Introduction
Although it is well-known that type 2 diabetes is an important global public health issue, affecting 240 million people worldwide1 and 20.6 million people in the USA2, it is less reported that residents of the Appalachian United States may be a notable at-risk population. Diabetes was found in over 20% of residents of the Stroke Belt, a region that contains much of southern Appalachia3. In the Cincinnati, Ohio area, first generation white Appalachians (individuals who live or were raised in an Appalachian county) had an 81% increased risk and second generation white Appalachians (individuals whose parents live or were raised in an Appalachian county) had a 70% increased risk for diabetes over the general population of greater Cincinnati4. The Appalachian region as a whole has greater health disparities and higher mortality rates from the leading causes of death when compared with non-Appalachian areas5.
Given that the Appalachian region includes counties from the entire state of West Virginia and parts of 12 other states6, most state data concerning diabetes fail to detail specifics pertaining to the Appalachian region as a whole. Thus, type 2 diabetes incidence and prevalence among Appalachian residents who are impacted by low socioeconomic status (SES) and its associated health risks are poorly documented and understudied. Context and cumulative effects of SES have been shown to have important influences on health outcomes and diabetes self-management7. Persons with low SES are less likely than those with high SES to see an endocrinologist for care; for example, 67% with higher SES will see endocrinologists, while 50% with lower SES will see only GPs8. Health behaviors, access to and processes of care, and distal mediators (eg personal characteristics, health providers, communities, healthcare systems) are powerful influences on health outcomes. Little is known currently about the availability of diabetes education programs, strategies for diabetes education, or access to educational services in the Appalachian region.
Disease management primarily occurs outside of the observation of medical professionals with only a small amount of time spent in either conversation or treatment. A recent report cautioned that less than 12% of those with diabetes were actually meeting recommended goals for blood glucose, blood pressure or cholesterol levels and little change was noted from the previous decade9. A later report State of Diabetes in America: Striving for Better Control identified that, in a nationwide survey of 157 000 persons with type 2 diabetes, approximately 98% of those diagnosed agreed that blood sugar control is important, but 51% did not know the results of their last A1C test10. While pharmaceutical options and technologies become more available and refined, this inability to meet recommended clinical targets is perplexing.
Since the 1980s, a growing appreciation for diabetes education has occurred, accompanied by beliefs that education is essential for both diabetes prevention and self-management. However, simply knowing that diabetes education programs are being implemented says little about important elements such as the educator's qualifications, time spent teaching a content area, who receives what kinds of follow up, teaching strategy effectiveness, the length or frequency of education, availability of on-going education, or problems of access.
Diabetes self-management education
Education is a key component of diabetes prevention and self-management and provides individuals with skills and information essential for disease management and prevention of co-morbidities. Education plays a central role in improving glycemic control, enhancing quality of life, and reducing the risk of long-term complications11. Since the 1930s, diabetes education has been viewed as an important process in teaching individuals to manage diabetes12. Healthy People 2010 set a diabetes-related goal to increase the 1998 proportion of individuals with diabetes who receive formal diabetes education to 60%13. In 2000, 50% of US individuals with diabetes had received formal diabetes education14. People who have received diabetes education are more likely to self-monitor their blood glucose on a daily basis than those who have not had diabetes education15. However, lack of motivation, physician referrals, program availability, and health insurance status prevent many individuals from attending diabetes education classes16. Additionally, residence in health professional shortage areas generally implies a lessened access to medical specialists17.
The availability of certified diabetes educators (CDEs) may be limited based on geographic location, a particular concern for those living in relatively impoverished regions such as Appalachia18. Diabetes educators and other health professionals are challenged to reframe their roles and practices in ways that empower individuals to meet stated concerns, clarify authentic priorities, and operate within the limits of patient resources19. An absence of well- prepared diabetes educators is likely to mean that services are provided by nurses who may or may not be well-prepared to deliver current diabetes education or understand the best practices for diabetes management. Residents of rural regions are more likely to have needs different from those residing in urban areas20. Thus, it is important to consider additional burdens on diabetes educational needs that might be placed on individuals and families living in remote areas when they have long been challenged by generational poverty, lack of employment or under-employment, lower levels of educational attainment, and underserved medical areas17,21,22. Research suggests that many people in Appalachia place great value in faith, family, community, honesty, independence, self-reliance, place, and traditions23-26. Diabetes education efforts should be cognizant of such issues.
Individuals typically attend formal diabetes education programs through physician referral and consider the programs to be the single source of diabetes information27. Certified diabetes educators are primarily responsible for providing diabetes education because they possess the distinct and specialized knowledge needed to promote quality care for persons with diabetes28. However, persons qualified as a CDE are not available in all rural areas. The aim of this study was to examine provider perceptions concerning the provision and accessibility of diabetes education, according to levels of economic distress and rurality throughout the Appalachian region.
Methodology
Study design
In 2006, a cross-sectional 40 item survey concerning diabetes education, healthcare providers, services, and resources was distributed to the health departments (HDs) and Federally Qualified Health Centers (FQHC) for all 410 counties then designated6. These counties are dispersed across 13 states, including all of West Virginia and portions of 12 other states. The survey instrument was constructed by a research team knowledgeable about diabetes education issues, with input from several diabetes experts. It was then pilot-tested with approximately 30 diabetes educators. Based on feedback from the pilot test, the short-answer instrument was modified and then reviewed again by several diabetes and community experts.
Potential participants were initially identified through a search for HD and FQHCs in Appalachian counties. Questionnaires were mailed to the identified facilities accompanied by a letter that asked for the person most knowledgeable about diabetes to complete the survey. Certified diabetes educator participants were identified through the most current internet list of those living in Appalachian counties and certified by the American Association of Diabetes Educators. A cover letter was included to explain the purpose of the study along with an informed consent form, and a stamped, self-addressed return envelope. The Institutional Review Board from the Ohio University Office of Research and Sponsored Programs approved the study protocol and questionnaire data collection.
A total of 850 surveys were mailed with 197 surveys returned and 182 of these surveys were complete and used in the analysis. Thus, the total return rate of surveys was 23.2% with 21.4% useable surveys. Many FQHC sites had multiple sites (n=43) where 2-12 agencies had some affiliation with one another. This information was unknown when the surveys were mailed, but became clear when some survey recipients wrote notes on their completed questionnaires or inquired prior to completing them. At least one questionnaire was return from 17 of these multi-sites (39.53%).
Of the total 182 returned questionnaires, 54 were derived from FQHC sites, 81 from HD, and 47 from diabetes educators (46 employed in hospitals or clinics and one from a health department). Over one-third of the Appalachian counties (37%; 152/410) were represented in the survey responses.
To determine the extent to which respondents from various counties are representative of the non-respondent counties, several census-derived variables were examined for all counties in the Appalachian region. No statistically significant county differences were found in percentage minority, poverty, unemployment, high school graduates, mean per capita income, number of physicians per 100 000 population, or health, social, or educational workers. While respondent counties (35.4%) were more likely to be urban than non-respondent counties (27.6%), the actual differences were small and may be reflective of fewer facilities being located in more rural locations. Rurality was measured and defined according to the Rural-Urban Continuum, developed by the Economic Research Service, a branch of the United States Department of Agriculture. This classification system is used to differentiate between metropolitan and nonmetropolitan areas. These two areas are further subdivided into a nine-part county code consisting of three metropolitan groups and six non-metropolitan groups. The Rural-Urban Continuum is also used to classify counties, census tracts, and zip codes by their degree of rurality29.
The survey had a broader base of questions than discussed in this article; a separate article describes the provider perspectives29. Several questions on this descriptive survey instrument focused on diabetes education. Specifically, questions were included that identified the person with primary responsibility for providing diabetes education and the characteristics of diabetes education classes (frequency, length, type of participants, and attendance patterns). According to the healthcare providers' points of view, patient barriers to accessing education and provider problems with offering diabetes education were itemized. Participant responses were also considered in terms of cultural appropriateness and reading level of patient education materials.
Long-term measure of socioeconomic status for county of survey origin: Based on US Census Data from 1960 to 2000, the authors classified county of origin for each of these questionnaires into a measure of historical SES, that is distressed or at-risk (DAR) versus non-distressed or at-risk (NDAR). In 4 out of 5 decennial census years from 1960 to 2000, distressed counties exhibited poverty and unemployment at least 1.5 times the national average and per capita market income (PCMI) at no more than two-thirds of the national average or poverty of at least twice the national average plus meeting either the unemployment or PCMI criteria. At-risk counties were defined with the threshold for poverty and unemployment at 1.25 with the same PCMI criterion or meeting two of the three distressed criteria. The non-distressed and non-at-risk (NDAR) counties did not meet either of these sets of criteria.
Data sources: Information regarding provider perceptions of diabetes education, its characteristics and barriers were collected through the present study questionnaire. United States Census data were the source of historical SES, physician availability, health, social and educational worker availability, poverty rates and percentage of the population younger than 18 years.
Data analysis
All questionnaire data entry and statistical analyses were conducted with SPSS version 14.0 (SPSS Inc., Chicago, IL, 2005; www.spss.com). Descriptive analyses were performed according to the dichotomized DAR status variable. Crosstabs of categorical variables were tested with the χ2 statistic and corresponding p-value. All significance tests were compared to the p-value <0.05.
Via an iterative modeling process, demographics, characteristics of diabetes education, patient barriers and patient education materials were tested as dependent variables in separate backwards logistic regression models. Each of these models was adjusted for the effects of the following independent variables: DAR status, percentages of poverty and residents at least 65 years of age, level of population density (rurality), and type of responding organization (health department vs clinic/hospital). The primary independent variable was DAR status. Other independent variables or covariates were chosen due to their relationship with DAR status. Individuals over age 65 years were chosen over individuals 17 years and under due to the disproportionate burden of diabetes carried by population of elders. Adjusted odds ratios (aOR) and their 95% confidence intervals were calculated. Since each of these OR were calculated with cross-sectional data, the prediction of either the dependent variable or the principal independent variable and their associated interpretations were considered appropriate. Therefore, in general, these models were interpreted as DAR predicting the dependent variable with NDAR status as the referent level.
Results
Of the 82 questionnaires originating from DAR locations and the 100 questionnaires from NDAR locations, the DAR responses were more likely to be from rural locations (p <0.001) (Table 1). Respondents from HDs tended to be from DAR locations(p=0.041). Although no differences in health, social and educational workers by DAR status were observed, the mean number of physicians per 100 000 in DAR locations, 59.1, was approximately one-third those in NDAR locations, 166.9 (p < 0.001). The poverty rates in DAR areas were almost double those for NDAR (20.5% vs 12.9%, p<0.001) and the percentage of children under 18 years was higher in DAR areas, but the proportions of residents who were at least 65 years were similar for both DAR and NDAR status.
To what extent any diabetes education programs and separate type 1 and type 2 diabetes education classes were offered was not influenced by DAR status (Table 2). Family participation was found almost three times more often in DAR versus NDAR locations (2.87 [1.11, 7.41]), when adjusting for rurality, percentage poverty, percentage elderly and type of healthcare setting. Classes were more likely to be offered on a single day than multiple days in DAR locations (2.42 [1.02, 5.71]). The DAR locations had a lower percentage of patients attending at least one diabetes class. The rate of attendance, however, was associated more with healthcare settings where only 17.1% of health departments, 28.8% of clinics and 57.7% of hospitals reported a greater than 50% patient attendance at any diabetes education classes (p=0.002). A CDE was 70% less likely to be the primary educator for DAR sites than for NDAR sites (aOR=0.33 [0.13, 0.85]; p=0.022). Nurses were equally likely to be the primary educator at both DAR and NDAR sites (p not significant). Health literacy was more of a concern than general literacy level for all locations and DAR areas were over twice as likely as NDAR areas (2.66 [1.10, 6.45]; p=0.031) to report health literacy as a concern.
Providers estimated what they thought were some of the significant barriers standing in the way of patients attending diabetes education sessions (Table 3). Transportation issues, including travel time, lack of public transport, having no one to drive them, and gas money, were considered moderate to important patient barriers for provider respondents in both DAR and NDAR areas. Literacy was also considered to be a moderate barrier for patients in both DAR and NDAR areas. In contrast, DAR providers (40.3%) versus NDAR providers (64.6%) were less likely to perceive a lack of insurance as a barrier (p=0.003). Providers also rated their perceived resource limitations in terms of providing diabetes education programs. The DAR providers were significantly more likely than NDAR providers to report a lack of staff. Again, lack of insurance was a larger issue for NDAR providers (aOR=0.35 [0.18, 0.68]; p=0.002).
The DAR providers were more likely to report a lack of teaching resources, a difference that was no longer significant when adjusting for potential confounding factors. A lack of space became more important, however, for the DAR group after adjusting for confounders. No differences by DAR status in lack of provider time or patient reading level were observed.
In terms of the areas of education needed, many topics were considered important. Education concerning physician visits was found to be more important for NDAR areas and there was some evidence to suggest that medical management issues were more important for DAR locations. Otherwise, the other areas of education - including maintaining health routines, understanding medication, monitoring glucose, exercise, proper eating, and obesity - were found to be similarly important for both DAR and NDAR locations.
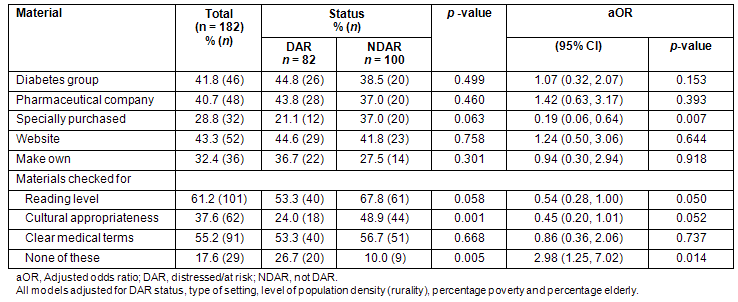
Regarding home-use diabetes education materials, DAR areas were 80% less likely than NDAR areas to use materials that they specifically purchased (p=0.007) (Table 4). The DAR and NDAR areas were equally likely to use materials received from national diabetes organizations, pharmaceutical companies, websites, and other groups or make the materials themselves. More than half of both DAR and NDAR respondents reported that they reviewed their home-use educational materials for reading level and clear medical terms. However, DAR areas were approximately 50% less likely than NDAR areas to review these materials for reading level (p=0.050) or cultural appropriateness (p=0.052). In addition, DAR sites were three times less likely than NDAR sites to review their materials for any of these characteristics (p=0.014).
Table 1: Characteristics of the sample, according to distressed-at-risk status30,31
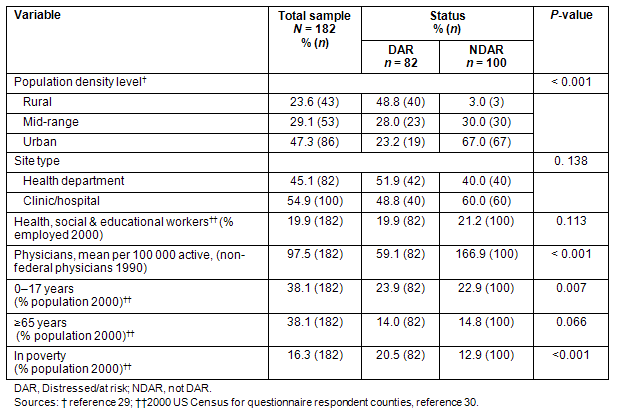
Table 2: Characteristics of diabetes education programs in Appalachia, according to distressed-at-risk status
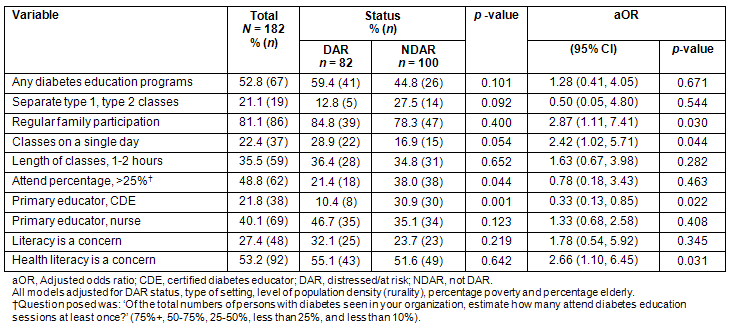
Table 3: Patient barriers, programmatic needs and areas of education needed for diabetes education sessions, according to distressed-at-risk status
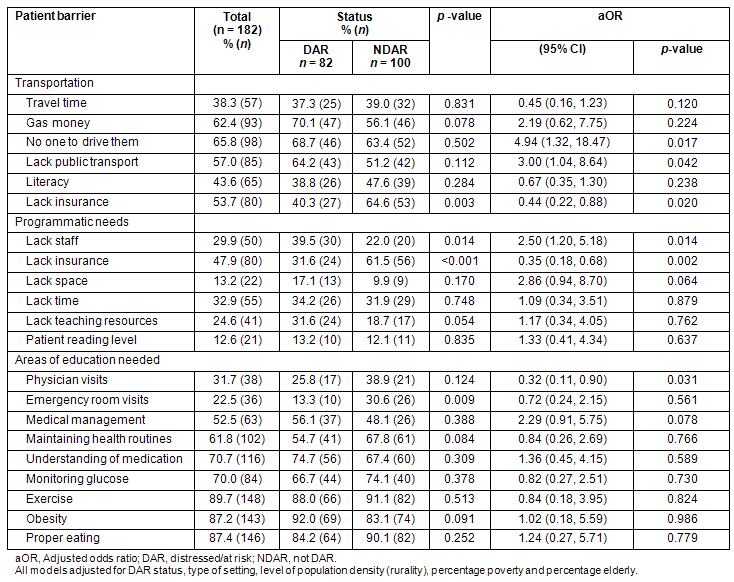
Table 4: Characteristics of diabetes home-use education materials, according to distressed-at-risk status
Discussion
Perceptions of health professionals regarding the delivery of diabetes education in distressed-at-risk (DAR) counties versus non-distressed-at-risk (NDAR) counties across the Appalachian region were examined for differences in perception based on location. Although some aspects of diabetes education were found to be less favorable in the more economically depressed DAR counties, many of the barriers to providing education affected patients and health professionals in both DAR and NDAR locations.
This study is one of the few studies to focus on the delivery of diabetes education in Appalachia. It serves as a useful hypothesis generating project for further examination of the issues surrounding diabetes education across a largely rural region. However, the sample size could be improved in a future study. The authors also did not fully account for the effect of questionnaires and their data that represented multiple sites. In describing Appalachia in terms of historically DAR and NDAR counties, the non-traditional categories may be confusing for consumption of the study results. By conducting a study of perceptions, the study data are by nature more qualitative and perhaps less repeatable than a study of facts and quantitative data.
Certified diabetes educators were less likely to be the primary providers of diabetes education in DAR areas compared to NDAR areas, while registered nurses were equally likely to be the primary providers of diabetes education. A registered nurse who is a CDE is more likely to be employed in a hospital than in a clinic or health department. This comparison of nurses does not distinguish between nurses who are CDEs and those who are not. It has been previously identified that nurses providing diabetes education may not be adequately prepared32. Given the tremendous changes in medical care over the last decade, any healthcare providers who have not kept pace will be likely to be providing less than optimal care. However, the cross-national Diabetes Attitudes Wishes and Needs (DAWN) study found that nurses should be more involved in care for their diabetes patients33. Adequacy of registered nurses' knowledge about diabetes and competence in providing diabetes education is an area that warrants further investigation.
Both DAR and NDAR sites offered diabetes education. A reference point for diabetes education set by the Behavioral Risk Factor Surveillance System questionnaire estimated that 50% of individuals with diabetes have ever attended diabetes education classes14. In this questionnaire, respondents from DAR locations were less likely than those from NDAR locations to report that at least half of their patients with diabetes had ever attended diabetes education classes. Less than 20% of HDs, found more often in DAR than NDAR areas, reported meeting the national standard estimate of formal education attendance. However, almost 60% of the CDEs participating from hospitals, had at least 50% of their patients with diabetes attending classes. Given that even limited formal diabetes education has been shown to improve self management outcomes for individuals with diabetes, it is troubling that many persons diagnosed with diabetes in Appalachia may not have access to diabetes education classes34.
Participants indicated that family involvement in diabetes education was encouraged by the majority, regardless of DAR status. The importance of family support has been documented35-38. Given the importance of family to those who identify with the Appalachian region, some greater intentional involvement of family members in diabetes education encounters may be beneficial23,26. When dietary routines were the concern, persons with diabetes encountered in healthcare settings were likely to identify differing levels of family support based on cultural heritage, family traditions, and food experiences that often fluctuated over time39. This study failed to gather information about the levels or types of family participation in the diabetes education activities, outcomes of this involvement, or the competence of the diabetes educators to work with families. These are compelling areas relevant to diabetes education that merit additional research.
Participants reported transportation issues and insurance coverage as primary barriers to attendance at diabetes educational sessions. Transportation was more commonly an issue for those residing in DAR locations, while lack of insurance was a greater issue for those in NDAR locations. Research regarding access to transportation and medical attention for chronic health conditions has confirmed that lack of transportation access results in less frequent care22. For example, research indicates that distance between a patient's residence and the healthcare facility negatively affect the access to care for cardiovascular disease40 and may have similar influence on diabetes outcomes. Therefore, it is essential that health care providers stress the importance of diabetes education and assess whether existing resources are available to overcome lack of transportation or other existing barriers.
The study findings indicated that those in NDAR locations were more likely to consider lack of insurance to be a barrier to diabetes education. This is an interesting finding, given that concerns for lack of insurance are usually associated with unemployment. Residents of NDAR locations, however, may be less likely to afford or be eligible for third-party reimbursement programs. Research indicates that the most common barrier to providing health care to persons with diabetes stems from no reimbursement from a third party16. Individuals with diabetes who lack insurance are less likely to access diabetes education classes compared with those who are covered by private insurance, Medicare, Medicaid or have health care provided by the Department of Veterans Affairs14. Economic needs have also been found to influence the provision of diabetes education and patient care in other parts of the USA27,41,42. Given the importance of the ability to self-manage diabetes independent of health professionals, access to diabetes education seems critical for reducing high costs linked with complications association with diabetes. National policies are needed to assure that all persons diagnosed with diabetes have access to diabetes education regardless of where they live.
While literacy was a moderate concern to the respondents, low health literacy was considered a more important factor related to the provision of diabetes education across the Appalachian region. Literacy needs have been found to be similar for both urban and rural clinics43. Although levels of health literacy do not affect whether individuals with diabetes are offered education, those who are uninsured or underinsured are more likely to have lower health literacy44. Additionally, low health literacy has been associated with negative diabetes outcomes such as poor glycemic control, retinopathy and cerebrovascular disease44. This study raises special concern about the need to address literacy and health literacy concerns when providing diabetes education to those residing in DAR as well as NDAR Appalachia.
Regarding the care providers' ability to offer educational sessions, study findings showed that lack of time, staff and teaching resources were relevant to not being able to do so. Sprague et al. have identified that problems with these same components, for example funding, staffing and materials, show insufficient internal organizational support for providing diabetes education27. In addition, educational areas that were deemed important for individuals with diabetes in Appalachia, such as exercise, dietary needs, maintaining healthy routines, and medication management were supported in the literature27,45.
In terms of the cultural sensitivity of diabetes education material for home use, DAR locations were less likely than NDAR areas to review these for appropriateness. Furthermore, DAR locations were also less likely to check the materials for reading level or clear use of medical terminology. Tailoring educational materials to those with low literacy needs can improve blood glucose control46. Since DAR areas are more likely to use materials given to them rather than purchase materials, they may have fewer human and financial resources to vet their patient education materials compared with NDAR areas. Patient education materials have been assessed at reading levels more than two levels higher than what is recommended for the average American adult43. Participants identified both literacy and health literacy as moderately important issues for those with diabetes. This perception could lead to a lack of attention to the adequacy of specific diabetes education material for individual needs. The perception that literacy concerns were being addressed could be an overestimation of the services rendered and deserves more carefully constructed research.
Overall, the diabetes education providers responding to this questionnaire perceived many similarities of concerns for educational programs in both DAR and NDAR areas of Appalachia. In terms of educational need, it appears that those diagnosed with diabetes living in the Appalachian region may not differ significantly from other parts of the USA. Study findings demonstrate that respondents from Appalachia perceive similar areas of need for persons with diabetes regardless of local economic conditions. In Appalachia, diabetes education is a challenge and underserved areas may face growing gaps between resources and needs. Although services are perceived to be available, measures of quality were not addressed in this study and should be considered in future research. Questions raised about family support, low health literacy, and outcomes of diabetes education warrant further examination.
References
1. WHO Media Centre. Diabetes. (Online) 2009. Available: http://www.who.int/mediacentre/factsheets/fs312/en/ (Accessed 12 September 2008).
2. Centers for Disease Control and Prevention. National diabetes fact sheet: general information and national estimates on diabetes in the United States, 2005. Atlanta, GA: US Department of Health and Human Services, Centers for Disease Control and Prevention, 2005.
3. Voeks JH, McClure LA, Go RC, Prineas RJ, Cushman M, Kissela BM et al. Regional differences in diabetes as a possible contributor to the geographic disparity in stroke mortality: the reasons for geographic and racial differences in stroke study. Stroke 2008; 39(6): 1675-1680.
4. The Health Foundation of Greater Cincinnati. 2005 Greater Cincinnati Community Health Status Survey: White Appalachian chart book. Cincinnati: University of Cincinnati, 2005.
5. Halverson J, Ma L, Harner E. An analysis of disparities in health status and access to health care in the Appalachian Region. (Online) 2004. Available: http://www.arc.gov/research/researchreportdetails.asp?REPORT_ID=82 (Accessed 3 May 2010).
6. Appalachian Regional Commission. Home page. (Online) no date. Available: http://www.arc.gov/index.jsp (Accessed 2 June 2010).
7. Brown AF, Ettner SL, Piette J, Weinberger M, Gregg E, Shapiro MF et al. Socioeconomic position and health among persons with diabetes mellitus: a conceptual framework and review of the literature. Epidemiology Review 2004; 26: 63-77.
8. Chin MH, Zhang JX, Merrell K. Specialty differences in the care of older patients with diabetes. Medical Care 2000; 38(2): 131-140.
9. National Diabetes Information Clearinghouse. Diabetes dateline: most people with diabetes do not meet treatment goals. (Online) 2004. Available: http://diabetes.niddk.nih.gov/about/dateline/spr04/1.htm (Accessed 9 August 2008).
10. American Association of Clinical Endocrinologists. State of diabetes in America. (Online) no date. Available: http://www.aace.com/public/awareness/stateofdiabetes/DiabetesAmericaReport.pdf (Accessed 9 August 2008).
11. Visser A, Snoek F. Perspectives on education and counseling for diabetes patients. Patient Education and Counseling 2004; 53(3): 251-255.
12. Bartlett EE. Historical glimpses of patient education in the United States. Patient Education and Counseling 1986; 8(2): 135-149.
13. Centers for Disease Control and Prevention. Levels of diabetes-related preventive-care practices - United States, 1997-1999. MMWR-Morbidity and Mortality Weekly Report 2000; 49: 954-958.
14. Nelson KM, Chapko MK, Reiber G, Boyko EJ. The association between health insurance coverage and diabetes care: data from the 2000 Behavioral Risk Factor Surveillance System. Health Services Research 2005; 40(2): 361-372.
15. Pan L, Mukhtar Q, Geiss MA, Division of Diabetes Translation, National Center for Chronic Disease Prevention and Health Promotion, CDC. Self-monitoring of blood glucose among adults with diabetes - United States, 1997-2006. MMWR -Morbidity and Mortality Weekly Report 2007; 56(43): 1133-1137.
16. Funnell MM, Donnelly MB, Anderson RM, Johnson PD, Oh MS. Perceived effectiveness, cost, and availability of patient education methods and materials. Diabetes Educator 1992; 18(2): 139-145.
17. Liu JJ. Health professional shortage and health status and health care access. Journal of Health Care for the Poor and Underserved 2007; 18(3): 590-598.
18. Behringer B, Friedell GH. Appalachia: where place matters in health. Prevention and Chronic Disease 2006; 3(4): A113.
19. Anderson RM, Funnell MM. Patient empowerment: reflections on the challenge of fostering the adoption of a new paradigm. Patient Education and Counseling 2005; 57(2): 153-157.
20. O'Brien T, Denham SA. Diabetes care and education in rural regions. Diabetes Educator 2008; 34(2): 334-347.
21. Arcury TA, Gesler WM, Preisser JS, Sherman J, Spencer J, Perin J. The effects of geography and spatial behavior on health care utilization among the residents of a rural region. Health Services Research 2005; 40(1): 135-155.
22. Arcury TA, Preisser JS, Gesler WM, Powers JM. Access to transportation and health care utilization in a rural region. Journal of Rural Health 2005; 21(1): 31-38.
23. Coyne CA, Demian-Popescu C, Friend D. Social and cultural factors influencing health in southern West Virginia: a qualitative study. Prevention and Chronic Disease 2006; 3(4): A124.
24. Hayes PA. Home is where their health is: rethinking perspectives of informal and formal care by older rural Appalachian women who live alone. Qualitative Health Research 2006; 16(2): 282-297.
25. Tessaro I, Smith SL, Rye S. Knowledge and perceptions of diabetes in an Appalachian population. Prevention and Chronic Disease 2005; 2(2): A13.
26. Lohri-Posey B. Middle-aged Appalachians living with diabetes mellitus: a family affair. Family and Community Health 2006; 29(3): 214-220.
27. Sprague MA, Shultz JA, Branen LJ, Lambeth S, Hillers VN. Diabetes educators' perspectives on barriers for patients and educators in diabetes education. Diabetes Educator 1999; 25(6): 907-916.
28. National Certification Board for Diabetes Educators. Home page. (Online) no date. Available: http://www.ncbde.org/ (Accessed 10 September 2008).
29. Denham SA, Wood LE, Remsberg K. Diabetes care: provider disparities in the US Appalachian region. Rural and Remote Health 10: 1320. (Online) 2010. Available: http://www.rrh.org.au (Accessed 2 June 2010).
30. Economic Research Service. Briefing rooms. Measuring rurality: Rural-Urban Continuum Codes. (Online) 2004. Available: http://www.ers.usda.gov/briefing/rurality/ruralurbcon/ (Accessed 10 August 2008).
31. US Census Bureau. US Census 2000. (Online) 2000. Available: www.census.gov (Accessed 11 April 2010).
32. El-Deirawi KM, Zuraikat N. Registered nurses' actual and perceived knowledge of diabetes mellitus. Journal of Vascular Nursing 2001; 19(3): 95-100.
33. Siminerio LM, Funnell MM, Peyrot M, Rubin RR. US nurses' perceptions of their role in diabetes care: results of the cross-national Diabetes Attitudes Wishes and Needs (DAWN) study. Diabetes Educator 2007; 33(1): 152-162.
34. Irvine AA, Mitchell CM. Impact of community-based diabetes education on program attenders and non-attenders. Diabetes Educator 1992; 18(1): 29-33.
35. Carbone ET, Rosal MC, Torres MI, Goins KV, Bermudez OI. Diabetes self-management: perspectives of Latino patients and their health care providers. Patient Education and Counseling 2007; 66(2): 202-210.
36. Carter-Edwards L, Skelly AH, Cagle CS, Appel SJ. 'They care but don't understand': family support of African American women with type 2 diabetes. Diabetes Educator 2004; 30(3): 493-501.
37. Epple C, Wright AL, Joish VN, Bauer M. The role of active family nutritional support in Navajos' type 2 diabetes metabolic control. Diabetes Care 2003; 26(10): 2829-2834.
38. Wen LK, Shepherd MD, Parchman ML. Family support, diet, and exercise among older Mexican Americans with type 2 diabetes. Diabetes Educator 2004; 30(6): 980-993.
39. Denham SA, Manoogian MM, Schuster L. Managing family support and dietary routines: Type 2 diabetes in rural Appalachian families. Family Systems Health 2006; 25(1): 36-52.
40. Whiteis DG. Third world medicine in first world cities: capital accumulation, uneven development and public health. Social Science and Medicine 1998; 47(6): 795-808.
41. Bell RA, Camacho F, Goonan K, et al. Quality of diabetes care among low-income patients in North Carolina. American Journal of Preventive Medicine 2001; 21(2): 124-131.
42. Chin MH, Cook S, Jin L, Drum ML, Harrison JF, Koppert J et al. Barriers to providing diabetes care in community health centers. Diabetes Care 2001; 24(2): 268-274.
43. Johnson JL, Stern EB. Readability of patient education materials: a comparison of rural and urban cardiac rehabilitation sites in Minnesota. Journal of Cardiopulmonary Rehabilitation 2004; 24(2): 121-127.
44. Schillinger D, Grumbach K, Piette J, Daher C, Palacios J, Diaz-Sullivan G et al. Association of health literacy with diabetes outcomes. JAMA 2002; 288(4): 475-482.
45. Funnell MM, Anderson RM, Nwankwo R, Gillard ML, Butler PM, Fitzgerald JT et al. A study of certified diabetes educators: influences and barriers. Diabetes Educator 2006; 32(3): 359-362, 364-356, 368-372.
46. Rothman R, Malone R, Bryant B, Horlen C, DeWalt D, Pignone M. The relationship between literacy and glycemic control in a diabetes disease-management program. Diabetes Educator 2004; 30(2): 263-273.


