Introduction Context Work disability prevention programs, aimed at reducing the incidence of workplace injuries and their associated work absences and costs, are typically developed in urban areas, with little attention given to their suitability for the rural context (note that the terms 'rural' and 'remote', as well as 'northern' or 'outback' used in countries including Canada and Australia relate to separate yet overlapping constructs; for simplicity, the term 'rural' was used for all). In this article, work disability prevention outcomes were defined as the incidence of occupational injury and the duration of associated work absence. Little is known about work disability in rural areas despite a large proportion of workers in industrialized countries being rural workers, including workers in the healthcare sector1-4. Healthcare workers in particular are vulnerable to poor work disability outcomes, including high injury rates, prolonged work absences, and high associated costs5-7. Accordingly, they present an excellent opportunity to compare rural and urban workers' rates of occupational injury and work absence duration. Despite the high costs of occupational injury and work absence8, which may be more significant in rural than urban areas, work disability and rural health have been studied in isolation. To understand rural workers' vulnerability to poor work disability outcomes, and to examine the interface between the fields of work disability prevention and rural health, a comprehensive literature review of work disability prevention for healthcare workers in rural areas was conducted. Issue Healthcare workers appear to be particularly vulnerable to occupational injury and prolonged work absence duration. In the USA in 2005, the healthcare sector accounted for the second largest number of non-fatal injuries and illnesses among all sectors, representing over 30% of all workplace injuries and illnesses involving time lost from work5. Similarly, in British Columbia, Canada, health care is responsible for the second largest proportion of lost work days due to occupational injury or illness, behind construction workers7. In Australia, the incidence of serious occupational injury claims is greater in health and community services than in any other industry6. Up to one-fifth of healthcare workers in industrialized countries live and work in rural areas, facing different working and social conditions than their urban counterparts9,10. Workers in rural areas face three unique challenges that may make them vulnerable to higher rates of poor work disability outcomes. First, rural residents are less healthy compared with urban residents in Australia, Canada, New Zealand, and many other developed countries10,11. They have overall poorer health, lower life expectancy, and higher infant mortality10. Rates of disability, violence, accidents and poisoning are greater in rural areas than in urban areas12. The health of residents in rural communities in Canada has been shown to decrease as the distance to an urban center increases12. Second, rural healthcare systems differ from urban systems in that they are more poorly resourced10,12. In Canada, although the per capita distribution of primary physicians may be relatively equal in rural and urban areas, the availability of specialist care is drastically reduced in rural areas10. Distance from and access to primary care services are additional major challenges10. Third, rural healthcare workers are socio-demographically different from urban healthcare workers, as will be discussed. Work disability prevention and rural health have been highly compartmentalized fields. This review aimed to provide a novel perspective on these fields by focusing on their junction and highlighting areas of vulnerability for work disability for rural workers, with a particular focus on healthcare workers. In this review, three main questions were asked:
- Are rural healthcare workers injured at work more frequently than urban healthcare workers?
- Is the duration of work absence more prolonged for rural healthcare workers who experience an occupational injury compared with urban healthcare workers?
- What are the risk factors for poor work disability prevention outcomes for rural healthcare workers, are these different from those in urban areas, and do they occur more frequently among rural healthcare workers?
The online databases of academic journals MEDLINE, CINAHL, and EMBASE were searched to identify all relevant English-language studies published between 1 January 2000 and 6 October 2009. The search was date restricted to ensure identified rural-urban disparities were representative of the contemporary context. In addition, the websites of research centers and government agencies in Australia, Canada, and the USA were searched with a focus on rural health or occupational safety (Fig1). Finally, the reference lists of articles selected for inclusion in the present review were hand-searched for additional articles of relevance, published since 1 January 2000.
The following concepts were used in the search: 'Rural' AND 'Work, occupational injury, work disability or risk factors' AND 'Countries or regions', with NOT 'Agricultural workers, non-working age populations, non-work related injuries' (Table 1). A broad cross-sector approach was chosen to ensure inclusion of studies of healthcare workers as a distinct group among other sectoral groups. Initially, the search was conducted using only the concepts for 'Rural' and 'Work, occupational injury, work disability or risk factors'. However, over half of the returned articles addressed agricultural workers and agricultural families or rural areas in developing countries; therefore, the exclusion criteria were expanded to remove articles about agricultural workers, non-working age populations, non-work related injuries, and low-income countries. Articles were included if they discussed occupational injury, associated work absence duration or known risk factors (such as poor disability management) for poor work disability outcomes among rural healthcare workers (Fig2); or if they included rural/urban comparisons of outcomes or risk factors in their analyses. Articles were selected that focused on high-income countries because of the potential for large differences in high-income and low-income countries' occupational categories, rural context-specific variables, and occupational health and safety practices13. The search concepts for rurality, work disability outcomes, and risk factors will be discussed in greater detail.
Table 1: Search terms used to identify literature about rural occupational injury, associated work absence duration and risk factors.

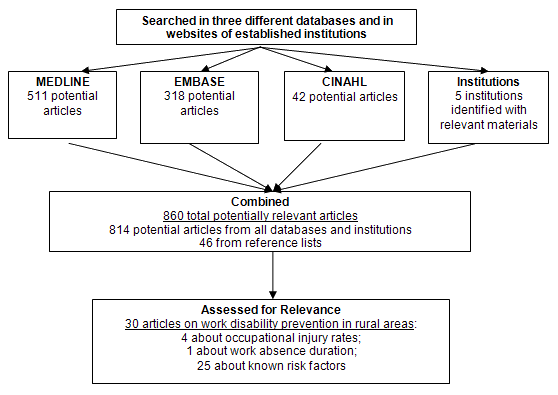 Figure 1: Search strategy to identify literature about rural occupational injury and associated work absence.
Figure 1: Search strategy to identify literature about rural occupational injury and associated work absence.
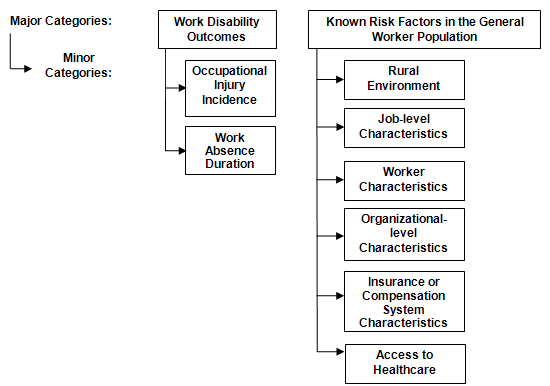 Figure 2: Major and minor search categories used to identify literature about rural occupational injury, associated work absence and risk factors.
Definition of rurality
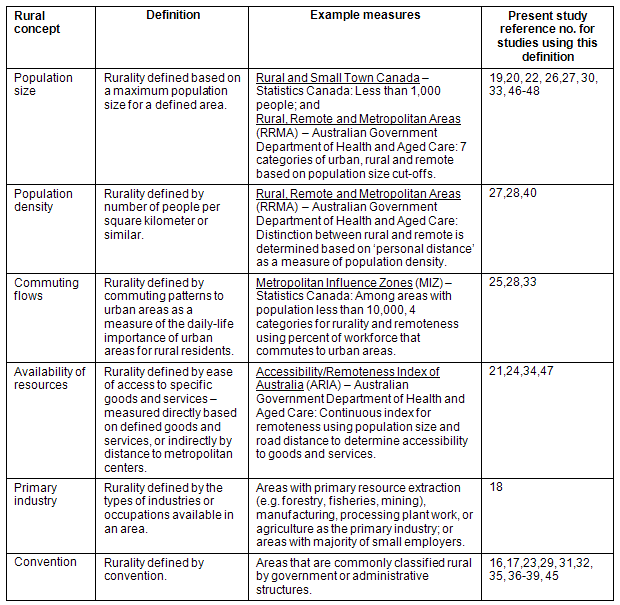
A common theme in the rural health literature is the lack of a single, clear definition of 'rural'. Common definitions incorporate notions of community size, distance to population centers, access to services, occupational landscapes (such as employer size, and main industries) or commuting patterns14,15. The search was not restricted to a single definition of rurality; rather, a variety of terms was used to identify articles about rural populations, rural health, rural health services, and medically underserved populations, and combined these with terms to identify work injury and disability prevention. Ultimately, the following definitions of rurality were accepted for inclusion in this review: small population size, low population density, primarily agricultural industry composition, lack of accessible goods and services, lack of accessible specialist healthcare in an area with low population size or density, limited commuting to population centers, and areas conventionally classified as rural by their governments (Table 2).
Table 2: Definitions of rurality used in the identified literature about rural occupational injury, associated work absence and risk factors16-48
Figure 2: Major and minor search categories used to identify literature about rural occupational injury, associated work absence and risk factors.
Definition of rurality
A common theme in the rural health literature is the lack of a single, clear definition of 'rural'. Common definitions incorporate notions of community size, distance to population centers, access to services, occupational landscapes (such as employer size, and main industries) or commuting patterns14,15. The search was not restricted to a single definition of rurality; rather, a variety of terms was used to identify articles about rural populations, rural health, rural health services, and medically underserved populations, and combined these with terms to identify work injury and disability prevention. Ultimately, the following definitions of rurality were accepted for inclusion in this review: small population size, low population density, primarily agricultural industry composition, lack of accessible goods and services, lack of accessible specialist healthcare in an area with low population size or density, limited commuting to population centers, and areas conventionally classified as rural by their governments (Table 2).
Table 2: Definitions of rurality used in the identified literature about rural occupational injury, associated work absence and risk factors16-48
 Outcomes
Two primary outcomes were focused on: occupational injury rates and associated work absence duration (Fig2). Injury rate measures that were accepted included point prevalence rates of work-related illness or injury, including work-related pain, and incidence rates of workplace injuries or illnesses per worker or per full-time equivalent. Work absence duration measures that were accepted included point prevalence rates of return to work (ie, the proportion of workers who returned to work by a specified time), and the mean or median duration of work absence after a specified time interval, for time to first return to work or cumulative days of work absence over a given period.
Selection of risk factors
To understand the risk factors associated with potential rural-urban disparities in work disability outcomes, studies were identified that assessed or discussed known risk factors for work disability, with or without relating them directly to work disability. Search terms for risk factors are listed in the 'Work, occupational injury, work disability or risk factors' search concept (Table 2). Known risk factors for occupational injury and prolonged work absence duration were identified based on public health knowledge of rural health10, systematic reviews49-50, and internationally recognized conceptual frameworks in work disability prevention51 (Fig2 gives categories of risk factors).
Results
The database and institutional searches identified 814 references, 25 of which were selected for inclusion. Review of the reference lists of these 25 articles, led to the identification of an additional 46 potentially relevant articles. Of the 860 references identified in this way, a total of 30 were selected for inclusion: 5 addressing work disability prevention outcomes and 25 discussing known risk factors. The findings of these studies are described in detail here, and summarized in Tables 3 and 4 (work disability prevention outcomes, and risk factors, respectively).
Table 3: Summary of the identified literature about occupational injury and work absence duration in rural workers16-20.
Outcomes
Two primary outcomes were focused on: occupational injury rates and associated work absence duration (Fig2). Injury rate measures that were accepted included point prevalence rates of work-related illness or injury, including work-related pain, and incidence rates of workplace injuries or illnesses per worker or per full-time equivalent. Work absence duration measures that were accepted included point prevalence rates of return to work (ie, the proportion of workers who returned to work by a specified time), and the mean or median duration of work absence after a specified time interval, for time to first return to work or cumulative days of work absence over a given period.
Selection of risk factors
To understand the risk factors associated with potential rural-urban disparities in work disability outcomes, studies were identified that assessed or discussed known risk factors for work disability, with or without relating them directly to work disability. Search terms for risk factors are listed in the 'Work, occupational injury, work disability or risk factors' search concept (Table 2). Known risk factors for occupational injury and prolonged work absence duration were identified based on public health knowledge of rural health10, systematic reviews49-50, and internationally recognized conceptual frameworks in work disability prevention51 (Fig2 gives categories of risk factors).
Results
The database and institutional searches identified 814 references, 25 of which were selected for inclusion. Review of the reference lists of these 25 articles, led to the identification of an additional 46 potentially relevant articles. Of the 860 references identified in this way, a total of 30 were selected for inclusion: 5 addressing work disability prevention outcomes and 25 discussing known risk factors. The findings of these studies are described in detail here, and summarized in Tables 3 and 4 (work disability prevention outcomes, and risk factors, respectively).
Table 3: Summary of the identified literature about occupational injury and work absence duration in rural workers16-20.
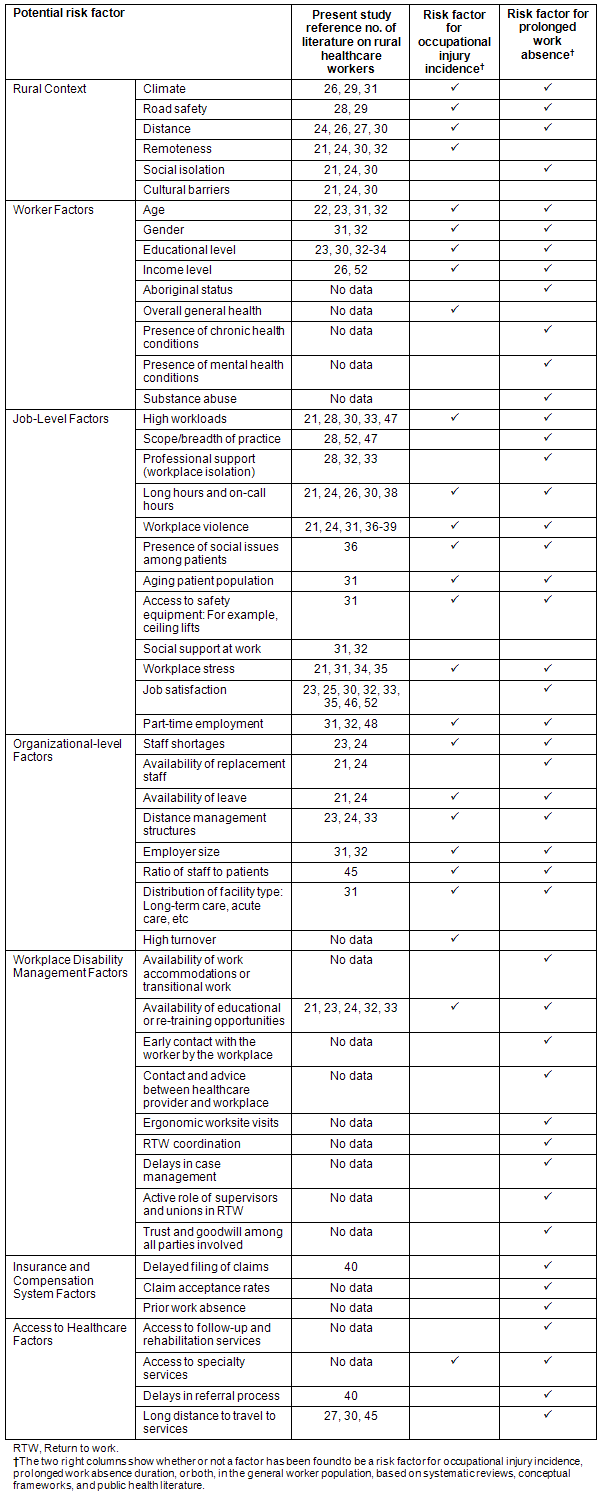
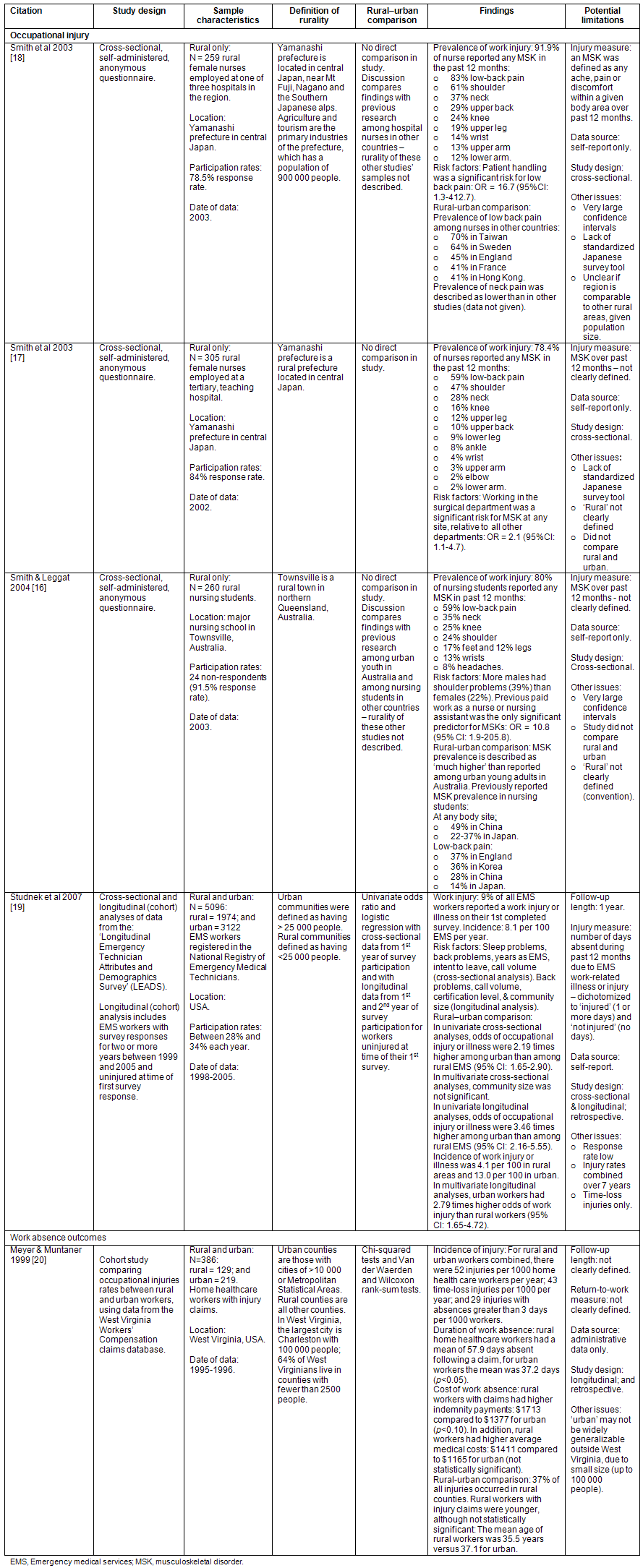 Table 4: Known risk factors for occupational injury and poor work disability outcomes21-40,45-48,52.
Table 4: Known risk factors for occupational injury and poor work disability outcomes21-40,45-48,52.
 Occupational injury rates
Four studies specifically assessed injury among rural healthcare workers16-19 (Table 3). Rates of workplace injuries/illnesses were remarkably high in rural healthcare workers: Smith et al, in a series of studies, found that 12 month incidence rates of musculoskeletal disorders (MSKs) among rural healthcare workers were 80% in Australian nursing students16, 80% in Japanese nurses17, and 92% in another study of Japanese nurses18. Lower back pain was the most common type of disorder, with prevalence rates ranging from approximately 60%16,17 to 83%18.
Available studies comparing rural with urban healthcare workers have used previously published data from different countries. In these studies, rural healthcare workers were noted to have higher incidence rates of MSKs compared with the urban workers. Smith and Leggat16 compared findings of their study of Japanese nurses with the findings of an Australian study of young urban workers and concluded that 37% of young male workers and 32% of young female workers of any occupation in urban areas reported back pain in the previous year53, considerably less than the 60% of rural Australian nursing students in the Smith and Leggat16 study. When comparing rural with urban nurses, Smith et al18 found lower prevalence rates of low back pain in urban healthcare workers from other countries (41% of nurses in Hong Kong54 and 70% of nurses in Taiwan55) compared with nurses in rural Japan (83% of nurses in rural Japan18). However, the differences were not consistently found for other MSKs; for instance, the 12 month period prevalence rate of shoulder symptoms was 60% in Australia56, compared with 61% in rural Japan18. Overall, the comparability of urban with rural rates in these studies is seriously limited by the use of rates from other countries and other studies, and the lack of clear description of the urban and rural areas surveyed.
A longitudinal study of American emergency medical service (EMS) workers19 pointed to an opposite pattern, whereby urban EMS workers (defined as those in communities of > 25 000 people) were 2.8 times more likely than rural workers (in communities < 25 000 people) to have an occupational injury or illness, after controlling for call volume, certification level and previous back problems. This study raises the possibility that urban EMS workers may have higher exposure to risk factors than their rural counterparts.
Are rural workers injured at work more frequently? Although the evidence is conflicting, and limited by the fact that only one study directly compared rural with urban injury rates19, the reviewed findings suggest that injury or illness rates for rural healthcare workers may be higher than for urban healthcare workers, within the same occupational category, with the exception of EMS workers.
Work absence duration
Only one study, from the USA, examined work absence duration (Table 3)20. This study showed that, in West Virginia, work absence duration was more prolonged in rural home healthcare workers than in urban workers (rurality was defined as all counties without a city of at least 10 000 people and not located in a Metropolitan Statistical Area as defined by the US Census). The difference was large: rural workers had an average of 57.9 days of absence following an occupational injury, while urban workers averaged 37.2 days of absence20. The authors suggested that rural-urban differences in work absence duration may be related to reduced access to medical care or to workplace characteristics, such as unsafe work environments associated with higher levels of poverty among rural home healthcare clientele20.
Is duration of work absence more prolonged for rural workers? There is limited information about work absence duration among rural healthcare workers. The one available study20 found that rural home healthcare workers had longer average work absences than urban workers. More research is needed to determine if these findings are generalizable to other healthcare occupations, and in other settings.
Risk factors for injury and poor disability management outcomes
Potential risk factors were categorized (Table 4) as rural environment, worker characteristics, job-level characteristics, organizational-level characteristics, disability management characteristics, insurance or compensation system characteristics, and access to healthcare issues (Table 3). Interestingly, these a priori categories mapped closely to the main sources of work stress identified in a 2009 systematic review of remote area nurses in Australia: remote context, workload and scope of practice, community and workplace violence, and organizational issues such as poor management21.
In this review, 25 articles focused on risk factors. Of note, no study directly examined the relationship between the risk factors and work disability prevention outcomes, and very few studies examined workplace disability management processes.
The rural environment
For many healthcare workers, the isolation and beauty of rural environments is part of the attraction of rural areas22-24, and satisfaction with one's community can be an important predictor of rural healthcare workers' job satisfaction23,25; however, the geography and climate of rural areas can increase the vulnerability of rural healthcare workers. Rural workers must often travel large distances26,27, on sometimes dangerous roads24,28. In addition, hazardous weather conditions can compound dangerous road conditions in rural areas, particularly for home healthcare workers29. Home healthcare workers can be forced by inclement weather to stop seeing their clients if road access is reduced and, as a result, their income may be reduced during winter months29. Furthermore, icy sidewalks can increase the risk of slips, trips and falls29. Both climate and dangerous roads, combined with longer distances (and longer travel times), are clearly risk factors for occupational injury, as well as factors that complicate return-to-work processes by making the commute to work more challenging.
Social aspects of rural life also present challenges for workers. The insular and close-knit nature of a small community makes healthcare workers highly visible21,30. As a result, many healthcare workers report being approached for health-related advice during their non-working hours, making it difficult to maintain a work-personal life boundary24,30. In addition, being injured, absent from work, and facing return-to-work issues are highly private processes that can become difficult to manage in small communities where privacy is difficult to protect.
Many rural healthcare workers find the social isolation of rural life challenging21. The majority of rural healthcare workers did not grow up in the communities where they work, and so are often viewed as outsiders24,28. In Canada, 98% of nurses working in the northern territories and 40% of nurses working in rural British Columbia were educated in other provinces30, and 26% of physicians working in Canadian rural areas across the country graduated from medical schools outside of Canada57. Similarly, nearly half of the primary care physicians in rural parts of Florida were born outside the USA2; while in Australia, international medical graduates were found to make up over 30% of the rural medical workforce, but only 20% of the total medical workforce49. As a result, healthcare workers in rural areas often have a steep learning curve in cultural competency24,30. Rural nurses in both Canada and Australia have described the challenges of working with patients from unfamiliar cultures, especially when there are language barriers, religious or spiritual differences, differing views of gender roles or conflicting attitudes towards health and wellness21,24,30.
Worker characteristics
Work absence duration and number of episodes of work absence are increased in older workers58 and among women50. Rural nurses are often older than urban nurses31,32, possibly because older nurses are more likely to have the experience to perform at the high skill level required in rural nursing23. However, despite the challenging nature of rural nursing practice23,28,30,33, rural nurses have lower education levels than urban nurses30,32,57 and limited access to continuing education30-34.
No literature was found documenting levels of chronic health conditions, including mental health conditions, in rural healthcare workers, which are factors known to affect work absence duration in the general population of workers59-68. However stress is a recurring and important theme for rural healthcare workers21,31,34,35, and is associated with rural nurses having a greater likelihood of taking time away from work31.
Workplace characteristics
Workplace characteristics that are known risk factors for both prolonged work absence and the incidence of occupational injury in the general worker population include high job strain (for duration58,69-72 and for incidence70); low support at work69,70,72,73; time management aspects of work, such as number of hours worked and presence of shift work74,75; and high physical demands, which are associated with absence duration under all circumstances examined76 and with injury when combined with low rewards70. In addition, high job insecurity and poor organizational climate are associated with a higher incidence of workplace injuries74.
Workplace characteristics can also be beneficial. The positive interpersonal aspects of work, including improved nurse relationships with physicians, improved decision-making processes75, and higher levels of respect and support77, are associated with shorter work absence duration in the general worker population and appear to be of particular relevance for healthcare workers. Although these factors have not all been studied with a rural-urban lens, they are partly addressed by research on rural and urban healthcare workers, as will be discussed.
The heavy workloads of rural nurses have been particularly well documented21,28,30,32,33, with rural nursing being described as a 'multi-specialist' profession rather than a generalist one28, meaning that rural nurses need 'both a great diversity and depth of knowledge'(p.75)28. The multi-specialist nature of rural nursing is due to many factors, such as limited professional support available in rural healthcare settings, limited or no back-up for rural nurses, lack of physicians routinely available to provide on-the-spot consultations21,28, and the complex health needs of rural populations10,23. In many cases, a single rural nurse may be the sole healthcare provider in the community32, and even when rural nurses are working with colleagues, they may feel less supported at work and are more likely to report that their managers and supervisors set poor examples for safety31. Rural nurses are also less likely to believe that their own health and safety are high priorities for management31. Low support at work has been shown to be associated with prolonged work absence among all healthcare workers69,70,72,73.
Rural healthcare workers are often required to work long hours and have heavy on-call demands21,24,26, which may place them at increased risk for injury, or workplace violence, particularly for nurses working alone or in isolation. For example, GPs in rural Iceland are routinely on-call between 5 and 14 days each month26. Burdensome on-call demands are also reported from rural healthcare workers in Australia21,24 and Canada30. High workloads and long hours can present challenges for return to work for healthcare workers, and may result in prolonged work absence, especially if a worker is only physically able to return to shorter hours or modified duties74-76.
Exposure to violence has been identified as a major concern for rural healthcare workers24,31,36-38. Nurses are concerned about being on call and having to make house calls at night, with inadequate support and protection24, including inadequate safety features in buildings21. In an Australian study, 86% of remote area nurses reported experiencing violence or aggression at work in the previous 12 months, compared with 43% of urban nurses21. They also reported receiving limited or delayed support following critical incidents, such as violence24. However, working in a rural healthcare setting does not appear to confer higher risk of workplace violence. Although rural paramedics in Australia reported experiencing high levels of workplace violence, with 87.5% reporting some type of violence over a 12 month period, urban paramedics were equally likely to have experienced workplace violence39.
Possibly as a result of their higher exposure to certain workplace risks, there are also certain positive trends in workplace health and safety in rural areas, especially in terms of preventive measures. Indeed, Australian rural nurses, compared with urban nurses, were less likely to report blood-borne pathogens or noise levels as risks in their workplaces, more likely to receive training about workplace violence, more likely to have workplace health and safety inspections, and more likely to feel qualified to use safety equipment31. Although rural nurses report spending more time lifting and transferring patients than do urban nurses, they also report more frequent use of lifting devices or safety belts31. In addition, high skill discretion and decision authority are associated with reduced job strain78, an important risk factor for prolonged work absence, and the multi-specialist nature of rural nursing may provide protection against high job strain for rural nurses. Tellingly, high decision latitude, autonomy and work discretion have been found to be associated with high levels of job satisfaction among rural healthcare workers, including physicians52 and nurses32, as well as contribute to rural physicians' higher levels of job satisfaction compared with urban physicians52.
Organizational factors
Job-level risk factors may be exacerbated by organizational-level risk factors. Lack of replacement staff is a major source of stress and burnout for rural nurses and hampers their ability to take leave for personal, medical, or professional development reasons21,24. Lack of replacement staff can increase workload, which in turn can increase the risk of injury and present a challenge for return to work. It can also create resentment among co-workers, who may be required to increase their workloads24. Even when replacement staff are available, rural healthcare workers describe them as typically inexperienced and the workload of a returning worker can be great because of the work left incomplete by the replacement worker24. Importantly, healthcare workers who feel less replaceable, or who believe that their absence would be unfair to colleagues, are more likely to continue working while ill or injured79.
Rural healthcare workers are commonly managed by regional administrative structures located far away23,24,33. Rural nurses report believing that centrally located administrators fail to understand the challenges of rural nursing, especially the high workload and broad practice scope24,33. When asked to give advice to administrators, rural nurses in Canada stressed the importance of programs and policies developed specifically for rural areas rather than simply for urban settings, and the need for education and travel opportunities to gain experience with rare health conditions33. Rural nurses often report being left out of the decision-making process when administrators are located in urban areas23,33, and perceive distant managers as inaccessible and non-responsive to their concerns, lacking innovative thinking and not being engaged with workers or their communities24.
Workers in smaller facilities are known to have fewer opportunities for modified work duties following an occupational injury, due to the limited number of positions available in these facilities80. Within healthcare, rural workers appear to be more likely to work in smaller facilities. In Australia, for example, a national survey of nurses found that 90% of rural and remote nurses worked in facilities with less than 1000 employees, compared with 45% of urban nurses31. Community, palliative and nursing home care settings are also known to have higher rates of occupational injury20, and a higher proportion of rural nurses work in community, palliative or aged care31. Community care workers have less control over the safety of their environment, often work alone, and typically have no access to assistive equipment20; while in palliative and nursing home care, factors such as restricted patient mobility and increased rates of dementia affect the likelihood that workers will be injured81.
Insurance and compensation systems
Limited information was available about insurance and compensation system differences for rural and urban workers. An American study from Washington State found differences between rural and urban areas in claim filing time with the time from injury to claim filing longer in rural areas40. Rural providers filed 61% of their patients' claims within 7 days, whereas urban providers filed 70% within 7 days40. Delays in the processing of claims are associated with longer time to return to work41, not only due to the simple addition of days in the process, but possibly due to workers' sense of unfairness of the process42. Importantly, perceived procedural and relational injustice in the workplace has been shown to be associated with longer work absence duration among healthcare workers43,44.
Access to health care
Delays and difficulty accessing healthcare can significantly affect duration of work absence; challenges with access to healthcare in rural areas are well documented10. An Australian study highlighted the challenges for access to rehabilitation care, due to long distances covered, and higher client-therapist ratios for rural occupational therapists45. A similar study from Nebraska found that rural occupational therapists were routinely expected to travel large distances, often over 161 km (100 miles), to see patients27.
Are risk factors for poor work disability prevention outcomes different for rural workers? The studies discussed suggest that rural healthcare workers may be particularly vulnerable to poor work disability prevention outcomes because of their increased exposure to risk factors for poor work disability outcomes: older age, lower education levels, high workloads (long hours, extensive on-call demands, complex patient needs), low professional support, exposure to violence, lack of replacement staff, and working in small facilities and high-demand subsectors (community, palliative, and home care). They may face delays in the healthcare and compensation systems, as well as obstacles to access to the healthcare system for their own return-to-work issues. Finally, they operate in systems managed by regional administrations who are often located far away, and poorly attuned to the specific needs of rural healthcare workers.
Methodological limitations of studies of work disability prevention and associated risk factors in rural areas
Several methodological limitations in the literature about rural work injury and disability management were noted:
Occupational injury rates
Four studies specifically assessed injury among rural healthcare workers16-19 (Table 3). Rates of workplace injuries/illnesses were remarkably high in rural healthcare workers: Smith et al, in a series of studies, found that 12 month incidence rates of musculoskeletal disorders (MSKs) among rural healthcare workers were 80% in Australian nursing students16, 80% in Japanese nurses17, and 92% in another study of Japanese nurses18. Lower back pain was the most common type of disorder, with prevalence rates ranging from approximately 60%16,17 to 83%18.
Available studies comparing rural with urban healthcare workers have used previously published data from different countries. In these studies, rural healthcare workers were noted to have higher incidence rates of MSKs compared with the urban workers. Smith and Leggat16 compared findings of their study of Japanese nurses with the findings of an Australian study of young urban workers and concluded that 37% of young male workers and 32% of young female workers of any occupation in urban areas reported back pain in the previous year53, considerably less than the 60% of rural Australian nursing students in the Smith and Leggat16 study. When comparing rural with urban nurses, Smith et al18 found lower prevalence rates of low back pain in urban healthcare workers from other countries (41% of nurses in Hong Kong54 and 70% of nurses in Taiwan55) compared with nurses in rural Japan (83% of nurses in rural Japan18). However, the differences were not consistently found for other MSKs; for instance, the 12 month period prevalence rate of shoulder symptoms was 60% in Australia56, compared with 61% in rural Japan18. Overall, the comparability of urban with rural rates in these studies is seriously limited by the use of rates from other countries and other studies, and the lack of clear description of the urban and rural areas surveyed.
A longitudinal study of American emergency medical service (EMS) workers19 pointed to an opposite pattern, whereby urban EMS workers (defined as those in communities of > 25 000 people) were 2.8 times more likely than rural workers (in communities < 25 000 people) to have an occupational injury or illness, after controlling for call volume, certification level and previous back problems. This study raises the possibility that urban EMS workers may have higher exposure to risk factors than their rural counterparts.
Are rural workers injured at work more frequently? Although the evidence is conflicting, and limited by the fact that only one study directly compared rural with urban injury rates19, the reviewed findings suggest that injury or illness rates for rural healthcare workers may be higher than for urban healthcare workers, within the same occupational category, with the exception of EMS workers.
Work absence duration
Only one study, from the USA, examined work absence duration (Table 3)20. This study showed that, in West Virginia, work absence duration was more prolonged in rural home healthcare workers than in urban workers (rurality was defined as all counties without a city of at least 10 000 people and not located in a Metropolitan Statistical Area as defined by the US Census). The difference was large: rural workers had an average of 57.9 days of absence following an occupational injury, while urban workers averaged 37.2 days of absence20. The authors suggested that rural-urban differences in work absence duration may be related to reduced access to medical care or to workplace characteristics, such as unsafe work environments associated with higher levels of poverty among rural home healthcare clientele20.
Is duration of work absence more prolonged for rural workers? There is limited information about work absence duration among rural healthcare workers. The one available study20 found that rural home healthcare workers had longer average work absences than urban workers. More research is needed to determine if these findings are generalizable to other healthcare occupations, and in other settings.
Risk factors for injury and poor disability management outcomes
Potential risk factors were categorized (Table 4) as rural environment, worker characteristics, job-level characteristics, organizational-level characteristics, disability management characteristics, insurance or compensation system characteristics, and access to healthcare issues (Table 3). Interestingly, these a priori categories mapped closely to the main sources of work stress identified in a 2009 systematic review of remote area nurses in Australia: remote context, workload and scope of practice, community and workplace violence, and organizational issues such as poor management21.
In this review, 25 articles focused on risk factors. Of note, no study directly examined the relationship between the risk factors and work disability prevention outcomes, and very few studies examined workplace disability management processes.
The rural environment
For many healthcare workers, the isolation and beauty of rural environments is part of the attraction of rural areas22-24, and satisfaction with one's community can be an important predictor of rural healthcare workers' job satisfaction23,25; however, the geography and climate of rural areas can increase the vulnerability of rural healthcare workers. Rural workers must often travel large distances26,27, on sometimes dangerous roads24,28. In addition, hazardous weather conditions can compound dangerous road conditions in rural areas, particularly for home healthcare workers29. Home healthcare workers can be forced by inclement weather to stop seeing their clients if road access is reduced and, as a result, their income may be reduced during winter months29. Furthermore, icy sidewalks can increase the risk of slips, trips and falls29. Both climate and dangerous roads, combined with longer distances (and longer travel times), are clearly risk factors for occupational injury, as well as factors that complicate return-to-work processes by making the commute to work more challenging.
Social aspects of rural life also present challenges for workers. The insular and close-knit nature of a small community makes healthcare workers highly visible21,30. As a result, many healthcare workers report being approached for health-related advice during their non-working hours, making it difficult to maintain a work-personal life boundary24,30. In addition, being injured, absent from work, and facing return-to-work issues are highly private processes that can become difficult to manage in small communities where privacy is difficult to protect.
Many rural healthcare workers find the social isolation of rural life challenging21. The majority of rural healthcare workers did not grow up in the communities where they work, and so are often viewed as outsiders24,28. In Canada, 98% of nurses working in the northern territories and 40% of nurses working in rural British Columbia were educated in other provinces30, and 26% of physicians working in Canadian rural areas across the country graduated from medical schools outside of Canada57. Similarly, nearly half of the primary care physicians in rural parts of Florida were born outside the USA2; while in Australia, international medical graduates were found to make up over 30% of the rural medical workforce, but only 20% of the total medical workforce49. As a result, healthcare workers in rural areas often have a steep learning curve in cultural competency24,30. Rural nurses in both Canada and Australia have described the challenges of working with patients from unfamiliar cultures, especially when there are language barriers, religious or spiritual differences, differing views of gender roles or conflicting attitudes towards health and wellness21,24,30.
Worker characteristics
Work absence duration and number of episodes of work absence are increased in older workers58 and among women50. Rural nurses are often older than urban nurses31,32, possibly because older nurses are more likely to have the experience to perform at the high skill level required in rural nursing23. However, despite the challenging nature of rural nursing practice23,28,30,33, rural nurses have lower education levels than urban nurses30,32,57 and limited access to continuing education30-34.
No literature was found documenting levels of chronic health conditions, including mental health conditions, in rural healthcare workers, which are factors known to affect work absence duration in the general population of workers59-68. However stress is a recurring and important theme for rural healthcare workers21,31,34,35, and is associated with rural nurses having a greater likelihood of taking time away from work31.
Workplace characteristics
Workplace characteristics that are known risk factors for both prolonged work absence and the incidence of occupational injury in the general worker population include high job strain (for duration58,69-72 and for incidence70); low support at work69,70,72,73; time management aspects of work, such as number of hours worked and presence of shift work74,75; and high physical demands, which are associated with absence duration under all circumstances examined76 and with injury when combined with low rewards70. In addition, high job insecurity and poor organizational climate are associated with a higher incidence of workplace injuries74.
Workplace characteristics can also be beneficial. The positive interpersonal aspects of work, including improved nurse relationships with physicians, improved decision-making processes75, and higher levels of respect and support77, are associated with shorter work absence duration in the general worker population and appear to be of particular relevance for healthcare workers. Although these factors have not all been studied with a rural-urban lens, they are partly addressed by research on rural and urban healthcare workers, as will be discussed.
The heavy workloads of rural nurses have been particularly well documented21,28,30,32,33, with rural nursing being described as a 'multi-specialist' profession rather than a generalist one28, meaning that rural nurses need 'both a great diversity and depth of knowledge'(p.75)28. The multi-specialist nature of rural nursing is due to many factors, such as limited professional support available in rural healthcare settings, limited or no back-up for rural nurses, lack of physicians routinely available to provide on-the-spot consultations21,28, and the complex health needs of rural populations10,23. In many cases, a single rural nurse may be the sole healthcare provider in the community32, and even when rural nurses are working with colleagues, they may feel less supported at work and are more likely to report that their managers and supervisors set poor examples for safety31. Rural nurses are also less likely to believe that their own health and safety are high priorities for management31. Low support at work has been shown to be associated with prolonged work absence among all healthcare workers69,70,72,73.
Rural healthcare workers are often required to work long hours and have heavy on-call demands21,24,26, which may place them at increased risk for injury, or workplace violence, particularly for nurses working alone or in isolation. For example, GPs in rural Iceland are routinely on-call between 5 and 14 days each month26. Burdensome on-call demands are also reported from rural healthcare workers in Australia21,24 and Canada30. High workloads and long hours can present challenges for return to work for healthcare workers, and may result in prolonged work absence, especially if a worker is only physically able to return to shorter hours or modified duties74-76.
Exposure to violence has been identified as a major concern for rural healthcare workers24,31,36-38. Nurses are concerned about being on call and having to make house calls at night, with inadequate support and protection24, including inadequate safety features in buildings21. In an Australian study, 86% of remote area nurses reported experiencing violence or aggression at work in the previous 12 months, compared with 43% of urban nurses21. They also reported receiving limited or delayed support following critical incidents, such as violence24. However, working in a rural healthcare setting does not appear to confer higher risk of workplace violence. Although rural paramedics in Australia reported experiencing high levels of workplace violence, with 87.5% reporting some type of violence over a 12 month period, urban paramedics were equally likely to have experienced workplace violence39.
Possibly as a result of their higher exposure to certain workplace risks, there are also certain positive trends in workplace health and safety in rural areas, especially in terms of preventive measures. Indeed, Australian rural nurses, compared with urban nurses, were less likely to report blood-borne pathogens or noise levels as risks in their workplaces, more likely to receive training about workplace violence, more likely to have workplace health and safety inspections, and more likely to feel qualified to use safety equipment31. Although rural nurses report spending more time lifting and transferring patients than do urban nurses, they also report more frequent use of lifting devices or safety belts31. In addition, high skill discretion and decision authority are associated with reduced job strain78, an important risk factor for prolonged work absence, and the multi-specialist nature of rural nursing may provide protection against high job strain for rural nurses. Tellingly, high decision latitude, autonomy and work discretion have been found to be associated with high levels of job satisfaction among rural healthcare workers, including physicians52 and nurses32, as well as contribute to rural physicians' higher levels of job satisfaction compared with urban physicians52.
Organizational factors
Job-level risk factors may be exacerbated by organizational-level risk factors. Lack of replacement staff is a major source of stress and burnout for rural nurses and hampers their ability to take leave for personal, medical, or professional development reasons21,24. Lack of replacement staff can increase workload, which in turn can increase the risk of injury and present a challenge for return to work. It can also create resentment among co-workers, who may be required to increase their workloads24. Even when replacement staff are available, rural healthcare workers describe them as typically inexperienced and the workload of a returning worker can be great because of the work left incomplete by the replacement worker24. Importantly, healthcare workers who feel less replaceable, or who believe that their absence would be unfair to colleagues, are more likely to continue working while ill or injured79.
Rural healthcare workers are commonly managed by regional administrative structures located far away23,24,33. Rural nurses report believing that centrally located administrators fail to understand the challenges of rural nursing, especially the high workload and broad practice scope24,33. When asked to give advice to administrators, rural nurses in Canada stressed the importance of programs and policies developed specifically for rural areas rather than simply for urban settings, and the need for education and travel opportunities to gain experience with rare health conditions33. Rural nurses often report being left out of the decision-making process when administrators are located in urban areas23,33, and perceive distant managers as inaccessible and non-responsive to their concerns, lacking innovative thinking and not being engaged with workers or their communities24.
Workers in smaller facilities are known to have fewer opportunities for modified work duties following an occupational injury, due to the limited number of positions available in these facilities80. Within healthcare, rural workers appear to be more likely to work in smaller facilities. In Australia, for example, a national survey of nurses found that 90% of rural and remote nurses worked in facilities with less than 1000 employees, compared with 45% of urban nurses31. Community, palliative and nursing home care settings are also known to have higher rates of occupational injury20, and a higher proportion of rural nurses work in community, palliative or aged care31. Community care workers have less control over the safety of their environment, often work alone, and typically have no access to assistive equipment20; while in palliative and nursing home care, factors such as restricted patient mobility and increased rates of dementia affect the likelihood that workers will be injured81.
Insurance and compensation systems
Limited information was available about insurance and compensation system differences for rural and urban workers. An American study from Washington State found differences between rural and urban areas in claim filing time with the time from injury to claim filing longer in rural areas40. Rural providers filed 61% of their patients' claims within 7 days, whereas urban providers filed 70% within 7 days40. Delays in the processing of claims are associated with longer time to return to work41, not only due to the simple addition of days in the process, but possibly due to workers' sense of unfairness of the process42. Importantly, perceived procedural and relational injustice in the workplace has been shown to be associated with longer work absence duration among healthcare workers43,44.
Access to health care
Delays and difficulty accessing healthcare can significantly affect duration of work absence; challenges with access to healthcare in rural areas are well documented10. An Australian study highlighted the challenges for access to rehabilitation care, due to long distances covered, and higher client-therapist ratios for rural occupational therapists45. A similar study from Nebraska found that rural occupational therapists were routinely expected to travel large distances, often over 161 km (100 miles), to see patients27.
Are risk factors for poor work disability prevention outcomes different for rural workers? The studies discussed suggest that rural healthcare workers may be particularly vulnerable to poor work disability prevention outcomes because of their increased exposure to risk factors for poor work disability outcomes: older age, lower education levels, high workloads (long hours, extensive on-call demands, complex patient needs), low professional support, exposure to violence, lack of replacement staff, and working in small facilities and high-demand subsectors (community, palliative, and home care). They may face delays in the healthcare and compensation systems, as well as obstacles to access to the healthcare system for their own return-to-work issues. Finally, they operate in systems managed by regional administrations who are often located far away, and poorly attuned to the specific needs of rural healthcare workers.
Methodological limitations of studies of work disability prevention and associated risk factors in rural areas
Several methodological limitations in the literature about rural work injury and disability management were noted:
- There is limited documentation of the definitions of rurality, impeding direct comparison of study findings.
- Rural-urban comparisons are often made by comparing rural workers with urban workers from different studies, from different populations, and even from different countries.
- There are a limited number of studies relating risk factors to work disability outcomes.
- Most study findings have not been stratified by factors known to be related to work disability outcomes in healthcare workers including type of facility, type of nursing practice, or workplace factors such as job strain.
- Data about work disability prevention outcomes come primarily from Japan and the USA, while data about risk factors come primarily from Australia, potentially reducing the comparability of outcomes with risk factors, and potentially reducing the generalizability and applicability of findings to other contexts.
- No study has explicitly examined the outcomes of Aboriginal populations, despite their substantial representation in rural populations in many countries.
- Few risk factor studies have used longitudinal designs or multivariate statistical approaches, which greatly limits the certainty with which causal relationships between risk factor and outcome can be inferred.
This review points to a glaring lack of evidence about work disability prevention issues for healthcare workers in rural areas. Of the 860 references identified, 5 articles addressed specifically work disability prevention outcomes (with only 1 addressing work absence duration), and 25 focused on risk factors for work disability outcomes. Of those 25 studies, none directly related risk factors to work disability outcomes. The limited evidence is nevertheless consistently suggestive of higher rates of injury in rural healthcare workers compared with urban healthcare workers. Limited evidence points to more prolonged work absences in rural healthcare workers, and suggests that injury rates and work absence duration across the rural-urban continuum vary substantially according to occupational category. Of note, EMS workers and paramedics may not follow the same pattern as other healthcare workers. This finding suggests that urban settings may lead to higher levels of exposure to risk factors for EMS workers and paramedics than rural settings. The profile of the healthcare worker in rural areas emerges as one of an older worker facing extremely high work demands including long hours and high on-call demands, who is expected to be a multi-specialist with little educational or professional support, in a context of staffing shortage, and who responds to a patient population that presents with complex health and social needs. Workplace violence, lack of replacement staff, and challenges unique to rural contexts including hazardous roads, harsh climates, long distances, and isolation, are key risk factors for poor disability outcomes in rural healthcare workers. In addition, rural healthcare workers may face frustrations associated with being managed by centralized regional administrations, as well as delays and access challenges in the healthcare system following an occupational injury. Comparison with other sectors The findings of this review, that rural healthcare workers are highly vulnerable to work injury and prolonged work absence, and experience high prevalence of risk factors for poor work disability outcomes, are also found in the few studies of rural workers in other industrial sectors40,82-84. In addition, rural workers from other sectors likely share some of the risk factors for poor work disability outcomes identified in this review, including lack of access to health care and insurance systems, harsh climate and large distances, and limited access to re-training or continuing education opportunities, because these risk factors are largely determined at or above the community level. As a result, community-level interventions may hold the key to addressing work absence duration and work injury for all rural workers. A pilot program in rural upstate New York recently demonstrated the potential of community-level interventions to successfully reduce work absence duration, through a program of dedicated return-to-work coordinators working at the county-level, rather than at employer-level85. Strengths and limitations There are certain limitations to this review. First, systematic quality assessment of the reviewed studies was not performed and, consequently, we presented a narrative rather than systematic review. Second, the impact of various legal frameworks were not considered; this is a complex question that goes beyond the objectives of this review. Third, and for the same reason, the impact of immigration policy related to the legal frameworks was not considered. Fourth, direct and indirect costs of injury and work absence as an outcome were not examined. The strengths of the review are, first and foremost, that this review is the first to focus on the topic of work disability in rural healthcare workers. The comprehensiveness of the review represents a key strength - the search strategy was developed in such a way as to maximize the identification of all relevant studies, which is important when a review addresses a topic for the first time. Finally, both quantitative and qualitative studies were included in the review. Recommendations Although the data are sparse, several recommendations emerge from this review. In particular, this literature review suggests two promising future avenues to improve the work disability outcomes of rural healthcare workers:
- Healthcare and workers' compensation policies and processes should be tailored to the unique needs of workers in rural areas, taking into account access to healthcare challenges.
- More research is needed about rural-urban differences in work absence duration and about the relationship between risk factors for occupational injury and work disability prevention outcomes.
At the policy and practice levels, future research should focus on developing ways to improve access and quality of healthcare for rural workers, including a focus on the unique needs of Aboriginal healthcare workers. It should also focus on examining rural-urban differences for workplace disability management processes. These recommendations need to be tempered by the fact that important methodological limitations are pervasive in this area of research. It will be critical in future studies to address these by using comparable samples to examine rural-urban disparities and by developing a common definition of rurality applicable to multiple jurisdictions. The use of geographic information systems (GIS) techniques could potentially allow for a finer, and more systematic, categorization of rural and urban communities. These considerations may permit more rigorous documentation of the disparities in work disability outcomes of rural and urban workers, and in developing a better understanding of the sources and risk factors associated with these disparities. Finally, policy developers and administrators should be aware of the vulnerability of rural healthcare workers and ensure that occupational injury and work absence duration programs are tailored to meet the needs of rural workers. Acknowledgements This research was conducted at the Occupational Health and Safety Agency for Healthcare (OHSAH), and supported by funding from the New Emerging Team for Health in Rural & Northern British Columbia (NETHRN-BC) and from the British Columbia Environmental and Occupational Health Research Network (BCEOHRN). References 1. Australian Government Department of Health and Ageing. Report on the audit of health workforce in rural and regional Australia, April 2008. Commonwealth of Australia, Canberra: Australian Government Department of Health and Ageing; 2008. 2. Brooks RG, Mardon R, Clawson A. The rural physician workforce in Florida: a survey of US- and foreign-born primary care physicians. Journal of Rural Health 2003; 19(4): 484-491. 3. Canadian Institute for Health Information (CIHI). Canada's Health Care Providers, 2007. Ottawa: Canadian Institute for Health Information; 2007. 4. Hooker RS. Physician assistants and nurse practitioners: the United States experience. Medical Journal of Australia 2006; 185(1): 4-7. 5. National Institute of Occupational Safety and Health. State of the Sector: Healthcare and Social Assistance. Identification of research opportunities for the next decade of NORA, Report no.2009-139. Atlanta, GA: Department of Health and Human Services (NIOSH), 2009. 6. SafeWork Australia. Health and Community Services, Health information sheet. Canberra, ACT: SafeWork Australia, 2007. 7. WorkSafeBC. WorkSafeBC Statistics 2008.Vancouver, BC: WorkSafeBC, 2008. 8. Hashemi L, Webster BS, Clancy EA, Volinn E. Length of disability and cost of workers' compensation low back pain claims. Journal of Occupational and Environmental Medicine 1997; 39(10): 937-945. 9. Australian Institute of Health and Welfare. Demography. Canberra, ACT: Australian Government, 2008. 10. Romanow RJ. Rural and Remote Communities. In: Building on values: The future of health care in Canada. Saskatoon, SK: Commission on the Future of Health Care in Canada, 2002; 159-170. 11. Smith KB, Humphreys JS, Wilson MG. Addressing the health disadvantage of rural populations: how does epidemiological evidence inform rural health policies and research? Australian Journal of Rural Health 2008; 16(2): 56-66. 12. Ryan-Nicholls KD. Health and sustainability of rural communities. Rural and Remote Health 4(1):242. (Online) 2004. Available www.rrh.org.au (Accessed 6 October 2010). 13. Radon K, Ehrenstein V, Nowak D, Bigaignon-Cantineau J, Gonzalez M, Vellore AD et al. Occupational health crossing borders part 2: Comparison of 18 occupational health systems across the globe. American Journal of Industrial Medicine 2010; 53(1): 55-63. 14. du Plessis V, Beshiri R, Bollman RD, Clemenson H. Definitions of rural. Rural and Small Town Canada Analysis Bulletin 2001 3(3). Ottawa, ON: Statistics Canada, 2001. 15. du Plessis V, Beshiri R, Bollman RD, Clemenson H. Definitions of rural. Report no.61. Ottawa, ON: Statistics Canada, 2002. 16. Smith DR, Leggat PA. Musculoskeletal disorders among rural Australian nursing students. Australian Journal of Rural Health 2004; 12(6): 241-245. 17. Smith DR, Ohmura K, Yamagata Z, Minai J. Musculoskeletal disorders among female nurses in a rural Japanese hospital. Nursing Health Science 2003; 5: 185-188. 18. Smith DR, Kondo N, Tanaka E, Tanaka H, Hirasawa K, Yamagata Z. Musculoskeletal disorders among hospital nurses in rural Japan. Rural and Remote Health 3(3):241. (Online) 2003. Available www.rrh.org.au (Accessed 6 October 2010). 19. Studnek JR, Ferketich A, Crawford JM. On the job illness and injury resulting in lost work time among a national cohort of emergency medical services professionals. American Journal of Industrial Medicine 2007; 50(12): 921-931. 20. Meyer JD, Muntaner C. Injuries in home health care workers: an analysis of occupational morbidity from a state compensation database. American Journal of Industrial Medicine 1999; 35(3): 295-301. 21. Lenthall S, Wakerman J, Opie T, Dollard M, Dunn S, Knight S et al. What stresses remote area nurses? Current knowledge and future action. Australian Journal of Rural Health 2009; 17(4): 208-213. 22. Brockwell D, Wielandt T, Clark M. Four years after graduation: occupational therapists' work destinations and perceptions of preparedness for practice. Australian Journal of Rural Health 2009; 17(2): 71-76. 23. Molinari DL, Monserud MA. Rural nurse job satisfaction. Rural and Remote Health 8: 1055. (Online) 2008. Available www.rrh.org.au (Accessed 6 October 2010). 24. Weymouth S, Davey C, Wright JI, et al. What are the effects of distance management on the retention of remote area nurses in Australia? Rural and Remote Health 7(3):652. (Online) 2007. Available www.rrh.org.au (Accessed 6 October 2010). 25. Penz K, Stewart NJ, D'Arcy C, Morgan D. Predictors of job satisfaction for rural acute care registered nurses in Canada. Western Journal of Nursing Research 2008; 30(7): 785-800. 26. Olafsson S. Out of hours service in rural areas: An observational study of accessibility, attitudes and quality standards among general practitioners in Iceland. Scandinavian Journal of Primary Health Care 2000; 18: 75-79. 27. Peterson C, Ramm K, Ruzicka H. Occupational therapists in rural healthcare: A 'Jack of all trades'. Occupational Therapy and Health 2003; 17: 55-62. 28. MacLeod M, Browne AJ, Leipert B. Issues for nurses in rural and remote Canada. Australian Journal of Rural Health 1998; 6(2): 72-78. 29. Skinner MW, Yantzi NM, Rosenberg MW. Neither rain nor hail nor sleet nor snow: provider perspectives on the challenges of weather for home and community care. Social Science and Medicine 2009; 68(4): 682-688. 30. MacLeod ML, Kulig JC, Stewart NJ, Pitblado JR, Knock M. The nature of nursing practice in rural and remote Canada. Canadian Nurse 2004; 100(6): 27-31. 31. Timmins P, Hogan A, Duong L, Miller P, Kearney G, Armstrong F. Occupational health and safety risk factors for rural and metropolitan nurses: Comparative results from a national nurses survey. Canberra, ACT: Australian Safety and Compensation Council, 2008. 32. Andrews ME, Stewart NJ, Pitblado JR, Morgan DG, Forbes D, D'Arcy C. Registered nurses working alone in rural and remote Canada. Canadian Journal of Nursing Research 2005; 37(1): 14-33. 33. MacLeod ML, Martin Misener R, Banks K, Morton AM, Vogt C, Bentham D. 'I'm a different kind of nurse': advice from nurses in rural and remote Canada. Nursing Leadership (Toronto, Ontario) 2008; 21(3): 40-53. 34. Albion MJ, Fogarty GJ, Machin MA. Benchmarking occupational stressors and strain levels for rural nurses and other health sector workers. Journal of Nursing Management 2005; 13(5): 411-418. 35. Pinikahana J, Happell B. Stress, burnout and job satisfaction in rural psychiatric nurses: a Victorian study. Australian Journal of Rural Health 2004; 12(3): 120-125. 36. Alexander C, Fraser J. Occupational violence in an Australian healthcare setting: implications for managers. Journal of Healthcare Management 2004; 49(6): 377-390. 37. Tolhurst H, Baker L, Murray G, Bell P, Sutton A, Dean S. Rural general practitioner experience of work-related violence in Australia. Australian Journal of Rural Health 2003; 11(5): 231-236. 38. Tolhurst H, Talbot J, Baker L, Bell P, Murray G, Sutton A et al. Rural general practitioner apprehension about work related violence in Australia. Australian Journal of Rural Health 2003; 11(5): 237-241. 39. Boyle M, Koritsas S, Coles J, Stanley J. A pilot study of workplace violence towards paramedics. Emergency Medicine Journal 2007; 24(11): 760-763. 40. Sears JM, Wickizer TM, Franklin GM, Cheadle AD, Berkowitz B. Expanding the role of nurse practitioners: effects on rural access to care for injured workers. Journal Rural Health 2008; 24(2): 171-178. 41. Sinnott P. Administrative delays and chronic disability in patients with acute occupational low back injury. Journal of Occupational and Environmental Medicine 2009; 51(6): 690-699. 42. Franche RL, Severin CN, Hogg-Johnson S, Cote P, Vidmar M, Lee H. The impact of early workplace-based return-to-work strategies on work absence duration: a 6-month longitudinal study following an occupational musculoskeletal injury. Journal of Occupational and Environmental Medicine 2007; 49(9): 960-974. 43. Elovainio M, Kivimaki M, Vahtera J. Organizational justice: evidence of a new psychosocial predictor of health. American Journal of Public Health 2002; 92(1): 105-108. 44. Hepburn CG, Franche RL, Francis L. Successful return to work: The role of fairness and workplace-based strategies. International Journal of Workplace Health Management 2010; 3(1): 7-24. 45. Boshoff K, Hartshorne S. Profile of occupational therapy practice in rural and remote South Australia. Australian Journal of Rural Health 2008; 16(5): 255-261. 46. Harris MF, Proudfoot JG, Jayasinghe UW, Holton CH, Davies GPP, Amoroso CL et al. Job satisfaction of staff and the team environment in Australian general practice. Medical Journal of Australia 2007; 186(11): 570-573. 47. Hutten-Czapski P, Pitblado R, Slade S. Short report: Scope of family practice in rural and urban settings. Canada Family Physician 2004; 50: 1548-1550. 48. Sloan C, Pong R, Rukholm E, Larocque S, Pitblado JR. Full-time/part-time employment of nurses in small hospitals in rural and northern Ontario: Current status, issues and options. Sudbury ON: Center for Rural and Northern Health Research, Laurentian University, 2006. 49. Alexander C, Fraser JD. Education, training and support needs of Australian trained doctors and international medical graduates in rural Australia: a case of special needs? Rural and Remote Health 7(2):681. (Online) 2007. Available www.rrh.org.au (Accessed 6 October 2010). 50. Steenstra IA, Verbeek JH, Heymans MW, Bongers PM. Prognostic factors for duration of sick leave in patients sick listed with acute low back pain: a systematic review of the literature. Occupational and Environmental Medicine 2005; 62(12): 851-860. 51. Loisel P, Durand M-J, Berthelette D, Vezina N, Baril R, Gagnon D et al. Disability prevention: New paradigm for the management of occupational back pain. Disease Management & Health Outcomes 2001; 9(7): 351-360. 52. Ulmer B, Harris M. Australian GPs are satisfied with their jobs. Family Practice 2002; 19: 300-303. 53. McMeeken J, Tully E, Stillman B, Nattrass C, Bygott IL, Story I. The experience of back pain in young Australians. Manual Therapy 2001; 6(4): 213-220. 54. Yip Y. A study of work stress, patient handling activities and the risk of low back pain among nurses in Hong Kong. Journal of Advanced Nursing 2001; 36(6): 794-804. 55. Chiou WK, Wong MK, Lee YH. Epidemiology of low back pain in Chinese nurses. International Journal of Nursing Studies 1994; 31(4): 361-368. 56. Lusted MJ, Carrasco CL, Mandryk JA, Healey S. Self reported symptoms in the neck and upper limbs in nurses. Applied Ergonomics 1996; 27(6): 381-387. 57. Pong RW, Pitblado JR. Geographic distribution of physicians in Canada: Beyond how many and where. Ottawa, ON: Canadian Institute for Health Information, 2006. 58. Alexopoulos EC, Burdorf A, Kalokerinou A. Risk factors for musculoskeletal disorders among nursing personnel in Greek hospitals. International Archives of Occupational and Environmental Health 2003; 76(4): 289-294. 59. Collins JJ, Base CM, Sharda CE, Ozminkowski RJ, Nicholson S, Billotti GM et al. The assessment of chronic health conditions on work performance, absence, and total economic impact for employers. Journal of Occupational and Environmental Medicine 2005; 47(6): 547-557. 60. Franche RL, Carnide N, Hogg-Johnson S, Côté P, Breslin FC, Bültmann U et al. Course, diagnosis, and treatment of depressive symptomatology in workers following a workplace injury: A prospective cohort study. Canadian Journal of Psychiatry 2009; 54(8): 534-546. 61. Kessler RC, Barber C, Birnbaum HG, Frank RG, Greenberg PE, Rose RM et al. Depression in the workplace: Effects on short-term disability. Health Affairs 1999; 18(5): 163-171. 62. Kessler RC, Greenberg PE, Mickelson KD, Meneades LM, Wang PS. The effects of chronic medical conditions on work loss and work cutback. Journal of Occupational and Environmental Medicine 2001; 43(3): 218-225. 63. Kessler RC, McGonagle KA, Zhao S, Nelson CB, Hughes M, Eshleman S et al. Lifetime and 12-month prevalence of DSM-III-R psychiatric disorders in the United States: Results from the National Comorbidity Survey. Archives of General Psychiatry 1994; 18(5): 163-171). 64. Nordin M, Hiebert R, Pietrek M, Alexander M, Crane M, Lewis S. Association of comorbidity and outcomes in episodes of nonspecific low back pain in occupational populations. Journal of Occupational and Environmental Medicine 2002; 44(7): 677-684. 65. Ash P, Goldstein SI. Predictors of returning to work. Bulletin of the American Academy of Psychiatry and Law 1995; 23(2): 205-210. 66. Dozois DJA, Dobson KS, Wong MK, Hughes D, Long A. Factors associated with rehabilitation outcome in patients with low back pain (LBP): Prediction of employment outcome at 9-month follow-up. Rehabilitation Psychololgy 1995; 40(4): 243-259. 67. Garcy P, Mayer T, Gatchel R. Recurrent or new injury outcomes after return to work in chronic disabling spinal disorder: Tertiary prevention efficacy of functional restoration treatment. Spine 1996; 21(8): 952-959. 68. Lotters F, Franche RL, Hogg-Johnson S, Burdof A, Pole JD. The prognostic value of depressive symptoms, fear-avoidance, and self-efficacy for duration of lost-time benefits in workers with musculoskeletal disorders. Occupational and Environmental Medicine 2006; 63(12): 794-801. 69. Bourbonnais R, Mondor M. Job strain and sickness absence among nurses in the province of Quebec. American Journal of Industrial Medicine 2001; 39(2): 194-202. 70. Koehoorn M, Demers PA, Hertzman C, Village J, Kennedy SM. Work organization and musculoskeletal injuries among a cohort of health care workers. Scandinavian Journal of Work and Environmental Health 2006; 32(4): 285-293. 71. Seago JA. Work group culture, stress, and hostility. Correlations with organizational outcomes. Journal of Nursing Administration 1996; 26(6): 39-47. 72. Verhaeghe R, Mak R, Maele V, Kornitzer M, De Backer G. Job stress among middle-aged health care workers and its relation to sickness absence. Stress & Health 2003; 19(5): 265-274. 73. Petterson IL, Hertting A, Hagberg L, Theorell T. Are trends in work and health conditions interrelated? A study of Swedish hospital employees in the 1990s. Journal of Occupational Health and Psychology 2005; 10(2): 110-120. 74. Gershon RR, Stone PW, Zeltser M, Faucett J, MacDavitt K, Chou SS. Organizational climate and nurse health outcomes in the United States: a systematic review. Industrial Health 2007; 45(5): 622-636. 75. Shamian J, O'Brien-Pallas L, Thomson D, Alksnis C, Kerr M. Nurse absenteeism, stress and workplace injury: What are the contributing factors and what can/should be done about it? International Journal of Sociology and Social Policy 2003; 23(8/9): 81-103. 76. Shields M, Wilkins K, Statistics Canada, Health Canada, Canadian Institute for Health Information. Findings from the 2005 National Survey of the Work and Health of Nurses. Ottawa, ON: Statistics Canada, 2006. 77. Franche RL, Smith P, Ibrahim S et al. Multimorbidity, depression, and pain in the workplace: Potential risk factors for work absence in Canadian nurses. In: Proceedings, 2009 British Columbia Healthcare Workplace Health, Safety & Wellness Conference. 14-15 September 2009; Kelowna, BC; 2009. 78. Labriola M, Lund T, Burr H. Prospective study of physical and psychosocial risk factors for sickness absence. Occupational Medicine (London) 2006; 56(7): 469-474. 79. McKevitt C, Morgan M, Dundas R, Holland WW. Sickness absence and 'working through' illness: a comparison of two professional groups. Journal of Public Health Medicine 1997; 19(3): 295-300. 80. Eakin J, Clarke J, MacEachen E. Return to work in small workplaces: Sociological perspective on employers' and workers' experiences with Ontario's strategy of self reliance and early return. Report no.60. Toronto: Institute for Work & Health, 2003. 81. Myers D, Silverstein B, Nelson NA. Predictors of shoulder and back injuries in nursing home workers: a prospective study. American Journal of Industrial Medicine 2002; 41(6): 466-476. 82. McPhee CS, Lipscomb HJ. Upper-extremity musculoskeletal symptoms and physical health related quality of life among women employed in poultry processing and other low-wage jobs in Northeastern North Carolina. American Journal of Industrial Medicine 2009; 52(4): 331-340. 83. Young AE,, Cifuentes M, Wasiak R, Webster BS. Urban-rural differences in work disability following occupational injury: are they related to differences in healthcare utilization? Journal of Occupational and Environmental Medicine 2009; 51(2): 204-212. 84. Young AE, Wasiak R, Webster BS, Shayne RG. Urban-rural differences in work disability after an occupational injury. Scandinavian Journal of Work and Environmental Health 2008; 34(2): 158-164. 85. Lipscomb HJ, Moon SD, Li L, Pompeii L, Kennedy MQ. Evaluation of the North Country on the Job Network: a model of facilitated care for injured workers in rural upstate New York. Journal of Occupational and Environmental Medicine 2002; 44(3): 246-257.





