Introduction
Indigenous children in Australia are those who identify as Aboriginal, Torres Strait Islander or both. Such children represent 4.7% of the Australian child population1. In the Northern Territory - a vast area with a population of approximately 200 000 - approximately 40% of children aged 4-14 years are Indigenous and some 80% of such children live in rural or remote areas1.
Increasing exposure to non-Indigenous lifestyles has had a marked impact on Indigenous health, particularly Indigenous child health. Indigenous children are more likely to be hospitalised than other Australian children, and are at higher risk of disease and injury2. They experience greater disability and reduced quality of life due to ill health, partake in higher levels of health risk behaviours (eg petrol sniffing) and are more exposed to violence in the home. In 2002, Indigenous child mortality rates were 2.7 times those of non-Indigenous children2. Indigenous children are also more than twice as likely to have been born underweight than other Australian children2, with low birth weight babies being more prone to ill health, including dental ill-health, in later life3,4.
Among the more profound Indigenous lifestyle modifications to have impacted on health is change in diet5. The food intake of Indigenous Australian children has undergone rapid modification in the last decade, with a diet that was rich in fiber, protein and low saturated fat being replaced by one in which refined carbohydrates and saturated fats predominate6. Such dietary changes, together with an increasingly sedentary life-style, have had a grave impact on the general health of remote Indigenous children, with the prevalence of obesity and type II diabetes among such children escalating in recent years7.
Up until the 1980s, Indigenous Australian children were recognised as having better oral health than their non-Indigenous counterparts8-11. Recent evidence suggests, however, that Indigenous children now have, on average, twice as much (and in some communities, up to five times as much) tooth decay as their non-Indigenous counterparts12,13. In one study of remote Indigenous children, less than 10 percent of tooth surfaces with experience of decay had been treated with a filling, and more than 90% of child dmfs (the sum of decayed, missing and filled deciduous tooth surfaces) was made up of either decayed or missing surfaces14.
This study is part of a wider investigation examining the feasibility and impact of introducing water fluoridation plants into remote communities in the Northern Territory's Top End. The purpose of this report is to describe the self-reported use of dental services, dental health behaviours and dietary characteristics relevant to fluoride intake of Indigenous children in these communities. The article provides some insights into dental behavioural characteristics of children in a remote Australian Indigenous context, and should be useful in the design and application of oral health promotion initiatives in this and similar settings.
Methods
In 2003, small-scale fluoridation plants were installed in two remote communities in the 'Top End' of the Northern Territory with naturally low fluoride levels in the water and with a high prevalence of child dental disease. Another community was selected as a comparison site (natural levels of water fluoride low). The study population for purposes of our investigation comprised all children aged between 4 and 12 years (inclusive) in the three communities hereafter referred to as Community A, B or C (Figure 1). Uncertainty of population estimates and high mobility of residents between communities and houses within communities15,16 precluded a random sampling approach. We therefore aimed to interview as many carers of children in the target age range as possible. For each child, data on carers' highest level of educational attainment and the child's age, sex, use of dental services, dental care behaviours, diet and household water source was obtained. The questionnaires were administered by a project officer assisted by a local community member in carers' homes or other locations in and around the community, depending on where carers could be located and their preference for location and time of interview. The dietary questions were based on those by Levine17 who found that children who consumed cariogenic food and beverage products in the evening had markedly more dental caries than their counterparts who did not. Ethical approval was obtained from the formally constituted ethics committee and the Indigenous sub-committee for this region. Informed consent was obtained from the carers.
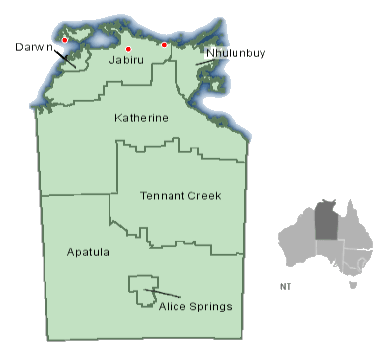
Figure 1: Location of the three study communities in relation to Darwin, Northern Territory (communities highlighted in red).
Data were analysed using SPSS vers 13.0 (SPSS Inc; Chicago, IL, USA) and levels of statistical significance were set at p<0.05. The c2 test was used to measure statistically significant differences between proportions.
Results
In total, 214 carers completed questionnaires for 409 children; 131 (32.0%) from Community A, 158 (38.6%) from Community B and 120 (29.3%) from Community C. The response rate of the child survey based on Census data (generally regarded as an undercount) was 55% across the three communities, ranging from 47% in Community B to 72% in Community A. Response rates based on other population estimates were somewhat lower (Table 1).
Table 1. Coverage area of interview data
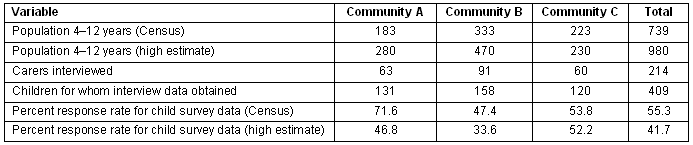
Approximately one-third of carers had had no secondary schooling (36%) and one-fifth (21%) could not recall their highest level of educational attainment (Table 2).
Table 2. Education characteristics of carers by location
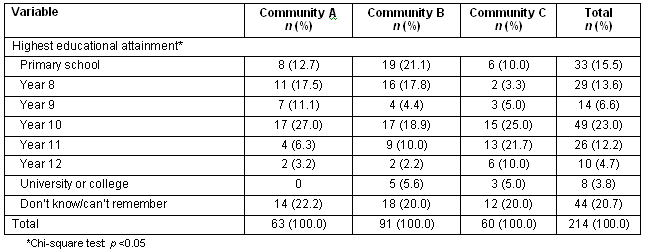
The ages of children for whom data were obtained were reasonably evenly spread across the target age range, with slightly smaller numbers in the higher and lower ages. There were no significant differences between communities by sex (Table 3).
Table 3. Demographic characteristics of children by location
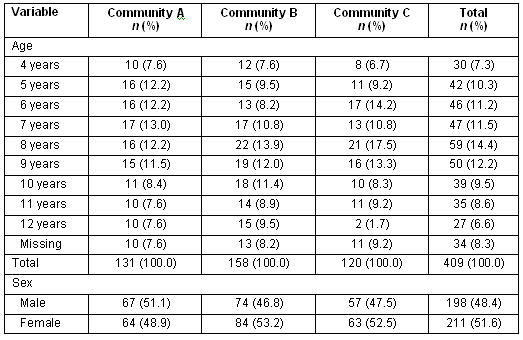
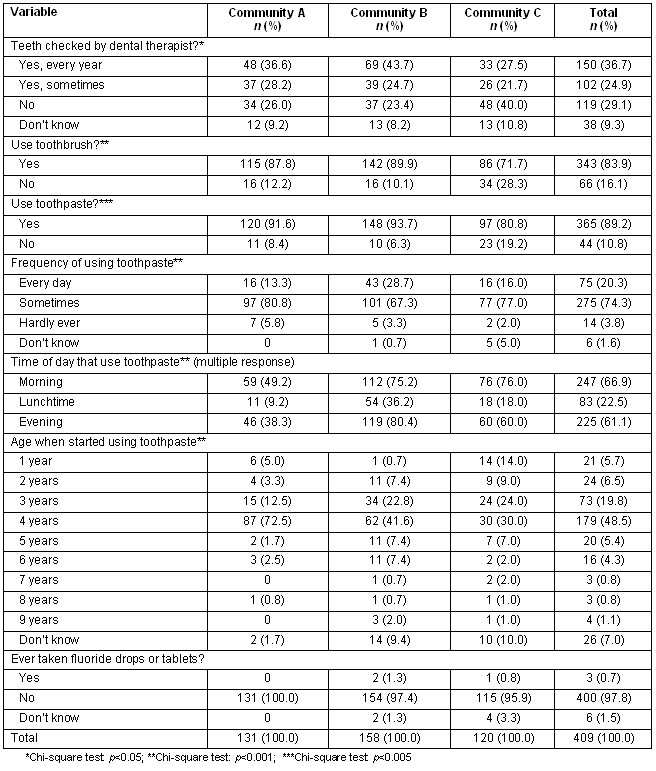
Approximately one-third (37%) of children were reported to have had their teeth checked every year by a dental therapist, although this varied significantly between communities (range 28% to 44%; Table 4). Most children (84%) were reported to use a toothbrush, but again there were significant community variations (Table 4). While 89% of children were reported to use toothpaste (with a similar significant variation between communities), only 20% of these children were reported to use it every day (Table 4). Time of toothpaste use was reasonably evenly distributed between morning (67%) and evening (61%), with some children reportedly using it twice a day, and a small proportion reporting use at lunchtime (23%). Across all communities, the most common age that toothpaste application began was 4 years (49%) and less than 2% of children had ever taken fluoride tablets or drops.
Table 4. Self-reported use of dental services and dental behaviour characteristics of children by location
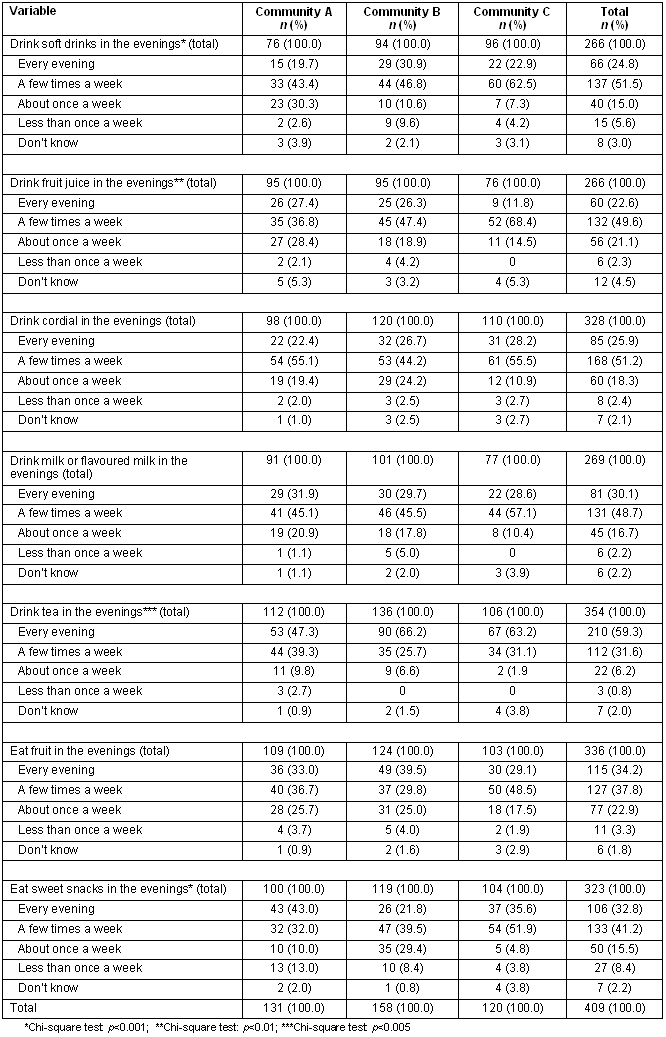
Over three-quarters of children who reportedly consumed softdrinks, cordial, milk or flavoured milk in the evenings drank such beverages at least a few evenings each week (Table 5). Over 90% of children across the three communities who reportedly drank tea, and about three-quarters of those who consumed sweet snacks, did so at least a few evenings each week (Table 5).
Table 5. Self-reported dietary characteristics of children by location
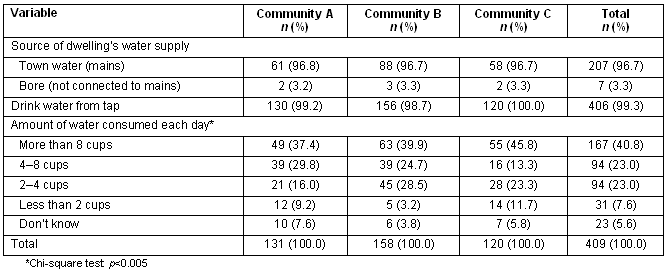
Almost all (97%) carers reported that their house was connected to the community water supply (Table 6) and most (99%) children sourced their drinking water from a tap (household or otherwise; Table 6). Approximately two-thirds (64%) of children were reported to drink more than 4 cups of water a day
Table 6. Household water source and self-reported water consumption of children by location
Discussion
This cross-sectional investigation of remote-dwelling Indigenous children has shown:
- low levels of regular dental preventive care
- irregular application of toothpaste use
- late onset of toothpaste utilisation
- negligible implementation of alternate fluoride sources (drops or tablets)
- high consumption of sweetened drinks and snacks in the evenings
- almost universal connection of houses to the public water supply.
The study provides some insights into factors that may contribute to the poor and declining state of dental health in Indigenous children.
The prevalence of child use of dental services reported by carers was lower than reported figures for the general Northern Territory child population18. This is despite the Northern Territory School Dental Service (SDS) visiting each community in the study several times annually. The under-utilisation of such services may be due to a number of reasons including:
- limited awareness of preventive dental measures
- inability to obtain consent from carers for child dental check-ups and follow-up care
- high mobility of children
- low school attendance limiting opportunities for SDS therapists to deliver services
- short duration of SDS visits
Limited dental service utilisation has also been reported among remote-dwelling Indigenous children in New Zealand19 and Alaska20.
Low levels of carer education, together with high toothpaste costs and difficulties in establishing tooth-brushing routines due to a number of different households being stayed in a given week21, may contribute to the low prevalence of toothpaste use in our study compared with that reported in the general Australian child population22. The most frequently reported age that toothpaste was first used was 4 years, which perhaps reflects pre-school commencement and consequent initiation of institution-organised oral hygiene strategies. However, only 20% of children were reported to use toothpaste every day. It is recommended that brushing of teeth begin soon after the emergence of primary teeth (around 6 months of age), low-concentration fluoride toothpaste use to commence at the age of 18 months and for teeth to be brushed twice a day (with the child needing assistance up until at least the age of five years)23. Late onset of tooth brushing with a fluoride toothpaste is a predictor of poor child oral health outcomes24.
Children in our study had a higher reported frequency of cariogenic food and beverage consumption than their average Australian counterparts7, which may have been due to:
- lack of healthy food available in communities2
- lack of culturally appropriate information on healthy food available in communities or
- lack of nutritional knowledge by carers.
People in remote communities have limited access to fresh food produce, although there is generally no shortage of cariogenic food and beverage items5. The motivation to purchase fresh food produce is often marred by cost, with vegetables and fruit frequently being more expensive than less nutritious food options6. Our findings are supported by Gracey, who reported that consumption of carbonated beverages and confectionary among remote-living Indigenous children had almost become the cultural norm7.
The Top End of the Northern Territory experiences a tropical climate with an annual temperature range of 19-35°C25. That most children were reported to drink over 4 cups of water each day, and to drink tea every evening, was consequently unsurprising and bodes well with the introduction of water fluoridation plants as a means of reducing child caries levels.
Limitations of this study
Obtaining reliable self-report information from remote-dwelling Indigenous populations is acknowledged as being difficult26 and our study was no exception. The generalisability and precision of the findings are limited by the response rates and the non-random sampling process. Biases may also have been introduced by community residents introducing the data-collector to carers who were generally more educated, of higher socio-economic status and who spoke English with more ease. Locating families in the poorer parts of each community was frequently not possible due to the reluctance of community assistants to go there. Furthermore, the dietary and water consumption questions were difficult to administer and carers frequently struggled with quantities, frequencies and the usual patterns of their children (who often ate at relatives homes). A degree of caution should therefore be exercised when interpreting the investigation's findings.
Conclusion
Our study is noteworthy for being a rare example of the use of face-to-face interview techniques to obtain remote-dwelling Indigenous child dental self-care and dietary information. The findings provide a useful basis for further investigations to enhance promotion of dental health and delivery of dental services in these and other remote community settings.
Acknowledgements
The authors gratefully acknowledge the participation of community residents, specifically those who aided in administering the survey and facilitating community relationships, the assistance of Harold Ulamari in community liaison and fieldwork and the support of the Northern Territory Children's Dental Service staff. This project was supported by a NHMRC Strategic Research Development Grant 219204/OH047. Ross Bailie is supported by an NHMRC Fellowship Grant 283303.
References
1. Australian Bureau of Statistics. Indigenous Profile 2001 Census of Population and Housing. Canberra: Australian Government, 2001.
2. Australian Institute of Health and Welfare. Australia's Health 2004. Canberra: AIHW, 2004.
3. Nicolau B, Marcenes W, Bartley M, Sheiham A. A life course approach to assessing causes of dental caries experience: the relationship between biological, behavioural, socio-economic and psychological conditions and caries in adolescents. Caries Research 2003; 37: 319-326.
4. Kuh D, Ben Shlomo Y. A life course approach to chronic disease epidemiology. Oxford: Oxford University Press; 1997; 3-14.
5. Burns J, Irvine J. Nutrition and growth. In: N Thomson (Ed.). The Health of Indigenous Australians. Melbourne, VIC: Oxford University Press, 2003; 75-93.
6. Australian Bureau of Statistics. The Health and Welfare of Australia's Aboriginal and Torres Strait Islander Peoples, 2005. Canberra: Australian Government, 2005.
7. Gracey M. Historical, cultural, political, and social influences on dietary patterns and nutrition in Australian Aboriginal children. American Journal of Clinical Nutrition 2000: 72; 1361-1367.
8. Barrett MJ. Dental observations on Australian Aborigines, Yuendumu, Central Australia, 1951-52. Australian Journal of Dentistry 1953; 57: 27-38.
9. Kailis DG. Dental conditions observed in Australian Aboriginal children resident in Warburton and Cundeelee mission, Western Australia. Australian Dental Journal 1971; 16: 44-52.
10. Kailis DG. Prevalence of dental caries in Australian Aboriginal children resident in Carnarvon, Western Australia. Australian Dental Journal 1971; 16: 109-115.
11. Barrett MJ, Williamson JJ. Oral health of Australian Aborigines: Survey methods and prevalence of dental caries. Australian Dental Journal 1972; 32: 37-50.
12. Tennant M, Namjoshi D, Silva D, Codde J. Oral health and hospitalisation in Western Australian children. Australian Dental Journal 2000; 45: 204-207.
13. Schamschula RG, Cooper MH, Adkins BL, Barmes DE, Agus HM. Oral conditions in Australian children of Aboriginal and Caucasian descent. Community Dentistry and Oral Epidemiology 1980; 8: 365-369.
14. Bourke C, Baima D, Allister J, Spencer AJ. Caries experience of Aboriginal children in South Australia. Journal of Dental Research 1999; 78: 951.
15. Paice J, Dugbuaza T, Taylor J. Issues in estimating families. In: Proceedings, Australian Population Association Conference; December 1996; Adelaide, South Australia.
16. Taylor J. Measuring short-term population mobility among Indigenous Australians: Options and implications. Australian Geographer 1988; 29: 125-136.
17. Levine RS. Caries experience and bedtime consumption of sugar-sweetened food and drinks - a survey of 600 children. Community Dental Health 2001; 18: 228-231.
18. Armfield JM, Roberts-Thomson KF, Slade GD, Spencer AJ. Child Dental Health Survey, Northern Territory 2000. Adelaide: The University of Adelaide, 2003.
19. National Health Committee. Improving child oral health and reducing child oral health inequalities. Wellington: New Zealand Ministry of Health, 2003.
20. Sekiguchi E, Guay AH, Brown LJ, Spangler TJ Jr. Improving the oral health of Alaska Natives. American Journal of Public Health 2005; 95: 769-773.
21. Nganampa Health Council. Dentistry in remote Aboriginal communities. Alice Springs: Nganampa Health Council, 2001.
22. Harford J, Spencer AJ, Roberts-Thomson KF. Oral Health. In: N Thomson (Ed.). The health of Indigenous Australians. Victoria: Oxford University Press, 2003; 313-338.
23. Centre for Disease Control and Prevention. Brush up on health teeth fact sheet. (Online) 2005. Available: http://www.cdc.gov/OralHealth/factsheets/brushup.htm (Accessed 8 September 2005).
24. Ferreira MA, Mendes NS. Factors associated with active white enamel lesions. International Journal of Paediatric Dentistry 2005; 15: 327-334.
25. Smitz P, Evans M, Cruttenden P et al. Lonely Planet - Australia, 12th edn. Melbourne, VIC: Lonely Planet, 2004; 954.
26. Couzos S, Lea T, Murray R, Culbong M. 'We are not just participants--we are in charge': the NACCHO ear trial and the process for Aboriginal community-controlled health research. Ethnicity and Health 2005; 10: 91-111.




