Introduction
Australia is facing a significant dental workforce shortage. It has been estimated that by 2010, Australia will be approximately 1000 dental professionals short of workforce requirements1. Consistent with trends observed with medical practitioners, it is expected that the greatest impact of this shortage will be in rural and remote areas.
Dental education in Australia and throughout the world is going through a period of significant change, some of which is targeted at addressing the workforce issues2-7. At The University of Western Australia, this change commenced 8 years ago with the replacement of a discipline-based dental curriculum with an outcome-based learning curriculum. During the final year of the new curriculum, students undertake a pre-graduation internship that consists of three terms of compulsory clinical placements and a single optional placements term. A personal and professional development program is intertwined within these four terms. One of the optional placements is a rural, remote and Indigenous placement (RRIP) option, developed by the Western Australian Centre for Rural and Remote Oral Health. Since approximately 2004, the rural content of the curriculum has been increased. The RRIP program is part of a comprehensive strategy to address the current shortage of rural dental practitioners8, and similar outplacement models have been established in medicine and allied health curricula9-11. The rural and remote outplacement model is also consistent with changes in the education sector to move away from discipline-based curricula towards an increased utilisation of experiential learning12. This study is a description of the program's development and design, student evaluation and outcomes after 4 years (2002-2005).
Rural and remote program development and design
Previous international and national research suggested an increased likelihood for health graduates to choose rural practice if they have a rural background, or were exposed to rural practice during their education13,14. The goal of RRIP was to encourage more students into rural practice after graduation by providing positive rural experiences. The program was developed collaboratively with a number of stakeholders including rural dental practitioners, Aboriginal medical services (AMS) representatives and Indigenous community representatives. The program was designed to give students the opportunity to experience a variety of rural lifestyles, while being actively involved in the supervised provision of a broad spectrum of dental care services. To meet these outcomes, RRIP is a three-week rotation through a selection of locations, involving both private practices and AMS dental clinics. Placements sites include industrial fishing, mining, farming and wine-making regions in Western Australia. The placement length of 3 weeks was in accordance with the length of the other optional placements offered through the School of Dentistry, as necessitated by the existing timetabling of the final year of the course. Rural and remote was defined as being outside the Perth metropolitan area (ie rural and remote zones as defined by the Rural Remote Metropolitan Area classification system [RRMA] with populations ranging from less than 5000 to less than 100 000)15.
Dental practitioners in each setting were recruited as supervisors and became honorary clinical consultants for The University of Western Australia. The program started in 2002 and a total of 78 students participated (through to December 2005). An additional site was added in 2003 (the state of Northern Territory). Transport to and from the Northern Territory was sponsored by the local Australian Dental Association branch in an effort to increase exposure of students to the unique environments of the region. These interstate placements are included in the analysis as part of the RRIP program. Although similar programs have been established by other dental schools since then, this program was the first of its kind in Australia.
Assessment of students
Student assessment consisted of two equally weighted parts. First, students were required to prepare a written paper on one of the allocated topics, relevant to the area they had visited. Initially there was a choice of three topics but in later years this increased to five. This assessment method aligns with the overall aims of the program, especially in the broad category of thinking critically. It provides the opportunity to develop arguments, reflect, evaluate, assess and judge. The assignments reflect the students' knowledge and are linked to their personal experiences during the outplacements. The majority of the students have completed the assignments to a high standard and have demonstrated in-depth understanding of the issues related to oral health in their placement areas, as well as highlighting possible strategies for the improvement of oral health of the populations in these areas.
Second, the supervisors provided feedback on student performance based on a set of criteria which include: professionalism, preparation of cases, patient rapport, record keeping, diagnostic skills, clinical judgement, clinical skills, attendance, co-worker rapport, and initiative. Feedback from the supervising dentists was very positive, with most stating that the students demonstrated sound clinical knowledge and competencies, fitted in well with existing staff and patients, and displayed professional behaviour and attitudes while on their placements.
Student evaluation of the rural, remote and Indigenous placement
An assessment of students' attitudes to rural practice and rural life is an essential part of the program, in order to evaluate the impact of the rural experience. The assessment may also provide evidence to support increased rural exposure for undergraduate dental students, and allows the program to be refined from the feedback. Students participating in RRIP completed two forms of evaluation: program evaluation and outcomes evaluation.
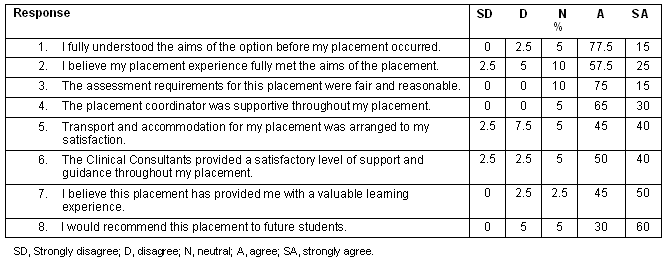
Program evaluation: This was completed by all students who on the program, was anonymous and consisted of a questionnaire primarily focused on the logistical issues associated with the outplacements, such as appropriateness of accommodation, adequacy of support, value of the learning experience, and the fulfilment of program aims. The students were given the opportunity to answer questions on a Likert scale with five possible responses ranging from 'strongly disagree' to 'strongly agree'. The majority of the students answered 'agree' or 'strongly agree' to positive statements about the placement (Table 1). To the statement 'I would recommend the placement to future students', 90% indicated that they 'agree' or 'strongly agree' with the statement (Table 1).
Students went on outplacement for 3 weeks, visiting one, two or three clinics during that time, depending on their location. Just over two-thirds of the students agreed that 3 weeks was sufficient time to provide them with adequate experience of rural dental life, as well as rural life. They felt the time was adequate to allow an insight to life in a rural town as well as to experience the procedures common in rural practice with a wide range of patients. Of those who did not think 3 weeks was adequate, over one-third of the students (38.5%) indicated that 4 weeks would have been better to allow travelling to remote Aboriginal communities and settling into town life. Supervisor feedback also identified that a week in each location is insufficient time.
Table 1: Student outcome response to rural placement
Outcomes Evaluation: Students' perceptions of different issues that relate to rural practice, including the differences between rural and urban practice, differences in the patient base and the perceived reasons for unsuccessful recruitment of rural practitioners were evaluated through a series of open-ended questions.
More than 78% of students reported never having experienced rural life before their placement. The qualitative data indicates that the perceived advantages of rural practice include broader scope of treatment needs and the relaxed and friendly atmosphere. The commonly perceived disadvantages of rural practice were the lack of technical and specialist support, longer waiting lists for patients and lower availability of equipment (Table 2). The differences in the patient base were also noted, including that rural patients were commonly perceived as friendlier and less demanding than their urban counterparts; a higher percentage of Aboriginal patients; generally poorer overall health; and a short-term outlook on treatment methods (Table 3).
Students were also asked to provide insights into their perceptions of the difficulties in recruitment (and retainment) of dental practitioners in rural practices. The most common feedback included isolation from family, friends and other support bases; lack of facilities and social activities; and pre-conceived negative ideas about rural life (Table 4).
Table 2: Perceived differences between rural and urban dental practice
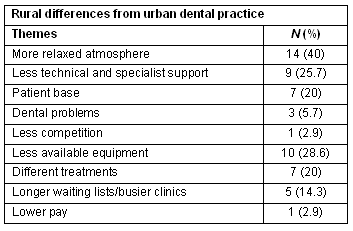
Table 3: Observed differences between rural and urban patients
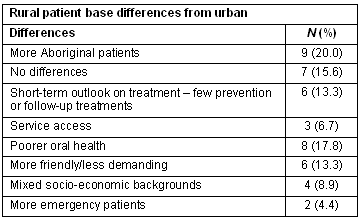
Table 4: Reasons for difficulty of rural dentist recruitment

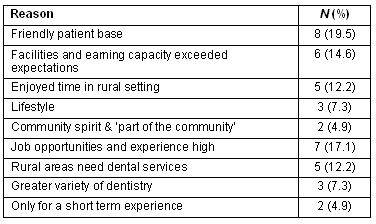
Most students (83%) indicated they would consider rural practice, with 79% of all considering rural practice before completing the placement. The reasons students indicated for practising in a rural area when they graduated included: many job opportunities and experience; friendly patient base; and the facilities and earning capacity exceeded expectations (Table 5). Only three students indicated they were not interested in practising in a rural area with reasons being:
The outplacement allowed me to be exposed to a rural area and I have realised that it is not for me.
An enjoyable experience though isolation from family and friends would be difficult.
Relocation to a quieter rural setting too difficult. Less chance of doing more complex elective procedures. Patients only seeking relief of pain. Reduced access to luxury items.
Table 5: Reasons students provided to explain why they would consider practising in a rural area
Graduate survey
Data were collected post-graduation to assess the location of practice (within the first year of graduation) following participation in the RRIP program. These data were collected using both the published dental register (of Western Australia) and direct phone (and/or email) contact to determine practice location, for graduates of all years participating in the program (2002-2005).
All those contacted were informed that the single question about location of practice (within the first year after graduation) was for research purposes. A total of 143 students graduated during 2002-2005 study period, and almost 55% of these students were involved in RRIP. Almost 80% of the graduates (77%, n = 111) could be contacted. In 2003, 26% of the students who participated in the program in 2002 were employed in a rural area within the first 12 months of graduating. Of those from the 2003 class, 38% of those who participated in the program were practising rurally in Western Australia after graduating. From the 2004 class, 60% of the students who took part in the RRIP program were employed in a rural area in their first year after graduation. For those graduating at the end of 2005, 48% of all RRIP participants were working in rural or remote areas within 6 months of graduation, when the survey was conducted. Rural and remote was defined as being outside the Perth metropolitan area (ie rural and remote RRMA zones with populations ranging from less than 5000 to less than 100 000)15.
Discussion
The program design was based on previous international research which reported the positive effect of a rural medical outplacement experience on rural retainment after graduation13,14,16-19. This was supported by a study into the rural working patterns of nursing students in Australia, where changed intentions of those participating in the placement were observed and reported9-11.
Evidence from subsequent Australian studies on the effectiveness of rural exposure during training, however, are variable13. According to Orpin this reflects the relative short history of these programs, the lack of standardisation among schools, and difficulties in controlling for the effects of pre-existing rural orientation. The ultimate test of the effectiveness of undergraduate interventions will be the eventual evening-out of the workforce maldistribution. This is, however, a long-term prospect13.
After only 5 years, it is too early to tell if this program does encourage students into eventual rural practice. Undergraduate feedback suggests that most students who eventually work in a rural location had considered the possibility prior to the outplacement, and that the outplacement rotation was not the reason they chose rural practice. Some graduates, however, did choose rural practice because of their rural undergraduate experience. This is consistent with earlier research among nursing and allied health students who were more likely to enter rural practice after voluntary rural placements14.
In the short term, the analysis of student attitude towards rural practice assists in evaluating the impact of rural placement, and feedback from participants provides some insights into the students' perceptions of this experience. Undergraduates participating in this program were generally very positive about the experience and, for the majority (95%), it was valuable learning experience. This confirms the results of an earlier Australian study which found that rural attachments for health discipline students are worthwhile learning experiences20. The program remains optional, and the fact that the majority of students choose to do it each year (after feedback from their peers) is an indication that the students find it an enjoyable and worthwhile experience.
Previous work among medical students has shown that the timing of a rural outplacement is important, and that those that do a rural outplacement in their final year are more inclined to become rural doctors than those who did it in their third year21.
This model is in a continuous process of refinement; the use of a tool such as that developed by Adams et al. to measure student attitudes to rural practice and rural life across three dimensions is one aspect that could be implemented in future programs22.
Another example of an innovative approach to rural recruitment include the US Rural Summer Studentships program19, where a handful of medical students are offered eight-week summer jobs performing health research on a topic they have proposed. This program allows them the opportunity to participate in both health research and clinical practice while working towards their own educational outcomes. Responses from the project were very positive, and a longer placement coupled with a research element could be a consideration for future dentistry outplacements.
A number of other options also exist for refining the outplacement program. One under consideration is making the placements compulsory, which has the advantage of exposing all undergraduates to rural practice. However students with fixed commitments (eg family) may be disadvantaged. The nursing study10 prepared participants for their rural placement exceptionally well, with many meetings and team-building exercises undertaken prior to placement. This was as much to ensure student preparedness as it was to ascertain the suitability of the applying students, some of whom were thought to be participating simply for tourism benefits. Feedback has indicated that the current model is well received by the participants and a prolonged placement may encourage a negative outcome, with students perceiving they have 'done their time', rather than generating a genuine interest in future rural practice. A previous study among nursing and allied health students also found that increased time spent in a rural area during a course may be unnecessary or counterproductive if the goal is to increase the rural workforce14.
Conclusion
Ongoing refinement, evaluation and monitoring of the program are occurring and the follow up of graduate participation in rural practice is continuing. The model cannot yet claim to be a successful model for the recruitment and retention of dentists to rural areas. It does, however, provide most participants with a positive rural experience and fosters positive attitudes to rural practice. The 2002-2005 trial of the RRIP program, coupled with other rural initiatives in the dental curriculum, are expected, in the longer term, to facilitate and help address the projected shortage of rural dental professionals. Based on the outcomes of the RRIP program, rural outplacements have become an integral part of the curriculum.
Acknowledgments
The authors wish to especially thank Nicola Johnston, Leanne Coombe, Kirrilee Smith Gina Arena and Dave Holley who have contributed over many years to the development, implementation and review of this program. The authors would like to acknowledge the long-term efforts of Alice Evans and Jill Evans in support of the placements' administration.
References
1. Australian Research Centre for Population Oral Health. Working papers of the ARCPOH/Australian Institute of Health and Welfare Dental Statistics and Research Unit workshop on the dental labour force. Adelaide, SA: ARCPOH/AIHW, 2002.
2. Kerosuo E, Ruotoistenmaki J, Murtomaa H. Report on the development of a new dental curriculum at Helinski. European Journal of Dental Education 2001; 5: 23-30.
3. Ismail AI. Some potential outcomes of the new dental curriculum developed by the Faculty of Dentistry, Dalhousie University, Canada, in the early 1990s. Journal of Dental Education 2001; 65: 1196-1198 (Letter).
4. Martinez-Alvarez C, Sanz M, Berthold P. Basic sciences education in the dental curriculum in Southern Europe. European Journal of Dental Education 2001; 5: 63-66.
5. Bertolami CN. Rationalising the dental curriculum in light of current disease prevalence and patient demand for treatment: form versus content. Journal of Dental Education 2001; 65: 725-743.
6. Kelly M, McCartan BE, Schmidt HG. Cognitive learning theory and its application in the dental curriculum. European Journal of Dental Education 1999; 3: 52-56.
7. MacNeil MA, Walton JN, Clark DC, Tobias DL, Harrison RL. Structuring a clinical learning environment for a hybrid-PBL dental curriculum. Journal of Dental Education 1998; 62: 723-745.
8. Steele L, Pacza T, Tennant M. Rural and remote oral health; problems and models for improvement: a Western Australian perspective. Australian Journal of Rural Health 2000; 8: 22-28.
9. Courtney M, Edwards H, Smith S, Finlayson K. The impact of rural clinical placement on student nurses' employment intentions. Collegian 2002; 9: 12-18.
10. Neill J, Taylor K. Undergraduate nursing students' clinical experiences in rural and remote areas: recruitment implications. Australian Journal of Rural Health 2002; 10: 239-243.
11. Woloschuk W, Tarrant M. Does a rural educational experience influence students' likelihood of rural practice? Impact of student background and gender. Medical Education 2002; 36: 241-247.
12. Hendricson WD, Cohen PA. Oral health care in the 21st Century: implications for dental and medical education. Academic Medicine 2001; 76: 1181-1206.
13. Orpin P, Gabriel M. Recruiting undergraduates to rural practice: what the students can tell us. Rural Remote Health 5: 412. (Online) 2005. Available: www.rrh.org.au (Accessed 8 August 2007).
14. Playford D, Larson A, Wheatland B. Going country: rural student placement factors associated with future rural employment in nursing and allied health. Australian Journal of Rural Health 2006; 14: 14-16.
15. Department of Primary Industries and Energy and Department of Human Services and Health. Rural, remote and metropolitan areas classification. 1991 Census edition. Canberra, ACT: AGPS, 1994.
16. Brooks RG, Walsh M, Mardon RE, Lewis M, Clawson A. The roles of nature and nurture in the recruitment and retention of primary care physicians in rural areas: a review of the literature. Academic Medicine 2002; 77: 790-798.
17. Cardador MT, Rosenbaum M. Enhancing medical students' participation in the rural community. Academic Medicine 1998; 73: 604.
18. Denz-Penhey H, Murdoch JC, Lockyer-Stevens VJ. 'What makes it good makes it really bad.' An exploration of early student experience in the first cohort of the Rural Clinical School in The University of Western Australia. Rural Remote Health 4: 300. (Online) 2004. Available: www.rrh.org.au (Accessed 8 August 2007).
19. Zorzi A, Rourke J, Kennard M, Peterson M, Miller K. Combined research and clinical learning make rural summer studentship program a successful model. Rural Remote Health 5: 401. (Online) 2005. Available: www.rrh.org.au (Accessed 8 August 2007).
20. McAllister L, McEwan E, Williams V, Frost N. Rural attachments for students in the health professions: are they worthwhile? Australian Journal of Rural Health 1998; 6: 194-201.
21. Rolfe IE, Pearson SA, O'Connell DL, Dickinson JA. Finding solutions to the rural doctor shortage: the roles of selection versus undergraduate medical education at Newcastle. Aust N Z J Med 1995; 25: 512-517.
22. Adams ME, Dollard J, Hollins J, Petkov J. Development of a questionnaire measuring student attitudes to working and living in rural areas. Rural and Remote Health 5: 327. (Online) 2005. Available: www.rrh.org.au (Accessed 8 August 2007).



