Context
For those residing in rural and isolated parts of Canada, obtaining quality mental health services is often an unfulfilled wish. Whether considering a fly-in only community in Canada's far north, a small town in southern Ontario or even an agricultural based community in western Canada, the challenges are as diverse as the settings to which 'rural' or 'isolated' apply. Waiting times for effective and timely treatment for those with mental illness are known to be poor and well below those of other high-priority health areas1. Disparities between rural and urban individuals with mental illness include higher rates of symptoms of distress2 and higher rates of hospitalization3 for those in rural areas. In contrast, lower rates of schizophrenia and organic brain syndrome have been found2 and a recent Canadian survey found lower rates of depression in rural areas4. Additionally, for remote or isolated regions of Canada, the essential relationship between primary care providers (such as family physicians or nurse practitioners) and specialty mental health services in tertiary centres is often weak or non-existent.
One model of care provision, known as 'shared' or 'collaborative' care, attempts to decrease barriers between primary care providers and mental health providers. Recent evidence has supported collaborative care's effectiveness in Canada, including in the care of persons experiencing moderate, severe, or persistent mental illness5-8. Other international models have been introduced9,10, and this model has been formally endorsed by numerous professional bodies including the College of Family Physicians and Canadian Psychiatric Association, as a possible means to effectively enhance service provision where difficulties exist to for those attempting to access mental health services11,12. This model of care was also endorsed as a way to transform mental health care delivery in the 2006 report by Canadian Senators Kirby and Keon13.
A component of the work of the Canadian Collaborative Mental Health Initiative (CCMHI) is 'a toolkit', funded through the federally sponsored Primary Care Transition Fund. The CCMHI was guided by an advisory-consortium of representatives of twelve Canadian healthcare professional bodies with the intent of improving the primary care delivery of mental health of Canadians. Specifically, the CCMHI's intent was to enhance resources, promote program development and deepen the concept of collaborative mental health care in Canada by promoting collaboration among primary healthcare and mental healthcare providers, consumers, families and caregivers. As a part of this process, a number of aids were developed for establishing collaborative practices, including a general toolkit as well as eight population-specific toolkits designed to be used in conjunction with the general toolkit. These toolkits are not intended to be clinical practice guides, but rather offer practical advice about different aspects to consider when striving to establish successful collaborative initiatives.
A framework for all eight toolkits was assigned by the CCMHI for optimization as practical tools to assist providers and planners with the implementation of collaborative initiatives, to help mental health consumers and their family members understand mental illness and work with other members of the care team, to inform educators of the benefits of interprofessional education, and to provide tools to teach about collaborative mental health care. The content of each toolkit was developed by an expert interprofessional panel (working group) established by CCMHI. The working groups were to seek representation from provider stakeholders including medicine, social work, psychology, pharmacy and nursing as well as consumers from across Canada.
Issue
One such toolkit, the Rural and Isolated (R&I) Toolkit, sought to improve collaboration in the delivery of mental health services for those living in rural and isolated areas of Canada14. The intent of this article is to provide a synopsis of this particular toolkit (the full toolkit is available online at the CCMHI website at http://www.ccmhi.ca/en/products/toolkits/providers.htm). This synopsis will include a highlight of eight key messages derived from the R&I Toolkit and concludes with a visual guide for initiating collaborative mental health care practices in rural and isolated areas.
Rural and isolated context
Cultural diversity, a fundamental Canadian characteristic, is as true of rural communities as urban15. Canadians residing in rural and isolated areas are not a single, homogenous group, but a culturally unique and diverse population. While many rural communities are located in large agricultural regions, others are close to major urban centres, while others are coastal or located in the most remote areas of Canada's north. When considering rural and isolated populations in Canada, it is particularly important to look at the needs of Aboriginal peoples because they constitute one of the largest segments of isolated populations.
In spite of their diverse nature, rural and isolated communities have common problems in health status, and access to health care and health professionals, especially family physicians15,16. Health indicators consistently reveal that significant disparities exist in health outcomes 'between people who live in the northern part of Canada versus the south, and between people who live in Atlantic Canada and the rest of the country'17. Rural and isolated Canadian communities frequently encounter the considerable demographic, economic, social and ecological challenges associated with geographic isolation, depopulation and aging populations, environmental decay and depletion of natural resources.
The health of a community appears to be related to the remoteness of its location. Communities show progressive deterioration in health the greater their distance is from urban areas. Residents of rural health regions not only have a lower life expectancy than the national average, but they also experience higher rates of disability, violence, poisoning, suicide and accidental deaths than do their urban counterparts18.
When compared with their urban counterparts, rural and isolated residents encounter more mental and physical health issues yet they have fewer resources to help address these problems. People in rural and isolated areas have lower levels of education and lower standards of living than urban populations. Access to allied health services and initiatives, such as nutrition services, may be inconsistent or too costly for residents in rural areas19. In addition, rural and isolated communities frequently have aging populations and experience youth migration to larger centres as young people search for better job opportunities. Enhancing timely access or coordination of mental health services for consumers in isolated areas may increase tenure within their home communities, and increase compliance with care20.
Defining the population
There is no one standardized definition of rural and isolated populations. Aspects relating to the quality of life in rural and isolated populations are seldom incorporated in current definitions. For the purpose of the R&I Toolkit, rural and small-town communities were defined as those with 10 000 or fewer residents and situated outside the commuting zones of large metropolitan areas and cities21. 'Isolated' implies having limited or no road access and no ready access to specialized services.
Consultation process
The R&I working group was selected by members of CCMHI organizing committee on the basis of their involvement with primary care or mental health care in rural or isolated areas in Canada. Representation was diverse, comprising a wide array of geographical regions (across six provinces) and disciplines, including family medicine, psychiatry, social work, pharmacy, psychology, nursing, and consumers. The members actively brought input from rural road-accessible as well as fly-in communities that included Northern Ontario and Manitoba, the Northwest Territories and Labrador.
The consultative process of the R&I Working Group sought input from consumers, families and caregivers, as well as providers and members of the twelve nationally represented associations in CCMHI, for the purpose of soliciting rich input for R&I Toolkit content development (Fig1).
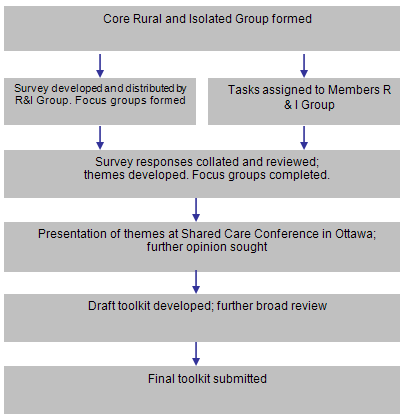
Figure 1: The Rural and Isolated Toolkit consultative process.
The R&I Working Group collected data through surveys distributed via e-mail, fax or surface mail, telephone contact and focus groups. Mental health consumers participated in the survey design and development process and, later, during the review of emerging themes. Of the 48 surveys distributed, 30 completed surveys were returned (62%). Two focus group discussions were conducted with mental health care providers: one in Labrador and the other in Northern Manitoba. Questions from the written survey formed the basis of the questions asked during the focus group. One focus group session was digitally recorded and later transcribed. The other was recorded on paper by a researcher. Later, findings from both groups were reviewed for key themes by the R&I Working Group.
Lessons learned
Key messages
A number of thematic issues or messages were agreed on from the consultative process. These messages were: access to services, interprofessional education, consumer involvement, evaluation and research, models of collaboration, ethics, funding, and policy and legislation.
Access to services: Numerous access challenges exist in rural and isolated regions of Canada. These include insufficient numbers of healthcare professionals and resources, travel barriers and costs created by the distance from healthcare professionals in urban centres. Strategies for improving access include: using diverse channels of communication (such as radio, television, newspaper and the internet) to disseminate healthcare information; creating regional health authority sub-organizations or other bodies to help high-risk groups; developing self-help manuals for consumers to foster health promotion and prevention; using telemedicine to overcome distance and isolation from service; and providing transportation.
Interprofessional education: Interprofessional education was recommended as a means of addressing current and emerging health and human resource issues. It is defined as occasions when two or more professions learn from and about each other to improve collaboration and the quality of care11.
Educational opportunities such as these were believed to provide numerous benefits to consumers, providers, educators and students, and the health delivery system. For the consumers, these included improved coordination and integration of care. For providers, interprofessional approaches allowed for clearer, more consistent goals in delivering care and enabled the provider to learn new skills and approaches to care through a 'train the trainer' view to learning. Benefits to students include improved modeling for future practice, and appreciation of other disciplines22,in 11.
Consumer involvement: Rural and isolated regions successfully providing care often depend on 'local' solutions that, by necessity, require the service user to be included. The respondents believed that consumer centredness can be promoted by having inclusive meetings between consumers and providers; providing consumer/client advocate/complaints officers to address consumers' needs; enabling consumers to make self-referrals to mental health; and supporting transportation to mental health services outside of rural areas.
Evaluation and research: The response indicated that evidence-based research is needed to assist in better planning and service delivery for rural and isolated populations, and creativity is required to plan and support this type of research. This is required within a context of involving community members in a way that will ensure community needs are being addressed. Overcoming the anticipated obstacles of distance, gathering local input to priority areas and recognizing cultural factors and beliefs about mental illness were considered important. High suicide rates were of particular concern, as they are several times the national average in many Aboriginal communities.
Program developments in isolated regions of Canada often are modeled on programs found successful in larger centres. When implemented, services are not often evaluated for success. Showing success in terms of evaluation was seen as necessary in creating leverage for change. Particular care needs to be taken to ensure evaluation tools are appropriate to rural and isolated populations. These programs deserve analysis of their effectiveness and appropriateness to the locality with both quantitative and qualitative evaluation.
Models of collaboration: Although there are a number of 'best practice' approaches, the success of rural and isolated collaborative initiatives appears to require flexibility: local adaptations make each effort unique, such as two clinicians working locally, fly-in visits, or distance video conferencing. Successful programs often attempt to bridge recognized gaps in existing clinical services with resourceful solutions.
Other important considerations include the use of multidisciplinary teams with flexible role assignments, assisted by community advisory committees and consumers. Successful programs supported existing informal collaboration, such as that of clergy and teachers with clinicians. Sufficient training in quality care, continuing education in mental health areas, and supervision for skill development were highly recommended. Specific successful collaborative programs are noted in the full toolkit appendix.
Ethics: The ethical challenges associated with the development of collaborative initiatives in rural and isolated regions are frequently understated or ignored in the planning and development of such projects. Ethical foundations for community practice embrace diversity, inclusion, empowerment, participation, social justice, advocacy, and interdependence23. These ethical foundations facilitate participation across cultures when health professionals incorporate them into the values that underpin their practice and consistently integrate them in the work they do24. A variety of ethical issues are encountered within public health and rural and isolated community practice, and continue to keep practitioners, rural and isolated communities, and society as a whole 'ethically engaged'. These issues include: respecting individual autonomy yet benefiting the entire rural community (for example, the right to privacy versus informed consent may conflict with sharing individual information for the benefit of the entire rural population's health; and ensuring inclusion and diversity in rural and isolated community participation).
Funding: Funding-related challenges were found to exist throughout the mental health delivery systems among communities and participants during the toolkit development. Financial incentives were thought necessary to attract health professionals. Funding directed to the provision of primary resources to consumers who both need and utilize higher levels of mental health care to prevent more costly service utilization is needed. The consideration of funding specifics include mandating resources to collaborative care initiatives, developing family physician skills in mental health, along with a prioritization towards prevention measures.
Policy and legislation: Government policy development and planning for rural and isolated services was considered lacking in most parts of the country. Some provinces do have strategic plans for primary healthcare services, although mental health is not addressed adequately. In spite of the increased understanding that rural health problems are unlikely to be adequately addressed by mainstream programs alone25, many healthcare planners, providers and administrators continue to rely solely on the use of urban-focused approaches, rather than designing models to suit the unique circumstances of rural communities. Reliance on the use of urban models will create barriers for rural and isolated communities in their efforts to achieve equal status with urban counterparts.
The R&I Toolkit focused primarily on providing unique insights regarding the establishment of a responsive collaborative mental health service from those in the field. For success, this approach also needs to consider potential obstacles related to policy and legislative issues. For instance, discrepancies exist between federal and provincial jurisdictions, particularly for Aboriginal people, that put limits on service delivery. Respondents to the toolkit survey described being under the age of 16 years as an obstacle to care. Several specific barriers for Aboriginal people included service limits if living off-reserve, the stigma of using medical transportation, and confusing funding distinctions between provincial and federal policy.
Solutions proposed and detailed in the full toolkit include considering mandating core-competency skills in the training of mental health workers, and moving from short-term to longer-term funding that includes mental health promotion. Finally, a Canadian mental health policy such as that sought through the Kirby report13 and newly formed Mental Health Commission gives reason for hope to many in underserved areas.
Conclusion
The R&I Toolkit was developed for providers and funders to facilitate the provision of mental health in rural and isolated areas: to capitalize on local opportunities while doing so in a collaborative manner. Such innovation necessitates a broad dialogue, an effective model or concept map for service delivery and key community 'champions' to lead implementation efforts.
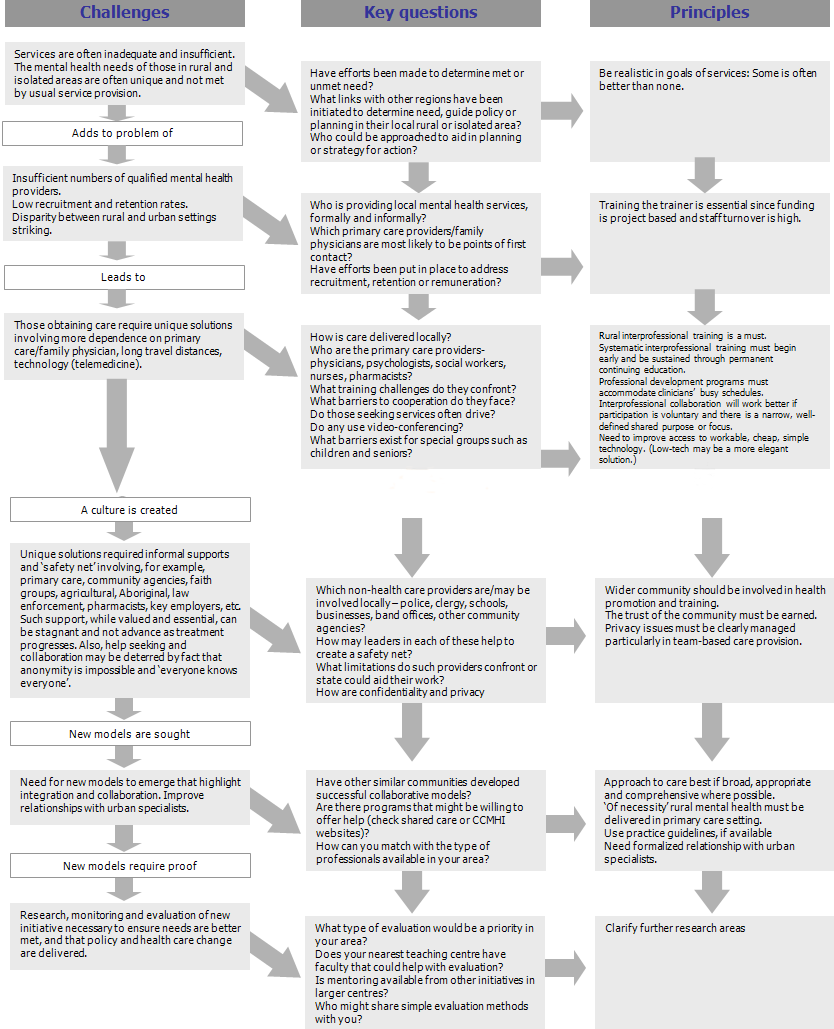
Figure 2: Steps and processes towards implementing collaborative care services in rural and isolated areas: challenges (column 1); key questions (column 2); principles of implementation (column 3).
As a visual guide and overview, a flow diagram is offered (Fig2) detailing the challenges associated with rural and isolated mental healthcare service delivery; specifying key questions to be asked; and offering principles to follow when contemplating the implementation of collaborative care initiatives in rural and isolated regions. Figure 2 attempts to provide a synthesis and practical application of the toolkit by describing major obstacles or barriers to collaboration in rural and remote areas, questions to assist in addressing related issues and listing principles appropriate to consider.
Acknowledgements
Sari Ackerman, Nick Kates, Anne Marie Crustulo and Tracey Henrickkson's support is acknowledged as well as members of the Rural and Isolated working group, and members of the general Toolkit working group. Funding for this toolkit was provided through the Primary Health Care Transition Fund of the Government of Canada.
References
1. Esmail N, Walker MA. Waiting your turn, 17th edn. Vancouver,BC: The Fraser Institute, 2007.
2. Dottl SL, Greenley JR. Rural-urban differences in psychiatric status and functioning among clients with severe mental illness. Community Mental Health Journal 1997; 33(4): 311-321.
3. Rost K, Adams S, Xu S, Dong F. Rural-urban differences in hospitalization rates of primary care patients with depression. Psychiatric Services 2007; 58(4): 503-8.
4. Mitura V, Bollman RD. The health of rural Canadians: a rural-urban comparison of health indicators. Rural and Small Town Canada Analysis Bulletin, vol. 4(6). Ottawa: Statistics Canada, 2003.
5. Craven MA, Bland R. Better practices in collaborative mental health care: an analysis of the evidence base. Canadian Journal of Psychiatry 2006; 51(6;Suppl1): 7S-72S.
6. Haggarty J, Haslam D, Houlding C, Armstrong D. Clinical findings of a cluster randomised control pilot trial of a Canadian Shared Care service for those with chronic mental illness. Primary Care and Community Psychiatry 2008; 13(1): 19-25.
7. Haggarty J, O'Connor B, Dubois S, Blackadar AM, McKinnon T, Boudreau D et al. A pilot study of a Canadian shared mental health care programme: changes in patient symptoms and disability. Primary Care and Community Psychiatry 2008; 13(1): 27-35.
8. Maar MA, Erskine B, McGregor L, Larose TL, Sutherland ME, Graham D et al. Innovations on a shoestring: a study of a collaborative community-based Aboriginal mental health service model in rural Canada. International Journal of Mental Health Systems 2009; 3: 27.
9. Kowanko I, de Crespigny C, Murray H. Better medication management for Aboriginal people with mental health disorders and their carers. Adelaide, SA: Imprint Design, 2003.
10. Sutor B, Agerter DC. Collaborative psychiatric care in a rural family medicine setting reduces health care utilization in depressed patients. Minnesota Medicine 2007; 90(1): 39-41.
11. Curran V, Ungar T, Pauzé E. Strengthening collaboration through interpersonal education: a resource for collaborative mental health care educators. Ottawa: Health Canada. (Online) 2006. Available: http://www.ccmhi.ca/en/products/toolkits/educators.htm (Accessed 3 March 2010).
12. Nasmith L, Oandasan I, Waters I, Way D, Jones L. Interdisciplinary education in primary health care: moving beyond tokenism. In, Proceedings, College of Family Physicians of Canada Family Medicine Forum 2003; 23-25 October 2003; Calgary, AB. 2003.
13. The Standing Senate Committee on Social Affairs. Out of the shadows at last: transforming mental health, mental illness and addiction services in Canada. The Committee: 2006. (Online) 2006. Available: http://www.parl.gc.ca/39/1/parlbus/commbus/senate/com-e/soci-e/rep-e/rep02may06-e.htm (Accessed 1 January 2010).
14. Haggarty J, Henriksson T, Ryan-Nicholls KD, Cornish P, Devlin A, Lehman R et al. Establishing collaborative initiatives between mental health and primary care services for rural and isolated population: A companion to the CCMHI planning and implementation toolkit for health care providers and planners. (Online) 2006. Available: http://www.ccmhi.ca/en/products/toolkits/providers.htm (Accessed 7 March 2010).
15. Ryan-Nicholls KD. Health and sustainability of rural communities. Rural and Remote Health 4: 242. (Online) 2004. Available: www.rrh.org.au (Accessed 25 May 2010).
16. Hartley D. Rural health disparities, population health, and rural culture. American Journal of Public Health 2004; 94(10): 1675-1678.
17. Commission on the Future of Health Care in Canada. Building on values - the future of health care in Canada. Final Report. Ottawa: Government of Canada, 2002.
18. Statistics Canada. Health indicators 2001. Ottawa: Statistics Canada, 2001.
19. Ogasawara S. Interior Health Rural Health Services Planning Framework 2004/05, Appendix C: Interior Health Nutritional Services: Issues and Concerns. (Online) 2005. Available: http://www.interiorhealth.ca/uploadedFiles/Information/Health_Service_Planning/AppendixCRural.pdf (Accessed 12 March 2010).
20. Brown SA, Parker JD, Godding PR. Administrative, clinical, and ethical issues surrounding the use of waiting lists in the delivery of mental health services. Journal of Behavioral Health Services & Research 2002; 29(2): 217-228.
21. Bollman R. Rural and Small Town Canada Analysis Bulletin, vol. 1(1). Ottawa: Statistics Canada, 1998.
22. Grant RW, Finnocchio LJ, California Primary Care Consortium Subcommittee on Interdisciplinary Collaboration. Interdisciplinary collaborative teams in primary care: a model curriculum and resource guide. San Francisco, CA: Pew Health Professions Commission, 1995.
23. Racher FE. The evolution of ethics for community practice. Journal of Community Health Nursing 2007; 24(1): 65-76.
24. Racher FE, Annis RC. Respecting culture and honoring diversity in community practice. Research and Theory for Nursing Practice 2007; 21(4): 255-270.
25. Humphreys J, Hegney D, Lipscombe J, Gregory G, Chater B. Whither rural health? Reviewing a decade of progressing rural health. Australian Journal of Rural Health 2002; 10(1): 2-14.
Abstract
Context: For those residing in rural and isolated parts of Canada, obtaining quality mental health services is often an unfulfilled wish. Rural and isolated communities share the problems of health status and access to care. Health deteriorates the greater the distance from urban areas in the following dimensions: lower life expectancy than the national average; higher rates of disability, violence, poisoning, suicide and accidental death; and more mental and physical health issues than those who live in urban areas. The Canadian Collaborative Mental Health Initiative (CCMHI) was formed to provide, in part, a practical means to encouraging collaborations between primary care and mental health providers.
Issue: This article provides a synopsis of the Rural and Isolated (R&I) toolkit developed through the CCMHI, which was intended to develop primary care and mental health collaboration in such areas. This toolkit was developed using focus group discussions with mental health providers, and surveys completed by providers and consumers.
Lessons learned: Key messages from the consultative process included: access to services; interprofessional education; consumer involvement; research and evaluation; models of collaboration; ethics; funding; and policy and legislation. A flow diagram was devised to detail the synthesis and practical application of the toolkit, as well as the challenges, key questions and principles of implementation associated with collaborative care initiatives in rural and isolated regions.
Key words: collaborative care, isolated, mental health, primary care.



