Oral health is not only about healthy teeth; it is also an integral part of overall health. Oral health can be achieved through effective preventive and curative dental services1. However, considerable evidence shows sociodemographic and rural-urban disparities in dental service utilization2-4. Incremental and persistent tooth loss is associated with poor access to professionally provided preventive services and poor option-taking in the receipt of dental treatment5. A study using county-level data suggested that older adults living in a county with a high dentist-to-population ratio were more likely to use dental services2, highlighting the importance of adequate dental care provision. Poor oral health in rural areas is related to limited availability of dental services4. In addition, the cost of dental services is an important barrier to dental care attendance6; the issue of affordability in dental services has contributed substantially to poor oral health, especially in those socioeconomically advantaged individuals, including but not limited to people with low income and those with inadequate dental insurance coverage7. Unaffordability of dental services worsens oral health in several segments of population, including the elderly, poor children, minorities and those with severe systemic diseases or disabilities8.
In 1995, the government of Taiwan introduced a national health insurance (NHI) program that covers all residents. The NHI program was intended to ensure accessibility to health care at a reasonable cost9. An observational study revealed that, after the introduction of the NHI program, the newly insured used more than twice the amount of outpatient visits and hospital admissions than before the implementation of the NHI; as a result, those previously uninsured showed the same amount of healthcare contacts as the previously insured group. The newly insured also experienced an increase in emergency department visits10. The NHI program extended the existing insurance coverage from 57% of the population (mostly the employed) to everyone, including children, the elderly and non-working adults, who are consequently the segments of the population who primarily benefited from the NHI program11.
The implementation of the NHI program is expected to improve the affordability of healthcare services, including dental services, for socially vulnerable people, most of whom live in rural areas in Taiwan. In the context of the universal health insurance coverage in Taiwan that greatly removes financial barriers to dental care, this study aimed to assess whether sociodemographic and rural-urban variations in dental service utilization still exist in Taiwan after 15 years of the NHI implementation through examining the urban-rural disparity in preventive and curative dental service utilization. Dental service utilization by people by age and sex stratifications was also examined to determine the variation in utilization across demographic variables in Taiwan under the universal NHI system.
Data sources
The data analysed in this study were retrospectively retrieved from the claims of the NHI Research Database (NHIRD) provided by the NHI Administration (NHIA), Ministry of Health and Welfare. The NHIRD provided all inpatient and ambulatory medical claims for around 99% of Taiwanese people12. The NHIRD covered all inpatient and outpatient claims and medical orders, and information on healthcare providers, including medical institutions and healthcare workers. The identification numbers of all healthcare providers are encrypted to ensure privacy. The NHIA performs quarterly expert reviews on a random sample for every 50-100 ambulatory and inpatient claims to ensure the accuracy of claim files13. In this study, the claims data of ambulatory care visits were used; these data were from a representative sample of one million beneficiaries randomly selected from all beneficiaries registered in 2005. The age and sex distributions of this random sample are comparable to the entire population of Taiwan in 200514.
Study design and sample
This retrospective cohort study was based on the one million people randomly selected in 2005, and dental service attendance information was retrieved from the ambulatory care claims between 2005 and 2010. Only 998 014 people who had completed information on age, sex and urbanization were retained in the analysis. Dental care visits were further classified into types of dental care (ie preventive care and curative care). Preventive care includes regular dental examinations and scaling. Curative treatment includes filling cavities, root canal therapy, periodontal treatment, dentures and other prosthetic treatments15. Preventive and curative dental care information was determined by using the medical order codes of the NHI medical claims. The prevalence of dental care visits was calculated as the ratio of number of dental care visits to total person-years observed from the study population in 2010. Patients' residential or employment areas were categorized into five levels of urbanization according to the classification scheme proposed by Liu et al16.; these authors considered the following indicators in determining levels of urbanization: population density, proportion of residents with college or higher education, percentage of elderly (≥65 years) people, proportion of agriculture workforce, and number of physicians per 100 000 people. Urbanization values of 1 and 5 indicate the most and least level of urbanization, respectively.
Statistical analysis
The person-years accumulated for each study subject were calculated from the first day of 2005 (or date of NHI enrolment) to the last day of 2010 (or date of NHI termination). First, the overall and specific prevalences of dental service attendance were presented according to various age, se, and urbanization stratifications, as well as the type of dental service attendance. The prevalence of dental care visit was then fitted into a Poisson regression model to assess the independent effect of age, sex and urbanization on dental service utilization by adjusting for calendar year. The statistical analyses were performed with Statistical Analysis Software v9.4 (SAS Institute Inc., www.sas.com).
Ethics approval
Access to research data has been reviewed and approved by the National Health Research Institutes Review Committee (NHIRD-102-021). Because the medical claims data for all personal identification numbers were encrypted, obtaining the informed consent from each study patient was waived.
The utilization rate of preventive dental service was estimated at 455.8 per 1000 person-years in Taiwan, and the utilization rate of curative services was roughly doubled at 938.5 per 1000 person-years. Children aged 15 years or less showed the lowest rate of preventive services (178.6 per 1000 person-years), but they had the highest rate of curative services (1592.0 per 1000 person-years). Except for the ages 35-44 years and ≥65 years, older ages were generally associated with higher dental service utilization rate than people aged 15 years and older, regardless of the type of dental care. Males had lower rates of preventive (421.2 vs 489.6 per 1000 person-years) and curative services (862.6 vs 1013.0 per 1000 person-years) than females (Table 1). A clear gradient relationship was found between levels of urbanization and utilization rate of dental services (Fig1).
Table 2 shows the adjusted rate ratio (RR) of dental services in relation to age, sex and urbanization. Compared with elderly people (≥65 years), children (<15 years) had an obviously lower rate (RR=0.40) of preventive services but a higher rate of curative services (RR=1.84). All age groups except children and younger people aged 15-24 years were associated with higher rates of preventive services, with an age-specific RR ranging from 1.06 to 1.26. All age groups except children and those aged 55-64 years were associated with significantly low rates of curative services, with an age-specific RR ranging from 0.86 to 0.99. Furthermore, females had significantly higher rates of preventive (RR=1.14) and curative (RR=1.18) services than males.
Compared with those from the least urbanized areas, people from the most urbanized areas had the highest RRs of preventive and curative services but with a greater RR noted for preventive services (RR=1.57 vs RR=1.42). Regardless of the type of dental services, clear urbanization gradient relationships were found. Specifically, the RR of dental services increased with high levels of urbanization.
Table 1: Dental service utilization rates according to sociodemographic characteristics
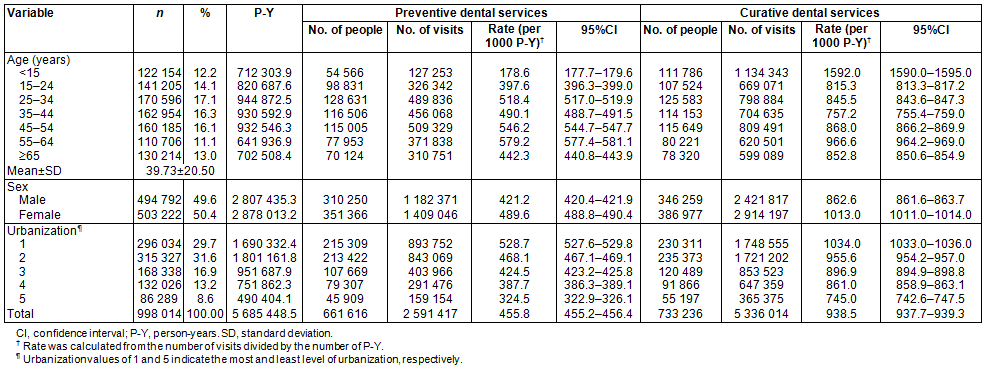
Table 2: Rate ratio of dental service utilization in relation to age, sex, and urbanization
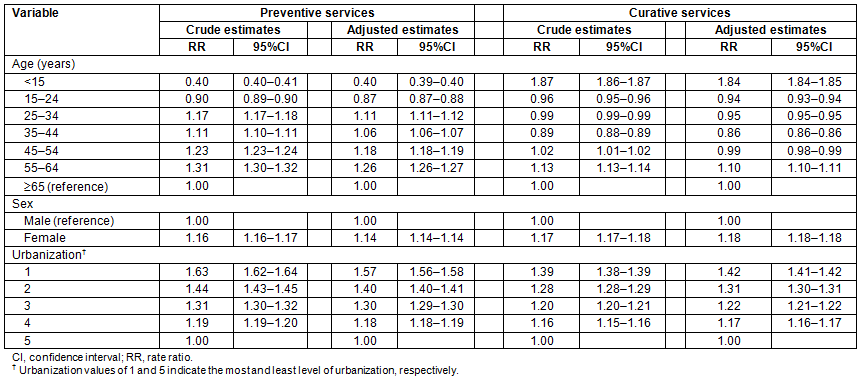
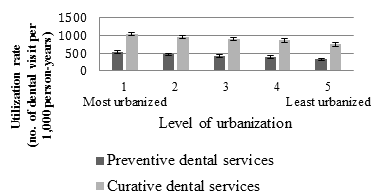
Figure 1: Relationship between level of urbanization and utilization rate of dental services.
Discussion
After 15 years of the NHI implementation, large disparities by demographics and geography in the use of dental services still exist in Taiwan. Such disparity is probably attributable to factors other than financial barriers. Female residents visited dentists more frequently than males; younger people (<24 years) received a very limited number of preventive dental services. Compared with the people living in the least urbanized areas, those from the most urbanized areas exhibited significantly higher rates of preventive and curative dental services; a greater estimated rate ratio was noted for preventive services than for curative services (1.57 vs 1.42). Although nearly every resident of Taiwan visited a dentist for curative care in a year as recommended17, only 45.58% of people in Taiwan made one dental visit for preventive dental services.
Universal coverage of dental services at a reasonable cost is expected to make impressive strides towards improving welfare coverage and increasing affordability of dental care services. However, factors other than affordability may still account for the demographics and geography disparity in dental utilization under the universal health coverage. A Thai study found that, even with universal coverage, inequality and inequity in oral healthcare utilization still exist. The poor are more likely to access and utilize services at subsidized public facilities, particularly community hospitals, as opposed to the wealthier who tend to utilize services at private facilities18. Non-financial factors also include but are not limited to accessibility, distribution of oral health services, oral health knowledge and practices, and prevalence of oral diseases19. Inadequate public transport supply in an area may pose adverse influence on the access to dental services20. Although NHI's offering universal health coverage to all citizens and proper financial incentives have resulted in equal geographic distributions among the key healthcare providers in Taiwan, the distribution of dentists in Taiwan has remained unequal, with northern parts of Taiwan and urban areas accessing far more dentists than others21,22. The limited accessibility to dental services in remote and rural areas may contribute to the urbanization disparity in dental service utilization. Rural areas are often associated with low education levels, which are related to low levels of health literacy and poor use of healthcare services23. Not all studies have found associations between oral health literacy and dental utilization24; however, many studies have reported that increased oral health literacy is associated with improved oral health status25. Lower education level and oral literacy may have also accounted for the urban-rural difference in dental service utilization, especially utilization of preventive dental services, as observed in the present study.
This study noted that children (<15 years) in Taiwan had the least prevalence of preventive dental service utilization but had the highest prevalence of curative dental service. Previous studies found that caregiver education £12 years is associated with fewer preventive dental care visits by their children26. Inadequate awareness of the availability and necessity of dental care in early childhood because of parents' attitude may limit children's receipt of recommended prophylactic visits27. Although the exact reasons for inadequate preventive oral care utilization by Taiwanese children are unknown, oral care providers caring for children should play a vital role as advocates of early and regular prophylactic dental visits by children.
The methodological strengths involved in this study included using a sample that is highly representative of the entire Taiwan population. The preventive and curative dental care services were also analysed separately, thereby allowing proper interpretation of the study results. With such a large sample size, the study was able to perform detailed stratified analyses according to age, sex, and geographic area28.
The data showed an apparent urban-rural disparity in preventive and curative dental service utilization in Taiwan in 2010 after 15 years of the NHI implementation. The NHI program aims to improve affordability of medical care services, including dental services. Men and women of all ages in Taiwan generally made fewer than expected preventive dental visits. In addition, unmet preventive dental care remains one of the most urgent oral healthcare needs among Taiwanese children. Hence, actions aiming to improve oral health outcomes in underserved populations may help reduce oral health inequalities and ameliorate rural-urban disparity; and such actions are necessary within the healthcare workforce and the wide policy environment.
Acknowledgements
This study was funded by the Ministry of Science and Technology (MOST 104-2314-B-006-019).
References
1. Benjamin RM. Oral health: the silent epidemic. Public Health Reports 2010; 125(2): 158-159.
2. Lee W, Kim SJ, Albert JM, Nelson S. Community factors predicting dental care utilization among older adults. Journal of the American Dental Association 2014; 145(2): 150-158.
3. Bhagavatula P, Xiang Q, Szabo A, Eichmiller F, Kuthy RA, Okunseri CE. Rural-urban differences in dental service use among children enrolled in a private dental insurance plan in Wisconsin: analysis of administrative data. BMC Oral Health 2012; 12: 58.
4. Vargas CM, Dye BA, Hayes KL. Oral health status of rural adults in the United States. Journal of the American Dental Association 2002; 133(12): 1672-1681.
5. Thomson WM. Social inequality in oral health. Community Dentistry and Oral Epidemiology 2012; 40(Suppl 2): 28-32.
6. Chrisopoulos S, Luzzi L, Brennan DS. Trends in dental visiting avoidance due to cost in Australia, 1994 to 2010: an age-period-cohort analysis. BMC Health Services Research 2013; 13: 381.
7. Locker D, Maggirias J, Quinonez C. Income, dental insurance coverage, and financial barriers to dental care among Canadian adults. Journal of Public Health Dentistry 2011; 71(4): 327-334.
8. Kleinman ER, Harper PR, Gallagher JE. Trends in NHS primary dental care for older people in England: implications for the future. Gerodontology 2009; 26(3): 193-201.
9. Cheng TM. Taiwan's new national health insurance program: genesis and experience so far. Health Affairs 2003; 22(3): 61-76.
10. Cheng SH, Chiang TL. The effect of universal health insurance on health care utilization in Taiwan. Results from a natural experiment. JAMA 1997; 278(2): 89-93.
11. Chang YK, Hsu CC, Chen PC, Chen YS, Hwang SJ, Li TC, et al. Trends of cost and mortality of patients on haemodialysis with end stage renal disease. Nephrology 2015; 20(4): 243-249.
12. Lu JF, Hsiao WC. Does universal health insurance make health care unaffordable? Lessons from Taiwan. Health Affairs 2003; 22(3): 77-88.
13. Bureau of National Health Insurance. Regulations governing contracting and management of National Health Insurance medical care institutions. (Internet) 2014. Available: www.nhi.gov.tw/English/webdata/webdata.aspx?menu=11&menu_id=295&WD_ID=295&webdata_id=3284 (Accessed 16 November 2014).
14. NHRI, National Health Insurance research Database, Taiwan, http://nhird.nhri.org.tw/date_cohort.html (Accessed 24 July 2016).
15. Listl S. Income-related inequalities in dental service utilization by Europeans aged 50+. Journal of Dental Research 2011; 90(6): 717-723.
16. Liu CY, Hung YT, Chuang YL, Chen YJ, Weng WS, Liu JS, et al. Incorporating development stratification of Taiwan townships into sampling design of large scale health interview survey. Journal of Health Management 2006; 4: 1-22.
17. McCarthy M. Millions of US children do not get the recommended preventive care, CDC reports. BMJ 2014; 349: g5639.
18. Somkotra T, Detsomboonrat P. Is there equity in oral healthcare utilization: experience after achieving Universal Coverage. Community Dentistry and Oral Epidemiology 2009; 37(1): 85-96.
19. Ogunbodede EO, Kida IA, Madjapa HS, Amedari M, Ehizele A, Mutave R, et al. Oral health inequalities between rural and urban populations of the African and Middle East Region. Advances in Dental Research 2015; 27(1): 18-25.
20. Rocha CM, Kruger E, McGuire S, Tennant M. Role of public transport in accessibility to emergency dental care in Melbourne, Australia. Australian Journal of Primary Health 2015; 21(2): 227-232.
21. Kreng VB, Yang CT. The equality of resource allocation in health care under the National Health Insurance System in Taiwan. Health Policy 2011; 100(2-3): 203-210.
22. Yang CH, Huang YT, Hsueh YS. Redistributive effects of the National Health Insurance on physicians in Taiwan: a natural experiment time series study. International Journal for Equity in Health 2013; 12: 13.
23. Sood N, Bendavid E, Mukherji A, Wagner Z, Nagpal S, Mullen P. Government health insurance for people below poverty line in India: quasi-experimental evaluation of insurance and health outcomes. BMJ 2014; 349: g5114.
24. Burgette JM, Lee JY, Baker AD, Vann WF Jr. Is dental utilization associated with oral health literacy? Journal of Dental Research 2016; 95(2): 160-166.
25. Lee JY, Divaris K, Baker AD, Rozier RG, Vann WF Jr. The relationship of oral health literacy and self-efficacy with oral health status and dental neglect. American Journal of Public Health 2012; 102(5): 923-929.
26. Quinonez RB, Pahel BT, Rozier RG, Stearns SC. Follow-up preventive dental visits for Medicaid-enrolled children in the medical office. Journal of Public Health Dentistry 2008; 68(3): 131-138.
27. Valdes XL, Greenwell A, Theriot J, Franco S. Access barriers to dental care for Medicaid patients. The Journal of the Kentucky Medical Association 2007; 105(10): 491-495.
28. Jollis JG, Ancukiewicz M, DeLong ER, Pryor DB, Muhlbaier LH, Mark DB. Discordance of databases designed for claims payment versus clinical information systems. Implications for outcomes research. Annals of Internal Medicine 1993; 119(8): 844-850.
