Introduction
Diabetes mellitus is an important cause of death, illness and disability across Canada, North America, and the world. It affects approximately 4.8% of Canadian adults - 20 years of age and older - which equates to over a million Canadians1,2. By 2010 it is estimated that 250 million people worldwide will suffer from diabetes3.
Having diabetes substantially increases one's risk of developing blindness, end stage renal disease, lower limb amputations, and dying from coronary artery disease, cerebrovascular disease, or peripheral vascular disease2,3,4. Type 2 diabetes is of particular concern to Aboriginal people because of higher prevalence rates, early age of onset, and - in many tribes - more serious course5,6 Type 2 diabetes has gone from being nearly nonexistent in the North American native Indian population in 1940 to current epidemic proportions5-11. According to a report published by Health Canada (2000), the prevalence rate of diabetes among the First Nations people in Canada is two to three times that of the general population of Canada5,6.
Although it is well documented that diabetes is strongly associated with morbidity and mortality, less is known about how this disease affects functional health status and sense of wellbeing. Health-related quality of life (HRQOL) is a subjective term which basically refers to perceived discrepancies between one's expectations and one's actual physical, emotional, and social functioning. As one might predict, people with diabetes rate their HRQOL significantly less favorably, on average, than people without diabetes12-15. A literature review on the broad topic of health-related quality of life among Aboriginal diabetics found no Canadian publications, and only a few American publications14,16. One of the American publications was a study by Johnson et al., entitled Health-related quality of life of Diabetic Pima Indians 14. HRQOL was assessed in 54 diabetic Pima Indians living in southern Arizona using the SF-36 Health Survey. SF-36 scores for these 54 Pima Indian diabetics were lower than those published elsewhere for non-Aboriginal diabetic population groups. The Pima Indian study design did not allow for investigation of the relative impacts of such things as gender, race, age, weight - all risk factors for developing diabetes - on health-related quality of life scores.
The Bella Coola Valley is an isolated rural community located in the central coast region of British Columbia17. According to the 2001 Census 2285 people live in the Bella Coola Valley, with 46% of these people estimated to be of Aboriginal descent18,19. Bella Coola Valley is part of the traditional territory of the Nuxalk Nation, a tribe of Salish-speaking Coastal Indians20-23. Age-adjusted prevalence rates for Type 2 diabetes in this Aboriginal population is more than two and half times that of the non-aboriginal population (12.5% vs 4.8%)24. One-third of Nuxalk Indians 65 years and older have diabetes. Age, weight, aboriginal status, but not sex, are all associated with having diabetes in this population. The development of diabetes in both Aboriginal and non-Aboriginal people living in the Bella Coola Valley is clearly associated with the presence of multiple co-morbidities including hypertension, hypercholesterolemia, coronary artery disease, cerebrovascular disease, and neuropathy25. Rates of diabetes associated co-morbidities were similar for both Aboriginal and non-Aboriginal diabetic populations.
The specific objective of this present study was to investigate HRQOL in diabetics living in Bella Coola Valley. We were particularly interested in finding out whether or not significant differences between diabetics and non-diabetics remained after taking into account the relative impacts of age and ethnicity (Aboriginal vs non-Aboriginal).
Methods
Community participation
This research project has been carried out in a participatory fashion, following the recommendations outlined in a recently published policy statement entitled A Guide for Health Professionals Working with Aboriginal Peoples26-28. A goal of these recommendations is to make the relationship between Aboriginal people and non-Aboriginal healthcare providers a fair and honorable one.
There was consultation with the Nuxalk Band Council, community members and local healthcare providers on our plans to study determinants of health and disease of people living in the Bella Coola Valley. Dr Thommasen participated in potlatches (ceremonial meetings) asking for community support and explained the types of health projects we were planning to do. Prior to collecting data we obtained letters of support from the Nuxalk Band Council, from the Bella Coola Transitional Health Authority, and from Central Coast Regional District. Ethics approval to collect data was obtained from Research Ethics Committee's located at both the University of British Columbia, and at the University of Northern British Columbia. The results and the manuscript were reviewed and approved for publication by both Nuxalk Health professionals and by United Church Health Services health professionals.
Chart review details
Two retrospective reviews of clinic charts were conducted by HT. The first chart review was done in July-August 2001 to determine an 'active' September 2001 clinic population. Names and addresses were tabulated onto an electronic spreadsheet and these were used for the mail-out HRQOL survey which was happening simultaneously.
The second chart review took place in the spring of 2003. Clinic charts of patients on the September 2001 Clinic population list were reviewed for the following information: age, sex, Aboriginal status; smoking status, height and weight; presence or absence of diabetes and other chronic conditions. Aboriginal status for the study population was determined from multiple sources - Nuxalk Band lists, a locally available genealogy, clinic chart, and from the survey29,30,31,32. The diagnosis of diabetes was based on the 1998 clinical practice guidelines for the management of diabetes in Canada2,33.
Health and health care survey
A Health and Health Care Survey was offered to all adults living in the Bella Coola Valley between August 2001 and May 200230. The aim of this investigation was to obtain some baseline self-reported data on the health status and overall quality of life of all residents of the Bella Coola Valley of British Columbia aged 17 years or older, and to measure the impact of a set of designated health determinants on their health and quality of life. An identification number was given to each questionnaire sent out. A single investigator (HT) was the only one able to link this number to the 2001 clinic patient list. This information was used for the purposes of re-mailing, and for linking questionnaire responses to retrospective clinic chart review information. All recipients were asked to read an informed consent form or were read an informed consent form prior to completion of a questionnaire.
The precise questions from the survey which were used in this study are shown in Appendix I. The first 36 questions consisted of the 36-item Medical Outcomes Study Short Form (SF-36) questions34-37. The 36-item Medical Outcome Study Health Survey 36-Item Short Form (SF-36) is one of the most frequently used and widely used tools for assessing health-related quality of life. It is sometimes referred to as the 'gold standard' for health status measurement and its norms for several populations provide useful benchmarks for other developed countries. The SF-36 scale works best as a health profile measure with eight dimensions, rather than as a single summative measure. The eight different health dimensions/health concepts evaluate an individual's:
- physical functioning [PF] (10 items)
- social functioning [SF] (2 items)
- bodily pain [BP] (2 items)
- role limitations caused by physical health problems - role-physical [RP] (4 items)
- role limitations caused by emotional problems - role-emotional (RE) (3 items)
- emotional well-being - Mental Health [MH] (5 items)
- energy/fatigue - Vitality [VT] (4 items)
- general health [GH] perceptions (5 items).
In addition, it has a single item addressing perceived change in health status over the preceding year - health transition. The SF-36 scale scores range from 0 to 100, with higher scores indicating better functioning, wellbeing, and state of health. Reliability and validity of the SF-36 have been demonstrated for both insulin-dependent diabetes mellitus and NIDDM patients2,35,38,39,40.
Besides the SF-36 questions, there were items from the United States Centers for Disease Control and Prevention, Behavioral Risk Factor Surveillance System (BRFSS) pertaining to number of unhealthy days and special limitations\problems16. Eight items from the BRFSS were used in this study (Appendix I).
Statistical analysis
Chart and survey-derived information was entered into an electronic spreadsheet (EXCEL), with names and addresses removed. Results were summarized using EXCEL. Formal data analysis was done with SPSS Windows software (SPPS Inc., Chicago, IL, USA). In all tests, a 0.05 level of significance was used.
Domain scores for the SF-36 instrument were computed following the protocol of Ware and associates34. Demographic characteristics - age, gender, and ethnicity - were used to assess response rates by comparing diabetic and non-diabetic respondents to the whole Bella Coola Valley population.
One-way analysis of variance was used to compare the four study groups (diabetic/non-Aboriginal, diabetic/Aboriginal, non-diabetic/non-Aboriginal, non-diabetic/Aboriginal) with respect to each of the SF-36 domains and each of the unhealthy day's outcomes.
Two-way analysis of covariance was then used to assess the effect of diabetes and Aboriginal status, while controlling for age41.
c2 statistical analyses was used to determine whether more Aboriginal diabetics report their health is worse now compared with one year ago.
Results
After excluding clinic charts of people no longer living within the Bella Coola Valley and not currently living in the Bella Coola Valley, 2329 patients made up the September 2001 clinic population list - approximately 104% of the May 2001 census estimate18,19. An estimated 47% of the September 2001 clinic population was of Aboriginal descent which is also similar to the 2001 census estimate (46%) for the Bella Coola Valley18,19. Of the 2329 clinic population 1771 were adults (≥ 17 years old), and 127 of these people had diabetes mellitus. Of the 127 people with diabetes mellitus, 126 diabetics were classified as having Type 2 diabetes mellitus. There was only one Type 1 diabetic living in the Bella Coola Valley at the time of the chart review and that person did not complete a survey.
A total of 675 useable Health and Health Care surveys were returned. Of these, 72 were from people with Type 2 diabetes mellitus. Survey respondents did not answer all questions, so number of responses varies from survey question to survey question. An estimated 1771 Bella Coola adult residents were eligible to complete this survey. So the estimated overall response to the survey was 38% (675/1771), and the diabetic response rate was 57% (72/127).
With respect to the non-diabetic survey responder population, comparisons to the known non-diabetic adult Bella Coola Valley population reveals that relatively fewer non-diabetic Aboriginal people completed the survey (34% vs 41%: p = 0.005) and relatively more non-diabetic women completed the survey (58% vs 49%: p < 0.001). The average age of non-diabetic survey responders was older (47.5 vs 42.6 years: p < 0.001) than the known non-diabetic adult Bella Coola Valley population.
With respect to the diabetic survey responder population, comparisons to the known diabetic Bella Coola Valley population reveals no significant differences with respect to proportion of Aboriginal people completing the survey (61% vs 55%: p = 0.41), proportion of women completing the survey (51% vs 46%: p = 0.44). The average age of diabetic survey respondents was similar (60.2 vs 59.9 years: p = 0.87) to that of the known diabetic population.
Compared with all other diabetic groups, more Aboriginal diabetics report their health is worse now than one year ago (p = 0.035) (Table 1).
Table 1: Health now compared with one year ago
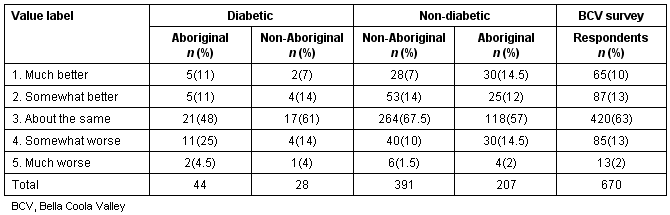
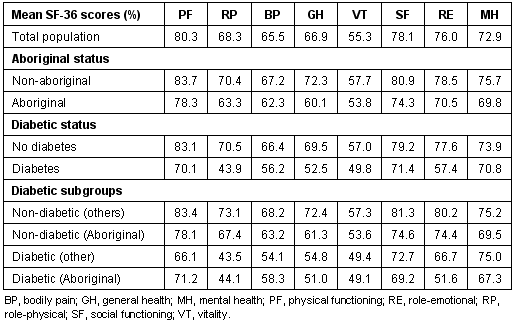
Table 2 summarizes the eight SF-36 profile scores according to diabetic and Aboriginal status. Mean scores for Aboriginal people in our study were lower than mean scores for non-Aboriginal people in all 8 health-related quality of life (SF-36) scales. Mean scores for diabetic people were lower than mean scores for non-diabetics in all 8 health-related quality of life scales. Aboriginal diabetics reported the lowest mean SF-36 scale scores for five of the eight subscales and second lowest means scores for the other three.
One-way Analysis of Variance reveals the differences between the four diabetic subgroups are all statistically significant. The p values were < 0.001 for all scales except for bodily pain (p ≤0.003) and vitality (p ≤0.016).
Table 2: SF-36 HRQOL scores for Bella Coola Valley
Age is a significant covariate for physical functioning, role physical, body pain, general health, mental health, health transition but not for vitality, social functioning or role emotional (Table 3).
Two-way Analysis of Variance with age as the covariate with Aboriginal status and diabetic status as the two main factors reveals Aboriginal status has a significant main effect on general health and physical functioning (because of an interaction effect) (Table 3). The main effect of diabetes is strongly significant for role physical, role emotion, and general health; weakly significant for body pain, vitality, social functioning, and physical functioning (because of interaction effect). Only for mental health is there no evidence of a diabetic effect. The interaction of aboriginal and diabetes status is significant for physical functioning only which means that, for the most part, any difference between diabetics and non-diabetics is present for both Aboriginals and for non-Aboriginals, and the difference is approximately of the same magnitude.
Table 3: Two-way Analysis of Variance for SF-36 scale scores
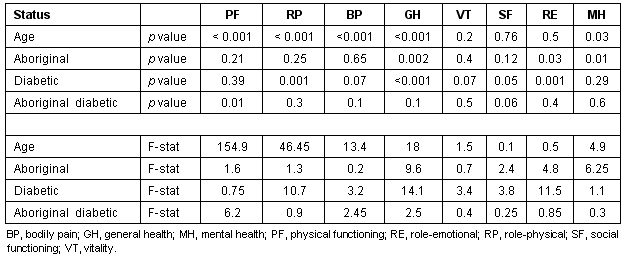
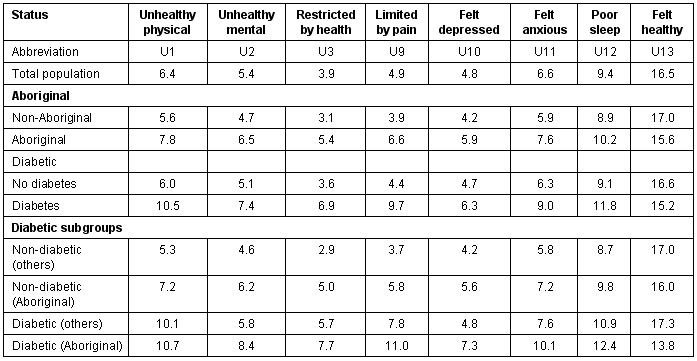
Table 4 summarizes the unhealthy days for the Bella Coola Valley. Compared with non-Aboriginal people, the average number of unhealthy days for Aboriginal people was higher in all 7 health-related domains - physical, mental, pain, depressed, anxious, health restricted, sleep. Aboriginal people also reported lower mean number of feeling healthy days in the past month. Similarly, mean number of unhealthy days for diabetics were greater than mean scores for non-diabetics in all health-related domains. Aboriginal diabetics reported the highest mean number of unhealthy/limitation days, and reported the lowest mean number of healthy days in the past month.
Table 4: Unhealthy days data for Bella Coola Valley
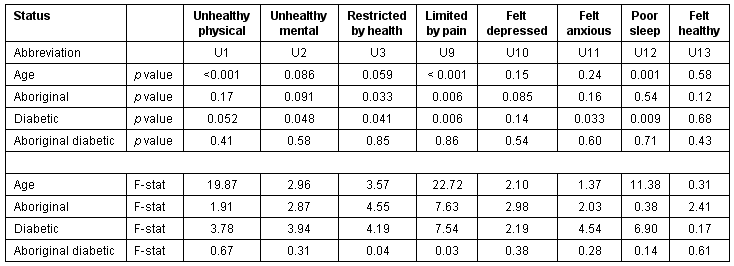
One-way Analysis of Variance reveals the differences between the four diabetic subgroups are statistically significant (p ≤0.05) for all unhealthy day questions except for poor sleep and felt healthy questions.
Age is a significant covariate (p < 0.05) for number of unhealthy physical days (U1), number of days limited by pain (U9), and number of poor sleep days (U12) (Table 5).
Two-way Analysis of Variance with age as the covariate with Aboriginal status and diabetic status as the two main factors reveals the interaction of aboriginal and diabetes status is not statistically significant for any of the unhealthy/limitation days which means that any difference between diabetics and non-diabetics is present for both Aboriginals and for non-Aboriginals, and the difference is about the same magnitude. Having diabetes is associated with significant negative impacts on all variables except for the number of days feeling depressed, and number of days feeling healthy in past month. Aboriginal status is associated with significant negative impacts on only two variables: namely, number of days restricted by health and the number of days limited by pain.
Table 5: Two-way Analysis of Variance for unhealthy days data
Discussion
Health care providers should strive to understand the physical, emotional, and social impacts chronic disease and its treatments have on patients/clients. Such patient-centered knowledge can be incorporated into chronic disease treatment strategies designed to improve or enhance function in every day life and improve or enhance health-related quality of life. Improved health-related quality of life may also lead to fewer office visits and hospitalizations and hence reduce healthcare costs12,16.
With respect to diabetes, this means than healthcare professionals should not just focus on objective vital signs (eg blood pressure), physical examination findings (eg retinopathy, nephropathy, heart disease), and laboratory tests (eg hemoglobin A1c values). Rather, healthcare professionals should strive to also understand the subjective impact diabetes and its management has on a diabetic's physical and mental functioning - that is, their health-related quality of life. Ideally, treatment of diabetic patients should result in both improved glycemic control and better health-related quality of life42.
HRQOL was assessed in this study using both Medical Outcomes Study Short Form 36-item health survey (SF-36)34-36, and Centers of Disease Control and Prevention (CDC) Unhealthy Day questions16. Both are well established with good reliability, brevity, validity, responsiveness, and comparability. Both were designed to evaluate aspects of functional status and subjective wellbeing.
Within the Bella Coola Valley population, increasing age, Aboriginal status, and having diabetes were all found to be associated with poorer self-reported health-related quality of life scores. Although other studies have demonstrated increasing age13,14,16, Aboriginal status14,16,29,30, and diabetes13,14,16,35,38-40,43,44 are associated with poorer self-reported health-related quality of life scores, it does not appear that anyone has studied all three variables within one single population.
Mean scores for Aboriginal people in our study were lower than mean scores for non-Aboriginal people in all 8 health-related quality of life (SF-36) scales. Compared with non-Aboriginal people, Aboriginal people also had more unhealthy days. The precise reasons for lower scores in the Aboriginal population compared with the non-Aboriginal population remains to be determined. Presumably it reflects the fact Aboriginal peoples tend to have a poorer combination of health determinants. Compared with non-Aboriginal people, Aboriginal people - including those living in the Bella Coola Valley:
- have a higher smoking rate5,6,25,29,45-47
- have less formal education6,29,48
- are more likely to be unemployed - have high rates of unemployment29,48
- earn lower incomes than others - have high rates of poverty6,29,30,38,48
- have higher rates of illness/comorbidity (eg diabetes, hypertension, heart problems, cancer, arthritis/rheumatism, trauma )5,6,11,12,25,26,29,49-53
- suffer from high rates of post-traumatic stress/residential school syndrome6,29,54
- have higher age-adjusted mortality rates and lower life expectancy at birth6,29,55.
All these factors are associated with poorer self-rated health6,30,56, poorer community/population health6,29, and lower health-related quality of life scores6,30,56-59 compared with communities/populations with lower prevalence of these indicators. The interaction among all these variables is complex and not easy to sort out30,16,56,57. For example, higher education is associated with higher income, greater job security, better housing, better sense of control over one's life circumstances, which presumably explains the better health and higher overall quality of life scores.
Our data also reveal that even after controlling for age and ethnicity, diabetes mellitus significantly impacts one's day to day functioning and one's self-rated health perception. In general, health-related quality of life scores reported for Bella Coola diabetics are comparable with those reported for other diabetic populations, and they are much lower than those reported for other non-diabetic populations12,14,16,43,60-63.
The reason for lower health-related quality of life scores for diabetics is probably multifactorial. Compared with non-diabetic people, diabetic people - including those living in Bella Coola Valley:
- tend to be overweight6,16,25,64-69
- are more likely to be sedentary and less likely to exercise30,16,61,70
- are much more likely to have co-morbidities (eg hypertension, coronary artery disease, hypercholesterolemia)3,5,6,9-12,16,29,40,59,61,71-76 and suffer from complications such as painful polyneuropathy, upper gastrointestinal symptoms (eg pain, dyspepsia, reflux, diarrhea, constipation, incontinence), impotence, retinopathy, nephropathy, and amputations3,13,14,40,44,61,63,71,74-81
- are more likely to suffer from morbidity associated with high (hyperglycemia) and low (hypoglycemia)42,61,71,82.
All these things have been shown to negatively affect HRQOL.
Lower HRQOL scores may also reflect the fact that diabetes is a complicated disease to manage because there is no cure, and so optimal management involves asking patients to make numerous lifestyle changes of life-long duration14,39,42,60,83,84. People with diabetes are asked to follow prescribed diets, exercise regularly, stop smoking, take medications, monitor glucose levels regularly, be on the look out for complications, and some are asked to administer their own insulin. One study showed that higher quality of life was associated with greater perceived ease of adherence to treatment regimen. Unfortunately, few diabetics are able to comply with all the lifestyle changes asked of them85.
Finally, lower HRQOL scores in some diabetics may reflect poor coping strategies and/or negative emotional outcomes. Previous research has shown that depression and anxiety negatively impact patient reported quality of life. While some diabetics cope well with their chronic disease, others adopt less effective coping strategies which manifest as anxiety, withdrawal, depression, self-blaming, blaming others, denial, aggression, shame, hopelessness, and even anger86. Depression, for example, is said to be two- to four-fold more common in individuals with diabetes compared with the general population44, with prevalence rates as high as 31.7% being reported38,87. Diabetics with a diagnosis of depression score significant lower on every dimension of the Short Form Health-Related Quality-of-Life Questionnaire (SF-36) compared with those diabetics who are not depressed87. Apparently low health-related quality of life scores in diabetics is not due to a 'labeling' phenomena73,88. Labeling refers to the negative impact of being diagnosed with a chronic illness (eg hypertension and abdominal aortic aneurysm) can have on one's perception of wellbeing.
The strengths of this study include the fact that SF-36 items and Healthy days items were correlated with a chronic disease - diabetes - which was confirmed by clinical chart review to ensure that the 'gold standards' for diagnosing diabetes were met. The study does, however, suffer from some limitations. The sample size of Aboriginal diabetics and non-Aboriginal diabetics is relatively small. Not everyone living in the valley completed the health questionnaire. However we did review diabetic responder and non-responder charts, so it is known how much the survey responder group differs from the overall clinic recorded prevalence - which was not much. Our data suffer from limitations inherent in collecting medical chart information - especially incomplete information and non-standardized measurements. Reliability of the data could have been strengthened by having an independent review of a random sample of charts to assess for congruent findings between reviewers. Notwithstanding these limitations, the main objective of this study, to understand the relationship between diabetes and various self-reported health measurements for an isolated rural population, was still achieved.
A worthwhile study would be to compare clinic chart information (eg duration of diabetes, glycoslyated hemoglobin (HgA1c)60 levels, co-morbidity number13 and insulin usage13,60) to see whether or not there are any correlations between chart specific information and HRQOL data86.
Conclusion
Over the past 20 years, an epidemic of Type 2 diabetes mellitus has quietly developed among people living in the rural, remote community of Bella Coola. Our study revealed that diabetics report significant impairment in health-related quality of life compared with people who do not have diabetes. Aboriginal people report significant impairment in HRQOL compared with non-Aboriginal people. Aboriginal diabetics report the worst health-related quality of life scores.
Acknowledgements
The authors wish to acknowledge the staff at the Bella Coola Medical Clinic for survey assistance. Dr Thommasen would like to acknowledge the Community-Based Clinician-Investigator Program for financial support.
References
1. Expert Committee of the Canadian Advisory Board. Clinical practice guidelines for the management of diabetes in Canada. Canada Medical Association Journal 1998; 159(Suppl 8): S1-S29.
2. Canadian Diabetes Association. 2003 Clinical Practice Guidelines for the Prevention and Management of Diabetes in Canada. Canadian Journal of Diabetes 2003; 27(Suppl 2): S1-S152. Available: http://www.diabetes.ca/cpg2003/ (Accessed 15 August 2005).
3. Lloyd A, Sawyer W, Hopkinson P. Impact of long-term complications on quality of life in patients with type 2 diabetes not using insulin. Value in Health 2001; 4: 392-400.
4. National center for health statistics. National Vital Statistics Report, July 24, 2000: 48(11). Hyattville, MD: CDC, 2000.
5. Bobet E. Diabetes among First Nations People: Information from the 1991 Aboriginal Peoples Survey carried out by Statistics Canada. Health Canada, Cat. # H34-88/1998E. Ottawa: Ministry of Public Works and Government Services Canada, 1998; 31.
6. First Nations and Inuit Regional Health Survey National Steering Committee. First nations and Inuit Regional health Survey national Report. (Online) 1999. Available: http://www.naho.ca/firstnations/english/pdf/key_docs_1.pdf (Accessed 15 August 2005.
7. Evers S, McCracken E, Antone I, Deagle G. The prevalence of diabetes in Indians and Caucasians living in southwestern Ontario. Canadian Journal of Public Health 1987; 78: 240-243.
8. Pioro MP, Dyck RF, Gillis DC. Diabetes prevalence rates among First Nations adults on Saskatchewan reserves in 1990: comparison by tribal grouping, geography and with non-First Nation people. Canadian Journal of Public Health 1999; 87: 325-328.
9. Macaulay AC, Montour LT, Adelson N. Prevalence of diabetic and atherosclerotic complications among Mohawk Indians of Kahnawake, PQ. Canadian Medical Association Journal 1988; 139: 221-224.
10. Young TK. The Health of Native Americans: Towards a Biocultural Epidemiology. New York: Oxford University Press, 1994
11. MacMillan HL, MacMillan AB, Offord DR, Dingle JL. Aboriginal health. Canadian Medical Association Journal 1996; 155: 1569-1578
12. Stewart AL, Greenfied S, Hays RD, Wells K, Rogers WH, Berry SD, McGlynn EA, Ware JE. Functional status and well-being of patients with chronic conditions. Journal of the American Medical Association 1989; 262: 907-913.
13. Jacobson AM, Samson JA, de Groot M. The evaluation of two measures of quality of life in patients with type I and type II diabetes. Diabetes Care 1994; 17: 267-274.
14. Johnson JA, Nowatzki TE, Coons SJ. Health-related quality of life in diabetic Pima Indians. Medical Care 1996; 34: 97-102.
15. Camacho F, Anderson RT, Bell RA, Goff DC, Duren-Winfield V, Doss DD, Balkrishnan R. Investing correlates of health related quality of life in a low-income sample of patients with diabetes. Quality of Life Research 2002; 11: 783-796.
16. Centers for Disease Control and Prevention (CDC). Measuring healthy days: population assessment of health-related quality of life. Atlanta, GA: CDC, November 2000; 40.
17. Thommasen HV, Newbery P, Watt WD. Medical History of Central Coast of British Columbia. BC Medical Journal 1999; 41: 464-470.
1. BC Stats. P.E.O.P.L.E. 27, BC Ministry of Management Services. PO Box 9410, Stn Prov Govt Victoria, BC; 2003.
19. British Columbia Vital Statistics Agency. 2001 British Columbia census. Victoria, BC: Government of British Columbia, 2003.
20. Kennedy DID, Bouchard RT. Bella Coola Indians. In: W Suttles (Ed.). Handbook of North American Indians. Washington, DC: Smithsonian Institute, 1990.
21. McIlwraith TF. The Bella Coola Indians. Toronto: University of Toronto Press, 1992.
22. Thommasen HV. Prehistoric medicine on BC's Central Coast. BC Medical Journal 1999; 41: 343-346.
23. Acheson S. Culture, contact, demography and health among the Aboriginal peoples of British Columbia. In: A Persistent Spirit: Towards understanding aboriginal health in British Columbia PH Stephenson, SJ Elliott, LT Foster, J Harris (Eds). Canadian Western Geographical Series, Volume 31. University of Victoria, Victoria: Western Geographical Press, 1995
24. Patenaude J, Tildesley H, McArthur A, Thommasen A, Thommasen H. Prevalence of diabetes mellitus among aboriginal and other people living in a rural and remote community - the Bella Coola Valley. British Columbia Medical Journal 2005; Summer: [in press].
25. Thommasen HV, Patenaude J, McArthur A, Tildesley H. Diabetes related disorders and diseases among Aboriginal and other people living in the Bella Coola Valley. Rural and Remote Health Journal 4: 319. (Online) 2004. Available: http://rrh.org.au (accessed 15 August 2005).
26. Smylie J [Aboriginal Health Issues Committee]. A Guide for Health Professionals Working with Aboriginal Peoples: Health Issues affecting Aboriginal peoples. Journal of the Society of Obstetricians and Gynaecologists of Canada 2001; 100: 54-68.
27. Macaulay AC, Gibson N, Freeman W et al. Participatory research maximizes community and lay involvement. BMJ 1999; 319: 774-778.
28. Cave AJ, Ramsden VR. Hypothesis: the research page. Participatory action research. Canadian Family Physician 2002; 48: 1671-1672.
29. British Columbia Provincial Health Officer. A Report on the Health of British Columbians: Provincial Health Officer's Annual Report 2001. Feature report: The Health and Well-being of Aboriginal People in British Columbia. Victoria (BC): Ministry of Health and Ministry Responsible for Seniors; 2002.
30. Michalos AC, Thommasen HV, Anderson N, Zumbo B. Determinants of health and the quality of life in the Bella Coola Valley. Social Indicators Research 2005; 72: 1-50.
31. Thommasen HV, MacKenzie T, Klein MC, Lynch N, Reyes R, Grzybowski S. Bella Coola Hospital obstetric maternal outcomes: 1940 to 2001. Canada Journal of Rural Medicine 2005; 10: 13-21.
32. Thommasen HV, Klein MC, MacKenzie T, Grzybowski S. Bella Coola General Hospital perinatal outcomes: 1941 to 2001. Canada Journal of Rural Medicine 2005; 10: 22-28.
33. Meltzer S, Leiter L, Daneman D et al. 1998 clinical practice guidelines for the management of diabetes in Canada. Canadian Medical Association Journal 1998; 159(Suppl 8): S1-S29.
34. Ware JE, Snow KK, Kosinski M, Gandek B. SF-36 Health Survey: Manual and Interpretation Guide. Boston, MA: The Health Institute, New England Medical Center, 1993.
35. McDowell I, Newell C. Measuring health: A guide to rating scales and questionnaires, 2nd edn. New York: Oxford University Press, 1996; 447-456.
36. McHorney CA, Ware JE, Raczek AE. The MOS 36-Item Short-Form Health Survey (SF-36): II. Psychometric and Clinical Tests of Validity in Measuring Physical and Mental Health Constructs. Medical Care 1993; 31: 247-263.
37. McHorney CA, Ware JE, Lu JFR, Sherbourne CD. The MOS 36-Item Short-Form Health Survey (SF-36): III, tests of data quality, scaling assumptions, and reliability across diverse patient groups. Medical Care 1994; 32: 40-66.
38. Kaholokula JK, Haynes SN, Grandinetti A, Chang HK. Biological, psychosocial, and sociodemographic variables associated with depressive symptoms in persons with type 2 diabetes. Journal of Behavioral Medicine 2003; 26: 435-458.
39. Jacobson AM, Samson JA, deGroot M. The evaluation of two measures of quality of life in patients with type I and type II diabetes. Diabetes Care 1994; 17: 267.
40. Woodcock AJ, Julious SA, Kinmonth AL, Campbell MJ. Problems with the performance of the SF-36 among people with type 2 diabetes in general practice. Quality of Life Research 2001; 10: 661-670.
41. Snedecor GW, Cochran WG. Statistical methods. Ames, Iowa: Iowa State University Press, 1980.
42. Weinberger M, Kirkman MS, Samsa GP et al. The relationship between glycemic control and health-related quality of life in patients with non-insulin-dependent diabetes mellitus. Medical Care 1994; 29: 1173-1181.
43. Ohsawa I, Ishida T, Oshida Y, Yamanouchi K, Sato Y. Subjective health values of individuals with diabetes in Japan: comparison of utility values with the SF-36 scores. Diabetes Research and Clinical practice 2003; 62: 9-16.
44. Claiborne N, Massaro E. Mental quality of life: an indicator of unmet needs in patients with diabetes. Social Work in Health Care 2000; 32: 25-43.
45. Mitura V, Bollman RD. The health of rural Canadians: A rural-urban comparison of health indicators. Statistics Canada, cat. no. 21-006-XIE. Rural and Small Town Canada Analysis Bulletin 2003; 4: 1-23.
46. Angus Reid Group for the Heart and Stroke Foundation of BC and Yukon. Tobacco Use in BC 1997. (Online) 1997. Available: http://www.healthplanning.gov.bc.ca/tobacrs (Accessed 15 August 2005).
47. Statistics Canada. Canadian Community Health Survey (2000/2001). (Online) no date. Available: http://www.statcan.ca/english/freepub/82-221-XIE/00503/tables/html/2115.htm (Accessed 15 August 2005).
48. Thommasen CT, Thommasen HV. Health Profile Bella Coola Valley and Bella Bella, British Columbia Vancouver: Vancouver Coastal Health Authority, Coast Garibaldi Health Services, October 2003.
49. British Columbia Provincial Health Officer. A report on the health of British Columbians: Provincial Health Officer's annual report 1996. Victoria (BC): Ministry of Health and Ministry Responsible for Seniors; 1997.
50. Foster LT, MacDonald J, Tuk TA, Uh SH, Talbot D. Native health in British Columbia: A vital statistics perspective. In: PH Stephenson, SJ Elliott, LT Foster, J Harris (Eds). A persistent spirit: towards understanding aboriginal health in British Columbia. Canadian Western Geographical Series, Volume 31. Victoria: University of Victoria. Western Geographical Press, 1995; 43-94
51. Young TK. The health of Native Americans: toward a biocultural epidemiology. Oxford: Oxford University Press, 1994; 265.
52. British Columbia. Provincial Health Officer (PRW Kendall). A report on the health of British Columbians: Provincial Health Officer's annual report 1999. Victoria, BC: Ministry of Health and Ministry Responsible for Seniors, 2000; 184.
53. Karmali S, Laupland K, Harrop R et al. Epidemiology of severe trauma among status Aboriginal Canadians: a population-based study. Canada Medical Association Journal 2005; 172: 1007-1011.
54. Barton S, Thommasen HV, Tallio B, Zhang W, Michalos AC. Health and quality of life of residential school survivors, Bella Coola Valley. Social Indicators Research 2005; 73: 295-312.
55. Thommasen HV, Thommasen CT, Martiquet P, Jin A. Causes of death among status Indian and other people living in the Bella Coola Valley local health area (1987-2001). British Columbia Medical Journal 2004; 46: 179-187.
56. Michalos AC, Zumbo BD, Hubley A. Health and the quality of life. Social Indicators Research 2000; 51; 245-286.
57. Michalos AC. Social indicators research and health-related quality of life research. Social Indicators Research 2004, 65: 27-72.
58. Camacho F, Anderson RT, Bell RA, Goff Jr DC, Duren-Winfield V, Doss DD, Balkrishnan R. Investigating correlates of health related quality of life in a low-income sample of patients with diabetes. Quality of Life Research 2002; 11: 783-796.
59. Bardage C, Isacson DGL. Hypertension and health-related quality of life: an epidemiological study in Sweden. Journal of Clinical Epidemiology 2001; 54: 172-181.
60. Nerenz DR, Repasky DP, Whitehouse FW, Kahkonen DM. Ongoing assessment of health status in patients with diabetes mellitus. Medical Care 1992; 30: MS112-MS124.
61. Klein BEK, Kelin R, Moss SE. Self-rated health and diabetes of long duration: the Wisconsin Epidemiologic Study of Diabetic Retinopathy. Diabetes Care 1998; 21: 236-240.
62. Greenfield S, Kaplan SH, Silliman R et al. The uses of outcomes research for medical effectiveness, quality of care, and reimbursement in Type II diabetes. Diabetes Care 1994; 17: 32-39.
63. Gralnek IM, Hays RD, Kilbourne A, Naliboff B, Mayer EA. The impact of irritable bowel syndrome on health-related quality of life. Gastroenterology 2000; 119: 654-660.
64. Self B, CL Birmingham, Elliott R, Zhan W, Thommasen HV. Prevalence of overweight adults living in a rural and remote community - the Bella Coola Valley 2004.
Journal of Eating and Weight Disorders 2005; [in press].
65. Lean ME, Han TS, Seidell JC. Impairment of health and quality of life using new US federal guidelines for the identification of obesity. Archives of Internal Medicine 1999; 159: 837-843.
66. Fontaine KR, Barofsky I. Obesity and health-related quality of life. Obesity Reviews 2001; 2: 173-182.
67. Ford ES, Moriarty DG, Zack MM, Mokdad AH, Chapman D. Self-reported body mass index and health-related quality of life: findings from the behavioral risk factor surveillance system. Obesity Research 2001; 9: 21-31.
68. Larsson U, Karlsson J, Sullivan M. Impact of overweight and obesity on health-related quality of life - a Swedish population study. International Journal of Obesity 2002; 26: 417-424.
69. Doll HA, Petersen SEK, Stewart-Brown SL. Obesity and physical and emotional well-being: associations between body mass index, chronic illness, and the physical and mental components of the SF-36 questionnaire. Obesity Research 2000; 8: 160-170.
70. Brown DW, Balluz LS, Heath GW et al. Associations between recommended levels of physical activity and health-related quality of life: Findings from the 2001 Behavioral Risk Factor Surveillance System (BRFSS) survey. Preventive Medicine 2003; 37: 520-528.
71. UK Prospective Diabetes Study Group. Quality of life in type 2 diabetic patients is affected by complications but not by intensive policies to improve blood glucose or blood pressure control (UKPDS 37). Diabetes Care 1999; 22: 1125-1136.
72. Glasgow RE, Ruggiero L, Eakin EG, Dryfoos J, Chobanian L. Quality of life and associated characteristics in a large national sample of adults with diabetes. Diabetes Care 1997; 20: 562-567.
73. Edelman D, Olsen MK, Dudley TK, Harris AC, Oddone EZ. Impact of diabetes screening on quality of life. Diabetes Care 2002; 25: 1022-1026,
74. Ahroni JH, Boyko EJ. Responsiveness of the SF-36 among veterans with diabetes mellitus. Journal of Diabetes and its Complications 2000; 14: 31-39.
75. Talley NJ, Young L, Bytzer P, Hammer J, Leemon M, Horowitz M. Impact of chronic gastrointestinal symptoms in diabetes mellitus on health-related quality of life. American Journal of Gastroenterology 2001; 96: 71-76.
76. Martinez-Castelao A, Gorriz JL, Garcia-Lopez F, Lopez-Revuelta K, De Alvaro F, Cruzado JM. Perceived health-related quality of life and comorbidity in diabetic patients starting dialysis (CALVIDIA study). Journal of Nephrology 2004; 17: 544-551.
77. Galer BS, Gianas A, Jensen MP. Painful diabetic polyneuropathy: epidemiology, pain description, and quality of life. Diabetic Research and Clinical Practice 2000; 47: 123-128.
78. Siddique R, Ricci J, Stewart WF, Sloan S, Farup C. Quality of life in a US national sample of adults with diabetes and motility-related upper gastrointestinal symptoms. Digestive Diseases and Sciences 2002; 47: 683-689.
79. Pinzur MS, Evans A. Health-related Quality of Life in patients with Charcot foot. American Journal of Orthopedics 2003; October: 492-496.
80. Padua L, Saponara C, Ghirlanda G et al. Health-related quality of life in type 1 diabetic patients and influence of peripheral nerve involvement. Neurological Science 2001; 22: 239-245.
81. De Berardis G, Franciosi M, Belfilglio M et al. Erectile dysfunction and quality of life in type 2 diabetic patients. Diabetes Care 2002; 25: 284-291.
82. Thommasen HV, McArthur A, Tiernay M, Nast S, Tildesley H. Do rural diabetics benefit from the occasional visit to an urban based diabetic education centre? British Columbia Medical Journal 2004; 46: 467-471.
83. Okano GJ, Malone DC, Billups SJ et al. Reduced quality of life in veterans at risk for drug-related problems. Pharmacotherapy 2001; 21: 1123-1129.
84. Hanestad BR, Albrektsen G. Quality of life, perceived difficulties in adherence to a diabetes regimen, and blood glucose control. Diabetic Medicine 1991; 8: 759-764.
85. Bloom-Cerkoney KA, Hart LK. The relationship between the health belief model and compliance of persons with diabetes mellitus. Diabetes Care 1980; 3: 594-598.
86. Lundman B, Norberg A. Coping Strategies in People with Insulin-dependent Diabetes Mellitus. Diabetes Educator 1993; 19: 198-204.
87. Goldney RD, Phillips PJ, Fisher LJ, Wilson DH. Diabetes, depression, and quality of life. Diabetes Care 2004; 27: 1066-1070.
88. Adriaanse MC, Snoek FJ, Dekker JM et al. No substantial psychological impact of the diagnosis of Type 2 diabetes following targeted population screening: The Hoorn Screening Study. Diabetes Medicine 2004; 21: 992-998.




