The genesis of this special issue 'Human Health at the ends of the earth' was stimulated by the reinvigorated interest in promoting circumpolar health during the International Polar Year (IPY) 2007-2008. The IPY occurs approximately every 50 years and is a major international polar research program intended to expand the boundaries of our understanding of the Polar Regions. However unlike previous polar years (1882-1883, 1932-1933 & 1957-1958) the 4th Polar Year, for the first time, focused significant attention to the human dimension of Arctic research, and in particular circumpolar health and wellbeing.
The circumpolar regions of the world include the areas in and around the Arctic and Antarctic circles. In the north, countries that touch the Arctic Circle include the USA (Alaska), Canada, Greenland, Iceland, Norway, Finland, Sweden, and the Russian Federation (Fig1). In the south, only Antarctica is considered 'circumpolar'. The climate in the Arctic varies geographically from severe cold in arid uninhabited regions to temperate forests bordering coastal agrarian regions. Approximately 4 million people live in the Arctic regions, roughly defined by 60°N latitude, with almost half residing in northern regions of the Russian Federation. These populations consist of varying proportions of Indigenous and non-Indigenous peoples1 (Fig1). For example, in Nunavut, Canada and Greenland approximately 85% of inhabitants are Inuit; however, in Iceland less than 1% are considered Indigenous peoples. In some northern regions, the proportion of Indigenous peoples, such as the Indigenous peoples of northern Europe, the Sami, may be difficult to discern because census data do not always include the designation. In Antarctica, the residents are transient scientists, explorers and occupational workers including passing shipping traffic. At both ends of the earth, remote access to health care is a concern; furthermore, at both ends of the earth, climate change has a disproportionate effect, compared with the non-circumpolar regions.
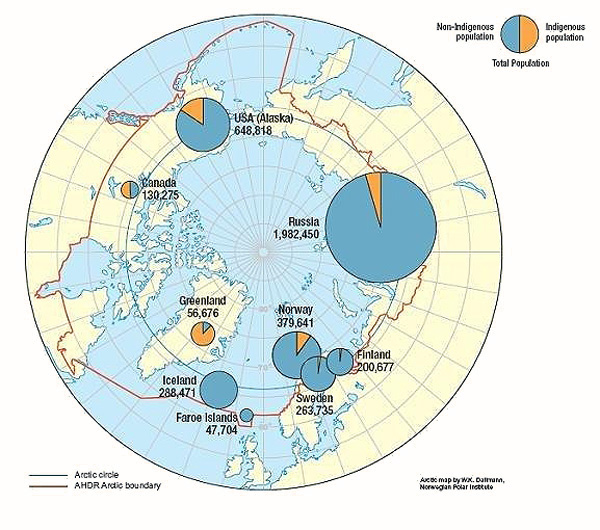
Figure 1: Map showing the Arctic Circle and a boundary of the circumpolar Arctic region as defined by the Arctic Human Development Report, including proportions of Indigenous and non Indigenous populations of the Arctic (reproduced with the permission of AHDR Stefansson Arctic Institute, Iceland).
Peoples of the northern circumpolar region continue to depend on subsistence hunting and fishing for a significant proportion of their diet. However, environmental contaminants are having an effect on food security2. Increased rates of infant mortality, birth defects, chronic disease and decreased life expectancy are concerns for some Indigenous populations in the Arctic3-7. For example, mortality rates for heart disease and cancer, once much lower among the Indigenous populations of the USA, Canada, and northern European countries, are now similar to their respective national rates. The Indigenous populations of Alaska, Canada, and Greenland have higher mortality rates for unintentional injury and suicide. Similarly, the infant mortality rate in Inuit populations is consistently three times higher than the rest of Canada3,8. A number of cohort and population studies are addressing these concerns with the input and involvement of the Indigenous peoples who have intimate insights into the impacts. Other health concerns of the Indigenous peoples of the Arctic include the high prevalence of certain infectious diseases, such as hepatitis B, Helicobacter pylori, respiratory syncytial virus (RSV) infections in infants, and sexually transmitted diseases9, as well as heath impacts associated with exposures to environmental pollutants, rapid economic change and modernization10. In addition, those living in Arctic regions are particularly vulnerable to the influences of climate change which are affecting food sources, the prevalence of infectious diseases, sanitation and water sources, as well as transport infrastructure, such as ice roads. The overarching effects of climate change are expected to impact on these populations disproportionately for years to come11.
For the Antarctic region, resident numbers are small so studies tend to be descriptive or qualitative. In some instances human health research in these remote stations has been used to inform and better understand elements of human behavior in space (additional information is available at http://humanresearch.jsc.nasa.gov/analogs/analog_antarctica.asp). Communities such as Argentinean Esperanza Base in Antarctica have family residents; medical services tend to be based on standards of the nation state of the base in Antarctica. Each of these locations focuses on acute care, utilizes a medivac system, and relocates individuals who are no longer able to work for any medical reason. Chronic conditions are rare in this region because affected individuals do not elect to live in such locations and would generally not be offered employment.
The depth and breadth of the articles in this special issue illustrate the vastness of human health issues in the circumpolar regions of our world. The articles include original research, project reports, including reports from ongoing IPY research projects, review articles and short communications. In addition, the authors hail from a variety of locations: Canada, Denmark, Greenland, Norway, Siberia, Sweden, and the UK. There are several themes apparent in the articles included in this special issue: the health status of individuals living in circumpolar regions; the impact of place on health; the accessibility of health services; and the preparation of health professionals.
The articles related to health status include residents from Canada, East Siberia, Greenland and Sweden. The articles from Canada include the Inuit in Nunavut, the Cree in Northern Ontario and the Inuit of Nunavik, Quebec. Gauthier, Simard and Blais focus on the necessity for rapid testing of game animals (ie traditional foods) for E. coli and Salmonella among residents in the Eastern Arctic to prevent health problems12. Two other articles are a result of the IPY project. In the Nunavut Inuit Child Health Survey, Egeland, Faraj and Osborne address Inuit preschoolers and recommend that overcrowded houses and poverty issues still require attention13. Pacey, Nancarrow and Egeland focus on oral health, noting that the Inuit have experienced higher rates of dental caries and calling for nutritional education to arrest this concern14. The Swedish population health survey is also the focus of an article. Igl, Johansson and Gyllensten discuss their representative population cross-sectional sample which combined community health and basic science research, comparing the health outcomes of those who lived a traditional lifestyle with those living a more modern lifestyle15. Differences between lifestyles and between sexes were noted. For those with traditional lifestyles, females more often had cardiovascular disorders, whereas males had orthopedic concerns. Mortality in extremes of weather conditions in the East Siberian city of Yakutsk is the focus of the report by Revich and Shaposhnikov16. Interestingly, both extreme heat and cold significantly increase the rate of mortality, which was found to be largely due to coronary heart disease and other non-accidental causes. Bonefeld-Jorgensen reviews the risks and effects of persistent organic pollutants (POPs) on the Arctic ecosystem in Greenland17. The findings note that although POPs are present in traditional foods, the positive effects of consuming such food needs also to be considered. A clinical outcome in Greenland is considered by Homøe and Jensen, who discuss acute mastoiditis among residents18. Although high rates of acute otitis media in small children would suggest an increased risk, this study clarifies that acute mastoiditis is not more common in this population. However, when it does occur, immediate medical and sometimes surgical management must be undertaken to prevent serious sequelae.
An over-riding theme for most manuscripts was the impact of place on health. Several of the submissions focus on personnel who work and therefore live, at least part-time, in circumpolar regions. Harris, Marquis, Eriksen, Grant, Corbett, Lie and Ursin focus on British Antarctica personnel who over-winter in one of the world's darkest places19. The study included a variety of testing including saliva cortisol, recording body complaints and concerns with sleep. They found no evidence of undue stress related to over-wintering among the personnel they followed, adding to our knowledge about the impacts of extreme changes on health.
The effects of climate change and its impacts become especially apparent, heightening our awareness that place really does matter. Nancarrow and Chan discuss climate change and the impacts on country food harvest from the perspective of Inuit from two communities in Nunavut20. Individuals spoke of their observations of the changes in availability of caribou, marine animals, birds and plants. Impacts on their diet were recognized, emphasizing that food security has been affected by climate change. One other article also focused on the lifestyle impacts of climate change, this one documenting impact on the Cree in Northern Ontario, Canada. Lemelin, Matthews, Mattina, McIntyre, Johnston, Koster, and the Weenusk First Nation at Peawanuck also confirm how climate change is prompting community members to make adaptive changes in their lifestyle demonstrating overall the Cree, consistent with history, are showing their resiliency21. The title 'Climate change, wellbeing and resilience in the Weenusk First Nation at Peawanuck: the Moccasin Telegraph Goes Global'21 brings in a second explored theme, of how combining the traditional with modern forms of communication is enhancing the Cree's ability, but with some challenges, to learn more about the issues affecting their traditional existence.
The third theme is the accessibility of health services which, like the previous theme, is a common thread in many of the submissions. Two submissions focused on the challenges of accessing services in northern Canada. Miller Mifflin and Bzdell discuss in their project report the way they were able to create a more equitable physiotherapy delivery system for those residents of the Baffin (Qikiqtani) region of Nunavut who are referred for services22. Their system of establishing priorities could be considered for other similar locales, or even in rural southern locations that are experiencing comparable concerns. O'Neill presents a review article, eloquently outlining the challenges that mental healthcare providers face in delivering care in northern locales23. Suggestions are given to guide practitioners about successful living and providing care under demanding circumstances.
The final theme, preparation of health professionals, is the focus of three articles. James, O'Brien, Bourret, Kango, Gafvels, and Paradis-Pastori describe their collaborative work to create a culturally safe midwifery program to meet the needs of Inuit families24. The history of traditional birthing contrasts with current practices and lays the groundwork for developing a robust birthing education program that is available in local communities. Finally, two inter-related articles focus on retaining physicians in northern Finland. The first, authored by Straume, Sondena and Prydz focuses on a postgraduate model that includes training groups for family physicians25. The longitudinal results are promising, indicating retention was positively affected by the intervention. In the final submission, Straume and Shaw talk about an intern support model also used to enhance retention of physicians26. Not only are professional concerns addressed through the use of this model, but also social factors including the experience of isolation, explaining, at least in part, its success.
Taken together, all the articles in this special issue of Rural and Remote Health inform us about the complexity of health and healthcare services in circumpolar regions. They serve as a baseline but also remind us that terms such as 'rural,' 'remote' and 'northern' are contextual experiences where place matters everyday on an individual and collective level.
References
1. Stefansson Arctic Institute. Arctic Human Development Report. Akureyri, Iceland: Stefansson Arctic Institute, no date.
2. Meakin S, Kurvits T. Assessing the impacts of climate change on food security in the Canadian Arctic, (GRID- Arendal) 2009. (Online) 2009. Available: http://www.grida.no/_res/site/file/publications/foodsec_updt_LA_lo.pdf (Accessed 1 May 2010).
3. Luo ZC, Senecal S, Simonet F, Guimond E, Penney C, Wilkins R. Birth outcomes in the Inuit-inhabited areas of Canada. Canadian Medical Association Journal 2010; 182(3): 235-242.
4. Petrova JG, Vaktskjold A, Vyzletsova PG. The incidence of neural tube defects in Norway and the Arkhangelskaja Oblast in Russia and the association with maternal age. Acta obstetricia et gynecologica Scandinavica 2009; 88(6): 667-672.
5. Vaktskjold A, Talykova L, Chashchin V, Nieboer E and Øyvind Odland J. The Kola birth registry and perinatal mortality in Mončegorsk, Russia. Acta obstetricia et gynecologica Scandinavica 2005; 83(1): 58-69.
6. Arbour L, Gilpin C, Millor-Roy V, Pekeles G, Egeland GM, Hodgins S, Eydoux P. Heart defects and other malformations in the Inuit of Canada: a baseline study. International Journal of Circumpolar Health 2004; 63(3): 251-266.
7. Young TK, Bjerregaard P (Eds). Arctic populations in transition. Toronto: University of Toronto Press, 2008.
8. Statistics Canada. Infant mortality rates, by province and territory, Table 102-0504. (Online) 2010. Available: http://www40.statcan.gc.ca/l01/cst01/health21a-eng.htm (Accessed April 2010).
9. Koch A, Bruce M, Homøe P. Infectious disease. In: TK Young, P Bjerregaard (Eds). Arctic populations in transition. Toronto: University of Toronto Press, 2008.
10. Bjerregaard P, Berner J, Øyvind Odland J. Environment and living conditions. In: TK Young, P Bjerregaard (Eds). Arctic populations in transition. Toronto: University of Toronto Press, 2008.
11. Parkinson A, Sustainable development, climate change and human health in the Arctic. International Journal of Circumpolar Health 2010; 69(1): 99-105.
12. Gauthier M, Simard M, Blais B. Prevalence of Escherichia coli O157:H7 and Salmonella in traditional meats derived from game animals in Nunavik. Rural and Remote Health 10: 1329. (Online) 2010. Available: www.rrh.org.au/journal/article/1329 (Accessed 18 June 2010).
13. Egeland G, Faraj N, Osborne G. Cultural, socioeconomic, and health indicators among Inuit preschoolers: Nunavut Inuit Child Health Survey, 2007-2008. Rural and Remote Health 10: 1365. (Online) 2010. Available: www.rrh.org.au/journal/article/1365 (Accessed 18 June 2010).
14. Pacey A, Nancarrow T, Egeland G. Prevalence and risk factors for parental-reported oral health of Inuit preschoolers: Nunavut Inuit Child Health Survey, 2007-2008. Rural and Remote Health 10: 1363. (Online) 2010. Available: www.rrh.org.au/journal/article/1368 (Accessed 18 June 2010).
15. Igl W, Johansson A, Gyllensten U. The Northern Swedish Population Health Study (NSPHS) - a paradigmatic study in a rural population combining community health and basic research. Rural and Remote Health 10: (Online) 2010. Available: www.rrh.org.au/journal/article/1363 (Accessed 18 June 2010).
16. Revich B, Shaposhnikov D. Extreme temperature episodes and mortality in Yakutsk, East Siberia. Rural and Remote Health 10: 1338. (Online) 2010. Available: www.rrh.org.au/journal/article/1338 (Accessed 18 June 2010).
17. Bonefeld-Jorgensen E. Biomonitoring in Greenland: human biomarkers of exposure and effects - a short review. Rural and Remote Health 10: 1362. (Online) 2010. Available: www.rrh.org.au/journal/article/1362 (Accessed 18 June 2010).
18. Homøe P, Jensen R. Acute mastoiditis in Greenland between 1994-2007. Rural and Remote Health 10: 1335. (Online) 2010. Available: www.rrh.org.au/journal/article/1335 (Accessed 18 June 2010).
19. Harris A, Marquis P, Eriksen H, Grant I, Corbett R, Lie SA, Ursin H. Diurnal rhythm in British Antarctic personnel. Rural and Remote Health 10: 1351. (Online) 2010. Available: www.rrh.org.au/journal/article/1351 (Accessed 18 June 2010).
20. Nancarrow TL, Chan HM. Observations of environmental changes and potential dietary impacts in two communities in Nunavut, Canada. Rural and Remote Health 10: 1370. (Online) 2010. Available: www.rrh.org.au/journal/article/1370 (Accessed 18 June 2010).
21. Lemelin H, Matthews D, Mattina C, McIntyre N, Johnston M, Koster R, and the Weenusk First Nation at Peawanuck. Climate change, wellbeing and resilience in the Weenusk First Nation at Peawanuck: the Moccasin Telegraph goes global. Rural and Remote Health 10: 1333. (Online) 2010. Available: www.rrh.org.au/journal/article/1333 (Accessed 18 June 2010).
22. Miller Mifflin T, Bzdell M. Development of a physiotherapy prioritization tool in the Baffin Region of Nunavut: a remote, under-serviced area in the Canadian Arctic. Rural and Remote Health 10: 1466. (Online) 2010. Available: www.rrh.org.au/journal/article/1466 (Accessed 18 June 2010).
23. O'Neill L. Mental health support in northern communities: reviewing issues on isolated practice and secondary trauma. Rural and Remote Health 10: 1369. (Online) 2010. Available: www.rrh.org.au/journal/article/1369 (Accessed 18 June 2010).
24. James S, O'Brien B, Bourret K, Kango N, Gafvels K, and Paradis-Pastori J. Meeting the needs of Nunavut families: a community-based midwifery education program. Rural and Remote Health 10: 1355. (Online) 2010. Available: www.rrh.org.au/journal/article/1355 (Accessed 18 June 2010).
25. Straume K, Sondena M, Prydz P. Postgraduate training at the ends of the earth - a way to retain physicians? Rural and Remote Health 10: 1356. (Online) 2010. Available: www.rrh.org.au/journal/article/1356 (Accessed 18 June 2010).
26. Straume K, Shaw D. Internship at the ends of the earth - a way to recruite physicians? (Online) 2010. Rural and Remote Health 10: 1366. Available: www.rrh.org.au/journal/article/1366 (Accessed 18 June 2010).


