Periodontal disease, a chronic inflammatory disease in which periodontal tissue is destroyed by biofilm formed on the tooth surface and a bacterial host response, is one of the main causes of tooth loss in middle-aged individuals. Attention to the importance of disease prevention has increased due to the association of periodontal disease with systemic diseases including cardiovascular disease and diabetes, as well as tooth loss1,2. However, a study in 2013 found that Korean males older than 40 years of age had a 37.9% prevalence of periodontal disease, and one of every two males older than 50 years and at least one-third of females of the same age group had periodontal disease3. Gingivitis and periodontal disease produced the highest increase in medical cost rates among frequent outpatient diseases. Medical care expenses in Korea increased by 36.7% in 2014 compared to 2013, significantly impacting healthcare expenses4. The increased expense was especially significant for rural residents, who are more likely to have a lower socioeconomic status than residents of large urban centers. The prevalence of periodontal disease in Korean adults was 21.4%, 30.0%, and 32.6% in metropolitan cities, mid-sized cities, and rural areas, respectively with the highest prevalence found in rural areas5. In particular, among older residents in rural areas with low health service accessibility, the high rates of tooth loss and low socioeconomic status have considerable effects on the oral health-related quality of life6,7.
The healthcare system should provide essential healthcare services to all residents, including vulnerable individuals. However, at least 93% of healthcare institutions in Korea are private institutions, most of which are located in metropolitan cities. With regard to the regional distribution of dental clinics in 2011, Seoul, a metropolitan city, housed 30.6% of all dental clinics (4595 sites), while Gangwon, a rural province, housed only 2.1% (314 sites), illustrating the unequal distribution of healthcare facilities8. Seoul has a population of approximately 10.3 million in an area of 605.2 km2 and a population density of slightly more than 17 000 people/km2. On the other hand, Gangwon-do has a population of 1.5 million in an area of 11 704 km2 and a population density of 75 people/ km2. Seoul has over 30% of the dental clinics in South Korea and only approximately 20% of the residents, while Gangwon-do has 2.1% of the dental clinics and approximately 3% of the residents (based on an estimated population in South Korea of 50.7 million as of 2016)9,10. The clinics in Gangwon-do must treat a larger relative client base than those in Seoul and also service larger average geographic areas. This places high demands on their resources, which are very limited compared to those in Seoul. According to previous studies, periodontal disease in the elderly is positively correlated with metabolic syndrome risk as measured by cholesterol level, fasting plasma glucose level, and body mass index11. The proportion of elderly residents is high in agricultural areas compared to urban centers12. Therefore, it is necessary to build a system to manage the oral health of residents, such as the middle-aged and those living in rural areas, who are at high risk of developing periodontal disease.
In primary care or public health settings, effective and non-invasive interventions to reduce gingivitis are low-cost preventive measures for improving oral health13. Korean community health centers and rural health subcenters, which are representative public health settings, were designed to reinforce health service accessibility in vulnerable areas through an act in 1980 that established special measures for health services in farming and fishing communities14. The functional focus of community health centers has gradually shifted from disease treatment to prevention and disease control and to providing services appropriate to regional conditions15. Therefore, it is important that oral health providers plan and conduct oral health projects in public health settings to establish strategies for training and interventions to be maintained and applied in clinical settings.
The most basic and widely known procedure to prevent periodontal disease is the removal of biofilm on the gingival margin through mechanical plaque control16. Gingivitis is a significant risk factor in the clinical progression of chronic periodontitis17. Although gingivitis does not necessarily progress to periodontitis, it always precedes periodontitis18. Symptoms of gingivitis include red, swollen gingiva and bleeding. It is possible to restore the gingiva to a healthy state through proper self-oral hygiene behaviors such as toothbrushing, application of oral health products and professional oral hygiene care19. A recent study found periodontal health improvements in plaque, calculus, and gingivitis indexes after an average of three sessions of education and professional care among the elderly, mental patients, and patients hospitalized in an intensive care unit20,21. Another recent effort toward behavior change and periodontal health promotion in the form of a personalized education program targeted adults older than 20 years22,23.
The bleeding on probing (BoP) index has been widely used as a tool for determining gingival inflammation and periodontal health stability24. The BoP score is an early and more sensitive indicator than probing pocket depths and visual signs of inflammation (redness and swelling)25. In order to promote oral health and prevent oral diseases, primary healthcare and public health interventions must be provided26. However, previous studies have been mainly performed on patients visiting dental clinics, and government-led oral health projects have mainly targeted children and the elderly, neglecting adults in rural areas with low medical service accessibility. Therefore, community-centered efforts to reinforce health-promotion capacity through improvement of oral health practices in adulthood, such as prevention, education, and oral health care, are needed.
The purpose of this study is to analyze the effects of a dental health program on oral hygiene status and BoP score change. The program in question consisted of four 45-minute education and professional oral hygiene sessions for each subject held at 2-week intervals. At the completion of the educational and cleaning sessions in the experimental group, scaling was performed at the week 8 visit for both groups. Afterwards, a multiple regression analysis was conducted to determine what factors influenced the changes in BOP score and hygiene status. Dental hygienists performed a preventive oral healthcare program with adults older than 40 years who visited a rural public health subcenter with limited medical services.
Methods
Sample
Study subjects included middle-aged adults older than 40 years who lived in Hongcheon-gun, Gangwon-do, or Yeoju-si, Gyeonggi-do from June 2014 to December 2014 (Fig1). A total of 83 subjects participated in the program; 46 people were selected as study subjects, excluding 37 people who had a prior oral health assessment. A total of 42 people were included in the final sample after four subjects dropped out due to personal circumstances during the study period. Voluntary participants were recruited through a community newspaper, an advertisement on a community health center homepage, and a notice at the health center. In order to assess the efficiency and accessibility of the oral health project, three of the recruited participants were selected for a pilot study, which was conducted once a week for 4 weeks.
Inclusion criteria included age older than 40 years, BoP score of at least 15%, and PHP index of at least 3.0. Study subjects included individuals taking daily medication for systemic diseases such as hypertension and diabetes. Subjects who had fewer than 10 teeth, had received periodontal treatment including scaling within the previous 6 months, or who had normal periodontal pocket depths (1-3 mm) without gingival bleeding were excluded. Additionally, individuals with infectious disease (HIV, AIDS, hepatitis A) or needing periodontal surgery prior to the oral care program were also excluded.
The required study sample size was calculated to identify differences in plaque control effects between the intervention and control groups27,28. The calculation of the effective sample size considering a 1:1 allocation at a statistical significance level ⍺=0.05, Z⍺/2=1.96, and statistical test power Zβ=0.84 found that 20 people were needed in each group. Therefore, a total sample size of 46 people was determined to be an effective sample size for this study, considering a 10% dropout rate.
The program was assessed by two trained dental hygienists who performed repeated objective assessment of oral hygiene status and also received training to ensure conformity and objectivity relating to BoP score and PHP index. The reliability measurement between the investigators showed that the ICC (intra-class correlation coefficient) for BoP score was 0.903, and the Kappa coefficient measured by the presence of plaque on five surfaces of five teeth was 0.755, indicating a high degree of conformity29.
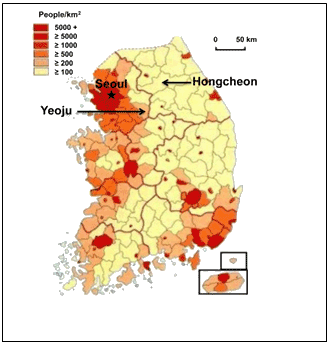
Figure 1: Map of South Korea, showing Hongcheon and Yeoju.
Oral hygiene care program
At baseline, all subjects listened to an explanation of the program and provided written consent. Subjects who agreed to participate in the study answered a questionnaire assessing their general characteristics, medical history, alcohol consumption, smoking status, and other oral health practices. In addition, they received a clinical evaluation including BoP score, PHP index and 1:1 individual education for prevention of periodontal diseases and a pamphlet personally produced by an educator. After subject selection, they were randomly allocated into intervention and control groups based on the order of their visit (Fig2).
Weeks 2, 4, and 6 visits: For the intervention group, professional oral hygiene care was provided for 8 weeks at 2-week intervals. Each session lasted about 45 minutes, and a plaque check and professional cleaning for gingival health improvement were also performed. The toothpick method, where the bristle of a toothbrush is pushed into the interdental region, was used with a semi-stiff toothbrush with 2×6 lines of bristles. Chlorhexidine was applied to the toothbrush in order to provide anti-plaque and anti-gingivitis effects.
Week 8 visit: After 8 weeks, dental scaling was performed both in the intervention and the control groups, and mouthwash was provided. Both an ultrasonic scaler and hand scaler were used for the scaling procedure.
Week 16 visit: To assess the persistence of the program, gingival condition and plaque index were assessed after 16 weeks.
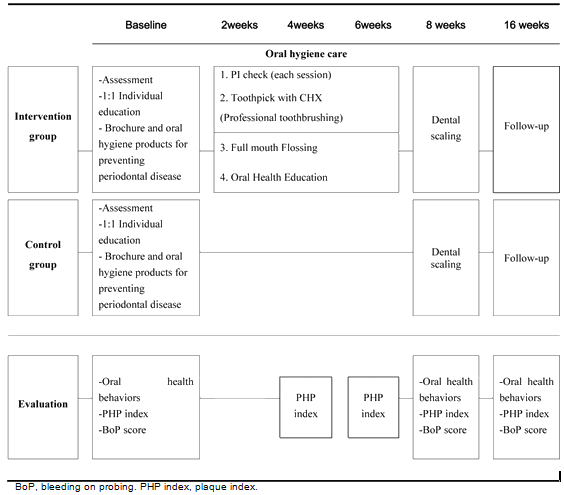
Figure 2: Study design flowchart.
Clinical measurements
PHP index: For the plaque index, the maxillary teeth were measured in order of 16, 11, and 26, and the mandible teeth were measured in order of 36, 31, and 46, using Podshadley and Haley's Patient Hygiene Performance Index30. A score was calculated based on the presence of plaque on each of the above tooth areas (0=no, 1=yes), by dividing the total score by the total number of tooth surfaces.
BoP score: The intervention effect was evaluated with %BoP, an early indicator of gingivitis or periodontal disease. The bleeding on probing assessment (%BoP) was performed with a mirror and a periodontal probe. The marginal gingiva surrounding each tooth was classified into proximal, distal, buccal and lingual surfaces, and the amount of bleeding appearing within 15 s after measurement of periodontal pocket depth on the four sides of the marginal gingiva was indicated as a percentage.
Analytic strategy
The Shapiro-Wilk normality test was performed in this study, and the results showed that normality was satisfied with a score of 0.094 for BoP score and 0.200 for PHP index. For the general characteristics of the subjects, descriptive statistics and χ2 tests were performed, while independent t-test and one-way ANOVA were performed for the analysis of plaque index and BoP score according to general characteristics. Changes in plaque and gingivitis before and after the program were analyzed with repeated-measures ANOVA. When the repeated measures ANOVA test was carried out, within-subject effects, between-subject effects, and interaction effects were considered for the analysis. Within-subject effects were analyzed when the intervention group and control group were held constant at set points in time, with the analysis of the BoP score and PHP index. Between-subjects effect was examined when time was held constant, and the differences in BoP score and PHP index values between the two groups and the differences between the individual subjects were analyzed.
Finally, factors affecting BoP score change were analyzed with hierarchical multiple regression analysis. All statistical analyses were performed with PASW Statistics v20.0 (SPSS; http://www.spss.com). A two-tailed test was performed at a significance level of p<0.05.
Ethics approval
The study was approved by the Yonsei University Wonju College of Medicine Institutional Research Ethics Review Board (registration number YWDR-14-7-047; approval date 5 June 2014).
Results
Demographic characteristics
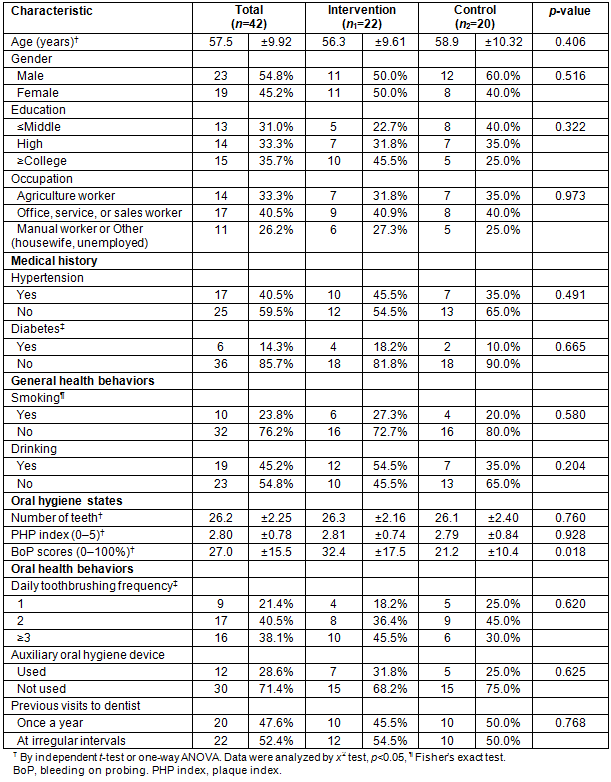
Table 1 describes the sociodemographic characteristics and oral health statuses of the subjects. Their mean age was 57.5 years, and there was no significant age difference between the two groups. With regard to oral health status, the intervention group had a higher BoP score, but there were no significant differences between the groups for the other variables.
Plaque index
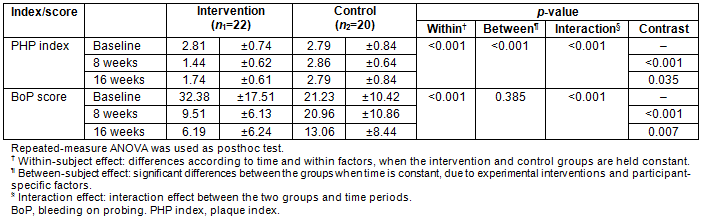
Mauchly's sphericity test showed that the PHP index satisfied the sphericity assumption with p=0.976. The repeated measure ANOVA of the PHP index showed that the plaque index decreased significantly in the intervention group, and there were differences between the groups at each time point. In addition, there was an interaction effect between group and time in the PHP index change (Table 2; Fig3).
BoP score
The results of the repeated-measure ANOVA for BoP score showed that, within the same group, the BoP score decreased over time (p<0.001). In addition, the posthoc test of the BoP score comparison showed that the BoP score decreased by 22.87 in the intervention group and 0.27 in the control group between baseline and the eighth week but exhibited a further decrease of only 3.32 between the eighth week and the 16th week in the intervention group and of 7.9 in the control group. This demonstrated a change in BoP score over time between the intervention and control group (Table 2; Fig3).
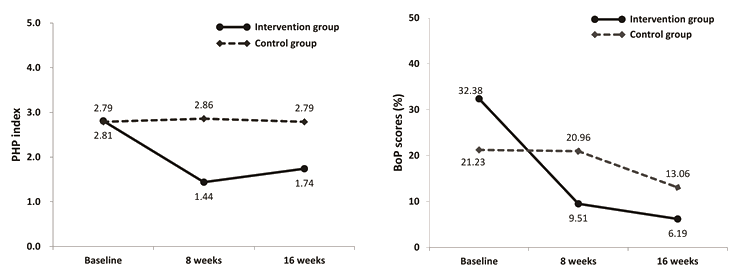
Figure 3: Changes in plaque (PHP) index and bleeding on probing (BoP) score by group.
Factors affecting decrease in BoP score between baseline and the 16th week
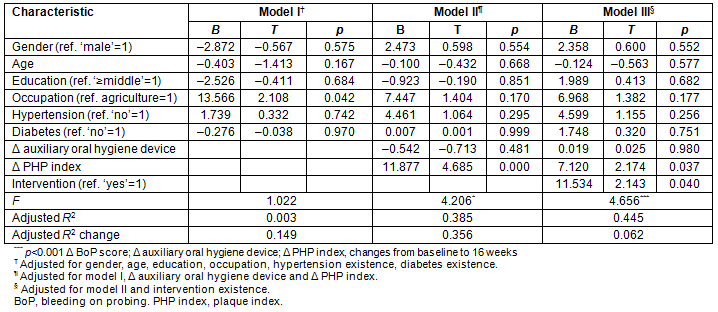
In order to identify factors affecting the change in BoP score between baseline and the 16th week, a hierarchical multiple regression analysis was performed (Table 3). General characteristics and history of chronic disease such as hypertension and diabetes were added to model I, change in oral hygiene conditions was added to model II, presence of intervention was added to model III, and R2 change due to model change was determined. Based on the R2 value, model I explained 3% of the BoP change, while model II explained 38.5% of the BoP change. Model III, which contained the general characteristics and the altered oral hygiene condition, explained 44.5% of the BoP change. In model I, BoP score change increased significantly in the group engaged in agriculture. In model II, the results showed that if the reduction in PHP index between baseline and the 16th week increased by one unit, the BoP score decreased by 11.877, after adjustment to the general characteristics. In the results of the final model III, there was a significant increase in BoP score (t=2.143, p<0.05) in the intervention group compared to the control group, along with an increased reduction of the PHP index between baseline and the 16th week (t=-2.174, p<0.05).
Discussion
Although daily care for prevention of adult periodontal disease is important, it is likely to be neglected due to lack of education, procedural know-how, and concern. This is especially true for rural residents who have low socioeconomic status. Such residents do not have the means, education, or incentive to engage in preventative oral hygiene practices, and the reduced availability of dental education and services in rural regions further limits their access to quality and effective oral health care. Continuous care for adult periodontal disease focusing on behavior changes is essential. In the present study, the oral hygiene care program administered to Korean residents older than 40 years with lower accessibility to dental health services was more effective in improving oral hygiene conditions and reducing gingival bleeding than conventional one-time scaling.
Professional toothbrushing (toothpick method) is known to improve periodontal inflammation through proper gingival stimulation and effective plaque removal31,32. This procedure helps to reduce the invasion of inflammatory cells and increases fibroblasts or collagen through the physical stimulation of the gingiva33. The present study also showed a continuous decrease in the plaque index with professional toothbrushing combined with chlorhexidine prior to scaling. In other words, meticulous removal of supragingival plaque, including bacteria accumulated around the gingival margin, was especially important in controlling and preventing periodontal disease34.
A study by Matuliene et al35 reported a full-mouth bleeding score of 30 or more to be a risk factor for tooth loss. The mean BoP score in the early intervention group was 32.4% in the present study, indicating unhealthy gingiva. After the study intervention, BoP decreased by 22.87% in the intervention group and 0.27% in the control group between baseline and 8 weeks. In addition, the BoP decreased by 3.32% in the intervention group and 7.9% in the control group after scaling. With a decline of 15% or less considered to constitute a successful non-surgical periodontal treatment36, the present oral care program carried out in adults older than 40 years living in rural areas in Korea was considered to be effective.
Woo and Kim reported that one-time education in the proper toothbrushing method and oral hygiene product use was insufficient to improve oral hygiene, as the education effect often regressed and disappeared within 4-6 weeks after education, suggesting the need for systematic repeated education37. In the present study, repeated professional education on an effective toothbrushing method resulted in a decrease in the plaque index, which was maintained and even continued to decrease. The present study showed through models II and III that this trend was almost entirely due to the changes in oral hygiene behavior prompted by an increase in education sessions and an additional increase in the continued care period after 16 weeks. According to Zander et al38, oral health management programs are essential in agricultural rural areas, and a recent study39 also suggests the necessity of sustainable oral health management for the improvement of oral health in rural areas.
Although the control group did not show early significant change, the BoP score was improved after scaling in the eighth week of the intervention. Routine scaling is a well-known preventive measure for periodontal disease, but it is difficult to receive regular professional scaling in areas with limited medical service accessibility. In the areas of Gangwon-do and Gyeonggi-do, where the present study was performed, the community health subcenter was the only medical center within a 1 h drive. The limited access to medical care facilities in these areas demonstrates an urgent need for active preventive education and support. In addition, most people visit a dental clinic when they are already experiencing health problems, and they might be less motivated to visit a dental clinic to receive preventive treatment or minimize the scope of treatment40. Increased distance and limited availability to services, as is the situation in most rural dental clinics, are not likely to increase residents' motivation to visit. Therefore, the implementation and expansion of primary oral health services for the prevention of periodontal disease by oral health professionals working at community health centers could contribute to the resolution of regional imbalances in areas with lower dental service accessibility.
Conclusions
There are several limitations to the present study. First, the study sample might not be representative of the general population, as it included only subjects with relatively good periodontal health, excluding individuals with severe tooth mobility or requiring surgery. It is possible to manage subjects with relatively healthy gums or gingivitis with a community healthcare program focused on prevention services. Second, although the subjects were allocated randomly in order of visit, the initial BoP score was higher in the intervention group than in the control group. This might have contributed to the decline in BoP score after the end of the intervention. Third, a comparison with a no-treatment group was not performed for ethical reasons. However, only one subject dropped out of the oral care intervention, and subjects reported a high degree of satisfaction with professional toothbrushing education and oral healthcare education. In the present study, professional care and continuous oral health education for 8 weeks prior to scaling among adults older than 40 years resulted in a change in oral health behaviors and substantial reduction in gingival bleeding. Therefore, in order to reduce the burden of unequal access to dental care among different rural areas, community-based primary oral healthcare centers and services designed to prevent periodontal diseases should be expanded.
It is important to have regular dental checkups in order to prevent periodontal diseases and ultimately decrease out-of-pocket medical expenses and enhance dental health. In Korea, the National Health Check-up project has been included in the National Health Insurance plan and dental checkups are covered, but barely half of the population is taking advantage of the benefit compared to general health checkups41. Such checkups are crucial for people residing in rural areas, even more so than those living in urban centers where there is convenient access to numerous dental facilities and residents have higher incomes on average. This study suggests that oral healthcare management can improve overall dental health in rural areas, and it is crucial to expand access to dental health checkups in order to prevent various tooth diseases in rural populations.
References
