full article:
IntroductionA national survey in 2010 reported a density of 219.0 medical doctors per 100 000 people in Japan1, and Ibaraki Prefecture has the second lowest. This is especially in the Hitachi Medical Care Zone and the Hitachiota-Hitachinaka Medical Care Zone in northern Ibaraki (Fig1), where the density is 115.0 medical doctors per 100 000 population, and the total population is approximately 628 0002,3. The University of Tsukuba Hospital is the hub for medical care in the prefecture and is the authors' base of clinical activity (F1). It takes 1-2 hours by car to travel the 60-120 km from Tsukuba to these zones. The number of elderly single patients there has increased4,5, and these people have difficulty travelling to specialty outpatient clinics in Tsukuba. These zones have only four full-time plastic surgeons6,7. Therefore plastic surgeons rotate through clinics to perform minor surgeries. During these rotations, a case with a mild hematoma was noted. It was fortunately absorbed without any invasive procedures. However, hematomas cannot always be resolved conservatively. This experience led the authors to devise a simple, novel method of Penrose-drain fixation.
The Penrose drain was first reported in 18898,9. This device drains fluid exuded postoperatively from the subcutaneous, subfascial, intraperitoneal or retroperitoneal cavities and prevents accumulation of blood or other fluids. The Penrose drain is usually sutured to the skin, but is occasionally fixed against migration with tape or a safety pin. To prevent retrograde infection, the drain should be removed after wound discharge has decreased10.
In this retrospective study, cases in which Penrose drains were fixed using the new method and those using a conventional fixation method were compared.
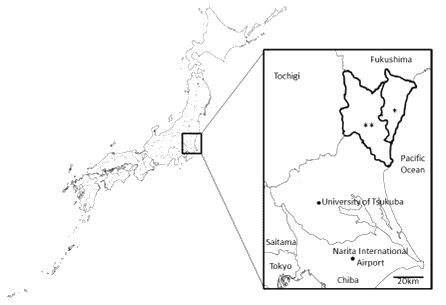
Figure 1: Surgeries in the study cases were performed in outpatient clinics in the Hitachi (*) and Hitachiota-Hitachinaka (**) medical-care zones (see inset) of Ibaraki Prefecture (magnified in the inset) in Japan. These two zones include seven cities, one town, and one village (Hitachi, Takahagi, Kitaibaraki, Hitachiota, Hitachiomiya, Hitachinaka, Naka, Daigo, and Tokai).
Patients
The medical records of patients who underwent minor surgeries involving Penrose drains were retrospectively analyzed. The surgeries were performed from April 2012 to March 2015 in outpatient clinics of hospitals in northern Ibaraki (Fig1) affiliated with University of Tsukuba Hospital. This area encompasses the Hitachi and Hitachiota-Hitachinaka healthcare zones, as shown in the map in Figure 1. There was no available certified nurse in wound, ostomy and continence nursing who could remove wound drains in the institutions at this study. For each case, the patient's age, sex, body mass index and lesion; and the surgical site, closure technique (a simple closure or a closure with local skin flaps or anchor sutures), method of fixing and removing the Penrose drain, and any complications related to the Penrose drain, were recorded. Patients who said they could not come to the outpatient clinic until removal of stitches had drains fixed to their wound dressings, whereas patients who said they could come to the outpatient clinic on postoperative day 1 or 2 had the drain fixed to their skin. When the authors analyzed the medical records at this study, the former were assigned to the method group, and the latter to the control group. Patients taking anticoagulants were not excluded, and anticoagulants were not suspended at the time of surgery. The cases were divided into two groups according to the method of fixing the Penrose drain.
Penrose drains
In each case, a Penrose drain (Penrose Drain AR, type A No.4, 0121004, Huji Systems Corporation, Tokyo, Japan) was inserted into the subcutaneous layer and fixed either by the new method or by the conventional method of suturing the drain to the skin. Some Penrose drains were shortened or reduced in width before use, according to the amount of accumulating fluid; these changes were independent of the fixation technique. The entire length of the Penrose drain carries radio-opaque markers to prevent losing the drain in case of breakage, especially at the suture site.
Penrose-drain fixation methods
Penrose drains that were sutured to the skin used 4-0, 5-0, or 6-0 nylon sutures, as with other skin sutures. Penrose drains fixed by the new technique were sewn onto the wound dressings, which were gauze, Adaptic Dressing (7.6 × 7.6 cm, 514010, Nippon Sigmax Co., Ltd., Tokyo, Japan), Adaptic Finger Dressing (L, 2.8 cm, 3.0 × 12.7 cm, 514052, Nippon Sigmax Co., Ltd.), Adaptic Toe Dressing (L, 2.8 cm, 4.0 × 7.6 cm, 514054, Nippon Sigmax Co., Ltd.), or Sofratulle (10 × 10 cm, Sanofi K.K., Tokyo, Japan) (Fig2). In the control group, the Penrose drain was sewn to the skin on the wound margin using conventional methods.
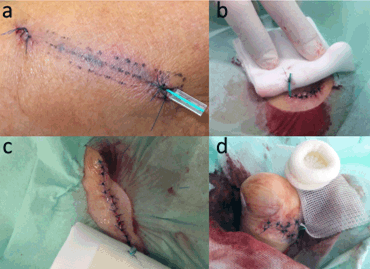
Figure 2: Photographs taken just after Penrose-drain fixation showing (a) conventional fixation after a piece of wood was removed from the left forearm, and (b-c) the new method of Penrose-drain fixation, used with various wound dressings. The Penrose drain was directly sutured to the wound dressing rather than to the skin. (b) The drain was sutured to an Adaptic dressing after the removal of an epidermal cyst from the right back; (c) to gauze after the removal of a lipoma on the right shoulder; and (d) to an Adaptic Toe Dressing after the removal of a ganglion from the first toe on the right foot.
Wound closure
Dermostitching was performed with 4-0, 5-0 PDS-II (Z463H/Z464H, Johnson and Johnson K.K., Tokyo, Japan) or 4-0, 5-0 nylon sutures (HP1304NB45-KF2/HP1305NB45-KF2, Alfresa Pharma Corporation, Osaka, Japan). Dermostitching was omitted in palms and plantar cases. Superficial skin suturing was performed with 4-0, 5-0, or 6-0 nylon (HP1306NB45-KF2, Alfresa Pharma Corporation).
Postoperative precautions explained to patients
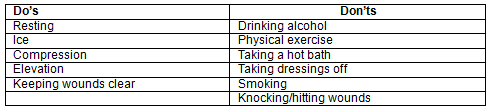
All patients were instructed to avoid drinking alcohol, taking a bath or exercising on the day of surgery (Table 1, right column). Patients in the new-method group were instructed to remove the whole wound dressing on postoperative day 1 or 2 and to check whether the Penrose drain was removed with the dressing; if so, they were to return to the clinic on one of postoperative days 7-14 for suture removal. Patients were instructed to visit another doctor if the Penrose drain was not automatically removed. Patients in the control group were instructed to come to an outpatient clinic within a few days of surgery, when the wound discharge was sufficiently reduced, to have the Penrose drain removed by other doctors.
Regardless of the method of drain removal (automatic or by a doctor), the patients in both groups were instructed to remove the dressing, wash the wound with tap water, and apply ointment and a new adhesive plaster on the wound each day until the sutures were removed.
Statistical analysis
Data are presented as means ± standard deviations for continuous variables and as the total number for binary variables. Statistics were analyzed by Fisher's exact test. All statistical analyses were performed with EZR11 (Saitama Medical Center, Jichi Medical University, Saitama, Japan), which is a graphical user interface for R (The R Foundation for Statistical Computing, Vienna, Austria). More precisely, it is a modified version of R Commander designed to add statistical functions frequently used in biostatistics.
Ethics approval
At the time of the study, the hospitals in which surgeries were performed had no ethics committee. The research was a retrospective research involving anonymized records available in the authors' data sets where appropriate informed consent had already been obtained. The study followed ethical principles of the University of Tsukuba Hospital and the Declaration of Helsinki.
Results
A total of 65 cases of minor surgery performed on outpatients under local anesthesia were assessed. In each surgery, a Penrose drain was fixed either by the new method, in which the drain was fixed to the wound dressing, or by the conventional method of suturing the drain to the skin. The new-method group included 54 Penrose drains placed in 48 lesions in 44 patients; the control (conventional-method) group included 36 Penrose drains in 25 lesions in 21 patients.
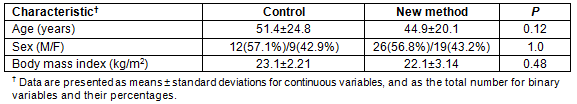
The patient demographics are shown in Table 2. The average patient age was 44.9±20.1 years in the new-method group, and 51.4±24.8 years in the control group. There were 25 men (56.8%) and 19 women (43.2 %) in the new-method group, and 12 men (57.1%) and 9 women (42.9 %) in the control group. The average body mass index was 22.1±3.14 in the new-method group, and 23.1±2.21 in the control group.
The numbers of patients who used anticoagulants or antiplatelet drugs were 1 (2.3%) in the new-method group and 3 (14.3%) in the control group. There was no significant difference among them.
Surgical sites, lesions and closure techniques
Surgeries included in this study were performed on the head and neck (22.9%), trunk (45.8%), upper extremities (16.7%), and lower extremities (14.6%) in the new-method group (Fig3, top right); and on the trunk (64.0%), upper extremities (20.0%), and lower extremities (16.0%) in the control group (Fig3, top left).
In the new-method group, the surgeries were performed to treat benign tumors (62.5%), malignant or borderline-malignant tumors (4.2%), trauma-related lesions (4.2%), for aesthetic reasons (16.7%), and other (12.5%) (Fig3, middle right); in the control group, surgeries were performed for benign tumors (32.0%), trauma-related lesions (8.0%), aesthetics (44.0%), and other (16.0%) (Fig3, middle left).
In the new-method group, wounds were closed with simple closure in 75.0% of cases, and with local flaps or anchor sutures in 25.0% of cases (Fig3, bottom right); in the control group, wounds were closed with simple closure in 48.0% of cases, and with local flaps or anchor sutures in 52.0% of cases (Fig3, bottom left).
In the new-method group, all 54 Penrose drains (100%) were automatically removed with the wound dressing without the assistance of a physician; none of the drains in the control group were automatically removed. This was a significant difference between the two groups.
Neither group had any Penrose-drain-related complications, such as massive hematoma requiring additional treatment, retrograde infection, seroma or breakage and straying of the drains. There was no significant difference in complications between the two groups.
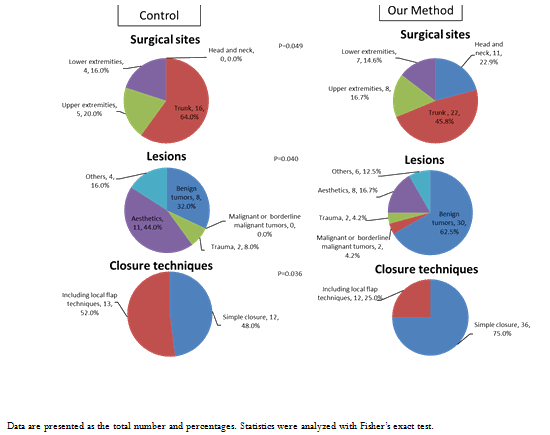
Figure 3: Surgical site (top), reason for surgery (middle) and closure technique (below) for cases in the control (left) and new-method (right) groups.
Discussion
In this study, using the new Penrose-drain fixation technique successfully prevented hematoma in the analyzed cases without any risk elevation of complications in rural remote areas, where postoperative management might be poor. This new method has the potential to reduce complications that arise from not using a Penrose drain when it would be advisable but is not practical because of the limited availability of postoperative care. The cost of patients, time of surgeons and general healthcare costs that were necessary for the removal in the conventional management were not necessary with the new technique. A search of the literature indexed in PubMed with automatic, remove, Penrose, drain did not reveal any methods of Penrose-drain insertion designed for intentional automatic removal, so this is a first report of the Penrose drain in such a use.
Even in patients taking anticoagulants, the new fixation method can be used safely without suspending anticoagulant treatment. Compression is the most important general postoperative precaution (Table 2, left), followed by rest, icing and elevation. Compression is particularly important, because platelets, which affect primary hemostasis in the acute postoperative phase, are activated by shear stress12-14.
A review article about 678 cases of consecutive superficial facelifts reported no significant difference in major hematoma rates among groups treated with drains, pressure dressing, fibrin glue or tumescence (overall 4.4%)15. Comparing tumescence with and without adrenaline, these authors found hematoma rates of 4.8% in the adrenaline-containing group and 0% in the no-adrenaline group. They identified that rebound hypertension caused the increased hematoma formation. Other researchers said that a preoperative blood pressure omore than 150/100 mmHg was associated with a 2.6-fold greater incidence of hematoma16. Intraoperative hypotension increased the risk of hematoma and attributed this to rebound hypertension17,18. A consensus from these articles is that blood pressure should be well controlled throughout the entire perioperative period. In the present cases, there is no information about perioperative blood pressure, but invasiveness of surgery of these cases is supposed to be much lower than that of these facelift cases.
This new fixation technique could be used safely in those low invasive small minor surgeries for outpatients.
Limitations of this study and of the new method
This study and the new method have a few limitations. First, the surgical sites, lesions, and closure techniques differed significantly between the new-method and control groups. There is some possibility that these significant differences, especially closure techniques, which have differences in area of dissection, affected the results. This method should be tested with an additional randomized, controlled trial.
Second, the new method of Penrose-drain fixation requires the same type of compression, with taping or bandaging, as conventional fixation to the skin. If there is any possibility of hemorrhage or of moderate to heavy discharge, the Penrose drain should be conventionally sutured to the skin because of the length of time the drain may be required. Suction drains may be necessary in some cases.
Third, the Penrose drain should not be shorter than its long diameter, in case of breakage at the sutures or stitches. This reduces the potential of the Penrose drain to stray into the subcutaneous layer due to its elasticity.
Fourth, although complications related to Penrose drains were not observed in this study, it is difficult to say that the new method is completely safe. The results of this method should be observed in a larger number of cases.
Despite these limitations, the new method has advantages for minor skin surgeries where surgeons might otherwise hesitate to insert Penrose drains due to the low availability of postoperative care, such as in rural or remote areas.
The new Penrose-drain fixation method is especially advantageous for surgeons who perform small surgeries in remote areas with no resident practising physicians. This useful method should be studied further with a larger number of cases. This method should be tested in a non-inferiority trial under randomized, controlled conditions.
References
1 Survey of physicians, dentists and pharmacists. 2010. Available: http://www.mhlw.go.jp/english/database/db-hss/dl/spdp_2010.pdf (Accessed 16 December 2015).
2 Table 3, brief overview. Survey of physicians, dentists and pharmacists. 2012. Available: http://www.pref.ibaraki.jp/hokenhukushi/koso/iji/koso/stachischics/populachion/2012.html (Accessed 12 April 2015).
3 Survey of physicians, dentists and pharmacists. 2012. Available: http://www.e-stat.go.jp/SG1/estat/List.do?lid=000001116353 (Accessed 16 December 2015).
4 Population. 2015. Available: http://www.pref.ibaraki.jp/hokenfukushi/chofuku/choju/stats/documents/shibetsu150101.pdf (Accessed 12 April 2015).
5 Table 16, Population in recent 6 years. 2013. Available: http://www.pref.ibaraki.jp/kikaku/tokei/fukyu/tokei/betsu/jinko/nenpo/jinko25/index.html
6 Table 14, Brief overview, from Survey of Physicians, Dentists and Pharmacists. 2012. Available: http://www.pref.ibaraki.jp/hokenfukushi/koso/iji/koso/stachischics/health-welfare-report/2012.html (Accessed 12 April 2015).
7 Table 5 - 08, from Survey of Physicians, Dentists and Pharmacists. 2012. Available: http://www.e-stat.go.jp/SG1/estat/List.do?lid=000001116353 (Accessed 12 April 2015).
8 Drainage in abdominal surgery. The Journal of the American Medical Association 1890; 14: 264-266.
9 The persons behind the name: Charles Bingham Penrose. Plastic and Reconstructive Surgery 1982; 70(3): 397-399.
10 Patient preparation for safe removal of surgical drains. Nursing Standard 2007; 21(49): 39-41.
11 Investigation of the freely available easy-to-use software 'EZR' for medical statistics. Bone Marrow Transplant 2013; 48(3): 452-458.
12 Platelets and shear stress. Blood 1996; 88(5): 1525-1541.
13 Practical hemostasis and thrombosis. Hoboken, NJ: Wiley-Blackwell, 2009; 2.
14 Haematology. Bloxham, UK: Scion Publishing, 2010; 334-336.
15 Avoiding hematoma in cervicofacial rhytidectomy: A personal 8-year quest: Reviewing 910 patients. Plastic Reconstructive Surgery 2004; 113: 381.
16 The study of hematomas in 500 consecutive face lifts. Plastic Reconstructive Surgery 1977; 59: 694.
17 The effect of cigarette smoking on skin-flap survival in the face lift patient. Plastic Reconstructive Surgery 1984; 73(911).
18 Hematoma formation in deep plane rhytidectomy. Archives of Facial Plastic Surgery 2000; 2(4): 240-242.
