Context
Background
Recent reforms undertaken within the Mental Health Service in southern Queensland recognised that cultural issues were of significant concern to Indigenous consumers. Consequently, a major initiative commenced in 1999 to review the cultural safety of Indigenous people accessing the District Mental Health Service in south-east Queensland. Cultural safety refers to making sure that cultural difference is respected. The purpose of the review was to assist with implementing the 'State Mental Health policies and plans and in particular the National Mental Health Plan'1, 'Queensland Mental Health Policy Statement for Aboriginal and Torres Strait Islander People'2 and the 'Ten Year Mental Health Strategy for Queensland'3.
In line with these developments, the Toowoomba District Mental Health Service (TDMHS) in South East Queensland has developed a 'Model of Service Delivery'4 which outlines the range of services provided for all consumers across their lifespan. Indigenous consumers of the TDMHS come from a wide area of communities in the surrounding shires such as Charleville, Chinchilla, Dalby, Goondiwindi, Kingaroy, Roma, Stanthorpe, St George and Warwick (rural, remote and metropolitan areas (RRMA) 4-7). The TDMHS recognised that these Indigenous consumers have unique needs and that this area of service delivery required greater attention and further development. A symposium was organised by the service to bring together a range of speakers and participants to discuss issues and work towards developing strategies to enable the service to better meet the needs of Indigenous consumers in this rural region of south-east Queensland.
The Toowoomba District Mental Health Service Indigenous Mental Health Symposium was held on the 2nd and 3rd December 2004. The participants came from across Queensland and other Australian states to discuss the challenges of improving the delivery of culturally safe mental health services to Indigenous people accessing the service.
The theme of the symposium was 'Service Capacity Building'. Speakers and a workshop focussed on a wide range of topics with the aim of sharing knowledge and strategies for improving the mental health service delivery to Indigenous consumers. Presented in this report is an overview of the proceedings from this workshop.
Participants
An important aspect of this symposium was the mix of delegates who contributed. Ninety delegates attended, 40 of whom were Indigenous. The symposium was well attended by delegates from Central Australia, Cape York, Sydney and throughout Queensland, some of whom were experts in this area and invited speakers. A range of non-government and government agencies were represented by delegates who came from a range of disciplines such as psychiatry, psychology, social work, Aboriginal health/mental health, nursing and other mental health support fields. Table one shows the breakdown of professions represented by symposium participants. This mix of participants resulted in discussions that encompassed many disciplines and emphasised the multidisciplinary nature of the conference theme: service capacity building.
Table 1: Delegate professions represented at the Indigenous Mental Health Symposium
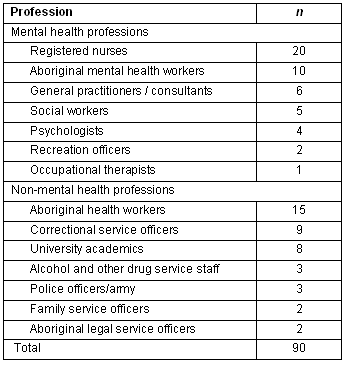
Approximately 60 delegates participated in the symposium workshop. Data from this workshop are presented in aggregate form as responses from the participants. Formal consent was not obtained from individual participants but the workshop facilitator advised prior to commencement that the workshop proceedings would be disseminated in aggregate form as part of a journal article for future publication.
Issues
The symposium program consisted of key note speakers and invited papers, and culminated with an afternoon workshop that collated the symposium's main issues and themes. This gave the delegates a chance to reflect, discuss, debate and brainstorm their major issues of concern. A group facilitator guided the discussion and organised the delegates into groups to evaluate, discuss and propose action to be taken on each of the major issues raised at the symposium.
The objective of the workshop was, 'Identifying ways to meet Indigenous mental health needs'. The workshop consisted of four stages:
- The first stage put this objective to the group as a question, 'How can we meet the mental health needs of Indigenous people'? Delegates were asked to respond in turn to this question and their responses were collated on a white board until no new responses emerged from the group. Each response was further discussed to define what it meant to the group. Table two lists these responses taken from the group and presents them as major themes with accompanying definitions.
- The second stage entailed the entire group voting on those themes considered most important to discuss in greater depth. The group was limited to identifying seven themes because of time considerations.
- These themes were then ranked according to the potential impact each theme had on meeting the needs of Indigenous mental health consumers. Table two lists these as the first seven themes.
- The remainder of the workshop involved splitting into seven small groups to discuss in greater depth these seven themes (one theme per small group).
- Finally a member from each group reported in plenary on the results of their discussion and identified strategies to address, implement or improve the issues associated with their theme.
The feedback and recommendations arising from these small group discussions will be discussed briefly.
Table 2: Responses to, 'How can we meet the mental health needs of Indigenous people'?
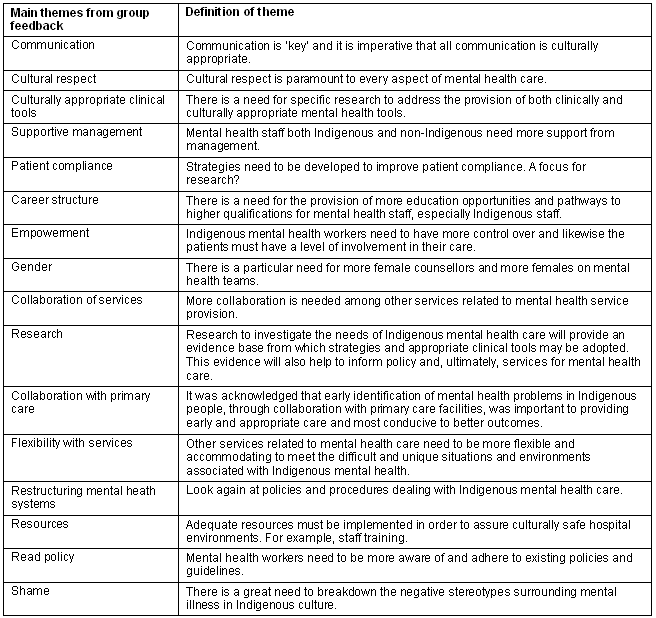
Lessons learned
Communication
A major consensus of the afternoon was that communicating with Indigenous mental health patients can be problematic. By problematic we refer to the discrepant understanding of Indigenous culture by those who work in the area of Indigenous mental health5. Consideration of the powerful link between communication and trust is a vital component of their care. Although the last decade has seen a greater emphasis placed on communication with Indigenous patients in practice, the reality is that misunderstanding and miscommunication in mental health treatment and care is common and results in negative effects for patients and carers6. Recommendations included:
- Greater involvement of Indigenous people. For example, including family or community members in the treatment and care of Indigenous mental health patients.
- Dedicated Indigenous health care facilities staffed by both Indigenous and non-Indigenous health care workers and clinicians who are culturally aware.
- Research into improved methods of achieving and maintaining better communication between patients and carers.
Cultural respect
The theme of cultural respect is closely related to communication. It relates to greater awareness of culture, leading to greater understanding, leading to greater cultural respect on the part of non-Indigenous mental health workers and clinicians toward Indigenous consumers5-8. Mandatory cultural awareness programs have been implemented across Queensland Health staff but more needs to be done to achieve the understanding to effectively communicate with Indigenous mental health patients. Recommendations included:
- Expanding and updating current cultural awareness programs in hospitals and training programs for medical students, health workers, clinicians and consultants.
- Merging these cultural awareness programs with community programs to promote increased understanding and respect on the community level as well as the individual level.
Culturally appropriate clinical tools
The issue 'culturally appropriate clinical tools' is also associated with communication such that it would stem from understanding and effective communication between health workers, clinicians and consultants and Indigenous consumers. This was seen as a 'Catch 22' scenario. In other words, in order to produce culturally appropriate tools, effective communication is vital5,6. However it is recognised that, fundamentally, communication is poor, so until that improves, producing tools to deal with Indigenous mental health consumers' needs will remain problematic. Recommendations included:
- Specific research to address the best ways to improve communication between mental health workers/clinicians and their patients.
- This might involve development of appropriate tools. For example, development of culturally appropriate questionnaires and survey tools in a language and delivered in a manner that Indigenous mental health patients understand. It is suggested that this will help reduce misdiagnosis of patients' symptoms.
- The involvement of Indigenous people was seen as paramount to this process and to achieve success and credibility.
Supportive management
It was noted that both Indigenous and non-Indigenous mental health staff need more support from management. Management meant higher level supervisory staff who support mental health staff. Issues such as flexibility of rostering and more support for attending community programs and up-skilling opportunities were cited. The delegates agreed that this was related to career structure and discussion involved strategies to encourage team building as well as greater recognition of achievement and competencies9. Recommendations included:
- A clear pathway to progress to higher skills and training for Indigenous mental health workers.
- More opportunities for achieving higher qualifications and support from management to allow time off to pursue these opportunities.
Patience compliance
Patient compliance was recognised as a major difficulty across all disciplines of health care and is not unique to Indigenous mental health consumers. However it was again noted that communication could play a major part in improving patient compliance among Indigenous mental health consumers5,6,10. Recommendations included:
- More education of the early warning signs of mental health problems within Indigenous communities.
- Involvement and education of family members and significant others in these signs.
- Positive role models, particularly for young people, to discourage drug and alcohol abuse.
- The formation of Indigenous support groups in areas of the most need.
- Specific research that might test interventions to improve compliance.
Career structure
A recognised need for the provision of a more structured pathway to higher qualifications for mental health workers was another dominant issue. This was related to supportive management. In particular there should be clearer pathways to higher qualifications for Indigenous mental health workers and staff9. Recommendations included:
- The formation of a forum for the development and subsequent supervision of a structured pathway to higher qualifications. This forum could be led by both Indigenous and non-Indigenous experts in the field of mental health.
- A peer group support structure for those workers undergoing training and higher qualifications.
- Mentoring schemes for junior staff members by more senior Indigenous and non-Indigenous staff.
Empowerment
Indigenous mental health workers need to have greater input into patient care. Inappropriate guidelines and outdated polices were partly responsible for the difficulties encountered by mental health workers with certain types of patients and in some regions. Likewise, there should be a movement toward a greater level of patient involvement in their own care. Again the group discussed the implementation of more education opportunities for the Indigenous workforce which relates directly to previous themes and corroborates this need. Better education of mental health workers would be conducive to greater ownership of the service by the Indigenous workforce9. Furthermore, it was recognised that greater empowerment on an individual level would also lead to better linkage between the services provided by these individuals and the community. Recommendations echoed those put forward for previous themes of career structure and supportive management discussed above but also included:
- When appropriate, involve the patient in his/her care.
- Likewise, involve the family and significant community members in order to provide support and guidance to the patient while in care.
Limitations
Further elaboration on the major themes and how they might be researched would have been a worthwhile exercise and outcome of the symposium. Unfortunately the time constraints of the workshop, which was held in one afternoon, would not allow this. A further limitation of these findings was the absence of consumers or mental health patients at the workshop. While this forum was intended to focus on the perspectives of those working in the system, clearly consumer perspectives also need to be considered in any policy changes arising from these conference recommendations.
Conclusions
The consensus of the participants was that the issues discussed were important and that research is needed in several areas to address these. The findings of this Indigenous Mental Health Symposium support the organisation of another symposium in 2006. Participants suggested a number of topics to be included in the 2006 symposium, and these, plus an update on related progress and action in the interim, will be considered.
Statements on the recommendations of this symposium are proposed for inclusion into two major documents within the TDMHS. These are the recommendations arising from the 'Indigenous Mental Health Needs Analysis'7 and the Queensland Indigenous mental health policy statement at the proposed TDMHS Aboriginal and Torres Strait Islander Mental Health one day planning forum in May 2005. These important documents provide the TDMHS with information to assist with development of a strategic framework to further improve its delivery of mental health service to Indigenous people accessing the service. The outcomes and further recommendations of this forum will be reported in a future publication.
Acknowledgements
Financial sponsorship was provided by the Toowoomba Hospital Mental Health Unit and Eli Lilly (Australia), and Astra Zeneca assisted by assisting in the costs of setting up and running the symposium.
References
1. Australian Health Ministers. National Mental Health Plan. Canberra AGPS, 1992.
2. Queensland Health. Queensland Mental Health Policy Statement for Aboriginal and Torres Strait Islander People. Brisbane: Queensland Health, 1996.
3. Queensland Health. The Ten Year Mental Health Strategy for Queensland. Brisbane: Queensland Health, 1996.
4. Toowoomba District Mental Health Service. Model of Service Delivery. Toowoomba: Toowoomba District Mental Health Service, 2001.
5. Eley D, Hunter K, Baker P, Young L, Hunter E, Hannah D. The tools and methodologies for investigating the mental health needs of Indigenous consumers: it's about communication. Australasian Psychiatry 2006; 14:(in press).
6. Hunter E. Communication and Indigenous Health. Australian Doctor 2004; 4 June: 35-42.
7. Toowoomba District Mental Health Service. Indigenous Mental Health Needs Analysis Project Final Report. Toowoomba, Qld: Toowoomba District Mental Health Service, 2003.
8. Hunter E. 'Best intentions' lives on: untoward health outcomes of some contemporary initiatives in Indigenous affairs. Australian and New Zealand Journal of Psychiatry 2002; 36: 575-584.
9. Hunter E. Staying tuned to developments in Indigenous health: reflections on a decade of change. Australasian Psychiatry 2003; 11: 418-423.
10. Aleksandar J, Bullen C. The Aboriginal concept of time and its mental health implications. Australasian Psychiatry 2003; 11: 40-44.

