Introduction
Rural communities and hospitals continue to struggle to attract health professionals1,2. Though the disciplines of medicine and nursing perhaps attract the most public attention, the nature of a smaller integrated system in a rural setting requires enhanced communication and cooperation among professionals in many disciplines, most of which are also under-represented in rural areas. The causes of the maldistribution of health professionals are complex, but one aspect has been unfamiliarity with and stereotyping of rural practice among students currently training. Schools in the different professions often address this by developing rural rotations, courses, and externships, to provide students opportunities to live and work in a rural setting3-5. The basis of this model is that students who have practiced and learned in these environments may be more likely to choose these settings for practice after graduation. Many programs have also been created to provide opportunities for students to work in interdisciplinary teams6-10. It was felt that there was an opportunity to combine both approaches by building an interdisciplinary component into a rural summer experience. The area of geriatrics provided a focus because it is a significant need in rural areas and it requires effective interdisciplinary care.
The project was conducted as part of the author's work within The Area Health Education Center (AHEC) program. The AHEC is a federal, state and grant-funded organization to promote health professionals working in underserved areas.
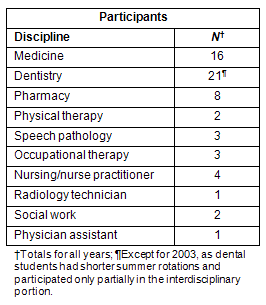
This article describes the development, implementation, and impact of that interdisciplinary component which was offered for students participating in a summer rural experience in Warsaw, New York, from 2003 to 2009. It is difficult to coordinate schedules and academic credit among different schools and universities, so the work was done over the summer. There was no academic credit and it was not an official course for the students. Students received a stipend to participate and either lodging or a mileage allowance for travel. Students came from a wide variety of health related disciplines (Table 1). They were recruited through the professional schools at the University at Buffalo, but also students from other colleges and Universities who had ties to the local area participated. These students were identified through the local AHEC.
Table 1: Participants by discipline with totals for all years
Seminar content and development
The Wyoming County Community Hospital was the base for the experience. Leaders within the administration and clinical disciplines affirmed their interest and capability in providing solid experiences in various settings for the discipline-specific part of the summer work. The majority of the students' six-week experience was spent in the hospital or office setting, participating in the work of a busy rural healthcare system. The interdisciplinary component consisted of a weekly half-day seminar/session, which is the focus of this article.
The learning objectives of the interdisciplinary component had two principle themes, to: (i) model, enhance, and teach communication among students from different health disciplines; and (ii) provide insight into rural living and work.
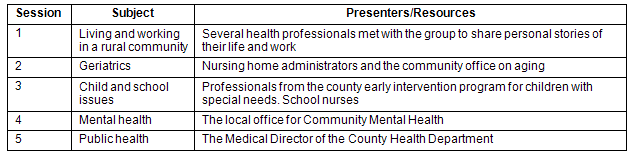
For the first 2 years the curriculum consisted of seminars and discussion of topics relevant to rural living and work (Table 2). All were facilitated by the author with guests and speakers from the local community.
Table 2: Interdisciplinary Seminar 2003-2004
Although the student feedback indicated the seminars were interesting and helpful, they did not adequately address the objective of modeling interdisciplinary clinical care and communication. This became apparent in their evaluations and in the observation that the discussions often involved students' personal perspectives rather than encouraging communication in their professional roles. For this reason, the subsequent 5 years involved a more clinically focused approach to allow students to practice interdisciplinary work.
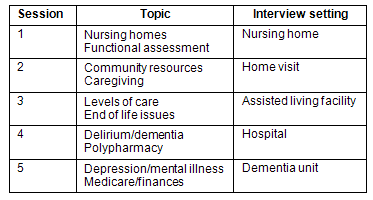
The area of geriatrics supplies an excellent field for interdisciplinary work11. Older patients often have multiple needs, and miscommunication among health providers carries increased risk among these patients. Also, geriatric care is an area of need in many rural areas12. The first two learning objectives were maintained and a secondary objective was added to expose the students to basic issues for the care of the elderly. The half-day sessions involved three components: (i) a discussion of geriatric topics; (ii) a visit with a patient by students in interdisciplinary pairs; and (iii) a discussion about the patients seen. The topics and the setting in which the patients lived changed each week (Table 3).
The curriculum allowed the students to model issues of patient communication and building rapport in their patient interviews. Then in the discussion it was possible to practice interdisciplinary interpretation and reaction to issues such as loss of independence, mobility, care giving needs, end-of-life, polypharmacy, and others.
Table 3: Interdisciplinary Seminar 2005-2009
Results
Students were asked to evaluate the experience relative to the goals by filling out questionnaires. Unfortunately the questions were not the same from year to year because many questions sought specific formative feedback to make changes to aspects of the curriculum. However, two questions were the same each year: (i) Did you find the interdisciplinary half-day session worthwhile? (worth taking time from the discipline-specific work); and (ii) Was the opportunity to interact with students from other disciplines helpful? Every student answered 'yes' to both of these questions. Most of the students felt positively about their summer rural experience, but all of them felt the interdisciplinary work enhanced it. The questionnaire did not ask students to identify their discipline, so no comparisons can be made. This is consistent with most evaluations of interdisciplinary teaching13-16.
Regarding the interdisciplinary communication objective, the following are representative comments:
This was particularly educational for dental students, because I learned a lot of important things that may not necessarily be emphasized in my dental classes. I was able to contribute to our discussions a lot, which made me feel happy and useful.
Seeing patients in pairs helped me a lot. Because I was relatively inexperienced in patient care, my partners explained and taught me certain things that I can use in the future.
In the medical profession, opinions between the various professions can be widespread. The opportunity to discuss situations that effect all the profession was invaluable. Also, trust between the professions is essential.
Regarding the goal of rural exposure there was some variability depending on the student's previous life experience, but for some students the experience was 'eye opening'.
I have learned that the rural setting is a reasonable place to work, even for someone born and raised in the city. I have been able to see many similarities between the two settings.
It is a great learning experience and it provides a view of rural life that people in urban communities have never seen.
Discussion
It can be difficult to assess the long term impact of learning experiences10. Yet providing a positive opportunity to gain both knowledge and personal experience in a new area, in a unique way, may have such impact. However, there are several challenges to such a program.
The very different levels of training and clinical experience led to an educational challenge to make the experience relevant and interesting to all. A student just beginning undergraduate training in Physical Therapy is very different than a second year medical student. This was addressed in several ways. The patient interviews focused on eliciting the patients' stories, not on a formal medical interview. The students were asked to learn about the person, their perception of their health, and their interaction with the healthcare system. During discussion, the group could work together to formulate a problem list, and then talk about how problems might be addressed. The students taught each other. The pairs combined students who were further along in training with those less experienced. The group discussions focused on eliciting everyone's reactions, how they felt about the patient they saw, rather than on a more formal diagnostic assessment.
The experience also has logistical challenges. Warsaw is about a one hour drive from Buffalo, the city where the medical, pharmacy, dental and many other health professional schools are located, so some students chose to commute rather than live in the community. The AHEC completed a hospitality house which allowed students to live in the community and also interact with each other informally, and the students who did this generally obtained a better sense of the rural life. Students from rural backgrounds are influenced less by the living experience3,17.
Funding also presented a challenge. The local AHEC obtained much of the funding from a local foundation committed to the specific needs of this rural community, and clearly not all rural communities have such resources. The quality of the experience and student feedback influenced the School of Dentistry to fund their students who participated. All of the resource people from the community volunteered their time and effort. For 2 years the Director of Nursing at the local nursing home co-facilitated the group, but the time commitment was too great for this to continue. The author received support from the AHEC, through the foundation grants.
Conclusion
This project represents an attempt to address three timely and crucial issues: (i) inadequate numbers of health professionals in rural areas; (ii) poor communication and understanding among different health disciplines; and (iii) the need for more knowledge about and commitment to caring for the elderly.
What was learned, and what can be conveyed to others trying to address these issues? The tightly packed curriculum of most professional schools, and the silo organization of the disciplines, makes a summer experience conducted outside the regular academic calendar more practical and less problematic. Students at different stages in their education and far different levels of clinical experience can interact and learn from one another. Their comments attested to the importance and impact of interdisciplinary interaction. One student wrote:
The overall experience was fantastic. The ability to discuss with people of different professions helps to break some of the barriers medical professions create. Knowing where other professions are coming from helps in understanding a situation or patient better. And in the end, understanding a patient is the best way to give the most appropriate and efficient care.
Involving students in conversations with the elderly without expectations for making diagnoses or providing care can emphasize the human and personal aspects of geriatrics, often overlooked in later training focusing on professional care and assessment. Negative stereotypes of rural practice, of old people, and of health disciplines other than one's own can be broken down by relatively simple educational interventions. These experiences can provide clinical and educational opportunities often cherished by the students.
Acknowledgements
The author thanks the Western New York Rural Area Health Education Center for all their programmatic and logistical support; and the William F Thiel trust for financial support.
References
1. Bushy A, Leipert BD. Factors that influence students in choosing rural nursing practice: a pilot study. Rural Remote Health 5(2): 387. (Online) 2005. Available: www.rrh.org.au (Accessed 5 November 2010).
2. National Conference of State Legislatures. Health Care Workforce Frequently Asked Questions. (Online) 2007. Available: http://www.ncsl.org (Accessed 23 March 2010).
3. Woloschuk W, Tarrant M. Does a rural educational experience influence students' likelihood of rural practice? Impact of student background and gender. Medical Education 2002; 36(3): 241-247.
4. Shannon CK, Baker H, Jackson J, Roy A, Heady H, Gunel, E. Evaluation of a required statewide interdisciplinary Rural Health Education Program: student attitudes, career intents and perceived quality. Rural Remote Health 5(4): 405. (Online) 2005. Available: www.rrh.org.au (Accessed 5 November 2010).
5. Pathman DE, Steiner BD, Jones BD, Konrad TR. Preparing and retaining rural physicians through medical education. Academic Medicine 1999; 74(7): 810-820.
6. McNair R, Stone N, Sims J, Curtis C. Australian evidence for interprofessional education contributing to effective teamwork preparation and interest in rural practice. Journal of Interprofessional Care 2005; 19(6): 579-594.
7. Norris TE, House P, Schaad D, Mas J, Kelday JM. Student providers aspiring to rural and underserved experiences at the University of Washington: promoting team practice among the health care professions. Academic Medicine 2003; 78(12): 1211-1216.
8. Edwards J, Smith P. Impact of interdisciplinary education in underserved areas: health professions collaboration in Tennessee. Journal of Professional Nursing 1998; 14(3): 144-149.
9. Slack M, McEwan M. Pharmacy student participation in interdisciplinary community-based training. American Journal of Pharmaceutical Education 1993; 57(3): 251-257.
10. Hamilton CB, Smith CA, Butters JM. Interdisciplinary student health teams: combining medical education and service in a rural community-based experience. Journal of Rural Health 1997; 13(4): 320-328.
11. Brooks J, Fox DP, Okagbue-Reaves J, Lukomski A. Best practices for an interdisciplinary team-taught course. Educational Gerontology 2009; 35: 818-830.
12. Toner JA, Ferguson KD, Sokal RD. Continuing interprofessional education in geriatrics and gerontology in medically underserved areas. Journal of Continuing Education in the Health Professions 2009; 29(3): 157-160.
13. Lumague M, Morgan A, Mak D, Hanna M, Kwong J, Cameron C et al. Interprofessional education: the student perspective. Journal of Interprofessional Care 2006; 20(3): 246-253.
14. Medves J, Paterson M, Chapman CY, Young JH, Tata E, Bowes DA et al. A new inter-professional course preparing learners for life in rural communities. Rural Remote Health 8(1): 836. (Online) 2005. Available: www.rrh.org.au (Accessed 5 November 2010).
15. Neill M, Hayward KS Peterson T. Students' perceptions of the interprofessional team in practice through the application of servant leadership principles. Journal of Interprofessional Care 2007; 21(4): 425-432.
16. Hayward KS, Powell LT, McRoberts J. Changes in student perceptions of interdisciplinary practice in the rural setting. Journal of Allied Health 1996; 25(4): 315-327.
17. Owen, JA, Conaway MR, Bailey BA, Hayden GF. Predicting rural practice using different definitions to classify medical school applicants as having a rural upbringing. Journal of Rural Health 2007; 23(2): 133-140.
