Introduction
There has been sufficient documentation to establish that the public health infrastructure in the USA is deteriorating throughout all geographic regions. Healthy People 2010 identifies public health infrastructure (Focus Area 23) as one of 28 necessary focus areas to achieve the two overarching HP 2010 goals, to: (i) increase quality and years of healthy life; and (ii) eliminate health disparities1. While there has been a fair amount of research and discussion about general public health infrastructure issues, little attention has been given to the rural dimensions of this topic2. The special issues and considerations of rural communities are often overlooked or underestimated.
The vast majority of the USA is rural. According to 2000 US Census data, 2292 counties (72.9%) out of a total of 3141 counties within the USA are designated as rural3. Eighty-three percent of the nation's land is in a rural area; 25% of the nation's population resides in a rural area. Rural communities confront challenges and limitations not faced by urban communities that affect the manner in which they are able to prevent, serve and respond to public health needs. A large number of these rural areas lack adequate health resources and are designated as health professional shortage areas (HPSAs) and/ or medically underserved areas (MUAs).
According to the landmark Institute of Medicine report4, 'no citizen from any community, no matter how small or remote should be without identifiable and realistic access to the benefits of public health protection...' (p.144-5). However, rural citizens experience significant health disparities5. Rural communities face geographical, personnel, infrastructure, and funding challenges and many have no formal public health or healthcare infrastructure. Local health departments, where they do exist, have less capacity and fewer resources. According to Hajat, Stewart, and Hayes, a greater proportion of rural local public health agencies (72%) list budget restrictions as a barrier to obtaining needed staff, and a higher percentage (29%) of rural respondents indicate difficulty in attracting candidates to their geographic, area compared with metropolitan Local Public Health Agencies (LPHAs) and suburban LPHAs6. The challenge of maintaining, let alone strengthening, a public health workforce is greater in rural areas than urban centers because of a variety of issues including location, educational opportunities, and financial constraints that impact on recruitment and retention of personnel7,8. Further, the public health workforce in rural and urban areas is aging and retiring, but this is particularly so for public health nurses who provide the majority of care in rural areas9. This lack of formal public health infrastructure and trained public health professionals has a deleterious impact on rural populations.
Public health systems are defined as 'a complex network of individuals and organizations that have the potential to play critical roles in creating the conditions for health'10 (p.28). Historically, rural communities have had to supplement public health services with the broader public health system, such as community health centers, rural health clinics or emergency medical service providers, where they exist, functioning as primary sources of care. Due to the lack of formal public health infrastructure and trained professionals in rural areas, this broader system is critical. The broader public health system workers are found not only in local health agencies, but also in other public, private and non-profit organizations and agencies concerned with the public's health7. These agencies and organizations in rural areas encompass more diverse professions not usually considered part of the traditional public health workforce, including: Head Start personnel, school nurses, zoning and planning personnel, community health center staff, community hospital workers, veterinarians, dentists, social workers, tribal council members, long-term care workers, home health personnel, Agency on Aging staff, community action group members, Cooperative Extension personnel, and church members and employees8.
Rural communities may differ significantly across geographic regions and even within the same region. This diversity of rural communities necessitates local solutions to local challenges8. Increasingly, systems approaches that improve community relationships, strengthen social networks and expand connectivity are being used to increase community planning efforts and strengthen public health capacity, which ultimately lead to community collaboration, planning, action and improved health status through sustainable community efforts. The 2002 edition of the Institute of Medicine report calls for a renewed exploration and strengthening of partnerships with the local medical community, voluntary services community, media, businesses and industry, and academic institutions necessary to have an active and robust public health system10. Consequently, it is imperative that the broader rural public health system collaborates locally toward a common goal of improving existing rural public health capacity and the health of rural residents.
The authors acknowledge that numerous models and approaches exist that engage and organize communities around community-identified problems and solutions. The purpose of this article is to: (i) suggest a strategy regularly used by the authors that encourages relationship building and serves as a catalyst for rural communities to work together to initiate and make changes based on the local assets and dynamics; (ii) provide a descriptive overview of this strategy; and (iii) provide an illustrative case in which this strategy has been used.
Background
The Texas A&M Health Science Center, School of Rural Public Health has pioneered a Rural Health Roundtable (RHR) strategy that has demonstrated effectiveness in engaging a target audience in a rural community or communities; identifying local strengths and resources, existing relationships and gaps within the current system; distinguishing the broader, non-traditional rural public health system and additional stakeholders; identifying and educating local decision-makers; and working together to address a specific rural health issue. This strategy has been used successfully in a number of venues to elicit a wide variety of outcomes including improving local emergency preparedness, bioterrorism and pandemic influenza planning; developing networks of interested health professionals working in the HIV/AIDS arena; initiating local capacity building processes; facilitating dialog to identify local resources and access issues; and identifying coalition building, obesity prevention and rural disaster planning best practices and success stories. Figure 1 provides an RHR graphical overview, illustrating stakeholders and outcomes for rural community emergency planning.
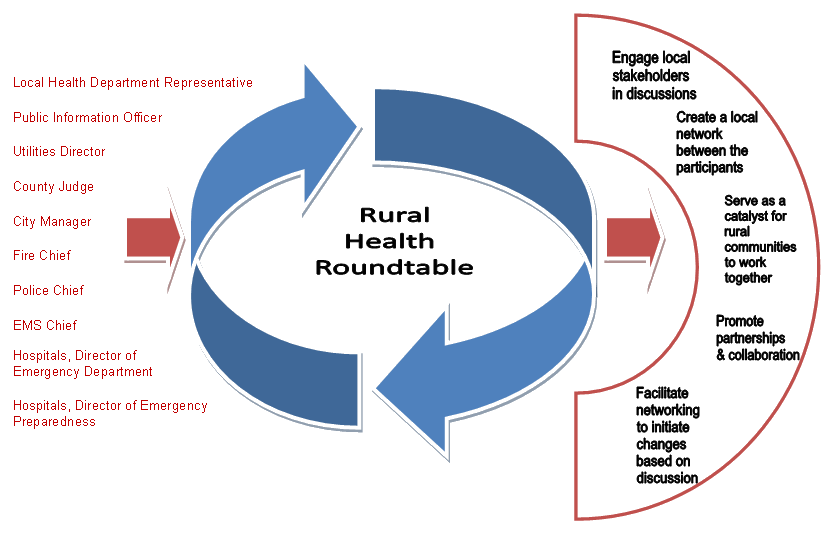
Figure 1: Rural community emergency planning using the Rural Health Roundtable strategy.
The purpose of the RHR is to engage local stakeholders in a face-to-face discussion about a particular public health issue. This informal, facilitated discussion endeavors to create a local network between the participants and is neither a needs assessment nor a focus group. The Roundtable strategy lends itself to replication and application in rural communities for various public health issues.
The illustrative case for using this strategy will be provided around rural community emergency planning. Given the lack of formal public health infrastructure, rural communities are dependent on non-traditional partners and volunteers in preparedness planning and response. According to Nelson, Lurie, Wasserman, & Zakowski, 'responsibility for the preparedness of the nation's communities lies not only with governmental agencies but also with active, engaged, and mobilized community residents, businesses, and nongovernmental organizations' or the broader public health system11 (p.S9).
Methods
The subsequent methodology for the RHR planning process is not chronological in nature; planning occurs concurrently.
Topic and target questions
A specific, relevant public health topic is identified for the roundtable discussion. Pre-determined, discussion-stimulating questions are used to guide the discussion. Although the discussion will differ according to each group, these questions are interrelated to ensure redirection of straying discussions. The discussion questions are designed to:
- identify local strengths and assets (local resources)
- identify existing working relationships and partnerships
- identify what is currently in place regarding the topic
- identify best practices or success stories
- identify gaps or holes in existing system or services regarding the topic
- identify training, learning and skill needs of stakeholders to enhance local capability and participants' preferred methods for learning
- identify the extended public health network and who else should be at the table regarding the topic
- collectively identify one focus issue (pick low hanging fruit) which can be addressed and develop a plan of action to allow multidisciplinary collaboration
- identify three activities that each participant would like to accomplish in their community within the next month.
Audience identification
Because the broader public health system is needed to supplement public health and healthcare services in rural populations, it is necessary to identify appropriate stakeholder categories. The stakeholder categories include those disciplines within the broader public health network that are involved in providing services or are responsible for the public health topic of interest. Stakeholder categories will vary depending on the health topic. Within the community or communities participating in the RHR, individual stakeholders are selected, by name, to take part in the Roundtable discussion. Various resources and local, regional and state contacts are utilized to identify individual stakeholders. It is preferable that a central location within the community or among communities is selected to convene the Roundtable for convenience, as well as being a neutral site that encourages participants to share openly. Before selecting a date, it is helpful to contact key community stakeholders to ensure no conflicting meetings or activities are scheduled for tentative dates.
'Cold calls' are made by telephone to potential participants to explain that the RHR is a two-hour, facilitated discussion, typically held over lunch; to extend an invitation to participate in the Roundtable; to determine their interest; and to receive referrals of other local stakeholders who should be invited to attend. Attempts are made to obtain a balance in the representatives present, so the Roundtable discussion is not too heavily weighted for any one discipline, community or organization.
Ensuring attendance
After contacting potential participants by telephone, formal invitations are mailed to those indicating interest, with a request to RSVP. Including a map and directions to the RHR site is helpful. All stakeholders who were previously mailed an invitation are phoned again prior to the Roundtable to confirm their attendance and to obtain a lunch order. This call further encourages their attendance because the participant has made a 'commitment' to a meal that will be ordered specifically for them.
Rural health roundtable discussion
On the day of the Roundtable, stakeholders arrive at the site, sign-in, fill out a contact information form and pick up their lunch. Approximately 15 min are allowed for participants to get settled, begin eating and converse with other participants. This creates an informal, social environment and helps encourage open dialogue and discussion once the Roundtable begins. The facilitator extends a welcome, describes the purpose of the RHR and invites participants to make self-introductions. The dialogue begins with the facilitator asking the target questions to guide the discussion. An individual other than the facilitator records detailed, hand-written notes.
On conclusion, participants are told the information they discussed will be used for local planning and incorporated into materials or upcoming events hosted for them by the facilitating organization. To promote collaboration and problem solving using existing assets, the group collectively identifies a local issue and develops a plan of action to address this issue. Following the Roundtable, all participants are instructed to complete a process evaluation to provide the facilitating organization with feedback and recommendations and to learn of three activities participants would like to accomplish in their communities within the months following the Roundtable.
Follow up
Communication: It is imperative that the facilitating organization continue communication with the RHR participants and nurture the relationships once the RHR has concluded. The facilitating organization can maintain contact by offering current information and resources, opportunities for collaboration, technical assistance and notification of upcoming events, such as continuing educational activities. Continuing education opportunities may include those offered by the facilitating organization or other activities available throughout the region or state. Continuing education activities and other events can be used as tools to connect rural stakeholders throughout the state or region who have similar interests. These activities and events provide additional opportunities for stakeholders to work together and continue to expand their existing network.
Evaluation: A follow-up evaluation may be conducted to identify and assess changes made in the community to ameliorate the selected public health issue. Detailed, specific notes taken at the Roundtable reflect the qualitative information conveyed by the participants. Notes are compiled and arranged by topic, extricating common themes, proposed participant solutions to address concerns or gaps, and best practices or success stories. This information establishes baseline data that can be compared with data collected during a follow-up evaluation or Roundtable discussion.
The baseline data is used to identify and assess change that occurred between the initial roundtable discussion and follow up. Evaluation measures include:
- Are more and different strengths and assets identified?
- Are relationships stronger? Are networks denser?
- Are communities improving, expanding, and/ or creating new best practices?
- Are communities resolving the gaps or holes indicated at the initial Roundtable discussion?
- Are learning and skill needs being met? Have stakeholders sought out and attended educational and skill building activities?
- Are necessary stakeholders involved who were not previously involved? Did the larger group of stakeholders become part of the broader public health network?
- What progress has been made in the three activities identified individually?
- What advancements have been made in the one area collectively identified by the group?
- Has the group held additional meetings, developed a coalition, hosted community activities etc to address the public health issue?
Results
The RHR strategy can result in short-term, intermediate and long-term outcomes using various evaluation tools, such as process evaluations and qualitative comparisons based on the roundtable discussions. While no formal quantitative evaluations have been conducted for this methodology to attest to its effectiveness in impacting the long-term health of participating communities, future plans exist to quantify existing qualitative data and to conduct social network analyses to graphically illustrate increases in network or partnership development.
Short-term outcomes
One short-term outcome of the Roundtable process is an information exchange among community stakeholders. The discussion results in the sharing of current activities and efforts, resources available locally or regionally, and gaps in community planning and in the broader public health system. The Roundtable discussion reflects the services, responsibilities and existing issues of attending organizations and agencies, as well as the collective assets available to promote partnerships and collaboration, and makes changes based on the issues discussed. The Roundtable generates qualitative summaries of the discussion, with common themes, proposed participant solutions, lessons learned and best practices or success stories. The Roundtable discloses and provides suggestions for issues in which the community or communities are contending and initiates further discussions, activities or the development of resources to accurately reflect comments.
Roundtables can also serve as a forum to promote educational and training opportunities. There is a general consensus that rural public health workers lack formal training in the concepts and principles of public health. According to the Center for Disease Control's Public Health's Infrastructure report, 78% of local health department personnel did not graduate with public health degrees12. Reaching out to these rural stakeholders, through the RHR, and notifying them of and encouraging participation in continuing education opportunities, results in a better educated and trained rural public health workforce and increased knowledge, skills and abilities to manage public health issues. Further, the Roundtables serve as an opportunity to reach out to the expanded, non-traditional rural public health system to increase their awareness and knowledge of public health issues.
Intermediate outcomes
The intermediate outcomes of the Roundtable discussion include it serving as a catalyst to build stakeholder networks in rural communities, facilitating a broader and more inclusive ongoing dialogue, and enhancing communication to evolve the local network that will continue once the facilitating organization leaves. Local groups are empowered to take ownership, plan and problem solve with existing assets. Roundtable participants begin making actual changes in their community, such as seeking out information, holding meetings, developing coalitions, hosting community activities and involving other stakeholders to address the public health issue.
Long term
While smaller communities have limited resources available, rural community stakeholders consistently indicate that their single greatest local resource is the people in the community. Based on the issues discussed, stakeholders begin working together as team to initiate changes that can impact on the long-term health of their community. Follow-up evaluations and assessments can determine the effectiveness of the Roundtable methodology and subsequent community activities and efforts by identifying and measuring both process and outcome changes that occur over time.
Illustrative case
The Rural Ready Communities (RRC) project was created to help ensure that community health centers, rural health clinics and emergency medical service providers in non-hospital Texas counties have an emergency plan that can be integrated with other local planning efforts. During the project period there were 65 counties in Texas without a hospital. Figure 2 shows the counties in Texas without hospitals and the type of health system provider within those counties. Twelve RHR were convened with broad groups of local stakeholders to form networks for integrated planning, to identify and share rural emergency planning common themes and best practices, and to develop an emergency planning guide, based on these discussions, for rural healthcare systems. While the focus of this article is on the Roundtable strategy, the RRC project also included development of the rural community emergency planning guide, an advisory committee to provide project guidance and support, and a year-end statewide workshop to introduce and instruct participants using the planning guide.
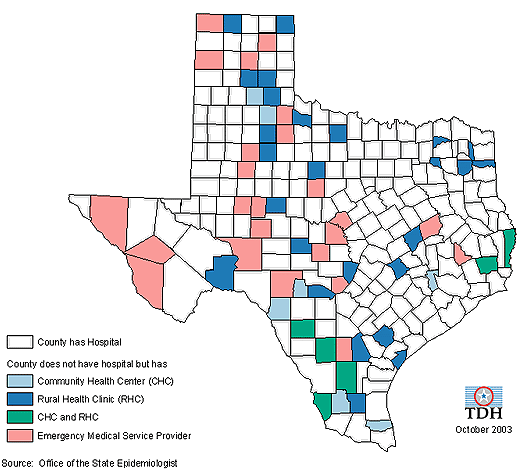
Figure 2: Texas Counties without hospitals.
Short-term outcomes
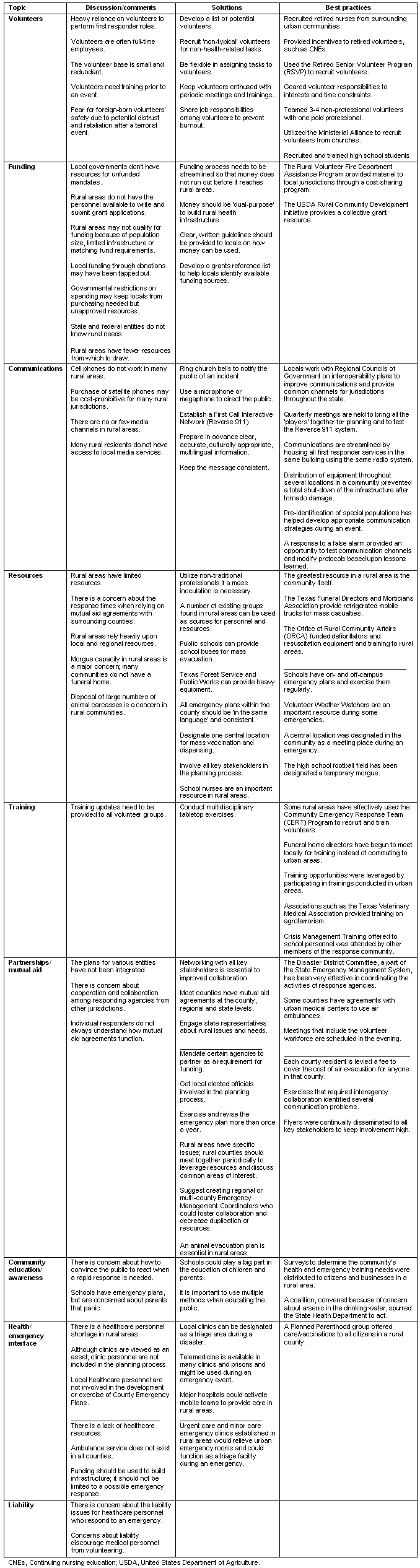
The total attendance for the RHR in the RRC project was 215 attendees from 59 Texas counties with an average of 17.9 attendees per roundtable. Table 1 illustrates the variety of RHR stakeholder attendee categories involved in improving rural community emergency preparedness planning. The RHRs generated qualitative summaries of the discussion, with common themes, proposed participant solutions, lessons learned and best practices or success stories. These thematic categories included volunteers; funding; communications, both between first responders and other rescue workers and with the public; resources; training; partnerships and mutual aid agreements; community education and awareness; interface between health and emergency personnel/ systems; and liability. Table 2 further conveys the RHR discussions in terms of the common themes, proposed participant solutions and best practices identified, but this listing is by no means comprehensive. For the purposes of this article, best practices are loosely defined as participant-identified activities or methods that were successful in their community. The information provided by RHR participants enabled the creation of a rural emergency planning guidance document.
Table 1: Disciplines represented at Rural Health Roundtables for the Rural Ready Communities Project

Table 2: Rural Health Roundtables: common themes, proposed participant solutions and best practices
Because there is a general consensus that rural public health workers lack formal training in the concepts and principles of public health, the Roundtables also served as a forum to promote educational and training opportunities. The Roundtable was used as an opportunity to increase the awareness and knowledge of public health issues within the broader rural public health system, and to promote the statewide conference that would introduce and explain use of the planning guide.
Intermediate outcomes
In an attempt to learn more about the impact of RHRs in the RRC project, an evaluation tool to measure intermediate outcomes was created and mailed to 178 RHR participants, 7-9 months subsequent to the RHRs. Ninety-two evaluations were returned, a response rate of 51.7%. The evaluation was conducted to learn about the perceived benefits of RHRs and the types of activities in which Roundtable participants had engaged after the Roundtables. Eighty-five percent of the Roundtable participants perceived the RHR as having long-term benefits for their community and/ or organization. Roundtable participants indicated that the following took place as a result of participating in the RHRs:
- 65% met an individual at the Roundtable whom they had not previously known
- 30% contacted an individual after the Roundtable to discuss emergency preparedness
- 53% met with others in their county
- 27% met with others in surrounding counties
- 28% held a collaborative meeting to discuss emergency preparedness and response
- 23% practiced their plan using a drill or tabletop exercise
- 49% participated in local planning activities
- 37% raised community awareness or provided emergency preparedness public education
- 14% held education and/ or training activities
- 37% attended other trainings, conferences or emergency preparedness related events
- 29% increased community involvement
- 54% shared information within their county
- 33% shared information among other counties
- 39% involved other organizations, agencies, or individuals in planning
- 39% involved clinics or emergency medical services in their county in the planning process
- 20% entered into Mutual Aid Agreements with other counties, organizations, and/ or agencies
- 11% formed a coalition for rural community emergency planning
- 24% inventoried emergency and health provider resources in their county
- 34% inventoried emergency equipment, supplies, or other items
- 19% purchased items/ equipment to assist in emergency planning or response
- 28% sought out healthcare resources available in their county
- 32% increased volunteer participation
- 27% addressed a specific topic(s) of concern.
Discussion
The RHR, using the methodology discussed above, has demonstrated its value as an effective tool in working with rural communities. Initiated in 1999, the methodology has been refined and enhanced over the past 8 years to more effectively reach stakeholders, ensure attendance and participation, promote sharing and discussions, build stakeholder networks and encourage continued communication and collaboration.
Rural community members are generally considered the communities' most valued asset. Through their close relationships, well-developed networks and shared experiences, rural residents bring a great deal of strength and resiliency to their communities. Because the community as a whole depends on each other for the common good, residents hold one another accountable and are willing to spend their free time helping the community through volunteer activities associated with community schools, churches, and service organizations.
Rural communities have fewer human and financial resources and residents cannot necessarily rely on, or have access to, public health and medical professionals to assume planning responsibilities. Using the RRC project as an illustrative case, rural community members must be the driving force in not only developing emergency response plans, but also in continually updating plans, tapping into existing planning structures, exercising plans and sustaining the interest and commitment of those involved. The accountability and interdependence mentioned previously helps facilitate and advance the planning processes. Many rural residents fill multiple roles through various volunteer and elected positions, serving on committees, and assisting in community projects. These shared associations may help facilitate better collaboration and cooperation among the segments of the community. Common membership in organizations such as parents teacher association/parent teacher organization, faith-based organizations and committees, athletic leagues, and civic organizations, encourages communication and the dissemination of information throughout the community. Key stakeholders, or those known for 'getting things done', are easily identified in rural communities and this designation carries with it a credibility that allows the key stakeholders to lead, delegate and/or accomplish necessary tasks.
Members of rural communities are often required to be particularly creative when addressing emergency preparedness issues due to lack of local resources. With fewer resources at their disposal, rural communities have learned to identify and utilize their unique strengths to overcome resource deficits when responding to emergencies and natural disasters. Rural communities have coped effectively with disasters in the past and have used the lessons learned to prepare for the challenges of responding to new types of emergencies and public health threats.
Limitations
Several limitations exist for this strategy. There are geographic limitations in that this strategy has only been utilized in rural communities in Texas, South Dakota and Maine, USA. Efficacy depends on several other factors, including consistencies in methodology and staffing, characteristics of participating community stakeholders, continued communication and readiness of communities to address specific public health issues. No formal quantitative evaluations have been conducted for this strategy to attest to its effectiveness in impacting the long-term health of participating communities. Initial qualitative results indicate an expansion of local networks, improved collaborative planning and increased community activities, efforts and information sharing. Additionally, the RRC project was funded by the Texas Department of State Health Services (DSHS) Hospital Preparedness Program. However, during this time period, Centers for Disease Control and Prevention Public Health Preparedness and Department of Homeland Security funding were also available at the state, regional and/or local levels. The resulting activities cannot necessarily be attributed solely to this project and participation in the RHRs.
Conclusion
Through the RHRs, rural residents gained an understanding of the vital role of community members in planning and response efforts; the importance of collaborative, multidisciplinary planning and response procedures and practices; and the existence of shared strengths and resources to enable the protection of life and property. Ultimately, it is a community effort with community-wide involvement that will enable rural areas to successfully face the challenges of planning for and responding to all public health emergencies.
It will be the responsibility of public health professionals to effectively shape the programs and policies needed to improve population health during the coming century10, which should occur at the federal, state and local levels. The Roundtable brings together the broader, non-traditional rural public health system in face-to-face discussions to jointly identify and address local public health issues and the local dynamics that affect these issues. Rural Health Roundtables can create linkages among rural stakeholders, as well as between rural community and other local, regional and state planning efforts, activities and resources. It serves as a catalyst of change for communities to improve their health, to prepare them for the unknown, and to strengthen or create networking among neighboring communities. The RHR strategy has significant potential for replication and application to all areas of rural public health.
Acknowledgements
Funding for the Rural Ready Communities project was provided by the Texas DSHS. Special thanks to the DSHS Hospital Preparedness Program and the Texas Health Institute (formerly the Texas Institute for Health Policy Research) for their collaboration on this project.
References
1. US Department of Health and Human Services. Healthy People 2010, 2nd edn; vol II. Washington, DC: US Government Printing Office, 2000.
2. National Advisory Committee on Rural Health. Rural Public Health: Issues and Considerations: A Report to the secretary, US Department of the Health and Human Services. National Advisory Committee on Rural Health, 2000.
3. US Census Bureau. US Census Bureau home page. (Online) 2000. Available: www.census.gov (Accessed 13 November 2008).
4. Institute of Medicine. The Future of Public Health. Washington, DC: National Academies Press, 1988.
5. Ricketts TC. Rural health in the United States. New York: Oxford University Press, 1999.
6. Hajat A, Stewart K, Hayes K. The local public health workforce in rural communities. Journal of Public Health Management Practice 2003; 9(6): 481-488.
7. Quiram B, Meit M, Carpender K, Pennel C, Castillo G, Duchicela D. Rural public health infrastructure: a literature review. In: L Gamm, L Hutchison (Eds). Rural Healthy People 2010: A companion document to Healthy People 2010, vol 3. (Online) 2005. Available: http://www.srph.tamhsc.edu/centers/rhp2010/Volume_3/Vol3Ch5OV.pdf (Accessed 14 November 2008). College Station, TX: The Texas A&M University System Health Science Center, School of Rural Public Health, Southwest Rural Health Research Center, 2008.
8. University of Pittsburgh, Center for Rural Health Practice. Bridging the health divide: the rural public health research agenda. (Online) 2004. Available: http://www.upb.pitt.edu/uploadedFiles/About/Sponsored_Programs/Center_for_Rural_Health_Practice/Bridging%20the%20Health%20Divide.pdf (Accessed 14 November 2008).
9. Health Resources and Services Administration (US). The public health work force enumeration 2000. New York: Center for Health Policy, Columbia University School of Nursing, 2000.
10. Institute of Medicine. The future of the public's health in the 21st century. Washington, DC: National Academies Press, 2002.
11. Nelson C, Lurie N, Wasserman J, Zakowski S. Conceptualizing and defining public health emergency preparedness. American Journal of Public Health 2007; 97: S9-S11.
12. Center for Disease Control and Prevention. Public health's infrastructure: every health department fully prepared; every community better protected, a status report. (Online) 2001. Available: http://www.uic.edu/sph/prepare/courses/ph410/resources/phinfrastructure.pdf (Accessed 14 November 2008).
