Introduction
Numerous studies have examined healthcare use at the end of life. A key issue of many of these studies is whether people died in acute-care hospitals or alternate settings, such as at home, in a hospice, or in a nursing home1-12. In such studies, the proportion of hospital deaths is typically used as an indicator of a potentially inappropriate care setting at the end of life8,9. This is particularly the case for certain terminal illnesses, notably cancer, where great advances have been made in the last few decades in providing more comfort-oriented (palliative), as opposed to cure-oriented care in appropriate settings, such as at home, in hospices or specially designated palliative care units in hospitals.
Besides examining the location of death per se, transitions into acute-care settings at the end of life, such as in the last one or 6 months before death10, have also been used to reflect inappropriate care settings as individuals are approaching death. Although many hospitalizations are appropriate, transitions into acute-care settings at the end of life may also indicate medicalization of the dying process. Moreover, any care-setting transition at the end of life can be stressful, suggesting this is an issue worth examining13,14.
Studies of whether transitions into hospital differ between rural and urban settings have yielded inconsistent results. Two Canadian studies (both conducted in Nova Scotia) showed that rural cancer patients were more likely to die in hospital than their urban counterparts4,15. However, a study conducted in Italy showed a greater proportion of home deaths occurred in rural areas8. The Italian study also demonstrated that such overall patterns can mask more specific regional effects, for living in certain rural regions was associated with an increased likelihood of dying in hospital8.
One reason for these discrepant findings may be differences in local health systems, including the availability of healthcare resources. Research shows, for example, that the likelihood of hospital death is increased among residents of areas with more available hospital beds16-18. Depending on how available health service resources are in rural versus urban areas, differing transition patterns would, therefore, emerge.
The disadvantages in accessing health care services experienced by those in rural areas is well established. For instance, hospitalization due to ambulatory-care sensitive conditions (those avoidable with appropriate primary care), are more likely in rural areas19,20, suggesting access to primary health care, such as family physicians, is more difficult in rural regions. Similarly, rural residents, although no less likely to receive home care than their urban counterparts, have been found to receive fewer provider days in a recent US study21. Such access issues may help to explain the increased likelihood of hospitalization in rural areas in the Canadian studies4,15, because they may reflect reduced access to end-of-life care in other settings, such as at home.
It is also important not to over-generalize these findings, however, given the possibility of specific regional circumstances in access to health care. For instance, a remote Northern region in the province of Manitoba, Canada, was shown to have higher family and specialist consultation rates than in urban regions, attributable to the specific organization of health care services in that region where physicians are hired on a salary basis via a medical unit dedicated to providing health care in that region22. This is different from most of the rest of the province where a fee-for-service system is the norm, with some rural or remote regions in Manitoba having difficulty retaining physicians, thus, potentially jeopardizing access.
In the present study hospital use at the end of life was examined in one mid-Western Canadian province, Manitoba. As is the case throughout Canada, Manitoba has a universal healthcare system. Thus, healthcare use, including care at the end of life in any care setting, be it in hospital or at home, or the type of care (eg acute vs palliative, ie care for terminally ill patients) should not be influenced by an individual's financial means or personal healthcare insurance.
The study had three objectives. First, in order to add to the sparse and inconsistent literature on hospital transfers in rural areas, the difference between hospitalizations in rural/remote and urban regions was examined. Second, the relationship between the availability of healthcare resources and hospital transfers was explored as a way of explaining potential regional variation. Third, the day-to-day patterns of hospitalizations was examined in more detail across rural and urban regions. In this case, what was of interest was whether the daily rates of hospitalization in the final days before death were the same across rural/remote and urban regions.
Methods
Data sources
The main data source was administrative healthcare records collected by the provincial health ministry in administering the universal health care system. Specifically accessed were hospital discharge data, which provide complete records of all hospitalizations in the province for the entire population. The quality of the data has been examined extensively, with numerous studies indicating that the data are complete, reliable, and valid23-26. Vital statistics data were used to derive cause of death and demographic information (age and sex). Information regarding health service resources was obtained from publicly available statistical reports compiled by the provincial health ministry27.
Sample
The study sample was derived from a complete cohort who died in Manitoba in the period 2003-2004, as determined from vital statistics data. Excluded from this cohort were individuals aged less than 19 years and those living in long-term care institutions, yielding a final sample (n = 6523) of adults who lived in the community (ie were not institutionalized).
Measures
Predictor variables: Decedents' region of residence was defined according to regional health authority boundaries, assigning individuals to a region based on their residences' postal code. This approach was chosen because Manitoba's healthcare system is regionally organized, with each of 11 health regions providing the governance structure to oversee both acute care and community-based care within that geographic area. For the present purposes, and consistent with the provincial health ministry's classification, 9 regions were identified as rural/remote. Because of the small population and, consequently, small number of deaths in the 3 remote regions, these were combined into one, making 7 rural/remote regions. Some of these contain small cities (the largest has a population of 13 000); however, the population density is low (<6 individuals/km2). Two regions were defined as 'urban' because they exclusively encompass 2 larger cities (population 650 000 and 48 000 with a population density of approximately 1000 and 28, respectively).
In terms of health service resources, the number of hospital beds and nursing home beds were included because previous research has shown these to be related to hospitalization16-18. Also included was the number of physicians and home-care services, the latter because palliative care (ie care for terminally ill patients) provided in people's homes is organized through the regionally administered homecare program. Each of these measures was expressed as a rate (per 1000 population) for a given region.
Demographic variable: Demographic variables included in the analyses were age groups (19-64, 65-74 and >75 years) and sex. Using cause of death from vital statistics data, the decedents were further grouped into disease categories using methodology developed by Fassbender28. These disease categories are conceptually linked to distinct functional trajectory groups of dying identified from the literature29-31:
- terminal illness, which includes predominantly cancer deaths and tends to be characterized by a relatively rapid functional decline shortly before death
- organ failure (eg chronic obstructive pulmonary disease, congestive heart failure), which is characterized by a relatively slow, steady decline that is interrupted by periods of severe exacerbations of the disease
- frailty, which is associated with a steady decrease in functional abilities, ultimately culminating in death
- a further group was made of sudden deaths (eg due to accidents) and all remaining deaths (eg due to mental illness).
Outcome variable: Two outcome measures were included: hospitalizations and hospital days, as derived from hospital data. Only hospitalizations within the province of Manitoba were included. Previous research32 indicates that only a small proportion (<2%) of hospital use by Manitoba residents occurs outside the province; thus, excluding out-of-province hospitalizations should have little impact on the results. Given that hospital use increases markedly in the last month before death10,33, hospitalizations were counted for the last 30 days before death. For hospital days (for those with at least one hospitalization) the focus was the final 29 days. Because much of palliative care (defined in Manitoba as care for terminally ill individuals) is provided in hospital settings, either in special palliative care units or specifically designated beds, any hospitalizations or hospital beds flagged in the data as being 'palliative' were excluded. As only relatively few individuals (6.5% of decedents) were hospitalized more than once in the last 30 days before death, this variable was subsequently dichotomized into 'never hospitalized' or 'hospitalized at least once'.
Analyses
Two sets of analyses were conducted. First, logistic regression was used for the dichotomous variable of hospitalized, and a generalized linear model (GLM) with a negative binomial distribution was used for the highly skewed measure of hospital days. Several regressions were computed, one with region of residence in the model and, subsequently, additional models with each of the 4 health care resource variables substituted for region. Age groups, sex and trajectory groups were included in all analyses.
Second, a grow curve model was used to examine specific patterns of hospitalization on a day-by-day basis in the last 14 days before death. Growth curve models were appropriate because they allowed the examination of change over time (in this case measured in days) and allowed examination of both linear and curvilinear growth. Thus, using growth curve models, it was possible to test whether daily hospitalization rates were constant across regions over the 14 days, or whether rates increasingly diverged over time. In all growth curve models, the day of death was coded as the origin of time. Thus, the coefficients of the lower order terms can be interpreted at day of death34, reflecting the likelihood of dying in hospital versus elsewhere.
Results
Table 1 shows the number of decedents in each of the 9 regions of residence. Over half of deaths occurred in one urban region (Urban region 1), which makes sense given that this region (encompassing one city) also constitutes about 60% of the population of the province. Table 2 shows the substantial variation in healthcare resources across the 9 regions, with rural/remote regions generally having fewer physicians and variable access to other healthcare resources. Table 3 provides descriptive information of the number of individuals who were hospitalized at least once in the last 30 days before death, as well as the number of hospital days. Noteworthy is the variation in the percentage of people hospitalized across regions, ranging from 55.6% to 70.2%. The average number of hospital days per person also varied across regions.
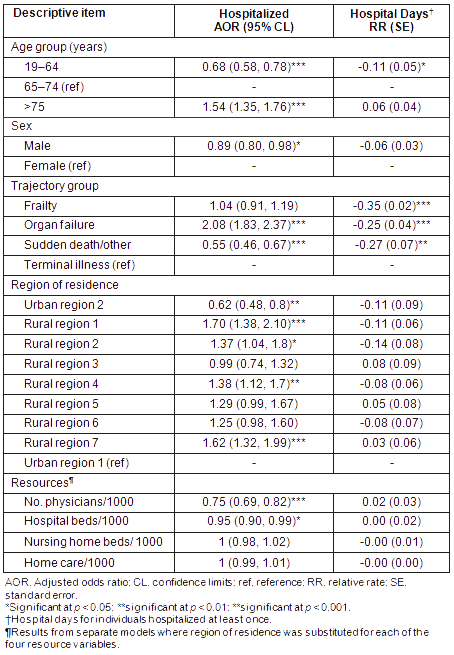
Results from the regression analyses (Table 4) show that, relative to the comparison (Urban region 1), residents of 4 of the 7 rural/remote regions had higher odds of being hospitalized in the last 30 days before death. In contrast, residents of Urban region 2 had lower odds of being hospitalized. Hospital days, in contrast, did not differ significantly from Urban region 1. Further analyses with healthcare resources in the model suggest that this regional variation in hospitalization is, at least in part, attributable to the availability of physicians and the number of hospital beds (per 1000 population). Neither nursing home beds nor home-care services were related to either the odds of being hospitalized or hospital days.
Table 1: Descriptive profile of decedents
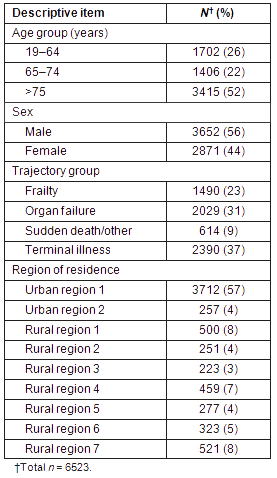
Table 2: Healthcare resources by region
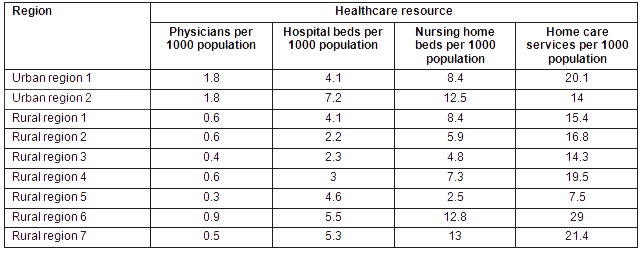
Table 3: Hospital use before death
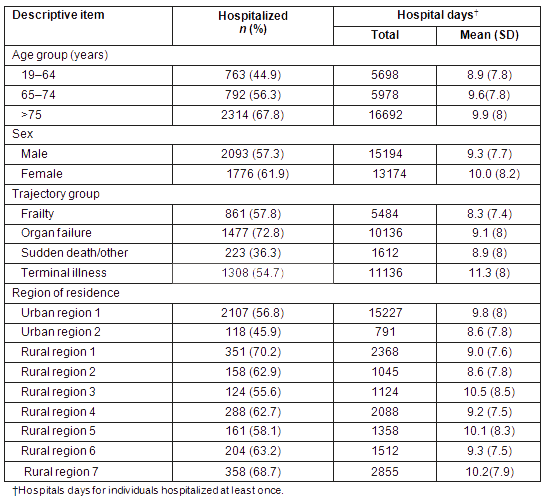
Table 4: Regression results: hospitalizations and hospital days
Regarding the pattern of hospitalizations during the 14 days before death (Fig1) that determines if there were any regional differences in hospitalization trajectories, individuals aged 19-64 and 65-74 years were less likely to die in hospital than those aged over 75 (Table 5). Similarly, males were less likely to die in hospital than females, while individuals with organ failure were more likely to die in hospital than those with terminal illness. Trajectory group was also both a predictor of linear and quadratic growth, indicating that the rate of hospitalization at time of death differed among the 3 groups (frailty, organ failure and sudden death/other, respectively), relative to terminal illness, with the rate also increasingly diverging over time. More specifically, individuals in the frailty group were increasingly more likely to be hospitalized as death approached, relative to the terminal illness group, as were individuals with organ failure and, to a lesser extent, those in the sudden death/other causes group.
The effects for regions of residence were not significant, with only two exceptions: both the linear and curvilinear growth effects for Rural region 2 relative to Urban region 1, were significant. Decedents in this rural region were increasingly more likely to be hospitalized as death approached, relative to Urban region 1. In terms of healthcare resources, two significant effects emerged. Having more physicians and more hospital beds per 1000 population was associated with a reduced likelihood of dying in hospital.
Table 5: Summary of growth curve models
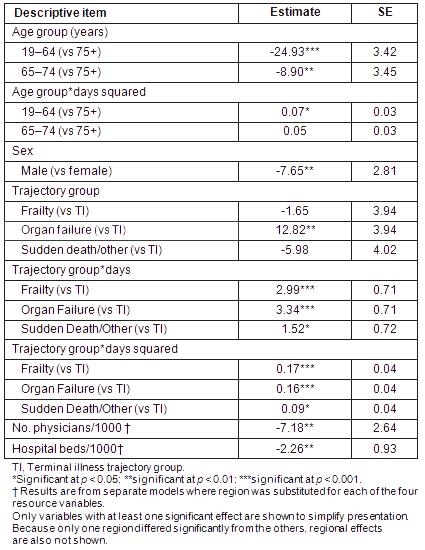
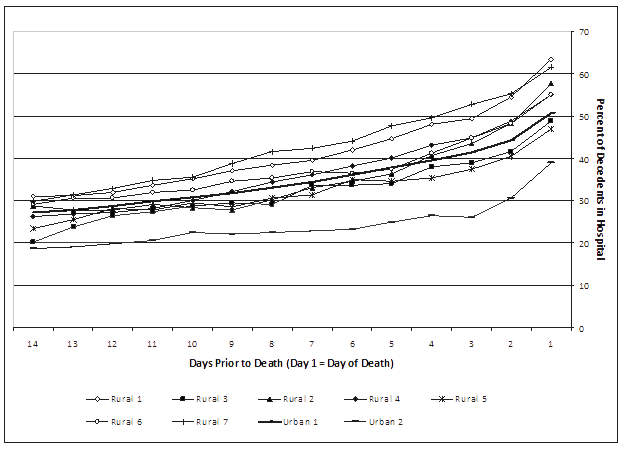
Figure 1: Daily pattern of hospitalizations across regions
Discussion
The present study was inspired by the paucity of research into healthcare use at the end of life in rural areas. The findings contribute to this literature by showing that, in one Canadian province (Manitoba), substantial variation across regions exists in transfers into hospital in the last month before death. Residents of 4 of the 7 rural/remote regions had higher odds of being hospitalized at the end of life, relative to residents of an urban centre, although the days in hospital did not differ among those hospitalized.
The increased likelihood of hospitalizations in certain rural regions may be explained by the availability of healthcare resources. In this respect, the present findings indicate that having a greater number of physicians per 1000 population decreased both the odds of hospitalization, and also the likelihood of death in hospital. Physician supply was consistently lower in rural/remote compared with urban areas. Having fewer physicians available may, in turn, lead to a greater tendency to hospitalize, a finding that corroborates previous research that suggests rural residents are more likely to be hospitalized for illnesses that could have been treated by family physicians or other primary-care providers19,20.
Hospital bed supply was also related to both hospitalization and hospital deaths, with a greater number of beds per 1000 population being related to lower odds of being hospitalized and reduced likelihood of hospital deaths. This is contrary to previous research, which shows that a greater number of hospital beds were associated with an increased likelihood of dying in hospital16-18. That the present study found the opposite pattern likely needs to be interpreted within the context of the health system in the province of Manitoba, where health services are heavily concentrated into one urban centre (labeled here Urban region 1). For example, 75% of all physicians are based in the city, including the vast majority of specialist physicians, as well as the only 2 tertiary hospitals in the province that provide specialized care for complex cases. Moreover, palliative care services for individuals who are terminally ill are more established in the city, which has been home to 2 large hospital-based palliative care units for several decades. Thus, the present findings are reasonably interpreted as a reflection of the overall relative resource richness in the urban centre relative to rural/remote regions.
Besides rural/urban and health care resource differences, individual characteristics also predicted hospital transfers. Noteworthy are the findings for trajectory groups, which were used here as a way of conceptualizing functional trajectories at the end of life29,30. The findings indicate that the groups meaningfully differentiated between patterns of hospital use. For instance, individuals with organ failure had more than twice the odds of being hospitalized in the last month before death than those with terminal illness; however, those hospitalized incurred fewer hospital days. This is consistent with the finding that there was greater acceleration in hospitalization rates for individuals with organ failure close before death, as compared with those with terminal illness, which suggests that individuals with organ failure tended to be hospitalized shortly before death and also were more likely to die in hospital.
Whether these hospital deaths were appropriate or whether individuals might have been cared for in alternative settings cannot be determined from the present study. However, this is an issue that should be examined further, given that individuals who died of organ failure constituted one-third of all decedents.
Limitations
This study had a number of limitations. One concerns the use of administrative data which, although it allows detailed examination of hospital use, does not provide any information on other issues that may influence hospital use, such as specific physician practice patterns that may influence the likelihood of hospitalization in a given geographic area. These data do not allow examination of the quality of care individuals received in hospital, nor can they determine whether individuals were hospitalized or died in hospital by choice. Although research indicates that most people want to die at home35,36, the decision as to whether a home death is possible is not always easy because it affects not only the dying individual, but also family members37.
In the present study analyses were conducted at the regional level. Although this makes sense given that the healthcare system is administered within regional health authorities in Manitoba, it may also mask local patterns, for example, whether people in certain rural towns or villages are more likely to being hospitalized than in others. Another issue that was beyond the scope of this study but should be examined in the future, is whether people were hospitalized 'close to home'. In rural areas, individuals might be more likely to be hospitalized out of region, thereby placing an extra burden on them and their families.
Conclusion
The present study suggests that residents of some rural/remote regions may be disadvantaged in terms of access to an appropriate care setting at the end of life. However, the substantial variation across rural/remote regions also indicates that conclusions should not be over-generalized. Rather, local differences in healthcare resources must be taken into account when examining healthcare use at the end of life. While many rural/remote regions will have fewer resources available, this may not always be the case.
Acknowledgments
The authors acknowledge the contribution of Manitoba Health in allowing access to administrative healthcare records. The results and conclusions are those of the authors and no official endorsement by Manitoba Health is intended or should be inferred. This research was supported by a grant from the Canadian Institutes of Health Research. Author V. Menec holds a Canada Research Chair in Healthy Aging.
References
1. Wilson DM, Northcott HC, Truman CD, Smith SL, Anderson MC, Fainsinger RL et al. Location of death in Canada: a comparison of 20th century hospital and non-hospital location of death and corresponding population trends. Evaluation & Health Professions 2001; 24(4): 385-403.
2. Flory J, Yinon YX, Gurol I, Levinsky N, Ash A, Emanuel E. Place of death: U.S. trends since 1980. Health Affairs 2004; 23(3): 194-200.
3. Weitzen S, Teno JM, Fennell M, Mor V. Factors associated with site of death: a national study of where people die. Medical Care 2003; 41(2): 323-335.
4. Burge F, Lawson B, Johnston G. Trends in the place of death of cancer patients, 1992-1997. Canadian Medical Association Journal 2003; 168(3): 265-270.
5. Higginson IJ, Astin P, Dolan S. Where do cancer patients die? Ten-year trends in the place of death of cancer patients in England. Palliative Medicine 1998; 12(5): 353-363.
6. Hunt, RW, Fazekas BS, Luke CG, Roder DM. Where patients with cancer die in South Australia, 1990-1999: A population-based review. Medical Journal of Australia 2001; 175(10): 526-529.
7. Davison D, Johnston G, Reilly P, Stevenson M. Where do patients with cancer die in Belfast? Irish Journal of Medical Sciences 2001; 170(1): 18-23.
8. Constantini M, Balzi D, Garronec E, Orlandini C, Parodi S, Vercelli M et al. Geographical variations of place of death among Italian communities suggest an inappropriate hospital use in the terminal phase of cancer disease. Public Health 2000; 114(1): 15-20.
9. Heyland DK, Lavery JV, Tranmer JE, Shortt SED, Taylor SJ. Dying Canada: is it an institutionalized, technologically supported experience? Journal of Palliative Care 2000; 16(Suppl): S10-S16.
10. Menec VH, Lix L, Nowicki S, Ekuma O. Health care use at the end of life among older adults: does it vary by age? Journal of Gerontology: Medical Sciences 2007; 62A(4): 400-407.
11. Andersson M, Hallberg IR, Edberg AK. Health care consumption and place of death among old people with public home care or special accommodation in their last years of life. Aging Clinical and Experimental Research 2007; 19(3): 228-239.
12. Houttekier D, Cohen J, Bilsen J, Debroosere P, Verduyckt P, Deliens L. Determinants of the place of death in the Brussels metropolitan region. Journal of Pain and Symptom Management 2009; 37(6): 996-1005.
13. Burge FI, Lawson B, Crichley P, Maxwell D. Transitions in care during the end of life: changes experienced following enrolment in a comprehensive palliative care program. BMC Palliative Care 2005; 4(1): 3.
14. Klinkenberg M, Visser G, van Groenou MI, van der Wal G, Deeg DJ, Willems DL. The last 3 months of life: care, transitions and the place of death of older people. Health and Social Care in the Community 2005; 13(5): 420-30.
15. Burge FI, Lawson B, Johnston G. Where a cancer patient dies: the effect of rural residency. Journal of Rural Health 2005; 21(3): 233-238.
16. Mitchell SL, Teno JM, Miller SC, Mor V. A national study of the location of death for older persons with dementia. Journal of the American Geriatrics Society 2005; 53(2): 299-305.
17. Yun YH, Lim MK, Choi KS, Rhee YS. Predictors associated with the place of death in a country with increasing hospital deaths. Palliative Medicine 2006; 20(4): 455.
18. Pritchard RS, Fisher ES, Teno JM, Sharp SM, Reding DJ, Knaus WA et al. Influence of patient preferences and local health system characteristics on the place of death. SUPPORT Investigators. Study to Understand Prognoses and Preferences for Risks and Outcomes of Treatment. Journal of the American Geriatric Society 1998; 46(10): 1242-1250.
19. Chen LW, Zang W, Sun J, Mueller KJ. The magnitude, variation, and determinants of rural hospital resource utilization associated with hospitalizations due to ambulatory care sensitive conditions. Journal of Public Health Management Practice 2009; 15(3): 215-222.
20. Cloutier-Fisher D, Penning MJ, Zheng C, Druyts EB. The devil is in the details: trends in avoidable hospitalization rates by geography in British Columbia, 1990-2000. BMC Health Services Research 2006; 16(6): 104.
21. McAuley WJ, Spector W, Van Nostrand J. Formal home care utilization patterns by rural-urban community residence. Journal of Gerontology: Social Sciences 2009; 64B(2): 258-268.
22. Martens PJ, The Need to Know Team, Fransoo R, Burchill C, Burland E. Health status and healthcare use patterns of rural, northern and urban Manitobans: is Romanow right? Healthcare Policy 2006; 2(1): 108-127.
23. Roos LL, Mustard CA, Nicol JP, McLerran DF, Malenka DJ, Young K et al. Registries and administrative data: organization and accuracy. Medical Care 1993; 31(3): 201-212.
24. Roos LL, Nicol JP. A research registry: uses, development, and accuracy. Journal of Clinical Epidemiology 1999; 52(1): 39-47.
25. Roos LL, Gupta S, Soodeen R, Jebamani L. Data quality in an information-rich environment; Canada as an example. Canadian Journal on Aging 2005; 24(Suppl 1): 153-170.
26. Roos NP. Establishing a population data-based policy unit. Medical Care 1999; 37(6 Suppl): JS15-26.
27. Manitoba Health. Manitoba Health Annual Statistics 2003-2004. Winnipeg: Manitoba Health, 2004.
28. Fassbender K, Smythe JG, Carson M, Finegan BA, Boothe PM. Costs and Utilization of Health Care Services at End of Life. Edmonton: Institute for Public Economics, 2006.
29. Lunney JR, Lynn J, Foley DJ, Lipson S, Guralnik JM. Patterns of functional decline at the end of life. Journal of the American Medical Association 2003; 289(18): 2387-2392.
30. Lunney JR, Lynn J, Hogan C. Profiles of older Medicare decedents. Journal of the American Geriatric Society 2002; 50(6): 1108-1112.
31. Chen JH, Chan DC, Kiely DK, Morris JN, Mitchell SL. Terminal trajectories of functional decline in the long-term care setting. Journal of Gerontology: Medical Sciences 2007; 62A(5): 531-536.
32. Martens PJ, Fransoo R, Burland E, Jebamani L, Burchill C, Black C et al. The Manitoba RHA Indicators Atlas: Population-Based Comparisons of Health and Health Care Use. Winnipeg: Manitoba Centre for Health Policy, 2003.
33. Mukamel DB, Bajorska A, Temkin-Greener H. Health care services utilization at the end of life in a managed care program integrating acute and long-term care. Medical Care 2002; 40(12): 1136-1148.
34. Biesanz JC, Deeb-Sossa N, Papadakis AA, Bollen KA, Curran PJ. The role of coding time in estimating and interpreting growth curve models. Psychological Methods 2004; 9(1): 30-52.
35. Fried TR, van Doorn C, O'Leary JR, Tinetti ME, Drickamer MA. Older persons' preferences for site of terminal care. Annals of Internal Medicine 1999; 131(2): 109-112.
36. Townsend J, Frank AO, Fermont D, Dyer S, Karran O, Walgrove A, et al. Terminal cancer care and patients' preference for place of death: A prospective study. British Medical Journal 1990; 301(6749): 415-417.
37. Stajduhar KI, Davies B. Variations in and factors influencing family members' decisions for palliative home care. Palliative Medicine 2005; 19(1): 21-32

