Introduction
There is a widely acknowledged disparity between the health of Aboriginal and Torres Strait Islander people and non-Indigenous Australians, with a 15-20 year difference in life expectancy still existing for Indigenous Australians, and higher morbidity when measured using almost any indicator1. There are many historical, sociocultural, political and financial reasons for this disparity, which have been covered elsewhere and are outside the scope of this discussion2,3.
Aboriginal Community Controlled Health Services (ACCHS) have been set up across Australia (in settings from urban to remote) to provide culturally appropriate and accessible primary health care for Indigenous Australians. Although the nature and scope of these varies, the unifying factor is that of community control, being governed by a community-elected board of directors4. They largely provide team-based multidisciplinary care across a range of health areas, and Aboriginal Health Workers are important in care provision. Qualitative studies assessing the acceptability of this model of service delivery to Indigenous patients are lacking; however, attendance figures, satisfaction ratings and overseas experience suggest that they are responding appropriately to patient needs5-8.
Townsville Aboriginal and Islander Health Service (TAIHS) is a large ACCHS in a provincial city, which provides medical, social, dental and allied health services to approximately 10 000 patients, of whom 80% are Indigenous. Townsville ATSIC region has 16 875 Indigenous people (5.2% of population) of whom 70% are Aboriginal and 30% Torres Strait Islander9.
In 1992, Bridges-Webb, Britt and colleagues published their large study (widely known as the AMTS) assessing more than 110 000 consultations performed by 495 randomly selected Australian general practitioners in two one-week study periods 6 months apart10. This landmark study collected data about patient demographics, reason for encounter, problems managed, treatment and referrals, and has formed the basis for much subsequent analysis of consultations in the general practice setting.
In 1995, the development and collection of standardized information on primary health care encounter data was identified as a high priority health information issue. In response, the Australian Institute of Health and Welfare and the University of Sydney Family Medicine Research Unit have been collaborating on a national, ongoing survey of general practitioner activity, titled "Bettering the Evaluation and Care of Health" or BEACH11. These data are collected from a continuing rolling sample of general practitioners using a questionnaire developed from the one used in the original AMTS study. Data about problems managed and patient reasons for encounter are coded using ICPC-2PLUS (ICPC2PLUS; Family Medicine Research Unit, University of Sydney, NSW, Australia). This classification of terms has been developed and extended from the International Classification of Primary Care (Version 2), developed by the World Organisation of Family Doctors, which in turn is regarded as the international standard in classifying data for primary care. Recently, the Townsville arm of the BEACH Morbidity and Treatment study has also been completed, providing information about general practice consultations in the Townsville region using a similar kind of questionnaire12.
It is important to understand consultations in primary care with Indigenous people, and how these might differ from consultations with other Australians. The 2003 BEACH report added to our knowledge by comparing consultations involving Indigenous people (1374 encounters or 1.4%) and non-Indigenous people in mainstream general practice13. This report found that Indigenous patients were significantly younger than non-Indigenous patients and more likely to be seen in rural or remote areas, following the population distribution. The number of problems managed per encounter with Indigenous Australians was almost identical to that of non-Indigenous Australians (147.7 per 100 Indigenous encounters compared with 148.1 per 100 total encounters); however, there were some differences in the nature of the problems managed between the two groups13.
In general, little has been published studying consultations within a community-controlled health service, and comparing these with consultations within the wider arena of Australian general practice. In 1994, Thomas and colleagues adapted the questionnaire used in the AMTS study for use in a community controlled health service setting. They analysed consultations at Danila Dilba Aboriginal Community Controlled Health Service in Darwin, according to similar variables14. They found that, compared with Australian general practice, consultations at Danila Dilba were more complex, with more new patients, more young patients, more problems managed per consultation, more new problems, and more consultations leading to emergency hospital admissions. The balance of problems managed at Danila Dilba was also substantially different from that of Australian general practice, although they were only able to compare data with dated Australia-wide information15.
Thus, it seems there are two separate constructs worthy of consideration. Are differences between consultations in an ACCHS and mainstream general practice solely attributable to differences in the Indigenous and non-Indigenous populations, or are there inherent differences in the way care is provided within the ACCHS structure that have an impact on care provision?
The aim of this study was to characterize consultations at TAIHS in terms of patient demographics and the content and process of consultations, and compare them with relatively contemporaneous and geographically similar data from mainstream general practice and with data from a geographically distant provincial ACCHS.
Methods
We conducted a prospective questionnaire audit of consultations. Data were collected for two fortnightly periods in October 2000 and May 2001. Fortnightly collection periods were chosen, instead of the one-week periods used in the Danila Dilba study, to even out perceived variations in consultations performed from week to week based on fortnightly social security payments. Data were collected for all consultations performed in the medical section of TAIHS during the study period, including the maternal and child health section and the eye health section, but excluding other allied health and Saturday consultations. It was intended to also gather data for all outreach and home visits during the study periods; however, for logistical reasons this was incomplete.
The questionnaire was very similar to the one used by Thomas at Danila Dilba14. This questionnaire was, in turn, based on the one used to collect data in the AMTS study10; however, with changes made to reflect differences in consultation patterns in Indigenous primary health care when compared with mainstream general practice. The main changes made (also used for the TAIHS study) were an increase in the possible numbers of patient reasons for encounter (from three to six) and problems managed (from four to eight) that could be recorded. The questionnaire described consultations using the following variables: date of consultation; patient age; ethnicity and gender; postcode and whether or not they were new to the practice; where they were seen; the provider of the service (doctor, nurse, health worker etc); Medicare level of consultation; patient reasons for encounter; problems managed; treatment and medications given; investigations; admissions; follow-up; and referral.
New problems were defined as problems that had not previously been managed by any health worker, or new episodes of a recurrent condition. It was possible to record up to three providers for any patient consultation, reflecting the team approach used in ACCHS. As in the Danila Dilba and BEACH studies (but unlike the AMTS) it was possible to record both prescription and non-prescription drugs given.
Completion of questionnaires
Paper questionnaires were completed during and immediately following consultations by the provider/s of that consultation.
Coding
Answers to closed questions were pre-coded on the questionnaire. Where possible, missing variables were completed by reference to the clinical record. Answers to the open-ended questions (patient reasons for encounter [PRE], problems managed, and medications) were coded later using ICPC-2 PLUS Launchpad software. This is an updated and refined version of the ICPC classification used in the previous studies. Medications were coded using a classification based on the bimonthly MIMS drug index16.
Analysis
Data were entered into an Access database, cleaned and analysed using SPSS software (SPSS Inc, Chicago, IL, USA) for categorical and numerical variables; 95% confidence intervals of proportions and means were calculated17. Chi-square tests were used to compare categorical variables, and as normality assumptions were not met for many numerical variables, non-parametric tests such as the Mann-Whitney and Kruskal-Wallis tests were used to test associations between numerical and categorical variables, where appropriate. Missing values were excluded from the calculation of proportions. Where more than one response was possible per consultation, results were expressed as rates per 100 encounters to facilitate comparison with the other studies.
Danila Dilba (Darwin ACCHS) study
This study collected information on all consultations at Danila Dilba for two separate study weeks, 6 months apart in 1994 (a total of 583 consultations). The questionnaire was based on the AMTS with changes made as discussed above. Data were collected by a researcher from patient files at the end of the day, rather than by the treating doctor immediately after each consultation14,15.
Townsville BEACH study
This report used the standard BEACH methodology of having a large sample of GPs report on consultations with 100 consecutive patients, completing the standard paper report form after each consultation11. The Townsville report used results from 41 Townsville GPs reporting on 4100 encounters in 199812.
Reliability study
A reliability study was performed in late 2000. Ten per cent of records (n = 63) from the first data collection period were randomly selected and retrieved, and the questionnaires recoded (while blinded to the original coding, and each others' coding) by both the original coder (LG) and the principal researcher (SL) to check intraobserver and interobserver coding reliability. Intraobserver and interobserver reliability were both calculated by means of percentage agreement. Intraobserver reliability was generally high, with the lowest value being for PRE (84.6%). When this was modified to agreement at ICPC2 level (first three figures of ICPC2+ codes) this rose to 90.1% agreement. Similarly, interobserver reliability was very high (>95% agreement) for all except PRE and problems managed. These had agreement of 70.8% and 68.9% initially; however, when condensed to the grouping code of the first three digits (ICPC2 level), this rose to 82.0% and 87.7% respectively. It was felt that these grouping levels were the most clinically relevant, and so this level of reliability was considered acceptable.
Ethics approval
This project was approved by the elected Board of Management of the Townsville Aboriginal and Islander Health Service, and the Townsville Cross-Cultural Partnership group, as well as by the Research Evaluation and Ethics Committee of the Royal Australian College of General Practitioners. Patients were informed about the study by means of notices in the waiting room, flyers given to them at reception and by the treating doctor, and gave verbal consent to their consultation data being included.
Results
Comparison between two data collection periods
Overall data were collected for 638 consultations for the first data collection fortnight, and 575 consultations for the second data collection period. There was a significantly higher proportion of patients in the 25-44 year age bracket in the first data collection period (31.9%; 95%CI [28.3, 35.5]) compared with the second (24.7%; 95%CI [21.2, 28.2]); however, in all other ways the groups were statistically similar (table available on request).
Patient demographics
At TAIHS significantly more male patients (45.9%; 95%CI [43.1, 48.7] compared with 41.0%; 95%CI [39.5, 42.5]), significantly more children in all age groups less than 15 (27.9%; 95%CI [25.4, 30.4] compared with 15.7%; 95%CI [14.6, 16.8]), and significantly fewer people older than 65 years (6.6%; 95%CI [5.2, 8.0] compared with 18.3%; 95%CI [17.1, 19.5]) were seen when compared with mainstream Townsville general practice, and similar proportions to the Darwin ACCHS (Fig 1).
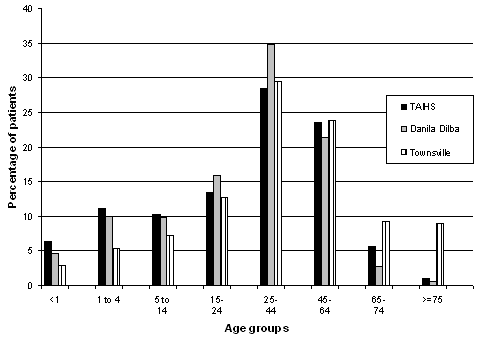
Figure 1: Comparison of age of patients among sites. TAIHS, Townsville Aboriginal and Islander Health Service.
Consultations involving an Aboriginal patient were 59.4%, and 18.8% involved a Torres Strait Islander patient, and 8.4% involved a patient who identified as Aboriginal and Torres Strait Islander. Smaller numbers were of South Sea Islander origin (1.3%), and other ethnicities (mostly Caucasian) 12.1%. There were 44 consultations where ethnicity was not recorded. Ethnicity was not reported for Danila Dilba, but the Townsville BEACH survey reported 2.02 per 100 consultations involved Indigenous patients12.
Location of consultations and provider
Consultations undertaken at the general TAIHS clinic were 771/1213 (63.6%), and 367 (30.3%) at the maternal and child health clinic, 18 (1.5%) at the diabetes clinic, 49 (4.0%) were outreach visits and only 8 (0.7%) were home visits. This compares with 18.6% of Danila Dilba consultations being home visits (after excluding nursing home and hostel visits). The Townsville BEACH study found a home visit rate of 1.9% (and 0.9% for nursing home visits.)
Health workers saw the patient at TAIHS in 224/1213 (18.5%) of consultations, nurses (two out of four Indigenous) participated in 513 (42.3%) of consultations, a medical officer saw the patient in 1070 (88.2%) of consultations and allied health providers were involved in 93 (7.7%). While 644/1213 (53.1%) of consultations involved two providers, 22 (1.8%) involved 3 providers.
The Danila Dilba study found that 42.6% of their consultations involved an Aboriginal health worker only, and a health worker and a doctor managed 53.5%; only 3.9% were managed by a doctor alone without input from a health worker. The Townsville BEACH survey did not collect information about providers of care other than GPs; however, no Aboriginal health workers are employed in private general practice in Townsville.
Medicare level
Of the 789 consultations billed to Medicare by vocationally registered doctors, 558 (70.7%) were standard consultations, 179 (22.7%) long consultations, 11 (1.4%) were extended consultations. In the Townsville BEACH study 73.6% of consultations were standard, and 6.9% were long consultations.
Problems managed
In total, 648/1209 (53.6%) of consultations involved the management of one problem, 390 (32.3%) involved two problems, and some involved three, four or five. However three consultations involved the management of six or more problems. A total of 1994 problems managed were recorded, with a mean number of 1.65 problems managed per consultation (95% CI [1.60, 1.70].) There was no difference between the two data collection periods.
Danila Dilba recorded an average of 1.58 problems managed per consultation (95% CI [1.51, 1.65]), and the local BEACH study recorded 1.45 problems per consultation [1.37, 1.52].
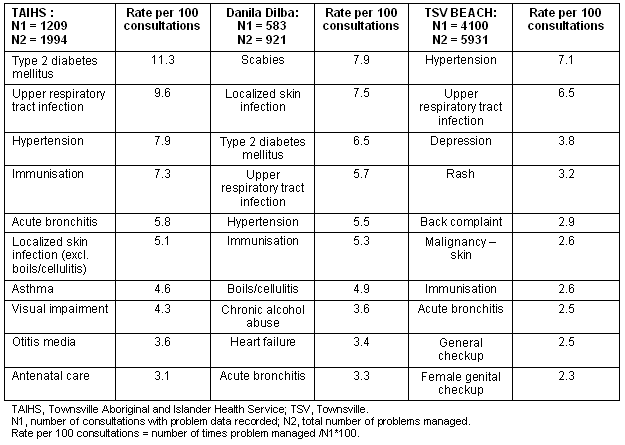
The most common problems managed at TAIHS included type 2 diabetes mellitus (11.3 times per 100 consultations), hypertension (7.3), upper respiratory tract infections (URTI; 9.6) and antenatal care (Table 1). Other problems commonly managed were hyperlipidaemia, medication reviews, depression, scabies and dermatophytoses, administrative reviews (social security forms, certificates), back pain and sleep problems. High levels of type 2 diabetes mellitus were also managed at Danila Dilba (6.5 per 100 consultations), although they most commonly managed scabies (7.9), and localized skin infections (7.5). TAIHS managed scabies, skin infections and alcohol abuse less commonly than Danila Dilba, but overall six of the top 10 problems managed were common to the two ACCHS. The top problems managed in Townsville mainstream general practice were hypertension (7.1), URTI (6.5) and depression.
Table 1: Top 10 problems managed as a rate per 100 consultations
Medications
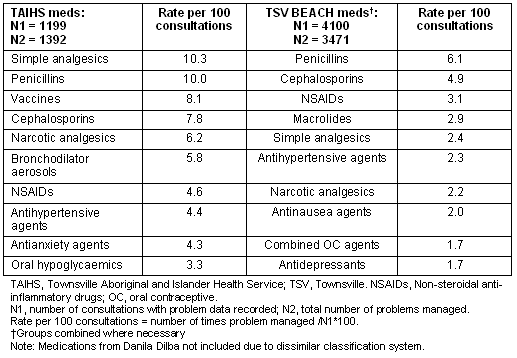
At least one medication was given for 66.6% of consultations (compared with 67.2% at Danila Dilba and 84.6% for BEACH). The average number of medications given per consultation was 1.16 (95% CI [1.09, 1.23]). Table 2 summarises medications given at a consultation. Simple analgesics were the most commonly prescribed medication at TAIHS (10.3 per 100 consultations). Antibiotics were next, with penicillins at 10.0% and cephalosporins at 7.8%. In mainstream general practice antibiotics were most commonly prescribed, occupying three out of four of the top spots. Data from Danila Dilba was classified using a different system, so it is not directly compared here.
Table 2: Medications prescribed or given at consultations as a rate per 100 consultations
Investigations
Overall at TAIHS one or more investigations were performed at 380/1171 or 31.3% of consultations. The majority of these were simple blood or urine tests. This compares with only 13.6% of Danila Dilba consultations, and 39.0% of local BEACH consultations.
Admissions and follow up
In total, 22/1213 consultations (1.8%) resulted in a hospital admission (emergency or elective), of which 11 (0.9%) were emergency department referrals. This is similar to the 1.5% of Danila Dilba consultations resulting in emergency admissions, and much more than the 0.1% of Townsville BEACH consultations.
Discussion
This study characterizes in some detail a large number of consultations at TAIHS. By using similar methodology to previous studies, and by achieving acceptable levels of reliability, we have been able to compare our work with Townsville general practice and Darwin ACCHS. More recently, data comparing consultations with Indigenous and non-Indigenous Australians in mainstream general practice reported from the first 5 years of the BEACH study have also become available and have been used for comparison13. Importantly, the development and continual refinement of well-validated coding systems for the content of general practice consultations, such as ICPC-2 PLUS, enables more accurate description and comparisons among services18.
Limitations and strengths of the study
There are some limitations to the data collected and analysis performed. When collecting data over a limited timeframe, there are always concerns about whether it is possible to generalise from this data to what happens over a broader time period. We elected to use two fortnightly data collection periods to minimise this problem, however it is possible that our sample is still not an accurate representation. We were dependent on the care provider completing the questionnaire at the time of the consultation. This resulted in a probable under-representation of home visits and outreach visits, due to logistical difficulties. The other question is about generalisability of our findings to other locations.
We were able to show good inter-coder and intra-coder reliability in our coding of clinical questionnaires. It is impossible to accurately validate the recording of PRE and problems managed by clinicians on the questionnaire. However, it was felt that immediate data collection by the service providers would provide more complete information than relying on information recorded in the clinical record, which varied according to treating practitioner, and may also under-represent the contribution made by health workers, nurses and allied health professionals to the consultation. Danila Dilba used chart review by the investigators at the end of each day to collect their data and their data was collected considerably earlier. The coding strategy used, the ICPC-2 PLUS system has been shown to have good face and consensual validity, and was developed to suit Australian general practice based on the internationally recognized International Classification of Primary Care system18.
Differences in patient populations
Consultations at TAIHS differ demographically from those performed in mainstream general practice in the Townsville region, and much of this difference may be accounted for by differences in the demographic features of local Indigenous and non-Indigenous populations. For instance, in the 2001 census, 39% of the Australian Indigenous population was aged less than 15 years, compared with 20% of the non-Indigenous population, and only 3% of the Indigenous population was aged 65 years or older, compared with 13% of the non-Indigenous population19. Age-standardisation would remove age as a confounder in this analysis. This has not been done, because consultations became more complex in terms of numbers of problems managed with increasing age of the patient, and thus age-standardisation would most likely further accentuate the greater complexity of consultations with Indigenous patients. In addition there are methodological issues with age-standardizing data from multiple datasets.
Problems managed in consultations
Significantly more problems were managed per consultation at TAIHS when compared with Townsville general practice, and the numbers were similar to those from Danila Dilba. Types of problems managed differed among all three datasets. Different patterns of regional epidemiology could help to explain some of the difference between types of problems managed in Darwin and Townsville. For example, Torres Strait Islanders, who make up 30% of the Townsville Indigenous population, have the highest prevalence of diabetes in the country20,21.
However it is important to remember that many factors other than differences in disease prevalence may affect these figures - in particular differences in accessibility of services, help-seeking behaviour when unwell, cultural beliefs and choice of treatment regimens.
It is interesting to note that national data from the first five years of the BEACH survey involving mainstream general practitioners showed the same demographic differences with the younger age distribution of Indigenous Australians, but no difference in the numbers of problems managed per consultation between Indigenous and non-Indigenous patients13. This suggests several possibilities: patients who attend an ACCHS for their medical care could be sicker with more problems, patients may selectively attend private practice for some problems and ACCHS for other, or that ACCHS are particularly responsive to the range of health issues facing each patient and provide more comprehensive care. This requires further investigation using qualitative methodologies. The higher rate of emergency admissions from the two ACCHS suggest that the patient population may be sicker, as would be expected from statistics about Aboriginal health status22. High reported levels of satisfaction with the service provided by TAIHS some years ago support our assertion that primary health care provided in a well run ACCHS is both acceptable and comprehensive5.
Providers of health care
Aboriginal and Torres Strait Islander health workers could appear to be relatively under-utilised at TAIHS when compared with Danila Dilba. There are differences in accreditation and training for AHWs between Queensland and the Northern Territory, and differences in the blend of staff at each service could also play a role. For example, at TAIHS at the time of the survey there were fewer AHWs but two Indigenous registered nurses employed. It is widely acknowledged that health workers play an important clinical role in the interpretation and communication of health business, and their local community knowledge, language skills and health training make them invaluable members of the treating team23. It seems likely that Indigenous nurses could provide a similar 'cultural brokerage' role. Almost every consultation at TAIHS involved a health worker or a nurse seeing the patient at some stage; however, the vast majority involved a doctor as well, in contrast to Danila Dilba where 42.6% of consultations involved an AHW only. There are several potential reasons for this. First, patient expectation in the community is that they should be able to see a doctor with their health complaints in most cases, and second the operation of the Medicare system at the time demanded medical involvement, and did not reward consultations with non-medical professionals24. TAIHS receives block grant funding from the Commonwealth, but is also dependent on 'bulk-billing' rebates from Medicare to supplement its income. This effect of financial pressures was raised as a concern by Thomas15, because of its potential to undermine the work done by health workers. The impact of new enhanced primary care Medicare item numbers in rewarding team-based multidisciplinary care remains to be evaluated in the Indigenous primary health care setting (in urban, provincial and remote settings). A weakness of this study is the lack of a qualitative component assessing the cultural acceptability of patients' practice experience and preferences regarding care providers.
It may be important to rethink the role of the health worker, so that their expertise and skills are valued and utilised to full capacity25, while respecting the right of patients to obtain medical care from a doctor, as appropriate. This issue becomes even more important when considering some of the medical recruitment and retention issues in more rural and remote areas, and alternative models of acceptable service provision26.
Conclusions
This study reveals demographic differences and greater complexity of consultations at TAIHS when compared with local general practice and national general practice, probably reflecting the greater illness and health needs of the ATSI patient population. TAIHS has some similarities with another ACCHS in northern Australia, and both appear to provide care differently when compared with mainstream general practice. The greater number of problems managed per consultation in ACCHS compared with Indigenous patients in mainstream general practice, supports the assertion that ACCHS fill an important role in the health system by providing care for their largely Indigenous patients with complex care needs. Further study is required to better understand the contribution to quality of service made by the ACCHS sector.
These findings have financial and organizational implications for ACCHS in other areas of the country and for other providers of primary health care for Indigenous Australians. Further work remains in dissecting the differences in primary health care provided to Indigenous people within the mainstream general practice setting and the ACCHS sector in different parts of the country.
Acknowledgements
Thanks must be extended to all the clinical and reception staff at Townsville Aboriginal and Islander Health Service (TAIHS), whose cooperation was essential in the collection of data used in this study. Thanks also to the Registrar Scholarship and Research Fund of the Royal Australian College of General Practitioners for funding the study, and the Board of Management of TAIHS and the Townsville Cross-cultural partnership group for their support. Thanks to Dr David Thomas of Danila Dilba (Darwin Aboriginal Community Controlled Health Service) and Professor Helena Britt at the Family Medicine Research Unit for advice. Thanks to Professor Richard Hays for comments on the manuscript.
References
1. Australian Bureau of Statistics. National Aboriginal and Islander Survey: Detailed Findings. Canberra: Australian Bureau of Statistics, 1994.
2. Miller P, Torzillo P. Health, an indigenous right: a review of Aboriginal health in Australia. Australian Journal of Medical Science 1996; 17: 3-11.
3. Ring I, Elston J. Health, history and reconciliation. Australian and New Zealand Journal of Public Health 1999; 23: 228-231.
4. National Aboriginal Community Controlled Health Organisation. (Online) no date. http://www.naccho.org.au (Accessed 16 May 2006).
5. Speare R, Kelly KA. Health needs of Aboriginals and Islanders in the Townsville region: the role of black medical services. Townsville: Anton Breinl Centre, James Cook University, 1991.
6. Ring IT, Firman D. Reducing indigenous mortality in Australia: lessons from other countries. Medical Journal of Australia 1998; 169: 528-533.
7. Shannon C, Carson A, Atkinson RC. Perspectives on Aboriginal community controlled health services: The manager. Medical Journal of Australia 2006; 184: 530-531.
8. Panaretto KS, Lee H, Mitchell M, Larkins SL, Manessis V, Buettner PG et al. Impact of a collaborative shared antenatal care program for urban Indigenous women: a prospective cohort study. Medical Journal of Australia 2005; 182: 514-519.
9. Australian Bureau of Statistics. Population Distribution, Indigenous Australians. AusStats 4705.0. 2001 Census. Canberra: Australian Bureau of Statistics, 2002.
10. Bridges-Webb C, Britt H, Miles D, Neary S, Charles J and Traynor V. Morbidity and treatment in general practice in Australia 1990-1991. Medical Journal of Australia 1992; 157 (Suppl.): S1-S56.
11. Britt H, Sayer GP, Miller GC, Charles J, Scahill S, Horn F, et al. BEACH: Bettering the evaluation and care of health: A study of general practice activity. Six month interim report. (General Practice Series no. 1; Report No.: AIHW cat. no. GEP 1). Canberra: Australian Institute of Health and Welfare, 1999.
12. Townsville Division of General Practice, Family Medicine Research Unit University of Sydney. Divisional BEACH report. Sydney, NSW: University of Sydney,1999.
13. Britt H, Miller GC, Knox S, Charles J, Valenti L, Henderson J et al. General practice activity in Australia 2002-2003. AIHW Cat. No. GEP 14. Canberra: Australian Institute of Health and Welfare, 2003.
14. Thomas DP. Clinical consultations at an Aboriginal community controlled health service: how are they different to consultations with Australian general practice? Newcastle: University of Newcastle, 1995.
15. Thomas DP, Heller RF, Hunt JM. Clinical consultations in an Aboriginal community-controlled health service: a comparison with general practice. Australian and New Zealand Journal of Public Health 1998; 22: 86-91.
16. MIMS. MIMS Bimonthly Index. October-November 1999 edn. Sydney: MIMS, 1999.
17. Bland M. An Introduction to Medical Statistics. Oxford: Oxford University Press, 1987.
18. Britt H. A new coding system for computerised clinical systems in primary care - ICPC-2 PLUS. Australian Family Physician 1997; 26: S79-S82.
19. Australian Bureau of Statistics. Year Book Australia, 2004. Canberra: Australian Bureau of Statistics, 2004.
20. McDermott R, Schmidt B, Sinha A, Mills P. Improving diabetes care in the primary healthcare setting: a randomized cluster trial in remote Indigenous communities. Medical Journal of Australia 2001; 174: 497-502.
21. De Courten M, Hodge A, Docose G, King I, Vickery J, Zimmet P. Review of the epidemiology, aetiology, pathogenesis and preventability of diabetes in Aboriginal and Torres Strait Islander populations. Canberra: Commonwealth of Australia, AGPS, 1998.
22. Thomson N. A review of Aboriginal health status. In: J Reid, P Trompf (Eds). The health of Aboriginal Australia. Sydney: HBJ, 1991; 37-79.
23. Trudgen R. Why warriors lie down and die. Darwin: Aboriginal Resource and Development Services Inc, 2000.
24. Mayers NR, Couzos S. Towards health equity through an adult health check for Aboriginal and Torres Strait Islander people. Medical Journal of Australia 2004; 181: 531-532.
25. Mitchell M, Hussey LM. Perspectives on Aboriginal community controlled health services: The Aboriginal health worker. Medical Journal of Australia 2006; 184: 529-530.
26. Smith JD. Australia's Rural and Remote Health. Melbourne: Tertiary Press, 2004.
Abstract
Introduction:
Despite the widely acknowledged health disparities between Indigenous and non-Indigenous Australians, little is known about consultations in primary care with Indigenous people. In particular, the nature of consultations in the Aboriginal Community Controlled Health Service (ACCHS) sector has been rarely studied. Data collection about consultations in primary care has been steadily improving, with good quality data now available on an ongoing basis about patient demographics, risk factors and consultation content in private general practice. This study aimed to characterise consultations at Townsville Aboriginal and Islander Health Service (TAIHS) in terms of patient demographics and consultation content. These could then be compared with existing datasets for local consultations in mainstream general practice and from a geographically distant ACCHS.Methods: We conducted a prospective questionnaire audit of all consultations at Townsville Aboriginal and Islander Health Service (TAIHS) over two fortnights, 6 months apart in 2000 and 2001. The questionnaire was adapted from one used in previous general practice surveys, and was completed by the treating clinician at the end of each consultation. The questionnaire described consultations using the following variables: date of consultation; patient age; ethnicity and gender; postcode and whether or not they were new to the practice; where they were seen; the provider of the service (doctor, nurse, health worker etc); Medicare level of consultation; patient reasons for encounter; problems managed; treatment and medications given; investigations; admissions; follow up; and referral. Proportions with 95% confidence intervals were calculated to facilitate comparisons with other datasets. Comparison was made with previously reported data from mainstream Townsville general practice (via the local BEACH study report) and from Darwin ACCHS (Danila Dilba).
Results: Of 1211 consultations studied, 1994 problems managed were recorded. TAIHS patients had a significantly younger age distribution than patients in mainstream general practice (as did patients at Danila Dilba). TAIHS consultations involved the management of more problems (1.65 problems per consultation; 95%CI [1.60, 1.70]), when compared with mainstream general practice (Townsville BEACH study 1.45 problems per consultation [1.37, 1.52]; 1.48 for Indigenous patients). Danila Dilba recorded an average of 1.58 problems managed per consultation (95% CI [1.51, 1.65]). The most frequently managed problems differed between all three datasets, and at TAIHS the most common problems managed were type 2 diabetes mellitus (11.3 times per 100 consultations), upper respiratory tract infections (9.6) and hypertension (7.9). Aboriginal Health Workers (AHW) saw the patient at TAIHS in 224/1213 (18.5%) of consultations, nurses (two Indigenous) participated in 513 (42.3%) of consultations, and a (non-Indigenous) medical officer saw the patient in 1070 (88.2%) of consultations. The Danila Dilba study found that 42.6% of their consultations involved an Aboriginal health worker only, and a health worker and a doctor managed 53.5%; only 3.9% were managed by a doctor alone without input from a health worker.
Conclusions: The greater number of problems managed per consultation in ACCHS, compared with Indigenous patients in mainstream general practice, supports the assertion that ACCHS fill an important role in the health system by providing care for their largely Indigenous patients with complex care needs. The Medicare system as it was structured at the time did not encourage involvement of Indigenous health workers in provision of primary medical care. It remains to be seen whether introduction of the new enhanced primary care Medicare numbers will assist in this process. These findings have implications for ACCHS in other areas of the country and for other providers of primary health care for Indigenous Australians.
Key words: Aboriginal community controlled health service, Aboriginal health worker, consultation, general practice, Indigenous health, primary health care.



