Dear Editor
Complementary medicine (CM) therapies and products, such as acupuncture, massage, prayer, vitamins, herbs, and diet programs, are widely used by patients as an adjunct to primary care. Predictors of CM use are complex, and include socioeconomic characteristics, clinical conditions and type of CM therapy used1,2. It is not yet clear if rural patients use the same amount of CM, or use similar CM therapies, to those of urban patients. In a preliminary study, we compared CM use among rural and urban family medicine patients in the predominantly rural region of west central Indiana.
Incoming patients at three family medicine clinics in western Indiana (Clay City Center for Family Medicine, Worthington Family Medicine, Union Hospital Family Medicine Center in Terre Haute) were invited to participate in this study. Clay City and Worthington are small rural communities (population of 1000 and 1500, respectively), located 30-50 miles from an urban center, Terre Haute (population 57 000). At each site, participants completed a 'complementary medicine use survey', which examined patient use of 20 different CM therapies. Responses from the rural and urban populations were compared with the Pearson's χ2 test using a significance level of 0.053. Local availability of CM practitioners and products within each community was determined by: (i) inquiring at each clinic whether certain services were available; (ii) examining the vitamin/herb/supplement sections of local pharmacies and grocery stores; and (iii) examining the business directory in the local phone book.
Both rural and urban populations showed substantial use of chiropractic care, diet programs, lifestyle diet, massage, simple home remedies and vitamins (Table 1), followed by faith/ prayer healing, reflexology and relaxation techniques. The rural population used significantly less acupuncture (11% vs 28%, p<0.01), less herbal medicine (33% vs 56%, p<0.01), less osteopathic manipulation (16% vs 31%, p<0.01), and less yoga (9% vs 19%, p<0.05).
Table 1: Percentage of types of complementary medicine therapy used (rural vs urban)
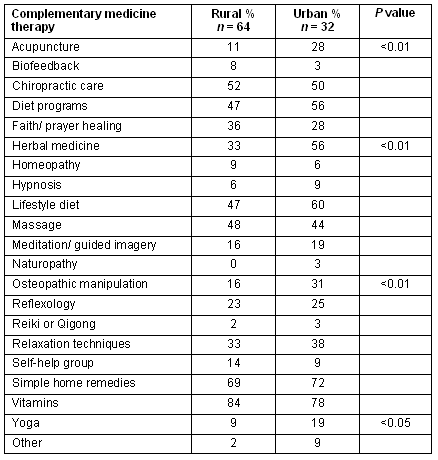
Our results show similar usage for 16 out of 20 CM therapies among rural and urban family medicine patients in western Indiana. Significant differences between the two groups were limited to acupuncture, herbal medicine, osteopathic manipulation and yoga. To understand these differences, we did a post-hoc analysis of CM availability at the rural and urban study sites. At the Union Hospital Family Medicine Clinic, one physician was board certified in medical acupuncture, and another, an osteopathic physician, included manipulation in his practice, so these therapies were readily available to our urban but not to our rural populations. Herbal medicine, another CM therapy with a significant rural-urban difference, is widespread and abundant in pharmacies and supermarkets in Terre Haute, but not in Clay City and Worthington. Chiropractic practitioners were widespread and accessible to both groups, possibly explaining the lack of difference in the use of this therapy.
In a rural family practice clinic in northern Pennsylvania, Del Mundo et al.4 observed that patients are more likely to use a CM therapy if it is locally available. However, Nichols et al.5 found that local availability was not a critical factor in care-seeking behavior among rural residents in North Dakota and Montana, and that, 'rural residents traveled significant distances [average of 25 miles] to visit the naturopathic provider who met their needs'. Our results suggest that CM use by rural patients may depend, in part, on local availability of providers and products.
Margaret Moga, PhD
Barbara Mowery, MD
Roy Geib, PhD
Indiana University School of Medicine
Indiana, United States of America
References
1. Palinkas LA, Kabongo ML. The use of complementary and alternative medicine by primary care patients: A SURFNET study. Journal of Family Practice 2000; 49: 1121-1130.
2. Barnes PM, Powell-Griner E, McFann K, Nahin RL. Complementary and alternative medicine use among adults: United States, 2002. Advance data 2004; 343: 1-20.
3. Munro BH. Statistical methods for health care research, 5th edn. Philadelphia: Lippincott Williams & Wilkins, 2005.
4. Del Mundo WFB, Shepherd WC, Marose TD. Use of alternative medicine by patients in a rural family practice clinic. Family Medicine 2002; 34: 206-212.
5. Nichols E, Weinert C, Shreffler Grant J, Ide B. Complementary and alternative medicine providers in rural locations. Online Journal of Rural Nursing Health Care 2006; 6: 40-46.


