Introduction
Despite Malaysia having a well-organized National Tuberculosis Control Program (TBCP) which provides easy access and free-of-charge services, the notification rate of tuberculosis (TB) in Sarawak (one of the states of Malaysia) is still high. In 2003, the rate was 79.9/100 000, twice the national target of 40/100 000 population. Although there has been a gradual decline since 2001, the incidence rate of TB still ranks third in Malaysia1. There were eight out of the 26 health districts with a TB notification rate of over 100/100 000 population in 20021. The notification rate of HIV was 3.46/100 000 population in 20032 with eight reported cases (0.5%) of TB coexisting with HIV1. Approximately 48.8% of the 1686 new cases of pulmonary TB (PTB) detected in the same year were smear positive.
The detection of TB in Sarawak relies heavily on passive case detection where the success is known to be influenced by factors such as patient motivation, degree of diagnostic suspicion by health-care workers and quality of laboratory services3. When patients who have any TB symptoms decide to seek main-stream medical treatment, they have a few options: government health clinics staffed by medical assistants (MAs) or physician assistants; out-patient departments in hospitals staffed by MAs; or private practitioners' clinics. Once TB is suspected, the MAs in the health clinic can request both radiographic and sputum microscopic examinations and then refer the patients to a doctor.
Almost all health clinics have an operational area covering a radius of 12.5 km, thus most parts of Sarawak are well covered by health services. The time taken to diagnose patients seen in health clinics can be lengthened, depending on the distance of laboratories and X-ray facilities. Figure 1 shows how TB may be diagnosed.
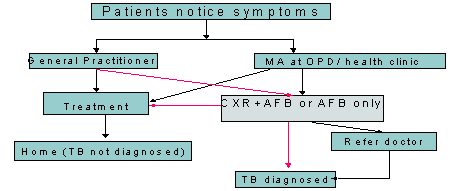
Figure 1: Steps to diagnosing TB.
It is assumed that the slow decline in TB incidence in Sarawak and the persistently high incidence in certain areas are, in part, related to a delay in case detection. A review of the records of one of the urban TB clinics showed that approximately 44% of its smear-positive PTB patients had their disease diagnosed more than 30 days after the onset of major TB symptoms, while in one rural TB clinic it was approximately 35%. A diagnosis interval of more than 30 days was considered a delay in diagnosis in some studies3. In Malaysia, two studies have been conducted on diagnostic delay4,5, assessing the diagnosis intervals and factors contributing to patients' and diagnosis delay. However, these results may not reflect the Sarawak situation because of its unique topographical features and multiethnic society. The current study aimed to investigate the length of delay, and analyze the factors linking the delay from onset of PTB symptoms until the commencement of treatment.
Methods
This study was approved by the ethics committee of both the funding organization and the Malaysian Ministry of Health, and conformed to ethical procedures for research in Malaysia. Informed consent was also obtained from each respondent.
An institution-based cross-sectional study was conducted from June 2003 to May 2004. Three divisions were randomly selected from the nine divisions in Sarawak. All the 10 TB clinics located in these divisions were included in the study. Two of these TB clinics provided services to a combination of urban and rural populations, while the other eight provided services to a rural population only. Patients were interviewed directly after their diagnosis of TB or while in hospital until the intended sample size was achieved. Patients above 15 years of age with smear-positive PTB who were mentally well were included in the study. Smear negatives and cases with a diagnosis based on X-ray, and relapsed cases were excluded.
We aimed for a sample of 320, because a sample of this size would allow us to include up to eight parameters in a regression model, using the rule of thumb that 20 observations with the event of interest (in our case 'delay') are required for each parameter in the model. Each study site was then assigned to recruit a sample size almost equivalent to 10% of new PTB cases registered in 2002.
A pre-tested semi-structured questionnaire was used to collect the study data. Medical assistants who manned the TB clinics were trained to perform the interviews. The questionnaire assessed socio-demographic details, major presenting symptoms of PTB, duration of major presenting symptoms, and the date of first health-care visit. The major symptoms asked about were the presence of a cough, production of sputum and haemoptysis. The interval between first medical consultation and the date of diagnosis was obtained through respondents' out-patient card and interview. The patients' TB registration card and TB registers were cross-checked to assure the quality of collected data.
Recommended standard procedures applied to the diagnosis of PTB in Malaysia are to collect and examine three sputum specimens from patients with suspected TB, one on-the-spot and another two early-morning specimens on two consecutive days6. Examination of sputum by direct microscopy for the presence of acid-fast bacilli (AFB) is performed at the laboratory nearest to the TB clinic. Pulmonary TB is confirmed when there are at least two AFB-positive smear results. As a quality assurance standard, every month 10% of the negative smears and all the positive smears are sent to the laboratory of the State TB Control Unit for further analysis.
Definitions of time intervals and delay
The following time intervals and delays were determined for each respondent: The patient intervalwas the time interval between the appearance of major pulmonary symptoms and the first medical consultation. Intervals longer than the median were considered indicative of a patient delay7.
The diagnosis interval was regarded as the time from the first medical consultation until the date of diagnosis. A diagnosis interval longer than the median was indicative of a diagnosis delay5.
The treatment interval was the time from diagnosis to initiation of treatment. Intervals of longer than the median were considered indicative of treatment delay8.
Data analysis
The software, SPSS vers 14 (SPSS Inc, Chicago IL, USA) was used for the analysis. The median was used as the cutoff point to dichotomize the dependent variable as the distribution of both patient and diagnosis intervals was positively skewed. Chi-squared tests were used to compare delay by patient characteristics. Univariate and multivariate logistic regression analyses were performed to assess the relative impact of predictor variables on the outcome variable (delay). Logistic regression was used due to the skewed distribution of dependent variables, and the main objective of the study was to determine the predictor variables for delay or non-delay in patients seeking treatment and obtaining a diagnosis. P-values of ≤0.05 were considered statistically significant.
Results
Patient characteristics
During the one-year study period, 316 new smear-positive adult PTB patients were recruited, of which 61.1 % were males and 38.9% females. The mean age was 44.2 years, range 15-70 years with a median age of 45 years. In terms of the distance between respondents' homes and the nearest health facility, kilometers or time taken was used, depending on whether the two points were connected by proper roads or not. For the 210 respondents who judged the distance by kilometer, 37.4% claimed they lived 10 km away from a health facility. Of the other 106 respondents, 25.4% said their house was more than 30 min away from any health facility. With regards to occupation, 22.8% were farmers, 18.7% housewives, 9.9% civil servants, 26.2% employed by private firms, 5.4% self-employed and 15.8% unemployed. For household income, 38.3% of respondents claimed a household income of less than ringgit Malaysian (RM) 300 per month, which was classified as indicative of poor families in Sarawak; 29.7% households had an income between RM301 and 600 (below the poverty line); and the remaining 32% of households lived above the poverty line. While 243 respondents (76.9%) had no history of an index case for TB, there was a positive history in 73 respondents (23.1%). The index case in this study included household contacts, workplace contacts and village contacts.
Patient delay
The median patient interval was 30 days, IQR (14-60 days). Of the 224 patients who volunteered the information, 48.4% claimed that they did nothing for their TB symptoms before seeking a medical consultation, 15.5% treated themselves with over-the-counter drugs, while 7% sought treatment from traditional healers. The remaining respondents claimed that they treated themselves as well as using traditional healers. The final decision to seek medical advice was most influenced by the severity of the symptoms (81%), while spouses, relatives and friends were other motivators (17%). Based on cumulative distribution, 42.7% of the respondents consulted a medical worker more than 30 days from the onset of TB symptoms. The longest delay was reported to be one year.
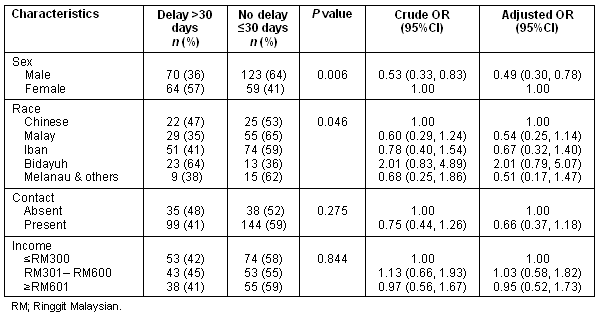
Patient delay was analysed by patient characteristics (Table 1). Significantly fewer male respondents (36%) had a patient delay, compared with female respondents (57%) (χ2 = 7.64 on 1 df, p = 0.006). There was also a statistically significant difference in patient delay by race (χ2 = 9.68 on 4df, p = 0.046), with the Bidayuh ethnic group having the highest (64%) patient delay. Using logistic regression analysis, (Table 1), only being female was associated with increased patient delay. The Hosmer and Lemeshow test provided a χ2 of 5.342 and was not significant (p = 0.142) showing an acceptable fit of the model. Over all 62.3% of cases were predicted correctly as to whether or not they had a patient delay. There was no significant interaction between independent variables.
Table 1: Association of patient characteristics and patient delay
Diagnosis delay
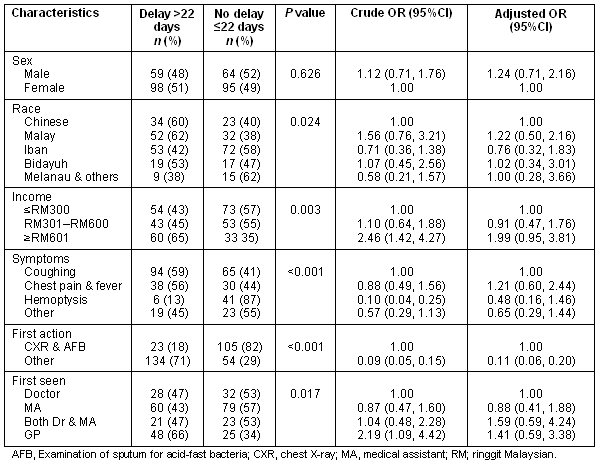
The median diagnosis interval was 22 days, IQR (1-60 days). Diagnosis delay varied by race (χ2 = 11.19 on 4df, p = 0.024), income (χ2 = 11.71 on 2df, p = 0.003), symptoms (χ2 = 32.66 on 3df, p < 0.001), first action taken (χ2 = 86.57 on 1df, p < 0.001) and who first saw the patient (χ2 = 10.19 on 3df, p = 0.017) (Table 2). Chinese and Malay ethnic groups, those on the highest income, those without haemoptysis, those not receiving a chest X-ray and AFB, and those visiting a GP all appeared to be the most at risk of diagnosis delay. However, when all variables were entered into the multivariate logistic regression, only first action taken remained statistically significant. In particular, those not receiving a chest X-ray and AFB were 9.1 times (95% CI 5.0-16.7) more likely to experience a diagnosis delay. The Hosmer and Lemeshow test showed an excellent model fit (χ2 = 3.90, p = 0.866). Over all, 64.3% of cases were predicted correctly. There was no significant interaction between independent variables.
Table 2: Association of patient characteristics and diagnosis delay
Treatment delay
The median time interval from the diagnosis of TB to the initiation of treatment was 0 days (range 0-7 days). Two hundred and ninety-nine (94.6%) of the respondents started treatment immediately on diagnosis, while the rest, 17 (5.4%) started treatment within 7 days of diagnosis.
Discussion
This present study found that the median patient interval was 30 days which was longer than two other studies undertaken in Peninsula Malaysia4,5. This finding could be related to the poorer transportation system in Sarawak. In Hooi's study4, the delay was found to be longer in males, those with lower than secondary education and drug users, which was not reflected in this study. In contrast, the results from this study are similar to studies undertaken in Vietnam9 and Bangladesh10, where female respondents had a longer patient delay. Although there is no status disparity amongst males and females in Sarawak, many women in the rural areas depend on their husbands or male relatives to bring them in for treatment, due to transportation difficulties. The patient interval was extended if the men were preoccupied with work.
When considering the median diagnosis delay of 22 days, it is similar to other studies conducted in Penang4, Ethiopia11, Tanzania12, and Japan13, which were between 3 weeks and one month. GP consultations could be a risk factor for diagnosis delay, as only 17.8% of respondents visiting a GP had radiographic and sputum microscopic investigations. Lack of these investigations during first consultation was found to be significantly associated with diagnosis delay. Penang4 and Ethiopia11 had a similar finding. This can be explained by the fact that most GP clinics are not equipped with TB diagnostic facilities. Respondents who presented with a cough only during their first medical consultation tended not to be diagnosed, reflecting a low index of suspicion. This is unexpected as Malaysia is an intermediate TB-burden country. Respondents who lived above the poverty line appeared to visit different GPs until the severity of their symptoms forced them to seek treatment in government clinics. The reason respondents sought treatment at GP clinics included shorter waiting and consultation times, and the fact that they could afford to pay for the service. The TBCP in Malaysia requires all GPs to notify the authorities when a TB case is diagnosed; however, greater effort is required to increase their index of suspicion, and proper diagnosis and management of TB is still needed. Other factors linked to diagnosis delay such as lower education14, and being female10 were not observed in this study.
The treatment interval observed in this study ranged from 0 to 7 days, which was shorter than other studies conducted in Seremban8, and Canada15. Delayed treatment initiation unnecessarily prolongs the periods of TB transmission in the community, and delayed treatment for hospital patients is believed to contribute significantly to nosocomial transmission15. Delays in treatment were not observed in this study because once a TB patient is detected, the nearest health clinic to the patient would be informed by telephone. The health worker from the health clinic then rapidly traced the patient.
It is recognized that this study has potential limitations due to the data collection method. First, the outcome measure of patient interval was self-reported, implying the possibility of a recall or self-presentation bias. To reduce the recall bias, questions targeted specifically major pulmonary symptoms and how long after the onset of symptoms they sought medical consultation. In addition, religious and other festivals were used to facilitate respondents' recall and to estimate the date of symptom onset. The result of this study may not be generalisable to all smear-positive PTB patients in Sarawak because only patients treated in government health facilities were interviewed, thus excluding patients from private health facilities.
Conclusion
This study found that gender was significantly associated with patient delay, because women depended on male family members to take them for treatment. The major factor associated with diagnosis delay was whether or not radiographic and sputum microscopic examination were performed during the first visit, and this was also related to whether the patient first visited a GP.
Acknowledgements
We are grateful to Dr Kamarudin Lajim and Mr HJ Sapiee Lundu, for their assistance in facilitating the data collection. We acknowledge the contribution of medical assistants manning the TB control units for data collection, and the patients for their willingness to participate in the study. Also acknowledged is Dr Chang Kam Hock, Universiti Malaysia Sarawak (UNIMAS) for reading and commenting on the initial draft. This research was made possible by a short-term grant of the Universiti Malaysia Sarawak.
References
1. Sarawak State Health Department. Laporan Tahunan Program Kawalan TB Negeri Sarawak Tahun 2003. Kuching: Sarawak State Health Department, 2004.
2. Sarawak State Health Department. Health facts 2003. Kuching: Sarawak State Health Department, 2004.
3. Dujardin B, Kegels G, Buve A, Mercenier,P. Tuberculosis control: did the program fail or did we fail the program? Tropical Medicine and International Health 1997; 2: 715-718.
4. Hooi LN, Case-finding for pulmonary tuberculosis in Penang. Medical Journal Malaysia 1994; 49: 223-230.
5. Liam CK, Tang BC. Delay in the diagnosis and treatment of pulmonary tuberculosis in patients attending a university teaching hospital. International Journal of Tuberculosis and Lung Disease 1997; 1: 326-332.
6. Ministry of Health, Malaysia. Direct Smear Microscopy 1st edn. Kuala Lumpur: TB/Leprosy Control Unit, Ministry of Health, Malaysia, 2000.
7. Demissie M, Lindtjorn B, Berhane Y. Patient and health service delay in the diagnosis of pulmonary tuberculosis in Ethiopia. BMC Public Health.2: 23. (Online) 2002. Available: http://www.biomedcentral.com/1471-2458/2/23 Accessed 16 September 2005).
8. Loh LC, Codati A, Jamil M, Noor ZM, Vijayasingham P. "Discovery to treatment" window in patients with smear-positive pulmonary tuberculosis. Medical Journal of Malaysia 2005; 60: 314-319.
9. Long NH, Johansson E, Lonnroth K, Eriksson B, Winkvist A, Diwan VK. Longer delays in tuberculosis diagnosis among women in Vietnam. International Journal of Tuberculosis and Lung Disease 1999; 3: 388-393.
10. Ahsan G, Ahmed J, Singhasivanon P, Kaewkungwal J, Okanurak K, Suwannapong N et al. Gender difference in treatment seeking behaviors of tuberculosis cases in rural communities of Bangladesh. Southeast Asian Journal of Tropical Medicine and Public Health 2004; 35: 126-135.
11. Yimer S, Bjune G, Alene G. Diagnostic and treatment delay among pulmonary tuberculosis patients in Ethiopia: a cross sectional study. BMC Infectious Diseases. (Online) 2005. Available: http://pubmedcentral.gov/ (Accessed 20 September 2005).
12. Wandwalo ER, Morkveo. Delay in tuberculosis case finding and treatment in Mwanza, Tanzania. International Journal of Tuberculosis and Lung Disease 2000; 4: 133-138.
13. Aoki M, Shimao T. Studies on factors influencing patients', doctors' and total delay of tuberculosis case-detection in Japan. International Journal of Tuberculosis and Lung Disease 1985; 60: 128-130.
14. Xu B, Jiang QW, Xiu Y, Diwan VK. Diagnostic delays in access to tuberculosis care in counties with or without the National Tuberculosis Control Programme in rural China. International Journal of Tuberculosis and Lung Disease 2005; 9: 784-790.
15. Greenaway C, Menzies D, Fanning A, Grewal R, Yuan L. FitzGerald Canadian Collaborative Group in nasocomial transmission of tuberculosis. American Journal of Respiratory and Critical Care Medicine 2002; 165: 927-933.
Abstract
Introduction:
Delayed diagnosis of tuberculosis (TB) can lead to an increased period of infectivity in the community, a delay in treatment and a severe form of the disease. The objective of this study was to determine the length of delay, and factors linking the delay from the onset of symptoms of pulmonary tuberculosis (PTB) until the commencement of treatment in Sarawak, Malaysia.Methods: An institution based cross-sectional study was conducted in 10 TB clinics in randomly selected divisions in Sarawak from June 2003 to May 2004. Delay was analyzed from two perspectives: (1) period between the onset of TB symptoms to any first medical consultation (patients' delay); and (2) period between the first medical consultation to the diagnosis of TB (diagnosis delay). Patients were interviewed on diagnosis or within the admission period using a semi-structured questionnaire.
Results: A total of 316 new smear-positive PTB patients participated in the study. The median patient interval was 30 days. Gender was found to be significantly associated with patient delay. The median diagnosis interval was 22 days. Respondents' incomes, health-care professional first consulted and actions taken by the health-care providers during the first consultation were significantly associated with diagnosis delay. The medium treatment interval was 0 days.
Conclusion: Both patients and health providers played a role in delaying TB diagnosis. Females appeared to have longer delay. Respondents living above the poverty line had diagnosis delay as they made more visits to GPs or different government clinics without proper investigations for TB. A mechanism is needed to increase all health-care providers' suspicion of TB so that proper investigations can be done during first consultation.
Key words: cross-sectional study, diagnosis delay, patient delay, Sarawak, tuberculosis.
You might also be interested in:
2013 - Retraction

