Introduction
Of the 16 professions on the Australian National Skill Shortage List 2004, 11 are in health1. Recently released figures indicate shortages in all states and territories of general and specialist registered nurses and most allied health specialists, as well as shortages or recruitment difficulties relating to enrolled nurses in most states/territories2. In Western Australia and New South Wales, enrolled nurse shortages are particularly evident in the aged care sector2. The shortage of health professionals nationally has resulted in pressures for vocational education and training (VET) workers to perform some of the tasks traditionally undertaken by professionals, with appropriate training and supervision.
The Department of Rural Health at the University of Tasmania, Tasmania, Australia, has undertaken a research project funded by the National Vocational Education and Training Research and Evaluation Program to locate, analyse and make accessible innovative models of health training and service delivery. The models that have been developed in response to a shortage of skill concentrate largely on VET trained workers in the health sector of the health and community services industries, including allied health workers. The study includes workers in mainstream health as well as special needs areas (Indigenous health, mental health services). Aged care workers are included because qualifications and training in this area appear to be increasingly forming a training and career pathway for health workers. The selected occupations are linked to VET qualifications which form part of the Australian Qualifications Framework, with a focus on certificates II to IV and diploma-level training. Examples of occupations for which VET qualifications apply are: Aboriginal and Torres Strait Islander health workers; enrolled nurses; personal care and nursing assistants, and special care workers (allied health assistants, residential care assistants, aged or disabled carers).
This study considers how the problem of health skills shortages requires a multi-faceted approach from government and industry, drawing on the recent Productivity Commission3 report on Australia's Health Workforce, and foreshadows the sorts of innovative solutions that have been developed to address local shortages of health professionals. These include up-skilling paraprofessionals, and adoption of a skill ecosystem approach4. Rural and remote areas in particular, have become home to a set of innovative service delivery models, such as multiskilling therapy assistants to work across several areas5, as well as a range of community-based solutions6. Collation and analysis of these innovative models will assist policy makers and practitioners to select appropriate models for various contexts. Findings from this research will appear in a report to be published by the National Centre for Vocational Education Research.
Brief overview of shortages in the health sector: statistics and models
According to the Australian Institute of Health and Wellbeing (AIHW) report7 in 2001, the largest occupational group in health was nursing workers (over half of those employed), and in community services occupations the largest group was aged/disabled carers.
There has been an adjustment of the mix of occupations in nursing toward lower paid occupations. Significantly for the VET sector which provides their training, the number of enrolled nurses decreased by 21% from 1996 to 20018. The national shortage of enrolled nurses is confirmed by the State Skills in Demand Lists2. At the same time, personal carers and nursing assistants, occupations that are lower paid than enrolled nurses, increased by 20%, apparently substituting for enrolled nurses or taking over some of the less skilled tasks of registered or enrolled nurses7. The Productivity Commission3 note that personal care workers now comprise the bulk of the workforce in the aged-care sector. Although there are skill shortages in the allied health area, specifically in relation to allied health professionals, statistics show that the number of therapy aides (also referred to as therapy assistants or allied health assistants) has almost doubled in the five-year period from 1996 to 20017.
The current structure of the national health and community services workforce has several characteristics that differentiate it from other industries' labour forces. In brief, these include the following:
High female proportion in the health workforce: Women make up 78% of the workforce, the highest proportion of all industries8. They are more likely than males to be in lower income occupations7 and to work part time. The high female representation in the health and community services workforce may affect supply of health professionals to accommodate the increasing demand of health and community services due to gender stereotyping, which discourages prospective male workers9.
Ageing health workforce: Australia has an ageing health workforce3. Within the health and community services labour force, 38%7 of workers are aged 45 years and over (Fig. 1). The fastest ageing occupations (those with the largest increases in the proportion of workers aged 45 years and over) are nurse managers, aged/disabled carers and personal care assistants. A likely decline in the number of health and community services workers as older workers retire, and an increase in the number of older people in the population, places pressure on the capacity of the health labour force. The aged-care sector is especially vulnerable to this pressure.
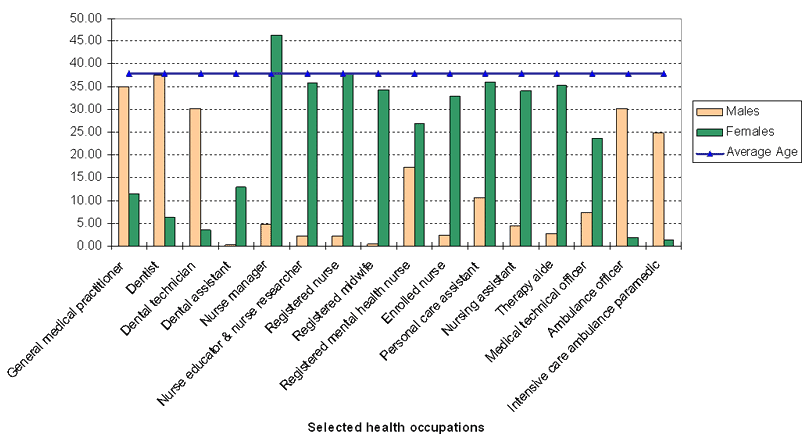
Figure 1: Employees aged 45 years and over in selected health occupations7,8.
Statistics indicate a low proportion of young people aged between 15 and 24 years (9.84%), in the health workforce7. As well, the Productivity Commission3 notes increasing difficulties in recruiting younger Indigenous people to the health workforce.
Geographical location of the health workforce: Access to a wide range of health and community services workers may be limited in rural and remote areas. This applies particularly to medical specialists, dentists, physiotherapists and other services relying on infrastructure and services of hospitals3.
This finding is supported by the Productivity Commission3, which expresses particular concern over the lack of access to health workers by Indigenous communities. While the majority of health workers work in capital cities (Fig 2), the situation is different for aged/disabled personal carers and enrolled nurses. For example, 151 per 100 000 population enrolled nurses are employed in other regions compared with 74 per 100 000 population in capital cities7. This suggests substitution of lower qualified workers for professionals may be taking place in rural and regional areas. When coupled with the decline in enrolled nurse numbers and the ageing of the workforce noted earlier, this also suggests a need for investment in VET sector training in rural and regional Australia.
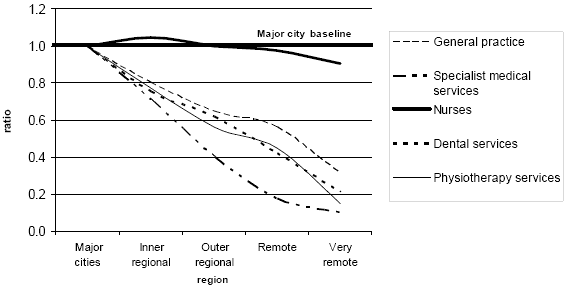
Figure 2: Practitioner to population ratios10.
Persistent job vacancies, hours worked, poor retention and pay rates: The health and community services industry has experienced ongoing recruitment difficulties. Vacancy levels have increased over the last 5 years11.
Poor retention in some health occupations can be a significant factor causing workforce shortages, compounding the shortages related to the low full-time participation rate. At any point in time there will be just over half of the eligible nursing workforce active in nursing, either full or part time. In the area of mental health, extremely high turnover rates have been noted12. Poor retention among nurses may be due to unsatisfactory working hours, relatively low remuneration, poor working conditions, structural constraints and highly specialised skills needs12.
Education and training levels: According to a report from the Department of Science, Education and Training (DEST)13, in May 2000, 57% of those working as enrolled nurses, personal care/nursing assistants and aged/disabled person carers had a basic vocational qualification, 24% had attained a diploma and 12% had no post-school qualification (Fig 3). Half of those without a post-school qualification were undertaking further studies. A majority of personal care and nursing assistants and aged/disabled person carers had no post-school qualifications.
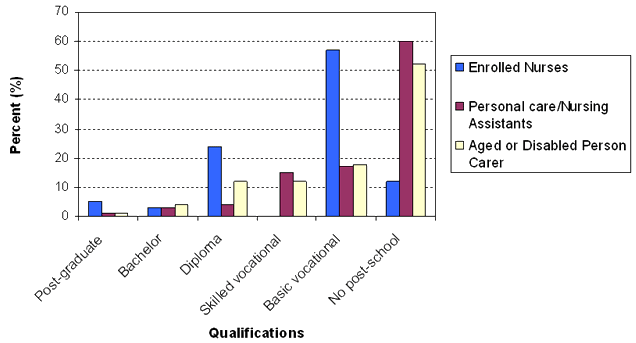
Figure 3: Qualifications profile of enrolled nurses, personal care/nursing assistants and aged/disabled person carers, Australia, 200013. Note: the post-graduate category includes higher degrees and post-graduate diplomas; the diploma includes undergraduate diplomas and associate diplomas. The percentages may not add up to 100 because of rounding errors14.
Models that address skill shortages: Clearly there is a place for innovative service delivery and training models to help reduce health skill shortages. These same issues are also being addressed internationally15,16. Such models are likely to focus on development of training and accreditation for new industry areas, and increasing employee retention and job satisfaction through appropriate professional development. These may be supplemented by creative recruitment and outreach strategies for potential employees, and other support services16.
Methods
A national project reference group of six was established. These people acted as representatives of various stakeholder groups, including the Community Services and Health Industry Skills Council, Australian Rural Health Education Network, health professional bodies, government health departments and health consumer groups. The reference group members acted as two-way communication channels with their professional communities at key stages of the project. Available statistics and literature on the structure of the national health workforce and perceived skill shortages in health were analysed.
With the assistance of nominations from the project reference group and their stakeholder communities, we identified over 70 models to address skills shortages, of which the majority were Australian, and which we broadly categorised as to type and level. Most of the identified models were in rural/regional areas where skill shortage and the need for innovative, partnership-based solutions were the greatest.
The researchers then selected and reviewed a mix of 50 innovative service delivery models and training solutions from Australia and international examples that could be transposed to the Australian context. 'Innovative' models are defined as models which introduce something new into the context and/or make a change in something established17. Selected models were judged to be effective (or likely to be effective) in reducing a skill shortage from the level that would otherwise have occurred. This judgement was either made by the nominator, or was drawn from written material, in some cases formal evaluations, in other cases recorded assertions of those involved in the models.
The 50 models were analysed by the researchers. Consistent with qualitative18 and inductive19 methodology, the models were analysed for commonalities or themes, and broad categories and spatial levels were identified (see later section on 'Synthesis of model types and levels'). These themes, categories and spatial levels were validated through feedback from the reference group.
Six were selected for writing up as case studies. These cover a diversity of situations and represent a range of innovative solutions. Key personnel involved in establishing and/or running the innovative models were interviewed by phone and asked to explain the process through which their model was established. Permission to name organisations was obtained in line with ethics approval. Readers of this article may contact the authors for more information on the models and case studies, which are not described in this article because of space restrictions.
Results
Two overarching themes emerge from the literature and from the analysis of models: use of a partnership approach to address skill shortages, and targeting specific groups for training and employment in health and community services occupations.
Partnership approaches
Partnership approaches vary from complex multi-sector partnerships with many partners to simpler arrangements between two organisations, usually a training provider and an employer. A skill ecosystem is an example of a complex partnership, in which a range of strategies are identified and implemented to improve productivity and better use of limited resources by facilitating greater collaboration. These strategies include, but are not restricted to, training solutions.
At a national level the partnership approach is being promoted through the Australian National Training Authority National Skill Ecosystem project4. Of relevance to the health industry is the demonstration project currently being undertaken in New South Wales by the Community Services and Health Industry Skills Council and Central Coast Health-Mental Health Services4. Strategies include strengthening the role of the Central Coast Consultative Committee (an existing structure with the capacity to enhance collaboration among organisations and facilitate the development of inter-agency regional plan); a professional development program that facilitates workplace learning opportunities in a range of generic and specific competencies; and facilitation of a structure for agency collaboration.
Another application of the skill ecosystem approach is the Queensland aged care skills formation strategy20,21. This is a state government initiative to address labour shortages in the aged-care sector, where government, industry and Registered Training Organisations (RTO) work together to identify reasons for labour shortages and develop strategies to address them. Strategies are developed in relation to education and training, workforce management, organisation, job design, industry image and industrial relations. Examples include up-skilling and extending the scope of practice for enrolled nurses, negotiating changes to certificate III to meet current and projected industry skill needs, establishment of an aged care skills formation sub-strategy for Aboriginal and Torres Strait Islander aged care, and a supply chain project to address the shortage of allied health workers in aged care.
Both of the skill ecosystems approaches are characterised by a long-term, evidence-based, collaborative approach to identifying and addressing skill needs. In particular, the first phase of each was spent on developing partnership infrastructure, including building trust, developing networks, and accessing and analysing data on industry skill needs.
There are many other examples of effective local and regional solutions to skills shortages involving a health service employer and a RTO, and sometimes other stakeholders as appropriate, who work together to customise a training solution for a particular workplace or work context. The most effective of these models also ensure that the training is aligned with national VET training package competencies. At a state level, the Midwest Murchison Therapy Assistant project in Western Australia5 arose in response to an increased focus on the use of allied health assistants, particularly in rural and remote areas. It was funded by the Australian government under the Regional Health Services initiative. Specifically, this model focuses on standardising the training offered to therapy assistants, to ensure quality and consistency of therapy services delivered by therapy assistants, regardless of their location. The project was undertaken collaboratively by the Midwest Murchison region and the Combined Universities Centre for Rural Health. One outcome of the project is the development of a model of therapy assistant training that incorporates generic therapy assistant requirements but has the flexibility to accommodate local conditions and requirements as well. This has since been adopted on a statewide basis, and is delivered by videoconference to rural allied health practitioners. Other outcomes include the documentation of designated roles for therapists, therapy assistants and managers, as well as the creation of minimum standards of supervision for therapy assistants and a process for monitoring supervision practices.
Targeted recruitment, training and employment approaches
The second theme identified in the literature is targeting particular groups who may not otherwise have considered a career in health, including disadvantaged groups. Existing employees are targeted for up-skilling in other examples.
At a national level, there is a focus on addressing unemployment and underemployment issues amongst disadvantaged groups of potential employees, such as the disabled, those over 45 years of age, and those from culturally and linguistically diverse (CALD) backgrounds, by targeting them for training or retraining to fill skill shortages in the health and community services sector22. Other models target specific groups of potential workers such as school students (through VET in Schools or similar programs23), or workers from other professions looking for a 'sea change'24. A number of health service employers target their own workers, with a view to either providing entry level qualifications to previously unqualified workers, or up-skilling existing workers to undertake work of a higher level (eg medication-endorsed enrolled nurses). Most models contain elements of successful vocational education and training programs such as flexible workplace arrangements, remedial education, careers counselling, supportive employers, financial assistance, appropriate funding structures, and a career ladder.
These approaches are in line with developments in other countries. For example, the Community College of Denver has developed an innovative program to help address nursing shortages25. This program focuses on upskilling Certified Nursing Assistants and other entry-level (lowest skill level) workers to become Licensed Practical Nurses (LPN). One of the key features of the program is the 'Learning Lab', an intensive, 30 week remedial course designed to take students with low reading, writing, and maths skills up to the college entry level proficiency that is required for entry into the LPN course. On completion of the Learning Lab, students begin the LPN course. This program is a part-time, evening and weekend worksite program and participating employers provide classroom space, coordinate work schedules for participants, and help to pay for tuition. The course allows certified nursing assistants and other entry-level staff to advance from the lowest development skill level to college-level courses in half the time required in traditional development education, and creates opportunities for a career ladder for the students.
In terms of targeted training, cultural appropriateness is a key ingredient of successful models. This is exemplified in the array of models designed to attract Indigenous people to the health sector. Some models focus broadly on increasing the number of Indigenous people working in the health sector26,27. In Australia, the Mt Isa Rural Health School program addresses the problems that health services in the remote northwest of Queensland face in recruiting and retaining Indigenous health workers, despite the fact that 25% of the population is Indigenous. In response to this issue, the Mt Isa Centre for Rural and Remote Health developed articulated education programs designed to promote, recruit and facilitate participation by Indigenous people in the health workforce. Success of this initiative is illustrated by the increased numbers of Indigenous students successfully completing higher-level vocational qualifications (eight students in 2004 and nine students in 2005 completed Certificate IV in Primary Health Care, compared with no completions prior to 2004). There is also evidence that the program has been successful in supporting Indigenous students to continue with their studies (in 2005, one student was completing an enrolled nursing certificate and three progressed to bachelor of nursing studies)27. Other models focus on training and/or up-skilling Aboriginal health workers to meet the specific health needs of their communities (for example, focusing on providing much-needed skills to workers in the area of oral health28). In the past there has been inconsistency across the country regarding the training and scope of practice of Aboriginal health workers depending on their location, which it is expected the current Health Training Package review will address.
Synthesis of model types and levels
Three categories of models were identified according to the mix of activities involved: training only, job and/or workforce redesign and training, and holistic. The most common models are training only, followed by job and/or workforce redesign and training. Only approximately 10% of models are categorised as holistic.
Training only models: These approaches are often, but not always, short term, designed to address an identified skills shortage in a defined workplace or geographical area as quickly and efficiently as possible. There are two broad categories of training:
- Targeted training made up the vast majority of training models. Many of these are in the aged-care sector. Three sub-groups are identified as targeted for training:
- Youth (eg VET in Schools training for aged care at Illawarra TAFE, Shellharbour College, New South Wales)
- Special needs groups (Indigenous/ethnic, low SES, rural and remote, older workers) (eg training to increase the number of Indigenous people in the health workforce in remote north-west Queensland)
- Other (the existing health support workforce, those returning to the workforce after an absence) (eg RSL Veterans' Retirement Village model which trains existing workers and recruits new workers who had not previously considered a career in health)
- Youth (eg VET in Schools training for aged care at Illawarra TAFE, Shellharbour College, New South Wales)
- Non-targeted training (often using flexible delivery or offering recognition of prior learning) (eg Illawarra TAFE's online aged-care training).
Job and/or workforce redesign and training models: These approaches vary in nature, but extend beyond short-term training solutions to include other strategies to ensure worker retention beyond the training/retraining period. There are three main areas of redesign:
- Upskilling and providing career pathways for existing workers (eg Endorsed Enrolled Nurses in Haemodialysis Units that trained enrolled nurses to fill a gap caused by a shortage of registered nurses)
- Mobility across health roles in line with multi-disciplinary team-based approaches to care (eg the Midwest Murchison Therapy Assistant project)
- Creation of new health-worker roles (eg the Top End Aboriginal Mental Health Worker program to support rural medical general practitioners or GPs).
Holistic models: These approaches are overarching and medium to long-term in nature, targeted largely to addressing projected skill shortages in a sustainable manner. These approaches involve ongoing consultation with and ownership of the skill shortage problem by all relevant stakeholders (government, industry, RTO etc). They employ a range of solutions to skill shortages in addition to training. Other strategies include job (re)design, industry image, industrial relations, and the effects of skill shortages in the supply chain.
The Mental Health Skills Ecosystem in New South Wales and the Queensland Aged Care Skills Formation Strategy are good examples. They covered relatively large geographical regions and include multiple stakeholders. Although interim successes and achievements are important in maintaining the commitment of stakeholders, overall results of such approaches are not likely to be seen for several years.
Broadly, models operated at one of three spatial different levels. These levels are determined by who has access to the model and the sphere of influence. Most models are either local or regional in scope.
Local: Developed and delivered in one geographical location or heath service only by limited number of stakeholders (eg one RTO, one health-care provider). May have been adapted/licensed for delivery elsewhere. Many of the training-only models are local and are customised for a specific community.
Regional: Developed by multiple stakeholders (often including government health, education and/or training departments) for application across a number of sites/communities within a geographical region. More than half the job and/or workforce redesign and training models have a regional focus.
State/national focus: Developed by stakeholders (involving or commissioned by government health, education and/or training departments) for widespread application either across a state or nationally. Examples are the Queensland Aged Care Skills Formation Strategy and Health Careers in the Bush, a Queensland statewide initiative to encourage and support recruitment of rural and remote Indigenous and non-Indigenous students into health careers. More of these models are being planned in other states, such as South Australia. The majority of holistic models have a statewide focus.
Barriers and enhancers to the development of skills shortage models
The key barriers identified to the development of models that were effective in reducing skill shortages are:
- Policy that is not sufficiently flexible to accommodate changing workplace needs
- Unwillingness of some senior government, VET and industry representatives to take risks in order to develop new models
- Delays in gaining endorsement/accreditation of new models
- Current VET monitoring and reporting systems that are largely quantitative and inadequate for evaluating holistic approaches to skills shortages
- Issues related to working in partnership, including different working cultures, ways of operating, priorities and timelines
- Health service workplace culture that is resistant to change
- Organisational boundaries (ie, when role redesign crosses different boundaries, such as health and community services, there may be implications for pay and grading of staff).
For training-only models, there are additional barriers in terms of technology, low educational levels of some trainees, lack of availability of health professionals to provide training and/or supervision, and the cost of training.
The key enhancers identified to the development of models are:
- High level of commitment by all partners to the model. This is seen in the VET in Schools projects and at the other end of the spectrum in the Queensland Aged Care Skills Formation Strategy.
- Co-location of partners, or effective communication channels. The co-location of the training college and aged facility in the Booroongen Djugun College VET in Schools program is an example. In another example, the New South Wales Mental Health Skills Ecosystem model uses a formal consultative committee to facilitate communication and coordination among mental health services agencies.
Enhancers to the effectiveness of the models are identified as:
- First considering organisation/work unit tasks, competencies required and job (re)design. This was seen in the Baptist Community Services' Care Supervisors role. Training developed for a specially created role as adjunct to registered nurses in aged care, allowing registered nurses to be released for clinical leadership and case management.
- High profile of the model within the community. A good example is the Riverland VET in Schools nursing pathway program, which enjoys a high level of commitment by education and industry, as well as parents and students, and is an embedded part of the schools' senior curriculum.
- Community-based nature of the model. Most of the successful models are highly valued by their community, however the high valuing of Aboriginal health workers by their communities is particularly apparent. Community participation in and ownership of the program and its sustainability is critical to program success and acceptance.
- Cultural fit of Indigenous and multicultural models. Within Australia, there is a range of Aboriginal health worker programs sensitive to community cultural traditions.
- Evidence of direct link between skills development and employment.
For training-only models, additional enhancers are identified as flexibility of partners in accommodating the needs of trainees, low training costs, choice of experienced preceptors or clinical supervisors to work with trainees, and the provision of professional development to trainers to increase their knowledge and skills in flexible learning technologies and methods.
Conclusions
The findings suggest that there needs to be a balance between short-term solutions to current skill shortages (training only), and medium- to longer-term solutions (job redesign, holistic approaches) that also address projected skills shortages, in order to reduce health workforce skill shortages. In addition, models that focus on addressing skills shortages in aged care can and do provide a broad pathway to careers in the health sector. Regardless of the model chosen, those that are likely to be effective in addressing skill shortages will exhibit the following characteristics:
- Responsibility for addressing skills shortage is jointly shared between the health sector, education and training organisations and government more broadly, with employers within the sector taking a proactive role.
- The training component is complemented by a focus on retention of workers, by providing better career paths and increased job satisfaction.
- Models either skilling/up-skilling existing employees or identify and target group(s) of potential employees who may not otherwise have considered a career in health (eg school students, over 45s, CALD workers, males who have worked in another profession and are seeking a sea change).
References
1. Department of Employment and Workplace Relations. DEWR job outlook. (Online) 2004. Available: http://www.workplace.gov.au/workplace/Category/Publications/LabourMarketAnalysis/NationalSkillsShortageList2004.htm (Accessed: 1 November 2005).
2. Department of Employment and Workplace Relations. Skills in demand lists: States and Territories 2005. (Online) 2005. http://www.workplace.gov.au/NR/rdonlyres/577827A0-D866-46A3-B236-896C38B6ED0E/0/SkillsInDemandByStateOct2005.pdf (Accessed: 22 December 2005)
3. Productivity Commission. Australia's health workforce. Research Report. Canberra: Productivity Commission, 2005.
4. Australian National Training Authority. ANTA national skill ecosystem project: The role of VET providers in delivering improved outcomes across skill networks. Phase 2 Final Report. Canberra: ANTA/NSW Department of Education and Training, 2005.
5. Goodale B, Lin I. Midwest Murchison region therapy assistant project (2003-2004) final report. WA Country Health Service. Perth: Government of Western Australia, 2005.
6. Cunliffe A. First steps in a journey. Proceedings, National Services for Australian Rural and Remote Allied Health (SARRAH) Conference; August 2004; Alice Springs, Northern Territory, 2004.
7. Australian Institute of Health and Welfare. Health and community services labour force 2001. AIHW cat. no. HWL 27 and ABS cat. no. 8936.0 (National Health Labour Force Series no. 27). Canberra: AIHW; 2003.
8. Australian Bureau of Statistics. Census of population and housing. (Online) 2001. Available: http://www.abs.gov.au (18 October 2005).
9. McQuaid R, Bond S, Robertson P. Gender stereotyping in career choice. Research report from Employment Research Institute. (Online 2004). Available: http://www.napier.ac.uk/depts/eri/research/genderstereo.htm (Accessed 1 November 2005).
10. Productivity Commission. Australia's health workforce. Research Report. Canberra: Productivity Commission, 2005; p. xxvii.
11. ABS. Job vacancies. (Online) 2005. Cat. 6354.0. Available: http://www.abs.gov.au (Accessed: 18 October 2005).
12. Community Services and Health Industry Skills Council. Report May 2005. Available: http://www.cshisc.com.au/docs/upload/CSHIndustrySkillsReport-FINAL160505.pdf (Accessed: 17 October 2005).
13. Department of Education, Science and Training. Job growth and replacement needs in nursing occupations. (Online) 2001. Available: http://www.dest.gov.au/archive/highered/eippubs/eip01_18/5.htm#2_6 (Accessed: 18 October 2005)
14. Australian Bureau of Statistics. Job growth and replacement needs in nursing occupations. (Online) 2001. Available: http://www.dest.gov.au/archive/highered/eippubs/eip01_18/5.htm#2_6 (Accessed: 18 October 2005).
15. UK Department of Health. Introduction to the skills escalator. (Online) 2005. Available: ttp://www.dh.gov.uk/PolicyAndGuidance/HumanResourcesAndTraining/ModelEmployee/SkillsEscalatorArticle/fs/en?CONTENT_ID=4055527&chk=ZI7IKI (Accessed: 14 November 2005).
16. Chapman S, Showstack J, Morrison E, Franks P, Woo L, O'Neil E. Allied health workforce: innovations for the 21st century. San Francisco: University of California, 2004.
17. Oxford University Press. Shorter Oxford dictionary, 3rd edn. Oxford: Clarendon Press, 1993.
18. Patton M. Qualitative research and evaluation methods, 3rd edn. Thousand Oaks, CA: Sage, 2002.
19. Johnson B, Christensen L. ducational research: quantitative, qualitative, and mixed approaches, research ed, 2nd edn. Boston: Pearson, 2004.
20. Queensland Community Services and Health Industries Training Council Inc. Aged Care Skills Formation Strategy 2005 Project Plan. Progress Report. Brisbane: Queensland Community Services and Health Industries Training Council Inc, 2005.
21. Department of Employment and Training. Skills formation strategies CD Rom. Brisbane: Queensland Government, no date.
22. Department of Education, Science and Training. Engaging the untapped workforce: training solutions for the community services and health industry. (Online) 2003. Available: http://www.cshisc.com.au/load_page.asp?ID=36 (Accessed 23 November 2005).
23. Schwab J. VET-in-schools for indigenous students: Success through 'Cultural Fit'. (Online) no date. Available: http://www.dest.gov.au/archive/Research/fellowship/docs/Jerry_Schwab/Jerry_Schwab.pdf (Accessed: 12 December 2005).
24. Martin K & Cameron K. Looking for a seachange? Proceedings: Community Services and Health Industry Skills Council Inaugural Conference, Making a Difference; 7-8 June 2005; Australian Technology Park, Sydney. Available: http://www.cshisc.com.au/docs/upload/Post-ConfPack2005-GuidetoSpeakersandPresns.pdf (Accessed: 12 January 2006).
25. Goldberger S. From the entry level to licensed practical nurse: four case studies of career ladders in health care. Boston, MA: Jobs for the Future, 2005.
26. Jones M, Heinric K. An innovative pathway to increasing the supply of indigenous workers in the CS&H industries. Proceedings: Community Services and Health Industry Skills Council Inaugural Conference, Making a Difference; 7-8 June, 2005. Available: http://www.cshisc.com.au/docs/upload/Post-ConfPack2005-GuidetoSpeakersandPresns.pdf (Accessed 12 January 2006).
27. Pashen D, Felton-Busch C, Blackman R, Solomon S. Educational pathways for indigenous students into health careers. Proceedings: Interprofessional Education conference; November 2005; Ho Chi Minh City, Vietnam. 2005.
28. Pacza T, Steele L, Tennant M. Development of oral health training for rural and remote Aboriginal health workers. Australian Journal of Rural Health 2001; 9: 105-110.


