careers
Career commitment: A large percentage of first years appear to enter training with already well-developed ideas about their future career path with 54.7% (n = 81) 'very' and 27.7% (n = 41) 'somewhat' committed to a particular career path. They were less committed to a particular practice environment (ie, rural or urban), although 58.8% (n = 87) indicated at least some pre-existing commitment to one or the other.
Final year students appear less settled in their commitment to both a career trajectory and a practice environment with a general shift towards the middle 'somewhat committed' position. Overall, by far the largest percentage of students (82.4% [n = 122] of first years and 82.7% [n = 72] of final years) do have at least some commitment to a particular career path, and two-thirds (58.8% [n = 87] of first years and 64.3% [n = 56] of final years) to a particular practice environment.
Career commitment by rural orientation: Cross-tabulation of career path commitment against rural practice orientation reveals a significant relationship among first year subjects. Of the 35 first years who were 'orientated to rural practice', 85.7% (n = 30) also indicated that they were 'very committed' to a particular career path (c2 = 18.845, p = <0.05). That is, there appears to be a particularly high sense of vocational commitment among those first years intent on a career in rural practice.
In comparison, of the 19.5% (n = 17) final years who report being orientated to rural practice, only 35.3% (n = 6) came into the 'very committed' category in terms of career path. The movement again appears to be towards the middle position with 52.9% (n = 9) being 'somewhat committed'. The numbers here are too small to warrant statistical testing.
When career path commitment is cross-tabulated with the broader measure of rural orientation the pattern is less pronounced but statistically stronger. Almost two-thirds (n = 36, 63.2%) of the 57 (38.5%) first years who agreed that they were 'the sort of person who would prefer to live and work in a rural area' were also 'very committed' to a particular career path (c2 = 53.22, p = <0.001). In comparison, of the 41 students who 'disagreed' with the statement ─ and therefore presumably had a preference for an urban environment ─ only 48.8% (n = 20) were 'very committed' to a specific practice environment.
While among the final year cohort there was a greater percentage of students who expressed a preference for the rural environment (56.3% [n = 49] compared with 38.5% [n = 57] for first years) the association with greater career path commitment among this group had all but disappeared with 38.8% (n = 19) indicating they were 'very committed' to a particular career path while 42.9% (n = 21) were 'somewhat' committed.
Overall there appears to be a particularly strong sense of vocation among those first years with an interest in rural practice whereas final year students, including those with some rural commitment, appear more open to a range of possibilities.
Career aspirations and practice intentions
Respondents were asked a number of questions designed to explore in more detail the issues surrounding future career path choices.
Practice environments: Respondents were asked to indicate the proportion of their career they expected to spend in capital city, rural, remote and/or overseas practice (Tables 6,7).
Table 6: First Year Students: 'I will work in . . .'
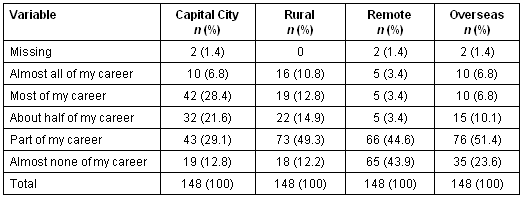
Table 7: Final Year Students: 'I will work in . . .'
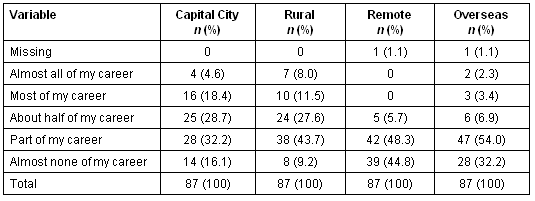
In terms of rural and capital city practice choices, there is a marked middle tendency with few indicating the extremes of intending to spend 'almost all' or 'almost none' of their careers in one or the other location. There appears to be a fall in even these small percentages between first and final years, with only 4.6% (n = 4) final years intending to spend 'almost all' of their careers in a capital city and only 8.0% (n = 7) committing to an almost entirely rural career. The total percentages for the three middle responses were remarkably steady across both categories and year groups at 79.1% (n = 117) and 79.3% (n = 69) for first and final years, respectively, for capital city practice and 77.0% (n = 114) and 82.8% (n = 72) for rural practice.
The pattern for remote and overseas practice is generally more polarised with the bulk of responses for both first and final years bunched around the 'part' or 'almost none' categories. There appears to be a greater readiness to work overseas than in remote areas with all but 23.6% (n = 35) of first years and 32.2% (n = 28) of final years intending to spend at least part of their professional practice lives overseas.
Overall, the responses suggest that both cohorts are very open to a variety of practice environments with only small numbers committed to, or ruling out, one environment or another. It does appear, however, that the capital city option is the one with widest appeal and the remote option the least, although even here almost two-thirds of students intend to spend some time practising in a remote area.
Practice conditions: Respondents were asked to rate the importance of certain factors in considering their future career choices (Table 8).
Table 8: Factors rated 'Important' or 'Very Important' in considering future career path
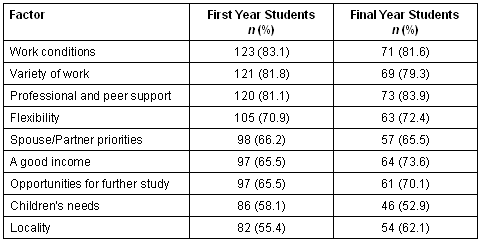
These questions were primarily designed to map changing patterns over time and between cohorts, not as a simple ranking. Nevertheless, these first data do provide some indication of students' career concerns.
Three factors related directly to the realities of day-to-day professional practice (professional and peer support; work conditions; and variety of work) were most often rated, by both first and final years, as 'very important' or 'important'. Factors frequently identified as issues in the rural practice literature (locality; flexibility; opportunities for further study; and spouse/partner and children's needs) while still seen as important, did not appear to be of major concern to the respondents. In particular, locality and children's issues rated quite lowly as a concern, even among the older final year students. There were few notable differences in response patterns between first and final year students. The most substantial difference was found in regard to 'income' which 8.1% more final than first year students rated as important or very important.
Perceptions of rural practice
Students were asked how informed they felt about rural practice (Table 9).
Table 9: How informed about rural practice by discipline
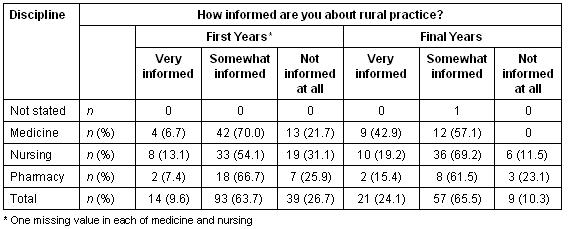
Approximately three-quarters of first years felt themselves to be at least 'somewhat informed' about rural practice, although only small numbers of these reported being 'very informed'. First year pharmacy and nursing students appeared to enter training a little less well informed than their medical colleagues. These students, especially the pharmacy students, also appeared to have made only modest gains by final year compared with medical students who all felt themselves at least 'somewhat informed'.
Respondents were then asked to indicate their agreement or disagreement with a series of statements about rural practice (Table 10).
Table 10: Agreement with statements about rural practice
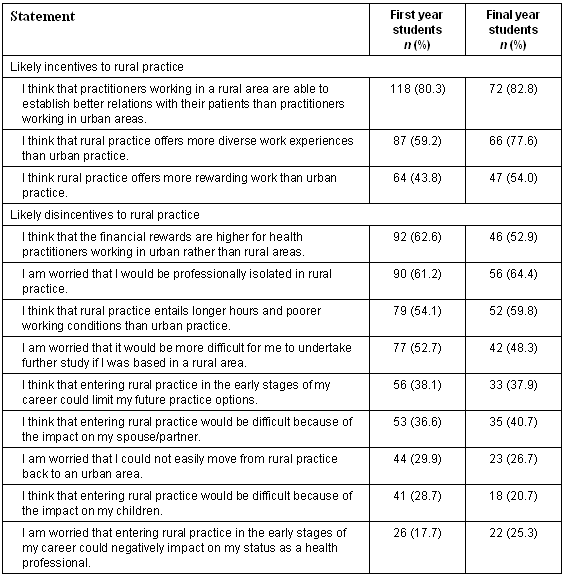
The most strongly held perception was that rural practice provides opportunities for better patient relations with 80.3% (n = 118) of first years and 82.8% (n = 72) of final years agreeing to this statement. Other than this, frequencies were generally below 60%, suggesting that the perceptions that students do have, whether they are positive or negative, are not particularly strongly formed. Issues of status, flexibility/mobility and the impact on partners and children, all of which are prominent concerns in the literature about rural practice, do not appear to have been picked up to any great extent by undergraduates.
The only issue on which there was a substantial difference between the two cohorts is that of 'diversity of practice' with 77.6% (n = 66) of the final years agreeing that rural practice offers more diversity of experience compared with only 59.2% (n = 87) of first years. Final years were less likely than first years to agree that urban practice provides better financial rewards than rural practice (n = 92, 62.6% vs n = 46, 52.9%) and more likely to agree that rural practice provides more rewarding work (n = 47, 54.0% vs n = 92, 62.6%).
Undergraduate exposure to rural health
Coursework: Most students in the Faculty of Health Sciences at the University of Tasmania have some exposure to rural health during their training, either through rural placement, rural curriculum content and/or membership of the undergraduate rural health club RUSTICA (Table 11). Rural curriculum content in all schools is developed and delivered by professionals with rural practice experience.
Table 11: Forms of rural health course content by discipline: final year students
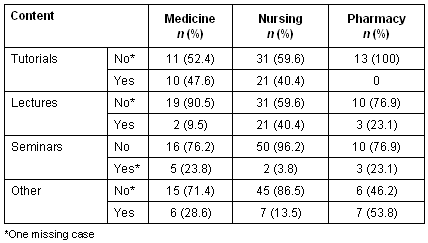
Although the majority of final year students (n = 51, 62.2%) recalled undertaking some form of rural coursework in the previous year, there was still a substantial portion (n = 31, 37.8%) who did not. Medical students were more likely than nursing or pharmacy students to remember such coursework (n = 16, 76.2% compared with n = 27, 51.9% and n =7, 53.8% for nursing and pharmacy, respectively).
The survey revealed quite a low level of agreement among students as to just what forms this rural coursework took within their schools. While this raises issues about reliability of the students' recall, it is also likely to be related to the degree to which rural coursework is presented in a manner that makes it clearly identifiable as such.
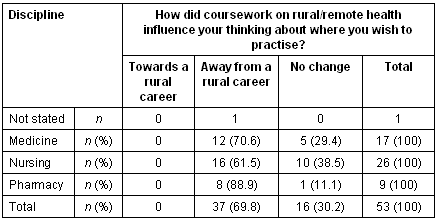
Coursework impact: When asked how this exposure influenced their thinking about eventual rural practice (Table 12), none of those who recalled undertaking rural coursework felt that it had influenced them towards a rural career. In fact, over two-thirds (n = 37, 69.8%) felt that this exposure had actually influenced them away from such a career. The remainder reported no change. There was strong support among students for increased rural and remote coursework with 74.0% (n = 37) of nursing students and 84.6% (n = 11) of pharmacy students indicating that they would like to see such content increased. Less than half of medical students (n = 10, 47.6%) shared this view.
Table 12: Coursework influence by discipline
Rural placement: All of the final year pharmacy and medical students and 71.2% (n = 37) of nursing students reported having undertaken some form of rural placement during training. At the time of the study, placements programs were generally short term (2 or 3 weeks) although Medicine did provide a full final year rural placement option for limited numbers of students. Three students only (two in medicine and one in pharmacy) reported that their placement experience influenced them towards a rural/remote career; whereas, 40.2% (35) overall reported placement influenced them away from a rural/remote career. This effect was relatively consistent across all disciplines.
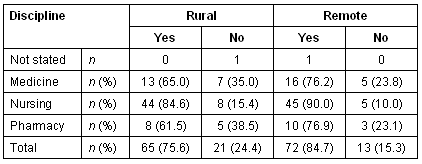
There was also strong support across the disciplines for more opportunities for both rural and remote placements particularly in respect of rural placements (Table 13).
Table 13: Support for increased opportunities for rural and remote placement
Rural scholarships: Of the 13 final year students holding a rural scholarship of one form or another, only 6 (46.2%) indicated that being a scholarship holder had influenced them towards rural practice while 2 (15.4%) felt that it had actually influenced them 'away' from a rural career.
Discussion
These early data suggest that the task facing those designing and delivering undergraduate interventions to these students may not be so much one of persuading them towards rural practice, as not souring an already established interest. They also highlight the need for very close attention to the quality, and evaluation of the efficacy, of these interventions which may, if not appropriately designed and delivered, have an overall deleterious effect on rural practice intentions.
Three-quarters of students responding to the survey appear receptive to the idea of living and working in a rural area with only one in 10 completely ruling out rural practice. This is not entirely unexpected because the strong link between rural origin and rural practice orientation is already well-established and this is a very rural sample. There are, however, still substantial numbers in the sample from non-rural backgrounds who are at least somewhat orientated to rural life and practice.
The majority of the students appear to have entered training with already well developed ideas about career path and preferred practice environment. This is particularly the case with those students with a rural orientation who appear to have a very strong sense of vocation. Even given the limits imposed by comparing different cohorts, the data from first and final years suggest that the undergraduate experience had done little to strengthen either the sense of vocation or interest in rural practice among these students. Not only are final year students somewhat more equivocal than first years in their commitment to rural practice, but also the relationship between origin and orientation appears weaker than for first years.
When questioned in more detail about the environments in which students expected to work on graduation, the most striking feature was the spread of the responses. Very few envisaged spending the bulk of their career in just one environment. This was particularly the case for the rural and urban practice split, with the vast majority expecting to spend at least part of their career in each setting. There was a narrower response range in terms of remote and overseas practice, because more than half of the students envisaged spending at least some time in remote practice and almost three-quarters planned some time working overseas. This provides support for a stronger focus on 'easy entry - gracious exit' models of rural and remote practice18.
First and final year students were also quite similar in the range of factors they nominated as being important in considering future career paths. Three factors topped the list for both cohorts, albeit in slightly different order: work conditions, variety of work and professional and peer support. These are all related to the immediate concerns of day-to-day professional practice. It is not surprising, given the effort and focus required to successfully train as a health professional that these 'getting out there and doing the job' issues would be uppermost in students' consideration.
The data show that most of these students entered training with some knowledge of, and quite well developed perceptions about, rural practice. While only medical students report a substantial increase in knowledge by final year, the pattern of detailed perceptions of all students remains quite similar for first and final year cohorts, especially in terms of the perceived disincentives. One positive stood out in both cohorts: they saw rural practice as conducive to better patient relations. The final year cohort also felt that it offered a more diverse practice experience. Both of these match quite well with the more important factors in practice decisions identified above. However, two of the most strongly perceived disadvantages of rural practice - professional isolation and longer hours - are also identified as major factors in choosing a career.
Importantly, many of the factors that emerge in the literature as major issues for mature rural practitioners do not appear to loom large for these undergraduates, either in terms of the important factors in career choice or in perceptions about the disincentives of rural practice. These disjunctions between undergraduate and mature practitioner concerns could be seen to support an argument that undergraduate views are of limited relevance in this context. However, while these concerns may change after a few years in practice, present concerns will be the ones to shape students' reactions to the undergraduate rural practice experience and crucial early career decisions.
All three disciplines within the Faculty provide students with exposure to rural practice, primarily through rural placement but also through limited coursework content. Although students had only patchy recall of coursework interventions, they were very supportive of increased coursework and placements. One concerning outcome of this study was the reported impact of these interventions. The overwhelming majority, across all three disciplines, reported that the rural course content actually discouraged them from pursuing rural practice and none reported that it influenced them towards that choice. Placement appeared a little more effective. Small numbers in medicine and pharmacy reported that placement had encouraged them towards rural practice and, except in pharmacy and unlike the coursework, the numbers reporting no effect were greater than those reporting a negative effect.
These results, above all, highlight the need for more detailed and structured evaluative research on the undergraduate experience within the Faculty, particularly the short- and long-term effectiveness of coursework interventions. They strongly suggest that the majority of the sample are well disposed towards rural practice, are open to a wide range of practice experiences and envisage spending at least part of their professional life practising in a rural area. The concern is that there is not a lot of evidence to suggest that this is translating into eventual patterns of practice and/or that the effort going into undergraduate interventions is having any substantial effect in consolidating that interest into commitment.
This may be related to the nature of the interventions. Overseas evidence is based largely on cases involving multiple intensive strategies including selective recruitment and full immersion in family and rural practice. The interventions in the present case are much more modest. Placements are generally short term (1-3 weeks) and coursework was in the form of quite restricted 'add-ons' or 'add-ins' to core curricula. It may also be related to the disjunctions between the expectations of new graduates and the realities of rural practice as it is presently structured in this state.
Even within the limits of what is a small sample, quite a low response rate and a pseudo cohort design, these data raise interesting questions around the undergraduate experience of rural practice. These are questions that will only be answered, and appear worth addressing, by more detailed high quality studies focussed specifically on the local and general contexts of undergraduate, and immediately post-graduate experience of rural practice.
Conclusion
While the ultimate measure of the success of undergraduate interventions will be workforce changes over time, it is clearly important not to wait that long to assess their efficacy. Steering students towards rural practice requires finding concordances between students' career and personal aspirations and their undergraduate experience of rural practice. This requires careful design of coursework, detailed planning of the placement experience and long-term strategies to address those aspects of rural practice that are of most concern to these emerging health professionals. All of this requires a good understanding undergraduates and the way they experience of rural health. It does not supplant the need for studies on the mature rural practice experience, but it cannot be assumed that an understanding of one can be generalised to the other.
References
1. Brooks R, Walsh M, Mardon R, Lewis M, Clawson A. The roles of nature and nurture in the recruitment and retention of primary care physicians in rural areas: A review of the literature. Academic Medicine 2002; 77: 790-798.
2. Campos-Outcalt D, Senf J, Watkins A, Bastacky S. The effects of medical school curricula, faculty role models, and biomedical research support on choice of generalist physician careers: a review and quality assessment of the literature. Academic Medicine 1995; 70: 611-619.
3. Dunbabin J, Levitt L. Rural origin and rural medical exposure: their impact on the rural and remote medical workforce in Australia. (Online) 2003. Rural and Remote Health 3: 212. Available: http://rrh.org.au (Accessed 19 September 2005).
4. Crump W, Barnett D, Fricker S. A sense of place: Rural training at a regional medical school campus. Journal of Rural Health 2004; 20: 80-84.
5. Easterbrook M, Godwin M, Wilson R. Rural background and clinical rotations during medical training: effect on practice location. Canadian Medical Association Journal 1999; 160: 1159-63.
6. Laven GA, Wilkinson D, Beilby J, Pratt N. Are medical students of rural origin more likely to become rural general practitioners than students of urban origin? A national case-control study. In: Procedings, World Rural Health 2002; 1-3 May 2002; Melbourne: World Organisation of Family Doctors (WONCA); 2002; 1-10.
7. Laven G, Beilby J, Wilkinson D, McElroy H. Factors associated with rural practice among Australian-trained general practitioners. Medical Journal of Australia 2003; 179: 75-79.
8. Laven G, Wilkinson D. Rural doctors and rural backgrounds: How strong is the evidence? A systematic review. Australian Journal of Rural Health 2003; 11: 277-284.
9. Wilkinson D, Beilby J, Thompson DJ, Laven GA, Chamberlain N, Laurence OM. Associations between rural background and where South Australian general practitioners work. Medical Journal of Australia 2000; 173: 137-140.
10. Rabinowitz HK. Recruitment, retention, and follow-up of graduates of a program to increase the number of family physicians in rural and underserved areas. New England Journal of Medicine 1993; 328: 1-11.
11. Peach H, Barnett N. Effects of an early rural placement on internship choices of medical students. Medical Education 2002; 36: 8.
12. Peach H, Trembath M, Fensling B. A case for more year-long internships outside metropolitan areas? Medical Journal of Australia 2004; 180: 106-108.
13. Wilkinson D, Laven G, Pratt N, Beilby J. Impact of undergraduate and postgraduate rural training, and medical school entry criteria on rural practice among Australian general practitioners: national study of 2414 doctors. Medical Education 2003; 37: 809-814.
14. Wilkinson D. Evidence-based rural workforce policy: an enduring challenge. Rural and Remote Health 3: 224.(Online) 2003. Available: http://rrh.org.au (Accessed 19 September 2005).
15. AMA/RDAA, Rural and Remote Area Working Group. AMA/RDAA Discussion Paper: Increasing Rural Medical Services. Discussion Paper. Canberra: Australian Medical Association and Rural Doctors' Association of Australia; 1998.
16. Brooks PM, Lapsley HM, Butt DB. Medical workforce issues in Australia: "tomorrow's doctors - too few, too far". Medical Journal of Australia 2003; 179: 206-298.
17. Wyn J. Youth transitions to work and further education in Australia. Procedings: American Educational Research Association 2004 Annual Meeting; April 12-16 2004; San Diego. 2004.
18. Boucher M, Lynch M. Easy entry, gracious exit. Newcastle: NSW Rural Doctors Network and Commonwealth Department of Health and Ageing, 2003.
Abstract
Introduction: There are still large gaps in the evidence base for the effectiveness of Australian undergraduate rural coursework and placements programs designed to increase the numbers of health graduates choosing rural practice. This article reports on an online survey conducted in 2004 of health science students at the University of Tasmania, Australia, designed as a part of a long-term study to test coursework interventions by tracking students' attitudes to, and experience of, rural practice from course entry to eventual practice.
Method: All first and final year students in medicine, nursing and pharmacy in the Faculty of Health Science were invited to complete an online survey exploring the undergraduate experience of rural health.
Results: The survey was completed by 148 first year and 87 final year students, a response rate of 32.4% and 23.1% respectively. Over one-third (38.5%) of first years and 56.3% of final years indicated a general preference for rural life and practice and almost 90% expected to spend at least some of their career in rural practice. There was a statistically significant relationship between rural practice orientation and rural origin among first years, although this relationship was weaker among final years. Of first years, 82.4%, and 82.7% of final years appear to have made at least some commitment to a particular career path, and two-thirds to a particular practice environment. Rurally oriented first year students were significantly more committed to a career path than those without that orientation, although this did not hold for final years. When asked how much of their careers they expected to spend in capital city, rural, remote and/or overseas practice, both first and final year students' responses were notable for their spread. Few ruled rural or urban practice in or out entirely with most opting for middle range responses of 'most', 'about half' or 'part' of their career. Over half of both years expected to spend some time in remote practice and 75.1% of first years and 66.6% of final years some time in overseas practice. The factors rated most important in relation to career choice were those related directly to the realities of day-to-day professional practice ─ professional and peer support, work conditions and variety of work. Approximately three-quarters of those entering undergraduate education felt themselves to be at least 'somewhat informed' about rural practice but, apart from medical students, were little better informed by final year. The only perception of rural practice very widely shared (by more than 80% of respondents) was the possibility of developing better patient relations. Many of the other factors frequently identified as major issues in the rural practice literature - locality, flexibility, opportunities for further study, and spouse/partner and children's needs - while recognised by some, do not appear to loom large with undergraduates either in terms of career choice or perceptions of rural practice. Most final year students recalled receiving specific rural health training through rural placements and/or rural curriculum content. Overall recall of coursework was patchy, although placements were well-remembered and there was good support for increases in both. None of those who recalled undertaking rural coursework felt that it had influenced them towards a rural career and over two-thirds (n = 37, 69.8%) felt that this exposure had actually influenced them away from such a career. Three students reported that undertaking a rural placement influenced them towards, and 35 away from, a rural/remote career.
Conclusion: The ultimate measure of the success of undergraduate interventions will be workforce changes over time. In the meantime more research is needed into undergraduate experience of rural health to provide the data needed for the careful design of coursework, detailed planning of the placement experience and long-term strategies to address those aspects of rural practice that are of most concern to these emerging health professionals.
Keywords: career choice, medical education, undergraduate.
You might also be interested in:
2016 - A pilot videoconference group stress management program in cancer survivors: lessons learned
2006 - Funding sources and consequences: the subverting of an Indigenous community outreach program

