Introduction
Iran has had a severe land mine problem in its western provinces since the 1980-1988 war between Iran and Iraq. In a survey of the Eylam Province, Jahunlu, reported a mortality rate of 36.4% in 1086 land mine victims during the period 1989-1999 in this province1. Mortality after land mine injuries is high and to a large extent prehospital2,3, indicating that effective treatment should be delivered in this phase. Training and organizing trauma care aiming at a reduction in mortality after mine injuries was implemented in 2001. An Iranian non-governmental organization (Iranian Mine Victim Rescue Centre) in cooperation with the Ministry of Health in Iran, Eylam Medical University and Norwegian physicians, initiated a training program in the land mine affected areas of the Eylam Province. The intention was to upgrade the performance of the already existing health infrastructure. The program draws on the experiences from similar successful low-cost prehospital trauma programs in Northern Iraq and Cambodia4-6.
The aim of this study was to describe the training and evaluate the effect using mortality, change in physiological function of victims after prehospital treatment and time intervals as outcome measures.
Materials and methods
The intervention was carried out in the district of Mehran in the Eylam Province, close to the Iraqi border. The rural areas of Mehran are heavily contaminated by land mines and unexploded explosive ordnances left over from the Iran-Iraq war. The target area also included 5 districts and villages in the vicinity of this city that lies on the border between Iran and Iraq. Mehran has nomads who arrive in the autumn and winter every year, and some of the inhabitants leave the city in the summer because the weather is very hot in this season (near 60°C). This results in a doubling of the population of Mehran during the winter. The official census reported the population of the region to be 46 981 in 1996, and after the US attack on Iraq it increased due to migration of pilgrims from other parts of Iran. In 2006 there were 57 889 inhabitants and nomads7.
The trauma system
The backbone of Iran's rural healthcare system are the behwarses, rural healthcare workers who are trained medical professionals at village level. These rural healthcare workers have 2 years training in primary healthcare and preventive medicine, and work under the supervision of GPs in a system of continuous education. They have previously had little or no responsibility for emergency care.
Most rural trauma victims are initially transferred to the Mehran Clinic, which is an emergency clinic staffed with emergency technicians who have been trained in basic trauma care and general physicians and nurses trained in advanced trauma care. On-call staffing is one GP and one nurse. The clinic has beds for overnight observation of patients not in need of surgery and admission.
Patients are either treated by the GPs in Mehran or transferred to the Eylam University Hospital. This is a trauma centre with an emergency ward, a radiological service including CT scanner, well-equipped operating rooms and an ICU. The hospital is staffed by four general surgeons, four orthopaedic surgeons, five gynaecologists, and specialists in anaesthesiology and emergency medicine. Transport time between Mehran and Eylam hospital is 40-50 min by ambulance. If transferred, patients are accompanied by an emergency technician in the ambulance to Eylam.
The training intervention
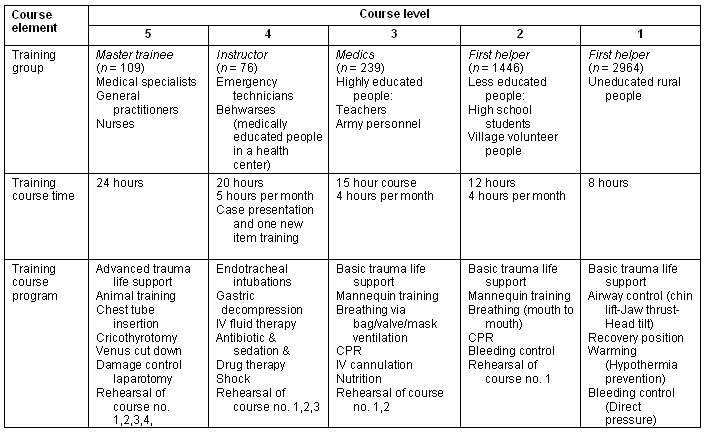
The training program was organized in accordance with experiences gained in similar programs in Afghanistan, Northern Iraq, Cambodia and Burma5,8, and was based on a manual for training prehospital care in low- and middle-income societies9. The training was targeted at different levels. A two-day course in advanced trauma care was given to specialist GPs and nurses (n = 109) in the Mehran Clinic and the Eylam University Hospital. Rural healthcare workers and emergency technicians (n = 76) received a simpler and shorter course over two days. Lay people (n = 4649) were given different courses in basic trauma care, depending on their previous knowledge, to enable them to function as first responders. These courses were of one to two days duration (Table 1). Refresher courses were held every month throughout the study period for the emergency technicians and rural health workers (groups 3,4). The training was initiated in 2001 and continued throughout the study period.
Table 1: Trauma care training program
Data collection
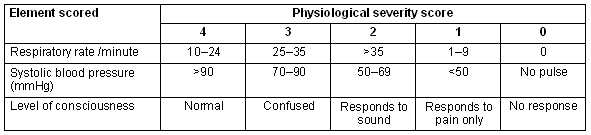
Patient medical data were gathered at two points. The first assessment was done at admission to the Mehran Clinic. A three-component physiological score was made using a scale similar to the Revised Trauma Score (RTS), as described previously10 (Table 2). The variables recorded were respiratory rate, systolic blood pressure and level of consciousness. Based on this assessment we calculated a Physiological Severity Score (PSS) using the standard RTS vectors, 0.9368 x GCS, 0.7326 x BP, and 0.2908 x RR11. In addition, an initial anatomical description of the injury with the cause of the injury, time and place of trauma and prehospital medical treatment was recorded. The final assessment was made on admission to Eylam University Hospital. This assessment included the same information as the initial assessment, and in addition the Injury Severity Score (ISS) was calculated using the Abbreviated Injury Scale 1990, update 98. Mortality rate was assessed using death within 30 days post-injury as the outcome. The treatment effect was calculated as the difference between the final PSS and the initial PSS.
Table 2: The simplified Physiological Severity Score in which the Glasgow Coma Scale component is replaced by a five-level scale of consciousness10
During the study period, a number of other victims of injuries were brought directly to Eylam University Hospital. They were registered in the emergency department in Eylam in a similar fashion. Thirty victims of mine injuries were found dead at the site of injury in the border area between Iran and Iraq and brought to Mehran. The coroner's reports on the victims were used for entering them into the database.
Treatment and data quality was supervised at monthly meetings between system supervisors and the emergency technicians and rural health workers.
Statistics
Data were recorded in injury charts for each patient. All analyses were performed using SPSS v11.0 (SPSS Inc; Chicago, IL, USA). Continuous variables are presented as means with the corresponding 95% confidence intervals (95% CI), and differences between means are given as 95% CI with the corresponding p value. To compare frequencies χ2 tests were used, and for comparison of means in continuous data t-tests or ANOVA with Bonferroni post-hoc tests were used. Comparisons of discontinuous data were performed using the Mann-Whitney test. Comparison of groups was two-tailed with statistical significance set at p < 0.05.
Ethical considerations
The training intervention was approved by and performed in accordance with the local authorities (the Governor of Eylam and the head of the University of Eylam) and the national health authorities in the Health Ministry of Tehran. The intervention did not include experimental or randomization procedures, only training and education.
Results
The study period was 3 years from January 2002 to December 2004.
Patients
In the period from January 2002 to December 2004, a total of 366 patients were treated in the system. In addition, information concerning 30 deceased victims was included, based on the coroner's reports.
The patients entered the system through the Mehran Clinic, and 226 of the victims were transferred to the Eylam University Hospital. Of the patients entering through the Mehran Clinic, 238 of the 366 had prehospital support by rural health workers or first responders before they were treated in the Mehran Clinic. Two or three rural health workers were always present in the Mehran Clinic to help nurses and emergency technicians in care of trauma victims.
During the same period a group of other victims was brought directly to the Eylam University Hospital (n = 245) as illustrated (Fig1). Patients brought directly to the Eylam University Hospital were not treated by personnel from the program. This group of patients was registered at admission to Eylam University Hospital as a convenience group for comparison.
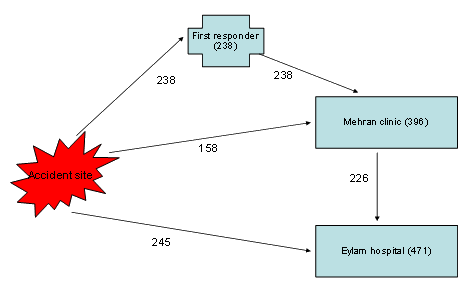
Figure 1: Flow chart for victims treated by the trauma chain in Eylam province.
Land mine injuries and explosives caused 28% of the injuries, while 57% were injured by assaults, knifings, car accidents, falls and other mechanisms, and 15% were injured by gunshots. Most of the victims were farmers and nomads. There were 552 men (86%) and 89 women (14%), and the average age was 31 years (range: 1-85 years); 86 victims (13%) were below 18 years of age. The case load varied among the years, with 108 victims (16.8%) in 2002, 327 victims (51.0%) in 2003 and 206 victims (32.1%) in 2004 (Fig2). Penetrating injuries (mine and bullet injuries and other penetrating wounds) were found in 483 victims (75%). The remaining victims (25%) had blunt injuries and burns.
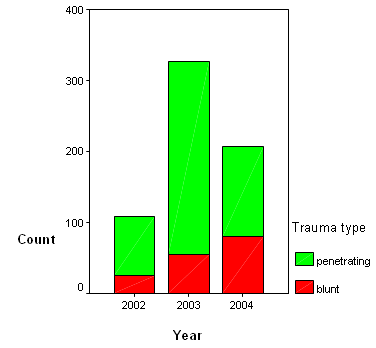
Figure 2: Distribution of patients and injury types by year.
Trauma severity
There was no difference in ISS between the group with treatment in the Mehran Clinic before referral to Eylam University Hospital, compared with victims admitted directly to Eylam University Hospital (Z = -1.89, p = 0.06). Median ISS for the group treated in Mehran before transferral was 9 with an interquartile range of 6-13; the group admitted directly had a median ISS of 9 with an interquartile range of 4-13.
The case mix was not identical. The group that received treatment in Mehran Clinic before transferral to Eylam University Hospital had a higher proportion of penetrating injury compared with victims brought directly to Eylam (85.4% vs 61.2%, 95% CI of difference 16.5-31.8%, p <0.0005).
Mortality
Total mortality was 10.3% (66/641) (95% CI 7.9-12.6%) and there was no significant difference between blunt and penetrating injury (8.2% vs 11%) (difference 2.8%, 95% CI of difference -7.9 to 2.4%, ns). When comparing mortality in the group that received treatment in the Mehran Clinic before referral to Eylam University Hospital with patients brought directly to Eylam (excluding the victims found dead at the scene) we found no difference (total mortality 36/611 or 5.9%, 5.5% the group treated in Mehran before transferral, 6.5% in the group brought directly to Eylam, 95% CI of difference -4.9% to 2.8%, ns). When considering mine injuries alone, the mortality was 20.7% (37/179) (95% CI 15.0-27.3%). Of these, 32 were dead when discovered and only 5 died during treatment, all before reaching the Eylam University Hospital.
Change in physiological function of victims after prehospital treatment
When considering all patients entering to the Mehran Clinic it was found that victims supported by first responders before arriving at Mehran had a PSS of 6.35 (95% CI 6.22-6.48) as compared with victims arriving at Mehran without first responder assistance en route to Mehran, who had a PSS of 6.29 (95% CI 6.06-6.52). There was no significant difference between the two groups (difference 0.07, 95%CI -0.19 to 0.32, ns).
The mean PSS at first assessment and at arrival in the Eylam University Hospital for the group that was eventually transferred to Eylam after being treated in Mehran Clinic is given (Table 3), and is compared with victims brought directly to Eylam. There was a significant improvement in PSS (mean improvement 1.11, 95% CI 0.98-1.24, p < 0.0005) during treatment and transportation, and the PSS at admission to Eylam University Hospital for these victims was higher than the group brought directly to Eylam University Hospital (difference 0.73, 95% CI of difference 0.55-.91, p < 0.0005) (Table 3).
Table 3: Physiological status of trauma victims at assessment in primary clinic and at admission to referral centre using the simplified Physiological Severity Score. All differences were significant
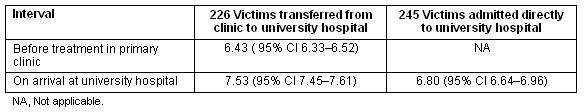
Time interval to admission
The time interval between the injury and admission to Eylam University Hospital was registered for 166 of the 226 patients transferred from Mehran to Eylam. The median time interval was 180 min, with an interquartile range of 120-270 min.
Discussion
This study shows that it is possible to use existing healthcare structures in rural areas to improve trauma care. By using the existing system of rural health workers an infrastructure was already in place with trained health workers in each village, and these were the backbone of the villager first-responder system.
Previous studies have indicated a mortality rate estimated at 36% after mine injuries1-3. The present study found a mortality rate of 21% after mine injuries, but with great variation among the years. The 2003 invasion of Iraq enabled thousands of people to cross the Iraq border for the pilgrimage to Kerbalah and Najaf, two holy shrines in Iraq for the Shia people. This unorganized crossing of the minefields in darkness at night resulted in a huge mortality, with most fatalities being discovered several days after their injury. As the first responders were not present in the otherwise forbidden military border zone, the impact of early basic life support could not be assessed in this setting.
The referral system for this area created an opportunity for cautious comparison of two similar but not randomized groups, because one group of injured were transported directly to Eylam University Hospital, while victims from the Mehran district received basic and advanced trauma care before reaching Eylam. Despite having a more severe physiological impact of injury, the group treated initially in Mehran and during transfer improved significantly in physiological function, assessed by the PSS, despite a delay from injury to final hospital admission of a median 3 hours.
Our 8 hour first-responder training did not result in any change in the PSS. Experience from similar training programs in Iraq11 suggests village first-responder training may need to be held over 2 days.
We also found no improvement in survival. The in-hospital mortality was low for both groups. The study was a training program, and the study time limit was set without prior knowledge of the number of victims who would be included, hence no power calculations could be performed in advance.
Variations in the spectrum of trauma were seen in the study period. Similar changes were seen in an Iraq study as well12. Although the training was designed for mine injuries, it seems to be suitable for caring for the victims of other injuries, and thus represents a strengthening of rural trauma care6. The cause of this change in injury panorama may be the changing conditions in society due to the pilgrimage. When the treatment system has strong local anchoring with medical leadership it seems to be able to accommodate such a change without compromised treatment quality12. The observational period of the present study did not allow for detailed assessment of treatment quality in different, changing trauma groups.
The present study may be limited by the use of a surrogate measure of physiological impact, the PSS, based on slightly modified variables as compared with the original RTS11. This modified PSS has been assessed in several articles previously with a high correlation to mortality5,10,12,13 and, thus, seems to be a reasonable and practical simplification of this measure. In addition, caution must be used in retrospectively comparing the outcomes of two patient cohorts. Given the impossibility of randomising such an intervention, the similarity of baseline data for each cohort in the present study gives confidence that this study's method was appropriate and useful for informing policy.
Conclusion
It was found that the existing rural healthcare system in Iran's western border area could be upgraded to care for mine victims and victims of other injuries mainly by using available resources. This system improved the physiological status of the victims during transportation, and was able to accommodate penetrating as well as blunt injury. The use of existing health structures should be considered when planning improvements.
Acknowledgements
The authors thank Torben Wisborg MD, PhD, Hammerfest Hospital, Norway, for his invaluable support and cooperation during the process of designing, implementing, auditing and reporting the program.
References
1. Jahunlu HR, Husum H, Wisborg T. Mortality in land-mine accidents in Iran. Prehospital Disaster Medicine 2002; 17: 107-109.
2. Andersson N, da Sousa CP, Paredes S. Social cost of land mines in four countries: Afghanistan, Bosnia, Cambodia, and Mozambique. BMJ 1995; 311: 718-721.
3. Ascherio A, Biellik R, Epstein A, Snetro G, Gloyd S, Ayotte B et al. Deaths and injuries caused by land mines in Mozambique. Lancet 1995; 346: 721-724.
4. Husum H, Gilbert M, Wisborg T. Training pre-hospital trauma care in low-income countries: the 'Village University' experience. Medical Teaching 2003; 25: 142-148.
5. Husum H, Gilbert M, Wisborg T, Van Heng Y, Murad M. Rural prehospital trauma systems improve trauma outcome in low-income countries: a prospective study from North Iraq and Cambodia. Journal of Trauma 2003; 54: 1188-1196.
6. Wisborg T, Murad MK, Edvardsen O, Brinchmann BS. Life or death. The social impact of paramedics and first responders in landmine-infested villages in northern Iraq. Rural and Remote Health 8: 816. (Online) 2008. Available: http://www.rrh.org.au (Accessed 17 November 2008).
7. Statistical Center of Iran. House and population census results - 1385. (Online) 2006. Available: http://www.sci.org.ir/portal/faces/public/census85/census85.natayej (Accessed 4 September 2007).
8. Husum H. Effects of early prehospital life support to war injured: the battle of Jalalabad, Afghanistan. Prehospital Disaster Medicine 1999; 14: 75-80.
9. Husum H, Gilbert M, Wisborg T. Save lives, save limbs. Penang, Malaysia: Third World Network, 2000.
10. Husum H, Gilbert M, Wisborg T, Van Heng Y, Murad M. Respiratory rate as a prehospital triage tool in rural trauma. Journal of Trauma 2003; 55: 466-470.
11. Champion HR, Copes WS, Sacco WJ, Lawnick MM, Keast SL, Bain LW Jr et al. The Major Trauma Outcome Study: establishing national norms for trauma care. Journal of Trauma 1990; 30: 1356-1365.
12. Wisborg T, Murad MK, Edvardsen O, Husum H. Prehospital trauma system in a low-income country: system maturation and adaptation during eight years. Journal of Trauma 2008; 64: 1343-1348.
13. Saghafinia M, Nafissi N, Mohabbi HA, Moharamzad Y. The Role of performing life support courses in rural areas in improving pre-hospital physiologic conditions of patients with penetrating injuries. Journal of the College of Physicians and Surgeons Pakistan 2008; 18: 538-541.
Abstract
Introduction: Iran has a major land mine injury problem in its border areas. Mine injuries have a high mortality and morbidity, and the injuries generally occur in remote areas. Iran has a well developed system of rural health workers and clinics, covering most border areas. These have mainly had prevention, immunization and curative treatment for medical conditions as their focus. We hypothesized that adding a short training in trauma care to the already existing system of rural health workers would improve the care for trauma victims. The objective of the present study was to describe the training and evaluate its effect using mortality and change in physiological function of victims after prehospital treatment as outcome measures.
Methods: The training was arranged in villages and clinics in the border area. Physicians, nurses and emergency technicians from a local emergency clinic, the Mehran Clinic, were given a two-day course with monthly refreshers; while rural healthcare workers and lay people were given shorter training courses in their villages. All patients treated were registered and patients were followed up. Physiological changes after treatment was assessed with a modified three-component 'revised trauma score'. Patients entered the system directly through the local emergency clinic (some with prehospital treatment before arriving at the local emergency clinic). Some were transferred to the referral university hospital, and there they could be compared with a convenience comparison group of patients transported directly to the referral university hospital without treatment during transportation.
Results: During the three-year study period 109 physicians, nurses and 76 emergency technicians (behwarses) were trained, while 4649 lay persons had first-responder training. A total of 366 patients were treated by the system. Prehospital support was given to 238 victims before admission to the primary clinic. We found no difference in mortality between patients with and without first-responder treatment. In all, 226 of these patients were transferred to the university hospital. During the period a group of 245 other victims of injury was admitted directly to the university hospital. The physiological status of the transferred victims improved significantly by treatment from the emergency clinic to the university hospital with a mean improvement in the Physiological Severity Score (PSS) of 1.11 (95% CI 0.98-1.24). The PSS of the intervention group was significantly higher than the status of the group brought directly to the university hospital without treatment during transportation (difference 0.73, 95% CI difference 0.55-.91, p < 0.0005).
Conclusions: We found that the existing rural healthcare system in Iran's western border area could be upgraded to care for mine victims and victims of other injuries by using available resources. This system improved the physiological status of the victims during transportation, and was able to handle penetrating as well as blunt injury. The use of existing health structures should be considered when planning improvements.
Key words: Iran, land mines, quality improvement, rural trauma, team work, trauma, trauma care.
You might also be interested in:
2017 - Health care in high school athletics in West Virginia


