Dear Editor
One of the difficulties inherent in studies of physician origins is that data is often collected at different points in time. Some studies use birth data, other studies use high school data, others use length of time in a particular geographic area.
Differences in origins are important to understand because major data sources have different measures of origins. The most extensive source of data is the American Medical Association Masterfile and birth origins can be coded for 95% of United States allopathic medical students1. High school location data is nearly 100% available from medical school admission materials that are also collected nationally by medical education associations. The Masterfile is the best secondary source of career and location outcomes, but it does not include high school location data. Admission databases have no career or practice location data. Studies need to compare birth origin data with high school data to allow some understanding of the geographic differences present in the two background measures.
Birth origins and high school locations for Nebraska medical school graduates were compared using simple distance measures in miles, rural-urban commuting area (RUCA) coding2 of birth city compared with high school city, and comparisons of geographic locations (instate, geographic type). The four main geographic types in RUCA coding are urban/urban focused, large rural, small rural, and isolated rural. The city origins listed are coded using the RUCA system.
Table 1: Comparison of birth city with high school city location for 1996-2005 matriculants of the University of Nebraska Medical Center (UNMC)
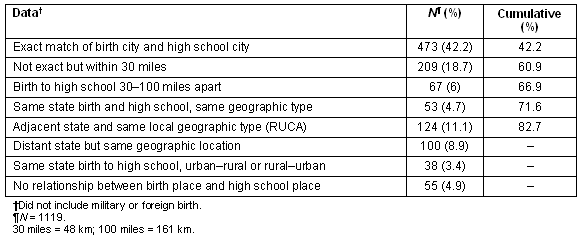
Birth city and high school city were exact matches for 42.2% or 473 of the 1119 students. Approximately 61% or 682 of the admitted students shared either exact place location or a 30 mile (48 km) radius for experiential place. It is common for rural children in Nebraska to attend high school in a location within 30 miles due to school district consolidations. A cumulative 67% graduated from high school within 100 miles (161 km) of birth. The similarities across origins increased to 71.6% with the addition of same state and same geographic location for birth and high school (urban to urban, rural to rural). Another 11.1% had the same urban or rural geographic location but in an adjacent state (all similar to Nebraska) for 82.7%.
This 82.7% is the best representation of same or similar origins. The foreign born component was not included in this study. Including this component would increase same or similar past 87%, because urban birth and high school locations are the rule in foreign born medical students, even though the transition over time involves a geographic change to another nation.
Using a RUCA coding with four levels of geographic coding (urban, large rural, small rural, isolated) 72.4% matched up exactly to the same geographic coding for birth and for high school.
Only approximately 5-15% of medical students were completely different using various geographic measures.
Similarities in birth and high school location allow either measure to be used in studies. Radical movements to very different types of geographic locations that might impact on studies were minimal.
There are strengths and weaknesses of using Nebraska medical students and geographic locations. States such as Nebraska do tend to have less mobile populations and this can reduce birth to high school movement. Mobility is greater in urban populations, but the change is unlikely to interrupt the overall birth to admission place shaped by parents, who are usually highest status or professionals and choose similar urban locations over time.
Future studies will continue to explore origins across the dimensions of admission probability, career choice, and practice location. One area in particular will be important to examine. Using longer term data and the birth origins in the Masterfile, the 1987-2000 medical school graduates who were born within 50 miles (80 km) of the two major metropolitan locations in the state had career and location choice decisions closer to those of physicians born in Omaha or Lincoln. This was not expected because these were towns coded as 'small rural' in the RUCA system (Seward, Blair, Nebraska City, Crete, Plattsmouth, Wahoo). These rural origin graduates born near major metropolitan areas were found in family practice careers and in rural locations at rates similar to urban-origin physicians. The physicians born in Nebraska small rural locations more than 50 miles away from major metropolitan areas (Fairbury, West Point, Holdrege, Aurora, McCook, Alliance, Wayne, Chadron) had the typical increased rural practice and family practice career decisions seen in rural-origin physicians. Newer geographic coding methods may need to extend the concepts of adjacency developed by Calvin Beale to aid in understanding career and location choice.
Other rural areas in the US adjacent to urban locations are transitioning to suburbs. Elkhorn was a small town just northwest of Omaha that was recently annexed into Omaha. Elkhorn did not register a single Nebraska medical student birth in the 1996-2005 matriculants. However, rapid growth resulted in 25 Elkhorn high school graduates becoming UNMC medical students (with more likely to be admitted to other medical schools). Of this 25, 18 were of large metropolitan birth (16 from nearby Omaha), four were of small rural birth, and three were from large rural birth. The 'new' rural origin admissions from rural-located suburbs or from locations within 50 miles of major metropolitan areas may not contribute the same rural workforce, especially with fewer family physicians who have triple the rural distribution rates.
Acknowledgement
The author would like to acknowledge the University of Nebraska Medical Center Admissions Office for assistance.
Robert C Bowman
Co-North American Regional Editor
Rural and Remote Health
References
1. Medical Marketing Service I. AMA Physician MasterFile. (Online) 2005. Available: www.mmslists.com (Accessed 1 July 2005).
2. Rural Health Research Centre. Rural-urban commuting area codes. Available: http://depts.washington.edu/uwruca/ (Accessed 13 October 2008).
