Introduction
This article outlines the development and content of a community-based research capacity building (RCB) framework for Aboriginal and Torres Strait Islander health workers (hereafter called health workers). The focus is on the major issues that enhance a proactive service delivery model using culturally appropriate research methods. Research capacity building is defined here as a planned, structured approach to increasing health workers' knowledge and skills about research so that they can assess and contribute to research and evaluation activities within their communities. To achieve maximum benefit, this should take place with active community consultation which builds processes and strategies associated with RCB that are both relevant and culturally appropriate for the community involved.
Health workers can play a major role in facilitating culturally appropriate healthcare delivery and program development through the acquisition of improved skills in the planning, monitoring and evaluation of these programs, as recognised in the recent rounds of the National Health and Medical Research Council (NHMRC) Capacity Building Grants in Population Health1. Indeed, the National Aboriginal Health Strategy and, more recently, the NHMRC encourage active involvement of health workers in all phases of planning health initiatives; including needs assessment, development, implementation and evaluation phases, notwithstanding cultural processes including information sharing and ownership, cultural respect for the individual, and the community2,3. However, such documents do not provide a framework for training health workers appropriately for these tasks. Additionally, formal course-based education programs for health workers tend to provide rudimentary theoretical overviews of the research process and are institutionally based. The framework described here, and developed through a consensus process with Aboriginal and Torres Strait Islander communities and representatives, is intended to provide practical, community-based RCB within health workers' own healthcare services and communities.
Background
Among Aboriginal and Torres Strait Islanders, the term 'research' is 'a dirty word' and many Aboriginal and Torres Strait Islander people are wary of research endeavours4. Research involving Aboriginal and Torres Strait Islander people in Australia has a chequered history, particularly in health-related fields, where much research in the past was often poorly designed, non-collaborative and based on cultural and social engineering theories5-8. The impact of these past practices persists today: '...the ways in which scientific research is implicated in the worst excesses of colonialism remains a powerful remembered history for many of the world's colonised peoples'9.
In this climate, the process of any research enterprise can be as important as the outcomes, in terms of building firm foundations for future collaboration and projects. Thus, there is considerable benefit for health workers, who generally have strong community credentials and high profile roles within the health workforce, to be more actively involved in developing, delivering and evaluating health programs. However, it is incumbent that health workers have appropriate training and skills for such roles. When, in 2002, we began the consultations and development process that has resulted in the development of the RCB framework outlined here, we found little evidence of RCB training within institutionally-based health worker education programs, which were rightly focused on providing core healthcare-related knowledge and skills. The apparent lack of culturally appropriate training in research and evaluation methodology, delivered on-site, suggested that health workers were unlikely to be well equipped to fulfil this role. However, the development of national programs such as the Primary Health Care Research, Evaluation and Development (PHCRED) program, which focuses on increasing research capacity across primary health care, presented an opportunity to assist in developing capacity building initiatives specific to the needs of Aboriginal and Torres Strait Islander healthcare organisations and the communities they serve.
Early opportunities and consultation
In 2001, the PHCRED program at James Cook University, Queensland, Australia (PHCRED-JCU), set as its primary goal enhancing access to research training and resources for primary healthcare workers. Because north Queensland has a sizeable Aboriginal and Torres Strait Islander population, it was appropriate that specific consideration be given to RCB for health workers. In 2002, PHCRED-JCU undertook some preliminary investigations into the research capacity of, and RCB opportunities for health workers, including looking for pre-existing dedicated RCB courses. At the time, the focus was on north Queensland, and consultations with various stakeholders raised concerns about limited research training opportunities specifically designed by, and for, Aboriginal and Torres Strait Islander health workers and services in north Queensland. The need for RCB to occur within health workers' workplace and community, as opposed to institutionally-based training, was also raised. Similar issues were raised and agreed at a national meeting of PHCRED organisations in 2002. This preliminary information was used to plan and provide a focus for a Queensland Aboriginal and Torres Strait Islander Research Forum hosted by PHCRED-JCU in 2003.
The 2003 Research Forum was held in Townsville, Queensland, Australia, with stakeholders from Queensland Aboriginal and Torres Strait Islander community controlled health organisations, the Queensland Aboriginal and Islander Health Forum (QAIHF), the Aboriginal and Torres Strait Islander Commission (ATSIC), Indigenous Health Unit, JCU, Aboriginal and Torres Strait Islander services representatives and PHCRED-JCU. During the consultation process, participants discussed perceptions of research and evaluation, and the role of these in service delivery for health workers. A need was identified to support health workers and organizations in acquiring research and evaluation skills to support culturally appropriate and effective health care provision. It was agreed that this would help address current inconsistencies and perceived inequalities in Aboriginal and Torres Strait Islander health initiatives that were considered by participants to be generally ad hoc. Participants felt that an holistic perspective needed to be adopted because this was considered appropriate to Aboriginal and Torres Strait Islander healthcare delivery and control in primary healthcare services. It therefore appeared that a program aimed at building research capacity in Aboriginal and Torres Strait Islander services, specifically health workers and communities, might best be enacted as an accredited course, which would consist of a series of connected 'topical' modules. To further complement accredited coursework, it was proposed that individualised workshops could be held for those health workers who did not wish to undertake formal training towards another qualification, but did require up-skilling in research and evaluation strategies with practical application in their workplace. The remainder of this article outlines the issues considered to be essential to RCB for health workers and their communities and which will likely enhance a proactive service delivery model using culturally appropriate research methods. We define 'proactive' as leading, or knowledgeably participating, in the planning and delivery of health services.
Research capacity building for health workers and their communities
Guiding principles in the development of the framework
Several core 'principles' underpinned the development of the framework. First, it is well documented that the health status of Aboriginal and Torres Strait Islander people is far below that of the non-Aboriginal and Torres Strait Islander population, and therefore is at the forefront of the national focus on health and service delivery initiatives10,11. Second, active Aboriginal and Torres Strait Islander community involvement in health service development, monitoring and improvement is considered essential1-4. Third, Aboriginal and Torres Strait Islander communities should be involved in on-going professional development of health workers in the community context. Fourth, community-based training is most likely to focus on specific learning and skills appropriate to community needs and expectations.
To ensure that we were not 're-inventing the wheel', we undertook a preliminary investigation of RCB opportunities for health workers in 2002 which included searching for dedicated RCB courses, but none of the latter were found. Participants at the 2002 National PHCRED and 2003 PHCRED-JCU Research Workshops reiterated the paucity of formal research training specifically developed for health workers within community-based services and settings.
During the period 2003-2005, the framework outlined here was reviewed and refined through meetings with Aboriginal and Torres Strait Islander community representatives from various areas across Australia. The overall aim of the framework is to supplement current education and training resources for health workers with research training modules that can be tailored for individual needs and undertaken in health workers' own communities. The underlying principle of the framework is to ensure that best practices for Aboriginal and Torres Strait Islander communities and services are established and/or maintained, by using culturally appropriate service delivery, monitoring and evaluation methods. The framework enables RCB at both the individual (health worker) and community levels because it focuses on developing skills and knowledge in research and evaluation strategies informed by collaborative consultation and participatory methods. This approach is thus intended as a two-way education process, with the community as an active player.
Because Aboriginal and Torres Strait Islander health services and, specifically, the roles and practices of health workers, involve the provision of direct care to individuals, family and the community at large, a community-based learning environment not only encompasses a holistic approach (individual, family, community) to the physical, emotional and social aspects of health, but can also ensure that RCB can be tailored specifically to the needs of the community. By being immediately and obviously of benefit to the community, particularly if the community has been actively involved in the development and implementation of the research/evaluation activity, it is possible that some of the historical concerns about research may be alleviated.
Every Aboriginal and Torres Strait Islander community is different, and community members expect that their community will be treated as unique in its own country. Throughout the development of the framework, the principles of conducting research ethically within each community have been paramount. These principles emphasize:
...the right to self-determination and to the management and preservation of their culture and heritage. At all stages, research with and about Aboriginal and Torres Strait Islander people must be based on a purposeful and mutually beneficial relationship between researchers and Aboriginal and Torres Strait Islander people.12
The research capacity building framework
The framework outlined here (Fig 1), is aimed at integrating RCB into education, skills development and practice for Aboriginal and Torres Strait Islander health workers, their communities and their health services. It is designed to be transferable across health service type, location and cultural protocols. Figure 1 displays the core elements required to improve services and their delivery, each of which constitutes a nominal 'module' within the RCB framework. Some detail about what each element (module) encompasses is outlined below. For efficiency of description, the framework has been depicted as six apparently discrete entities; however, in practice a more eclectic approach to the various issues could be taken in order to best meet the needs of individual health workers and communities. The diagram also demonstrates the cyclical nature of RCB, as a continual review is required of community primary healthcare needs and priorities and the role of service provision in meeting these effectively. Finally, the framework was developed with the intention that it be conducted in the community setting, thus potentially enabling more health workers to participate and gain understanding and skills of direct relevance to their community, through direct application to existing requirements. It is envisaged that, should a health worker seek a formal Vocational Education and Training (VET) award, each module would take approximately one academic semester to complete on a part-time, self-directed (distance-learning) basis. This VET-accredited course framework would draw upon suitable subjects from other VET and university courses to complement those specifically developed here. The underlying premise upon which this framework has been developed is that all coursework needs to be tailored to meet the specific learning requirements of each health worker enrolled in the program. It should be noted that some existing coursework programs are not amenable to 'tailoring' and therefore may not be able to be used in some settings.
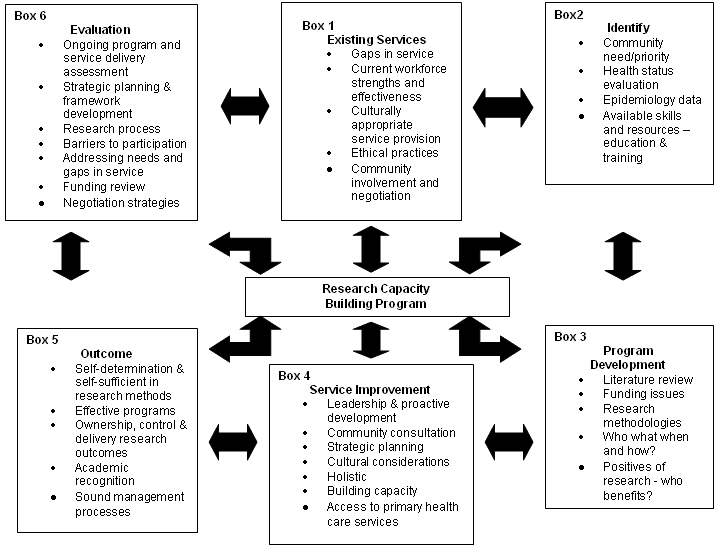
Figure 1: The research capacity building cycle - using culturally appropriate research methods to achieve a proactive service-delivery model. (Based on J Bailey, oral presentation, 2003).
Figure 1 illustrates the inter-relationships between individual RCB 'modules' (Boxes 1-6) and their application in defining best practice service delivery. Ideally, if a health worker intended to undertake the entire RCB program, they would most logically progress from Box 1 to Box 6. However, the diagram and checklists for each box enable a health worker to determine the most appropriate place to begin according to their existing knowledge and skills, and their specific need (eg establishment of an evaluation program for an existing service). Regardless of the module at which RCB training begins, the first step always is to detail community input and experiences of existing health services through a general introduction and 'scene setting' session. Additionally, although listed in Box 1, issues pertaining to ethical research practice would also be covered in the introductory session. For the purposes of explanation, we outline each module in numerical order from Box 1 to Box 6.
The first module (Box 1) focuses on developing an understanding of the key issues and processes involved in 'assessing' Existing Services, some of which are listed in the box. The module addresses the importance and means of identifying current strengths and shortfalls in existing services with specific regard to each community's needs and expectations. Additionally, participants learn a range of options for changing service delivery practices and directions so as to ensure that revisions are culturally appropriate and meet the community's needs. Issues covered include service delivery skills and knowledge, information collection, means of dealing with information shortfalls, information analysis and interpretation, and the need to focus on future service development. The importance of implementing continuous improvement processes and best practice management approaches is also covered.
The second module introduces a range of methods and measures for Identifying Need (Box 2) at the individual, community and service levels. A mixture of needs assessment processes is introduced, but with an emphasis on cultural appropriateness, acceptability and accessibility. Participants would work their way through 'hands on' exercises based on their own communities and experiences. These exercises include information gathering, interpreting and disseminating results, as well as the potential for joint ventures and/or strategic alliances.
The third module (Box 3) addresses issues that are important in Program Development, some of which are listed in the box. The module focuses on the 'what is' of program development. The importance of active community participation and its role in setting the 'ground rules' for research (both focus and activities) is emphasised. Participants will learn the utility of developing a research checklist specific to their 'research' needs and tailored to match their community's needs, resources and expectations. The purpose and benefit of the checklist is that it explicitly covers the issues of importance to a community that intending researchers need to know about and also need to complete before research activities begin. It is a form of non-legal 'contract' between researchers and communities, the purpose of which is to prevent subsequent distress or dispute. Although, the focus here is on research-related activities, the checklist process could just as easily be used for service providers new to a community.
Figure 2 is an example checklist that identifies appropriate methods for: preventing poor consultation; lack of communication; and infringement of values arising from cross-cultural insensitivity in services and research. By completing the checklist, researchers are acknowledging the community's specific concerns and requirements. Another element of the checklist is that it ensures that local research capacity needs are identified and tailored to each community. In other words, the research activity also builds research capacity in local people (health workers in this case) through their active participation in all elements of the process. This leads, then, to continuous improvement of culturally appropriate and ethical practices used to develop skills and strategies to promote the rights, needs and interests of the community.

Figure 2: Example of a research checklist to ensure culturally appropriate communication and recognition of community sensitivities.
The fourth module continues on from program development by considering issues related to Service Improvement, some examples of which are listed in Box 4. The module covers the concept of the continuous improvement cycle and the consequent need to identify areas within the health infrastructure and service development that are working well and not so well. Strategies needed to enhance competency and skills in research and training processes are also covered. Additionally, the module provides health provider organisations with a tool to meet growing health demands, education, training and delivery of culturally appropriate services to the community.
The next module addresses Outcomes and measures that will impact on community and service provision, some examples of which are listed in Box 5. The focus is to achieve the most successful and sustainable outcomes, by teaching and applying problem-solving strategies in purposeful ways, both in situations where the problem and the solution are clearly evident, and in situations that require creative thinking and approaches. This process is to ensure that short-term efficiency targets continue to be consistent with, and contribute to, long-term effective objectives.
The final module addresses Evaluation Methods, as outlined in Box 6 and includes appropriate collection and interpretation of data and applying findings to service delivery. The importance of subsequent monitoring and upgrading of organisations' strategic management of information and data, as part of the continuous cycle of improvement, are highlighted. Additionally, the role these play in justifying funding applications is emphasised. This is vital in order to facilitate essential information sharing and use between Aboriginal and Torres Strait Islander communities and services for the total wellbeing of all.
Discussion and conclusions
Active participation by Aboriginal and Torres Strait Islander communities is fundamental for effective research practices to be established and outcomes to be achieved. Community input will ensure that current guidelines and protocols meet the community's expectations and are incorporated into research practice, in line with NHMRC guidelines. The framework outlined here, which has received VET accreditation, provides the basis for RCB within Aboriginal and Torres Islander communities, with a particular focus on health workers. The aim is to provide Aboriginal and Torres Strait Islander people with a working knowledge of research ethics and methods so that they can both assist and monitor the development of culturally appropriate research activities that will lead to provision of the highest quality services back to the community. The framework sets out the core principles and elements of RCB, but is designed to be flexible - in terms of topics, aims and delivery - so that training programs can be assembled to meet the specific needs of health workers and their communities. The VET-accredited outline includes a number of potential course-work subjects from which to assemble a tailored training program.
In terms of the effectiveness of service needs and delivery, a wide range of issues are of relevance to Aboriginal and Torres Strait Islander health, many of which lie outside the direct responsibility of the clinical health sector. These include cultural, social, historical and economic issues, as well as those relating to the physical environment. The RCB framework outlined here presents a practical approach to enable Aboriginal and Torres Strait Islander health workers to be more proactive, self-reliant and self-sufficient within their community and health care settings. Additional benefits include eligibility for promotion, transfer, and cross-sectoral multi-skilling to most effectively assist their communities. This framework aims to empower Aboriginal and Torres Strait Islander people to: carry out their own research within their own service/community; involve themselves in the analysis and critiques of research to address and determine the outcomes of their social, cultural, economic and political issues; and fulfil their self-determination and self-management destinies.
Improvement in health outcomes for Aboriginal and Torres Strait Islander people can only be achieved when the community and services are empowered to act on their own behalf. The outcomes can be then used in the negotiation of service agreements between communities and health departments and mainstream services.
In summary, the aim is not to be scared of research. If it is in our hands and in our control, by people who we want to do the research with, it will make a difference. The next step is to test the RCB framework in the field.
Acknowledgements
This project was undertaken within the Department of Health and Ageing funded Primary Health Care Research Evaluation and Development (PHCRED) program at the Rural Health Research Unit at James Cook University (JCU), Queensland, Australia. The authors would like to extend their thanks and gratitude to those who have greatly assisted in and or contributed to the project: in particular the community reference group consisting of Elders, health personnel, academic consultants and stakeholders representing the Department of Health and Ageing, north Queensland Aboriginal and Torres Strait Islander community controlled health organisations, the Aboriginal and Torres Strait Islander Commission, Indigenous Health Unit JCU and Aboriginal and Torres Strait Islander services representatives and community members, PHCRED-JCU, Sue Latham for her dedication and her 'ultra laid back professionalism', as well as the team at the Rural Health Research Unit at JCU for their ongoing support. A very special thanks goes to Valerie Alberts (School of Medicine, JCU) and Jacinta Elston (Indigenous Health Unit, Faculty of Medicine, Health and Molecular Sciences, JCU) for their support.
References
1. National Health and Medical Research Council. Guidelines to applicants for capacity building grants in population health research: rounds 4 and 5. Canberra: NHMRC, 2006.
2. National Aboriginal Health Strategy Evaluation Committee. The National Aboriginal Health Strategy: An evaluation, Aboriginal and Torres Strait Islander Commission. Canberra: National Aboriginal Health Strategy Evaluation Committee, 1994.
3. National Health and Medical Research Council. National Statement on Ethical Conduct of Research Involving Aboriginal and Torres Strait Islander Peoples. Canberra: NHMRC, 1999.
4. VicHealth Koori Health Research and Community Development Unit. We don't like research ... but in Koori hands it could make a difference. Melbourne: VicHealth Koori Health Research and Community Development Unit, 2000.
5. Rigney IL. Internationalisation of an Indigenous anti-colonial cultural critique of research methodologies: a guide to Indigenist research methodology and its principles. In: Proceedings, Research and Development in Higher Education: Advancing International Perspectives. HERDSA Annual International conference; Adelaide, South Australia; 1997.
6. Holmes W, Stewart P, Garrow A, Anderson I, Thorpe L. Researching Aboriginal health: experience from a study of urban young people's health and well-being. Social Science and Medicine 2002; 54: 1267-1279.
7. Grove N, Brough M, Canuto C, Dobson A. Aboriginal and Torres Strait Islander health research and the conduct of longitudinal studies: issues for debate. Australian and New Zealand Journal of Public Health 2003; 27: 637-641.
8. Thomas DP. Reading doctors' writing. Race, politics and power in Indigenous health research 1870-1969. Canberra: Aboriginal Studies Press, 2004.
9. Smith LT. Decolonizing methodologies: research and Indigenous peoples. Dunedin: University of Otago Press, 2004.
10. Otim M. Aboriginal and Torres Strait Islander Health Economics and Policy Research. Discussion article no. 4. VicHealth Koori Health Research and Community Development Unit, 2001.
11. Australian Institute of Health and Welfare. Australia's Health 2002. AIHW: Canberra, 2003.
12. Australian Aboriginal and Torres Strait Islander Health InfoNet. Guidelines for Ethical Research in Aboriginal and Torres Strait Islander studies. Australia Institute for Aboriginal and Torres Strait Islander studies. (Online) 2000. Available: http://www.healthinfonet.ecu.edu.au/frames.htm (Accessed: 12 December 2006).
13. Bailey J, Alberts V. Ethics in cultural research practices within the university and Aboriginal and Torres Strait Islander communities: Nyinan-Binang - Indigenous Primary Health Research Group. HREC Bulletin, 15: 5-7. (Online) 2005. Available: http://www.nhmrc.gov.au/ethics/human/hrecs/reference/bulletin.htm (Accessed: 12 December 2006).
